Diabetes mellitus is one of the most common chronic diseases in the USA, with approximately 26 million diagnosed individuals, representing more than 8% of the total US population. The US Department of Health and Human Services has listed diabetes as one of six targeted priority conditions needing intervention to reduce racial health disparities1. Proper diabetes management is essential to prevent complications such as heart disease, renal failure, pregnancy complications, hypertension, blindness, nervous system damage, or metabolic imbalances2-6. This is especially important for older persons with diabetes, who have higher rates of heart disease, stroke, and concurrent disease7-10.
One indicator of inadequate diabetes control is hospitalization. Up to one-third of persons with diabetes require more than one hospitalization per year4. Despite a decline in the age-adjusted hospitalization rate among persons with diabetes to 51.9 per 1000 in 200611, diabetes accounts for more than 10% of all hospitalizations, second only to circulatory diseases12. Diabetes-related admissions also vary by age, income, and type of insurance4,5,13-15.
Those with complex care needs, such as persons with diabetes, often require care in multiple settings (ie inpatient and outpatient) as well as across specialties (eg primary care and sociality care)16,17. When a person with diabetes has been hospitalized, the referral process is key to reestablishing appropriate ambulatory care. Transitional care can be been defined as a set of actions designed to ensure the coordination and continuity of healthcare as patients transfer between locations or different levels of care18. When patients navigate these transitions across settings or providers, they are vulnerable to fragmentation of care, incomplete or miscommunications, and other issues that may adversely affect outcomes16,19-24. Proper care transitions can improve the quality of care for patients with chronic conditions by decreasing hospitalizations, decreasing emergency department use, increasing the receipt of preventive services, and achieving improved metabolic control17,25. These transitions can also be aided by the use of diabetes education programs26,27.
Several factors contribute to poor transitions of care. Increasing specialization within health care has led many providers, such as hospitalists, to practice in only a single setting. With hospitalists assuming the traditional role of primary care physicians in the treatment of hospitalized patients23, providers are often unfamiliar with the capacity of other care settings which may result in inappropriate, improper, or incomplete transfers to the community20. This, combined with a lack of communication and information transfer between hospital-based and primary care physicians16,19,22; inadequate information on discharge summaries22 inadequate patient education21; and patient barriers such as a lack of transportation, financial constraints, lack of health insurance, and access to providers17,28, can lead to poor follow-up care after hospital discharge.
Rural residents with diabetes experience difficulties in obtaining needed transitional care. Rural Black adults are less likely to be diagnosed and effectively treated for diabetes than other population groups29,30. Similarly, rural Hispanics are also more likely than Whites to have diabetes (either diagnosed or undiagnosed)31. Medicare Beneficiaries living in rural areas often have lower incomes and are in poorer health status than their urban counterparts32. Rural counties, particularly those with majority non-White populations, are predominantly classified as Health Professional Shortage Areas33, indicating a lack of providers available to residents of those counties. The Dartmouth Atlas also reported wide variation in post-discharge follow-up care across hospital referral regions34. Because rural residents comprise a larger proportion of the total Medicare population35 than of the total national population32, a more detailed knowledge about the experiences of rural beneficiaries would be beneficial to improve the efficiency of the Medicare program. Improved knowledge regarding issues such as service availability36, hospitalizations, readmissions, and quality of outpatient care and transitions of care will allow policy-makers to further support rural Beneficiaries, improve their care, and potentially improve the cost efficiency of the Medicare program by shifting care from inpatient to outpatient settings.
These disparities are further exacerbated by barriers faced by non-White patients with diabetes. Non-Whites have historically higher rates of diabetes prevalence and complications from diabetes3,37; yet lower rates of diabetic control and adherence to clinical guidelines, lower ambulatory service utilization, and higher hospitalization rates than Whites4,13,15,38,39.
Few studies have specifically examined post-hospitalization care transitions among rural residents with diabetes, particularly rural minorities. This study estimated both hospital admission rates for rural Medicare Beneficiaries with diabetes and the proportion of hospitalized patients with prompt post-discharge follow up in the outpatient setting. Particular emphasis was given to estimates across race subgroups, to determine if further disparities exist among these rural Medicare Beneficiaries.
Data and population
This analysis utilized the 2005, 5% Medicare sample, obtained from the Chronic Conditions Warehouse (CCW). The CCW was legislatively created by the US Medicare Prescription Drug Improvement and Modernization Act of 2003 and is maintained by the Research Data Center (RESDAC). The data included inpatient hospital stay claims, carrier claims (eg physician encounter claims) and beneficiary information such as demographic information and chronic illness diagnoses. Data were merged into one file by beneficiary. Information regarding the county of residence of the beneficiary was drawn from the 2007 Area Resource File (ARF), which contains geographic codes and descriptors which enable it to be linked to many other files and to aggregate counties into various geographic groupings40. The ARF contains more than 6000 variables regarding health facilities, health professions, measures of resource scarcity, health status, economic activity, health training programs, and socioeconomic and environmental characteristics.
The study population was limited to Beneficiaries who did not die during the year and did not have one of the following diagnoses: congestive heart failure, Alzheimer's disease, dementia, schizophrenia, chronic kidney disease, or end stage renal disease. Beneficiaries were also excluded if they were discharged to a long term care facility, another hospital, hospice, or with home health services. Theses exclusions reduced the study population to one in which care would only be received if sought at a physician's office or similar setting. Thus, only Beneficiaries who were hospitalized and discharged back into the community, or who were not hospitalized at all (for calculating rates) were included in the study.
Analysis
The dependent variable was the presence of a billed physician visit, in an office setting, within 30 days of discharge of an index hospitalization. Independent variables consisted of the Beneficiary's race (White, Black, Other), sex, age (65-74, 75-84, ≥85), and diabetes diagnosis. The CCW also includes indicators for twenty-one separate comorbid chronic conditions, based upon claims and diagnoses. A sum of the total number of comorbid conditions was used as an indicator of overall patient acuity.
Rurality was defined using the 2003 Urban Influence Codes (UIC)41. The UICs of 1 and 2 levels of rurality were classified as 'Urban' while all other UICs were classified as rural. Analysis across levels of rurality used three groups: 'Micropolitan Rural' (UICs 3, 5, and 8) 'Small Adjacent Rural' (UICs 4, 6, and 7) and 'Remote Rural' (UICs 9, 10, 11, and 12).
Other ecological characteristics drawn from the ARF included the ratio for primary care physicians per 1000 residents of a county (divided into quartiles) as a measure of access to physician care; the number of hospitals in the county (0, 1, or ≥2) as a measure of the healthcare infrastructure of the county; per capita income of the county (divided into quartiles) as a proxy for personal income; and region (Northeast, South, Midwest, West) to account for the regional variations that can occur in healthcare delivery34.
Initial analysis estimated the proportion of beneficiaries with diabetes, by the characteristics of interest, subset by rurality. Estimates of the proportion of those beneficiaries with diabetes that had at least one hospitalization in the year by the characteristics of interest were then calculated, also subset by rurality. Subsequent analyses were limited to those beneficiaries with diabetes and at least one hospitalization. Estimates of the proportion of hospitalized beneficiaries with a 30 day follow-up claim were produced by the characteristics of interest and subset by rurality. All differences across levels of rurality (using urban as the referent group) were tested using Wald χ2 tests at the α=0.05 level and adjusted for multiple comparisons using Bonferroni's method.
Multivariable ordinary least squares logistic regression, controlling for clustering at the county level, was utilized to determine factors associated with having a follow-up claim within 30 days of discharge. This analysis utilized three models, with a dichotomous indicator of having a 30 day follow up as the dependent variable. The first included only the four-level rural variable as the independent variable; the second model added the demographic information of the beneficiary (race, sex, age) as well as the number of comorbidities; the third and final model included the ecological factors (primary care physician to resident ratio, hospitals in the county, per capita income, and region).
All analyses were designated as exempt by the University of South Carolina Institutional Review board (HSA-4983).
Population characteristics and prevalence of diabetes
The initial sample, minus exclusions, totaled 1 411 346 beneficiaries. More than 14% had diabetes; this rate was higher among rural than urban residents (16.7% vs 13.5%, p <0.001; Table 1). Males, those under the age of 75 years, and non-Whites were all more likely to have diabetes. Rural residents, across these demographic characteristics, remained more likely to have diabetes. The prevalence of diabetes was also higher in rural areas across the ecological variables examined (primary care physician to population ratio, hospital availability, per capita income, and region). With the exception of remote rural counties, beneficiaries living in areas with proportionately fewer physicians were more likely to have a diagnosis of diabetes. Similarly, diabetes was more prevalent among beneficiaries living in a county without a hospital. Diabetes prevalence was inversely related to per-capita income. Beneficiaries living in the rural South had the highest rate of diabetes.
Table 1: Percentage diabetes prevalence among Medicare beneficiaries, by characteristics and rurality, 2005
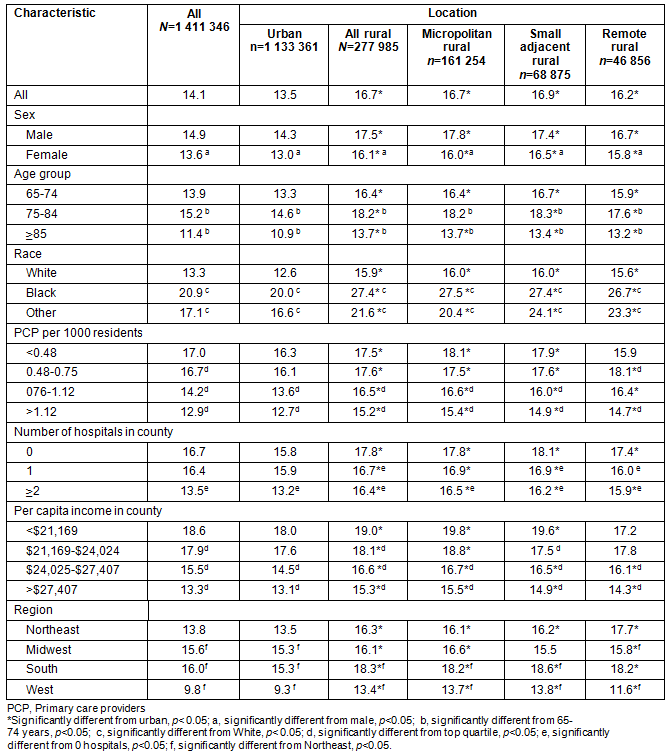
Hospitalization and follow-up among persons with diabetes
The estimated proportion of Medicare beneficiaries with diabetes that had at least one hospitalization in 2005 is provided (Table 2). Rural residents had significantly higher rates (13.0%) than urban residents (12.0%); this rate was highest among remote rural residents (13.7%). The hospitalization proportions were higher among females and older beneficiaries. Black beneficiaries were less likely to be hospitalized than their White peers in both urban and rural settings; persons of Other race residing in urban areas were also less likely to be hospitalized. Residents in counties with lower primary care provider ratios, more hospitals, and in the South and Midwest also had higher rates. In general, rural residents had higher rates across all the variables of interest.
Table 2: Percentage beneficiaries with diabetes with at least one hospitalization by rurality, 2005
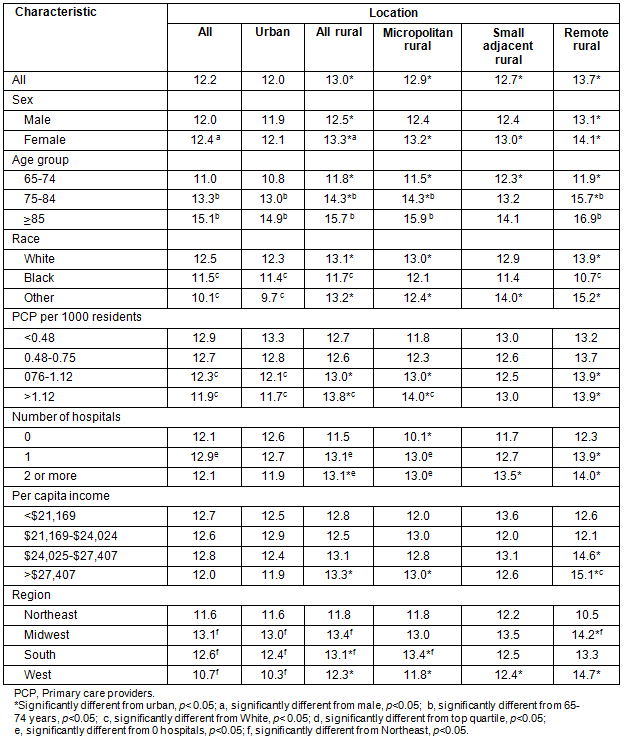
Unadjusted 30 day follow-up estimates
Overall, 88.5% of Medicare beneficiaries hospitalized in 2005 had a follow-up visit at a physician's office or in health clinic within 30 days (Table 3). This proportion was lower among rural residents (86.4%) and decreased with rurality; only 82.5% of remote rural Beneficiaries had a follow-up visit within 30 days. The proportion of beneficiaries with a 30 day follow up was lower for males and younger beneficiaries. In urban counties, Black beneficiaries were less likely than Whites to receive a 30 day follow up (86.1% vs 89.5%; Table 3), while beneficiaries of Other race did not differ. In rural counties, beneficiaries of Other race were less likely to receive a 30 day follow up than Whites (83.9% vs 86.5%), while Black beneficiaries did not differ. Black beneficiaries residing in small rural counties adjacent to metropolitan areas were more likely to receive prompt follow up than were urban Black beneficiaries. Among all beneficiaries, a 30 day follow up was more common among beneficiaries living in counties with higher physician/population ratios, at least one hospital, higher per capita income, and located in the Northeast. These rates all decreased as rurality increased.
Table 3: Percentage physician follow-up within 30 days among hospitalized beneficiaries with diabetes, 2005, by rurality
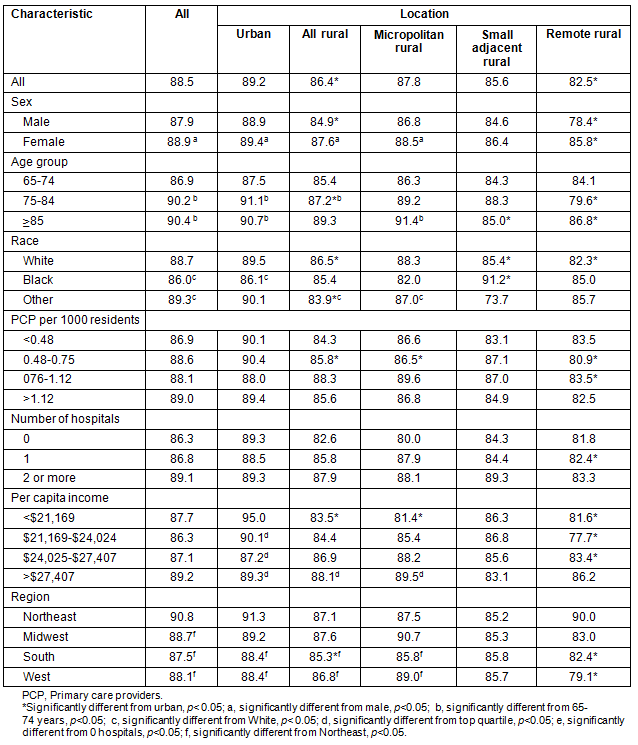
Adjusted 30 day follow-up estimates
The initial unadjusted analytic model found that living in remote rural counties was associated with a reduced odds of a follow-up physician visit within 30 days of discharge, compared with urban residence (Table 4, Model 1). Adding beneficiary characteristics did not significantly change the odds associated with rural residence (Table 4, Model 2). Adding county characteristics rendered rural-urban differences non-significant (Table 4, Model 3). Among county characteristics, only regional effects were significant, with all regions having reduced odds of prompt follow up compared with the Northeast. Beneficiary characteristics associated with reduced odds of 30 day follow up in the full model included male sex and Black race. Each additional comorbidity markedly increased the odds for 30 day follow up.
Table 4: Adjusted odds of having a follow-up physician claim within 30 days among hospitalized beneficiaries with diabetes, 2005
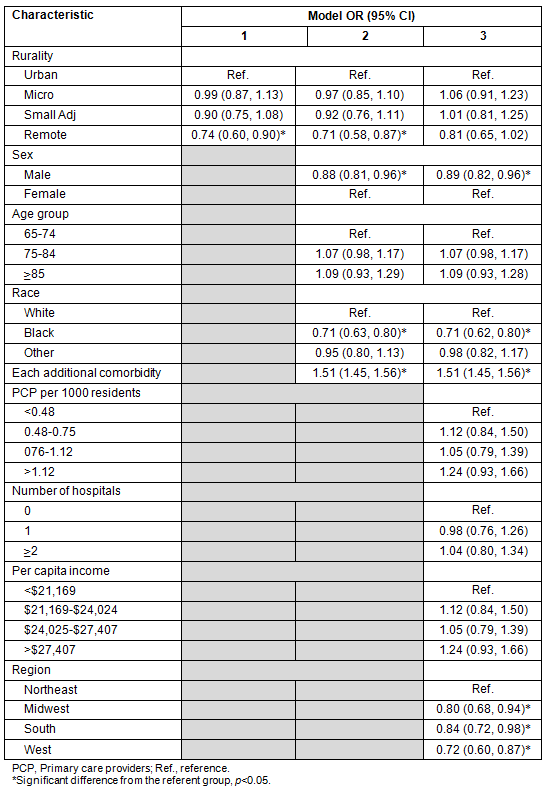
Discussion
The 30 day post-hospitalization follow-up rate was examined among beneficiaries with diabetes to determine if rural residence was associated with these rates. In the adjusted yet simplified analysis, residents of remote rural counties had a reduced odds for a 30 day follow up when compared to urban residents (OR 0.74, CI 0.60-0.90). However, when factors associated with visit behavior at both the individual and county level were added to the model, residents of rural counties were no less likely to have a follow-up visit within 30 days than their counterparts.
Because all subjects in the analysis were insured via Medicare, the hypothesis was that the remaining barriers to accessing healthcare services, such as access to providers, need, and personal preferences, would be associated with follow-up behavior. These results confirm that personal characteristics, such as race and sex, are associated with follow-up care, and may be indicative of either personal preferences or institutional biases. These findings also confirm a well-documented racial disparity in service utilization13,15,38. In addition, measures of need such as additional comorbidities and older age are also associated with seeking care. Physician availability, measured as primary care physicians per 1000 residents, was not associated with seeking care. This may indicate that even in areas with fewer providers, having a stable source of insurance in Medicare provides adequate access to services.
Even if the patient is motivated to seek proper follow-up care, additional barriers may reduce their ability to fulfill this desire. These barriers may include the lack of a usual source of care, not fulfilling a visit scheduled by the inpatient care team, inability to access the care itself, and lower levels of health literacy that would reduce their perceived need for the care39,40. For rural and non-White residents, travel difficulties exacerbate these barriers, further reducing the likelihood of a follow up42. Rural residents also lack adequate diabetes educational support, further exacerbating outcomes26,27.
Despite these indications, evidence remains that the transition from inpatient to outpatient care is not ideal in smaller rural areas. Research has documented several barriers to proper outpatient care, such as inadequate or unavailable discharge summaries and inadequate communication16,19-24,43. Further work is warranted to determine if these rural difficulties are compounded by regional differences. The Dartmouth Atlas indicated such a regional difference, but it is unknown if rurality and region compound or lessen these effects34. The findings do indicate a potential compounding effect, particularly in the West and Midwest; further examination of regional effects could lead to more targeted interventions.
Interventions aimed at improving the care provided have been shown to be effective, particularly for non-Whites and those with diabetes44. Additionally, in these areas technological solutions such as Health Information Exchanges and electronic communications45 are adopted in lower proportions than in larger areas with more resources. Little research, to date, has examined how healthcare providers in rural communities communicate for the purpose of transitions of care. Developing and implementing successful models that facilitate provider communication in a cost effective manner is critical to improving follow-up care among residents of smaller rural counties.
With proper follow up, subsequent hospitalization would be reduced, as would other inappropriate utilization of healthcare services such as emergency department visits17 Such care would also serve to prevent further morbidity via preventive service delivery and metabolic control of the patient's disease25. If the issue of inadequate follow-up care among rural Medicare beneficiaries is not addressed, the potential for higher hospitalization rates, morbidity, and premature mortality is increased. Programs and interventions improving post-hospitalization care would not only reduce the services and, thus, the costs associated with such care, but also improve the quality of life experienced by residents of these smaller rural areas.
Limitations
The analysis has several limitations. First, the data used were claims-based, and not intended to fully document clinical encounters. Second, detailed information regarding the beneficiaries in the analysis was not available; information such as household income, having a usual source of care, or personal preferences regarding health care would be important to more fully understand the topic at hand. Finally, it is unknown what proportion of those discharged had a true need for follow-up care. The assumption was that 100% of those discharged needed such care, but it is possible that different groups needed the care at different rates. A sub-analysis of only those instructed to obtain such care may yield differing results.
Despite the limitations, the findings from this analysis indicate that residents of smaller rural areas are less likely to obtain follow-up care within 30 days of a hospital discharge. It was possible to identify those factors related to follow-up care that were more common among these rural residents, such as sex, race, and comorbidities. Interventions and programs aimed at improving the rate of post-hospitalization follow-up care would be beneficial for the Medicare system, the beneficiaries, and the areas in which they live.
Acknowledgement
This manuscript was prepared under Grant Award No 6 U1C RH 03711-04-01 with the Federal Office of Rural Health Policy, Health Resources and Services Administration.
References
1. Agency for Healthcare Research and Quality. List of priority conditions for research under Medicare Modernization Act released. Rockville, MD: AHRQ, 2004.
2. Beckman JA, Creager MA, Libby P. Diabetes and Atherosclerosis. JAMA 2002; 287(19): 2570-2581.
3. Centers for Disease Control. National diabetes fact sheet: General information and national estimates on diabetes in the United States, 2007. Atlanta, GA: CDC, 2008.
4. Jiang HJ, Stryer D, Friedman B, Andrews R. Multiple hospitalizations for patients with diabetes. Diabetes Care 2003; 26(5): 1421-1426.
5. Robbins JM, Webb DA. Hospital admission rates for a racially diverse low-income cohort of patients with diabetes: the Urban Diabetes Study. American Journal of Public Health 2006; 96(7): 1260-1264.
6. Selvin E, Marinopoulous S, Berkenblit G, Rami T, Brancati F, Powe N et al. Meta-Analysis: Glycosylated Hemoglobin and Cardiovascular Disease in Diabetes Mellitus. Annals of Internal Medicine 2004; 141(6): 421-431.
7. Andersson DK, Svärdsudd K. Long-term glycemic control relates to mortality in type II diabetes. Diabetes Care 1995; 18(12): 1534.
8. Kuusisto J, Mykkanen L, Pyorala K, Laakso M et al. Non-insulin-dependent diabetes and its metabolic control are important predictors of stroke in elderly subjects. Stroke 1994; 25(6): 1157-1164.
9. Kuusisto J, Mykkanen L, Pyorala K, Laakso M et al. NIDDM and its metabolic control predict coronary heart disease in elderly subjects. Diabetes 1994; 43(8): 960.
10. Moss SE, Klein R, Klein B, Meuer SM et al. The association of glycemia and cause-specific mortality in a diabetic population. Archives of Internal Medicine 1994 154(21): 2473.
11. Centers for Disease Control and Prevention. National Center for Health Statistics, Division of Health Care Statistics, data from the National Hospital Discharge Survey and Division of Health Interview Statistics, data from the National Health Interview Survey. (Online) 2011. Available: http://www.cdc.gov/diabetes/statistics/dmfirst/fig3.htm (Accessed 23 May 2012).
12. Centers for Disease Control and Prevention. National Diabetes Surveillance System. (Online) 2011. Available: http://www.cdc.gov/diabetes/statistics/index.htm (Accessed 23 May 2012).
13. Howard DL, Hakeem F, Njue C, Carey T, Jallah Y. Racially disproportionate admission rates for ambulatory care sensitive conditions in North Carolina. Public Health Reports 2007; 122(3): 362-72.
14. Jiang HJ, Andrews R, Stryer D, Friedman B. Racial/Ethnic Disparities in Potentially Preventable Readmissions: The Case of Diabetes. American Journal of Public Health 2005; 95(9): 1561-1567.
15. Laditka JN, Laditka SB. Race, ethnicity and hospitalization for six chronic ambulatory care sensitive conditions in the USA. Ethnicity and Health 2006; 11(3): 247-63.
16. Coleman EA. Falling Through the Cracks: Challenges and Opportunities for Improving Transitional Care for Persons with Continuous Complex Care Needs. Journal of the American Geriatrics Society 2003; 51(4): 549-555.
17. Cook C, Seifert K, Hull B, Hovan M, Charles J, Miller-Cage V et al. Inpatient to Outpatient Transfer of Diabetes Care: Planning for an Effective Hospital Discharge. Endocrine Practice 2009; 15(3): 263-269.
18. Coleman EA, Boult C. Improving the quality of transitional care for persons with complex care needs. Journal of the American Geriatric Society 2003; 51(4): 556-557.
19. Arora VM, Farnan JM. Care transitions for hospitalized patients. The Medical Clinics of North America 2008; 92(2): 315-324.
20. Coleman EA, Berenson RA. Lost in transition: challenges and opportunities for improving the quality of transitional care. Annals of Internal Medicine 2004; 141(7): 533-336.
21. Kripalani S, Jackson A, Schnipper J, Coleman E. Promoting effective transitions of care at hospital discharge: a review of key issues for hospitalists. Journal of Hospital Medicine 2007; 2(5): 314-323.
22. Kripalani S, LeFevre F, Phillips C, Williams M, Basaviah P, Baker D. Deficits in Communication and Information Transfer Between Hospital-Based and Primary Care Physicians: Implications for Patient Safety and Continuity of Care. JAMA 2007; 297(8): 831-841.
23. Pham HH, Grossman JM, Cohen G, Bodenheimer T. Hospitalists and care transitions: the divorce of inpatient and outpatient care. Health Affairs 2008; 27(5): 1315-27.
24. Van Walraven C, Mamdani M, Fang J, Austin P. Continuity of care and patient outcomes after hospital discharge. Journal of General Internal Medicine 2004; 19(6): 624-631.
25. Cabana MD, Jee SH. Does continuity of care improve patient outcomes? Journal of Family Practice 2004; 53(12): 974-980.
26. O'Brien T, Denham SA. Diabetes Care and Education in Rural Regions. Diabetes Educator 2008; 34(2): 334-347.
27. Denham S, Remsberg K, Wood L. Diabetes education in the Appalachian region: providers' views. Rural and Remote Health 10: 1321. (Online) 2010. Available: www.rrh.org.au (Accessed 23 May 2012).
28. Powell MP, Glvoer S, Probst J, Laditka S et al. Assessment of barriers to the delivery of Medicare reimbursed diabetes self-management education in rural areas. Columbia, SC: South Carolina Rural Health Research Center, 2004.
29. Hale N, Bennett K, Probst J. Diabetes Care and Outcomes: Disparities across Rural America. Journal of Community Health 2010; 35(4): 365-374.
30. Mainous AG 3rd, King D, Garr D, Pearson W. Diabetes and cardiovascular disease in rural African Americans. Columbia, SC: South Carolina Rural Health Research Center, University of South Carolina, 2003.
31. Mainous AG 3rd, Koopman R, Geesey ME. Diabetes and hypertension among rural Hispanics: Disparities in Diagnostics and disease management. Columbia, SC: South Carolina Rural Health Research Center, 2004.
32. MEDPAC. Medicare Payment Advisory Committee. A Data Book: Healthcare Spending and the Medicare Program. (Online) 2006. Available: http://www.medpac.gov/documents/jun10databookentirereport.pdf (Accessed 30 May 2012).
33. Probst J, Moore C, Glover S, Samuels M. Person and Place: The compounding effect of race/ethnicity and rurality on health. American Journal of Public Health 2004; 94: 1695-1703.
34. Goodman DC, Fisher E, Chang C, Raymond S, Bronner K. After Hospitalization: A Dartmouth Atlas Report on Post-Acute Care for Medicare Beneficiaries. (Online) 2011. Available: http://www.dartmouthatlas.org/downloads/reports/Post_discharge_events_092811.pdf (Accessed 23 May 2012).
35. DeLia D. Distributional issues in the analysis of preventable hospitalizations. Health Services Research 2003; 38(6 Pt 2): 1761-1779.
36. Rosenthal TC, Fox C. Access to health care for the rural elderly. JAMA 2000; 284(16): 2034-2036.
37. Young BA, Maynard C, Boyko EJ. Racial Differences in Diabetic Nephropathy, Cardiovascular Disease, and Mortality in a National Population of Veterans. Diabetes Care 2003; 26(8): 2392-2399.
38. Harris MI. Racial Ethnic Differences in Health Care Access and Health Outcomes for Adults With Type 2 Diabetes. Diabetes Care 2001; 24(3): 454-459.
39. Harris MI, Eastman R, Cowie C, Flegal K, Eberhardt M. Racial and ethnic differences in glycemic control of adults with type 2 diabetes. Diabetes Care 1999; 22(3): 403.
40. US Department of Health and Human Services. Area Resource File (ARF). 2007. Rockville, MD: US Department of Health and Human Services, Health Resources and Services Administration, Bureau of Health Professions, 2007.
41. US Department of Agriculture Economic Research Service. Understanding Rural America: County Types. (Online) 1997. Accessed: http://www.ers.usda.gov/publications/aib710/aib710l.htm (Accessed 23 May 2012).
42. Probst J, Laditka S, Want J, Johnson A. Effects of residence and race on burden of travel for care: cross sectional analysis of the 2001 US National Household Travel Survey. BMC Health Services Research 2007; 7(1): 40.
43. Witherington EMA, Pirzada OM, Avery AJ. Communication gaps and readmissions to hospital for patients aged 75 years and older: observational study. Quality and Safety in Health Care 2008; 17(1): 71-75.
44. Parrish M, O'Malley K, Adams R, Adams S, Coleman E. Implementation of the care transitions intervention: Sustainability and lessons learned. Professional Case Management 2009; 14(6): 282-293.
45. Chen Y, Brennan N, Magrabi F. Is email an effective method for hospital discharge communication? A randomized controlled trial to examine delivery of computer-generated discharge summaries by email, fax, post and patient hand delivery. International Journal of Medical Informatics 2010; 79(3): 167-172.


