Approximately 51 million people or 16% of the US population reside in the non-metropolitan or rural counties that make up 75% of the US land area. Counties may be classified as either metropolitan (urban) or non-metropolitan (rural) using the National Center for Health Statistics' (NCHS) urban/rural classification scheme. There are six classifications used in the NCHS scheme. These are:
Metropolitan counties:
- Large Central Metro County - Primary Metropolitan Statistical Areas (PMSA) or sub-areas that meet the qualification to be a Metropolitan Statistical Areas (MSA) but have a population of 1 million or more that contain the entire population of the largest principal city of the MSA or are completely contained within the largest principal city of the MSA or contain at least 250 000 residents of any principal city in the MSA.
- Large Metro Fringe County - MSA or PMSA population of 1 million or more that do not qualify as Large Central Metro Counties.
- Medium Metro County - MSA population of 250 000 to 999 999.
- Small Metro County - MSA population of 50 000 to 249 000.
Non-metropolitan counties:
5. With a city of 10 000 or more residents.
6. Without a city of 10 000 or more residents.
Of 3147 counties and county-like entities in the USA, 1090 or 34% were classified metropolitan counties (code 1 to 4). The remaining 2057 were classified as non-metropolitan (code 5 or 6) or 'rural'.
It is often asserted that rural populations have less access to health care than urban residents. A review of the US Department of Health and Human Services' Health Resources and Services Administration (HRSA) areas which have been designated as Medically Underserved Areas (MUAs) seems to support this assumption. HRSA designates regions as MUAs on the basis of several factors, including the ratio of primary medical care physicians per 1000 population, infant mortality rate, percentage of the population with incomes below the poverty level, and percentage of the population aged 65 years or over. MUAs may be entire counties in non-metropolitan areas, groups of contiguous counties or minor civil divisions, or census tracts in metropolitan areas1.
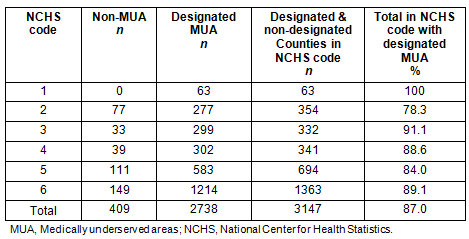
Of the 2738 counties with designated MUAs by HRSA, 1797 or 65.6% of the total are in non-metropolitan counties (Table 1). Eighty-four percent, or 583 of the 694 the non-metropolitan counties with a city of 10 000 or more (code 5), contained areas designated medically underserved and 89%, or 1214 of the 1363 non-metropolitan counties without a city of 10 000 or more (code 6), contained designated areas.
Table 1: Counties with designated Medically Underserved Areas according to the US Health Resources and Services Administration
For many of these communities, the local hospital is the most important provider of health care.
Hospital employment often the largest component of a rural county's healthcare sector total employment2. As such, the hospitals are particularly important to rural communities not only in terms of its contribution to overall health, but also to the county's economic development. Indeed, local hospitals have been described as '...a lynchpin for the development of local and regional healthcare services'3. High quality health care serves to promote economic development and attract new businesses4. Hospitals not only have a role in attracting new businesses to rural communities5, but they also tend to provide economic stability in economic downturns6. Additionally, by attracting revenues from outside of the community in the form of health insurance reimbursements, hospitals act as 'basic industries', thereby generating a multiplied economic impact.
Given the number of counties that contain MUAs, one would hypothesize that, in general, as a county become less metropolitan the percentage of county labor force employed by county hospitals would fall relative to the national average. The location quotient is the ratio between a local economy's sector employment and that of some geographic reference unit. As shown below, the geographic reference unit is frequently the country as a whole.

If the sector's share of employment within a local economy is greater than the share in the reference economy, the industry is assumed to be creating employment levels above that needed to serve the local economy. For example, if a county's hospital employment is 7.5% of total county employment, and at the national level (the reference economy) the sector employs 5% of the total workforce, then the county's location quotient is 1.5. Location quotients greater than 1 are deemed to signify that a sector is basic to the local economy and that the local economy is 'exporting' the proportion of the sector's output over that sufficient to support its needs; while those with location quotients of less than 1 are assumed to 'import' the goods or service. This 'export' production brings dollars to the community that flow through the local economy generating direct, indirect and induced economic impacts. The greater the net inflow of money from outside of the local economy, the greater will be the total local economic impact that the sector has upon the community.
In order to develop a metric to examine hospital employment levels in rural counties relative to urban counties, location quotients are calculated for all counties that reported some level of hospital employment in the 2010 Bureau of Census County Business Pattern (CBP) data. The CBP data are generated by the Bureau of Census annually. Data are reported for establishments, physical locations of economic activity and are classified using the North American Industrial Classification System (NAICS). The system classifies using a 2 to 6 digit classification scheme with each numerical level signifying greater specificity with respect to the primary activity of each establishment. The CBP includes data for private, non-farm employment and some government sectors. Data for establishments involved in agricultural production, data for self-employed individuals, employees of private households, railroad employees and most government activities are not included. However, data for government employment for NAICS sector 622, hospitals, are included.
The CBP reports employment statistics for full- and part-time employees' employment during the week of March 12 for each year. Data are collected at the national, state and county levels. The level of specificity contained in each geographic level of the data varies considerably. Data at the national and state levels contain several fields for NAICS data down to the 6 digit level. Aggregated information on the number of establishments, Mid-March Payrolls, Mid-March employment and annual payrolls are provided are reported by employment size category (1-4 employees, 5-9, 10-19 etc) at the state and national level. Flags indicating ranges for data suppression and imputed noise are also reported for each level.
County-level data contain far less granularity than the national and state level data. Unlike national and state level data, only the numbers of establishments by NAICS code by employment size class, mid-March employment, mid-March payroll and estimated annual payroll are reported in order to prevent the disclosure of proprietary data for the operations of an individual employer. While there are typically sufficient numbers of firms within a NAICS category at the national and state level to prevent the disclosure of proprietary information for individual firms, this is usually not the case for county-level data. Payroll and employment data are not reported for each employment size category which results in an enormous amount of the county-level data being suppressed. As the NAICS level of sector specificity increases, more and more data items are suppressed to prevent firm specific data disclosure which results in a tremendous amount of the county-level data being suppressed. In the 2010 CPB county-level dataset, 2493 of the country's 3147 counties indicated some level of employment in the hospital services sector. However, only 348 of these counties reported numerical data for hospital quarterly employment and payrolls. The remaining counties suppressed the numbers of employees and payrolls in order to ensure confidentiality. This makes it impossible to conduct meaningful inter-county comparisons at the national level. Fortunately, a number methods have been developed to estimate the suppressed data7.
Among the methods suggested to estimate the suppressed data is a two-stage strategy technique detailed by Isserman and Westervelt8. The technique utilizes data flags to narrow the range for suppressed data to produce consistent estimates at the industrial and geographic level. This is similar to the technique that is used by Headwaters Economics Inc which also uses data flags to generate estimates for the suppressed employment data9. The Headwaters procedure uses the midpoints of suppressed employment size classes as a starting point for data estimation.
As a first step in the estimation process, CBP data at the national, state and county level were extracted from the Census Bureau's database for the year 2010. The state and national data are used to generate estimates for average employment levels for each size class for the hospital sector, NAICS sector 622. These estimates are then modified using information from the data suppression flags to generate 'best' estimates for each employment size class suppressed county-level Mid-March employment data. As a check on accuracy, the estimated county employment levels for each state were summed and compared with reported state totals. The difference between the estimated state totals and the reported state totals was computed for each state. This difference was then divided by the reported state total to yield a measure of accuracy of the estimates. On average, the estimated data were within 1.8% of the reported state totals. The estimated county Mid-March employment levels were then adjusted to force the sum of the estimated employment to equal the unreported total, which was computed by summing data that were reported at the county level and subtracting this from the total reported data. This yielded adjusted totals of estimated and reported county-level data that equaled the total state employment levels.
A similar procedure was employed to produce county-level estimates of Mid-March payroll for NAICS 622 which served as a secondary check of the accuracy of the employment estimates. The first step in this process was to first estimate the level of Mid-March payroll data that was unreported or suppressed. This was done by summing the reported payroll data each size class at the state level, and subtracting it from the aggregated state total Mid-March payroll reported. The difference yielded the level of suppressed Mid-March payroll. A similar procedure was used to generate the number of Mid-March employees that were not reported. Next, average Mid-March payroll was computed for size classes with reported data by dividing reported payroll by reported Mid-March employment. Where data were suppressed for a particular size class, the unreported payroll totals were divided by the unreported employment to yield an average payroll figure that was then used for each unreported cell. These averages were then applied to each county level's adjusted employment by size class to yield estimates of county 622 Mid-March payroll. As with the employment estimates, the county-level data were summed for each state and then compared with the reported state level Mid-March Payroll. The aggregated unadjusted county sums were within 0.72% of the reported aggregated state data.
Location quotients for each county were computed by taking the ratio of estimated county NAICS sector 622 employment percentage to the ratio of NAICS 622 employment percentage for the USA. As previously noted, it was anticipated that county location quotients would be inversely related to the degree to which a county could be classified as rural. The mean location quotients for each county classification are shown (Table 2).
Table 2: Mean location quotients of rural counties
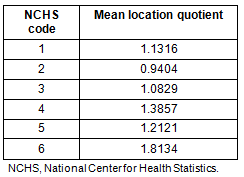
The most rural counties had the highest mean location quotients. The mean location quotient for large metro counties was above 1, as expected. This would imply that hospitals in these counties were 'exporting' specialized care not available in outlying areas. Location quotients for large fringe metro counties and medium metro counties were relatively close to 1, indicating levels of hospital employment sufficient to serve the local population. However, as counties became more rural, the location quotients tended to rise with the most rural counties (those without a city of 10 000 or more residents) having the highest location quotients. This indicates that hospital employment in the most rural counties relative to total county employment was higher than the national ratio. Given that the data presented in Table 1 indicates that 84% of the NCHS code 5 and 89% of the code 6 counties, the most rural classifications, are designated as being medically underserved, the higher location quotients and their implication of a higher proportion of regional hospital employment than for urban counties seems to be a counterintuitive outcome.
In order to explore the factors that might explain the unexpectedly high location quotients in rural counties relative to urban counties, the estimated employment and payroll data were combined with Census Bureau data detailing county percentages of uninsured residents10, data for county densities11, county median income levels and county urban-rural classifications from the Center for Disease Control12 to provide a county-level database with employment, payroll, income, density and health insurance data.
The location quotients were then regressed using ordinary least squares regression on the following continuous ratio scale independent variables:
- Total county employment: Total county quarterly employment
- Percent poverty: County poverty percentage - all ages
- Percent uninsured: Percentage of the county population
- Density: County population density, a measure of rurality
- Over 65 years: Percent of county residents 65 or older.
A model using log transformations of the variables was used in order to address severe heteroscedasticity in the untransformed data. The model yielded the results below (Table 3).
Table 3: Results of the model

Discussion
The results of the regression indicate that as the percentage of a county's population over age 65 and the county's poverty percentage rise, the county location quotient also rises. Increases in the total number workers employed, the percentage of the population that is uninsured and the county population density tend to lower the location quotient. Increases in the location quotient associated with increases in the county's percentage of the population over 65 are understandable. As proportion of the population receiving Medicare benefits increases, the flow of Medicare funding enables the county to support greater employment in the hospital services sector. Like Medicare, Medicaid brings external funding to the county's hospital. The effect of increases in the county's poverty level may imply that a relatively higher percentage of the population qualify for Medicaid coverage.
Increases in the county's uninsured population serve to reduce hospital revenues while increasing the costs associated with treating patients who cannot pay their bills. The negative effect of increases in population density may be due to the fact that increasing populations are associated with a more diverse economy, reducing the importance of the hospital service sector. Increases in the county's total number of workers employed serves to reduce the numerator of the location quotient formula, which would tend to lower the county's location quotient. In summary, location quotients tend to be higher in poor, rural counties with a high proportion of elderly residents.
A traditional interpretation of these relatively high location quotients would be that the counties were exporting hospital services, possibly providing services for even more rural surrounding counties which have no reported hospital employment (approximately 670 counties). More importantly, these results demonstrate that many rural counties are supporting a higher level of hospital employment than one would have anticipated. One inference that may be drawn from this is that funding from outside the community is supporting hospital employment levels greater than the county could be capable of supporting solely with local dollars. Two important sources of external revenue are the Medicare and Medicaid programs, both of which are related to the proportion of the population over 65 and the percentage of the population below the poverty level.
The Medicare program provides insurance coverage for eligible recipients who are aged 65 or older, who are under 65 but with a covered disability, and individuals with end-stage renal disease of any age. Beneficiaries may opt for several different coverage options. Medicare provides a number of programs to enrollees. These include Part A, which covers part of inpatient care in hospitals, skilled nursing facilities and hospice and home health care for qualified patients, and Part B, a coverage option for which beneficiaries pay an additional premium that provides coverage for a portion of physicians' services and outpatient care, services provided by physical and occupational therapists, and some additional home health care if they are designated are medically necessary. Part C is an alternative to Parts A and B that allows beneficiaries to receive care from other healthcare insurance plans and Medicare Advantage, a contract provider of services. Part D provides subsidized access to pharmaceuticals13. For fiscal year 2012, Medicare payments to health providers are expected to total $555.9 billion14.
Medicaid, a joint federal and state, means-tested program, was enacted in the same legislation that created Medicare. Medicaid provides essential medical and medically related services to qualifying low-income families with children, older individuals, and the disabled. It also provides supplemental coverage for some low-income Medicare beneficiaries for services not covered by Medicare, Medicare premiums, deductibles, and cost sharing. Medicaid is jointly financed by the states and the federal government. Federal spending levels are determined by the number of people participating in the program and services provided. Medicaid is funded with general revenues. Historically, the federal government's contribution under the federal medical assistance percentage (FMAP), has ranged between 50% and statutory maximum of 83% of the payments for services provided under each state Medicaid program15. The federal contribution rate is based on the state's per capita income. Medicaid coverage has been limited to low-income children, pregnant women, parents of dependent children, the elderly and the disabled. Establishing eligibility standards, benefits packages, payment rates and program administration are the responsibilities of states participating in the program. Federal spending on Medicaid was projected to be $273 billion in 2011 with state and local expenditures for Medicaid adding an additional $159 billion16.
Support for the idea that Medicare dollars are disproportionately important to rural communities is found in the Medicare Payment Advisory Commission's June 2012 'A Data Book: Health Care Spending and the Medicare Program'17. While approximately 16% of the population resides in rural counties, the Data Book indicates that 24% of the Medicare population resides in rural areas. Likewise, data indicates that while 13% of the urban residents receive Medicaid assistance, 16% of the rural population does18. Further, rural physicians receive 56% of their revenue from Medicare and Medicaid19.
Taken together, the finding that a high proportion of rural counties have medically underserved areas while having location quotients that are on average higher than those for urban counties suggests that the flow of Medicare and Medicaid dollars to rural communities enables them to support a higher proportion of the county workforce in the hospital sector than would be expected. While many of these counties have MUAs, the implication is that in the absence of the Medicare and Medicaid programs, their situation vis-à-vis the availability of health care would be worse than it is. Likewise, in the absence of these programs, the economies of many rural counties would suffer in that one of the most important county economic sectors, health care and hospitals in particular, would not be able to provide the levels of employment that it does. Given these results, recent legislation relating to health care not only has implications for rural health, but for rural economies as well.
The recently enacted Patient Protection and Affordable Care Act of 2010 (ACA) is an ambitious legislative initiative that greatly expands Medicare and Medicaid coverage to a large segment of the population. Among the provisions of the Act which have received the most attention are those that relate to expansions in the population eligible for Medicare and Medicaid coverage, and the requirement that individuals either purchase 'minimum essential coverage' or pay a penalty. Employers will be required to enroll new full-time employees in the coverage or pay fixed per-employee fees based on the number of individuals employed. Beginning in 2014, individuals who earn less than 133% of the poverty level will be eligible to enroll in Medicaid. It is anticipated that under the ACA, an additional 32 million individuals will be provided insurance coverage by 2014.
Funding for the program consists in large part of $716 billion will be taken from the current Medicare budget. Approximately 65% of these dollars will come from decreases in hospital and service provider reimbursement rates and payments to Medicare Advantage, a program where Medicare recipients can opt for private insurance carriers to provide their Medicare benefits. While Medicare reimbursement rates to hospitals will be reduced, some hospital administrators have embraced the new legislation. This is because they anticipate that large numbers of uninsured patients that hospitals have been required to treat in the past will be covered under the Act and that this may actually increase overall payments to hospitals. However, there is some concern that rural hospitals will be adversely affected by the Act. Accordingly, the Act contains specific provisions designed to protect rural hospitals. These protections include the extension of geographic fee adjustments which serve to increase fees to service providers in rural areas, and short-term adjustments and cost reimbursements for lab services provided by small rural hospitals.
Reductions in reimbursement rates for rural facilities could have potentially severe effects that might not be offset by increases in payments from newly insured patients. While the ACA will bring more individuals under the Medicare and Medicaid insurance umbrellas, it is possible that the reduction in reimbursements to providers may result in their refusal to accept the new Medicare patients.
Although the ACA has the potential for increasing coverage in rural areas and thereby providing a boost to rural economies, the Budget Control Act of 2011 (BCA) would have the opposite effect. The BCA imposes severe reductions in discretionary and nondiscretionary programs funded by the federal government beginning in 2013 and extending until 2021. In order to meet a budget reduction target of $1.2 trillion, a budget sequester provision will reduce spending across the board in most discretionary and non-discretionary programs. However, the Medicare program is somewhat protected in terms of the Act's impact on its budget. Under BCA, only up to 2% of Medicare's budget can be sequestered annually. Even so, it is estimated that this will translate to a budget reduction of $10.7 billion in 2013, rising to $16.4 billion in 2021. An economic impact study prepared by Tripp Umbach Healthcare Consulting in July of 2012 estimated that the direct, indirect and induced effects of these budget reductions will result in the loss of 496 000 jobs within the first 5 years of the sequestration period20. Originally scheduled to take effect on 2 January 2013, the sequester of Medicare funding was delayed until 1 March of that year. Preliminary estimates indicate that Medicare providers will be subjected to $11 billion in reimbursements in 2013. Counties with a high proportion of citizens over the age of 65 could see total hospital reimbursements fall. Low density, rural counties with a high proportion of uninsured residents and low median household incomes will therefore see increasing pressure on their hospital services sector. Given the relative importance of this sector to these counties, it is suggested that there will be adverse effects in terms of overall economic impacts. Should the reimbursement reductions be long lasting, this would tend to make the prospect of employment in these poor, rural counties unattractive for healthcare providers.
Conclusions
The analysis of county-level data suggested that poor, rural counties with a high proportion of residents over the age of 65 tend to have a higher proportion of their working population employed in the hospital services sector than do richer, urban counties. This finding raises the question of how these counties can support this relatively higher intensity of hospital employment in the absence of programs that provide external funding to support hospital hiring. The most important public programs providing this support are Medicare and Medicaid. Social Security is another source of federal funding important for rural populations. Sequestration and other cuts in funding could impact rural communities significantly. This can be even worse in states that fail to expand Medicaid and in states that fail to increase Medicaid reimbursements for services important in rural communities. This illustrates a lack of consistency in the nation's approach to healthcare policy, and the conflicts that are inherent in the conflicting goals of expanding the availability of health care and deficit reduction.
References
1. US Department of Health and Human Services, Health Resources and Services Administration. Medically Underserved Areas & Populations (MUA/Ps): Guidelines for MUA and MUP Designation. (Online) 1995. Available: http://bhpr.hrsa.gov/shortage/muaps/index.html (Accessed 10 November 2010).
2. US Bureau of Census. County Business Patterns: 2010. (Online) 2012. Available: http://censtats.census.gov/cgi-bin/cbpnaic/cbpdetl.pl (Accessed 24 October 2012).
3. Wakefield M. Rural Hospitals and Rural Economic Development: Testimony Before the Agriculture, Rural Development and Related Agencies Subcommittee of the Senate Committee on Appropriations, July 11, 2000. (Online) 2000. Available: http://www.gpo.gov/fdsys/pkg/CHRG-106shrg68476/html/CHRG-106shrg68476.htm (Accessed 15 December 2012).
4. Doeksen GA, Hohnson T, Willoughby C. Measuring the Economic Importance of the Health Sector on a Local Economy: A brief Literature Review and Procedures to measure Local Impacts. The Southern Rural Development Center. (Online) 1997. Available: srdc.msstate.edu/publications/archive/202.pdf (Accessed 10 July 2013).
5. Lyne J. Quality-of-Life Factors Dominate many Facility Location Decisions. Site Selection Handbook, Vol 33. Atlanta, GA: Conway Research, August 1988; 868-870.
6. Goodman WC. Employment in hospitals: unconventional patterns over time. Monthly Labor Review 2006; 129(6): 3-14.
7. Glaeser EL, Kallal HD, Scheinkman JA, Sheifer A. Growth in Cities. Journal of Political Economy 1992; 100(6): 1126-1152.
8. Isserman AM, Westervelt J. 1.5 Million Missing Numbers: Overcoming Employment Suppression in County Business Patterns Data. International Regional Science Review 2006; 29(3): 311-335.
9. Headwaters Economics. County Business Patterns Data Computation and Disclosure Estimation Process, June 8, 2010. (Online) 2010. Available: http://headwaterseconomics.org/wphw/wp-content/uploads/CBP_Documentation.pdf (Accessed 12 October 2012).
10. US Department of Commerce, Census Bureau. Small Area Health Insurance Estimates. (Online) no date. Available: http://www.census.gov/did/www/sahie/data/interactive/ (Accessed 3 November 2012).
11. US Department of Commerce, Census Bureau. U.S. Gazetteer. Census U.S. Gazetteer Files. (Online) 2010. Available: http://www.census.gov/geo/maps-data/data/gazetteer.html. (Accessed 7 November 2012).
12. US Department of Health and Human Services, Centers for Disease Control and Prevention. NCHS Urban-Rural Classification Scheme for Counties: January 2012. (Online) 2012. Available: http://www.cdc.gov/nchs/data_access/urban_rural.htm. (Accessed 5 October 2012).
13. Centers for Medicare and Medicaid Services. Medicare Trustees Report. (Online) 2012. Available: http://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/ReportsTrustFunds/index.html?redirect=/reportstrustfunds/ (Accessed 10 July 2013).
14. Congressional Budget Office. Medicare Baseline. (Online) 2012. Available: http://www.cbo.gov/sites/default/files/cbofiles/attachments/43060_Medicare.pdf .
15. Baumrucker EP. Medicaid: The Federal Medical Assistance Percentage. (Online) no date. Available: www.aging.senate.gov/crs/medicaid6.pdf .
16. US Department of Health and Human Services. 2011 Actuarial Report on the Financial Outlook for Medicaid. Washington, DC: US Government, 2011. Available: http://medicaid.gov/Medicaid-CHIP-Program-Information/By-Topics/Financing-and-Reimbursement/Downloads/medicaid-actuarial-report-2011.pdf
17. Medicare Payment Advisory Commission. A Data Book: Health Care Spending and the Medicare Program. (Online) 2012. Available: http://www.medpac.gov/documents/Jun12DataBookEntireReport.pdf (Accessed 21 November 2012).
18. North Carolina Rural Health Research and Policy Analysis Center. State Profiles of Medicaid & CHIP in Rural and Urban Areas. (Online) 2009. Available: http://www.shepscenter.unc.edu/medicaidprofiles/ (Accessed 22 October 2012).
19. Reschovsky JD, Staiti AB. Physician Incomes in Rural and Urban America: Issue Brief No. 92. (Online) 2005. Available: http://www.hschange.com/CONTENT/725/ (Accessed 9 December 2012).
20. Tripp Umbach Healthcare Consulting. The Negative Employment Impact of Medicare Cuts in the Budget Control Act of 2011. Available: www.aha.org/content/12/12sep-bcaeconimpact.pdf (Accessed 21 November 2012).
