The aging of the Canadian population, particularly in rural areas1, and the increasing migration to urban areas of younger people means the proportion of rural persons with dementia (PWD) will be increasing2. Care partners (informal caregivers) of PWD have reported the need for guidance related to the disease process, available support resources, and how to deal with difficult behaviours3,4, as well as the need for a 'coach and advocate' to help them navigate the healthcare system5. While healthcare practitioners (HCPs) are expected to take an active role in ensuring that PWD and their care partners are equipped with the knowledge they need to provide safe and quality dementia care, HCPs recognize that they often lack this knowledge6,7.
Research questions
The overall purpose of this research was to enable HCPs, care partners, and PWD to use dementia care information more effectively by examining their information needs, how these change over time, and how they access, assess, and apply the knowledge. Our specific research questions were:
- What are the stages of the dementia care journey and the types of information needed by rural community-based HCPs, care partners, and PWD at each stage?
- Where is this information accessed, how is it assessed, and how is it applied by rural HCPs, care partners, and PWD at different stages of the dementia care journey?
- What are the barriers and facilitators to knowledge exchange between and among rural community-based HCPs, care partners, and PWD?
Sample
The inclusion criteria were that participants were: (i) English speaking; (ii) lived in a rural area; and (iii) had presented with symptoms of dementia, or were providing formal or informal care or support to a PWD. Based on Statistics Canada's categorization, 'rural' was defined as living outside a major urban centre of more than 10 000 population8. Not surprisingly, participating PWD and their care partners identified as living in a rural area because Middlesex county is characterized in its own publications as 'farms and small towns surrounding London'9. A convenience sample of rural participants was recruited through the study collaborators: Alzheimer Society of London Middlesex county, Oneida Nation of the Thames, South West Community Care Access Centre (CCAC), and the local Victorian Order of Nurses (VON) in Southwestern Ontario, Canada. Purposive sampling followed to ensure that diverse perspectives, such as amount and types of services received, were included. Interested clients, their care partners, and the community-based HCPs assigned to these clients were contacted by the research assistant and invited to participate in the study and to provide written, informed consent.
Persons with dementia, their care partners, and their community-based HCPs were considered to be a dementia care network. Nine dementia care networks consisting of PWD (n=5), care partners (n=14), and HCPs (n=14) were included (Table 1). Only five of the nine PWD from these networks were willing and/or capable of participating in the study. All PWD were diagnosed with Alzheimer disease. Most PWD (n=4) had lived with dementia for less than 5 years, and one for more than 5 years. The networks each included one to three care partners. The care partners enrolled in the study included six spouses, five children, two grandchildren, and one nephew. Ten of the care partners had provided care for five or more years, and the remainder (n=4) for less than 5 years. The HCPs in the study included three case managers, one personal support worker, two social workers, three physicians, three VON coordinators, one nursing home administrator, and one volunteer. The composition of the nine networks and the services used by each network are provided (Table 1). Additional participant socio-demographic information is also provided (Table 2).
Table 1: Composition of networks and services used
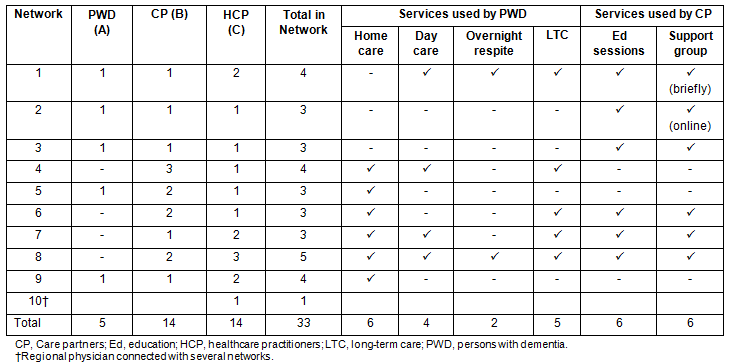
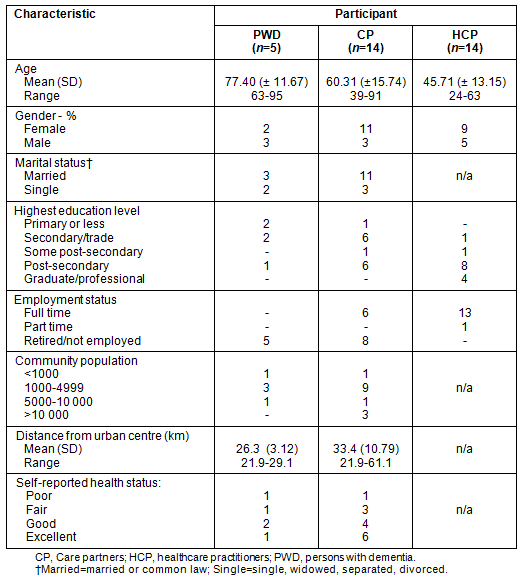
Table 2: Socio-demographic characteristics of participants
Procedure
A qualitative interpretive descriptive approach10,11 was used. Following this approach, themes and patterns within participants' subjective experiences were derived to inform understanding of knowledge exchange among rural HCPs, care partners, and PWD. Interview guiding questions were developed based on the research questions, and data were collected at three time points: (i) entry to the study (n=33); (ii) at 6 months (n=29); and (iii) at one year (n=18) until theoretical saturation was reached, that is until no new properties of categories emerged during data collection12. Eighty face-to-face interviews were audio-recorded and transcribed verbatim and memos and field notes were also captured. The qualitative software program NVivo9 (www.qsrinternational.com) was used to store, record the coding, and organize the interview data. Data collection and analysis occurred simultaneously.
Data analysis
Transcripts were coded using Lubrosky's thematic analysis13. Main ideas and topics that had the most meaning to participants were identified by the authors and coded using key phrases that emerged from the data. The codes were grouped into themes (a higher conceptual level) and sub-themes. By comparing and contrasting the coded data, sub-themes, themes, interrelationships and patterns were revealed. To ensure rigor, each member of the research team independently conducted the primary coding analysis. These preliminary conceptualizations were shared with the team for development and refinement of the themes and patterns, to ensure that the conceptualizations reflected the data presented by the study participants and to encourage the emergence of multiple perspectives around the interpretation of data. On a monthly basis all members of the research team met to discuss, compare, and refine the themes. Memoing and diagramming were also used to reflect on and understand the relationships among emerging categories14.
Qualitative rigor
To promote trustworthiness of the findings the following criteria were adhered to: (i) credibility; (ii) dependability; (iii) confirmability; and (iv) transferability15. Credibility included member checking and peer debriefing. Dependability was established through the use of triangulation of data collection approaches (eg interviews, observations over time). Confirmability was achieved through the monthly analysis discussions that ensured the researchers' conclusions were well grounded in data16. Transferability through 'thick description' of the findings enables the reader to determine whether the concepts are similar enough to transfer to other contexts or times15.
Ethics approval
Ethics approval was obtained prior to commencing the study from the Ethics Review Board, the University of Western Ontario (approval number 16979E) and Victorian Order of Nurses (VON) Canada (approval number 070810-01).
Q1: What are the stages of the dementia care journey and the types of information needed by rural community-based healthcare practitioners, care partners, and persons with dementia at each stage?
Longitudinal data revealed changing information needs during the long, gradual deterioration of the PWD as the symptoms of dementia progressed. The stages of the dementia care journey involved a series of critical decision points related to: (i) recognizing the symptoms; (ii) receiving a diagnosis; (iii) loss of independence; (iv) initiating and using home care and respite services; (v) long-term care (LTC) placement; and (vi) decisions related to end-of-life care. Each dementia care journey was an individualized experience, with overlapping stages, and not always linear in process.
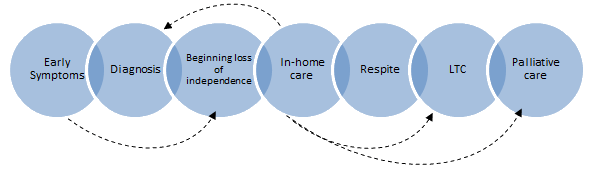
Figure 1: Dementia care journey: stages of knowledge exchange.
Recognizing the symptoms: Symptoms of dementia were first recognized by care partners. These led them to believe there was an underlying pathological process at work that included marked changes in behaviour and personality, misplacing objects, and forgetting or incorrectly remembering life experiences.
I'm really concerned about him because he's dropping weight. He's not eating. I've been in his house. His house is a mess. He's got guns in the house. He gets angry. (9C3-1, HCP referring to her uncle)
Some PWD denied symptoms, and some care partners dismissed symptoms as due to old age, which placed a strain on the marital relationship.
You just have to always keep on saying that's not the man I married. That's the hardest thing for the first few years until they are diagnosed. When I think back, that was one of the hardest things, 'cuz, well honestly I was ready to walk out of this house. (6B1-1, care partner)
A few care partners were alerted to the pathological nature of these behaviour changes by friends. Some care partners and PWD recognized the symptoms as being dementia-related. At this early stage, PWD and their care partners identified that they needed information about how to recognize early signs and symptoms of dementia, where and when to go for help, and how to manage behavioural changes.
Receiving a diagnosis: All of the participating PWD received a diagnosis of Alzheimer's disease. A diagnosis was helpful because it confirmed for PWD and their families that there were pathological changes occurring, they were not 'crazy', this disease had a name, and there was help available. Persons with dementia and their care partners needed information that would help them manage the symptoms and slow the progression of the disease. Information was frequently exchanged on healthy lifestyles such as eating 'healthy brain foods', keeping physically and mentally active, and available medications. However, not all physicians initially suggested that medication might be a treatment option, and family members had to request this information.
So he didn't give her any medicine, I had to make another appointment for that because I was thinking, after we had our meeting, maybe there's something out there that might slow it down, and put it on hold. (5B2-1, care partner)
Other types of information requested by care partners during this stage included potential safety issues, home care options, or other forms of help and support. Healthcare practitioners attempted to tailor the amount and kind of information to what the PWD and care partner/s could cope with and were interested in knowing at this stage.
Loss of independence: Care partners and HCPs preferred that the transfer of decision-making authority to another family member was completed while the PWD could still participate in this process. However, when this was not possible, guidance and information were often needed on how to ensure that decisions were made for the PWD in his/her best interests and based on the PWD's prior attitudes and interests. All of the participating PWD experienced aspects of decreasing independence that were identified as: (i) deferring to the care partner for care decisions; (ii) losing a driver's licence; and (iii) appointing a trustee or power of attorney (medical and/or financial). The type of information required was mainly support in navigating the healthcare system.
I've spent a lot of time with veteran's affairs; I know I spent at least nine or 10 months getting something called involuntary separation allowance...Boy did I ever have a lot of hoops to jump through on that one. (8B2-1, care partner)
During this stage, care partners requested information on how to have driving competency assessed. This was a stressful discussion between the PWD and care partner because living in a rural area made losing a driver's license particularly difficult when shops and services were accessible only by car. Rural family physicians who often had a long-standing relationship with the PWD, occasionally preferred to refer the PWD to a geriatrician to conduct the assessment and make this difficult decision.
Discussions about finances ranged from ensuring bills were paid to taking complete control of the PWD's finances, in some cases because of concerns about possible financial abuse. Children tended to ask and receive permission from the PWD before starting to handle finances. With spouses, this was less of a formal decision and more often a natural progression that occurred over time.
My mom and my uncle have been managing her finances, because there was some concern around that, where some family members may be taking advantage of that. So they've been managing that for my grandmother. (5B1-1, care partner)
In some instances, PWD participated in making care decisions to limit their independence and then later became irritable about them, not remembering they had helped make the decisions in the first place.
'I (PWD) don't go in your wallet, how do you know how much I have?' I said, 'Mom, you just showed me because you couldn't find your wallet and we found it together, and you looked at it'. (4B3-1, care partner)
Initiating and using home care services: The decision to initiate home care services was typically a major decision for rural care partners. Persons with dementia in six of the nine dementia care networks received home care services, and others were considering when and how to access this service. Because of the progressive nature of dementia, home care needs typically increased over time. The types of information needed by care partners during this stage included: what kinds and amount of services can be provided; how to access the services; what were the eligibility criteria and cost; and, who would be providing the services? Home care personnel also spoke about their information needs.
When I get a new client on I get a diagnosis that just gives me dementia, or this client has Alzheimer's with no follow up, no follow through of any information whatsoever. I go in half the time blind as to what level of dementia they have, form that they have, what stage they're in. (6C1-1, HCP)
A home-care case coordinator who placed personal support workers in rural homes spoke about needing to know what the broad care needs were of the care partner and PWD (eg hours per week required, family's flexibility, aspects of care needed, and PWD's likes, dislikes, routines, and difficult behaviours). Occasionally, the personal support workers knew the PWD or their family members because they resided in the same rural community.
Initiating and using respite programs: Persons with dementia in four of the nine networks attended respite day programs, and care partners in two other networks discussed the possibility of using day programs in the future. Two networks also used overnight respite. Healthcare practitioners and care partners discussed using respite day care programs to ensure that the PWD was in a safe environment and occupied for part of the day, allowing the care partners to have a break. Some PWD had difficulty accepting this care. Persons with dementia complained that there was little to do at these programs, and care partners spoke about the need for more engaging activities.
I pick her up and she would cry and they don't do anything, they sit all day. I kept talking to them and said 'Can't you get her involved? Let her do something. Wash dishes'. I keep telling her, 'You're going there to help, they need your help'. That's the type she was, you know, she would help anybody. (7B1-1, care partner)
A limitation to the respite programs was that transportation services were not available, except in one facility, because the distances between residents and the day programs were too great.
Long-term care facility placement: The longitudinal data clearly revealed over time the approaches used by the care partners to prolong keeping the PWD at home and how conflicted they felt about placing them in LTC. Care partners experienced feelings of guilt but recognized that it was the only way to ensure their family member's safety and wellbeing.
Well we sort of had a plan, if mom [PWD] was not going to be able to go to the washroom on her own anymore then it would be mandatory...as long as she's still toddling around to the washroom taking care of herself, that would be our straw. (4B3-1, care partner)
Care partners experienced a lot of anxiety regarding whether placement would happen too soon or not soon enough.
As time passed by they said you better get him on the list, so we said okay put him on the list, and we understand that when a vacancy comes up depending on the priority that you have given him, we understand we've got to make a decision right away. And basically that's what happened. We were getting by at home when the case worker said we have a vacancy and you've got 36 hours or something to decide whether you want to take it or not. (8B2-1, care partner)
Care partners typically needed some time to get used to the idea of LTC placement prior to seeking information in a practical sense. The desire to keep the PWD as close to home as possible due to the long travel distances in part governed their choices for LTC facilities. If the PWD knew someone, either a resident from their community or a HCP working at the facility, this also influenced their choice.
Community-based HCPs would discharge the PWD on admission to a LTC facility. The care partners reported that they missed this connection and would have appreciated some information and support in adjusting to this transition. By the end of the study, five of the nine PWD were living in a LTC facility.
End-of-life care: Healthcare practitioners spoke about the importance of discussing end-of-life care with care partners to let them know what to expect and their options for treatment and support. However, it was often a conversation that was delayed or avoided. One HCP identified the need to approach this topic with a great deal of sensitivity.
I think they would still benefit from some hospice and palliative care information...The only reason why I sort of hesitate is because you know sometimes you mention any sort of hospice or palliative care comment and families immediately seem to reserve themselves because of the issue surrounding death and expecting death and that's not something that is very easy to talk about. (7C1-1, HCP)
Family members also often avoided the conversation. However, in a couple of cases, family members were grateful that palliative care had been discussed with them, that they now knew what to expect and were more prepared for the future. Two PWD died during the study.
First they [mother and PWD] made the decision to keep him alive no matter what, whether it requires resuscitating machine or whatever, we want him kept alive so we can be together right until the very last moment. But then we [adult children] were trying to explain to them, but the very last moment is not going to be enjoyable by either of you, especially by the patient. After discussing pain and that, well, okay then, we will take him from that top level down to the middle level. So then mom went down and she told the nurse I've changed my mind, we're going to have him at this level. So that was explained well...Mom usually says, 'I don't want to talk about it'. Or 'We'll cross that bridge when it comes'. (8B2-2, care partner)
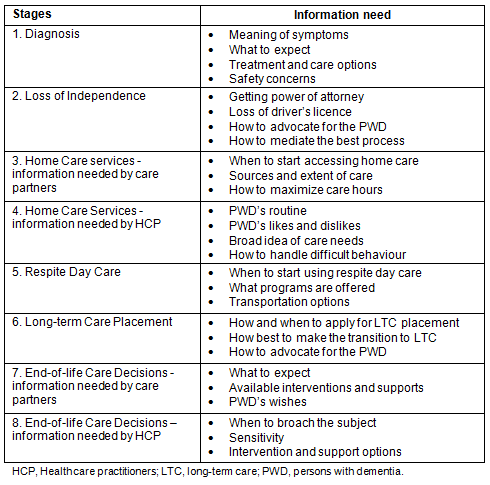
A summary of the stages of the dementia care journey and the information needed at each stage is provided (Table 3).
Table 3: Information needed at stages of the dementia care journey
Q2: Where is dementia care information accessed, how is it assessed, and how is it applied?
During the Recognizing the symptoms stage, care partners approached other family members and friends for advice and/or relied on previous personal experiences. Some care partners sought information on the internet. When HCPs became aware of initial symptoms in their clients, they occasionally performed cognitive screening assessments and, depending on the scores, made referrals to the family physician. Physicians were the primary source of information at the Receiving a diagnosis stage.
The people that have insight will be asking questions such as, 'Can I learn more about this? Can my family members learn more about this? Is there treatment offered? What can be done about this? Can it be reversed? Can it be slowed? Can it, you know, I want to make sure that it's not going to progress, I don't want to end up in a nursing home'. (10C1-1, HCP)
Persons with dementia also looked to family members for information and emotional support. Other PWD and their care partners expressed that they did not want to discuss the problem or look too far into the future.
At the Loss of independence stage, care partners accessed physicians or other HCPs to implement a medical power of attorney or assess driving competency, while bank employees were accessed for information about financial power of attorney. Friends who had been through similar decision-making processes were also sources of information.
Care partners reported that they accessed information regarding home care, respite programs, and LTC facility placement from family members who were HCPs, family physicians, CCAC, Alzheimer's Society staff, VON, health centers, support groups, and internet sites, including chat rooms. They would sometimes visit LTC facilities to observe and seek additional information. End-of-life decisions were made by discussing options with family members and with the PWD's physician.
Healthcare practitioners used the resources provided by their own organization, and additional information was accessed on the internet. Persons with dementia tended not to access dementia care information. Care partners and HCPs assessed the trustworthiness of the information received by whether the person providing the information was trusted or the agency producing the material was well established. In only one instance did a care partner make reference to trusting 'well-researched' information.
Q3: What are the barriers and facilitators to knowledge exchange?
Barriers to knowledge exchange: Lack of adequate rural community-based services and supports Healthcare practitioners frequently discussed not having enough time and the need to increase the length of time between client visits. As a result of being short-staffed and having inadequate funding, HCPs tended to provide more on-demand care focused on managing crisis situations, versus focusing on more 'stable' clients and their care partners. Large case loads and longer travel time meant they did not have time for routine follow up with PWD and their care partners. The HCPs travelled an average of 303 km per week.
You ask about how I prioritize...I maybe meet with a little elderly couple and they're fairly isolated, they don't have any children or supports in town. It would be good for them to come to something but how are they going to get there? I might take a more active role, following up with them, maybe helping them get registered for the transportation program. And encourage our intake gal to phone every time there's a meeting. Whereas, some people I would just hand them the schedule and expect that they will sort themselves out and they'll come to the meetings according to the schedule...This is sad really, but I try to do the minimum that I feel we can possibly do because...I don't have time to do any more than the minimum. And that is going to get much worse quite soon. And it's not ideal. It's not how I would choose to do things. (2C1-2, HCP)
Working in isolation from other healthcare practitioners and organizations At times, HCPs, such as personal support workers and physicians, had limited contact with other practitioners, even within their own organization. For example, a personal support worker discussed being very familiar with PWD and care partners because she saw these clients daily or weekly, yet had little opportunity to participate in case conferences and inform other HCPs about her clients.
Healthcare organizations performing similar roles and providing care to the same PWD and their care partners did not have formal links with each other that would enable the exchange of needed information on the client's change in health status, treatments, and care. One HCP spoke specifically about how she felt there needed to be government and organizational-level policy changes regarding communication between healthcare organizations:
We're all vying for a pot of money to make our own programs all work better and in the end, it's such a haze...'Take down all your silos, quit working in your own little box, and partner together', the benefit would be huge for clients and caregivers and our health tax dollar would stretch tenfold. (4C1-1, HCP)
Reluctance to seek assistance Many care partners were reluctant to seek assistance from formal and informal sources with their care responsibilities for the following reasons: not wanting to impose, valuing their independence, wanting to save resources until they were needed, and not wanting to disclose the diagnosis and need for help due to the stigma associated with dementia in their rural community. The wife of a PWD stated, 'I almost feel like people avoid him now, because you know they know' (1B1-1). Some care partners explicitly expressed that they were not interested in knowing about dementia care.
Limited energy Care partners who were approaching or experiencing physical and/or emotional burnout were not as likely to seek out information in their free time (eg by attending a support group).
I was going to the meetings [support groups] and then I stopped. I said to her [HCP], 'You know, I just feel like I'm Alzheimered to death'. It's all we talked about. That's all I hear about and I'm tired of it. You know I don't wanna have my day out talking about Alzheimer's. (1B1-2, care partner)
Denial Persons with dementia often denied that their symptoms were serious enough to be a concern or indicative of having dementia. Referring to his poor memory, one PWD stated, 'I feel it's a lot better than it had ever been' (1A1-1).
Facilitators of knowledge exchange: Collaborating with team members Healthcare practitioners who worked within a team were better able to discuss and decide collaboratively on needed care and services. Having good working relationships with HCPs in other organizations allowed for a more efficient and effective referral system, and helped ensure clients received the care they needed. Healthcare organizations that maintained formal ties were more aware of available programs, again helping to ensure proper referrals.
Whatever we feel we need assistance with, we'll approach whatever community organization is available that might have the educational information. (7C2-1, HCP)
Active help seeking Many of the rural care partners who were coping well and knew their community members proactively sought out the information and resources they needed by doing their own searching (eg on the internet) or contacting HCPs, friends, or family for dementia and resource information. Because they were actively seeking support, they tended to have more contact with HCPs.
The VON. I asked for help with the daycare. I asked for help for a volunteer visitor. (7B1-2, care partner)
Expertise
Care partners who were HCPs were more likely to have a basic understanding of dementia and/or the healthcare system and could access information more efficiently by building on what they already knew. Having a friend or family member who was a HCP enabled knowledge exchange as they served as a direct or indirect source of information about care and resources.
Trusting relationships A trusting relationship among the HCP, care partner, and PWD was important given the increasing need for care partners to be proactive in seeking information and care resources.
If you have a comfortable relationship with them, you're more apt to discuss things openly in the class [support group]. If you don't feel you can trust them or something, you're more apt to just sit there and listen and not interact. (2B1-3, care partner)
It was important to appreciate the challenges experienced by care partners and PWD, and to be willing to strategize and support them through their day-to-day difficulties rather than seeking solutions. As one HCP explained:
I think focusing on ways to ease the day-to-day journey is more effective and more helpful.These people are committed to care giving or else their loved one would've been in a home months ago and so if they're committed to care giving, let's help them, let's take them by the hand and walk with them and stand beside them and help them do what they really want to do, but it is so hard to do. (2C1-1, HCP)
Discussion
This research reveals the stages of the rural dementia care journey and the nature of the types of information needed at each stage. Furthermore, this research shows the range of sources that rural care partners and HCPs accessed to gain the dementia care information they needed. Not surprisingly, their most trusted sources were approached first. Care partners tended to seek out family members and friends. In addition, care partners and HCPs accessed information from local organizations and dementia care internet sites. All participants tended to rely on others to assess the reliability and validity of the primary source of evidence. While this may be an acceptable approach to assessing critical information, it indicates there is opportunity to promote more dynamic knowledge exchange processes.
Persons with dementia tended not to seek out information or services because of denial of their symptoms, leaving care partners potentially isolated in navigating this journey. This was a concerning finding and illustrates the importance of screening and early diagnosis so that PWD can receive appropriate treatments and supports, and that their wishes and plans for the future can be discussed and acted on. Further research is needed to determine how best to inform and support PWD throughout their dementia care journey.
The long travel distances and identified lack of funding for rural community-based services has led to a shortage of HCPs, resulting in inadequate time for case managers and other HCPs to visit 'stable' clients regularly and to develop trusting relationships. The infrequent visits could have devastating consequences for PWD and their care partners who had little motivation, energy, and possibly limited capability to actively seek out needed information and supportive services. Only by collaborating with care partners, PWD, and their involved HCPs on the plan of care and treatment is the provision of quality and safe dementia care possible. Rural community-based HCPs are ideally situated to promote collaboration and assist families in navigating the typical dementia care stages by providing them with anticipatory information and guidance throughout the journey4,5.
The study findings illustrate several barriers to exchanging dementia care knowledge between and among rural community-based HCPs, care partners, and PWD. The finding that inadequate community-based services and supports impede knowledge exchange among PWD and HCPs is well documented in the literature17-21. Adequate resources and forms of information are especially needed to heighten awareness of early signs and decrease the stigma of dementia so that a diagnosis is received and care plan is implemented in a timely manner. This finding is also highlighted in the 2012 WHO report titled 'Dementia: a public health priority' which recommends awareness-raising campaigns to decrease the stigma that contributes to social isolation and to delays in seeking a diagnosis and help22. Increased resources are also needed to ensure that rural community-based HCPs are proactively connecting with PWD and their care partners on a regular basis to provide the best available information to make informed decisions at each stage of their dementia care journey and to build trusting relationships. Rationing the number of supportive services provided and amount of information exchanged can contribute to increased use of more costly services, such as emergency rooms to sustain caregiving23.
Lack of resources limits the availability of rural community-based services and hinders proactive approaches to exchange dementia care knowledge. This barrier is compounded by the stigma attached to dementia, especially in small rural communities, and the tradition of independence among rural residents, both of which can discourage help seeking to the detriment of care partners and PWD19,24. Clients who were assessed as 'stable' and who had a care partner who appeared to be managing with their dementia care, were expected by the community-based HCP to find information on their own and to seek help when needed. However, several care partners revealed that they did not have the energy or wish to use the few hours they had to themselves to seek out information on dementia care, representing a disconnection between how they were perceived by HCPs and the reality of their caregiving experience.
Limitations
All participants were linked with at least one of the collaborating partners. Thus, the researchers did not include PWD and their care partners who were receiving no formal healthcare services. This is a limitation of the study because their experiences may differ from those experienced by the included participants.
This research makes an important contribution to knowledge exchange by illustrating the types of information typically needed, accessed, assessed, and applied at different stages of the rural dementia care journey. Rural community-based HCPs must be proactive in offering dementia care information because care partners often do not have the time, energy, skills, or knowledge to seek this out. The research reveals the importance of building trusting relationships through a caring, consistent approach that focuses on overcoming the daily challenges. Additional rural community-based resources are urgently needed to ensure that HCPs are able to adequately monitor, support, and provide the information needed by PWD and their care partners throughout their dementia care journey. This may require a redistribution of resources from acute care to rural community care that will result in a more equitable distribution of funds within an integrated health system25.
Acknowledgements
Funding for this study titled Developing Quality Dementia Care Decisions Through Knowledge Exchange in Rural Settings was gratefully received from the Alzheimer Society of Canada, in partnership with the Canadian Nurses Foundation, and the Canadian Institutes of Health Research - Institute of Aging.
References
1. Statistics Canada. Portrait of Seniors in Canada: Chapter 6. Aboriginal Seniors in Canada 2006. (Online) 2010. Available: http://www.statcan.gc.ca/pub/89-519-x/2006001/4122091-eng.htm (Accessed 1 November 2012).
2. Alzheimer Society of Canada. The Rising Tide: The Impact of Dementia on Canadian Society: Executive Summary. Toronto, ON: Alzheimer Society of Canada, 2010.
3. Forbes D, Markle-Reid M, Hawranik P, Peacock S, Kingston D, Morgan D, et al. Availability and acceptability of Canadian home and community-based services: perspectives of family caregivers of persons with dementia. Home Health Care Services Quarterly 2008; 27(2): 75-99.
4. Forbes DA, Neufeld A. Invited article: Discourse: Looming dementia care crisis: Canada needs an integrated theory of continuing care now! Canadian Journal of Nursing Research 2008; 4(1): 9-16.
5. Neufeld A, Kushner KE, Rempel G. Men negotiating the maze of care for a relative with dementia. In: Proceedings, Canadian Association on Gerontology, 36th Annual Scientific and Educational Conference; 1-3 November 2007; Calgary, AB. Canadian Association on Gerontology, 2007.
6. Forbes DA, Ward-Griffin C, Kloseck M, Mendelsohn M, St-Amant O, DeForge R et al. "My world gets smaller and smaller with nothing to look forward to": dimensions of social inclusion and exclusion among rural dementia care networks. Online Journal of Rural Nursing and Health Care 2011; 11: 27-42.
7. Jansen L, Forbes D, Markle-Reid M, Hawranik P, Kingston D, Peacock S et al. Formal service practitioners' perceptions of in-home care: informing dementia service quality. Home Health Care Services Quarterly 2009; 28(1): 1-23.
8. du Plessis V, Beshiri R, Bollman RD. Rural and Small Town Canada Analysis Bulletin Catalogue no. 21-006-XIE Vol. 3, No.3 (November 2001); Statistics Canada Catalogue no. 21-006-XIE. Ottawa, ON: Statistics Canada, 2001.
9. Ontario Ministry of Agriculture, Food, and Rural Affairs (OMAFRA). Middlesex County Rural Guide 2012. (Online) 2012. Available: www.middlesex.ca/living-here/rural-organization-guide (Accessed 1 November 2012).
10. Thorne S, Reimer Kirkham S, MacDonald-Emes J. Focus on qualitative methods interpretive description: a noncategorical qualitative alternative for developing nursing knowledge. Research in Nursing and Health 1997; 20(2): 168-177.
11. Thorne S, Reimer Kirkham S, O'Flynn-Magee K. The analytic challenge in interpretive description. International Journal of Qualitative Methods 2004; 3(1): 1-21.
12. Charmaz K. Constructing Grounded Theory: A practical guide through qualitative analysis. Thousand Oaks, CA: Sage, 2009.
13. Luborsky M. The identification and analysis of themes and patterns. In: J Gubium, A Sanker (Eds). Qualitative Methods in Aging Research. Thousand Oaks: Sage, 1994; 189-210.
14. Schreiber RS. The "how to" of grounded theory: avoiding the pitfalls. In: RS Schreiber, PN Stern (Eds). Using Grounded Theory in Nursing. New York: Springer, 2001; 55-83.
15. Lincoln YS, Guba EG. Naturalistic Inquiry. Newbury Park, CA: Sage, 1985.
16. Sandelowski M. The problems of rigor in qualitative research. Advances in Nursing Science 1986; 8(3): 27-37.
17. Fraser K, Estabrooks C. What factors influence case managers' resource allocation decisions? A systematic review of the literature. Medical Decision Making 2008; 28(3): 394-410.
18. Alcock D, Angus D, Diem E, Gallagher E, Medves J. Home care or long-term care facility: factors that influence the decision. Home Health Care Services Quarterly 2002; 21(2): 35-48.
19. Forbes D, Jansen L, Markle-Reid M, Hawranik P, Morgan D, Henderson S et al. Canadians with dementia: Gender differences in use and availability of home- and community-based health services. Canadian Journal of Nursing Research 2008; 40(1): 38-59.
20. Sims-Gould J, Martin-Matthews A. We share the care: Family caregivers' experiences of their older relative receiving home support services. Health & Social Care in the Community 2010; 18(4): 415-423.
21. Stajduhar KI, Funk LM, Roberts D, MacLeod B, Cloutier-Fisher D, Wilkinson C et al. Home care nurses' decisions about the need for and amount of service at the end of life. Journal of Advanced Nursing 2011; 67(2): 276-286.
22. World Health Organization. Dementia: a public health priority. Geneva: WHO, 2012.
23. Forbes D, Montague P, Gibson M, Hirdes J, Clarke K. Social support deficiency in home care clients. Perspectives: Journal of the Gerontological Nursing Association 2011; 34: 5-17.
24. Sims-Gould J, Martin-Matthews A. Distance, privacy and independence: rural home care. In: N Keating (Ed). Rural Aging: A Good Place to Grow Old? Bristol, UK: The Policy Press, 2008; 43-51.
25. Suter E, Oelke ND, Adair CE, Armitage GD. Ten key principles for successful health integration. Healthcare Quarterly 2009; 13: 16-23.







