Canada's First Nation populations appeared to have been severely impacted by the 2009 H1N1 influenza pandemic1,2. First Nation populations are predisposed to becoming ill from an infectious disease due to various reasons, including: living conditions, impoverished lifestyles, presence of co-morbidities, and (in some cases) being geographically remote2-5.
In 1876, the Indian Act entitled registered Indians on reserves to health care4. In Canada, the provision of health care (eg acute care, public health programs) to the general Canadian population is the responsibility of the provincial/territorial governments; however, registered Indians are entitled to additional non-insured health benefits (eg non-emergency medical transportation, prescription drugs, medical equipment, and dental care) provided by the federal government6. Therefore, First Nation communities are unique in that federal, provincial, and First Nation governments share responsibility for the delivery of healthcare services7. Historically, there has been a lack of coordination between the provincial and federal governments with regard to providing health care for Aboriginals4,6. During an influenza pandemic, the various involved government organizations have yet to clearly define roles and responsibilities and establish all necessary formal agreements7.
This study presents a retrospective insight into the barriers faced by three government sectors (ie federal, provincial, and First Nations) in three remote and isolated First Nation communities of northern Ontario, Canada, during the health sector response to the 2009 H1N1 influenza pandemic. In addition, participants identified culturally appropriate opportunities for improvement, which should be addressed in future pandemic plans.
Study community profiles
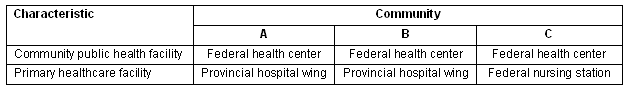
The three study communities (referred to as Community A, B, and C for anonymity) are located in northern Ontario, Canada. All three communities have similar living conditions and are considered geographically remote (the nearest service center with year-round road access is located >350 km away) and isolated (only accessible by planes year round)7. An elected Chief and Council (or Band Council) governs each First Nation community and are key decision-makers regarding the way a public health emergency is managed. Health Canada's First Nations and Inuit Health Branch (FNIHB) is responsible for the provision of primary health care (if provincial services are not available) and public health services in geographically remote and isolated First Nation communities5,7. For historical reasons and due to geographic location, all three study communities have a health center for community public health services and a primary healthcare facility for acute and/or chronic care6 (Table 1).
During an influenza pandemic, community public health personnel roles include immunizations, case and contact management, and education. Additionally, during an influenza pandemic, primary healthcare facility personnel are responsible for providing medical care and dispensing treatments. These primary healthcare facilities are covered by 24 hour nursing care with sporadic physician visits, and possess selected medical equipment; therefore, any patients requiring care beyond this must be transported to the nearest accommodating facility6.
Table 1: Characteristics of the study communities
Community-based participatory approach
The three communities were chosen for the following reasons: geo-spatial proximity to one another; community members expressed an interest in examining how effective their pandemic plan was in meeting the needs of the community; and the desire of the First Nations to actively participate in the planning process in preparation for the next public health emergency. The authors formed a partnership with the study communities and this research can be described as a community-based participatory approach8. All aspects of the study were developed and implemented in collaboration with a community-based advisory group formed of representatives from the communities' health centers and Band Councils9. For instance, the community-based advisory group played a collaborative role in designing the study, developing the interview questions, validating the study's results, and disseminating the findings10. This type of approach has been shown to be successful for research with Aboriginal communities because the research is conducted in a culturally appropriate manner and directly meets the needs of the communities8,9,11. Ethical clearance to conduct this research was granted by the Office of Research Ethics at the University of Waterloo.
Data collection and sources
Participants were purposively chosen from each study community as those who had the authority to represent and were particularly informative about their respective government body's involvement in the 2009 H1N1 pandemic response12. Specifically, the health director/supervisor, nurse-in-charge, and/or community health nurse at the health centers (or nursing station) were selected as the federal government representatives. The director of patient care and/or clinical coordinator at the hospital wings were the selected provincial representatives. Lastly, First Nations government representatives included the elected Chief and/or Deputy Chief of each community's Band Council.
Nine interviews were conducted with 13 adults during the period 9-23 February 2010 to gain a retrospective in-depth account of participants' experience during the 2009 H1N1 pandemic response12. As is culturally appropriate for the First Nation communities, verbal informed consent was obtained from participants10,13. Interviews were semi-directed to ensure consistent questions were asked based on academic literatures of healthcare service aspects of a pandemic response. This method also allowed for flexibility as participants were able to elaborate on what they felt was important14. Individual interviews were of 15 min to 1.5 hours in length and were conducted at a convenient place and time for the participant. All interviews were conducted in English; however, a Cree translator was available if the participants preferred that the interview was conducted in Cree13,15,16. With the participant's permission, interviews were audio-recorded, and detailed notes were taken.
Data management and analyses
Interviews were manually transcribed verbatim into electronic format. Collected data were organized according to 'theory-driven' and 'data-driven' codes using a combination of deductive and inductive thematic analysis17. Using a template organizing approach, the seven broad codes of the regional FNIHB pandemic influenza plan were used to provide a flexible guide to deductively code relevant data17-19. Via inductive coding, segments of data pertaining to supplies and equipment were coded as a newly emerged code20. For subsequent analysis and interpretation, the data were further categorized according to main interview trigger questions (ie positive aspects, barriers faced, and suggested improvements), always noting which community and government body the commenting participant represented17. This approach was chosen to allow for comparisons regarding the similarities and differences experienced during the pandemic response within and between each government body of the three study communities. The aforementioned data analysis was an iterative process completed by the author (NAC) and confirmed by the co-author (LJST) to ensure accuracy.
Members of each study community's pandemic committee validated the resulting eight codes. Attending members included representatives from various sectors involved in the community's pandemic response: Band Council, health center, hospital wing, nursing clinic, education, clergy, Northern store, water treatment plant, and emergency medical services. Eight to 10 people attended each community meeting and no changes were proposed. This validation method was chosen because the resulting codes would create the framework for each community's modified community-level pandemic plan; thus, directly applying the study's findings21.
Data analyses revealed eight codes; however, details of five codes (eg surveillance, antiviral medications, health services, emergency response, and communications) are presented in the present article. The remaining three codes (eg vaccine, supplies, and public health measures) were selectively omitted to present the most relevant results pertaining to how multiple government bodies influenced the pandemic response in the study communities. Representative quotes were used to highlight key findings; however, for the purpose of anonymity, information about the commenting participant is not disclosed22,23.
Surveillance
Influenza surveillance involves the collection of information about influenza-related cases in order to determine the severity and potential impact of influenza activity7. In general, participants representing the provincially run hospital wing believed that the surveillance system employed during the pandemic response worked well, despite being complicated initially. One participant mentioned that feedback from surveillance reports would be appreciated to ensure proper actions were being executed.
In Community A and B, some issues arose with regard to when specimens from patients should be taken for laboratory testing, because some federal representatives disagreed with their provincial counterpart's instructions. This led to pressure not to follow their respective organization's guidelines; for instance, a provincial representative mentioned:
... it was people wanting to put pressure on us, but we're walking a fine line because we had to follow the guidelines set down by the medical officer of health [provincial jurisdiction], but at the same time, try to relieve the pressure from public health [federal government personnel]... (Participant #2)
Some federal representatives noted that there was a lack of health information sharing with the provincial agency with regard to which patients were being tested in order to promptly and properly conduct case and contact management. These representatives noted that they only received a report if a positive case had been confirmed. In addition, federal representatives believed that the provincial hospital wing did not promptly set up a designated assessment area for patients with influenza-like illness (ILI) symptoms and suggested that improving influenza assessments should be a priority for the next time.
Antiviral medications
In two communities, participants agreed that the antivirals were efficiently distributed, in that patients who met the guidelines received the needed treatment. In contrast, federal and provincial participants from one community were in disagreement. Although the provincial representative stated that they followed the provided guidelines, federal participants believed that the antivirals were not efficiently distributed. It was reported that only 22 doses were distributed out of the 424 received doses even though many community members were displaying ILI symptoms. The federal representatives indicated that they would like antivirals to be better distributed, including for prophylactic purposes.
Health services
Representatives from each government body agreed that there was a lack of human resources, especially nurses, during the pandemic response in each study community. As one participant stated:
... they [nurses] were expected [to do] too much and they didn't have enough additional staff to do it. Cause [sic] the hospital room was really packed in the evenings, and they didn't have enough nurses to work with the people. And they did their best, and I think we, they were overtired, overburdened... (Participant #7)
Moreover, a participant remarked that due to the shortage of human resources, they were unable to follow up with ill families to provide necessary support and believed this should be improved. The participant remarked:
Even if there was a house... affected with H1N1, if a family were affected, we didn't even touch base on how we know what they're short on and stuff like that, what they need. (Participant #9)
Many participants mentioned that they want more human resources available for future pandemics, especially nurses and trained personnel with the expertise to deal with a public health emergency.
Emergency response
In one community, the federal representatives felt that certain aspects of the emergency response section of the pandemic plan were not adequately addressed in a timely manner. The federal representatives reported that isolation and quarantine issues were not specified and implemented. In addition, the federal representatives stated that details regarding a morgue were not adequately addressed and that there was no appropriate site in the community, especially if a public health emergency occurred in the spring. A federal representative questioned:
... we didn't go into it that if there were more deaths in the community, where would the bodies be stored? You know so, who would be handling the bodies? (Participant #10)
However, the provincial participant stated that the provincial organization had a morgue plan in place and had identified a potential site. Therefore, the federal participants believed that specific information regarding morgue, isolation, and quarantine issues should be properly outlined in the community-level pandemic plans after in-depth discussions with the community pandemic committee.
Communications
All provincial representatives stated that they were prepared for the outbreak, although it took a few days to implement aspects of the response and improvements could be made to increase efficiency. In contrast, some federal and Band representatives from each study community believed that their respective community was not prepared for the pandemic for various reasons, such as lack of resources and cooperation from key players of the community pandemic committee. A participant mentioned:
Yeah, so we weren't really ready for this pandemic situation. So, it's like that in a remote area, we're the last one to get the resources and it's very unfortunate... (Participant 7)
Some provincial representatives reported that they received contradicting guidelines from many sources and were initially extracting the best information from each source. Because this was confusing, they eventually decided to only follow their respective organization's direction, although these directions were sometimes ambiguous and changed frequently. Federal representatives also noted that they received different information than the provincial body at different times. The discrepancy between provincial and federal instructions led to multiple disagreements and confusion amongst the federal and provincial representatives from both Community A and B. As one participant mentioned:
As you can understand, we're provincial, the other side over there, is federal, so they were having their guidelines, and we were having our guidelines, and their guidelines sometimes were different than our guidelines, and we found that very confusing. (Participant #2)
Another participant noted:
... it was like a lot of different information coming in, it would have been nice just to see one, one person reporting and that would have been either the province or feds [sic], didn't matter what which one. It would have been nice to have one just at a region, you know, just had a regional one... (Participant #1)
One participant also noted that each agency had its own respective pandemic plan in addition to the community-level pandemic plan. With multiple pandemic plans in place, the participant stated that there was confusion with regard to each agency's roles and responsibilities during a pandemic.
Discussion
In general, participants reported many issues which may be attributable to the dichotomy (or trichotomy) of government bodies responsible for healthcare delivery during an influenza pandemic. Interestingly, participants from Community C did not report some of these issues, possibly due to the fact that both the health center and nursing station are federally funded. The Canadian Pandemic Influenza Plan for the Health Sector (CPIPHS)7 states that the involved government bodies have very few formal arrangements in place and gaps remain with regard to managing a pandemic influenza outbreak in First Nation communities; thus, the present study's results have informed the following recommendations which can be achieved by increasing formal communication and collaboration among the involved government bodies.
Improve communication plans
The Bellagio Group stresses the importance of equitable access to accurate and easily understood information during an influenza pandemic24. The CPIPHS7 states that it is the responsibility of all levels of the government (ie local, regional, provincial, and federal) to provide on-reserve First Nation communities with accurate, timely and consistent information during an influenza pandemic. However, participants reported that these multiple sources of information were sometimes inconsistent, misleading, and contradictory; therefore, participants suggested that one reliable source should provide the necessary information. It is recommended that all levels of government collaborate to create a consistent and complementary communication effort, especially when providing guidelines. Additionally, based on the literature, the authors recommend that the regional FNIHB be the source to provide the necessary information to First Nation communities.
Update community-level pandemic plans
Adequate preparedness plans should be developed and in place to mitigate the impact of an influenza pandemic25,26. The World Health Organization (WHO) has developed various tools to help countries with their preparation for an influenza pandemic, including a preparedness planning checklist25,27. While national planning is imperative to make recommendations and set standards, planning at the community level is also vital to warrant that these measures can be effectively implemented28. The WHO tools, along with the current national and provincial pandemic plans, offer universal methods which may not be feasible in remote and isolated First Nation communities due to their unique challenges (ie living conditions, lack of access to resources and health care etc.)2-5,7,25,27,29. The FNIHB regions have developed regional pandemic influenza plans and should continue to assist First Nation communities to develop community-level pandemic plans which are appropriately modified to specifically meet their requirements7.
For instance, the use of non-pharmaceutical interventions, such as isolation and quarantine, may be useful in mitigating the effects of a pandemic, especially due to the limitations of availability and effectiveness of pharmaceutical interventions like vaccines and antivirals5,30-35. Thus, it is important that community-level pandemic plans contain specific information about various non-pharmaceutical interventions that can be implemented. Also, in First Nation communities, it is important that pandemic plans respect their holistic approach to health and the use of traditional medicine practices36.
In addition, historic data has shown that over 70% of a population may become infected by a novel virus during a pandemic; therefore, plans to manage mass fatalities should be addressed in community-level pandemic plans7. These plans should be based on local needs and availability of resources, in addition to local limitations and cultural considerations7. For instance, northern remote and isolated communities may face difficulties transporting bodies to the place of burial and lack of funeral service personnel and resources7. Therefore, as suggested by participants, the aforementioned issues should be specifically addressed in community-level pandemic plans.
Furthermore, the CPIPHS7 provides a well-intentioned table outlining the roles and responsibilities of the partners involved in the management of a pandemic influenza in on-reserve First Nation communities. However, participants mentioned that roles and responsibilities were not clearly defined and executed at the local level. It is recommended that these communities, with the help of the government, outline the roles and responsibilities of each agency and include the details in the community-level pandemic plan, which will hopefully lay the foundation for a cohesive and effective pandemic response.
Increase human resources
In these northern remote and isolated communities, nurses work in an expanded role as they are the main providers of healthcare services6. Literature has shown that geographically isolated First Nation communities under normal circumstances suffer from shortages of trained healthcare professionals, particularly nurses, and are typically forced to rely on relief staff which can have negative effects on healthcare services4,22,37. During a public health emergency, such as an influenza pandemic, human resources will play a central role in the response and will be required to implement various pharmaceutical interventions and provide medical care for patients25,38. However, in an influenza pandemic, staff shortages may be exacerbated by various reasons, such as staff themselves becoming ill, transportation challenges, childcare/family obligations, and fear of exposure to the virus, to name a few28,38,39.
Health Canada's FNIHB is responsible for providing healthcare services to on-reserve First Nation communities and should continue to prioritize recruiting a full-time, permanent complement of nurses7. To aid in retaining nursing staff, recruited nurses should be provided with a proper orientation to prepare them for the demanding nature of the job and to learn about the importance of respecting First Nations' traditional values22,36. During an influenza pandemic, some broad strategies can be implemented to mitigate the effects on healthcare personnel, such as establishing designated clinics for patients with ILI symptoms and improving the surge capacity of the health sector39. A participant also suggested that during a public health emergency pre-approved vacation time should be postponed or cancelled to optimize the number of healthcare personnel. Furthermore, as suggested by participants, plans should be developed to deploy an interdisciplinary team of healthcare professionals with the expertise to deal with a public health emergency, such as communicable disease nurses and psychological support.
The presented research has various strengths in that it was a retrospective study that identifies the barriers and suggested improvements by participants who have a wealth of experience regarding their respective community's pandemic response. However, a limitation of the study is the inability to generalize some findings to the boarder population due to the non-random sample of participants and the unique characteristics of the study communities.
Remote and isolated First Nation communities are unique in that multiple government bodies share responsibility for the health of their community members during a public health emergency. This qualitative study presents a retrospective insight into the barriers that arose during the pandemic response of three communities possibly due to the dichotomy (or trichotomy) of government bodies responsible for the delivery of healthcare services and suggests recommendations which can be incorporated into future pandemic plans. Receiving contradicting guidelines and direction from multiple government sources is recommended to be addressed by developing a complementary communication plan. Also, government officials should continue to focus efforts to increase the availability of human resources and update community-level pandemic plans by adding community-specific detail.
While progress has been made, it is hoped that via formal communication and collaboration between the involved government bodies, the aforementioned issues will be addressed and will lead to an improved delivery of healthcare services in remote and isolated First Nation communities during a public health emergency.
Acknowledgements
The authors thank the First Nation communities that participated in the study for their invaluable contributions. This study was funded by the Canadian Institutes of Health Research (Institute of Aboriginal Peoples' Health), Indian and Northern Affairs Canada, and the Government of Ontario.
References
1. Kumar A, Zarychanski R, Pinto R, Cook DJ, Marshall J, Lacroix J et al. Critically ill patients with 2009 influenza A(H1N1) infection in Canada. JAMA 2009; 302(17): 1872-1879.
2. Kermode-Scott B. Canada has world's highest rate of confirmed cases of A/H1N1, with Aboriginal people hardest hit. BMJ 339: b2746. (Online) 2009. Available: http://www.bmj.com/content/339/bmj.b2746 (Accessed 10 November 2009).
3. Barker K. Canadian First Nations experience with H1N1: new lessons or perennial issues? International Journal of Tuberculosis and Lung Disease 2010; 14(2): 130.
4. MacMillan HL, MacMillan AB, Offord DR, Dingle JL. Aboriginal health. Canadian Medical Association Journal 1996; 155(11): 1569-1578.
5. Ministry of Health and Long-Term Care. Ontario health plan for an influenza pandemic 2008. (Online) 2003. Available: http://www.health.gov.on.ca/english/providers/program/emu/pan_flu/pan_flu_plan.html (Accessed 17 December 2009).
6. Tsuji LJS. A decade of change in the Mushkegowuk Territory (1987-1997): moving towards a self-governing health-care system. Canadian Journal of Native Studies 1998; 18(2): 233-254.
7. Public Health Agency of Canada. The Canadian pandemic influenza plan for the health sector 2006. (Online) 2006. Available: http://www.phac-aspc.gc.ca/cpip-pclcpi/ (Accessed 17 December 2009).
8. St Denis V. Community-based participatory research: aspects of the concept relevant for practice. In: WK Carroll (Ed). Critical strategies for social research. Toronto, ON: Canadian Scholars' Press, 2004; 292-302.
9. Macaulay AC, Delormier T, McComber AM, Cross EJ, Potvin LP, Paradis G et al. Participatory research with native community of Kahnawake creates innovative code of research ethics. Canadian Journal of Public Health 1998; 89(2): 105-108.
10. Kirby AM, Lévesque L, Wabano V, Robertson-Wilson J. Perceived community environment and physical activity involvement in a northern-rural Aboriginal community. International Journal of Behavioral Nutrition and Physical Activity 4: 63. (Online) 2007. Available: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2217526/pdf/1479-5868-4-63.pdf (Accessed 10 December 2009).
11. Davis SM, Reid R. Practicing participatory research in American Indian communities. American Journal of Clinical Nutrition 1999; 69(Suppl): 755S-759S.
12. Neuman WL, Robson K. Basics of social research: qualitative and quantitative approaches, Canadian edn. Toronto, ON: Pearson Canada, 2009.
13. Skinner K, Hanning RM, Tsuji LJS. Barriers and supports for healthy eating and physical activity for First Nation youths in northern Canada. International Journal of Circumpolar Health 2006; 65(2): 148-161.
14. Daly KJ. Qualitative methods for family studies and human development. Thousand Oaks, CA: Sage, 2007.
15. Tsuji LJS, Manson H, Vanspronsen EP, Wainman BC, Shecapio-Blacksmith J, Rabbitskin T. Identifying potential receptors and routes of containment exposure in the traditional territory of the Ouje-Bougoumou Cree: land use and a geographical information system. Environmental Monitoring and Assessment 2007; 127: 293-306.
16. Gates A, Hanning RM, Gates M, Isogai AD, Metatawabin J, Tsuji LJS. A school nutrition program improves vegetable and fruit knowledge, preferences, and exposure in First Nation youth. The Open Nutrition Journal 2011; 5: 22-27.
17. Fereday J, Muir-Cochrane E. Demonstrating rigor using thematic analysis: a hybrid approach of inductive and deductive coding and theme development. International Journal of Qualitative Methods 5(1). (Online) 2006. Available: http://www.ualberta.ca/~iiqm/backissues/5_1/pdf/fereday.pdf (Accessed 23 December 2010).
18. Crabtree BF, Miller WL. Using codes and code manuals: a template organizing style of interpretation. In: BF Crabtree, WL Miller (Eds). Doing qualitative research, 2nd edn. Newbury Park, CA: Sage, 1999; 163-177.
19. First Nations and Inuit Health Ontario Region. Pandemic Influenza Plan. (Online) 2009. Available: http://www.mnaamodzawin.com/H1N1Facts/FNIH%20Pandemic%20Influenza%20Plan%20October%2029%202009.pdf (Accessed 5 January 2010).
20. Boyatzis RE. Transforming qualitative information: thematic analysis and code development. Thousand Oaks, CA: Sage, 1998.
21. Sandelowski M. "To be of use": enhancing the utility of qualitative research. Nursing Outlook 1997; 45(3): 125-132.
22. Minore B, Boone M, Katt M, Kinch P, Birch S, Mushquash C. The effects of nursing turnover on continuity of care in isolated First Nation communities. Canadian Journal of Nursing Research 2005; 37(1): 86-100.
23. Knafl KA, Howard MJ. Interpreting and reporting qualitative research. Research in Nursing and Health 1984; 7: 17-24.
24. Johns Hopkins Berman Institute of Bioethics. Bellagio statement of principles. (Online) 2006. Available: http://www.bioethicsinstitute.org/web/page/906/sectionid/377/pagelevel/4/interior.asp (Accessed 17 December 2010).
25. Oshitani H, Kamigaki T, Suzuki A. Major issues and challenges of influenza pandemic preparedness in developing countries. Emerging Infectious Diseases 2008; 14(6): 875-880.
26. World Health Organization. Pandemic influenza preparedness and response: WHO guidance document, April 2009. (Online) 2009. Available: http://www.who.int/csr/disease/influenza/pipguidance2009/en/index.html (Accessed 23 December 2010).
27. World Health Organization. WHO checklist for influenza pandemic preparedness planning. (Online) 2005. Available: http://whqlibdoc.who.int/hq/2005/WHO_CDS_CSR_GIP_2005.4.pdf (Accessed 23 December 2010).
28. Hampton T. Pandemic flu planning fall short: many vulnerabilities in health care system. JAMA 2007; 297(11): 1177-1178.
29. Groom AV, Jim C, LaRoque M, Mason C, McLaughlin J, Neel L et al. Pandemic influenza preparedness and vulnerable populations in tribal communities. American Journal of Public Health 2009; 99(S2): S271-S277.
30. Aledort JE, Lurie N, Wasserman J, Bozzette SA. Non-pharmaceutical public health interventions for pandemic influenza: an evaluation of the evidence base. BioMed Central Public Health 7: 208. (Online) 2007. Available: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2040158/pdf/1471-2458-7-208.pdf (Accessed 10 June 2010).
31. Sullivan SJ, Jacobson RM, Dowdle WR, Poland GA. 2009 H1N1 influenza. Mayo Clinic Proceedings 2010; 85(1): 64-76.
32. Fedson DS. Pandemic influenza and the global vaccine supply. Clinical Infectious Diseases 2003; 36: 1552-1561.
33. Leung GM, Nicoll A. Reflections on pandemic (H1N1) 2009 and the international response. PLoS Medicine 7(10): e1000346. (Online) 2010. Available: http://www.plosmedicine.org/article/info%3Adoi%2F10.1371%2Fjournal.pmed.1000346 (Accessed 12 January 2011).
34. Oshitani H. Potential benefits and limitations of various strategies to mitigate the impact of an influenza pandemic. Journal of Infection and Chemotherapy 2006; 12: 167-171.
35. Low DE. Pandemic planning: non-pharmaceutical interventions. Respirology 2008; 13(Suppl1): S44-S48.
36. Assembly of First Nations. A First Nations wholistic approach to pandemic planning: a lesson for emergency planning. (Online) 2007. Available: http://www.afn.ca/cmslib/general/pan-planning20078310219.pdf (Accessed 20 November 2010).
37. Minore B, Boone M, Hill ME. Finding temporary relief: strategy for nursing recruitment in northern Aboriginal communities. Canadian Journal of Nursing Research 2004; 36(2): 148-163.
38. Ives J, Greenfield S, Parry JM, Draper H, Gratus C, Petts JI et al. Healthcare workers' attitudes to working during pandemic influenza: a qualitative study. BioMed Central Public Health 9: 56. (Online) 2009. Available: http://www.biomedcentral.com/content/pdf/1471-2458-9-56.pdf (Accessed 10 November 2010).
39. Wilson N, Baker M, Crampton P, Mansoor O. The potential impact of the next influenza pandemic on a national primary care medical workforce. Human Resources for Health 3: 7. (Online) 2005. Available: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1215505/pdf/1478-4491-3-7.pdf (Accessed 12 February 2011).
