Childhood obesity is a worldwide public health epidemic. In the USA, 19.6% of 6-11 year olds and 18.1% of 12-19 year olds are classified as obese, with rates having doubled and tripled, respectively, over the past 30 years1,2. Childhood obesity rates appear to be more pronounced among youth in rural areas of the USA3,4. Rural children are approximately 25% more likely to be overweight than their metropolitan counterparts5.
Low-income rural children may be at even greater risk. A 2007 survey of Maine parents with children enrolled in Medicaid/State Children's Health Insurance Program (SCHIP) ('MaineCare') found that 27% of all MaineCare children ages 2-18 years are overweight compared with 16% among Maine children in general. MaineCare children living in rural areas were at even greater risk, with 36% of MaineCare children in rural areas overweight compared with 27% in urban areas6. Reasons for rural-urban differences in obesity rates within families of comparable income are still unknown, but diet and limited access to healthy food may be factors.
To explore the contribution that the rural food environment may have on children's eating habits and childhood obesity, the authors were awarded a Robert Wood Johnson Foundation (RWJF) Health Eating Research (HER) grant. The mission of the HER program is to support research on environmental and policy strategies with strong potential to promote healthy eating among children to prevent childhood obesity, especially among low-income and racial and ethnic populations7.
The rural food environment
The availability of retail food outlets in communities that sell high quality, nutritious and affordable foods may be an important factor for encouraging families to select a healthy diet and potentially reduce obesity rates. Researchers have stressed the importance of community 'environmental' exposures that influence food intake, rather than on individual behavior when studying contributors to obesity8,9. Understanding the ways in which the food environment impacts childhood obesity may be a key component of designing interventions that increase the availability of fresh, healthy and affordable foods, thus improving the health of communities.
Some studies in urban areas have found that poor food environments in low-income neighborhoods (eg fewer supermarkets) affect fruit and vegetable consumption in low-income households, leading to high rates of obesity10-14. A 2008 comprehensive literature review found the association between the availability of healthy versus unhealthy food and obesity has been inconsistent across studies, suggesting that more research is needed15. In a more recent literature review examining the relationship between obesity and the community and consumer food environment, 5 of 7 studies reported significant associations between obesity rates and community food environment variables, subject to limitations. The authors call for additional studies of the food environment and obesity16.
Research and interest in this area has led to the term 'food desert', which describes areas with poor access to healthy and affordable food17. When people lack access to healthy food, they are often left with options such as convenience stores and fast food outlets, where food choices are usually more expensive and less healthy than in supermarkets18. Mapping has shown that food deserts are also frequently in areas with high rates of obesity and chronic, diet-related diseases17.
The association between the food environment and obesity has not been widely tested in rural areas where access to healthy foods is a challenge19. This lack of research has left policy-makers with little direction when targeting interventions in rural areas. Recent data from the US Department of Agriculture indicate that the highest food insecurity rates were in states with large rural populations, including Mississippi, New Mexico, Texas and South Carolina20,21. One study in a rural South Carolina county examined food-shopping options, finding a dearth of supermarkets and grocery stores. Almost 75% of the stores in the county that sold food were convenience stores, which stock fewer healthy food options than far-away grocery stores. Foods available at both supermarkets and convenience stores were more expensive at convenience stores and healthy versions of food were more expensive than the less healthy versions18. In a study of the food environment in rural Texas, researchers observed that fresh produce was not readily available in convenience or 'dollar' stores. Additionally, 70% of all food stores in the counties studied were convenience stores, with more dollar stores than grocery stores. Food selection and availability was considered more important than food choice, because rural consumers can only choose foods that are actually available to them22.
These rural studies indicate that access to healthy, affordable food in rural areas is not always available. More research is needed to measure and test how food environments vary by rural areas and how the availability and quality of food in these communities impact food choices.
Gaps exist in determining what food environment factors contribute to rural childhood obesity rates and what barriers rural residents face when trying to obtain food. To fill this gap, the present authors conducted a mixed-method study of the rural food environment in Maine. Results of the focus groups helped inform subsequent quantitative data collection, including determining where to target food audits in stores in each community and developing a series of survey questions about the home and community food environment to be included in Maine's annual telephone survey of SCHIP parents (K Fox, N Anderson, M L'Italien, A Yousefian, & D Hartley, unpubl. data, 2010). The present article summarizes the qualitative findings obtained during focus groups from the study.
The food environment (defined as food access, cost and quality for healthy foods such as fruits and vegetables, low-fat food items and whole grain products) was investigated in 6 rural low-income Maine communities with varying rates of obesity, to assess how food environments affect eating behaviors and obesity rates of rural children enrolled in MaineCare. A theoretical causal pathway was investigated from the community food environment to the home food environment (available healthy food and family behavior), to the child's food consumption, to the child's body mass index. For the focus groups, the parents of MaineCare children were asked about their food shopping habits, barriers faced when trying to obtain food, where they get most of their food, and what they perceive as healthy food.
Participants
In the spring of 2009, 6 focus groups were conducted (one in each study community). Participants were randomly selected from a list drawn from MaineCare eligibility data of parents who had one or more children enrolled in MaineCare. Participants were recruited via telephone and were informed of the purpose of the study, why they were selected to participate, and what they could expect during the focus group. They were also offered a US$60 gas card at the end of the focus group if they participated. Those agreeing to participate received 2 reminder phone calls prior to the focus group to increase their likelihood of attending.
Procedures
Focus groups were held at central, accessible locations within each study community. Before beginning each session participants were required to provide written informed consent, which included their agreement to have the session tape-recorded. Participants were made aware that they could choose not to answer any of the posed questions and were free to leave the group at anytime. Each focus group session lasted approximately 1 hour. At the end of each session, participants were given a US$60 gas card for their participation. Focus groups were led by a moderator who was accompanied by a note-taker/recorder, both of whom are authors of the study. All focus group procedures were approved by the University of Southern Maine's Institutional Review Board.
Instruments
Each focus group included 8 structured questions aimed at generating meaningful dialogue about food access (Table 1). These questions were developed and refined by a team of approximately eight researchers with expertise in nutrition, childhood obesity and public health.
Table 1: Focus group questions for rural healthy eating focus group
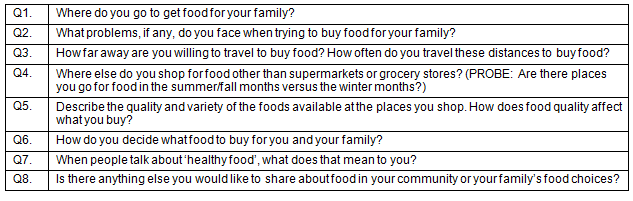
Focus group session recordings were transcribed by an independent consultant. Common themes were extracted by the authors and summarized based on the questions that were posed in the focus groups.
Results from the focus groups are presented in aggregate format to protect the confidentiality of participants and to summarize common themes and differences that emerged.
Participants
There were a total of 48 participants in the focus groups, ranging from 4 to 12 participants per group. Eighty percent of participants were female and 20% were male. Data were not collected about age or race/ethnicity; however, all participants were aged 18 years or older, and based on observation, nearly all were white/Caucasian.
Food sources
The majority of respondents in the 6 communities reported getting most of their food at large chain-supermarkets and box/super-stores (also known as super-centers or mega-stores - chain retail establishments that often include a grocery-section). Respondents indicated that they rarely do their food shopping in one place, but rather 'shop the sales and flyers', which requires visiting multiple stores to get the best prices and quality for their food. Many reported supplementing their bigger food shopping trips to large stores with visits to smaller, local food outlets that offer deals on specific items such as meats or dairy. There were only a handful of parents that reported doing 'one-stop-shopping' for all of their food, and most respondents are very well versed in which stores offer the best values for various items, which accept specific kinds of coupons, and what days the best quality items are available. Overall, respondents explained that in order to be able to afford the food they need for their families, much time and effort goes into looking through flyers for multiple stores, clipping coupons and pre-planning menus.
It is not like convenience all in one store - it is where the coupons are. We start at Shaw's...then we cross the road to Save-A-Lot and then we stop at Mountain's Market, because the milk and the sandwich meat are cheapest there.
Sales and coupons...you have to live on the coupons. My kids know Daddy will get them fruit - if it is on sale.
Problems and barriers: food costs and creative solutions
The most frequently reported barrier to obtaining food was cost. Participants reported having very tight budgets and explained the struggles they faced in order to get food on the table. Parents with many children and those with older children, such as teenagers who tend to eat more, seem to struggle the most to get their kids the food they need. Some parents reported forgoing paying utility bills in order to feed their children. Parents noted the recent rise in food costs and were frustrated that the cost of food had not gone down with gas prices, because this was largely the explanation for rising food costs.
It is not necessarily that I am buying quality, I am buying what fits in my budget and it is cheap and it is in my budget, because I have got to stretch what dollars I have got.
It is ridiculous. I thought groceries went up because of the gas prices and now the gas prices have come down by half and the groceries are still going up.
Because of high food costs, parents have come up with creative ways to make the food they buy last longer. Many rely heavily on their freezers to store the food they buy in bulk when it is on sale, with some participants having multiple large freezers in their homes. Freezers are also used for food obtained through hunting, fishing, picking wild berries and fiddleheads, and from what they and others grew in their gardens during the growing season.
If there is a sale I am grabbing it and I fill a freezer that way. That is the only way you can survive today. You can't do it any other way.
We hunt deer, we fish the lakes and the ponds and I mean anything that you can put in the freezer for winter. When things get bleak in the middle of January and February and you don't have two pennies to rub together, it is kind of nice to fall back on.
Other creative ways participants reported included supplementing what they buy with food obtained from local food banks, watering down milk and juice, mixing powdered milk with fresh milk, and mixing tofu into meat to 'bulk it up'.
Despite these efforts, many parents still reported difficulties in affording food, and those participants living in more remote rural areas appeared to be struggling more than those with closer access to urban areas. Generally all participants reported that affordability of food, especially high-quality, healthy food, is very difficult and something they worry about often.
Problems and barriers: travelling for food
Another reported barrier to obtaining food was related to travel distance and the cost of gas (petrol). While most participants reported owning or having access to a car, participants living in more remote settings cited transportation, travel time and gas money more often than those living closer to urban centers. Participants acknowledged that the high price of gasoline often negates the savings they receive from sales and the lower-priced stores to which they travel. Obstacles such as bad weather and unreliable transportation options complicate matters further.
Responses indicated that the distance parents will travel to buy food depends on how close their town is located to the major shopping venues, because this is where the best values are. In more remote locations, participants traveled more than 128.8 km (80 miles) round-trip to do their major grocery shopping. Those who lived in areas closer to urbanized areas reported only traveling 16-24 km (10-15 miles) each way to do their shopping. In efforts to save money on gas, those who reported traveling longer distances tended to consolidate their shopping trips with other tasks and errands. They also try to make the long trip to large box stores only once each month, and then buy the majority of their groceries at that time. Many parents keep coolers in their cars to transport perishables these far distances. Respondents reported supplementing these larger, monthly grocery trips with smaller trips to local stores for items that need to be replaced regularly, such as milk, eggs, and produce. The number of times that these trips were made varied from every few days to every 2 weeks.
I am only three and a half miles out, but a trip to town and then you run around and you go back - it is 15 miles minimum that I put on my car. If I do that every day it adds up...so I try to make my trips to town count... There is a purpose. There has got to be a reason to come to town.
Alternative food sources
Respondents in all study towns mentioned buying food at farmers' markets, including fresh fruits and vegetables, eggs, dairy and meats. They also reported that in the growing season there were plenty of roadside farm stands, and in some cases, farm-shares. One complaint about farm-shares was that there is a requirement to pay for the whole share initially, which is difficult, even though respondents were aware they would be saving money overall and getting fresh, local, quality foods. In some communities, participants mentioned bartering for fresh crops, eggs, dairy and meats from local farmers and/or family members or friends who grow or raise their own foods. Many respondents grow gardens, have chickens and in a couple of instances cattle. Some hunt and fish during the year and are able to freeze what they get.
I know that if my kids didn't pick their fruit when it is fruit season, I wouldn't be able to afford it now. They get out there and they pick their own strawberries, they pick their own blueberries.
The fact of the matter is you can't let your family starve...Every year I go out hunting and I go fishing during the summer. That is a way for me to bring it to the family without having to put that extra money out...I don't like killing, but it is a necessity in today's society - we don't have no choice.
It was the consensus that convenience stores and drug stores were only visited to buy food when absolutely necessary, given their very high prices and sometimes low-quality food. Participants from only one community discussed going to 'food pantries' (or 'food banks' - non-profit, charitable food distribution of mostly donated produce and products to those in need). It is unclear if participants from the other communities do not use food pantries, or if they were unwilling to admit to using them because of social stigma attached to their use.
Food quality and variety
Participants in each community were aware of which stores had the best quality and variety of foods, and which had the worst. Some even knew which days different stores received deliveries, and timed their shopping trips to have the best choice of fresher foods. Participants described the quality and variety of foods as being best at the chain grocery stores, although these stores tend to have expensive prices for produce, meats and diary. Participants did not seem impressed with the quality of produce at the bigger box stores. Those placing high importance on obtaining fresh fruits and vegetables reported traveling to specific stores for those items, even if they do the rest of their grocery shopping elsewhere.
We go down to Food City and we get all of our meats. We go to Save-a-Lot and get all of our vegetables and canned milks and stuff. Then we stop at the bread store and we load up there. Then we go to Hannaford or Walmart and get the rest that we need and then we are pretty much done.
Quality is a very hard qualifier in our household. I would love to feed my kids the best meat and best vegetables and the best fruits and everything; however, if I want to pay the light bill or if she needs new shoes for school, then this week it's potatoes because they're on sale. Next week we'll live on rice and chicken.
Deciding what food to buy
Affordability was the most commonly cited factor when participants reported how they decide what food to buy. Convenience and ease of preparation were also cited as important. Many parents wish to be able to offer their children healthier options but cannot afford healthy food all the time. However several parents reported making it a priority to feed their children fruit, vegetables, lean meats and whole grains and to stay away from processed, high fat or high-sodium foods. Some parents have children who are vegetarian or who prefer healthy snacks to junk food - they reported that feeding these children is difficult due to the additional cost, but that they do the best they can.
We would love to eat more fruits and vegetables and maybe even some of our kids want to go vegetarian. There is no way that we can afford that. When it is 50 cents for a box of macaroni cheese and it is four bucks for a head of lettuce, you know, there is an issue there.
The meaning of 'healthy food'
Participants were asked for their definition of 'healthy food' after all other questions were discussed, so as not to bias responses to healthy food only or make participants feel that they should be buying certain foods. Participants listed a number of qualities that make food 'healthy': low-sodium foods, whole grains, fruit and vegetables, lean meats and poultry, fish, low-fat dairy, organic, unprocessed, fresh and local foods. They suggested that fresh fruits and vegetables are the healthiest, frozen fruit and vegetables are the next healthiest, and canned produce is a last resort. They also explained that healthy food is generally more expensive and takes longer to prepare than unhealthy foods.
Some participants reported placing high importance on obtaining what they considered healthy food for their families, despite cost and other barriers. Others were more concerned with being able to put any food on the table, reporting that they tried to incorporate healthy options, but that simply affording food and feeding their children was a challenge. In general, participants appeared to have fairly accurate knowledge of which foods are healthy and which are not.
I don't understand ... I mean the junk food is cheaper and the healthy food is more expensive, you know? They are trying to get us to eat healthier, but they make the healthy food more expensive, so we can't afford it.
I can understand why a lot of people buy junk food, because junk food is cheaper than vegetables, but it is awfully expensive for vegetables today for kids.
Rural food deserts?
The term 'food deserts' refers to neighborhoods, particularly those in low-income areas, where residents do not live near supermarkets or other food retailers that carry affordable and healthy food. Residents of these neighborhoods, especially those who lack transportation rely more on smaller neighborhood stores that may not carry healthy foods or may offer them at higher prices16. Most studies of food deserts have focused on neighborhoods in urban settings. The notion of food deserts in rural areas may take on a different meaning. In the rural communities studied, where most families have access to cars and are used to driving long distances to reach services and employment, the term food desert may not apply. The parents spoken with recognized the inconvenience of driving 64.4 km (40 miles) each way to shop for food; however they explained that driving far distances is just a reality of rural life. Many commented that it would be easier and require less gas if there were bigger and cheaper stores nearby, but they were still able to get to larger stores, unlike the situation in urban food deserts where families may not have transportation to get to large grocery stores with healthier and more affordable options.
In urban areas, poverty is often concentrated in neighborhoods that are considered ghettos, which is also where food deserts are often situated. In rural areas, however, poverty tends to be more dispersed. Unlike in urban ghettos, respondents in the study communities reported access to cars with which they travel far distances to buy food. Because of these major differences, the concept of 'food desert' seems somewhat obscure.
The parents spoken with described a pattern of thoughtful food shopping. It is unclear whether low-income rural parents plan their food shopping more carefully than their urban counterparts as this study did not include an urban comparison. However, it may be that rural families have greater flexibility and opportunity to be more methodical in their food shopping since most have access to cars. This, in essence, creates a buffer or extension around these rural communities that might otherwise be considered food deserts. If rural residents are willing to travel 128.8 km (80 miles) round-trip to obtain food, then the boundaries for determining food deserts in rural areas should be calculated with this taken into consideration. In an urban setting, boundaries for food deserts may be more immediate than in rural areas. Physical distance is interpreted differently in rural and urban settings.
In addition to cars, rural residents reported using one amenity that most urban families cannot accommodate - large freezers. Nearly every participant in the focus groups mentioned utilizing freezers to store large quantities of food, especially bulk sale items and also foods they hunted, grew, bartered or collected themselves. Having the space to house a large freezer is a resource that is unique to families living in rural (and suburban) communities. It is unlikely that low-income urban families have the physical space to keep large freezers in their apartments. Having these options, in addition to having access to cars to travel longer distances to buy food, may contribute to making the notion of food deserts somewhat irrelevant in rural communities.
Although the meaning of food desert may be different in rural areas than in urban, it does not negate the fact that low-income rural families are struggling to provide food for their families. The participants seemed to have a firm knowledge about what constitutes healthy food. They also have developed creative skills for getting food. Despite having acquired these skills and knowledge, rural families are struggling. With these struggles in mind, policy-makers should consider the shopping patterns reported here when thinking about how to help rural residents better access affordable, healthy and quality foods. Customary approaches to remedying the problem of food deserts in urban areas, such as building more grocery stores, may not be necessary in rural areas. Additionally, focus group participants appeared to have a solid understanding of what constitutes 'healthy food', perhaps suggesting that there is less need for educational interventions about healthy food choices and more emphasis needed on other kinds of interventions targeting low-income rural families.
More creative approaches for food-access policy changes, subsidies and incentives are needed to match the complex and multi-faceted strategies that low-income residents utilize to feed their families. Possible options for supporting rural families in their struggles to obtain food include state supplements for gas for those on Medicaid or on food stamps. This could offset the high costs of driving to distant food outlets. Another way that gas costs could be supplemented is through incentive programs sponsored by grocery stores. These incentives offer credits toward gas costs when customers are regular shoppers at their stores. There are already some grocery stores in Maine partnering with gas stations to offer their customers discounts - although these offers are not specific to rural areas.
In addition to helping offset the costs of gasoline, policy-makers might consider subsidizing freezers for rural families. Storing bulk foods in freezers was expressed as a 'life-line' for rural families. While the initial cost of a large freezer may seem out of reach for a lower-income family, the savings on food costs over time were reported to be substantial. If rural families were offered assistance in purchasing freezers, it may help them to get and store the food they need. Further research is warranted to verify and quantify whether the use of freezers in rural communities is, in fact, a money-saving tool.
Other policy and programmatic approaches to remedying food access issues in rural communities could focus on mobilizing rural residents to start talking among themselves and with their local leaders about food access and quality. Focus group participants continued to speak to each other after the groups ended about how they obtain their food and 'stretch their dollars'. In one community, a group of mothers talked about farm-shares in the region. With this kind of information-sharing, community members can support each other and eventually create change. It might be helpful for rural families to have access to local support groups based on the issues of food and nutrition. Some residents felt strongly that their voices were not heard in their community. Helping organize residents and local leaders to talk about food and the health of their communities has the potential to mobilize rural residents in a way that allows them to be heard and to become their own advocates. Our informants expressed a need for such local leadership:
To have to ask for help is not because we are lazy, it is because we need assistance. It is not that we aren't willing to help ourselves, but we need some help. It would help if there was some guidance in this community.
Limitations
The use of qualitative data collection and a small sample size comes with limitations, including lack of generalizabiltiy and the possibility of bias in the sample of participants. Because there was little racial diversity among participants, findings may not be generalizable to all racial groups. Also, parents in the focus groups seemed to have a strong understanding of which foods are healthy. It is possible that those parents agreeing to participate in a focus group about food buying habits may place greater value on obtaining healthier foods than those who did not wish to participate. The $60 gas-card incentives were offered to mitigate this self-selection and attract a variety of parents into the focus groups, not just those placing a high value on healthy foods. These efforts, however, may not have been enough to avoid selection bias.
With focus groups, there is also the possibility of a group effect bias, where some participants may follow the lead of others, regardless of whether they agree. This may be the case in a small rural community especially, for participant anonymity is less likely. There were some instances where focus group members knew each other from the community, making it impossible to ensure confidentiality for participants. Focus group members were encouraged to not divulge any of the conversation outside the group.
Similarly, focus group members may have altered their answers to reflect more 'acceptable' responses regarding what and how they feed their children. Questions were purposefully asked about food in general, as opposed to 'healthy food' so not as to intimidate or influence focus group members' responses. The question about what 'healthy food' means was asked last in order to avoid bias in the answers to other questions about access, quality and barriers to getting food for their families. Despite these efforts, participants may have altered their responses.
Focus groups were conducted with low-income parents who had children enrolled in MaineCare in 6 rural Maine communities. Their responses depict the challenges that some rural Maine families face when trying to obtain food for their families. Cost, distance, and food quality were all factors that emerged as influential in rural low-income family's efforts to get adequate food. While some of these issues are not unique to rural families, the combination of challenges that rural low-income families face call for more rigorous study to identify promising interventions that will increase food access and quality in these communities.
Acknowledgements
The researchers would like to acknowledge the Robert Wood Johnson Foundation, Healthy Eating Research program (Building Evidence to Prevent Childhood Obesity grant #: 65051) and the Federal Office of Rural Health Policy for their support of this study.
References
1. Ogden CL, Carroll MD, Curtin LR, Lamb MM, Flegal KM. Prevalence of high Body Mass Index in US children and adolescents, 2007-2008. JAMA 2010; 303(3): 2009-2012.
2. Ogden CL, Carroll MD, Flegal KM. High Body Mass Index for Age Among US Children and Adolescents, 2003-2006. JAMA 2008; 299(20): 2401-2405.
3. Felton GM, Pate RR, Parsons MA, Ward DS, Saunders RP, Trost S et al. Health risk behaviors of rural sixth graders. Research in Nursing and Health 1998; 21(6): 475-485.
4. Liu J, Bennett KJ, Huran N, Zheng X, Probst JC, Pate RR. Overweight and physical inactivity among rural children aged 10-17: A national and state portrait. Columbia, SC: South Carolina Rural Health Research Center, 2007.
5. Lutfiyya MN, Lipsky MS, Wisdom-Behounek J, Inpanbutr-Martinkus M. Is rural residency a risk factor for overweight and obesity for U.S. children? Obesity (Silver Spring) 2007; 15(9): 2348-2356.
6. Anderson N, Thayer D. Children served by MaineCare, 2007: Survey findings. Portland, ME: University of Southern Maine, Muskie School of Public Service, 2008.
7. Healthy Eating research: building evidence to support childhood obesity. (Online) no date. Available: http://healthyeatingresearch.org/ (Accessed 28 July 2010).
8. Glanz K, Sallis JF, Saelens BE, Frank LD. Healthy nutrition environments: concepts and measures. American Journal of Health Promotion 2005; 19(5): 330-333, ii.
9. Cummins S, Macintyre S. Food environments and obesity - neighbourhood or nation? International Journal of Epidemiology 2006; 35(1): 100-104.
10. Morland K, Wing S, Diez Roux A, Poole C. Neighborhood characteristics associated with the location of food stores and food service places. American Journal of Preventive Medicine 2002; 22(1): 23-29.
11. Powell LM, Slater S, Mirtcheva D, Bao Y, Chaloupka FJ. Food store availability and neighborhood characteristics in the United States. Preventive Medicine 2007; 44(3): 189-195.
12. Rose D, Richards R. Food store access and household fruit and vegetable use among participants in the US Food Stamp Program. Public Health Nutrition 2004; 7(8): 1081-1088.
13. Wrigley N, Warm D, Margetts B. Deprivation, diet, and food-retail access: findings from the Leeds 'food deserts' study. Environment and Planning 2003; 35: 151-188.
14. California Center for Public Health Advocacy , PolicyLink, UCLA Center for Health Policy Research. Designed for disease: the link between local food environments and obesity and diabetes. Davis, CA: California Center for Public Health Advocacy, PolicyLink, UCLA Center for Health Policy Research, 2008.
15. Black JL, Macinko J. Neighborhoods and obesity. Nutrition Reviews 2008; 66(1): 2-20.
16. Holsten JE. Obesity and the community food environment: a systematic review. Public Health Nutrition 2009; 12(3): 397-405.
17. Whitacre PT, Tsai P, Mulligan J, National Research Council. The public health effects of food deserts: workshop summary. Washington, DC: National Academy Press, 2009.
18. Weinberg Z. No place to shop: food access lacking in the inner city. Race, Poverty, and the Environment 2000; 7(2): 22-24.
19. Liese AD, Weis KE, Pluto D, Smith E, Lawson A. Food store types, availability, and cost of foods in a rural environment. Journal of the American Dietetic Association 2007; 107(11): 1916-1923.
20. Nord M, Andrews M, Carlson S. Household food security in the United States, 2008. Economic Research report no. 83. Washington: USDA, Economic Research Service, 2009.
21. Springen K. Junk food county: Why many rural Americans can't get nutritious foods. The unhealthy truth about country living. Newsweek Web Exclusive 2007. (Online) 2007. Available: http://www.newsweek.com/2007/12/10/junk-food-county.html (Accessed 28 March 2011).
22. Bustillos B, Sharkey JR, Anding J, McIntosh A. Availability of more healthful food alternatives in traditional, convenience, and nontraditional types of food stores in two rural Texas counties. Journal of the American Dietetic Association 2009; 109(5): 883-889.



