In Canada, medical schools have increased general enrolment to address physician shortages and have encouraged students from rural communities to pursue medical careers in an effort to address physician shortages, particularly in rural areas. In addition, medical schools have opened in smaller and more rural communities with the intention of training local students who will stay and practice in these areas. These approaches to addressing physician shortages depend on the ability to recruit and retain program graduates.
A number of studies suggest that younger, more recently graduated physicians have different career expectations and practice patterns from their older counterparts1-4. A review of the literature found that while a large number of studies have examined physicians' location choices, these studies largely focus on rural physicians. The authors were unable to find studies that examined generational differences in the reasons related to work location choice.
Using the framework developed by Barer et al5, factors were examined that influenced differing generations of physicians to choose where they worked. The framework suggests that 6 groups of factors underlie practice location decisions: personal background, professional education, professional practice, personal/family, community, and economic factors. Personal background includes sex, rural background, age etc. Most studies that have examined the relationship between personal background and work location have focused on the relationship between rural practice and rural upbringing and have reported that, in general, physicians who came from a rural community were more likely than their urban counterparts to practice in rural communities5-14.
Professional education factors relate to the physician's training. Previous studies have examined the relationship between work location and medical school, exposure to rural medicine, post-graduate training site and speciality. For example, studies have reported substantial variation among medical schools in the proportion of graduates who practice in rural communities8,13,15 and province where they received their medical training16,17.
Personal/family and professional practice factors are among the most important in physicians' work location decisions. Personal/family factors include proximity to family and friends, spouse's preferences, suitability of professional/social peer group, educational, and extra-curricular opportunities for children. Professional practice factors describe the characteristics of the practice. The opportunity to establish and own a group practice and acquire diverse medical experience, reasonable on-call schedules, an available locum program, and access to specialists and referral networks have been cited as key elements in recruiting and retaining rural physicians5,8,10,13,14,18-23.
Frequently studied community factors include climate, recreational and cultural opportunities, and socio-economic status of the community. However, community factors have rarely been suggested as the most influential in physicians' work location choices.
Economic factors include gross income opportunities, practice costs, financial incentives, and employment opportunities for the spouse. Although economic incentives such as location bonuses, educational support, locum relief, and moving and housing allowances have some influence in recruitment14,18,19,21,24, financial considerations appear to have limited impact on the retention of rural physicians5,21,22,25-29.
Using qualitative interviews, the factors that influenced physicians of differing generations to choose a work location were explored. This study examined physicians trained at universities in Saskatchewan (SK), and Newfoundland and Labrador (NL), two Canadian provinces with long-standing physician shortages. Both provinces have relatively small populations (approximately 1 million and 500 000, respectively) spread over large geographical areas (651 900 and 405 720 km2, respectively). Approximately 40% of the populations in both provinces live in rural communities (population <10 000). The tertiary care centres are in Saskatoon (population 233 923) and Regina (population 194 971) in SK, and in St John's (population 181 113) in NL30. Regional hospitals in smaller urban centres (population <100 000). Each province has a single medical school. The small size and large rural component compound the challenges of physician recruitment and retention in these provinces. By understanding the factors that influence new generations of physicians, the aim was to inform recruitment strategies and, ultimately, improve physician retention, particularly among the younger generation of physicians. The focus was on recruitment to the provinces as a whole, since the largest communities in the provinces are small compared with most urban communities.
Qualitative interviews were conducted with different generations of physicians who completed undergraduate medical training at either Memorial University of Newfoundland (MUN) or University of Saskatchewan (USK). Generations were defined on the basis of year of graduation. Early-career physicians graduated between 1995 and 1999, mid-career physicians between 1985 and 1989, late-career physicians between 1975 and 1979, and end-career physicians between 1965 and 1969. Because MUN's first medical class graduated in 1973, end-career physicians were interviewed only from USK.
Using SPSS software (www.spss.com), the names of physicians were randomly drawn to recruit them to the study from databases of graduates used in previous studies16,31. The databases included the names and work locations of graduates.
Random drawing of names from the list of graduates from each medical school and each generation continued until three to five physicians who worked either in the home province or outside the home province were interviewed from each university in each generation. Recruitment was guided by saturation (ie when no new themes emerged from the data) as well as representation from strata (school/generation/location) of the recruitment framework.
To be included in the study, physicians had to be living in Canada or the USA (to limit long-distance costs), licensed to practice, and recently working in a clinical capacity (ie not exclusively administrative, teaching or research, or retired for more than 3 years). Physicians who were sponsored by foreign governments to study medicine at either university were excluded. The time period physicians served in the military was excluded from the analyses due to limited ability to choose their practice location.
Semi-structured interviews were conducted with consenting physicians between July 2007 and December 2008. Interviews took place in-person or by telephone and lasted between 10 and 45 min. Physicians were asked questions about the number and nature of work location changes over the course of their career, and the factors related to their decision to choose each location. Probes were based on the framework developed by Barer et al5. For each work location, the authors distinguished between locations in post-graduate residency training and once the physician had completed training. All but two interviews were audio-recorded and transcribed verbatim. A research assistant took notes to capture the conversation in those interviews.
Using a thematic analysis approach, a coding template was developed that built on the framework developed by Barer et al5.. The coding of an initial set of 6 interviews (3 from each province) were compared to ensure consistency of coding and to revise the coding template where necessary. Transcripts were then coded using NVivo software (www.qsrinternational.com), which is designed to assist in the organization and management of qualitative data. Although the focus was on generational differences, similarities and differences between universities, sexes and specialties (family physicians/GPs vs specialists) were also examined.
This study was approved by the ethics committees at MUN and USK. Data which could identify individual physicians have been edited in the quotations.
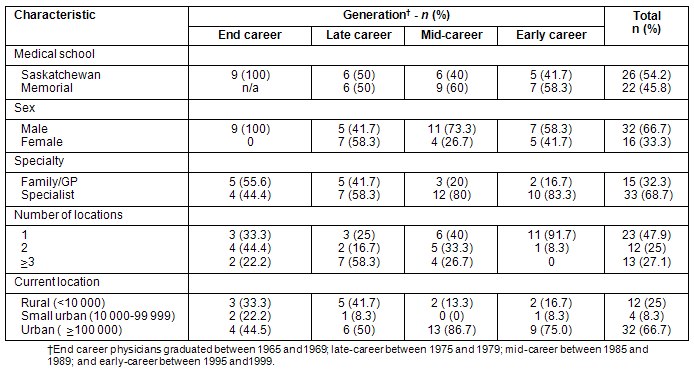
Interviews were conducted with 48 physicians whose characteristics are presented (Table 1). All but personal background factors were cited as influencing work location choices.
Table 1: Characteristics of study participants by generation
Personal/family factors
The desire to be near family and friends was cited as the primary consideration when choosing a work location, regardless of generation, sex, specialty type or school of graduation. For example, a participant said:
Well, it's where I grew up, my husband and I got married and we wanted to be closer to family while we were having kids, so that was the main reason.
For early-career physicians, a satisfying work-life balance was an important consideration. For many, the work-life balance was an attractive quality for returning to smaller provinces such as SK or NL, as described by the following quotation from a female specialist:
I knew that I would still be able to practice in an academic centre in St John's [capital city of NL] so I'd have the best of both worlds basically that an academic center would in Montreal or Toronto. However I would also be able to have a nice lifestyle. In bigger centers such as Montreal or Toronto, there's the high pressure for research and huge patient volumes and that sort of thing and so, I think you are sort of driven by your job. You don't have a lot of lifestyle.
Many older generation physicians commented on the emphasis that the younger generation placed on lifestyle:
You see, baby boomers and the people older than the baby boomers, they had a work ethic that said, 'If I'm going to be a doctor, and something has to get done, I will put that work ahead of any other plans I have'. I think they call the younger generation the millenniums. They will never put work ahead of their plans...
Unlike early-career physicians, older generation physicians cited a sense of adventure or wanting to see other parts of the country and world when choosing where to work: 'I decided to go do my internship in Toronto, in order to see something different. You know, go to the big city'. Another older generation physician noted that there were limited opportunities to travel prior to completing her undergraduate education:
Well, I think, when I graduated university I hadn't really traveled anywhere, and I always wanted to travel so for me, regardless of what I graduated in, I think I probably would have gone off to travel and work, at the same time.
Professional education factors
Residency training site was an important influence on physicians work location choices. As many physicians noted, completing residency training increased their familiarity with community and colleagues:
First of all, I did my [specialist] residencies in Toronto. So I knew the place and they knew me.
I did my residency here, and a job became available, and I was already established there, had a house, friends, those kinds of things.
Echoing USK physicians, a MUN-trained physician suggested that choosing to train outside SK or NL can limit future opportunities to return to the province:
Other places seem to like the residents to go away and get some training and then come back to work. Whereas Newfoundland in [specialty] tends to hire its own residents and really I was given kind of the impression that once you left, your foot was no longer in the door.
Professional practice factors
For many physicians, the ability to use their skills and knowledge fully was an important consideration in choosing a work location. Although the idea of having a full scope of practice was important, specialists and family practitioners differed in the criteria that allowed them a full scope of practice regardless of generation, sex, or university. For family physicians, wanting a full scope of practice was cited in reference to their decision to practice in a rural setting: 'I guess I wanted to go to a rural community ... I just thought it would be interesting as a family physician in terms of using all the skills that I had been trained to do...'. For highly specialized and academic physicians, their choice of work location was limited to teaching hospitals in large centres. These specialists noted that the patient population had to be large enough to support their clinical and research activities: 'So, if you got a patient population base of, what is it for St John's? Maybe 200 000. That's just too small to be highly, highly, highly specialized'.
Economic factors
For some physicians, remuneration was very influential in their work location decision, as is illustrated by the following quotation by a USK graduate who opted to work in Alberta because of higher incomes relative to other provinces:
Physician: Economics is an important factor, the pay, fee schedule was higher in Alberta... and taxes are less here.
Interviewer: Ok, so did that influence your decision to go to Calgary too?
Physician: To stay here? Yeah it did.
However, many physicians who chose to remain in SK or NL cited the lower cost of living in these provinces:
There would always be financial considerations but lots of places that you end up getting paid more, the cost of living or housing or etc is more. So, it doesn't necessarily work out any better.
Other physicians suggested that remuneration had limited influence in their decision, for example:
You're not going to keep me here by giving me money. You're going to keep me here by providing me with an opportunity that satisfies me personally.
Among end- and late-career physicians, male physicians rarely, if ever, made reference to their wives' employment opportunities when deciding where to work. References to the spouse were almost exclusively related to being near her family: 'My wife's family comes from Winnipeg, so it was a reason to be around'. An older generation female physician was more likely to refer to employment opportunities for her husband, regardless of his profession: 'My husband had a job he wanted to do in Winnipeg'. For younger generation physicians, however, employment opportunities for the spouse were important considerations in choosing a work location, regardless of sex. For example, one mid-career male physician noted on his decision to move to Calgary: 'First is, it's where my wife's career was'. Moreover, many younger generation physicians were married to other physicians and ensuring that both spouses were able to practice was important in choosing a work location:
And for both of us, we are fairly sub-specialized, so there wouldn't be too many places across Canada at that particular moment where we could have accepted a job.
Community factors
Community factors were cited by few participants. Proximity to an international airport was important to physicians who like to travel while proximity to mountains, bodies of water and hiking trails were cited by physicians who enjoyed outdoor recreational activities:
I like that it's a large city. I like to have a lot of outdoor activity opportunities, it's close to the mountains, an international airport so you can get away and travel easy as well.
Older generation physicians cited medical need in the community as an important influence on their work location decisions, particularly in reference to work in rural, remote or otherwise challenging locations, as described by an end-career physician:
Interviewer: What influenced you to choose [remote, Northern town] as a place to work?
Physician: Well, they needed doctors. It was a challenge.
'Recruitment' was an additional factor identified that did not fit with any of the existing categories of the Barer et al framework5. Recruitment refers to the efforts to seek out and attract physicians. Recruitment efforts were cited as another influential reason for choosing a work location, particularly for specialists who were completing residency training in other parts of the country or abroad. One MUN graduate said that a job offer from NL was instrumental in his decision to return to the province: '...if a job offer had not come unsolicited I can't really say if I would have worked strongly to come back to NL'. Recruitment efforts should take timing and the quality of the interaction into consideration. Recruiting during residency was particularly important: 'Partly the recruitment, that they had contacted me during my residency and expressed interest in having me practice there...' For both USK and MUN graduates, half-hearted recruitment efforts discouraged physicians from returning to SK or NL. For example, one USK graduate described his experience when interviewing for a position:
And I was asked to come back to look at a position in [SK]...half the people didn't show up for the interviews that I was scheduled to have with me... I guess they didn't want to seriously consider me coming back.
Despite the shortage of his specialty in the province, a MUN graduate noted that the lack of contact and information from NL dissuaded him from returning to the province, despite his desire to return:
You know when I was a resident in my last year I got dozen of job offers across the country and didn't hear a thing from NL.
Discussion
While a number of factors influence physicians' work location decisions, personal/family factors, specifically proximity to family, was frequently cited as the most influential factor in work location decisions. This finding further supports admission policies that reserve seats for local students (ie from the province) in order to improve the local physician supply.
The findings also highlight the importance of residency experiences in work location selection. Many physicians noted that their experiences during residency, their familiarity with the work environment and future colleagues, coupled with active recruitment efforts influenced where they chose to work. Individual physicians from both SK and NL noted that a lack of contact during residency or lukewarm recruitment efforts discouraged them from working in SK or NL.
While recruiting 'home grown' trainees may alleviate physician shortages, it should be noted that some analysts have cautioned that an over-reliance on these physicians may lead to an organizational culture that is unwelcoming to individuals trained at other institutions and to a uniformity of approach that may negatively affect education programs, institutional reputation and clinical practice32. The MUN and USK graduates acknowledged an unspoken understanding that alumni who opted to complete their residency out-of-province were unlikely to receive job offers from their home province. It may be that these local students who complete residency training elsewhere may not only be willing to return to SK or NL but may also alleviate the above concerns.
Working to the full scope of their skills was important to specific sub-groups of physicians. The exact nature and requirements needed to realize 'full scope' varied according to physician group. For example, rural family physicians wanted to care for a wider variety of patient problems and perform a greater range of procedures than their urban counterparts. Likewise, physicians with specialized training sought out locations where they would be able to exercise their additional skills and knowledge. For some physicians, this meant having access to a sufficiently large patient population or specific types of equipment and/or personnel. These findings suggest that, given the population and resources available in SK and NL, there may be limited opportunity for some physicians to work in these provinces.
The findings show that career choice has a limiting effect on alumni who are willing and able to work in rural or small urban centre. While studies have examined the factors related to students selecting careers in family medicine, the authors were unable to find Canadian studies that examined the specialists who worked in urban versus rural and small urban settings where more generalist skills are needed. Although US studies have examines the factors associated with general versus sub-specialist career choice33,34, these findings are unlikely to be generalizable to Canada, where primary care is generally provided by family physicians and GPs, rather than specialists. Further research is needed to understand the factors associated with a generalist specialist versus sub-specialist career choice in Canada.
Economic factors were also raised by many participants. However, physicians in the study were divided in terms of the importance of remuneration in their work location decisions.
While many factors for choosing a work location appear to be stable over generations, the findings highlight a number of generational differences. Early-career physicians place greater emphasis on work-life balance than older generation physicians. Late- and end-career physicians, in contrast, highlighted the medical need in the community as one of the stronger influences in their work location choices. These findings support reports that younger generation physicians may have different motivations for entering the profession and different expectations of their work life and career than their older counterparts1.
Younger generation physicians also place greater emphasis on spousal employment opportunities. This may reflect changes in society as a whole as well as changes in the physician workforce. For example, two-career households are increasingly the norm in North America; and physicians, regardless of sex, are likely to be married to spouses with their own careers and potential job markets35,36. Moreover, over the past 40 years, women comprise a significantly larger proportion of the physician workforce in Canada37. In addition to the increase in the number of two-physician households, there is also an increase in the number of male non-physician spouses. These changes have notable implications for both SK and NL. For example, while both provinces need rural physicians, rural communities may not be able to support the two physicians in a physician couple. Lack of employment opportunities for male non-physician spouses may also discourage female physicians from considering rural practice. The relatively small populations of these provinces may not be able to support physicians married to those in some specialists, thereby limiting the potential pool of physician alumni who may choose to work in these provinces.
Unlike early career physicians, a number of older generation physicians said their decision to move to another part of Canada or the world was motivated by a desire for adventure and to see new places. Early career physicians have greater exposure to different places and cultures, and more opportunities to travel, live and work away from their home province than older generations, particularly before completing their training. As a result, early career-physicians may be less likely to view their work as the means to realize a desire for adventure and travel.
Limitations
This qualitative study has limitations. Participants may not have accurately remembered their reasons for choosing a location. Their responses may also be influenced by social acceptability bias. Physicians may have felt obligated to give responses that are expected of them; for example, by under-reporting the influence of economic factors or over-reporting the influence of community need.
Generational differences in physicians' reasons for choosing a work location were documented. The factors that influenced physicians' decisions regarding work location appear to be largely stable over generations. However, early-career physicians place greater emphasis on work-life balance and spouse's employment than older generation physicians. These differences most likely stem from the changing profile of the physician workforce, as well as the different career expectations of younger generation physicians. While economic factors have been the main focus of recruitment and retention initiatives, this study's findings highlight the importance of multi-pronged strategies that address a range of factors, including the needs and expectations of younger generation physicians.
Acknowledgements
This study was funded by the Canadian Institutes of Health Research (PHE 81965), Newfoundland and Labrador Centre for Applied Health Research, Newfoundland and Labrador Industry Research and Innovation Fund, and Saskatchewan Innovation and Science Fund.
References
1. Bickel J, Brown AJ. Generation X: implications for faculty recruitment and development in academic health centres. Academic Medicine 2005; 80(3): 205-210.
2. Watson DE, Slade S, Buske L, Tepper J. Intergenerational differences in workloads among primary care physicians: a ten-year population-based study. Health Affairs 2006; 25(6): 1620-1628.
3. Watson DE, Reid RJ, Roos N, Heppner P. Growing old together: the influence of population and workforce aging on supply and use of family physicians. Canadian Journal on Aging 2005; 24(Suppl1): 37-45.
4. Watson DE, Katz A, Reid RJ, Bogdanovic B, Roos N, Heppner P. Family physician workloads and access to care in Winnipeg: 1991-2001. Canadian Medical Association Journal 2004; 171: 339-342.
5. Barer ML, Wood L, Schneider DG. Towards improved access to medical services for relatively underserved populations: Canadian approaches, foreign lessons. Vancouver: Centre for Health Services and Policy Research, University of British Columbia, 1999.
6. Bible BL. Physicians' views of medical practice in nonmetropolitan communities. Public Health Reports 1970; 85: 11-17.
7. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77: 790-798.
8. Carter RG. The relation between personal characteristics of physicians and practice locations in Manitoba. Canadian Medical Association Journal 1987; 136: 366-368.
9. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R et al. Rural background and clinical rural rotations during medical training: effect on practice location. Canadian Medical Association Journal 1999; 160: 1159-1163.
10. Holmes JE, Miller DA. Factors affecting decision on practice locations. Journal of Medical Education 1986; 61: 721-726.
11. Johnson SE, Baeumler WL, Carter RE. The family physicians: a comparative study of Minnesota and Wisconsin family physicians practicing in rural and urban communities. Minnesota Medicine 1973; 56(8): 713-718.
12. Mathews M, Park AD, Rourke JTB. The Contribution of Memorial University's medical school to rural physician supply. Canadian Journal of Rural Medicine 2008; 13(1): 15-21.
13. Payne JC. Practice and lifestyle preferences of rural family physicians. Ontario Medical Review 1992; March: 37-42.
14. Rourke JTB, Incitti F, Rourke LL, Kennard MA. Keeping family physicians in rural practice - Solutions favoured by rural physicians and family medicine residents. Canadian Family Physician 2003; 49: 1142-1149.
15. Rosenblatt RA, Whitcomb ME, Cullen TJ, Lishner DM, Hart LG. which medical schools produce rural physicians? JAMA 1992; 268: 1559-1565.
16. Mathews M, Rourke JTB, Park AD. National and provincial retention of medical graduates of Memorial University. Canadian Medical Association Journal 2006; 175(4): 357-360.
17. Ryten E, Thurber D, Buske L. The Class of 1989 and physicians supply in Canada. Canadian Medical Association Journal 1998; 158(6): 728-728.
18. Sempowski IP, Godwin M, Seguin R. Physicians who stay versus physicians who go: results of a cross sectional survey of Ontario rural physicians. Canadian Journal of Rural Medicine 2002; 7: 173-179.
19. Florizone A. SMA survey of rural physicians. Canadian Journal of Rural Medicine 1997; 2: 180-186.
20. Parker RS, Sorensen AA. The tides of rural physicians: the ebb and flow, or why physicians move out of and into small communities. Medical Care 1978; 16: 152-166.
21. Yang J. Potential urban-to-rural physician migration: the limited role of financial incentives. Canadian Journal of Rural Medicine 2003; 8: 101-106.
22. Janes R, Dowell A. New Zealand Rural General Practitioners 1999 Survey - Part 3: rural general practitioners speak out. New Zealand Medical Journal 2004; 117(1191): 1-9. Available: http://journal.nzma.org.nz/journal/117-1191/815/content.pdf
23. MacIsaac P, Snowdon T, Thompson R, Crossland L, Veitch C. General practitioners leaving rural practice in Western Victoria. Australian Journal of Rural Health 2000; 8: 68-72.
24. Costa AJ, Labuda Schrop S, McCord G, Gillanders WR. To stay or not to stay: factors influencing family practice residents' choice of initial practice location. Family Medicine 1996; 28: 214-219.
25. Canadian Policy Research Networks Inc. Health human resource planning in Canada - physicians and nursing work force issues. Ottawa: Commission on the Future Health Care in Canada, 2002.
26. Pathman DE, Konrad TR, King TS, Taylor DH, Koch GG. Outcomes of States' Scholarship, Loan Repayment, and related programs for physicians. Medical Care 2004; 42: 560-568.
27. Pathman DE, Konrad TR, Ricketts TC. The comparative retention of National Health Service Corps and other rural physicians - results of a 9 year Follow-up Study. JAMA 1992; 268: 1552-1558.
28. Sempowski IP. Effectiveness of financial incentives in exchange for rural and underserviced area return-of-service commitments: systematic review of the literature. Canadian Journal of Rural Medicine 2004; 9: 82-88.
29. Singer JD, Davidson S, Graham S, Davidson HS. Physician retention in community and migrant heath centres: who stays and for how long? Medical Care 1998; 36: 1198-1213.
30. Statistics Canada. 2006 Community Profiles. (Online) 2011. Available: http://www12.statcan.gc.ca/census-recensement/2006/dp-pd/prof/92-591/index.cfm?Lang=E (Accessed 12 December 2011).
31. Mathews M, Seguin M, Card R, Glacken G. 2007 Work locations of University of Saskatchewan medical graduates. St Johns: Division of Community Health & Humanities, Memorial University of Newfoundland, 2007.
32. Katz AN, DeWals P, West LJ. Report of the Inquiry into Allegations of Employer Misconduct at the Memorial University of Newfoundland and Eastern Health Corporation. (Online) 2008. Available: http://www.popadiukinquiry.ca/Popadiuk%20Inquiry%20Report%20March%202008.pdf (Accessed 14 July 2011).
33. Schwatrz MD, Durning S, Linzer M, Hauer KE. Changes in medical students' views of internal medicine careers from 1990 to 2007. Archives of Internal Medicine 2011; 17(8): 744-749.
34. Garibaldi RA, Popkave C, Bylsma W. Career plans for trainees in internal medicine residency programs. Academic Medicine 2005; 80(5): 207-215.
35. Sobeks NW, Justice AC, Hinze S, Chirvath HT, Lasek RJ, Chren MM et al. When doctors marry doctors: a survey exploring the professional and family lives of young physicians. Annals of Internal Medicine 1999; 130(4): 312-319.
36. Woodward CA. When a physician marries a physician: effects of physician-physician marriage on professional activities. Canadian Family Physician 2005; 51: 850-851.
37. Canadian Institute for Health Information. Health Personnel in Canada 1991 to 2000. Ottawa: CIHI, 2001.



