In a recent report, the Agency for Healthcare Research and Quality1 identified both rural residents and women as segments of the US population that experience health disparities, including disparities in access to medical care. In fact, research has shown rural residents experience important barriers to utilizing health care, including limited financial resources, lack of health insurance, lack of transportation, distance to care facilities, and shortages of qualified practitioners2-9 . Research on rural women's access to health care is more limited, but it suggests similar disparities to rural residents in general, such as lack of health insurance, lack of a primary care physician, and living in communities with few providers10,11. Other work has shown rural women are dissatisfied with the kinds of medical services available, which affects access12, or are largely unaware of options available to them for care13. Findings from studies in Canada support these themes, showing that women living in rural areas are not only geographically isolated from accessing care, but also experience a variety of sociocultural factors that impact their health-seeking behaviors13,14. In order to develop appropriate public health interventions that increase receipt of medical care, more research is needed to identify the personal and community factors that impact the health decision-making of rural women, especially those factors which impede rural women from utilizing health services when needed. This knowledge is especially important, because rural women are at significantly higher risk for poor health outcomes than their urban counterparts7,8. Additionally, rural women play the primary role in family healthcare decision-making10, making them the 'gatekeepers' for their families' health, and thus the health of the broader community12. Consequently, reducing health disparities among rural women requires that public health professionals better understand the components of and barriers to women's health decisions.
By seeking to understand the variety of factors that influence and ultimately may determine health behaviors, multilevel, ecological approaches developed in the fields of public health, psychology, and sociology have shown promise in identifying and addressing personal, social, and health problems15. Importantly, these approaches call us to situate phenomena in a context of intrapersonal, interpersonal, institutional, community, and larger cultural and policy factors, all of which influence the phenomena either directly or indirectly16,17. Health decisions and health behavior are a function of a dynamic and complex interaction of these factors16. From smoking cessation programs to obesity prevention, ecological perspectives, have been successful in investigating health behaviors18-21.
Reschovsky and Staiti8 and Davidson, Andersen, Wyn, and Brown22 distinguished between individual and community/systemic characteristics of healthcare access and outcomes. Decisions about and utilization of health services by low-income populations are influenced by individual characteristics including attitudinal, social and demographic predispositions, perceived and evaluated needs, and factors such as low socioeconomic status and lack of health insurance. Litaker, Koroukian, and Love's work23 is indicative of the importance of including a variety of contexts when exploring health behaviors and decision-making. For example, researchers have shown that poverty affects decision-making related to care, especially among food-insecure patients, or patients who are unable to acquire enough food to meet caloric needs due to insufficient money or other resources24. Indeed, recent studies have shown that poverty, food insecurity, and rurality have all been correlated with depression, which may also influence health decision-making25,26. Further, lack of after-hours care, longer appointment wait times in rural community clinics, and even age (ie adults compared with children and seniors) are all associated with lower levels of entry into and continuity of primary care6. Further, through the availability of qualified professionals and/or facilities for care, the community context facilitates or impedes the ability to meet health needs2,4,5,11,22,24.
Although research on factors associated with low-income rural women utilizing care is limited, findings to date suggest there are important personal and community barriers. For example, at the personal level, lack of insurance3,6,9,10 and limited financial resources4,8 have both been shown to be significant barriers to care and thus important influences on the health decisions made by rural women. Additional examples of personal-level barriers, some of which begin to exhibit the systemic interactivity of socio-ecological models by relating closely to other ecological levels, include lack of information and/or language barriers7,9 and perceived stigmas, especially related to mental health issues10,11. Beyond these individual-level barriers exist larger systemic or community-level impediments. At this level, lack of public transportation2,4, and distance to care facilities5,7 significantly impede healthcare access, as does a shortage of practitioners8,11.
Additionally, researchers have given increasing attention to prescription filling and adherence behaviors among underserved or disadvantaged populations. Adherence to prescriptions has been correlated with higher quality patient-physician relationships and few transportation problems27. Conversely, transportation difficulties, limited healthcare supply, lack of quality health care, social isolation, and financial constraints all have been shown to be key barriers to pharmaceutical care for rural adults28. The impact of financial constraints on prescription filling and adherence behaviors among rural and low-income populations cannot be overstated. A higher percentage of prescriptions are paid for with cash (18% vs 13%) and Medicaid (16% vs 10%) in rural areas than in urban areas27. While programs that provide outpatient medication assistance29-33, patient advocacy30, and identification of and assistance to high-risk populations31,34 have demonstrated effectiveness in overcoming financial and geographic barriers to health care and prescription access and utilization, these programs have not become widespread.
The purpose of this study was to examine individual and community variables associated with the health decisions of rural women specifically related to accessing a physician and filling prescriptions. Not seeking or adhering to care recommendations may extend the course of disease, thereby protracting patients' problems and increasing the burden of disease on the community. As such, a deeper understanding of the various factors influencing these decisions may have important implications for clinical practice and policy making. Specifically, this study sought to answer the following research questions:
- which demographic-, individual-, and community-level factors influence whether rural, low-income women visit a doctor when needed?
- which of these factors influence whether these women delay or forgo filling prescription medications?
Findings have the potential to increase contextual understanding of factors associated with rural women's health decisions, which may lead to development and testing of appropriate health services interventions for this underserved population.
Data
Analyzed data were from two sources. The primary data source came from a USDA-funded project known as Rural Families Speak (RFS, NC-223/NC-1011), which is a multi-state (CA, IN, IA, KY, LA, MD, MA, MI, MN, NE, NH, NY, OH, OR, SD, WV), longitudinal study of low-income rural women and their families designed to better understand how rural families were faring after national Welfare Reform in 1996. The RFS protocol was approved by an institutional review board at all study sites. Participants from 23 rural counties were included in the study. 'Rural' was defined using Butler and Beale's rural-urban continuum codes35, and the majority of participants (72.4%) lived in counties rated 6 (population of 2500 to 19 999, adjacent to metro area), 7 (population of 2500 to 19 999, not adjacent to metro area), or 8 (completely rural or <2500 urban population, adjacent to metro area). The remaining participants lived in states without Beale codes of 6 through 8. However, participants lived in counties with population centers that did not exceed 10 000. Data from women participating in RFS were matched to data from the Community Health Status Indicators Project (CHSI)36 based on the participants' county of residence. The CHSI is a publicly available, nationwide data set on over 200 public health indicators. Data were obtained from a variety of federal agencies, including the Department of Health and Human Services and the Centers for Disease Control, and are reported at the county level and. Reliability and validity for the dataset as a whole are not provided; however, data were compiled and calculated in such a way that definitions and calculations of health measures were consistent across communities (counties) and data sources.
Sampling and recruitment for 'Rural Families Speak'
A convenience sample of 413 participants was solicited for inclusion in wave 1 of RFS. Participants were recruited via flyers from places that serve low-income families, including social service agencies, Head Start programs, low-income housing units, and public health clinics. The flyers described study details and eligibility requirements. To be eligible women had to be at least 18 years, have at least one child under the age of 14, and be eligible for Food Stamps or the Supplemental Nutrition Program for Women Infants and Children (WIC). Interested volunteers called the state's study coordinator, who reconfirmed eligibility and scheduled interviews. On average, 18 participants came from each county (range 10-43 participants), and the percent of persons living at or below the federal poverty line in each county averaged 12.7% (range 4.8-23.1%).
Data collection for 'Rural Families Speak'
All participants provided informed consent prior to data collection. Trained interviewers conducted 3 in-person interviews in the participants' native language (English or Spanish), annually between 2000 and 2002. Both quantitative and qualitative self-report data were collected using an interviewer-administered questionnaire. Quantitative data included questions from validated instruments. Qualitative data included questions that pertained to specific constructs measured in the quantitative protocol. Depending on the study site, participants were compensated $20-$50 for their time based on regional rates of remuneration (ie differences in cost of living).
Sample
For the current study, quantitative data were analyzed only from Wave 3 (n = 266) collected in 2002 matched with county-level data from the CHSI. The focus was on Wave 3, because these data included an expanded section on health, and specifically the dependent variables of interest (not seeing a doctor when needed and delaying or not filling prescribed medications), which were not available in the first two waves. The health section was expanded in Wave 3, based on findings from the previous 2 years of data that revealed the importance of health in these rural women's lives. Additional data about the women's mental and physical health status, as well as new data on access to and utilization of health care, were included. Given that the RFS qualitative protocol was specific to the quantitative data collected, and given that quantitative county-level data were matched from another source, analysis of the qualitative data were not included in the current study, because the qualitative data could not be triangulated with the CHSI data.
Measures
The ecological models suggested by Reschovsky and Staiti8 and Davidson et al22 delineate 3 levels of independent variables: (i) intrapersonal; (ii) interpersonal; and (iii) community level influences. The present study measured variables according to this model.
The dependent variables included two self-reported, dichotomous variables that assessed two forms of health decision-making. The first variable was a report of whether in the last year the participant needed to see a physician but did not go (yes = 1/no = 0). Need was defined as having a health concern that the participant thought might require and/or improve with medical attention. The second variable was a report of whether in the last year the respondent did not fill or postponed filling medication that was prescribed by a healthcare provider (yes = 1/no = 0).
Intrapersonal demographic variables included age, race/ethnicity, marital status, educational attainment, employment status, and family level of poverty. Age was measured continuously. Race/Ethnicity was measured by 4 categories (White, Latina, Black, and other). Marital status was measured using 3 categories (single, married/living with partner, and divorced, widowed, or separated). Educational level also was measured in 3 categories (less than a high school degree (<12 years), high school degree or equivalent (12 years), and more than a high school degree (>12 years). Employment status was dichotomous (employed = 1/unemployed = 0). Family poverty level was measured continuously as the family's income as a percent of the federal poverty line in the year of data collection.
Three intrapersonal health variables were measured. Chronic health conditions were measured using the summed score on an index of 15 conditions based on Sturm and Wells'37 study of morbidities associated with poverty. These conditions included arthritis, asthma, back problems, bladder infections, cancer, chronic pain, diabetes, heart problems, hepatitis, high blood pressure, liver problems, migraines/headaches, permanent disability, reproductive problems, and seizure disorder. For each condition, women reported whether they had the disorder (1) or not (0). A higher score (range = 0-15) indicated more chronic health conditions. Chronbach's α for this scale was 0.57 in the sample. Depression was measured using the Center for Epidemiologic Studies-Depression Scale (CES-D), which was designed to measure depressive symptoms in the general population38. The instrument includes 20 items on a 4-point Likert scale. Total scores range from 0 to 60 with a cut-off score of 16 indicating symptoms of clinical depression. The cut-off score was used to categorize women as having or not having clinically significant depressive symptoms (1/0). Reliability for the CES-D in the general population and this sample was α = 0.85. An injury or illness in the last year was measured dichotomously (yes = 1/no = 0), indicating whether the participant had an injury or illness that affected activities of daily living.
Two interpersonal health variables were measured. Interpersonal health variables were defined as those factors that are commonly influenced by individual experience and decision-making in combination with outside influences, such as employment that provides health insurance, marriage to a partner who has health insurance, and/or interaction with others who may convey health-related information, such as a social worker, friend, family member, or religious advisor. Health insurance status was measured dichotomously (insured = 1/uninsured = 0). Whether the respondent believed there were primary care services available in her community was also measured dichotomously (yes = 1/no = 0).
Three community health variables were analyzed:
1. The rate of primary care physicians (measured continuously according to the number of primary care physicians per 100 000 people living in the county).
2. Whether there was a community health center in the county (measured dichotomously as yes = 1/no = 0).
3. Whether the county was in a health professional shortage area (also dichotomous as yes = 1/no = 0).
Data analysis
All data were analyzed using STATA 9.0 (STATA Corp; College Station, TX, USA). First, descriptive statistics were computed for the sample (proportions for categorical variables and means and standard deviations for continuous variables). Then univariate logistic regression models were run to assess individually the intrapersonal, interpersonal, and community factors associated with not seeing a physician when needed and delaying or not filling prescriptions. In order to capture the effects of all ecological models, a hierarchical variable entry procedure was used for each multivariate model and entered variables in 4 blocks corresponding with the four layers of ecological influence: intrapersonal demographic variables (age, race/ethnicity, educational status, marital status, family poverty level), intrapersonal health variables (chronic health conditions, depression, injury or illness in the last year), interpersonal health variables (health insurance status and belief that primary care physicians are available in the community), and community health variables (county primary care physician rate per 10 000 people, presence of a community health center, and whether the county is in a health physician shortage area). This approach is consistent with meeting the minimum requirement of 10 outcome events per predictor variable in logistic regression39. Probabilities were expressed as odds ratios, and significance was defined as p ≤0.05. The final multivariate models were used for interpretation.
Descriptive statistics
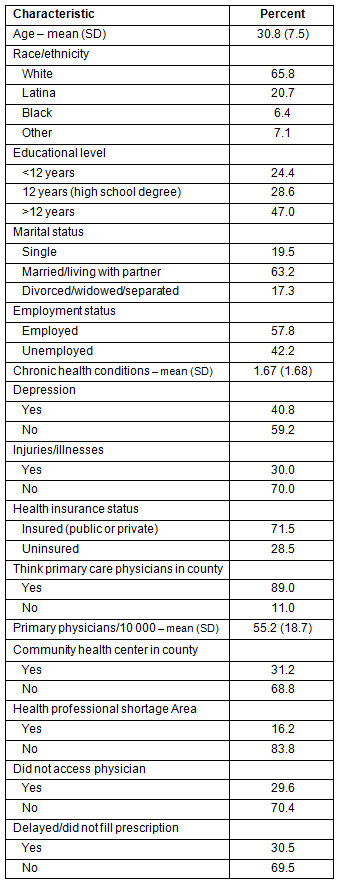
Demographic characteristics are presented (Table 1). Respondents were on average 30.8 years of age (SD = 7.5). The majority (65.8%) identified as White, followed by Latina (20.7%), Other (7.1%) and Black (6.4%). Just over one-half had a high school degree (28.6%) or less (24.4%), while 47.0% had some education beyond high school. Most respondents (63.2%) were married or living with a partner, while 19.5% were single and 17.3% were divorced, separated, or widowed. More than half were employed (57.8%), and nearly three-quarters (71.5%) had health insurance. The majority (89.0%) also believed there were primary care physicians available in their communities. There was a high prevalence of clinically significant depressive symptoms (40.8%). Women reported 1.67 chronic health conditions (SD = 1.68), and 30% reported an injury or illness in the last year. The average primary care physician rate per 10 000 people was 55.2 (SD = 18.7), and 16.2% of counties were in health professional shortage areas, while 31.2% had a community health center. Regarding unmet needs, 29.6% of participants reported they did not access a physician when they needed, and 30.5% reported delaying or forgoing filling prescriptions.
Table 1: Demographic characteristics
Physician access
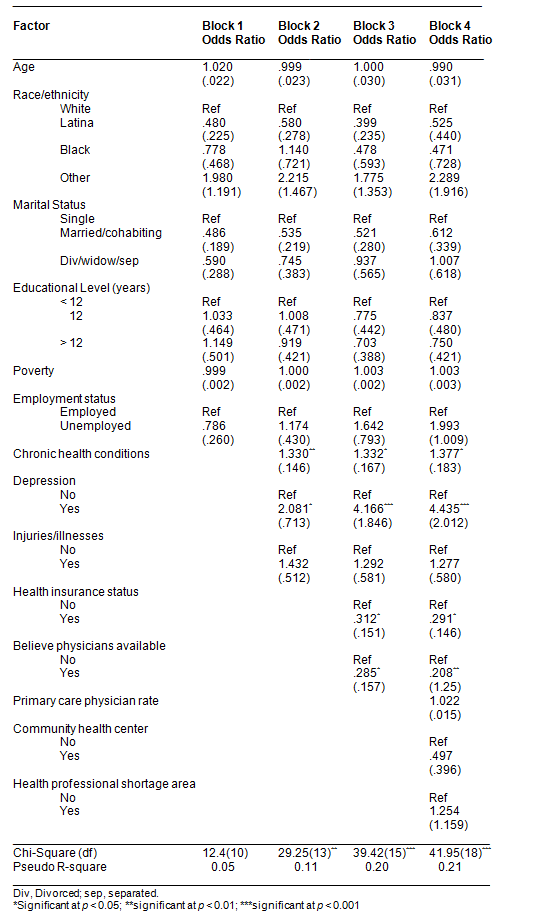
The results are presented of the multivariate logistic regression model for the probability of not accessing a physician when needed (Table 2). When the first block of demographic variables was entered, no statistically significant variables emerged. When the second block of health variables was entered, having more chronic health conditions (OR = 1.33, p = 0.01) and having clinically significant depressive symptoms (OR = 2.08, p = 0.03) were both associated with increased odds of not seeing a physician when needed. After entering the third block, depressive symptoms (OR = 4.17, p = 0.001) and chronic health conditions (OR = 1.33, p = 0.02) remained significant. Further, both having insurance (OR = 0.31, p = 0.02) and believing primary care physicians were available in the respondent's community (OR = 0.28, p = 0.02) were associated with decreased likelihood of not accessing a physician when needed. In the final model, after community variables were entered in block 4, there were no significant changes in the model. Women with depressive symptoms (OR = 4.44, p = 0.001) and more chronic health conditions (OR = 1.38, p = 0.02) were significantly less likely to access a physician when needed. Conversely, health insured women (OR = 0.29, p = 0.01) and women who believed primary care physicians were available in the respondent's community (OR = 0.21, p = 0.01) were significantly more likely to access a physician when needed. The community factors of physician rate, presence of a health center, and being located in a health professional shortage area were not associated with physician access.
Table 2: Multivariate logistic regression model for not accessing a physician when needed
Prescriptions
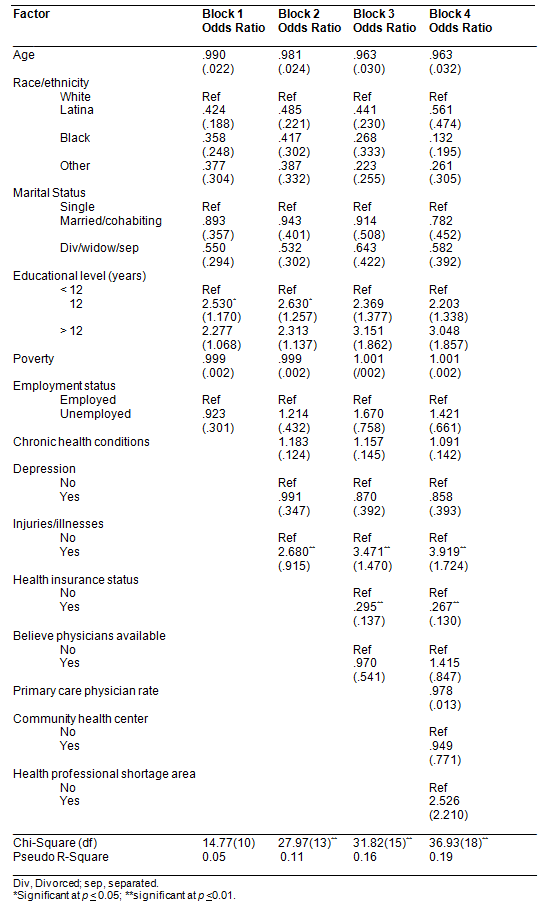
The results of the multivariate logistic regression model for not filling or postponing filling a prescription medication is presented (Table 3). Within the block of demographic variables, only having a high school degree was associated with an increased likelihood of delaying or not filling prescribed medications (OR = 2.53, p = 0.04). After entering the second block of health variables, having a high school degree continued to be associated with increased odds of delaying or not filling prescriptions (OR = 2.63, p = 0.04). Having an injury or illness was the only significant health variable, and it was associated with increased odds of delaying or not filling prescriptions (OR = 2.68, p = 0.004). When the interpersonal health variables were entered in block 3, high school degree was no longer significant. Injuries/illnesses in the last year continued to be statistically significant (OR = 3.47, p = 0.003), while having health insurance was associated with decreased odds of not filling prescriptions (OR = 0.29, p = 0.01). In the final model, after entering the community health variables, again injuries/illnesses and being insured were associated with delaying or not filling prescriptions. Women with health insurance were less likely to delay or not fill prescriptions (OR = 0.27, p = 0.01), while women with injuries and illnesses were more likely to delay or not fill prescriptions (OR = 3.92, p = 0.01).
Table 3: Multivariate logistic regression model for not filling prescriptions
Discussion
This study examined the relationships among intrapersonal, interpersonal, and community factors and health decision-making related to seeing a physician and prescription adherence in rural women. Findings suggest that intra- and interpersonal factors most influenced this sample of rural women's lack of access to care. Specifically, women with more chronic health conditions and depression were less likely to access a physician when needed. Conversely, women who believed primary care physicians were available in the community were more likely to access a physician when needed. Women with health insurance also were less likely to delay or forgo filling prescriptions, while women reporting injuries and illnesses in the last year were more likely to delay or not fill prescriptions. Community factors such as county primary care physician rate, living in a health professional shortage area, and living in a county with a community health center were not related to accessing physicians or adhering to prescriptions after controlling for intra- and interpersonal factors.
Women with more chronic health conditions and depression were less likely to go to the doctor when needed. This suggests that rural women may be at high risk for delaying seeking treatment for symptoms associated with chronic or emergent health conditions, especially when financial resources are limited, as in this sample. Research suggests that rural women with depressive symptoms may not recognize the symptoms as depression11. Thus, they may attribute somatic symptoms to something other than a mental health problem, or make a decision that the problem is not severe enough to seek treatment given other pressing needs in the family. Future research should investigate the role of poor mental health in healthcare decision-making, especially in rural areas where rates of mental health disorders among women are high40-42 and the perceived stigma associated with having a mental health problem that prevents many rural residents from seeking treatment43.
Believing that physicians were available in the community increased the likelihood that women sought a doctor when needed. This is an important finding, given the research that suggests low physician availability is a key barrier to healthcare access4,11,22. Interestingly, the actual availability of healthcare services (healthcare providers, community health centers, or living in a health professional shortage area) was not a significant factor in the model. This is counter to other research that has shown low provider availability in rural areas is a key barrier to be addressed11,44,45. This finding may reflect the nature of the dependent variable. That is, this study focused on women's perceived need for a physician and their decisions around prescribed medications, which likely involve different decision-making processes than accessing preventive care. Other research has suggested that availability is also subjective; that is, while there may be providers practicing in the area, the hours or location may not be suitable or they may be viewed as transient due to high rates of out-migration and thus not worth attempting to establish care46. Future research should examine factors associated with different kinds of healthcare seeking decisions (ie emergent versus routine/preventive) and interventions that simultaneously improve rural residents' knowledge about what medical services are available and increase the actual availability of services themselves should be developed and tested.
Given the current context of healthcare reform, an interesting finding was that health insurance was not associated with increased likelihood of seeing a physician when needed and not filling prescribed medications. This finding is counter to other research that has demonstrated health insurance is an important enabling factor that enhances access to care6,9,11,22. A partial explanation may be the already high rate of un-insurance in the sample (28.5%). In rural areas, health insurance coverage is particularly challenging, because most jobs are low-wage and provide few benefits3,10. Further, working rural residents may make too much to qualify for their state health insurance plans. As such, public health efforts should focus on educating low-income people regarding their eligibility for Medicaid and how to apply for insurance. Public policies to expand Medicaid eligibility for working poor families would especially benefit rural, low-income women like those in this sample47. Additionally, prescription assistance programs, while shown to be effective29-34, may need to be better utilized and expanded in rural areas to offset insurance and financial capacity shortfalls. Recommended practices related to Medicaid access include examination of Medicaid policies and procedures, education for providers and families, developing regional health networks or collaboratives, and involving consumers in defining access issues48,49. Previous research has identified stigmas associated with utilizing or needing to utilize Medicaid50. Consequently, research and practice efforts also should address how stigma within rural communities influences the decision to use or not use Medicaid and other health services for low-income people.
Having a serious injury or illness within the past year was associated with failure or delay in filling prescriptions when other factors were controlled. This finding suggests low-income women who experience unexpected health needs may forgo treatment due to limited financial resources. This is a serious public health concern, because rural areas experience high rates of unintended injuries51. Women may be prolonging illness and/or making themselves more susceptible to illnesses and injuries becoming chronic in nature, thereby compromising their long-term health and wellbeing. This offers further support for the need to expand Medicaid coverage and educate rural residents about what services are available to them.
Some studies have shown that rural women may access providers other than physicians, such as public health nurses52, and that many may opt for more traditional medicines or complementary and alternatives medicines53. Research should examine both the variety of providers rural women access, including the use of complementary and alternative therapies, and the types of conditions for which they seek different kinds of care. This would help researchers and practitioners better understand health behaviors and health decision-making among rural women, including the best ways to implement healthcare reforms.
The status of current research is simple and clear: rurality affects women's health in multiple ways54. Future research into the ecological factors influencing unmet healthcare needs will assist professionals and policy makers in reducing unmet needs. Feasibility and implementation studies for prescription assistance programs, high-risk patient advocacy, and rural healthcare infrastructure should be conducted. This study suggests that an ecological approach to understanding unmet healthcare needs is both useful and appropriate. Health decisions and health behaviors are the result of potentially complex and multi-factorial models, as suggested by the literature and some of the preliminary findings in this article. However, it is impossible to fully capture, expound, and integrate each of these factors in one article. Detailed research into separate ecological factors - intrapersonal, interpersonal, community, and policy - is thus needed to expand our knowledge of and ability to address unmet health needs for rural women. This research should not simply explore factors at each individual level, but should continue to integrate multiple ecologic levels in theory and analysis.
Limitations
While this sample includes women from rural areas in 16 states, the women in this study do not comprise a representative sample. As such, findings may not be generalizable to all rural, low-income women. In addition, data are self-reported. A review of actual medical records may be more accurate as women in this study may have under- or over-reported their physician and prescription access. Data also were taken from a cross-sectional sample. Therefore, no causal associations can be made. Future studies should include representative samples and data from medical records. Additionally, the study examined only two measures of unmet health needs among rural women - not accessing a physician when needed and failure or delay in filling prescriptions - both of which represent illness behaviors as opposed to preventive behaviors. Other potential ecological indicators of unmet needs should be examined, such as the role these factors in increasing preventive health behaviors and healthcare access. Such data may best be captured through qualitative or mixed-method research. Finally, this article assumes that accessing a physician when needed and prescription adherence are inherently 'desirable' activities in this population. However, rural woman may not necessarily agree with this assumption. In fact, a recent study showed that the underlying culture of self-reliance among low-income rural people contributes to a reluctance to seek medical care until a health problem interferes with daily functioning55. More research that explicitly incorporates the perspectives and underlying cultural beliefs of low-income rural women would improve understanding about values that influence health decision-making.
Findings from this study indicated significant influences on unmet needs at two ecological levels, intrapersonal and interpersonal, suggesting the need for expanded healthcare services and education related to available services. While community level factors were not significant, it is clear that knowledge about community healthcare systems, including available providers, was an important intrapersonal factor associated with health decision-making. As such, public healthcare systems need to focus not only on developing greater community capacity for providing care, including increasing the types and quality of available services, but also ensure that low-income women living in rural areas have the knowledge about these services. Greater consumer education is needed to overcome this barrier. Further, there is a need to conduct additional research, especially qualitative research and research that explores various ecological barriers, to better understand the phenomena at work when health needs are not met. This combined approach may improve access to care and improve the overall health and wellbeing of rural women in the USA.
Acknowledgements
This research was supported in part by USDA/CSREES/NRICGP Grant 2001-35401-10215, 2002-35401-11591, and 2004-35401-14938 and NIH/NIDA Grant 5 K12 DA014040-07 (Simmons). The opinions expressed herein are solely those of the authors.
References
1. Agency for Healthcare Research and Quality. 2006 National Healthcare Disparities Report, 07-0112. Washington, DC: US Department of Health and Human Services, 2006.
2. Arcury TA, Preisser JS, Gesler WM, Powers JM. Access to transportation and health care utilization in a rural region. Journal of Rural Health 2005; 21: 31-38.
3. Berk M, Schur C, Cantor J. Ability to obtain health care: recent estimates from the Robert Wood Johnson National Access to Care survey. Health Affairs 1995; 14: 139-146.
4. Boydell K, Pong R, Volpe T, Tilleczek K, Wilson ESL. Family perspectives on pathways to mental health care for children and youth in rural communities. Journal of Rural Health 2006; 22: 182-188.
5. Chan L, Hart LDG. Geographic access to health care for rural Medicare beneficiaries. Journal of Rural Health 2006; 22: 140-146.
6. Forrest C, Starfield B. Entry into primary care and continuity: the effects of access. American Journal of Public Health 1998; 88: 1330-1336.
7. Hartley D. Rural health disparities, population health, and rural culture. American Journal of Public Health 2004; 94: 1675-1678.
8. Reschovsky J, Staiti A. Access and quality: does rural America lag behind? Health Affairs 2005; 24: 1128-1139.
9. Sherrill W, Crew L, Mayo R, Mayo W, Rogers B, Haynes D. Educational and health services innovation to improve care for rural Hispanic communities in the USA. Rural and Remote Health 5: 402. (Online) 2005. Available: http://www.rrh.org.au (Accessed 21 February 2011).
10. Gaston M. 100% access and 0 health disparities: changing the health paradigm for rural women in the 21st century. Women's Health Issues 2001; 11: 7-16.
11. Simmons LA, Anderson E, Braun B. Health needs and health care utilization among rural, low-income women. Women & Health 2008; 47(4): 53-69.
12. Hemard JB, Monroe PA, Atkinson ES, Blalock LB. Rural women's satisfaction and stress as family health care gatekeepers. Women & Health 1998; 28: 55-77.
13. Roberts J, Falk M. Women and health: experiences in a rural regional health authority. (Online) 2009: Available: http://www.pwhce.ca/pdf/rha.pdf (Accessed 21 February 2011).
14. Sutherns R, McPhedran M, Haworth-Brockman M. Rural, remote, and northern women's health: Summary report. (Online) 2009: Available: http://www.pwhce.ca/pdf/rr/RRN_Summary_CompleteE.pdf (Accessed 21 February 2011).
15. Sallis J, Owen N. Ecological models of health behavior. In: K Glanz, B Rimer, F Lewis (Eds). Health behavior and health education: theory, research, and practice, 3rd edn. San Francisco, CA: Jossey-Bass, 2002; 462-484.
16. McLeroy K, Bibeau D, Steckler A, Glanz K. An ecological perspective on health promotion programs. Health Education Quarterly 1988; 15: 351-377.
17. Moos R. Social-ecological perspectives on health. In: Stone G, Cohen F, Adler N, editors. Health psychology: A handbook. San Francisco, CA: Jossey-Bass, 1980.
18. Documet P, Green H, Adams J, Weil L, Stockdale J, Hyseni Y. Perspectives of African American, Amish, Appalachian, and Latina women on breast and cervical cancer screening: Implications for cultural competence. Journal of Health Care for the Poor and Underserved 2008; 19: 56-74.
19. Dywer J, Needham L, Simpson J, Jeeney E. Parents report intrapersonal, interpersonal, and environmental barriers to supporting healthy eating and physical activity among their preschoolers. Applied Physiological Nutrition & Metabolism 2008; 33: 338-346.
20. Kim Y. Reducing disparities in dental care for low-income Hispanic children. Journal of Health Care for the Poor and Underserved 2005; 16: 431-443.
21. Sword W. A socio-ecological approach to understanding barreirs to prenatal care for women of low income. Journal of Advanced Nursing 1999; 29: 1170-1177.
22. Davidson P, Andersen R, Wyn R, Brown E. A framework for evaluating safety-net and other community-level factors on access for low-income populations. Inquiry 2004; 41: 21-38.
23. Litaker D, Koroukian SM, Love TE. Context and healthcare access: looking beyond the individual. Medical Care 2005; 43(6): 531-540.
24. Simmons L, Modesitt S, Brody A, Leggin A. Food insecurity among cancer patients in Kentucky: a pilot study. Journal of Oncology Practice 2006; 2: 214-220.
25. Huddleston-Casas C, Charnigo R, Simmons LA. Food insecurity and maternal depression in rural, low-income families: a longitudinal investigation. Public Health Nutrition 2009; 12(8): 1133-1140.
26. Lent MD, Petrovic LE, Swanson JA, Olson CM. Maternal mental health and the persistence of food insecurity in poor rural families. Journal of Health Care for the Poor and Underserved 2009; 20(3): 645-661.
27. Wroth TH, Pathman DE. Primary medication adherence in a rural population: the role of the patient-physican relationship and satisfaction with care. Journal of the American Board of Family Medicine 2006; 19: 478-486.
28. Goins RT, Williams KA, Carter MW, Spencer M, Solovieva T. Perceived barriers to health care access among rural older adults: a qualitative study. Journal of Rural Health 2005; 21: 206-213.
29. Harmon GN, Lefante L, W Roy, KH Ashby, D Jackson, D Barnard et al. Outpatient medication assistance program in a rural setting. American Journal of Health-System Pharmacy 2004; 61: 603-607.
30. Johnson PE. Patient assistance programs and patient advocacy foundations: Alternatives for obtaining prescription medications when insurance fails. American Journal of Health-System Pharmacy 2006; 63: S13-17.
31. Prutting SM, Cerveny JD, MacFarlance LL, Wiley MK. An interdisciplinary effort to help patients with limited prescription drug benefits afford their medication. Southern Medical Journal 1998; 91: 815-820.
32. Stewart MK, Redford R, Poe K, Veach D, Hines R, Beachler M. The Arkansas River Valley Health Cooperative: Building a three-pronged approach to improved health and health care. Journal of Rural Health 2003; 19: 384-390.
33. Torres MC, Herman D, Montano S, Love L. Pharmacy assistance programs in a community health center setting. Journal of the National Medical Association 2002; 94: 1077-1086.
34. Kripalani S, Price M, Vigil V, Epstein KR. Frequency and predictors of prescription-relate issues after hospital discharge. Journal of Hospital Medicine 2008; 3: 12-19.
35. Butler MA, Beale C. Rural-Urban Continuum Codes for Metro and Nonmetro Counties, 1993. Report No.: 9425. Washington, DC: US Government Printing Office, 1994 .
36. Health Resources and Services Administration. Community health status indicators project. Washington, DC: US Department of Health and Human Services, 2000.
37. Sturm R, Wells KB. Does obesity contribute as much to morbidity as poverty or smoking? Public Health 2001; 115: 229-235.
38. Radloff L. The CES-D Scale: a self-report depression scale for research in the general population. Applied Psychological Measurement 1977; 1: 385-401.
39. Peduzzi P, Concato J, Kemper E, Holford T, Feinstein A. A simulation study of the number of events per variable in logistic regression analysis. Journal of Clinical Epidemiology 1996; 49: 1373-1379.
40. Carruth A, Logan C. Depressive symptoms in farm women: effects of health status and farming lifestyle characteristics, behaviors, and beliefs. Journal of Community Health 2002; 27: 213-228.
41. Hauenstein EJ. No comfort in the rural south: women living depressed. Archives of Psychiatric Nursing 2003; 17: 3-11.
42. Simmons LA, Huddleston-Casas CA, Berry AA. Low-income rural women and depression: factors associated with self-reporting. American Journal of Health Behavior 2007; 31(6): 657-666.
43. Spoth R. Challenges in defining and developing the field of rural mental disorder preventive intervention research. American Journal of Community Psychology 1997; 25: 425-448.
44. Ricketts T, Johnson-Webb K, Randolph R. Populations and places in rural America. In: T Ricketts (Ed.). Rural health in the United States. New York: Oxford University Press, 1999; 7-24.
45. Schur C, Franco S. Access to health care. In: T Ricketts (Ed.). Rural health in the United States. New York: Oxford University Press, 1999; 25-37.
46. National Center for Nursing Research. Rural America: Challenges and opportunities. In: National Center for Nursing Research. Report of the priority expert panel on community-based health care: Nursing strategies. Bethesda, MD: NINR, 1999. http://www.ninr.nih.gov/.
47. Miller EA, Weissert WG. Geography still dictates Rx coverage for many near-poor and disabled persons. Journal of Aging Social Policy 2007; 19: 77-96.
48. Hartley D. Best practices in rural Medicaid managed behavioral health. Portland: ME: Maine Rural Health Research Center, 2008.
49. Solomon J. Helping families enrolled in Medicaid get prescription drugs. Hamilton: NJ: Center for Health Care Strategies, 2008.
50. Stuber J, Kronebusch K. Stigma and other determinants of participation in TANF and Medicaid. Journal of Policy Analysis and Management 2004; 23(3): 509-530.
51. Boland M, Staines A, Fitzpatrick P, Scallan E. Urban-rural variation in mortality and hospital admission rates for unintentional injury in Ireland. Injury Prevention 2005; 11: 38-42.
52. Leipert BD. Women's health and the practice of public health nurses in northern British Columbia. Public Health Nursing 1999; 16: 280-289.
53. Wardle J, Chi-Wai L, Adams J. Complementary and alternative medicine in rural communities: current research and future directions. Journal of Rural Health 2010. 27: Available: http://onlinelibrary.wiley.com/doi/10.1111/j.1748-0361.2010.00348.x/full.
54. Leipert BD, George JA. Determinants of rural women's health: a qualitative study in southwest Ontario. Journal of Rural Health 2008; 24(2): 210-218.
55. Murimi MW, Harpel T. Practicing preventive health: The underlying culture among low-income rural popuulations. Journal of Rural Health 2010; 26(3): 273-282.
Published 11 March 2011; modified 29 March 2011.
A correction was made to presentation of the data in Tables 2 and 3.

