Colorectal cancer (CRC) is the third leading cause of cancer mortality in men and women in the USA, with a lifetime risk of 5.5% for US men and 5.1% for US women1. CRC screening reduces mortality by identifying precancerous lesions and early stage cancers that are amenable to treatment. In 2008, the U.S. Preventive Services Task Force recommended the following as acceptable methods of screening for CRC in average-risk, asymptomatic individuals 50 to 75 years of age: annual high-sensitivity fecal occult blood testing (FOBT), sigmoidoscopy every 5 years with high-sensitivity FOBT every 3 years, or colonoscopy every 10 years2. Despite the benefits of CRC screening, only 58.6% of US adults between 50 and 75 report being up to date with recommended CRC screening3.
Rural residents have lower rates of appropriate CRC screening compared to their urban counterparts4. This may be in part because rural residents tend to have lower socioeconomic status, are more likely to live in a health professional shortage area, and are less likely to have health insurance compared to residents of urban areas4,5. However, data from a nationally representative sample showed that rural residents have lower rates of CRC screening even after controlling for socioeconomic variables, health insurance status, and residence in health professional shortage areas, suggesting that other characteristics influence compliance with CRC screening among rural residents4. Additionally, recent studies show that rural women have lower CRC screening rates compared to their male counterparts4,6-8 . While data from the 1980s to 2000s indicated higher rates of CRC screening in men compared with women9, nationally these gender disparities have attenuated over time, presumably due to increased public awareness of the benefits of CRC screening for both men and women. However, CRC screening rates in rural women continue to lag behind those of both rural men4,6,7 and urban women3,10-12.
What is known about CRC screening in rural areas is largely limited to secondary analysis of large population-based survey studies that document the disparities in CRC screening, but are unable to identify the reasons for these disparities. This study uses qualitative methods to explore reasons why rural women may be less likely to receive recommended CRC screening from the perspective of their primary care physicians (PCPs). The Rural Women's Health Care Project was developed to better understand persistent barriers to clinical preventive services, including CRC screening, among rural-residing women. The project involved forming a network of rural PCPs, members of which were interviewed about their perspectives on providing clinical preventive services to women in rural communities. This study describes those perspectives and considers the implications for interventions to improve CRC screening in rural women.
Sampling methodology
In 2010, the Rural Women's Health Care Project recruited a purposive sample of PCPs practicing in a 28-county region of central Pennsylvania to participate in semi-structured interviews about primary care delivery for adult women in rural areas. The region of central Pennsylvania is an appropriate setting for this study because it consists of a range of communities, including midsized and small towns as well as isolated rural areas. Rural Pennsylvania residents are 92% Caucasian, with lower educational attainment and lower household incomes than their urban counterparts13. In 2005-2009, only 18% of rural residents 25 years and over had a bachelor's degree or higher, compared with 29% of urban Pennsylvanians of the same age13. The per capita personal income in rural Pennsylvanian counties was $10,483 less than in urban counties in 200913. Among women in the most isolated rural areas of central Pennsylvania, 34% were in poverty or near poverty, compared with 27% in urban areas14. In 2008, there was one PCP for every 1501 rural residents, compared to one PCP for every 981 urban residents in Pennsylvania13.
Using the American Medical Association (AMA) Physician Masterfile, allopathic and osteopathic physicians who were actively practicing in a non-federal office-based practice were identified in the specialties of family practice, internal medicine, general practice, and obstetrics and gynecology. Physicians trained in obstetrics and gynecology (with no further subspecialty) were included, because in many locations they provide primary and preventive care to women15,16.
The sampling frame was limited to physicians whose practices were located in rural zip codes or in those immediately adjacent. Rural zip codes were defined using the Rural Urban Commuting Area (RUCA) codes (http://depts.washington.edu/uwruca)4,5, a census tract-based classification scheme that includes measures of population density, urbanization, and daily commuting. RUCA codes occur on a scale of 1 to 10, with 1 representing the most metropolitan/urban zip codes and 10 representing the most rural zip codes. For the purposes of this study, we considered RUCA codes 7-10 to be rural zip codes. Using these definitions, 85 physicians met the above inclusion criteria from rural zip codes, and 165 physicians met inclusion criteria from zip codes geographically adjacent to rural zip codes. All the physicians practicing in zip codes geographically adjacent to rural zip codes were in RUCA codes 4-6, which are considered 'micropolitan' or 'large rural' areas.
Most of the 250 physicians in the AMA Masterfile who fitted the selection criteria had been trained in family practice (60%) or internal medicine (27%). Eligible physicians were mailed a letter inviting them to participate in the Rural Women's Health Care Project. In response to the letter, 12 physicians contacted the project to volunteer to be interviewed, and were enrolled in the study. Additional physicians were then contacted by phone, and those interested in participating were scheduled for interviews, with priority given to physicians in rural zip codes. Thematic saturation was reached at the completion of 19 interviews, and enrollment was closed.
Interviews
The interview guide was designed to explore PCPs' opinions and practices regarding primary care services to adult women residing in rural locations. It was pilot tested and sequentially revised with a convenience sample of six PCPs at the investigators' home institution until wording of the questions was optimized. Interviews were conducted at physicians' offices or via telephone, based on PCP preference and interviewer availability. Two investigators were present at each interview, one to conduct the interview and one as note-taker. Verbal consent of all physician participants was obtained at the time of the interview. Each interview lasted 45-60 minutes, was digitally recorded using two recorders, and then professionally transcribed.
All interviews began with ascertainment of years in practice, type of practice setting, and reasons for practicing in rural locations. The semi-structured interview had four sections: CRC screening, reproductive health care17, intimate partner violence, and mental health care. The interview was designed to explore physicians' experiences and opinions regarding the care of adult women (aged 18 years and older) in their practice and community. This paper presents data from the CRC screening section.
In the CRC section of the interview guide (Table 1), physicians were asked about their CRC screening practices (ie who to screen, screening methods offered, use of reminder systems) and barriers to screening (ie relative ease or difficulty of obtaining CRC screening procedures, barriers specific to female patients, and what could help overcome those barriers). Interviewers used additional probes to keep the discussion on topic or request elaboration of ideas.
Analysis
Seventeen (out of 19) interviews were analyzed. The CRC section was not completed due to time constraints during one interview, and digital recording failed during another interview. Two members of the research team (LAR, CHC) independently analyzed each transcript to identify emergent themes, for which there was full agreement. Illustrative examples of the themes were selected using representative quotes from the participants. NVivo software v8 for qualitative data (QSR International; http://www.qsrinternational.com) was used to group the responses into appropriate theme categories.
Ethics approval
This study was approved by the Institutional Review Board at Penn State College of Medicine; approval number 33253EP.
Table 1: Interview guide: colorectal cancer screening

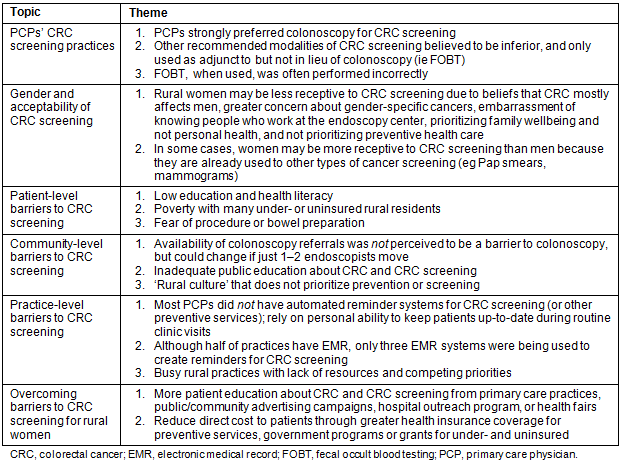
Of the 17 participants, 11 were trained in family practice, four in internal medicine, one in general practice, and one in obstetrics and gynecology (Table 2). The sample included 10 men and 7 women. Eight interviews were conducted in person in the participant's office, and nine by telephone. Practice types ranged from solo private practices to hospital-owned multi-specialty groups, and were located in 13 out of 28 counties in the target region; seven were in rural zip codes, and 10 were immediately adjacent to rural zip codes. All of the physicians reported providing primary care to rural women, spending at least 50% of an average week providing primary care to adults, with most doing so 80% of the week. The median number of years in practice was 25 (range, 1-38). Most physician participants had been in the same practice for their entire career, and only two had previously worked in urban locations. The predominant reason cited (by 11 physicians) for practicing in a rural area was growing up in a rural area, often in the same community where they now practice. Other physicians remained in their rural practice after serving in a National Health Service commitment, loan repayment program, or visa commitment.
The themes that emerged were in the topic areas of PCP's CRC screening practices, gender and acceptability of CRC screening, practice-level barriers to CRC screening, community-level barriers to CRC screening, and overcoming barriers to CRC screening for rural women (Table 3).
Table 2: Primary care provider characteristics (n=17)
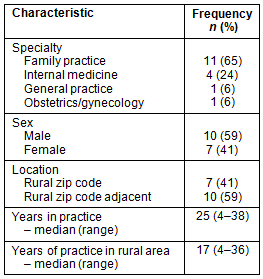
Table 3: Colorectal cancer screening in rural central Pennsylvania - themes
Preferred colorectal cancer screening method
The physicians were universally knowledgeable about CRC screening guidelines, endorsing the importance of beginning CRC screening at age 50, or earlier when appropriate due to family history or other risk factors. All 17 physicians definitively identified colonoscopy as their preferred CRC screening method, reporting their belief that other forms of screening were inferior. Only six PCPs (35%) use FOBT as a second-choice screening method when colonoscopy is declined by the patient, but several physicians commented that they considered FOBT a substandard screening tool, calling it 'not the best choice' or a 'poor second choice'. However, many of the PCPs who used FOBT as a second choice when patients declined colonoscopy were performing a single test for occult blood in the office as part of a digital rectal examination, rather than using the accepted FOBT screening protocol in which the patient is given three cards to collect samples at home2: 'I've really gotten away a lot from hemoccults which is simply data showing the poor sensitivity and specificity of it, but yeah I will do that ... if I'm doing a rectal exam'. Use of flexible sigmoidoscopy has been largely abandoned: 'We used to do sigmoidoscopies in the office, but ... why sweep the front porch when you [could] clean the whole house?'
Interestingly, some physicians were additionally screening for CRC outside of the current guideline recommendations, suggesting their belief that the accepted guidelines were insufficient. For example, four physicians offer FOBT before age 50 to average-risk persons. One PCP stated, 'I screen all the females over 40'. Thirteen physicians (68%) offer FOBT after age 50 in addition to colonoscopy screening, and seven physicians (41%) routinely perform FOBT screening with women during routine gynecologic examinations:
When I do a GYN exam, I always do a rectal and I do hemoccult testing even though they say that's not the right way to do it. But honestly, if you've ever given three hemoccult cards to somebody and told them to bring them back ... half the time you don't get them back and half the time they're so dried out that it's really hard to interpret what it was.
Gender and acceptability of colorectal cancer screening
Several physicians reported greater difficulty referring female patients for colonoscopy than male patients. PCPs reported that women were less concerned about CRC due to the belief that CRC mostly affects men. One PCP who perceived his female patients as more reluctant to undergo colonoscopy stated that, 'women believe that incidence of colorectal cancer is lower in them; they are more hung up on breast and ... endometrial cancer'.
Due to the nature of small rural communities, the PCPs reported that it would not be unusual for a patient to know someone who worked at the endoscopy center. While this was not perceived as a barrier for male patients, some physicians acknowledged that female patients were more likely to be embarrassed about 'who else is in the room' during the colonoscopy procedure. One physician explained, 'If they live right in that town and they know the people doing the procedures, the people in that room ... many will not have it done'.
Some physicians described gender-specific sociocultural norms in rural settings that contributed to reduced CRC screening, preventive care, and medical care in general. One physician explained that some rural women do not prioritize their own health, instead prioritizing the wellbeing of their families:
I think just the way they've been raised. They just take care of their family ... their husband ... the kids, they take care of the house and that's what they do ... they're on the bottom of the importance ladder.
Similarly, another PCP believed rural community norms led to reluctance among older women to pursue preventive health care:
When you get into the rural 65-70-75 year-old ladies, that basically were the farmer's wife and they had the kids ... these ladies are a little bit more reluctant to have things done. They were a hard, tough, group of women you know? They survived.
Three physicians (18%) reported greater success referring women for colonoscopy compared to men because their female patients are more receptive to cancer screening in general. Physicians stated that women were already used to having cancer screening (eg Pap smears, mammograms), so they were already aware of the importance of screening. One physician believed his female patients were 'a little more health-conscious' while 'men are a little more in denial about it'.
Patient-level barriers to colorectal cancer screening
Perceived patient-level barriers included low education levels, poverty, under- or uninsured status, and fear of procedure or bowel preparation. Most PCPs (71%) considered lack of education to be a barrier. This included low educational attainment in general, but specifically low health literacy, which was partly attributed to social isolation in rural communities resulting in lack of exposure to the media and being less computer-savvy compared to urban populations. One PCP stated about rural women, 'I think they're a little less savvy about health needs and about prevention than the suburban women'. PCPs reported lack of education as a barrier to CRC screening because patients had misconceptions about CRC, such as women believing that colorectal cancer mostly affects men, or that an asymptomatic person does not need CRC screening:
A lot of people think that there have to be symptoms going on before a problem or a screening test needs to be done.
I think the barriers ... are just educational - that some women don't believe that they are at as high a risk as men.
Ten physicians (59%) reported economic issues as a barrier to CRC screening in their rural practices. Specific issues included lack of insurance, insurance plans not covering preventive testing or requiring prohibitive co-pays, poverty (especially in light of the current economic crisis), and lack of transportation in rural areas: 'We are somewhat of a poverty-stricken area too, where not everybody drives and not everybody drives a car'. About insurance, one PCP elaborated, 'It's variable what their co-pay structure is for that procedure'. Another said, 'Some people don't have insurance or some insurances, unfortunately, don't cover screening tests'. Two PCPs spoke about prohibitive out-of-pocket costs for cultural groups that do not use health insurance: 'You talk about colonoscopy for screening and it just doesn't happen. They don't have an extra couple thousand bucks'.
Eleven physicians (65%) identified fear of the test or colon preparation as a barrier to CRC screening. Specific fears identified varied: 'They still continue to refuse it - whether or not it's because they're scared of the test - what they may find out'. Another PCP stated, 'Number one, they're afraid that their colon is going to be perforated'. Regarding the preparation, one PCP said, 'The word gets out ... that the preparation is not very pleasant'.
Community-level barriers to colorectal cancer screening
None of the PCPs believed availability of colonoscopy referrals was currently a significant barrier, in that endoscopy centers were available within driving distance and without significant wait times. Five physicians (29%) reported that colonoscopy services were available within their town or local community. Two PCPs offered colonoscopy services within their own internal medicine practices. This was the case because in previous years, when colonoscopy services were less available, physicians in those practices sought colonoscopy training so they could perform these procedures themselves. The remainder of physicians reported access to colonoscopy services within approximately 65 km of their practices. However, some physicians acknowledged having patients from remote rural areas far from the town where their practice is located, and these patients may travel even farther distances to the nearest colonoscopy services. Physicians also acknowledged that while colonoscopy services in their area were currently available, this could be subject to a significant change if one or two endoscopists were to relocate. One physician spoke about how availability of gastroenterologists could greatly change from year to year:
Ten years ago it wasn't that difficult to have colorectal cancer screening and then all of a sudden we had no gastroenterologists and now in the past three or four years we've had gastroenterologists again, but unfortunately rural Pennsylvania is not the most attractive place for specialists.
Community-level barriers identified included inadequate public education about CRC and CRC screening, and the presence of a 'rural culture' that does not prioritize prevention or screening. Eight physicians (47%) reported that some of their rural patients simply prefer not to undergo screening. Explanations included statements such as, 'Some say it's not broken, don't fix... I don't want to know what's wrong with me', 'They don't believe in treating anything until they're symptomatic', and 'They got through a whole lot in their life already ... I'm telling them they need a colonoscopy ... she'll say, give me a break'.
Practice-level barriers to colorectal cancer screening
Reminder systems - physician, physician extender, patient, and electronic systems: Nine PCPs (53%) personally initiate conversations with their patients about CRC screening, and rely on their own personal ability to remember to keep their patient up to date with CRC screening. Two practices task a nurse or medical assistant to identify preventive screening needs during the intake process. Three physicians' practices leverage their electronic medical record (EMR) systems to generate reminders about CRC screening and other preventive services (see below). In another practice, the health maintenance record notifies both the physician and the nurse of the patients' eligibility for CRC screening. One physician reported that patients have also started initiating the conversation: 'Believe it or not ... women getting close to 50 bring it up, because most of their plans say it's now a covered service and they should get it done'.
Nearly half (41%) of the practices had an EMR or computer-based charting system at the time of the interviews. Two physicians had EMR systems send an automatic alert to the physician during a clinical encounter when a patient was due for a colonoscopy. Another practice used their EMR to print a reminder sheet for each patient visit showing all health maintenance issues that were due to be addressed. These EMR reminder systems were only prompted during a patient's office visit. One physician who used automatic EMR alerts also used the EMR system to generate a list of patients over 50 who did not have a documented colonoscopy. Eligible patients were then notified by a staff member and offered colonoscopy scheduling. The physician set up this system, which was not dependent on an office visit, to identify patients who were not being seen routinely. Physicians who were not using their EMRs to assist with preventive services reported that either they did not find the EMR reminder systems to be useful (and thus did not activate them) or had not tried to use those functions.
Lack of time and effective reminder systems: Physicians identified lack of time as another practice-level barrier that inhibited effective CRC screening. Physicians often reported not having enough time to discuss preventive measures in their very busy rural practices, especially when only one physician is serving the community. One explained, 'I think the barrier could be how busy the doctors are ... we see sometimes 50-60 patients [a day]'. Unfortunately, if the opportunity to offer CRC screening were missed at one visit, there would be no opportunity to address it until the next office visit. Some physicians were optimistic that their EMR systems would improve CRC screening, but without an effective EMR reminder system they perceived that many patients due for CRC screening are missed. One PCP said, 'I think outside of [health system] where there's no electronic record, care is fragmented and people may have very intermittent visits ... and people with paper charts may not have a way of flagging or recognizing people who need colorectal screening'.
Overcoming barriers
Most physicians (78%) identified patient education as the most important way to overcome barriers to CRC screening:
Education is probably the biggest thing - talking to people about how important health preventative screening tests are and letting them know that you want to try to prevent problems, rather than wait and react to problems once they happen. I think if people would understand ... what exactly the procedure is like also, 'cause I think some people are afraid or nervous about what might be involved with the test and if they would understand that more, they may be more likely to kind of pursue it'.
Suggested educational venues included advertising campaigns, hospital outreach programs, health fairs, medical extenders discussing screening with patients, and use of educational materials within rural practices. One physician reported using educational materials on CRC screening in his practice, which he believed improved CRC screening rates. Several physicians wanted to see greater financial support from hospitals or the government to help overcome the cost barrier for patients who were under- or uninsured. For example, one PCP's patients previously could obtain colonoscopies through a grant for people without health insurance, and that PCP suggested similar programs for increasing CRC screening.
Discussion
This study explored PCPs' experiences and opinions about CRC screening services in rural central Pennsylvania to understand why women living in rural areas are less likely to receive recommended CRC screening compared with rural men and urban residents. Reasons were identified that may contribute to the CRC screening disparity related to PCPs' CRC screening practices (eg not using alternative screening modalities when colonoscopy is not possible), gender-related barriers to CRC screening in rural areas (eg belief that CRC mostly affects men, embarrassment of knowing people at the endoscopy center, prioritization of family issues over personal health), patient-level barriers (eg cost and health insurance issues, fear and perception of unpleasantness of colonoscopy), community-level barriers (eg inadequate public education about CRC and CRC screening, 'rural culture' that does not prioritize prevention or screening), and practice-level barriers (eg lack of effective reminder systems, lack of time).
It was not surprising that the PCPs uniformly preferred colonoscopy as a screening method, as it is the primary CRC screening method currently used in the USA. However, it was surprising to find that they largely abandoned all other forms of CRC screening, even for cases in which colonoscopy was not possible. Only one-third of the sample reported occasionally using FOBT for CRC screening when the patient deferred colonoscopy. Even in those cases, FOBT was usually performed during a digital rectal examination, rather than having the patient collect FOBT samples at home as recommended by the U.S. Preventive Services Task Force2. This finding was consistent with other studies reporting that physicians perceive the performance of FOBT as sub-par and offer it less often or with less confidence than colonoscopies, or do not offer it at all18-22. However, given the relatively lower CRC screening rates in rural communities, and especially among rural women, correctly performed FOBT could improve CRC screening rates and mortality when colonoscopy is not feasible. Increasing FOBT use has been successful in some settings22-24 and may be the most promising way to increase overall guideline-concordant CRC screening rates11,25,26. This may be particularly salient for resource-poor rural communities.
In rural areas, women are less likely to be up to date with CRC screening4,6,7. The PCPs did offer several explanations for this disparity, given their personal experiences providing primary and preventive care for women. Poor CRC-related knowledge was cited as an explanation - several physicians reported that CRC is not as prominent a concern for some women as breast or cervical cancer, or prostate cancer for men. The PCPs in our study identified embarrassment as a barrier to CRC screening that disproportionately affects women, specifically with regard to knowing people who work at the local endoscopy center. While embarrassment in general is a sentiment previously reported to be a major barrier to CRC screening, especially in women27-29, our data indicate that this is exacerbated in small rural communities where 'everyone knows everyone'. The PCPs reported the test preparation to be a greater barrier to colonoscopy screening in women than in men, which has also been reported previously30,31.
The PCPs reported that the most important patient-level barrier to CRC screening in women was low education and health literacy, and CRC-specific education was identified as the most important way to improve CRC screening rates in rural communities. While the PCPs welcomed CRC-related education in any venue, they believed that public education campaigns aimed at the specific needs of their rural communities would be particularly helpful. Tailoring or personalizing education methods to specific patients or populations has been shown to increase screening rates32. Advertising campaigns tailored to rural communities that used images and voices of real rural people mainly in their fifties (rather than actors or celebrities), and used simple, straightforward messages and lower-cost advertising methods (radio, weekly newspaper advertisements, posters, and postcards) have been found to be more effective in reaching rural populations than the equivalent mainstream campaign33.
The PCPs described a 'rural culture' in their communities, a societal-level barrier that de-emphasizes the importance of individual health and preventive health measures. They also described gender-specific sociocultural norms in rural settings that emphasize the role of women in caring for the needs of their family and household before their own, resulting in less engagement of female patients in preventive health services, especially screening. Further research to understand the barriers and facilitators of CRC screening from the perspective of rural women is needed to better understand how these cultural issues affect rural women's uptake of CRC screening. Health education programs can be aimed not only at increasing knowledge specific to CRC screening (eg that CRC affects women and men), but also the benefit of preventive screening in general. Capitalizing on rural women's desire to prioritize care of the family, these programs can also emphasize self-care as a mechanism for improving the care of others. Hopefully, increasing education about the importance of CRC screening will reduce the discomfort about discussing CRC screening with the doctors, and women will be less likely to avoid getting colonoscopies because of embarrassment.
Issues around insurance and cost of screening were also major barriers emphasized by the physician participants, and are aspects of healthcare access that affect rural populations disproportionately. Rural residents are significantly less likely than their urban counterparts to have employer-based health insurance because they are more often employed by small businesses (50% vs 37%), are more likely to work in low-wage jobs, and are more likely to be self-employed (33% vs 21%)34. Rural central Pennsylvania has an abundance of farming families, and 90% of farm and ranch families do not have health insurance35. This study's participants reported that participation of the government, hospitals, or insurance companies would be needed to lessen the financial barrier to colonoscopy screening. It is possible that rural residents may have the most to gain, with health insurance reform offered in the Affordable Care Act (ACA). Of note, this study was conducted prior to the ACA's mandatory first dollar coverage for CRC screening started in August 2012. Thus, the ACA could alleviate the problem of co-pays for CRC screening, identified by the PCPs as a barrier for their rural patient populations.
PCPs largely depend on their own ability to review preventive health services needs during routine clinic visits to ensure their patients are offered CRC screening. While this type of visit-dependent, PCP-dependent, and not systems-based CRC 'reminder system' is likely similarly used among PCPs in rural and non-rural locations, this may not be effective in rural communities if rural residents are truly less likely to value and follow up with routine primary and preventive care, as perceived by PCPs in this study. As more rural PCP practices obtain EMR systems, CRC screening may improve, because use of EMR technology has been proven to improve screening rates36. However, this study's data indicate that PCPs must believe that these systems are effective for them to be utilized. Furthermore, systems-based reminder strategies that are not visit-dependent should be explored. For example, this study reports the unique practice of one PCP who used his EMR to identify patients within his practice who were 50 years and older and did not have documented CRC screening. Clinic staff then contacted those patients to offer CRC screening counseling and colonoscopy referral. This strategy is not visit-dependent, and thus may be an attractive way of offering preventive screening to patients who do not regularly present for routine care. Of course, this type of approach to CRC screening requires additional clinic staff resources.
Limitations of this study must be considered. Although a diverse group of PCPs was interviewed in this study's rural target region and thematic saturation was believed to have been reached, the participants may not have represented all the experiences or opinions in the region. Additionally, the small sample size did not allow for comparisons across specialties. The findings may not be generalizable beyond rural central Pennsylvania, which is a largely Caucasian population with a mix of populations not found in many other states (Amish, Mennonite, Appalachian, etc.). These results represent the subjective opinions of the PCP participants and may differ from the opinions of women in the rural communities. Their opinions also may not represent barriers faced by women who never present for primary care. Future studies might address differences by PCP specialty and determine if PCP experiences differ in different rural contexts.
The reasons for the rural-urban and gender disparities in CRC screening are clearly multifactorial and complex. While availability of colonoscopy centers was initially hypothesized to be a significant barrier to CRC screening in rural communities, the results suggest otherwise. This study's findings suggest several interventions to potentially improve CRC screening among rural women. These include public health education campaigns that are specifically aimed at rural populations; PCP education regarding proper FOBT technique and the effectiveness of FOBT as a valid screening modality when colonoscopy is not possible; and reminder systems that are systems-based, visit-independent leverage electronic resources.
Acknowledgements
The Rural Women's Health Care Project was supported by a grant from the Penn State University Clinical and Translational Science Institute (CTSI). Drs Chuang (K23 HD51634) and McCall-Hosenfeld (K12 HD055882, Penn State BIRCWH Program) were supported by the Eunice Kennedy Shriver National Institute of Child Health and Human Development. None of the authors have any conflicts of interest.
References
1. American Cancer Society. Colorectal Cancer Facts & Figures 2008-2010. (Online) 2008. Available: http://www.cancer.org/cancer/colonandrectumcancer/detailedguide/colorectal-cancer-key-statistics (Accessed 3 September 2013).
2. U.S. Preventive Services Task Force. Screening for colorectal cancer: U.S. Preventive Services Task Force recommendation statement. Annals of Internal Medicine 2008; 149(9): 627-637.
3. Bennett KJ, Probst JC, Bellinger JD. Receipt of cancer screening services: surprising results for some rural minorities. The Journal of Rural Health 2012; 28(1): 63-72.
4. Coughlin SS, Thompson TD. Colorectal cancer screening practices among men and women in rural and nonrural areas of the United States, 1999. Journal of Rural Health 2004; 20(2): 118-124.
5. Zhang P, Tao G, Irwin KL. Utilization of preventive medical services in the United States: a comparison between rural and urban populations. Journal of Rural Health 2000; 16(4): 349-356.
6. Casey MM, Thiede Call K, Klingner JM. Are rural residents less likely to obtain recommended preventive healthcare services? American Journal of Preventive Medicine 2001; 21(3): 182-188.
7. Larson S, Correa-de-Araujo R. Preventive health examinations: a comparison along the rural-urban continuum. Women's Health Issues 2006; 16(2): 80-88.
8. Beydoun HA, Beydoun MA. Predictors of colorectal cancer screening behaviors among average-risk older adults in the United States. Cancer Causes & Control 2008; 19(4): 339-359.
9. Meissner HI, Breen N, Klabunde CN, Vernon SW. Patterns of colorectal cancer screening uptake among men and women in the United States. Cancer Epidemiology, Biomarkers & Prevention 2006; 15(2): 389-394.
10. Levy BT, Dawson J, Hartz AJ, James PA. Colorectal cancer testing among patients cared for by Iowa family physicians. American Journal of Preventive Medicine 2006; 31(3): 193-201.
11. Fan L, Mohile S, Zhang N, Fiscella K, Noyes K. Self-reported cancer screening among elderly Medicare beneficiaries: a rural-urban comparison. Journal of Rural Health 2012; 28(3): 312-319.
12. Holden DJ, Harris R, Porterfield DS, Jonas DE, Morgan LC, Reuland D, et al. Enhancing the use and quality of colorectal cancer screening. Evidence Report/Technology Assessment No.190. Prepared by the RTI International-University of North Carolina Evidence-based Practice Center. Rockville, MD: Agency for Healthcare Research and Quality, 2010.
13. Center for Rural Pennsylvania. Demographics: about rural PA. (Online) 2013. Available: http://www.rural.palegislature.us/demographics_about_rural_pa.html (Accessed 5 September 2013).
14. McCall-Hosenfeld JS, Weisman CS. Receipt of preventive counseling among reproductive-aged women in rural and urban communities. Rural and Remote Health 11(1): 1617. (Online) 2011. Available www.rrh.org.au (Accessed 5 September 2013).
15. Weisman CS. Women's health care: activist traditions and institutional change. Baltimore, MD: Johns Hopkins University Press, 1998.
16. Menees SB, Inadomi J, Elta G, Korsnes S, Punch M, Aldrich L. Colorectal cancer screening compliance and contemplation in gynecology patients. Journal of Women's Health 2010; 19(5): 911-917.
17. Chuang CH, Hwang SW, McCall-Hosenfeld JS, Rosenwasser L, Hillemeier MM, Weisman CS. Primary care physicians' perceptions of barriers to preventive reproductive health care in rural communities. Perspectives on Sexual and Reproductive Health 2012; 44(2): 78-83.
18. Rim SH, Zittleman L, Westfall JM, Overholser L, Froshaug D, Coughlin SS. Knowledge, attitudes, beliefs, and personal practices regarding colorectal cancer screening among health care professionals in rural Colorado: a pilot survey. Journal of Rural Health 2009; 25(3): 303-308.
19. Zapka JM, Klabunde CN, Arora NK, Yuan G, Smith JL, Kobrin SC. Physicians' colorectal cancer screening discussion and recommendation patterns. Cancer Epidemiology, Biomarkers & Prevention 2011; 20(3): 509-521.
20. Fenton JJ, Jerant AF, Von Friederichs-Fitzwater MM, Tancredi DJ, Franks P. Physician counseling for colorectal cancer screening: impact on patient attitudes, beliefs, and behavior. Journal of the American Board of Family Medicine 2011; 24(6): 673-681.
21. Flocke SA, Stange KC, Cooper GS, Wunderlich TL, Oja-Tebbe N, Divine G, et al. Patient-rated importance and receipt of information for colorectal cancer screening. Cancer Epidemiology, Biomarkers & Prevention 2011; 20(10): 2168-2173.
22. Lafata JE, Cooper GS, Divine G, Flocke SA, Oja-Tebbe N, Stange KC, et al. Patient-physician colorectal cancer screening discussions: delivery of the 5A's in practice. American Journal of Preventive Medicine 2011; 41(5): 480-486.
23. El-Serag HB, Petersen L, Hampel H, Richardson P, Cooper G. The use of screening colonoscopy for patients cared for by the Department of Veterans Affairs. Archives of Internal Medicine 2006; 166(20): 2202-2208.
24. Church TR, Yeazel MW, Jones RM, Kochevar LK, Watt GD, Mongin SJ, et al. A randomized trial of direct mailing of fecal occult blood tests to increase colorectal cancer screening. Journal of the National Cancer Institute 2004; 96(10): 770-780.
25. Fisher JA, Fikry C, Troxel AB. Cutting cost and increasing access to colorectal cancer screening: another approach to following the guidelines. Cancer Epidemiology, Biomarkers & Prevention 2006; 15(1): 108-113.
26. Inadomi JM, Vijan S, Janz NK, Fagerlin A, Thomas JP, Lin YV, et al. Adherence to colorectal cancer screening: a randomized clinical trial of competing strategies. Archives of Internal Medicine 2012; 172(7): 575-582.
27. Terdiman JP. Embarrassment is a major barrier to colon cancer prevention, especially among women: a call to action. Gastroenterology 2006; 130(4): 1364-1365.
28. Consedine NS, Ladwig I, Reddig MK, Broadbent EA. The many faeces of colorectal cancer screening embarrassment: preliminary psychometric development and links to screening outcome. British Journal of Health Psychology 2011; 16(3): 559-579.
29. Farraye FA, Wong M, Hurwitz S, Puleo E, Emmons K, Wallace MB, et al. Barriers to endoscopic colorectal cancer screening: are women different from men? American Journal of Gastroenterology 2004; 99(2): 341-349.
30. Jones RM, Devers KJ, Kuzel AJ, Woolf SH. Patient-reported barriers to colorectal cancer screening: a mixed-methods analysis. American Journal of Preventive Medicine 2010; 38(5): 508-516.
31. Friedemann-Sánchez G, Griffin JM, Partin MR. Gender differences in colorectal cancer screening barriers and information needs. Health Expectations 2007; 10(2): 148-160.
32. Geller BM, Skelly JM, Dorwaldt AL, Howe KD, Dana GS, Flynn BS. Increasing patient/physician communications about colorectal cancer screening in rural primary care practices. Medical Care 2008; 46(9 Suppl 1): S36-S43.
33. Campo S, Askelson NM, Routsong T, Graaf LJ, Losch M, Smith H. The green acres effect: the need for a new colorectal cancer screening campaign tailored to rural audiences. Health Education & Behavior 2008; 35(6): 749-762.
34. Blankenau J, Bailey J, Hudson J. The causes and consequences of the rural uninsured and underinsured. (Online) 2009. Available from: http://files.cfra.org/pdf/Causes-and-Consequences-of-Rural-Uninsured.pdf (Accessed 3 September 2013).
35. Bailey J. The top 10 rural issues for health care reform. (Online) 2009. Available from: http://files.cfra.org/pdf/Ten-Rural-Issues-for-Health-Care-Reform.pdf (Accessed 3 September 2013).
36. Vernon SW, Meissner HI. Evaluating approaches to increase uptake of colorectal cancer screening: lessons learned from pilot studies in diverse primary care settings. Medical Care 2008; 46(9 Suppl 1): S97-S102.


