Canada is well known for its rural heritage. Using the Statistics Canada definition, in 2004, 21% of Canadians lived in rural areas. However, only 9% of physicians practise rurally1. This shortage is even more pronounced for the rural specialist as only 2.4% of Canadian specialist physicians practise rurally1. To help sustain rural communities and small urban centres, as well as to increase access to health services, it is important for Canada to increase the number of specialty physicians practising in rural areas. In recent years there has been a shift from financial incentives to a focus on medical education as a means of rural recruitment2. Presently, all Canadian medical schools offer postgraduate training that includes some rural opportunities. However, the duration and requirements vary widely across speciality disciplines3.
There are many studies in the literature that have focused on the impact of rural family medicine residencies2,4-7. Relatively few have focused on training a specialty resident in a rural setting8-12. The literature is limited and tends to focus predominantly on programme descriptions8,11 and the views of rural preceptors10. Others describe programmes where participation in the rural rotation is optional or voluntary and thus may be studying a resident population with an existing bias towards rural practice8,9,12. Nevertheless, these studies do continue to support previous work suggesting that training in a rural community predicts practice location on graduation8,9.
A 2005 review of the literature found there were no studies that explored rural specialty education as a factor in choosing a rural practice location13. It stated that less populated areas lack a 'critical mass of patients' to support educational opportunities for specialist residents13. Since that publication there have been two published studies that have linked rural specialty postgraduate training as a factor in choosing a rural practice location. Rourke reported a 'profound effect' of residency training location from 1997 to 2004 as a predictor for practice location, with nearly 50% of residents graduating from rural training choosing to practise in rural communities8. Similarly, Hogenbirk found significantly more residents who participated in rural training located their practices in rural areas compared to matched non-participants following graduation9.
Distributed Learning and Rural Initiatives (DLRI) at the University of Calgary provides medical students and residents the opportunity to experience rural medical practice through rural and regional rotations. The Distributed Royal College Initiative (DistRCI) provides specialty Royal College residents with an opportunity to complete mandatory rotations with rural and regional preceptors. This project report explores the results from DistRCI rotation evaluations, and analyzes residents' experiences and attitudes towards the rotation, including potential practise in a regional centre, before and after their rotation. Social learning theory is used to interpret results.
The DistRCI seeks to increase placement for core specialty rotations outside of the metropolitan teaching centre. While smaller more subspecialized disciplines are starting to provide these rotations, they have been primarily dominated by the presence of General Internal Medicine and General Surgery postgraduates. Rotations range from four to eight weeks in duration and have specific goals and objectives established by their individual programmes for community-based core experiences. Residents follow the same call guidelines as those in the metropolitan centre but are exposed to a smaller group of colleagues treating patients with a broader undifferentiated presentation without the subspecialty or extensive infrastructure available in the larger cities. In this study, residents completed rotations at either Chinook Regional Hospital in Lethbridge, Alberta or Red Deer Regional Hospital in Red Deer, Alberta. Both communities have populations that are under 100,000 people14. Housing and transport are reimbursed to the resident in a timely manner to ensure there are no financial disincentives.
Between July 2010 and June 2011, 40 University of Calgary Royal College residents who completed a regional rotation were emailed an evaluation survey on completion of the experience. The survey consisted of 7 Likert scale questions regarding preceptors' knowledge of rotation goals, CanMEDS competency framework, residents' satisfaction with their regional experience, their interest in undertaking a similar rotation and future interest in practising in a regional community. Data were analyzed using descriptive statistics. McNemar's test was used to determine if there was a significant change in the likelihood of residents indicating they would be interested in practising regionally following the rotation15.
Two open-ended questions were available seeking comments about the training site and additional comments or recommendations. Two investigators, one completely independent of the individual programmes and the second who had no resident contact, reviewed all transcripts independently to identify emergent themes. They met and discussed the different independent analyses and iteratively worked to develop a common thematic structure and ensure the coding was being consistently applied.
Ethics approval was obtained from the Conjoint Health Research Ethics Board of the University of Calgary.
A total of 73% (29) of residents replied to the survey. Most residents were in their second year of training. The breakdown of responses between the training year and discipline are provided (Table 1). Because of the number of respondents and the wide variety of specialties represented, the analysis focuses on three main groups: General Surgery, General Internal Medicine and All Other Specialities (including anaesthesia, paediatrics, orthopaedics, nephrology, pathology and haematology). For this report, survey results were organized into three sections: overall resident satisfaction and recommendation; resident interest in a future rural rotation; and likelihood of the resident practising in a regional community. The survey questions and responses are provided (Table 2).
Table 1: Response rate and year of training
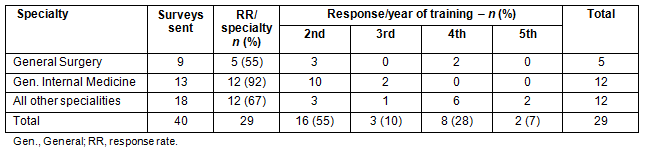
Table 2: Survey questions and results
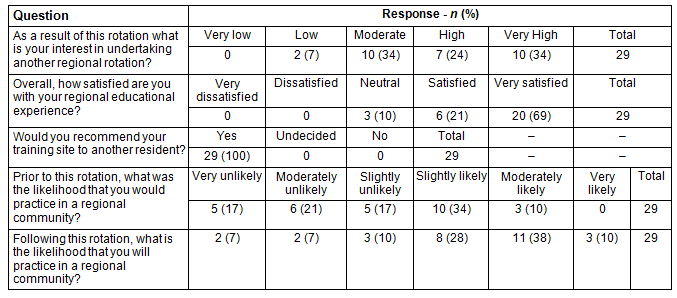
All respondents indicated that they would recommend their training site to another resident. As a group, residents responded (90%) that they were satisfied or very satisfied with their regional experience.
The majority (58%) indicated they would be highly or very highly interested in undertaking another regional rotation, while 34% responded they would be moderately interested in another regional rotation. Between the larger groups noted, internal medicine (66%) and all other specialties (58%) reported being highly or very highly interested in another rural rotation, whereas only 40% of surgery respondents were interested in another rotation.
The post-rotation survey asked residents to reflect on how likely they were to practise in a regional community both before and after completing the rotation. Accounting for rounding, 45% of residents reported that prior to the rotation they were likely to consider practising in a regional community. This opinion increased to 76% of residents following their rotation. Using McNemar's test, a significant tendency was found for residents who changed their opinion to be more likely to want to practise regionally after the rotation (p=0.022). When analyzing residents who reported a change in their likelihood of rural practice, we found only two residents reported a negative shift. Eleven of the 29 residents (38%) reported a change in opinion from unlikely before to likely following the rotation: of these, 9% were from surgery, 45% were from internal medicine and 45% were from all other disciplines.
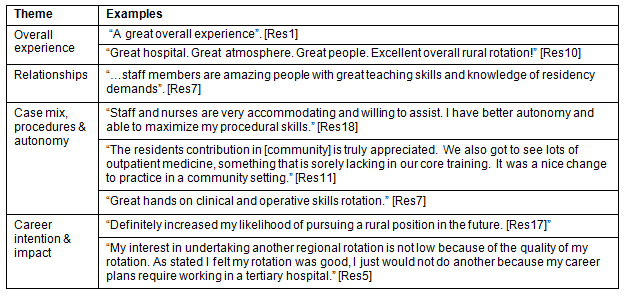
The analysis of the qualitative comments provides insight into these positive quantitative results. Qualitative analysis of the free text comments revealed four major themes (Table 3). There was a strong positive sentiment for the overall experience followed closely by the collegiality in relationships with medical and hospital staff.
Very collegial atmosphere. Excellent staff. [Res16]
The opportunity to perform procedures, the variety of the case mix and the autonomy of the learner were stressed as well.
The residents contribution in [community] is truly appreciated. We also got to see lots of outpatient medicine, something that is sorely lacking in our core training. It was a nice change to practice in a community setting. [Res11]
Different from [main site] with respect to case mix. As well, most staff were not trained in [the main site] so they often have a different approach. [Res2]
Table 3: Qualitative themes
Discussion
In contradistinction to Pong, we found significant value in the rural specialty rotation and no educational limitations from the perspective of the learner13. Specifically, the case mix of the patient presentations and autonomy were valued while the importance of relationships was also highlighted. This study has found a strong positive response from residents being satisfied or very satisfied with their regional educational experience; all residents replied that they would recommend their training site to another resident. A majority of residents indicated that they would be interested in undertaking another regional rotation. Residents completing regional rotations live and work in the regional communities and get to witness first hand the scope of work that regional specialists undertake. The type of resident-preceptor interaction that is experienced in the smaller regional hospitals provides residents with a type of relationship that is not always possible in the larger urban tertiary centres. Vygotsky, in social development theory, stressed social interactions and the role of the 'more knowledgeable other'16. In addition, in social learning theory it is possible that relationships with valued colleagues are a more critical factor in potential recruitment than previously thought.
This was a short survey of a small number of residents at one medical school. Although the response rate is reasonable, these numbers do not allow for a more granular interpretation of the results. It is therefore more prudent to view them as a total resident aggregate and as an early indication of the value of these rural rotations. It provides some direction as to why the rural rotation may be valued by the resident and why the rural rotation may have an impact on eventual practice location.
There are many factors that contribute to a physician's decision on practice location; however, the physician's experience during postgraduate training may factor heavily into that decision. In this study, there was a significant attitudinal shift in residents who stated that following their regional rotation they would be more likely to practise in a regional community. A longitudinal study of a larger group of specialty residents participating in rural rotations would be of interest both to confirm these findings and to assess the duration of the change in attitude.
While there is a recognized shortage of family physicians in most small rural communities, there is an equally critical shortage of specialists to service rural and regional hospitals. Specialty-based, rural distributed programmes are crucial in helping to expose residents to rural practice and therefore to potentially shift resident attitudes to practising in rural and regional areas. The impact of relationships may be a larger factor than previously considered.
Acknowledgement
The authors thank Dr Aliyah Kassam who reviewed the manuscript.
References
1. Pong RW, Pitblado J. Geographic distribution of physicians in Canada: beyond how many and where. Canadian Institute for Health Information, 2005. Available: https://secure.cihi.ca/estore/productSeries.htm?pc=PCC307 (Accessed 24 December 2011).
2. Krupa LK, Chan BTB. Canadian rural family medicine training programs: growth and variation in recruitment. Canadian Family Physician 2005; 51(6): 853.
3. Bates J, Frost H, Schrewe B, Jamieson J, Ellaway R. Distributed education and distance learning in postgraduate medical education. Members of the FMEC PG consortium, 2011. Available: http://www.afmc.ca/pdf/fmec/12_Bates_Distributed%20Education.pdf (Accessed 8 December 2011).
4. Lu DJ, Hakes J, Bai M, Tolhurst H, Dickinson JA. Rural intentions: factors affecting the career choices of family medicine graduates. Canadian Family Physician 2008; 54(7): 1016-1017.
5. Pong RW, Chan BT, Crichton T, Goertzen J, McCready W, RourkeJ. Big cities and bright lights: rural- and northern-trained physicians in urban practice. Canadian Journal of Rural Medicine 2007; 12(3): 153-160.
6. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R et al. Rural background and clinical rural rotations during medical training: effect on practice location. Canadian Medical Association Journal 1999; 160(8): 1159-1163.
7. Geske JA, Hartman T, Goodman B, Paulman P. Influence of a rural family medicine rotation on residency selection: MS3 verses MS4. Family Medicine 2011; 43(8): 556-559.
8. Rourke JT. A rural and regional community multi-specialty residency training network developed by the University of Western Ontario. Teaching and Learning in Medicine 2005; 17(4): 376-381.
9. Hogenbirk JC, Mian O, Pong RW. Postgraduate specialty training in northeastern Ontario and subsequent practice location. Rural and Remote Health 11(2): 1603. (Online) 2011. Available: www.rrh.org.au (Accessed 24 October 2012).
10. DeWitt DE, Migeon M, LeBlond R, Carline JD, Francis L, Irvby D. Insights from outstanding rural internal medicine residency rotations at University of Washington. Academic Medicine 2001; 76(3): 273-281.
11. Kairys S, Newell P. A rural primary care pediatric residency program. Journal of Medical Education 1985; 60(10): 786-792.
12. Jensen C, DeWitt D. The reported value of rural internal medicine residency electives and factors that influence rural career choice. Journal of Rural Health 2002; 18(1): 25-30.
13. Pong RW, Heng D. The link between rural medical education and rural medical practice location: literature review and synthesis. Sudbury, Ontario: Center for Rural and Northern Health Research, Laurentian University, 2005. Available: http://ruralontarioinstitute.ca/file.aspx?id=1b9b7a34-d7f2-4c6f-a1ee-0509a983611c (Accessed 8 December 2011).
14. Government of Alberta, Office of Municipal Affairs. 2010 official population list (as of 1 September 2010) (Online). Available from: http://www.municipalaffairs.alberta.ca/documents/msb/2010pop.pdf (Accessed 12 December 2011).
15. Elliott AC, Woodward WA. Statistical analysis quick reference guidebook: with SPSS examples. Sage Publications, 2006, 131-135.
16. Learning-Theories.com Knowledgebase and Webliography. Social development theory (Vygotsky) (Online). Available: http://www.learning-theories.com/vygotskys-social-learning-theory.html (Accessed 10 May 2012).

