Nurses represent the predominant professional healthcare providers worldwide, despite persistent shortages and maldistribution. In the USA nearly two-thirds of all rural healthcare providers are nurses; however, historically chronic nursing shortages plague rural and remote communities nationwide1-4. Skillman, Palazzo, Keepnews, and Hart's research using the 2000 National Sample Survey of Registered Nurses found that the nurse-to-population ratios in urban and large rural areas (by residence) were similar (830 and 794/100 000), but declined significantly in small rural and isolated small rural areas (723 and 719/100 000)5. Rural nurses tend to be older, less educated and earn 14-18% less than their urban colleagues. They are more likely to work full-time and in non-hospital settings than urban nurses5.
As noted in a recent Urban Institute study6, health professionals tend to practice near where they are educated. The location of most US schools of nursing, particularly at the baccalaureate level, in urban areas represents a challenge to meeting the rural nursing workforce needs. The Tri-Council for Nursing, which includes the American Association of Colleges of Nursing, the American Nurses Association, the American Organization of Nurse Executives, and the National League for Nursing, recently noted that 'diminishing the pipeline of future nurses may put the health of many Americans at risk, particularly those from rural and underserved communities, and leave our healthcare delivery system unprepared to meet the demand for essential nursing services'7. According to the National Center for Health Workforce Analysis8, the nursing shortage in the USA has been estimated to reach 27% by 2015 and an alarming 36% by 2020; however, the recent recession resulted in a temporary easing of the nursing shortage9. Nevertheless, according to the United States Registered Nurse Workforce Report Card and Shortage Forecast10, the shortage of registered nurses will return through 2030, with the south and the west (which have some of the highest percentages of rural areas) most affected.
An often-cited strategy, supported by research particularly in medicine, in addressing the shortage of rural healthcare providers is to recruit students who have grown up in rural areas, with the hope that health professionals who were raised in rural communities will be more likely to choose to practice in rural settings. The literature regarding the recruitment and retention of university students in general from rural and remote backgrounds, however, is limited, particularly in the USA. In high school, rural students tend to have lower achievement scores and higher dropout rates compared to non-rural students11. Among lower socioeconomic rural students who enroll in college, predictors of pursuit of higher education include early educational ambition and student involvement in the community and school activities12. Rural farm-raised students are almost as likely to attend college as are rural students raised by professional-managerial parents; however, the paths to obtaining education can be quite different. Farm-raised and lower socioeconomic status students are more likely to identify community support rather than parental influence and support for their decision to enroll in college12.
Several studies in the USA have shown no difference between rural and urban students' academic performance12-15 once they are enrolled in college. Parsons' research among students from rural backgrounds at the University of California, Berkeley, indicated that the differentiation in academic attainment of students comes from personal drive, self-confidence, assertive attitude, commitment to scholarship/goals, support of family/friends, relationships with professors, extracurricular activity participation, and the use of university-provided support services14. To address the unique needs and perspectives of students from rural backgrounds, some undergraduate institutions have instituted specialized rural student recruitment and retention support approaches. Suggested strategies for enhancing the recruitment and retention of rural students include on-campus support services, enhanced faculty accessibility, and guaranteed on-campus housing for rural freshmen14. Some studies also suggest that rural students favor smaller, in-person classes, with a sense of community on-campus16 and may need additional support related to technological competence17. From an international perspective, older research from Wales18 and Australia19,20 suggests that rural students may be academically disadvantaged.
In nursing, research related to students from rural backgrounds is quite limited, with most studies focusing on postgraduate employment. The limited research addressing the educational process with rural nursing students suggests that universities should be sensitive to the unique needs of these students, and be prepared to provide specialized resources for rural students who may need assistance in keeping learning a priority16. Wood compared the outcomes of nursing students in Georgia who attended a rural program with those in an urban program21. Of the total sample (N=136), 54% reported living in rural areas (72% at the rural school and 48% at the urban school) prior to enrollment. A significant relationship (p=0.0000) was found between practicing in a rural area and living in a rural area before school, with 54% of rural background students versus 8% of urban background students choosing rural practice. Similarly, Bushy and Leipert's qualitative results of surveys from 44 graduate and undergraduate nursing students from the USA and Canada who were attending a rural nursing conference indicated that those who have previous rural life experiences and connections are more likely to choose rural practice22.
In Australia, Playford, Wheatland, and Larson's research indicated that nursing graduates from rurally located nursing programs were twice as likely (odds ratio = 2.25) as graduates of urban located schools (50% vs 25%) to seek employment in rural and remote areas23. In an earlier study of 429 Australian nursing and allied health students, Playford, Larson, and Wheatland found that 'congruent with previous studies ... rural background almost tripled [odds ratio = 2.878, p=0.001] the odds of choosing rural employment'24. Other literature recommends tailoring nursing student recruitment and the educational experience to promote rural practice25,26.
Similar studies in other health disciplines, particularly medicine, suggest that recruiting and retaining students from rural backgrounds is an effective strategy in addressing rural healthcare needs. Studies suggest that students from rural backgrounds are underrepresented in medical schools, due to lower application rather than acceptance rates27. Willoughby, Arnold, and Calkins' research in Missouri indicated that rural medical students were more likely to be Caucasian and to have parents with lower levels of education compared with students from urban backgrounds28, but supported other research demonstrating similar levels of achievement in medical school29. The rural students had significantly higher high-school-related extracurricular activities and class rank, but significantly lower recommendations from admission interviewers compared with urban students. These researchers recommended that 'admissions committees might need to abandon 'metropolitan' mind sets when selecting students from nonurban areas'28. Abundant research dating back more than 30 years in the USA, Canada, New Zealand, and Australia, has also shown that growing up in a rural area is a major predictor of future rural medical practice30,31. Carter's research in Manitoba, Canada specifically indicated that, for medical students, attending high school in a rural area was the strongest predictor of eventually choosing a rural practice setting32. This important finding has not been studied among nursing students.
Thus, given the limited evidence addressing the recruitment and retention of nursing students from rural backgrounds, further research is indicated. Conceptually, this project was built on Long and Weinert's Rural Nursing Theory33, and particularly the 'insider/outsider' concept. This well researched mid-range theory, which has been tested with a variety of rural and remote populations internationally, suggests that within rural society 'insiders' (long-term community residents) are more readily accepted and trusted as healthcare providers. To achieve 'insider' status, however, may take generations. Thus, in building and maintaining a trusted rural nursing workforce, recruitment and retention of 'insiders' who have grown up in rural communities is a logical strategy.
The purpose of this study was to compare rural and urban nursing students in relation to application, admission, and retention/graduation trends at Boise State University School of Nursing. The university is located in Boise, Idaho, the largest urban area of the state. The School of Nursing is the largest nursing education program in the state with more than 700 undergraduate and graduate students. Idaho is one of the most rural states in the USA, with a population density of 7.3 persons/km2 (18.9 persons/mi2) compared to 33.7 persons/km2 (87.3 persons/mi2) for the nation34. Approximately one-third of the state's 1.56 million people live in rural areas35 and the state's 35 rural counties account for 88% of Idaho's land area36.
A recently completed assessment of the Idaho nursing workforce conducted by Boise State faculty in collaboration with the Idaho State Board of Nursing indicated that the current Idaho nurse-to-population ratio in the rural counties is 469/100 000 (compared to 916/100 000 in urban counties), a disparity of about half. For the purposes of this study, recruitment was defined as the attraction of students to the program as reflected in the application rate. Acceptance was operationalized using the acceptance rate for students admitted to the nursing major per year and overall. Retention was defined as the percentage of students who maintained registration or graduated from the program.
A retrospective longitudinal descriptive design was used. The sample included 1283 applicants, accepted students and graduates of the Boise State University nursing programs between 2005 and 2010. Existing data from the School of Nursing and the university's admissions office were examined. Similar to most bacalaureate nursing programs in the USA, students enter the university as 'pre-nursing' majors and complete required prerequisite courses in their first 1-2 years. They then must apply for admission to the nursing major, which can be a highly competitive process. During the period of the study, rural background was not considered in admission decisions at the School of Nursing and students had very limited exposure to rural practice as part of the nursing curriculum. The criterion for admission was a minimum of a 2.5 grade point average (GPA) on a four-point scale in prerequisite courses. Eligible applicants were then rank ordered based on GPA in the admission decision-making. No interviews or essays were included.
For this study, individuals were classified as rural or urban based on their high school zip code. The high school zip codes were crosslisted with their respective 2006 Rural-Urban Commuting Area (RUCA) codes. Based on WWAMI Rural Health Research Center guidelines37, RUCA codes 1.0, 1.1, 2.0, 2.1, 4.1, 5.1, 7.1, 8.1, and 10.1 were classified as urban and all other codes were classified as rural. Using this method, a total of 356 (28%) rural and 927 (72%) urban individuals were identified. To more fully explore the rural subgroup, the sample was also categorized by large rural cities/towns (n=182, 14%), small rural towns (n=113, 9%), and isolated small rural towns (n=61, 5%) (using the WWAMI Rural Health Research Center four-category classification)37. Demographic data (including age, self-identified ethnicity, gender, socioeconomic status, and first-generation college graduate status) were also collected along with GPAs in required prerequisite courses for accepted students.
The data were entered into the Statistical Package for the Social Sciences v17 (SPSS Inc.; http://www-01.ibm.com/software/analytics/spss) and analyzed quantitatively. Descriptive statistics related to demographic characteristics, application, admission, and retention/graduation rates were assessed. Differences in application, admission, and retention rates between rural and urban background students were tested statistically using a significance level of p<0.05.
Ethics approval
Approval to conduct the study was obtained through the University Institutional Review Board prior to data collection; Boise State University IRB approval # EX 187-MED10-042.
The sample consisted of 1283 individuals, including 914 who were accepted to the program (71.2% overall acceptance rate) over the period of the study. Included within the group of accepted students over the 5-year period were 322 current students and 592 graduates. The analysis indicated that 31% of applicants, 25% of current students, and 27% of graduates were from rural backgrounds (Table 1). Demographically, there were no significant differences between the rural and urban samples in relation to age, gender, parents' level of education, or income; however, the rural sample had a significantly (p=0.046) higher percentage of Caucasians (92.5% vs 88.7%). As shown in Table 1, among the rural students (who constituted approximately 36% of admitted students), 81% were female, 56% reported incomes of less than $36,000, and 44% were first-generation college. Over the 5-year period, the acceptance rate for rural students (66.3%) was significantly lower than for urban students (73.1%) (Chi squared = 5.886, p=0.015). The yearly acceptance rate for rural background students ranged from 46% to 71%. The mean entering GPA for accepted students was exactly the same (3.49) for the rural and urban subgroups. The retention/graduation rate over the period of study was high for both rural and urban students (92% overall), with no significant difference in retention/graduation rates between the rural (90%) and urban (94%) students (Table 2).
When the sample was examined using the three levels of rural background (large rural, small rural, and isolated), some interesting differences emerged, particularly in relation to the applicants and students from the most rural backgrounds (classified as 'isolated'). They constituted 5% of the sample (n=61), but had the highest acceptance rate (75%) and shared the highest retention rate with students from small rural backgrounds (96%). They also had the highest entering GPA (3.65), were the least likely to be first-generation college (22% vs 41% for the total sample), were the least culturally diverse (95% were Caucasian) and had the highest percentage of women (85%). In contrast, the students from the large rural communities emerged as the group with the weakest academic profile. They constituted 14% (n=182) of the total sample and had the lowest acceptance rate (64%), the lowest retention rate (85%), the lowest mean GPAs (3.42) and the highest percentage of first-generation college individuals (50.9%).
Table 1: Sample demographic characteristics
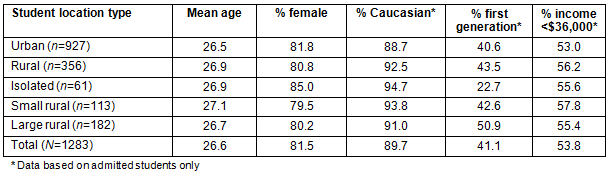
Table 2: Mean grade point averages, acceptance rates, and retention rates for rural and urban students
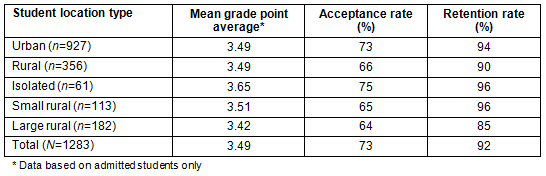
These findings suggest that a large urban university nursing program, located in a predominantly rural state, attracts a significant percentage of students from rural backgrounds. While retention/graduation rates are equally high, the acceptance rate for rural students overall is significantly lower than that for urban students. The limitations of the study include the fact that the data were based on only one institution and the ethnic diversity included in the sample was quite limited, but consistent with state and university demographics. In addition, the study was limited by the fact that data for some variables (parental education, income, and GPA) were voluntarily provided and available for only the admitted students.
The finding that applicants from rural backgrounds had a significantly lower acceptance rate than urban students, despite no differences in demographic characteristics except for ethnicity, is a major result and merits further exploration. Unfortunately, entering GPA data were only available for admitted students, thus it was not possible to assess preadmission academic competiveness between the rural and urban groups. However, given the fact that GPA was the major admission criteria used, it could be assumed that rural applicants may have had lower overall GPAs, thus reducing their acceptance rate. This may suggest that rural students lacked the educational background to complete the required prerequisite courses at a high enough level to be competitive, perhaps due to weaker educational preparation and/or academic counseling at the high school level.
In addition, perhaps students from rural backgrounds may not be as 'savvy' about the complexities of successfully navigating the application process to highly competitive nursing programs. Rural students may also be more challenged in adapting to the large urban academic environment, often far from family and community supports. As a result, pre-nursing students' optimal performance in challenging prerequisite coursework that is key to successful admission to nursing programs may be compromised because of these adaptation stresses. Further research is indicated to evaluate these possibilities.
The results related to differences among the rural subgroups suggest that students from rural backgrounds may differ in relation to their academic performance, as evidenced by retention/graduation rates. The results suggesting that students from the most rural/remote backgrounds enter with the highest GPAs and have the highest retention rates are particularly intriguing, given the often-limited financial and educational resources available to students from isolated areas. These students' achievement may be strongly influenced by the fact that they came from the most highly educated families, which was a particularly surprising finding, given that remote areas in the USA tend to have the lowest percentages of college-educated residents. This group may be exhibiting the 'frontier spirit', exemplified by the commitment and determination to overcome barriers. The findings suggesting that students from large rural areas are perhaps at highest risk academically, entering with the lowest GPAs and having the lowest retention rates, are equally interesting. One explanation might be that many of the large rural areas in Idaho have experienced rapid growth in the past decade which has severely impacted educational resources in local school systems. However, adapting to the urban university environment would be theoretically the least challenging for these students compared to students from smaller communities.
Further research is indicated specifically examining the unique aspects of the rural subgroups, particularly residents at the two ends of the rural continuum (isolated and large rural communities) in terms of achievement and academic needs. A qualitative exploration of applicants' knowledge of and experience with the application process may also aid in better understanding differences in acceptance and retention rates.
Educational implications of the findings are consistent with previous national and international studies related to the recruitment and retention of students from rural backgrounds. The findings from this study suggest that targeted recruitment of students, particularly from the most rural backgrounds, may be indicated, given their strong academic performance. The results indicate that students from large rural areas may be at highest academic risk, suggesting that this particular rural subgroup may need specialized retention interventions. Given the significant difference in acceptance rates between rural and urban applicants, greater efforts to recruit and help prepare rural high school and pre-nursing students to be successful in gaining admission to highly competitive professional nursing programs are needed.
Overall, further research is indicated to assess optimal strategies in preparing and recruiting students from rural backgrounds and promoting rural nursing practice in professional nursing programs. Outreach to rural elementary, junior high, and high school students is essential, using a health careers recruitment approach, like that described by Glasser29 and his associates, which is a collaboration between Cooperative Extension and the Area Health Education Center, the Center for Rural Health of the Illinois Department of Public Health and the University of Illinois in Rockford. Also, as widely suggested by other investigators24,27,28,38, considering rural background, particularly graduation from a rural high school, as a positive factor in the admissions decision-making process may be advisable to increase enrollment of rural students. The results indicating equal retention rates between nursing students from rural and urban backgrounds is encouraging and speaks to the strengths of rural students, despite cultural differences and often distance from family. Support programs for students from rural backgrounds in adapting to the urban university environment may be indicated, particularly for pre-nursing students. In addition, given the results from previous research that healthcare providers tend to practice near where they are educated, nursing education programs could consider increased efforts to provide outreach or satellite programs in rural areas to promote students staying and practicing in rural communities.
Implications for further research also include the need to identify predictors of rural employment in nursing, specifically addressing rural background of students as well as faculty as possible predictive factors. Similar to previous studies in medicine, large, prospective studies that include geographically and ethnically diverse samples are needed to assess this critical aspect. Studies evaluating the effect of inclusion of rural content and experiences within nursing programs on future rural employment are also indicated. Additionally, assessing the effect of the location (rural/urban) of the nursing educational program on future employment and long term career trajectories among nurses is recommended.
Policy implications include the need for support for educational equity for rural K-12 public educational systems. Rural students, particularly at the high school level, should have equal access to high quality instruction that prepares them well for higher education. Through distance education strategies many rural school systems are addressing this challenge; however, funding support and advocacy at the policy level is needed. Students from rural backgrounds could also be provided with specific incentives, including scholarship support that is tied to rural service after graduation. Some local communities currently provide this type of support, but expanded initiatives at the state and/or national levels are needed to effectively address future rural healthcare workforce needs.
This study represented the largest study to date addressing the issue of the recruitment and retention/graduation patterns of nursing students from rural backgrounds. The findings suggest that the recruitment of rural students may be an effective strategy in addressing the chronic rural nursing shortage. As the predominant providers of healthcare services in rural communities, nurses represent a critical resource. Concerted efforts on multiple levels are needed to ensure an adequate and well-prepared rural nursing workforce for the future.
Acknowledgements
This research was supported by the grant from the Jody DeMeyer Endowment, Boise State University, School of Nursing. The investigators acknowledge Dr Heather Young, Dr Joanne Noone, Diane Kenski and Shelley Sinclair for their assistance in the preparation of this manuscript.
References
1. Larson EH, Johnson KE, Norris TE, Lishner DM, Rosenblatt RA, Hart LG. State of the health workforce in rural America: profiles and comparisons. Seattle, Washington: WWAMI Rural Health Research Center, University of Washington, 2003.
2. LaSala KB. Nursing workforce issues in rural and urban settings: looking at the differences in recruitment, retention and distribution. Online Journal of Rural Nursing and Health Care 2000; 1(1): 8-17.
3. Movassaghi H, Kindig DA, Luhl N, Geller JM. Nursing supply and characteristics in the nonmetropolitan areas of the United States: findings from the 1988 National Sample Survey of Registered Nurses. Journal of Rural Health 1992; 8(4): 276-282.
4. Stratton TD, Dunkin JW, Juhl N. Redefining the nursing shortage: a rural perspective. Nursing Outlook 1995; 43(2): 71-77.
5. Skillman SM, Palazzo L, Keepnews D, Hart LG. Characteristics of registered nurses in rural versus urban areas: implications for strategies to alleviate nursing shortages in the United States. Journal of Rural Health 2006; 22(2): 151-157.
6. Boybjerg RR, Ormond BA, Pindus N. The nursing workforce challenge: public policy for a dynamic and complex market. (Online). Health Policy Center (Urban Institute), 2009. Available: http://www.urban.org/UploadedPDF/411933_professionalnurse.pdf (Accessed 28 December 2012).
7. Tri-Council for Nursing. Joint statement from the tri-council for nursing on recent registered nurse supply and demand projections. (Online) 2010. Available: https://www.aacn.nche.edu/Media/NewsReleases/2010/tricouncil.html (Accessed 28 December 2012).
8. U.S. Department of Health and Human Services, Health Resources and Services Administration, Bureau of Health Professions, National Center for Health Workforce Analysis. Toward a method for identifying facilities and communities with shortages of nurses. Washington, DC. (Online) 2007. Available: http://bhpr.hrsa.gov/healthworkforce/reports/methindentifysummary.pdf (Accessed 28 December 2012).
9. Staiger DO, Auerbach DI, Buerhaus, PI. Registered nurse labor supply and the recession - are we in a bubble? New England Journal of Medicine 2012; 366: 1463-1465.
10. Juraschek SP, Zhang, X, Ranganathan, VK, and Lin V. United States registered nurse workforce report card and shortage forecast. American Journal of Medical Quality 2012; 27(3): 241-249.
11. 11. Roscigno VJ, Crowley M. Rurality, institutional disadvantage, and achievement/attainment. Rural Sociology 2001; 66(2): 268-293.
12. McGrath DJ, Swisher RR, Elder GH Jr, Conger RD. Breaking new ground: diverse routes to college in rural America. Rural Sociology 2001; 66(2): 244-267.
13. Briscoe RL. Anticipated college attendance by urban and rural high school students. PhD dissertation. Ann Arbor, Michigan: University of Michigan, 1988.
14. Parsons JW. Undergraduate persistence rates of rural Californians at the University of California, Berkeley. PhD dissertation. Berkeley, California: University of California, Berkeley, 1992.
15. Sanders WB, Osborne RT, Greene JE. Intelligence and academic performance of college students of urban, rural and mixed backgrounds. Journal of Educational Research 1955; 49(3): 185-193.
16. 16. Maginnis C, Croxon L. Diversity in rural students: identifying student learning needs. Education in Rural Australia 2006; 15(2): 3-9.
17. Caison AL, Bulman D, Pai S, Neville D. Exploring the technology readiness of nursing and medical students at a Canadian university. Journal of Interpersonal Care 2008; 22(3): 283-294.
18. Dale RR, Miller PM. The urban or rural background of first year university students in relation to their academic performance. British Journal of Educational Psychology 1972; 42: 152-158.
19. Miller GW. Success, failure and wastage in higher education. London: Harrap, 1970.
20. Schonell FJ, Roe E, Meddleton IG. Promise and performance. Brisbane, Queensland: University of Queensland Press, 1962.
21. Wood D. Effects of educational focus on a graduate nurse's initial choice of practice area. Journal of Professional Nursing 1998; 14(4): 214-219.
22. Bushy A, Leipert BD. Factors that influence students in choosing rural nursing practice: a pilot study. Rural and Remote Health 5: 387. (Online) 2005. Available: www.rrh.org.au (Accessed 18 September 2013).
23. Playford D, Wheatland B, Larson A. Does teaching an entire nursing degree rurally have more workforce impact than rural placements? Contemporary Nursing 2010; 35(1): 68-76.
24. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Australian Journal of Rural Health 2006; 14(1): 14-19.
25. Omeri A, Ahern M. Using culturally congruent strategies to enhance recruitment and retention of Australian indigenous nursing students. Journal of Transcultural Nursing 1999; 10: 150-155.
26. Bumgarner SD, Means BH, Ford MJ. Building bridges: from high school to healthcare professional. Journal of Nurses Staff Development 2003; 19(1): 18-22.
27. Cullison S, Reid C, Colwill JM. Medical school admissions, specialty selection, and distribution of physicians. Journal of the American Medical Association 1976; 235: 502-600.
28. Willoughby TL, Arnold L, Calkins V. Personal characteristics and achievements of medical students from urban and nonurban Areas. Journal of Medical Education 1981; 56(9): 717-726.
29. Glasser M, Hunsaker M, Sweet K, MacDowell M, Meurer M. A comprehensive medical education program response to rural primary care needs. Academic Medicine 2008 83(10): 952-961.
30. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: a review of the literature. Academic Medicine 2002; 77: 790-798.
31. Laven G, Wilkinson D. Rural doctors and rural backgrounds: how strong is the evidence? A systematic review. Australian Journal of Rural Health 2003; 11(6): 277-284.
32. Carter RG. The relation between personal characteristics of physicians and practice location in Manitoba. Canadian Medical Association Journal 1987; 136: 366-368.
33. Long KA, Weinert C. Rural nursing: developing the theory base. Scholarly Inquiry in Nursing Practice 1989; 3(2): 113-127.
34. United States Census Bureau. Quick facts - Idaho. (Online) 2011. Available: http://quickfacts.census.gov/qfd/states/16000.html (Accessed 28 December 2012).
35. United States Department of Agriculture, Economic Research Service (USDA-ERS). (Online). Idaho: three rural definitions based on Census places. Available: http://www.ers.usda.gov/datafiles/Rural_Definitions/StateLevel_Maps/ID.pdf (Accessed 28 December 2012).
36. Idaho Department of Commerce. Five-year strategic plan for housing and community development programs. (Online) 2010. Available: http://www.commerce.idaho.gov (Accessed 28 December 2012).
37. WWAMI Rural Health Research Center. RUCA data: using RUCA data. (Online) 2010. Available: http://depts.washington.edu/uwruca/ruca-uses.php (Accessed 28 December 2012).
38. Pepper CM, Sandefer RH, Gray MJ. Recruiting and retaining physicians in very rural areas. Journal of Rural Health 2010; 26(2); 196-200.

