Asthma continues to be a major health concern in Canada1. As with many health indicators and outcomes, Aboriginal peoples experience greater disparities in respiratory health compared with non-Aboriginal Canadians2,3. Although asthma data for First Nations and Inuit communities are limited, recent sources suggest that the prevalence of asthma in Aboriginal children and youth ranges from 12% to 14% (on and off reserve)3-5, representing childhood asthma rates that are approximately 40% higher in First Nations and Inuit communities than in the general Canadian population. First Nations children are also twice as likely as their non-Aboriginal counterparts to be diagnosed with asthma5. In the face of such high prevalence rates, the importance of providing relevant educational materials to individuals, families and communities in order to manage and control asthma cannot be overstated6. The purpose of this study is to assess the cultural relevance of existing asthma education materials for First Nations and Inuit peoples. Five First Nations and Inuit communities from across Canada participated in the project.
The risks associated with the determinants of respiratory illness among First Nations and Inuit communities result from complex factors due to lack of resources, including under resourced housing (eg indoor air quality, cooking practices) and health education/promotion (eg smoke ceremonies, tobacco smoking)7-10. There are multiple barriers for Aboriginal communities seeking asthma information resources, including lack of resources, limited access to healthcare services, and social and cultural stigmas associated with seeking medical help11. Information in culturally relevant educational materials tends to be retained longer and is more likely to lead to health-related behavior change11,12. Yet theories designed to increase cultural relevance have been criticized for failing to identify how such programs can align with the cultural characteristics of participants13.
To overcome this gap, cultural sensitivity has been used to identify specific implications for tailoring health messages14. In this work, we use cultural respect; in other literature 'cultural sensitivity' is defined as the 'extent to which ethnic or cultural characteristics, experiences, norms, values, behavioral patterns, and beliefs of a target population, and relevant historical, environmental, and social forces are incorporated in the design, delivery and evaluation of targeted health interventions, including behavioral change materials'14. This approach has been used in a number of different (health) contexts, including HIV/AIDS15, asthma16, physical activity17, and drug and alcohol use18. Furthermore, cultural appropriateness of printed educational materials for minority groups has been shown to improve asthma knowledge and control, asthma-related outcomes and quality of life19,20.
In our study, cultural respect refers to characteristics21 such as appropriate language and culturally appropriate contexts22. Research has shown that cultural difference limits the use of health information, which in turn may have an impact on individual understanding of it23. Since cultural practices and behaviors are embedded in the everyday activities of First Nations and Inuit communities, it is essential to understand these practices when evaluating educational materials. In order to investigate the cultural relevance of asthma educational materials, the Asthma Society of Canada conducted a baseline exploratory study of experiences and perceptions of asthma in First Nations and Inuit communities24, which identified the need to develop culturally appropriate educational materials and resources as an integral factor in improving asthma management. Concomitantly, the Asthma Society of Canada evaluated existing asthma education materials and resources to identify how they could be adapted to enhance their relevance to the cultural and health-related needs of First Nation and Inuit communities.
The purpose of this article is to examine these findings in an effort to identify factors that will help guide the development of culturally relevant asthma educational materials for First Nations and Inuit peoples.
This study employed an evaluative methodology to assess existing asthma education materials, which included an evaluation assessment and evaluation study. The evaluation assessment included an environmental scan in order to identify questions, and to develop appropriate methods for gathering data. The evaluation study consisted of data collection and data analysis to determine findings about cultural relevance of existing asthma education materials.
A combination of quantitative evaluations (eg surveys) and qualitative techniques (eg open discussion, live chats) were used to assess printed and web-based asthma education materials. Five First Nations and Inuit communities from across Canada agreed to participate in the project. Participants were selected to represent homogeneous groups based on age and role: 6 to 12 years old (children), 12 and above (youth), parents and grandparents, community leaders and teachers, and community advisory group members. (eg Elders, healthcare providers, nurse practitioners, community health workers). The community advisory group members were key informants from First Nations and Inuit communities, including youth, elders, and community leaders with some knowledge of asthma. Recruitment of the sample target group members was facilitated by community outreach workers who worked directly with each community and used a range of recruitment methods (eg newsletter, flyers, and word of mouth). A number of evaluation techniques were used to select participants: survey questionnaire, live-chat (via webinar sessions), and open discussion forum. The final sample consisted of 68 survey respondents (52% response rate), 56 web-based seminar attendees, and 10 open discussion participants.
Data collection
An initial environmental scan was conducted to acquire printed asthma education materials and web-based resources currently available in English (eg USA, Canada, UK, Australia). The majority of documents, websites, and resources were located through Internet searches, by personal communication, and from key stakeholders such as the Asthma Expert Advisory Forum. Materials and resources were selected based on style, format, content, age appropriateness, and topics, and were categorized according to target groups. A total of 64 educational materials were selected for evaluation. Existing asthma educational materials, web-based materials and resources and asthma education sessions were evaluated through:
- Survey questionnaire
- Live chat (written responses)
- Open discussion forum.
Survey questionnaires: These were developed to evaluate the packages of printed asthma educational materials (Appendix 1). Four different surveys were developed, corresponding to each distinct target group, and an additional questionnaire was designed for teachers. In general, the questionnaires were designed to garner responses on preference and cultural relevance, and to obtain quantitative (five-point scale) and qualitative (written comments) feedback of participants on materials. Qualitative questions were used to identify perspectives on what elements would make educational materials more culturally relevant. Two independent researchers provided feedback and recommendations on administering the questionnaires. Parents assisted their children aged 6 to 12 in completing the survey. The number of materials in each package varied according to the target group. The survey questionnaire (available upon request from the corresponding author) consisted of 44 questions grouped in 6 sections: (i) consent form; (ii) demographics; (iii) asthma-related material; (iv) general questions; (v) personal feedback; and (vi) disclaimer. It was designed to gather quantitative (five-point Likert scale) and qualitative (written comments) feedback on topics such as learning style and format, as well as suggestions for cultural adaptation. Young children (aged 6 to 12) were provided with stickers for ranking (5 stars=excellent).
Live chat via webinar technology: This was used to evaluate web-based support resources and face-to-face asthma education sessions. A certified Asthma/Respiratory Educator delivered all educational sessions, which consisted of a short MS PowerPoint presentation in which participants provided feedback via open discussion through live chat and written responses to poll questions. The online web-based seminar sessions involved evaluating various websites and one e-learning module, during live chat/open discussions. Five sessions were conducted with a total of 56 (First Nations=54; Inuit=2) individuals participating. The webinar session for children (ages 6 to 12) was facilitated by a certified asthma /respiratory educator.
Open-discussion forum: In this forum, 10 advisory group participants (Elders, healthcare providers, family members, and community outreach workers) from four Canadian provinces (Nunavut, Newfoundland, Nova Scotia, Ontario) evaluated the selected asthma education materials, websites and programs. The education materials were divided into three categories: (i) printed asthma educational materials; (ii) asthma educational videos/CDs; and (iii) websites/e-Learning module. The same survey questionnaire (eg five-point rating scale, written comments) was used. The open discussion focused on suggestions for making materials culturally appropriate.
Data analysis
All quantitative survey data was analyzed with SPSS v14 (www.spss.com) using simple descriptive analytic techniques, and qualitative data were thematically analyzed into a coding scheme. Thematic analysis involves the creation and application of 'codes' to the data25,26. In this study, coding of the written comments involved close reading and coding of discrete units of text using a coding system developed using both inductive and deductive approaches; that is, the coding process was informed by the objectives of the research as well as the themes that emerged from the interview data.
The project was approved through a community agreement between the Asthma Society of Canada and each participating community. The agreements specified the joint roles and the main project deliverables. Participants signed consent forms and parents signed proxy assent forms for their children (≤18 years). Participants had the right to withdraw at any time without penalty during this study and also had the right to decline answering questions if she/he wished.
Assessment of printed asthma educational materials and resources
Assessment of printed asthma educational materials and resources is reported according to age and role groupings.
Children - 'fun and interactive': A total of 14 children aged 6 to 12 (n=9 girls; n=5 boys) participated. All children attended school and the majority (84.6%) of children reported having asthma/breathing problems and/or (71.4%) had a sibling with asthma and allergies. Eleven of 13 children learned about asthma from their mother (64.3%) or doctor (57.1%). The majority of children (84.6%) reported they accessed the Internet at least once per week. Most children (71.4%) said they preferred 'playing' when learning, followed by 'reading'.
Children reported they 'liked' or 'really liked' the 12 asthma educational materials they reviewed (73.7%) at the time, but preferred websites (80%), games and puzzles (71.7%), booklets (69.4%) and CD games (61.6%). The three top-rated materials were all websites (88.8%). Websites were viewed as providing 'fun and games' in asthma education. When asked what features they liked most about the websites, activities (eg games and puzzles) was chosen most frequently (64.3%), followed by color/drawings (57.1%), imaging and diagrams (35.7%), personal stories (21.4%) and videos and movies (14.3%).
When asked about the best way to learn about asthma, children indicated picture booklets (85.7%), activities (78.6%) and story booklets (71.4%). Children liked the fun and interactive content (eg pictures, diagrams, tear-out information) of booklets: 'they were fun to look at and read.' Respondents most liked booklet features such as pictures (71.4%) games (64.3%) story characters (57.1%) and colours (50%). One child noted: 'pictures show me where body parts go [lungs] and I didn't know that before.' Half of the participants mentioned that 'more pictures' would improve the booklets. Another child said, 'I would like to learn by looking at a picture guide.'
Most (75%) children noted games and puzzles as fun and reported 'paper game' and 'coloring' as the most fun. The majority of children (85.7%) understood what message the activities were communicating. When asked how to improve the usefulness of the games and puzzles, 'more activities' was chosen most often (42.9%), followed by 'more explanation about asthma and allergies' (28.6%). As for websites and booklets, in general children appreciated the fun and interactive opportunities these materials provided them.
Youth - 'engaging and exciting': A total of 18 youth aged 12 to 18 (10 girls, 8 boys) participated. Most (61.5%) reported they lived in a village or rural settings. The majority of youth (82.4%) attended school and had learned about asthma from their mother (55.6%) or doctor/nurse (44.4%). The majority of youth (85.7%) also reported they accessed the Internet on a daily basis.
In general, youth 'liked' or 'really liked' all 24 samples of educational materials. They preferred booklets (74.1%), CD games (70.6%) and brochures (63.3%). More generic materials such as brochures and action plans were less favored and diaries were unanimously least preferred. Booklets were described as engaging and interactive, and 'pictures' and 'storyline' were the preferred components of booklets. Youth emphasized that booklets helped them learn about asthma and suggested more 'written information' (50%) and more 'pictures and images' (22.2%) as improvements.
Youth preferred a combination of traditional booklets (66.7%) and digital website (50%) educational materials. More than half of respondents preferred visual modes of learning through pictures, diagrams, videos and DVDs, with fewer preferring auditory and text-based content in Native languages. Wish-list items included factsheets (61.1%), CDs/audio (44.4%), games and puzzles (33%), internet (33%) and videos/DVDs (33.3%). Most (70.6%) had never used an asthma action plan; however, 83.3% indicated they would be willing to use one. One youth remarked that, 'it was helpful reading about asthma' and another noted, 'Anyone with asthma should have an emergency asthma care.'
Parents and grandparents - 'informative and culturally appropriate': Twenty-two parents and grandparents completed the questionnaire. Most respondents (59.1%) lived on reserves. The majority of respondents (81%) indicated that children in their care had asthma/breathing problems and/or allergies. Of this group of caregivers, most (57.9%) were mothers, followed by fathers (21.1%), grandmothers (10.5%) and grandfathers (10.5%). Most respondents (76.2%) reported good access to the Internet, with over half (57.1%) using the internet 1 to 3 hours per day.
More than half (70%) of respondents reported having a good understanding of asthma and breathing problems, which they attributed to multiple sources of information, including physicians, nurse practitioners, pharmacists, asthma clinics, friends or the Internet.
Overall, parents and grandparents considered all educational materials (37 items) as good or excellent. However, this group preferred a range of materials, such as booklets (82.5%), websites (82.1%), and checklists/factsheets (80.1%). Asthma diaries were identified as the least favourite (69.7%). Notably, most respondents had no knowledge of asthma action plans, but the majority (95.5%) reported they would use one to improve care of their children.
The majority of participants (91%) indicated that the sample educational materials were culturally relevant or somewhat relevant; however, more than half (54.5%) recommended adding environmental factors common to Aboriginal communities (eg road dust, forest fire smoke) as relevant information to newly developed materials. Respondents reported the inclusion of information on Native remedies and holistic approaches would enhance the relevance of the materials. Finally, 68.2% of parents and grandparents believed the inclusion of spiritual connectedness would better meet cultural needs: 'You should incorporate a spiritual and culturally associated perspective, since Natives have a strong connection to that style of thinking.' Other cited examples of more relevant content included stories of Aboriginal people living with asthma, and information on housing issues (eg mould), as well as using different languages and visual learning formats (eg appropriate coloring, characters, images, and pictures).
The majority of parents and grandparents (77.3%) preferred visual learning (eg pictures/diagrams, internet, video) to reading (text-based information). They emphasized a desire to learn more about asthma triggers (eg pets, exercise, smoking) and environment controls in preference to general asthma information.
Teachers and community leaders - 'references to Aboriginal culture and traditional healing information': Fourteen teachers, healthcare providers, community leaders, educational counselors, outreach workers and program coordinators participated in this group. Half of these respondents had a child with asthma, and 62.5% reported that asthma and breathing problems were important community concerns. Participants identified a range of community barriers including air quality (eg dust, pollution), access to appropriate health care (eg physician, prescriptions), lack of knowledge, and access to education. The majority of respondents (85.7%) reported having internet access.
Overall, this group preferred e-learning (100%), checklists/factsheets (94.1%), booklets (92.3%) and websites (85.6%). When asked to identify the most useful materials for their communities, most respondents (71.4%) preferred more traditional materials such as booklets, followed by checklists/factsheets (57.1%) and information on asthma medications (42.9%). Like other respondent groups, when asked the easiest way to learn and retain new health-related information, this group found visually based learning modes most beneficial (78.6%), with materials available in native languages as a second preference (35.7%). Respondents recommended the addition of 'real-life' characters and pictures related to Aboriginal culture. Most respondents (71.4%) reported the importance of incorporating lifestyle (eg exercise, pets, smoking) and environmental (eg indoor/outdoor triggers) (50%) information in education materials.
More than half (61.5%) of respondents reported that the materials could be adapted to be more culturally relevant by including pictures/photos and content related to the culture (eg providing information on natural remedies), as well as using appropriate indigenous languages so that the materials are 'more understandable for parents and grandparents'. One community health worker noted:
A lot of kids are adopted by a grandparent and their education is very low to none and they often don't speak English ... educational materials need to be in different languages for people who do not speak or read English and French.
The majority of participants (78.6%) acknowledged their willingness to participate in the future development of educational materials.
Assessment of web-based support resources and materials
The overall findings from the online educational sessions indicated that participants enjoyed the interactive component and the immediate feedback from a health professional. Respondents preferred group education, especially children who preferred in-person support and reassurance, and 'someone to tell' them when learning.
Participants focused on content, design, format, and delivery/promotion as 'best practices' for the design of asthma education materials. Participants recommended content using 'real-life' stories and providing information differentiating asthma myths and facts. Participants identified the importance of environmental determinants of health (eg housing conditions, indoor/outdoor air quality, road dust) for First Nations audiences. Their concerns included smoking, childhood asthma, medication use, living conditions, and community awareness. They recommended that content for new materials focus on these concerns, thereby enhancing their relevance for Aboriginal community members.
Our results show that 'eye-catching' design strategies such as bright colors, age-appropriate pictures and characters, games, and cartoons are preferred strategies for sustaining attention. Interactivity was identified as a key program delivery 'best practice', and digital formats (ie websites) were widely accepted in these First Nations and Inuit communities. When asked about format preferences for developing new asthma materials, participants indicated that video/DVD (23.4%), activities for kids (14.8%), and posters, calendars, websites and webinars (8.5%) were preferred.
Delivery strategies that communicate available programs and materials were considered important for increasing community awareness. When participants were asked about webinar sessions, they cited visual interaction and immediate professional support (61.5%), ease of access to health professionals and the type of information (15%) as beneficial. When asked about 'future directions', respondents discussed the benefits of school programs and community-based venues such as 'asthma information nights' as ways of obtaining information and gaining health professional support.
All participants indicated that websites were 'engaging and interactive'. The majority of participants (92%) reported interest in using the e-learning module.
In educational webinars, two-thirds of these young children (66.7%) reported they enjoyed receiving 'a lot of information' and reported that it was 'fun'. Younger children (83%) stated their preference to learn about asthma from parents and by using games and puzzles (50%), posters/calendars (25%), and video/CDs (25%).
The majority of participants in the webinar session for parents, grandparents, community leaders and older children (96%) reported webinar sessions to be engaging and interactive. When asked what they like about webinar sessions, participants responded 'educational' (54%), 'informative' (23%), and 'interactive' (15%). More than half of participants (60%) preferred asthma education delivery by a healthcare professional and the majority (89%) indicated comfort in a group setting. Preferred delivery methods were virtual/audio modules (54%), online education (27%) and in-person education (19%).
The concept of asthma action plans was highly supported by all participants. A range of asthma action plans were ranked, and it was indicated that all plans required cultural adaptation to better suit the needs of First Nation and Inuit peoples. Almost half of participants suggested the addition of pictures/diagrams and culturally relevant information. Although the majority of participants (84%) had never used an asthma action plan, all participants indicated they would be willing to use such plans.
Assessment of asthma educational materials & resources - advisory group meeting
In general, participants (10 advisory group members) reported that asthma is 'something that is kept quiet,' not considered 'a serious condition' and disclosure is seen as problematic:
People who have asthma do not want to say they have asthma because people could be scared of them ... children see taking their medication as not cool.
Respondents reported that asthma was not considered a priority health concern in their communities and education was limited. For example, the majority of respondents had no knowledge about the extent to which asthma is related to broader concerns such as housing. With respect to asthma control and management, a range of community concerns were identified, including potential impact of traditional ceremonies and exposure to second-hand smoke, impact of environmental factors including poor housing (mould, mildew), lack of educational resources, access barriers to health services and to communicating with health professionals, lack of professional-development programs to improve professional expertise in asthma management, lack of healthcare coverage for medications, and lack of awareness at the community level.
Education was reported as key to proper asthma management. The majority of advisory group members noted that increasing public awareness and 'empowering children to make good choices' could be achieved through educating community members. For example, one participant noted: 'early childhood education is where asthma education should begin. It is important to teach [children] about asthma and to show them how to deal with it.'
All advisory group members preferred highly interactive resources that contained more visual content (ie pictures) and less text-based content (ie technical information). In particular, respondents suggested adding content to reflect the everyday living conditions of Aboriginal community members (eg on-reserve living conditions, second-hand smoke) by using Aboriginal art, images and native languages to enhance the cultural relevance of educational materials.
Advisory group members preferred printed materials (52%) (eg booklet, factsheet, posters), personal interaction (26%) (eg support groups, mentor) followed by audio/video (19%). When asked about 'negative' features, most participants identified materials that were 'too busy' with 'too much writing'.
When advisory group members were asked what features to consider when developing new materials they cited simple content, less technical language, balance between text and pictures, relevance to Aboriginal communities, and engaging. In particular, participants recommended content topics such as triggers, stress and its management, smoking, side-effects of asthma medication, and 'how to' information geared to children (ie use of inhalers) and 'real-life' situations that increase relevance to community members. Advisory group members also emphasized interactive and engagement formats to enhance learning and discussed the benefits of different formats to support diverse learning styles. For example, visual formats such as TV commercials, posters and games could be augmented by text-based formats such as an asthma emergency and information card, asthma action plans, and conversation maps (culturally appropriate roadmap game for children containing information about triggers, prevention strategies).
Discussion
The aim of this study is to assess the cultural relevance of existing asthma education materials for First Nations and Inuit peoples. Five First Nations and Inuit communities from across Canada participated in the project. As there were no available printed or web-based asthma education materials specifically targeted for these communities, diverse asthma educational resources were reviewed for this study. Although participants in all age categories liked the selection of asthma educational materials and resources, they also identified adaptations they perceived would create personal and cultural relevance.
Our study revealed that features such as pictures and images relating to First Nation and Inuit culture and real-life stories of people living and coping with asthma were preferred strategies to improve cultural appropriateness. Materials should also be tailored to include Aboriginal languages (ie Inuktitut) and include references to Aboriginal ceremonies and traditions. This finding is consistent with research identifying factors that influence initial interest21. Further, our findings demonstrate that visually based content in both printed and virtual form were preferred styles of learning among older children, parents/grandparents, and community leaders, while younger children preferred learning through play and interactive activities.
These findings indicate the need to develop new asthma educational materials and resources that are specifically tailored to meet the unique needs of First Nations and Inuit community members. Stewart and colleagues27 report that First Nations children and families affected by asthma and allergies face numerous barriers in accessing health care and social support. Our results are consistent, revealing the need for children to 'be taught in a fun way by doing activities' and the need for personal interaction with parents. Our findings emphasize that incorporating real-life stories and experiences of living and coping with asthma could improve cultural relevance and result in health behavior change12. Respondents suggested balancing the amount of text and images, and emphasized decreasing the technical information and increasing the interactive features. In general, young children preferred the interactivity of asthma education sessions delivered via webinars and the added value of receiving immediate feedback from and dialogue with health professionals.
Research has shown that Aboriginal cultures and languages contribute positively to health28. Our findings reinforce the value of understanding cultural beliefs and practices and engaging First Nation and Inuit community members directly. In particular, youth are the population group at highest risk of asthma morbidity and mortality3. These findings emphasize the importance of engaging First Nation and Inuit youth and parents when developing asthma education materials and resources. Engaging children and adults living with asthma is an important way of providing them with a source of collective legitimacy that raises awareness and recognition of their needs in the community21.
The methodology used in the project has several limitations. First, while these findings may contribute to our understanding of how to tailor printed and web-based educational materials to suit First Nations and Inuit community members, its generalizability across all Aboriginal groups may be limited. The small sample of First Nations and Inuit communities is also a limitation. Finally, this is the first project that evaluates the asthma education resources with First Nations and Inuit people in Canada. Although many asthma education materials were evaluated in this study, the findings do not address all asthma educational materials available in Canada.
Asthma is a growing concern in First Nations and Inuit communities2. It is important to reflect cultural needs and preferences when developing asthma education materials and resources29. Findings from this research emphasize the need to develop asthma education materials that are more relevant to First Nation and Inuit cultures and to directly engage community members in the process. Developing new culturally appropriate materials would potentially be more effective in reaching members of First Nation and Inuit communities and could increase the likelihood that members will adopt asthma prevention and management practices. Further research, however, needs to address the complex influence of cultural sensitivity and to design and test culturally appropriate health education resources.
Acknowledgements
The authors acknowledge the project partners the Assembly of First Nations, Inuit Tapiriit Kanatami, and AllerGen-NCE Inc; and that project funding was provided by the First Nations and Inuit Health Branch, Health Canada. The authors thank Sabrina Panetta, Luke Nicholas, Troy Williams, Tara Zupancic, Meridene Haynes, Elizabeth Conti, Zhen Liu, Elizabeth Sergeants, and Ivan Telitsyn for their work on the 'A Shared Voice' project and acknowledge Diana Royce for her helpful comments.
References
1. Garner R, Kohen D. Changes in the prevalence of asthma among Canadian children, Health Reports 2008; 19: 45-50.
2. Crighton EJ, Wilson K, Senecal S. The relationship between social-economic and geographic factors and asthma among Canada's Aboriginal populations. International Journal of Circumpolar Health 2010; 69: 138-150.
3. Garner R, Carrière G, Sanmartin C. The health of Inuit, Métis and First Nations adults living off-reserve in Canada: The impact of socio-economic status on inequalities in health. Cat. No. 82-622-X. No. 004. Ottawa, ON: Statistics Canada, 2010. Available: http://www.statcan.ca (Accessed 3 January 2012).
4. Public Health Agency of Canada. Life and breath: respiratory disease of Canada. Ottawa, ON: PHAC, 2007. Available: http://www.phac-aspc.gc.ca (Accessed 3 January 2012).
5. NAHO First Nations Centre. First Nations Regional Longitudinal Health Survey (RHS) 2002/03. Results for adults, youth and children living in First Nations communities. Ottawa, ON: NAHO, 2005.
6. Donelle, L, Hoffman-Goetz L. An exploratory study of Canadian Aboriginal online health care forums. Health Communication 2008; 23: 270-281.
7. Bashir, SA. Home is where the harm is: inadequate housing as a public health crisis. American Journal of Public Health 2002; 92(5): 733-738.
8. Ritchie AJ, Reading JL. Tobacco smoking status among Aboriginal youth. International Journal of Circumpolar Health 2004; 63: 405-409.
9. Ahluwalia SK, Matsui EC. The indoor environment and its effects on childhood asthma. Current Opinion in Allergy and Clinical Immunology 2011; 11(2): 137-143.
10. Stapleton M, Howard-Thompson A, George C, Hoover RM, Self TH. Smoking and asthma. The Journal of the American Board of Family Medicine 2011; 24(3): 313-322.
11. Kreuter MW, Strecher VJ, Glassman B. One size does not fit all: the case for tailoring print materials. Annals of Behavioural Medicine 1999; 21: 276-283.
12. Kumpfer KL, Alvarado R, Smith P, Bellamy N. Cultural sensitivity and adaptation in family-based prevention interventions. Prevention Science 2002; 3: 241-246.
13. Reese LRE, Vera EM. Culturally relevant prevention: the scientific and practical considerations of community-based programs. Counseling Psychologist 2007; 51: 918-927.
14. Resnicow K, Briathwaite RL, Dilorio C, Grlanz K. Applying theory to culturally diverse and unique populations. In: K Glanz, BK Rimer, FM Lewis (Eds). Health behavior and health education: Theory, research, and practice, 3rd edn. San Francisco, CA: Jossey-Bass, 2002; 485-509.
15. Majumdar B, Chambers T, Roberts J. Community-based, culturally sensitive HIV/AIDS education for Aboriginal adolescents: implications for nursing practice. Journal of Transcultural Nursing 2004; 15(1): 69-73.
16. Eley R, Gorman, D. Didgeridoo playing and singing to support asthma management in Aboriginal Australians. Journal of Rural Health 2010; 26: 100-104.
17. Teufel-Shone NI, Fitzgerald C, Teufel-Shone L, Gamber M. Systematic review of physical activity interventions implemented with American Indian and Alaska Native populations in the United States and Canada. American Journal of Health Promotion 2009; 23(6): S8-S32.
18. Gray D, Saggers S. Introduction. In: D. Gray, S. Saggers (Eds). Indigenous Australian alcohol and other drug issues: research from the National Drug Research Institute. Perth, WA: National Drug Research Institute, Curtin University of Technology, 2002.
19. Brotanek JM, Grimes K, Flores G. Leave no asthmatic child behind: the cultural competency of asthma educational materials. Ethnicity & Disease 2007; 17: 742-748.
20. Bailey EJ, Cates CJ, Kruske SG, Morris PS, Brown N, Chang AB. Culture-specific programs for children and adults from minority groups who have asthma. Cochrane Database Systematic Review 2009; 15(2): CD006580.
21. Yancura LA. Delivering culturally sensitive health messages: the process of adapting brochures for grandparents raising grandchildren in Hawaii. Health Promotion Practice 2010; 11(3): 400-407.
22. Parra-Medina D, Wilcox S, Thompson-Robinson M, Sargent R, Will JC. A replicable process for redesigning ethnically relevant educational materials. Journal of Women's Health 2004; 13: 579-588.
23. Yi YJ, Stvilla B, Mon L. Cultural influences on seeking quality health information: an exploratory study of the Korean community. Tallahassee, FL: School of Library and Information Studies Faculty Publications at DigiNole Commons, 2011.
24. The Asthma Society of Canada. A shared vision: Ensuring quality of life for adults and children with asthma and allergies in First Nations and Inuit communities in Canada. Toronto: ASC, 2009.
25. Charmaz K. Grounded theory in the 21st century: Application for advancing social justice. In: NK Denzin, YS Lincoln (Eds); The Sage handbook of qualitative research (3rd edn. Thousand Oaks, CA: Sage, 2005; 507-535.
26. Charmaz K. Constructing grounded theory: A practical guide through qualitative analysis. Thousand Oaks, CA: Sage, 2006.
27. Stewart M, Masuda JR, Letourneau N, Anderson S, McGhan S. "I want to meet other kids like me:" needs of children with asthma and allergies. Issues in Comprehensive Pediatric Nursing 2011; 34: 62-78.
28. McIvor O, Napoleon A, Dickie KM. Language and culture as protective factors for at-risk communities. Journal of Aboriginal Health 2009; Nov: 6-24.
29. Friedman DB, Hoffman-Goetz L. Assessment of cultural sensitivity of cancer information in ethnic print media. Journal of Health Communication 2007; 11: 425-447.
_______________________
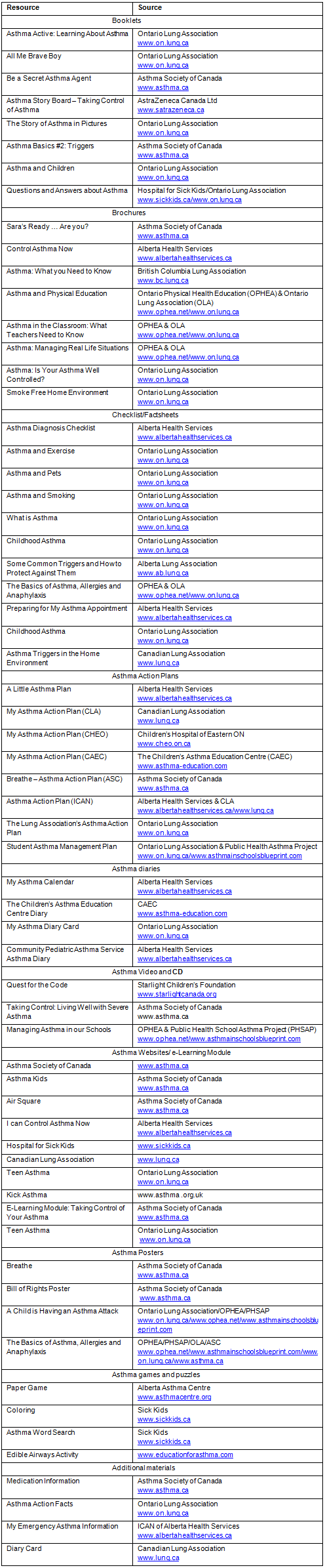
Appendix 1: Selected printed asthma educational materials