full article:
The World Health Organization report Increasing access to health workers in remote and rural areas through improved retention: global policy recommendations1 suggests that access to 'well prepared health professionals in sufficient numbers at the right time and right place' is critical to improving health outcomes in rural areas. In addition, Building on values: the future of health care in Canada2 highlights health disparities amongst rural and urban Canadians and cites geography as a determinant of health. In the province of British Columbia (BC), where the research took place, rural residents were generally reported to have higher rates of obesity, traumatic injuries and self-reported disability as compared to their urban counterparts3.
While geography is only one of many factors that contribute to health inequities, access to healthcare services has been cited as disproportionately poorer for rural residents1. In BC, residents of rural communities have identified access to, and the consistency and availability of, healthcare services as critical issues affecting their health4. One example of the impact of health resource shortages is the longstanding unavailability of occupational therapists (OTs) and physical therapists (PTs)5,6, resulting in limited access to and availability of rehabilitation services in rural BC7. This is cause for concern given the critical importance of accessible rehabilitation services for people with a wide range of physical, psychological and cognitive impairments and their associated disabilities, as outlined in clinical practice guidelines8-10.
Improving access to services, however, requires more than just increasing the number of health care providers1. Addressing workforce issues and health care provision in rural areas also requires a sound understanding of rural health, health care practice in rural areas, and the complexity of delivering services in rural areas11. While there is no single definition of 'rural'12,13, 'rurality' describes the combination of specific characteristics of a place including the size of the population, the density of population, access to services, and particular socio-economic variables such as occupation12,14. As noted by Bourke et al., addressing health care in rural areas requires an understanding of rurality and how this affects health11.
Medicine and nursing have long recognized the distinctiveness of providing health care in a rural context15-17. This recognition has assisted these professions to examine health service delivery models and to develop training programs that appropriately prepare physicians and nurses for this unique environment17-19. The scope, skills, knowledge and dimensions of nursing practice in rural, remote and northern communities have been well established20,21 and have resulted in education programs that offer and support these roles19.
In comparison to nursing and medicine, little research has been devoted to how the practice of OTs and PTs is influenced by rurality or the rural context22-24. Many of the features of rural practice such as the diversity of patients, variety of service models, limited resources, poor access to professional development opportunities, high prevalence of chronic diseases and traumatic injuries, and a high proportion of Aboriginal peoples, shape the practice of a range of health professionals. However, the effect of these characteristics on rural rehabilitation practice differs25-27. Nurses and physicians in rural communities characteristically work alongside each other or within a team17, whereas OTs and PTs in rural areas are more likely to work in sole charge positions or in settings such as the community with very few other healthcare professionals24,28. OTs and PTs working in rural areas have been found to practice with a high level of autonomy29. In addition, rural OTs and PTs are described as requiring skills in management and organization29-31, effective communication31, reflective practice31, as well as flexibility to adapt clinical programs to the rural context24.
The relatively small number of healthcare professionals in rural communities results in large caseloads containing a broad spectrum of health conditions27,32. As such, healthcare professionals tend to practice as generalists, routinely working with patients or clients who, in an urban context, would be referred to specialists in areas such as orthopaedics, neurology and cardiac rehabilitation28. Thus, the variety of demands placed upon OTs and PTs in rural areas limits opportunities for specialization22,28,33. Being a generalist in a rural practice requires enhanced skills in problem solving34,35, improvisation, networking35, communication, and management36, as well as a fundamental level of competence across their full scope of practice37. Understanding the influence of rurality on rehabilitation practice in Canada has the potential to inform professional training programs about the key features of rural rehabilitation, thereby assisting in the preparation of OTs and PTs for rural practice.
Much of the literature in the area of rural practice has come from Australia and, while there are some similarities to Canada with respect to geographical size, low population density, and healthcare challenges38, these countries differ in their political and healthcare systems39. As Canada builds its focus on primary health care (PHC), healthcare professions such as occupational therapy and physical therapy are attempting to define their positions in PHC40,41. PHC, as defined by Health Canada, is an approach that recognizes the broader determinants of health including population health, illness prevention and health promotion with services provided through a team approach to care42. This approach has been found to be a particularly appropriate, efficient and effective form of health service delivery in rural areas43. There is growing evidence that the expertise of rehabilitation professionals in the areas of chronic disease management, health promotion and illness prevention, as core dimensions of PHC, makes these professionals essential members of the PHC team44-46. Humphreys and Wakerman advocated for healthcare professionals such as OTs and PTs to play a greater role in the delivery of PHC in rural areas as a means of improving the allocation of scarce resources47.
The overall objective of this research was to construct an understanding of rural rehabilitation practice in the broader context of the current healthcare system. By contributing to a better understanding of rural rehabilitation practice, professional training programs can improve their preparation of graduates for rural practice, and healthcare decision makers can effectively integrate the role of OTs and PTs into PHC, ultimately improving access to rehabilitation services in rural areas and addressing health disparities to improve health outcomes for rural residents.
Researching complex clinical phenomena such as rural healthcare practice to inform education and practice requires a qualitative research method designed to assist with the translation and application of findings and their implications in clinical practice48. Interpretive description was developed by Thorne et al49 to answer research questions about clinical phenomena. The inductive process of exploring meanings and experiences of individuals and integrating these with the collective knowledge of the discipline constructs the contextual nature of clinical phenomena. Using this approach, a purposeful sampling strategy was chosen to ensure a broad range of perspectives. Potential participants were recruited through a letter of invitation mailed to the workplaces of OTs and PTs in rural communities in northern BC. Addresses of work sites were obtained through publically accessible health provider directories and listings. Each letter contained a description of the research project and a copy of the consent form. Potential participants were asked to contact the researcher if they were interested in participating.
OTs and PTs were eligible to participate in the study if they lived and worked in a rural and remote community in BC. For the purposes of this study, 'rural' was defined as communities with a population of fewer than 15 000. This was an adaptation of Statistics Canada's definition of 'rural and small town' which constitutes a population of fewer than 10 00012. The upper limit in the definition of a rural population was increased for the purposes of this study to include OTs and PTs from communities that provide outreach health services to more remote regions, as well as those who work in the private and industrial sectors.
The geographical and political region of northern BC was chosen as the research site because it encompasses two-thirds of the province, or 620 000 km2, but has a population of only 300 000, or less than one-tenth of the provincial population50. It has one metropolitan center with a population of 70 000, and four centers with populations between 10 000 and 18 00050. Thus, a large percentage of the region can be classified as rural. To gain diverse perspectives, participants were selected from a variety of distinct practices, both privately and publicly funded, and a wide range of practice experiences. Data collection took place through face-to-face, in-depth interviews. Conducting the interviews in rural communities upheld the importance of place and its role in developing research relationships, and allowed for the generation of rich data collected within the research context.
A semi-structured interview guide was created in keeping with exploratory research approaches. The interview questions examined experiences, situations, and meanings, and were open-ended to allow participants to share the elements of their practice they considered to be relevant to the focus of the research study. The research questions included: What are the skills you see as being unique to working as an OT/PT in a rural area? What are the barriers you face as an OT/PT in rural practice and what strategies do you employ to address these challenges? How did your professional training support or prepare you for your role as a therapist in a rural community? A pilot interview was conducted to test the question design and sequencing, as well as the procedures for recording the responses. Lessons from this pilot informed the design of the interview guide and subsequent interviews by increasing the clarity of the questions, the addition of demographic data and a question related to the participants' definition of 'rural'.
Due to the small community of health professionals in the region, extreme care was taken to ensure confidentiality of participants and anonymity of the data. Participants were asked to choose a pseudonym, which was used to identify the transcript, and all identifiers were removed from the data. Interviews were transcribed and entered into N-Vivo v9.0 (QSR International; http://www.qsrinternational.com) for analysis. Analysis followed the approach for interpretive description whereby participants' perceptions and experiences of their practice were coded. Using field notes to help provide the context, an inductive approach was then used to cluster the codes into themes. The themes were later collapsed into interpretive categories to capture the complex features of rural practice narrated by participants. Using the research questions as a framework, the findings were then interpreted within the context of existing literature and disciplinary knowledge to determine implications for application in education, research and primary healthcare policy. Interpretations were then returned to participants to elicit feedback and ensure the emerging understanding was grounded in their experiences and understandings of their OT or PT practice in a rural context.
Ethics approval
Ethics approval was obtained from the University of British Columbia Behavioural Research Ethics Board (H09-02742) and from the Northern Health Authority Research and Evaluation Committee (RRC-2009-0038).
A total of 23 letters of invitation were sent to hospitals, clinics, and community agencies, with the potential to reach 42 participants (16 OTs and 36 PTs). Twenty two responses were received. To maximize the variability of the sample, 6 OTs and 13 PTs were selected, from a variety of service delivery models, areas of practice and years of experience in rural practice (Table 1). This represented 37% of OTs and 36% of PTs working in the region that were eligible and invited to participate. Participants provided services to 15 different communities. More than half of the participants had practiced in an urban area for some length of time. Seventeen interviews were conducted face to face in the participant's community and two were conducted by telephone due to logistical constraints of travelling in winter. The duration of the interview ranged from 36 to 94 minutes; the median length was 62 minutes.
From the inductive analysis, it became apparent that a rural context and the aspects of rurality such as geography and access shaped participants' definition of health and influenced how they enacted their practice (Fig1). Participants described specializing in general practice and identified the ways in which they enacted a broader practice by stretching their role within their scope of practice to meet the needs of patients, and participation and partnership as means of providing service. Education was seen as a facilitator of practice, despite access challenges. Reflective practice, networking, and collaboration were deemed essential skills to maintaining competence in a rural area. Rural clinical placements during training, mentoring, and improving access to professional development were regarded as central to recruitment and retention. The ways in which participants enact their practice are embedded within the larger context of the healthcare system with a focus on primary health care.
Table 1: Work profile and demographic characteristics of participants
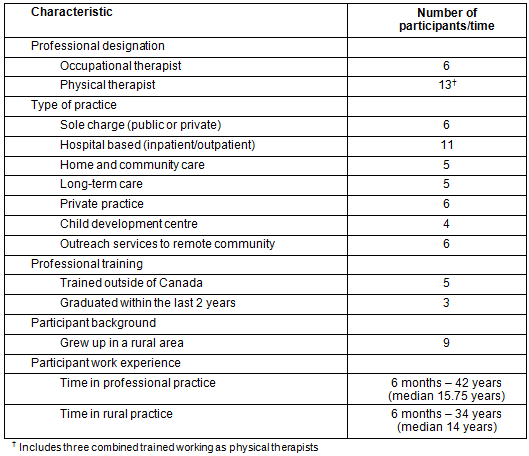
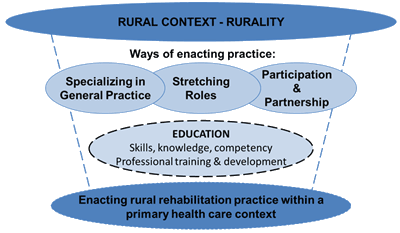 Figure 1: Interpretive categories from analysis.
Figure 1: Interpretive categories from analysis.
Defining health in a rural context - geography and access
Participants described the ways in which the rural context influenced the health of residents and in turn shaped their professional practice. This quote illustrates how the features of geography and access to services intersect, requiring this PT to provide rehabilitation services with restricted resources in a compressed period of time.
I think in the rural setting you've got a lot more people that are living closer to the poverty line where they haven't got the luxury of a benefit package. They can't stay home sick: if the clams are there, they've got to dig them; if the wood's there, they've got to go cut it. If the work's there, they have to take it because they don't know how many weeks they're going to be able to work this year. They haven't got the time to come in on a regular basis ... you may or may not get too many kicks at the can; you've got to, sort of, cover as much ground as you can in as short amount of time as possible. (PT-M)
The rural context shaped rehabilitation practice by broadening the definition that participants had of health and increasing their awareness of the effect that the determinants of health have on their patients:
The context becomes really huge and that sometimes somebody is just struggling with the other things that you don't feel like maybe that's much of what you learned at school to deal with ... it opens your practice up to a bigger definition of health and about social determinants and about wellness. (OT-P)
This larger perspective of health required participants to reach outside their prior conceptualization of practice, or what their professional training had prepared them for. In particular, it required them to adapt their service provision (treatment protocols, clinical practice guidelines, other evidence-based approaches or health service delivery models) to a bigger definition of health:
The one thing that does ring true for rural is you can't take a delivery, a health delivery model, for example, ortho patients that are only in four days and out they go. You cannot take that same model in an urban city, who has home support, has vendors, has flat roads, has good sidewalks, has transit, has [transportation for those requiring assistance], has all these services. (OT-M)
Specializing in generalist practice - equity-oriented care
Participants described how the complexity of working in rural communities results in the tendency to specialize in general practice. The rural practice context required participants to have a broad range of skills to deliver services in multiple settings to a varied caseload covering all areas of practice:
I think in an urban setting my practice would be more focused on one area. Whereas in rural I think in general you are just doing. You just take whatever comes at you and you have a little bit of all of those areas and I don't think in urban settings you would get that variety of experience, and needing to know what to do in all these different situations. (OT-C)
Maintaining a general practice was considered by many participants to be a necessity to ensure the provision of equitable services. They felt that focusing in one area and narrowing their practice would be denying service to others in the community in need. This sense of responsibility for equitable provision of services and social accountability was shared by many participants:
It would be very difficult to maintain a specialty in a rural practice because of the number of demands. Like you would be excluding somebody by doing that. I don't get that luxury of choosing because my conscience pulls me in the direction of 'Look, if you don't see this person, they are not going to see anybody.' (OT-M)
Participants felt that the distinct nature and unique features of their broad practice make this form of general practice more of a specialty:
Having a specialty is also recognizing someone is specialized in that. Being a generalist is also a specialty. (PT-S)
Many of the participants provided services for a wide geographical area and described their caseloads as very large and diverse, requiring a broad range of skills and knowledge from all areas of practice that were applicable across the lifespan. They described needing particularly strong skills in the areas of physical assessment, clinical decision-making, and problem-solving as they were frequently practicing in areas where there was limited access to health care and were treating patients who might not have been seen by another professional. Due to the limited access to healthcare services faced by their patients, participants perceived a sense of responsibility to possess the expertise to identify serious pathology and detect red flags related to medical conditions requiring referral to specialists. Therefore, despite being a generalist, they felt they needed advanced skills in areas such as assessment and differential diagnosis:
I think we have to be better at front line diagnosing and assessing. We certainly come across those things that had to be sent straight to hospital that couldn't wait to go see the family physician, that were life threatening. I guess it could just as easily happen in [a big city] as it could here. Sometimes I think we're a bit more out on our own here, if you are working in the [remote community] and nobody is there, there's no doctor around. If I miss the blood clot and there's no doctor and the nurse doesn't pick it up, well, I should have picked it up. (PT-MJ)
Participants described how the limited resources in rural areas, in particular health human resources, resulted in long waiting lists and the need to prioritize caseloads. Many participants described the personal and professional strain that large caseloads and long waitlists placed on them as a result of limited resources to meet community needs:
I'm having to make pretty tough decisions on how to prioritize the case load, that is overwhelming, because there is no other therapist. ... And I only work two days a week in each place, so I have to prioritize and pick the very, most compromised people, and how do I measure compromise? (PT-M)
Practicing as a generalist also necessitated being critically aware of situations that required resources and knowledge that may extend beyond the normal scope of practice. While all healthcare practitioners are encouraged to be reflective and critically aware, participants emphasized that working in isolation combined with their wide scope of practice presented additional challenges to maintaining competence and standards of practice:
I see that [competency] as becoming more burdensome as time goes on. I feel more challenged because I feel that there's areas that I would like to have more experience and expertise in but the more broad my caseload, the more difficult it is. That becomes a personal challenge to try and define your practice when perhaps your practice is not definable because it is so varied. And that just leads you to a whole host of issues and there's the challenge. (PT-J)
... what we need for continuing competency is those self-reflective skills where you know where you need to learn because you have thought about it. And off you go and find it or do it. (PT-K)
The challenges of maintaining this breadth of skills and knowledge amidst limited resources and fewer colleagues required them to be self-directed, resourceful and to seek out a professional network:
If you're in a rural place, your strive for excellence requires a skill set and a willingness to put yourself out there and to share and to be willing to learn from the resourceful people that you work with. And it's not about the lowest common denominator but it's percolating to see who the doc is that knows about this, who the nurse is who knows about that, what care aid has the experience in this. (PT-R)
Despite the networking and collaboration, another challenge faced by a number of participants was the limited understanding by other healthcare professionals of the scope of practice of PTs and, in particular, OTs. The shortage of health professionals in rural areas appeared to contribute to the limited recognition by other healthcare professionals of the value of rehabilitation and the lack of understanding of the role of OTs. This made it difficult to optimize rehabilitation services in the community:
... actually that's one of the things too about a rural area is that OT's were slower to go into those areas I think. So um, I have a hard time really know[ing] if people know what I do, because I've even recently met one of the doctors [who] just said 'yeah, I don't really know what an OT does', and I was kind of like 'Okay!!'. (OT-J)
The features of rurality, which include a larger definition of health, a broader set of skills, a general breadth of practice, limited access, isolated geography, and limited resources, resulted in OTs and PTs enacting their practice to meet the challenges of a rural context.
Stretching roles for client-centred rural rehabilitation practice
Participants described how the lack of resources and services in rural practice required them to stretch their role and work to their full scope of practice, but not outside it.
By using a broad range of skills in their scope and stretching their role beyond the normal expectations of the professions, participants felt that they could offer effective services and avoid denying services to patients in need:
I'm always battling that fine line of not overstepping and going beyond my scope but also not saying, 'Oh no, not me.' Like, 'That's not my responsibility' because I don't think that's effective therapy if every time you come against something you wouldn't be asked to do in a larger city, you say, 'Oh sorry, not OT practice. You've got to find someone else.' So you have a wider range of skills that you need if you choose to do that. (OT-M)
Stretching of roles also reflected a means of addressing the gaps in care that exist in many rural communities. In particular, this occurred in communities where there was only one OT or PT, and to seek the services of the other profession, patients would be required to travel long distances:
So as much as you will never sell yourself as a physio, you can't ignore that's something that maybe that patient needs ... how do you kind of also support that to happen and stretch your role a little bit to do all those things you never thought. (OT-P)
Participants were cautious in describing how they stretched their role, appearing to be cognizant of the boundaries of their scope of practice.
Although the role is primarily, obviously, PT, I think that I had to sort of adapt and, if you will, play at being other things, whether it was play at being somewhat OT focused or social work focused, counsellor focused. And not trying to sort of suggest that I was any of those things, but that ... with some experience you know how far you can go into those roles without stepping outside your own comfort zone or stepping inappropriately into one of those roles beyond your scope, beyond your experience. (PT-H)
Some of the PT participants expressed the desire to see their scope of practice increased due to the shortage of resources in rural areas and the need to increase efficiencies:
I don't think that our scope would have to expand tremendously but just a few basics. Because often times, we are suggesting that someone have an x-ray, or refer to the orthopaedic surgeon, then it just seems to be a waste of resources to have to refer back to the physician whose workload is that high. (PT-A)
Scope of practice issues were much more difficult for new graduates to grasp. They sought the experience and advice of more advanced practitioners and learnt skills that enabled them to draw boundaries around their practice and to recognize their own level of competence.
Despite the challenges, participants noted that the autonomy of rural practice, the breadth of their practice and the ways in which they stretched their roles comprised significant rewards of rural practice:
I think that my career has been as varied and as rewarding because I've had to stretch. I've had to stretch. I've had to respond out of my comfort zone. I've had to be challenged. (PT-R)
Participation and partnerships
The participants of this study described how their professional practice was shaped by the rural context and resulted in a rehabilitation practice that was characterized by participation in the broad health of individuals and in the community and a greater emphasis on inter-personal relationships within the community as much as it was oriented towards rehabilitation. Participation in an individual's health required the combination of understanding the context of an individual within their community:
I suppose the aspect of rural practice that does makes it different is that it is likely that you know the bigger picture of the person's life style and life and environment so there may be the sense more of being able to know where you are starting and where you are heading, what your goal is because the chances are that you will see them through the whole process, ... you will see them again, so what you do, will come back at you one way or the other. It would give you a sense of participation, more participation possibly in that person's life ... (PT-H)
Knowing individuals, the community and the context of practice led to enacting practice through active participation in the community, building relationships and partnerships with individuals and the community at large:
You are part of community and it's about supporting a community towards health and social determinants of health and supporting people to get community things happening for the family, like preserving of salmon and doing the smokehouse. So if it's supporting them to have that capacity to be fulfilling those huge roles that they play in community, then that's going a long ways towards managing their chronic disease. (OT-P)
Together these features offered an opportunity to provide seamless care and preventative services as well as enhancing health outcomes:
I take care [of] all areas in the community. There is a continuity of care for the person. Follow up is really good as compared to [the big city]. Back there, they have to do lots of referrals. 'Okay, I am done with this client. It's your turn.' You can arrange to see the person at home or arrange to do an out-patient basis or sometimes I even request a client to go to the acute care for admission. (OT-B)
Participants acknowledged that these practice skills were acquired over time and experience in a rural setting. However, they noted that they also need to be taught during the training of OTs and PTs and also through continuing professional development.
Access to continuing professional development
All participants noted that one of the greatest challenges to practicing in a rural area was the limited access to local opportunities for continuing professional development (CPD). Participants indicated that they shared a similar lack of access to that of clients in the context of their own professional development. Most CPD courses and workshops took place in urban areas which resulted in significant time away from work and expense associated with travelling:
The travel costs are always involved and that more than doubles the cost of the education because you have to travel. (OT-C)
Participants identified limited access to CPD and funding for CPD as barriers to attracting and retaining therapists to work in rural areas. They offered recommendations such as placements and mentorship to improve preparation for rural practice. A formal mentoring program that matched similar setting and learning style was noted as a way of assisting new graduates and those new to rural areas to meet the challenges of generalist and rural practice:
[I would recommend] that there's a strong basic mentoring system ... they get their own personal network of folks that they can contact almost like, in my view, like a branch phone out system that, 'okay, my first go-to person is here'. (PT-R)
Through the analysis of participants' perceptions and experiences, it became evident that the practice of OTs and PTs in a rural context was more than rehabilitation in a rural setting. Participants described how the rural environment and the geographical distance influenced the health of their patients, requiring them to consider the determinants of health as part of their assessment and treatment. It was also noted that the geographical features of rural areas created barriers to accessing care and resources. This complex web of geography and access were the defining features of how participants understood the impact of the rural context on their professional practice51. The complexity of the rural context has been identified in the literature27 and is reflected in the struggle to define 'rural' as an entity12,13,52-54. The findings of this study illustrate the importance of a place-specific definition of 'rural' as a starting point for understanding rural rehabilitation practice, which aligns with Williams and Cutchin's commentary on the need to focus on the contextual references to 'rural' rather than seeking a universally understood definition55.
Beyond the significance of context, the findings from this study expand knowledge of rural rehabilitation practice; specifically, the concept of specialist generalist and stretching their roles to provide relatively equal services. The rural healthcare literature frequently uses the terms 'specialized generalist' and 'generalist expertise' to describe health professionals delivering care in rural areas24,56. Participants in this research study preferred to be seen as generalists57, while conversely considering rural practice to be a specialty. They expounded the necessity of maintaining a broad expertise26 to meet the needs of a diverse caseload and cover areas of practice that might otherwise be reserved for a specialist58. The participants in this study expressed what appeared to be a moral responsibility, or moral agency59, to provide services equitably to all residents in the community. Desire to serve community needs has been shown as a common trait of rural practitioners60-62.
Participants in this study described stretching their skills and knowledge as necessary to meet the needs of the population who had limited access to healthcare services. Stretching of roles required participants to recognize the boundaries of their practice and the areas that overlapped with other professions. It became clear that the practice of OTs and PTs in a rural area with limited resources required the ability and capacity to work to full scope of practice. This required participants to take the initiative to develop the skills (such as advanced assessment skills) and networks necessary, and demanded a solid understanding of professional boundaries. Minisini et al noted that the challenge associated with practicing within scope but outside of competence resulted in a lower self-efficacy58. While participants reflected on the challenges of maintaining their competence in general practice, self-efficacy was not assessed.
Most participants explicitly noted the importance of reflective practice to increase their critical awareness and judgement to delineate professional scope and boundaries, and assess their competence. In a study of the attributes of allied health professionals in the Northern Territory, Australia, Thomas and Clark identified learning from mistakes and being a reflective learner and practitioner as necessary skills for professional practice31.
Participating in the community to better health and partnering with patients and community as means of delivering rehabilitation practice could be considered an example of community development as outlined in Battye and McTaggart's model of remote health service delivery63. It is consistent with the concept of understanding and valuing the culture that is considered a foundation of rural practice27,31,64. The importance of addressing the determinants of health as part of rural rehabilitation practice illustrates the overlap of rural rehabilitation practice with primary health care47,65, an area requiring greater exploration.
Consistent with the literature, one of the most significant challenges to rural practice faced by participants was limited access to continuing professional development24,36,57,61,66,67. However, this prompted participants to be more resourceful and seek out networks and mentorship57 where available. This reinforces the need to advocate for formal mentorship programs to increase peer support and for increased access to CPD. Participants noted that rural clinical education was an important aspect of preparing for rural practice and aiding in recruitment33,68,69.
Collaboration is often considered essential to rural practice as a means to mitigate resource shortages70 and allowing professionals the capacity to work to their full scope of practice43. Role clarification has been determined a core competency in interprofessional collaborative practice71. OTs in this study noted that other health disciplines did not have a clear understanding of what OTs do. Devine reported similar findings amongst OTs working in rural Australia29. The need for OTs to communicate their expertise to the public and to other professionals is addressed in a position paper on the role of OTs in PHC in Manitoba72.
The importance of collaboration prompted participants to recommend interprofessional education in training programs. Interprofessional education offers an ideal medium in which to teach content relevant to rural practice including health promotion, disease prevention, cultural safety, self-management, and team-based care33. Exposure to rural interprofessional learning opportunities73-75 and positive rural learning experiences have shown to result in improved rural recruitment and retention35,57,73.
The findings of this study provide examples of how the rural context influenced the practice of OTs and PTs. It illustrates how the participants in this study enacted their practice as generalists to provide equity-oriented care, and overcame challenges inherent in the rural context through stretching their roles in response to health human resource and health services shortages, working to the full extent of their scope of practice, and participating and partnering with the population they were serving.
Limitations of this research
Rigour in qualitative research analysis is enhanced by multiple readings and more than one person conducting the analysis76. One potential limitation of this research may be that the analysis was conducted by a single researcher who is a practicing PT. Conducting the analysis in collaboration with an OT with experience in rural practice would offer additional perspectives and add depth to the analysis.
An additional evaluative criteria used in qualitative research is the transferability of research77,78. . Many of the insights described in this study are specific to rehabilitation professionals working in their rural context; however, some of the challenges faced by these participants, in particular access to continuing professional development, may be applicable to other professionals working in rural and remote areas. Consequently the findings may be limited to the particular social, economic, cultural, and political features specific to the communities where participants lived and worked.
Implications for this research
The exploration of each of the interpretive categories that emerged from the data analysis (rural context, general practice as a specialty, stretching roles, participation and partnership), have helped to develop a deeper understanding of rural rehabilitation practice. The findings of this study have led to a number of recommendations which have implications for rehabilitation education, practice, and policy.
The findings illustrate the importance of curricular content in professional training programs that address the rural context. This may include greater emphasis on the determinants of health, inequities created through barriers to access, features of rural life that shape health, increased rural practice education placements and support for a rural rehabilitation education pathway from training programs through to CPD.
The implications for practice include greater recognition from other OTs and PTs that rural practice is a specialty that requires practicing to full scope with enhanced skills in areas to meet the demands of the rural context. While access to resources is limited, a number of strategies such as collaboration and partnering in the community were cited as strategies to overcome the challenges. From the perspective of policy and planning, this research offers an understanding of the breadth of the roles of OTs and PTs within healthcare teams that can enhance collaborative practice and the recognition and support to enable practitioners to practice to the full extent of their scope. This study adds depth to understanding how OTs and PTs enact their professional practice in rural areas and highlights the challenges and the rewards of rural rehabilitation practice.
References
1. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention: global policy recommendations. (Online) 2010. Available: http://whqlibdoc.who.int/publications/2010/9789241564014_eng.pdf (Accessed 28 October 2010).
2. Romanow RJ. Building on values: the future of health care in Canada. Ottawa: Privy Council, 2002.
3. Sorensen M, dePeuter J. Rural British Columbia: a ten year census analysis (1991-2001). Ottawa: Rural Secretariat, 2002.
4. Wong S, Regan S. Patient perspectives on primary health care in rural communities: effects of geography on access, continuity and efficiency. Rural and Remote Health 9: 1142. (Online) 2009. Available: www.rrh.org.au (Accessed 19 March 2009).
5. Canadian Institute for Health Information. Workforce trends of physiotherapists in Canada, 2007. Ottawa: CIHI, 2008.
6. Canadian Institute for Health Information. Workforce trends of occupational therapists in Canada, 2007. Ottawa: CIHI, 2008.
7. Northern Health Authority. Northern health rehabilitation strategy 2008-2012. Prince George, BC: Northern Health Authority, 2008.
8. Physician Working Group on Rehabilitation Services. Conversation on health: improving rehabilitation services for the people of British Columbia. Vancouver, BC: Government of British Columbia, 2007; 11.
9. American College of Rheumatology. Guidelines for the management of osteoarthritis Arthritis and Rheumatology 2000; 43(9): 1905-1915.
10. American College of Rheumatology Subcommittee on Rheumatoid Arthritis. Guidelines for the management of rheumatoid arthritis: 2002 update. Arthritis and Rheumatology 2002; 46: 328-346.
11. Bourke L, Humphreys JS, Wakerman J, Taylor L. Charting the future course of rural health and remote health in Australia: why we need theory. Australian Journal of Rural Health 2010; 18(2): 54-58.
12. du Plessis V, Beshiri R, Bollman R, Clemenson H. Definitions of rural. In: RD Bollman (Ed.). Rural and Small Town Canada Analysis Bulletin. Agriculture Division of Statistics Canada, 2001; 17.
13. Pitblado JR. So what do we mean by rural, remote and northern? Canadian Journal of Nursing Research 2005; 37(1): 163-168.
14. Muula AS. How do we define 'rurality' in the teaching on medical demography? Rural and Remote Health 7: 653. (Online) 2007. Available: www.rrh.org.au (Accessed 23 April 2009).
15. Curran V, Rourke J. The role of medical education in the recruitment and retention of rural physicians. Medical Teacher 2004; 26: 265-272.
16. Howie L. Contextualized nursing practice. In: J. Ross (Ed.). Rural nursing: aspects of practice. Dunedin, NZ: Rural Health Opportunities, Ministry of Health; 2008; 33-49.
17. Lee HJ, Winters CA. Rural Nursing: Concepts, Theory and Practice, 2 edn. New York: Springer, 2006.
18. Ross J. Rural nursing: aspects of practice. Dunedin, NZ: Rural Health Opportunities, Ministry of Health, 2008.
19. MacLeod MLP, Kulig JC, Stewart NJ, Pitblado JR, Banks K, D'Arcy C, et al. The nature of nursing practice in rural and remote Canada. Ottawa, ON: Canadian Health Services Research Foundation, 2004.
20. Mahnken JE. Rural nursing and health care reforms: building a social model of health. Rural and Remote Health 1(1): 104. (Online) 2001. Available: www.rrh.org.au (Accessed 30 July 2010).
21. Tarlier DS, Johnson JL, Whyte NB. Voices from the wilderness. Canadian Journal of Public Health 2003; 94(3): 180-185.
22. Struber JC. Recruiting and retaining allied health professionals in rural Australia: why is it so difficult? Internet Journal of Allied Health Sciences & Practice 2004; 2(2): 1-13.
23. Williams E, D'Amore W, McMeeken J. Physiotherapy in rural and regional Australia. Australian Journal of Rural Health 2007; 15(6): 380-386.
24. Bent A. Allied health in central Australia: challenges and rewards in remote area practice. Australian Journal of Physiotherapy 1999; 45: 203-212.
25. Sheppard L. Delivery of health services in rural and remote Australia. Internet Journal of Allied Health Sciences & Practice 3(4): (Online) 2005. Available: http://ijahsp.nova.edu/articles/vol3num4/sheppard.htm (Accessed 10 November 2008).
26. Sheppard L, Neilsen I. Rural and remote physiotherapy: its own discipline. Australian Journal of Physiotherapy 2005; 13(5): 135-136.
27. Bourke L, Sheridan C, Russell U, Jones G, DeWitt D, Liaw ST. Developing a conceptual understanding of rural health practice. Australian Journal of Rural Health 2004; 12(5): 181-186.
28. Sheppard L. Work practices of rural and remote physiotherapists. Australian Journal of Rural Health 2001; 9(2): 84-90.
29. Devine S. Perceptions of occupational therapists practising in rural Australia: a graduate perspective. Australian Occupational Therapy Journal 2006; 53(3): 205-210.
30. Boshoff K, Hartshorne S. Profile of occupational therapy practice in rural and remote South Australia. Australian Journal of Rural Health 2008; 16(5): 255-261.
31. Thomas Y, Clark M. The aptitudes of allied health professionals working in remote communities. International Journal of Therapy & Rehabilitation 2007; 14(5): 216-220.
32. Wakerman J, Humphreys JS, Wells RW, Kuipers P, Entwistle P, Jones J. Improving rural and remote health. Medical Journal of Australia 2007; 186(9): 486.
33. University of Melbourne. Relations and rewards are key strategies in recruitment and retention of rural physiotherapists. Part of a review for the Victorian Department of Human Services. (Online) 2005. Available: http://www.physioth.unimelb.edu.au/ruralphysio/downloads/DHS_Review2005.pdf (Accessed 16 October 2009).
34. Kohler E, Mayberry W. A comparison of practice issues among occupational therapists in the rural northwest and the rocky mountain regions. The American Journal of Occupational Therapy 1993; 47(8): 5.
35. Lee S, MacKenzie L. Starting out in rural New South Wales: the experiences of new graduate occupational therapists. Australian Journal of Rural Health 2003; 11: 36-43.
36. Mills A, Millsteed J. Retention: an unresolved workforce issue affecting rural occupational therapy services. Australian Occupational Therapy Journal 2002; 49(4): 170-181.
37. Services for Australian Rural and Remote Health (SARRAH). Transitions to rural practice - skills and competencies. (Online) 2009. Available: http://www.sarrahtraining.com.au (Accessed 17 August 2009).
38. Pong RW, DesMeules M, Lagacé C. Rural-urban disparities in health: how does Canada fare and how does Canada compare with Australia? Australian Journal of Rural Health 2009; 17(1): 58-64.
39. Lagace C, Desmeules M, Pong R, Heng D. Non-communicable disease and injury related mortality in rural and urban places of residence: a comparison between Canada and Australia. Canadian Journal of Public Health 2007; 98(Suppl 1): S62-S69.
40. Canadian Physiotherapy Association. Primary health care position statement. Toronto: Canadian Physiotherapy Association, 2009; 2.
41. Canadian Association of Occupational Therapists. Occupational therapy and primary health care. CAOT position statement. (Online) 2006. Available: http://www.caot.ca/default.asp?ChangeID=188&pageID=188 (Accessed 09 February 2009).
42. Health Canada. What is primary health care? (Online) 2010. Available: http://www.hc-sc.gc.ca/hcs-sss/prim/about-apropos-eng.php (Accessed 15 May 2010).
43. Wakerman J. Innovative rural and remote primary health care models: what do we know and what are the research priorities? Australian Journal of Rural Health 2009; 17: 21-26.
44. Nova Scotia Physiotherapy Advisory Group. Integrating physiotherapy in the primary health care model in Nova Scotia: an economic solution. Halifax: NSPAG, 2007.
45. Richardson J, Letts L, Chan D, Stratford P, Hand C, Price D, et al. Rehabilitation in a primary care setting for persons with chronic illness - a randomiz, ed controlled trial. Primary Health Care Research & Development 2010; 11(4): 382-395.
46. Jones RC, Copper S, Riley O, Dobbs F. A pilot study of pulmonary rehabilitation in primary care. British Journal of General Practice 2002; 52(480): 2.
47. Humphreys JS, Wakerman J. Primary health care in rural and remote Australia: achieving equity of access and outcomes through national reform. Discussion paper. (Online) 2009. Available: http://www.health.gov.au/internet/nhhrc/publishing.nsf (Accessed 21 September 2010).
48. Thorne S. Interpretive description. Walnut Creek, California: Left Coast Press, 2008.
49. Thorne S, Reimer Kirkham S, Macdonald-Emes J. Interpretive description: a noncategorical qualitative alternative for developing nursing knowledge. Research in Nursing and Health 1997; 20: 169-177.
50. BC Statistics. Socio-economic profiles health authorities. (Online) 2007. Available: http://www.bcstats.gov.bc.ca/data/sep/ha/ha_5.pdf (Accessed 27 September 2010).
51. Miller Mifflin T, Bzdell M. Development of a physiotherapy prioritization tool in the Baffin Region of Nunavut: a remote, under-serviced area in the Canadian Arctic. Rural and Remote Health 10: 1466. (Online) 2010. Available: www.rrh.org.au (Accessed 30 June 2010).
52. Humphreys JS. Delimiting 'rural': implications of an agreed 'rurality index' for health care planning and resource allocation. Australian Journal of Rural Health 1998; 6(4): 212-216.
53. Leduc E. Defining rurality: a general practice rurality index for Canada. Canadian Journal of Rural Medicine 1997; 2(2). (Online) 1997. Available: http://www.cma.ca/index.php?ci_id=37774&la_id=1 (Accessed 8 November 2009).
54. Rourke J. In search of a definition of 'rural'. Canadian Journal of Rural Medicine 1997; 2(3): 125. (Online) 1997. Available: http://www.cma.ca/index.php?ci_id=37774&la_id=1 (Accessed 29 October 2008).
55. Williams AM, Cutchin MP. The rural context of health care provision. Journal of Interprofessional Care 2002; 16(2): 107-115.
56. Stagnetti K. Occupational therapy practice in rural and remote South Australia. Australian Journal of Rural Health 2008; 16(5): 253-254.
57. Wielandt PM, Taylor E. Understanding rural practice: implications for occupational therapy education in Canada. Rural and Remote Health 10 1488. (Online) 2010. Available: www.rrh.org.au (Accessed 22 September 2010).
58. Minisini M, Sheppard L, Jones A. Self-efficacy beliefs and confidence of rural physiotherapists to undertake specialist pediatric caseloads: a pediatric example. Rural and Remote Health. 10: 1426. (Online) 2010. (Accessed 2 November 2010).
59. Edwards I, Delany CM, Townsend AF, Swisher LL. Moral agency as enacted justice: a clinical and ethical decision-making framework for responding to health inequities and social injustice. Physical Therapy 2011; 91(11): 1653-1663.
60. Daniels ZM, Vanleit BJ, Skipper BJ, Sanders ML, Rhyne RL. Factors in recruiting and retaining health professionals for rural practice. Journal of Rural Health. 2007; 23(1): 62-71.
61. Keane S, Lincoln M, Rolfe M, Smith T. Retention of the rural allied health workforce in New South Wales: a comparison of public and private practitioners. BMC Health Services Research 13: 32. (Online) 2013. Available: http://www.biomedcentral.com/1472-6963/13/32 (Accessed 1 July 2010).
62. Manahan CM, Hardy CL, MacLeod MLP. Personal characteristics and experiences of long term allied health professionals in rural and northern British Columbia. Rural and Remote Health 9: 1238. (Online) 2009. Available: www.rrh.org.au (Accessed 30 November 2009).
63. Battye KM, McTaggart K. Development of a model for sustainable delivery of outreach allied health services to remote north-west Queensland, Australia. Rural and Remote Health 3: 194. (Online) 2003. Available: www.rrh.org.au (Accessed 29 October 2008).
64. Farmer J, Bourke L, Taylor J, Marley JV, Reid J, Bracksley S, et al. Culture and rural health. Australian Journal of Rural Health. 2012; 20(5): 243-247.
65. Fricke M. Physiotherapy and primary health care: evolving opportunities. Winnipeg: Manitoba Branch of the Canadian Physiotherapy Association, College of Physiotherapists of Manitoba, Department of Physical Therapy, School of Medical Rehabilitation, University of Manitoba, 2005; 62.
66. Steenbergen K, Mackenzie L. Professional support in rural New South Wales: perceptions of new graduate occupational therapists. Australian Journal of Rural Health 2004; 12(4): 160-165.
67. Roots RK, Li LC. Recruitment and retention of occupational therapists and physiotherapists in rural regions: a meta-synthesis. BMC Health Services Research 13: 59. (Online) 2013. Available: http://www.biomedcentral.com/1472-6963/13/59 (Accessed 12 February 2013).
68. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Australian Journal of Rural Health 2006; 14(1): 14-19.
69. Solomon P, Salvatori PS, Berry SC. Perceptions of important retention and recruitment factors by therapists in Northwestern Ontario. Journal of Rural Health 2001; 17: 278-285.
70. Boone M, Minore B, Katt M, Kinch P. Strength through sharing: interdisciplinary teamwork in providing health and social services to northern native communities. Canadian Journal of Community Mental Health 1997; 16(2): 15-28.
71. Canadian Interprofessional Health Collaborative. A national interprofessional competency framework. Vancouver: College of Heath Disciplines, 2010.
72. Leclair L, Restall G, Edwards J, Cooper J, Stern M, Soltys P, et al. Occupational therapists and primary health care. Winnipeg: Manitoba Society of Occupational Therapists (undated).
73. McNair R, Brown R, Stone N, Sims J. Rural interprofessional education: promoting teamwork in primary health care education and practice. Australian Journal of Rural Health 2001; 9(Supplement): 19-26.
74. McNair R, Stone N, Sims J, Curtis C. Australian evidence for interprofessional education contributing to effective teamwork preparation and interest in rural practice. Journal of Interprofessional Care 2005; 19(6): 579-594.
75. Charles G, Bainbridge L, Copeman-Stewart K, Art ST, Kassam R. The Interprofessional Rural Program of British Columbia (IRPbc). Journal of Interprofessional Care 2006; 20(1): 40-50.
76. Creswell JW. Research design: qualitative, quantitative, and mixed methods appproaches, 3rd edn. Thousand Oaks, CA: Sage, 2009.
77. Morse JM, Barrett M, Mayan M, Olson K, Spiers J. Verification strategies for establishing reliability and validity in qualitative research. International Journal of Qualitative Methods 2002; 1(2): 13-19.
78. Lincoln YS, Guba EG. Naturalistic inquiry. Beverley Hills, CA: Sage, 1985.



