The mental health of Aboriginal adolescents is a well-documented priority in Canada1-3. Overall, Aboriginal children and adolescents in Canada endure difficult living conditions and experience poorer health outcomes compared to the Canadian population4-7. There are many factors identified that contribute to this situation including a history of colonialism that led to disadvantage via the social determinants of health8,9. The Aboriginal population in Canada comprises First Nations, Inuit, and Métis, who represent 4.3%10 of the Canadian population, and 10% of the population in north-eastern Ontario11. The Aboriginal population in Canada is growing four times faster than the non-Aboriginal population, resulting in communities with increasing numbers of children and youth10.
The term Aboriginal is used in this paper to reflect a broader international perspective, although this study refers primarily to one First Nations reserve community in Canada. Only First Nations people in Canada live on reserves. Many children from Aboriginal communities reach their teen years with uncertainty about their cultural identity, few proximal opportunities for advancement, and a sense of hopelessness about their future6,12. Youth suicide rates13,14 and incident rates of mental illness2,6 are higher in Aboriginal populations in Canada, compared to non-Aboriginal populations. These factors have led to a concern about the mental health of Aboriginal adolescents in Canada. Developing resilience and a sense of identity is particularly important, and it has been identified as a strategic objective for mental health promotion initiatives for Aboriginal and First Nations youth3,12,14-16. There is also a need to promote mental health and resilience within many other Aboriginal or Indigenous populations in other nations17-19.
Aboriginal health and promotion initiatives in Canada are often grounded in a holistic circular view of health and life7, and the Medicine Wheel is one framework that is used by many Aboriginal communities across the country20. However, it is not the only framework used: each community has a unique cultural heritage. Nevertheless, the Medicine Wheel has been used to guide the development of a wide variety of programs and initiatives because it reflects an inter-connected worldview. The Medicine Wheel usually includes the four dimensions of health: physical (body), mental (mind), emotional (heart), and spiritual (spirit)21,22. It represents a holistic view of health that is in harmony with the individual, the community, and the natural world21,23,24. This worldview helps many Aboriginal people to embrace life as an interconnected experience that is difficult to separate into component parts because each aspect of life has some influence on another aspect8,21,23. For instance, the health of an individual has an impact on the health of a community and the natural world25, and an individual's mental health has an impact on their physical, emotional, and spiritual health23.
Many Canadian First Nations communities have connected their health with their cultural heritage through the re-introduction of historical ceremonies, traditional practices, and a promotion of the Good Life23,26. This reconnection process has included many diverse programs and interventions that are developed through government agencies, helping organizations, and by communities themselves. The First Nations and Inuit Health Branch (FNIHB) of Health Canada has developed several mental health-related programs such as the Indian Residential Schools Mental Health Support Program, the National Native Alcohol and Drug Abuse Program, the National Aboriginal Youth Suicide Prevention Strategy, and the Brighter Futures and Building Healthy Communities program27.
Most First Nations communities receive funding from Health Canada to develop relevant local initiatives for their on-reserve populations. Often, there is very little evidence reported on the efficacy of these programs. The primary purpose of this study was to evaluate the impact of a culturally relevant Outdoor Adventure Leadership Experience (OALE) on the resilience and well-being of adolescents from Wikwemikong Unceded Indian Reserve in north-eastern Ontario.
Outdoor adventure as a therapeutic intervention
A growing body of evidence suggests that outdoor adventure28-30 and wilderness therapy31,32 programs have potential as a mental health intervention for adolescents33-36. Gass, Gillis, and Russell32 summarized the findings from nine literature reviews and six meta-analyses completed in outdoor adventure and wilderness therapy. Their summary highlighted varied program models and outcomes identified in the literature. However, they concluded that these types of programs and interventions resulted in two broad outcome areas based on findings reported in most studies: positive and significant development of self-concept; and the development of adaptive and social skills due to the unique group-based treatment milieu32. The theoretical foundations of outdoor adventure and wilderness therapy programs is often traced back to the Outward Bound Process Model32,37. Despite the mounting evidence in non-Aboriginal populations, there is a paucity of evidence related to the effectiveness of outdoor programming in Aboriginal populations. There is also a dearth of published research on how to design, implement, and evaluate these programs. Nevertheless, outdoor and land-based programming is prevalent in many Aboriginal communities, and it holds promise as a culturally relevant health promotion modality for Aboriginal adolescents on reserves3,38. Takano aptly described examples of several land-based programs within a few Aboriginal communities in Canada39. These programs had many unique elements, but a common theme was that they reflected a deep bonding or connecting process with the land39.
Community leaders from Wikwemikong collaborated with university researchers - primarily from Laurentian University in Sudbury, Ontario, Canada - to develop and implement the OALE intervention. The OALE is a 10-day intensive program involving a wilderness canoe expedition homeward through the traditional territory of Wikwemikong. The Medicine Wheel20-22 and the Outward Bound Process Model32,37 were used as developmental frameworks40. The Outward Bound Process Model illustrates how a participant achieves positive change and personal growth by progressing through a series of challenges in a supportive small group environment where successive problems are addressed, solved, and then reorganized into learnings that may transfer to life beyond the outdoor experience37.
The OALE included many natural challenges such as rapids, portages, navigation, and open-water crossings. Participants were assigned day leadership responsibilities, and the experience included a half-day solo component. Group discussions and talking circles41,42 occurred each night around a campfire, and other program components were interwoven into the routine of the travel day. Program staff and guides from Wikwemikong facilitated the experience, mentored the youth participants, and implemented program elements as needed and when appropriate. Hence, although the process and context of the OALE was culturally unique, it was also similar in some ways to other non-Aboriginal wilderness travel programs that adhered to the Outward Bound Process Model. More details of the program have been published elsewhere43,44.
Early in the development of the program, the collaborative research team realized the importance of empirically measuring outcomes of the OALE intervention as an objective evaluation of its effectiveness. The team believed that measuring effectiveness at two different time periods after the intervention would quantify both the magnitude and sustainability of any impact. Understanding some of the other intervening factors between the time periods would provide important contextual factors that may have influenced outcome scores. This would provide credible data that would help improve the program and help secure continued funding for the program into the future.
Resilience and wellbeing
The OALE was designed to promote resilience and wellbeing. There are many varied theories and definitions of resilience in the literature45,46; however, Wagnild's simple operational definition of resilience was selected: 'the ability to successfully cope with change or misfortune'(p. 15)47 because it is focused on the individual; and it also informed the development of the measure of resilience used in this study. Others have offered definitions that are sensitive to culture and context48,49 and include family, environment, and community factors50-52. For the purpose of this paper, wellbeing is defined as the combined inclusive nature of holistic health as it is reflected by the four dimensions of the Medicine Wheel20. The Medicine Wheel is also the preferred framework to use for health promotion initiatives in Wikwemikong.
One primary and two exploratory research questions were addressed in this study: (1) Does the OALE promote resilience and wellbeing for Wikwemikong adolescents? (2a) Are results sustainable for 1 year after the OALE? and (2b) What are some intervening factors that may explain changes in results 1 year after the OALE?
The collaborative research team originally sought measurement scales that were developed specifically for Aboriginal adolescents. While there were a plethora of scales from mainstream North American populations, no measures of resilience or mental wellbeing had been developed for Aboriginal adolescents. The team selected a scale to assess resilience as the primary outcome, and also selected several brief scales that reflected the four dimensions of health (physical, mental, emotional, and spiritual) from the Medicine Wheel framework. These were reviewed and approved by the community to ensure that they were appropriate for use in the community. The review (evaluation process and criteria used) is described in detail in the methods section.
The project was conducted by a collaborative research team comprising health leaders from Wikwemikong Unceded Indian Reserve and academic researchers, primarily from Laurentian University. A mixed-method design43,53 was used to evaluate the impact of the OALE program on the resilience of adolescents from the Wikwemikong Unceded Indian Reserve in northern Ontario, Canada. In particular, this study used a concurrent embedded strategy whereby the quantitative approach guided the project, and the embedded qualitative approach provided a supplemental explanatory purpose53.
Population and sample
Wikwemikong is a relatively large First Nation encompassing 413 km2 in the Georgian Bay area of Lake Huron54. The on-reserve population is 259254, and most people live in several village areas on the main part of the reserve on the east end of Manitoulin Island55. This reserve is located 170 km from the nearest large urban center (Sudbury) and delivers its own educational and healthcare programs. The target population of adolescents 12-18 years living on reserve in Wikwemikong was estimated at approximately 45043. OALE participants were recruited through various promotional campaigns coordinated by the Waasa Naabin Community Youth Services Centre. Adolescents for a comparison group were recruited from a summer youth employment program in the community. There was no cost for the adolescents to participate, and they were pre-screened for physical and mental health issues prior to inclusion in the sample43. Over a 2-year data collection period, 73 adolescents participated in the OALE, and 8 repeated the experience. The program and study involved six separate excursions (three each summer), with most excursions including two separate travel groups for a total of 11 distinct travel groups. Other details about the OALE program and sample have been described in a previous publication43.
Questionnaire measures
A comprehensive survey package, comprising various scales that measured resilience and wellbeing, was compiled into a Health and Well-Being Questionnaire (HWBQ). A local Community Research Steering Committee (CRSC) in Wikwemikong provided oversight and guidance through all phases of the research and the development of the survey package, including the review and selection of all scales and questions included. The CRSC included two adolescent representatives. There were numerous iterations of and changes to the survey package over several months, before the final version of the HWBQ was complete. Early in the process, the CRSC concluded that an examination of resilience and mental health could not be completed without also examining other aspects of wellbeing based on the interconnected holistic view of health represented by the Medicine Wheel. The HWBQ consisted of seven distinct scales:
- 14-item Resilience Scale (RS-14)47
- Mental Component Score (MCS) from the SF-12v256
- Physical Component Score (PCS) from the SF-12v256
- Scale of Positive and Negative Emotion - Balance (SPANE)57
- Flourishing Scale (FS)57
- Self-Esteem Scale (SES)58-60
- Satisfaction with Life Scale (SWL)61.
Several other items (questions) from other sources were also included. The selection criteria, adaptation, and justification for use of these scales and items are provided below.
Six main criteria were used by the CRSC for the selection and inclusion of each scale:
- evidence of strong psychometric properties (reliability and validity)
- track record of support and use with Aboriginal youth populations (with normed data if available)
- sensitivity to short-term changes
- positively measured and reinforced health and wellness rather than illness and dysfunction
- support and use within outdoor adventure contexts
- appropriate and acceptable to the community.
None of the scales in the final version of the HWBQ met all of these criteria, and none had been developed or normed within an Aboriginal adolescent population. Nevertheless, the CRSC evaluated and selected the most appropriate scales that were to be included, and the final version of the HWBQ package of scales was approved for use in the community. The HWBQ was pilot tested with the CRSC, and then reviewed with a small group of non-Aboriginal adolescents in the target age range. Item #4 of the RS-14, 'I usually take things in stride', was not understood well by these adolescents, so after discussion with scale developer, Gail Wagnild, it was changed to: 'I don't let things upset me for long.'
After a detailed review of the literature, resilience was identified as the primary construct of interest. Ahern, Kiehl, Sole, and Byers completed a comprehensive review of the literature for measures of resilience appropriate for adolescent populations62. From their findings, they concluded that the 25-item Resilience Scale (RS-25) developed by Wagnild and Young63 was the best instrument to use with adolescent populations. The RS-25 had strong psychometric properties, and it had been used in a variety of populations including different cultures (Russian, Mexican, Irish, Australian) and contexts including young adults, adolescents, adolescent mothers, and homeless adolescents. The RS-25 was the most common resilience scale used to assess outdoor adventure programs in non-Aboriginal contexts64-69. The original version of the RS contained 25 items and exploratory factor analysis, with data from an outdoor context67, supported a scale with 10 fewer items loading on only one factor. In January 2009, Wagnild released a 14-item version (RS-14) of the RS. From the strong psychometric properties, long history of use, conclusions of Ahern and colleagues62, acceptance within Wikwemikong, and application within several outdoor adventure contexts, the RS-14 was deemed the most appropriate primary outcome measure.
A secondary (confirmatory) scale was selected to measure overall mental health to verify the primary analysis. This confirmatory scale was the MCS, which is the mental health subscale from the SF-12v256. The SF-12v2 is a generic global health measure that is one of a suite of measures (including SF-36v2 and SF-8TM) designed to assess physical and mental health70. These measures are among the most prevalent tools for assessing self-reported health70,71. They have been used in thousands of studies in many different nations and cultures70. The SF-12v2 is a shorter version (12 questions) of the SF-36v2 that is purported to be very robust and appropriate for use when combined in large questionnaire packages that include other measurement scales56.
Beyond the RS-14 and MCS, five additional scales (PCS, SPANE, FS, SES, SWL) were included in the HWBQ as supportive measures to assess the four dimensions of health and wellbeing. The HWBQ also included selected items (questions) from two additional aspects of wellbeing, social support (SS) and spiritual values (SV), from the Canadian Community Health Survey60. Four additional questions related to community values (CV) were included from the Child and Youth Resilience Measure72. The final version of the HWBQ package was approved for use in the community by the CRSC. It was designed to include short scales and questions that reflected the four dimensions of health and wellbeing from the Medicine Wheel without imposing undue burden on adolescent respondents. A total of 78 items were included in the HWBQ, and this included six items measuring demographic variables and self-reported mental health. Table 1 summarizes the scales that were included in the questionnaire package, along with the corresponding dimension of health assessed.
Open-ended structured questions were appended to a second version of the HWBQ that was administered one year after the OALE. These questions were designed to identify to what extent participants attributed changes in their resilience and wellbeing scores to the OALE or other intervening factors in the 12-month period following the end of the OALE intervention.
Table 1: Scales and dimensions of the Health and Well-Being Questionnaire

Data collection
The HWBQ was administered initially 1 day before the OALE (T1) and 1 month after the OALE (T2). The HWBQ was also administered at two similar time periods to a comparison group of adolescents from Wikwemikong who did not participate in the OALE. The HWBQ was administered 1 year after the OALE (T3) in order to explore the sustainability of changes over time. Collecting data at T3, and including other wellbeing scales beyond the RS-14 (as recommended by the CRSC), was on a confirmatory and exploratory basis only. The open-ended structured questions were only appended to the HWBQ at T3.
Ethics approval
Ethics approval for this study was obtained from the Laurentian University Research Ethics Board (approval number 2009-03-03-R5) and the Manitoulin Anishinabek Research Review Committee. Informed consent and assent was obtained for all participants. The study was approved in the Wikwemikong community by the Health Services Committee and Chief and Council.
Analysis
The primary hypothesis was that resilience would improve from T1 to T2. Thus, a priori sample size calculations (paired-sample t-test) using the RS-14 were completed using the G*Power v3.0.1 analytical software (http://www.gpower.hhu.de/en.html). This yielded a minimum sample size requirement of n=44 (based on effect size=0.50, power=0.90, p=0.05). A sample size of 44 was achievable in Wikwemikong; however, it was recognized that this would restrict the number of analyses that could be performed. Thus, sample size was also a limitation of the study, which is discussed later in the article.
Responses from the HWBQ were entered into Microsoft Excel v14, and the data entry error rate was assessed. Summary scores were computed in Excel, with the exception of the SF-12v2 scales that were computed by the QualityMetric Health Outcomes Scoring Software v4.0 (QualityMetric; http://www.qualitymetric.com). All quantitative analyses were completed using the Statistical Package for the Social Sciences v19.0 (SPSS Inc.; http://www.spss.com). Each scale included in the HWBQ was examined graphically for kurtosis and skewness, and using the Kolmogorov-Smirnov statistic to assess the degree of normality of the distribution73.
Resilience, using the RS-14, was assessed by comparing scores from T2 to baseline (T1). The MCS scores were analyzed to confirm any changes, given resilience is a construct of mental health. The RS-14 change scores from the participant group were also interpreted within the context of the change scores from the comparison group. Analyses of all other scales over the three time periods were exploratory due to the small sample size and large number of dependent variables. Effect sizes (ES) were calculated using Hedges' g74 and were interpreted based on Cohen's suggested standard benchmarks for interpreting ESs as small (0.2), medium (0.5), and large (0.8)75.
Qualitative data were analyzed using NVivo v9.0 (QSR International; http://www.qsrinternational.com/products_nvivo.aspx), based on responses to the open-ended questions at T3. Content was analyzed inductively and coded to thematic concepts76. The intent of this analysis was to provide context for the interpretation of the primary quantitative analysis in order to determine if there were any intervening factors that helped explain any changes in resilience.
There were 73 adolescents who participated in the OALE over two summers, and 61 (83.6%) completed the full HWBQ package at T1 and then completed the 10-day OALE experience. Only one youth was excluded from participation prior to the commencement of the OALE due to a physical health concern, and two other youth were excluded for minor physical health issues that developed during the excursion and prevented them from completing the OALE. Participants ranged in age from 11.9 to 18.7 years with a mean age of 14.6, and 64.4% (n=38) were male. Less than half (42.4%; n=25) of all participants lived in a family situation with both parents. No participants self-identified as non-Aboriginal. Further descriptive details about the sample have been published elsewhere43. There were 47 (64.4%) adolescents who completed the HWBQ approximately 1 month after the OALE (T2), and 33 (45.2%) who completed the HWBQ approximately 1 year later (T3).
Normality of scale score distributions was confirmed by histograms, boxplots, and use of the Kolmogorov-Smirnov statistic73. Two cases were found to contain outliers on multiple scales, and they were removed from all analyses to enhance normality for the RS-14, the MCS, and three other scales (SE, FS, and SWL). Their removal did not affect directionality or significance of results. Thus 59 participants (80.8%) were included in the primary analysis at T1. The HWBQ was also administered to a comparison group of 31 adolescents from Wikwemikong who did not participate in the OALE. This was originally intended to be a comparison group over a similar time period as the experimental group (T1 to T2); however, only nine complete data sets were received (T1 and T2).
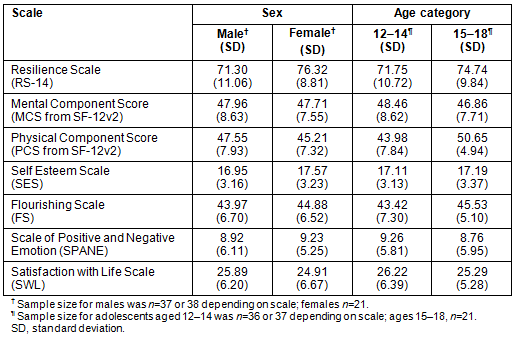
The HWBQ included seven scales, and Table 2 portrays the mean scores of each of the seven measures at baseline (T1) with the internal consistency of each scale. Table 3 depicts scale scores at baseline by sex and age category.
Table 2: Scale score means and reliability at baseline (T1)
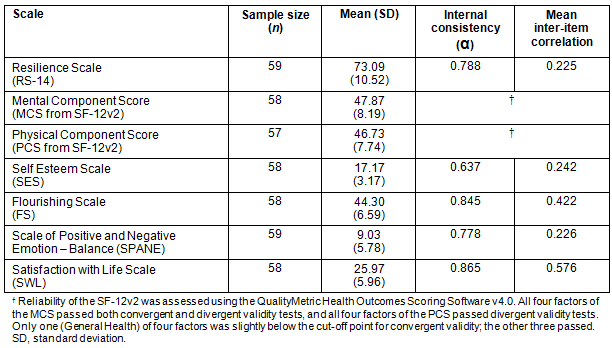 Table 3: Mean scale scores by sex and age category at baseline (T1)
Table 3: Mean scale scores by sex and age category at baseline (T1)
This study was designed a priori to assess changes (T2-T1) in resilience as the primary outcome measure. A paired-samples t-test was conducted to evaluate the impact of the OALE intervention on participants' resilience scores (RS-14) from baseline (T1) (1 day pre-intervention), to T2 (1 month post-intervention). This resulted in 46 matched pairs between T1 and T2. There was a statistically significant increase in resilience scores from T1 (mean=73.65, standard deviation (SD)=9.78) to T2 (mean=77.05, SD=9.07), t(45)=-2.64, p=0.011 (two-tailed). The mean increase in resilience was 3.40 (95% confidence interval (CI) 0.81-5.98). Hedge's g indicated a small to medium effect size (ES=0.36).
The change scores (T2-T1) for the OALE participants (n=46) were also interpreted in the context of the change scores for a comparison group from Wikwemikong (15-20 years) who did not participate in the OALE; however, only 9 complete data sets were received (T1 and T2). There was a notable difference in resilience change (Δ) scores for the OALE participants (mean Δ=3.39, SD=8.70) and comparison group (mean Δ=-16.05, SD=22.65). The magnitude of the difference in scores (mean Δ=19.44) was very large (ES=1.63).
The HWBQ was also administered 1 year post-intervention (T3) to explore whether any changes in resilience were stable over time. There were 33 matched pairs between T1 and T3, and the change in resilience was very small (mean Δ=0.34, ES=0.03). Assessing mental health via the MCS was designed to confirm any noted changes in resilience. The mean MCS score increased over the three time periods, and the mean change from T3 to T1 was small to medium (mean Δ=3.57, ES=0.40). Figure 1 displays the change score analysis and confidence intervals for the RS-14 and MCS over the three different time periods. Both resilience and mental health scores improved from T1 to T2; however, there was a divergence of results at T3. Mental health scores continued to improve at T3 compared to T2 and T1; however, resilience scores at T3 were lower compared to T2, reverting back to a level similar to the original pre-OALE score at T1.
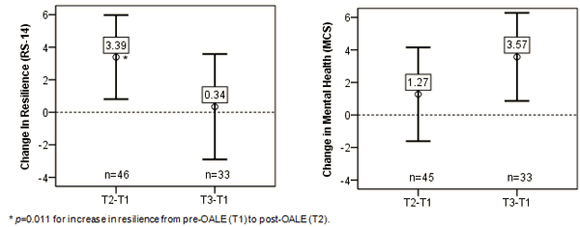 Figure 1: Change in resilience and mental health over three different time periods.
Figure 1: Change in resilience and mental health over three different time periods.
Figure 2 displays an exploratory subgroup analysis of resilience by sex and age category. There seemed to be a trend towards more pronounced effects for younger males (ages 12-14 years) from T1 to T2. However, this figure must be interpreted with caution due to small sample sizes. Most participants seemed to revert back to pre-OALE levels of resilience 1 year after completing the program (T3).
The results presented thus far suggest that the OALE had an important short-term effect on resilience. No inference testing was completed with the other wellbeing scales; however, the data were examined for observable trends in order to explore possible changes in other dimensions of wellbeing. Figure 3 depicts these trends over time for the six additional scales from the HWBQ. All six scales showed a positive change from T1 to T2, with this trend remaining at T3 for mental health (MCS), balance of emotion (SPANE), and satisfaction with life (SWL).
The individual items (questions) relating to social support, spiritual values, and community values were each combined to provide a summary score for each construct. These constructs appeared to behave as scales since internal consistency (social support: α=0.865; spiritual values: α=0.774; community values: α=0.743) and mean inter-item correlations (social support: inter-item correlation (IIC)=0.480; spiritual values: IIC=0.462; community values: IIC=0.434) were similar to the established scales in Table 2. Figure 4 portrays changes over the three time periods for social support, spiritual values, and community values. The trends were very similar to the scales portrayed in Figure 3. All outcomes improved at T2, but there were varied results at T3, with some scales decreasing.
There were 33 adolescents who completed the HWBQ at T3 and 26 (78.8%) who responded to the open-ended questions appended to the questionnaire. These questions were designed for self-reflection, but also to probe for other intervening factors that may have contributed to any changes in resilience and mental health over the 12-month period after completion of the OALE. Most respondents indicated that the experience was beneficial for personal growth (gaining independence, interacting with others, learning skills, persevering, and contributing to success at school) with comments such as, 'I am more independent and able to take care of myself', 'it helped with leadership and group work', and 'I do my homework now, and complete work that has to be done.' No respondents reported that the OALE was detrimental in any way.
A number of intervening factors were identified that may have contributed to changes in resilience and wellbeing. There were numerous comments related to other events in the broader community that may have had an impact on the resilience and mental health of the youth participants over the year following the OALE. Six comments described recent fatalities that seemed to have a negative impact, and several comments related to life stressors (eg school projects) and bad influences (friends) that led to bad choices (eg consuming alcohol). On the other hand, there were five comments describing community and school programs (other than the OALE) that had a positive impact. The most common intervening factor related to changes in family and living situation. Many adolescents described significant events in the stability of their home life related to moving, changes in family membership (eg cousins moving in or out), and relationships between family members. A few of these comments were favorable, such as 'new home contributes to my ideal life.' However, many of the comments described unfavorable circumstances such as 'my family recently got into a fight and so I moved somewhere else for a while to figure things out.' Most of the intervening factors seemed to be unrelated to the OALE; however, one adolescent related a benefit of the OALE (perseverance) directly to an intervening factor:
On the OALE, 2nd day through the trip, I wanted to give up and go home. I was sore, tired, cold, and just wanted to go home. But I stuck through with it to the end. With relation to my uncle's passing I did exactly that. I stuck through and was strong about it and tried not to let it effect [sic] my life somewhat.
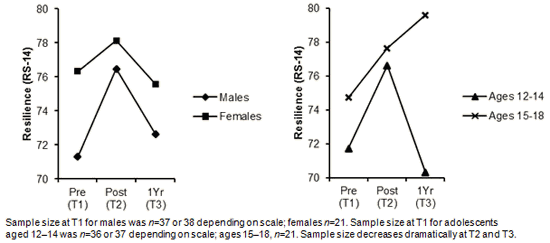 Figure 2: Change in resilience by sex and age group.
Figure 2: Change in resilience by sex and age group.
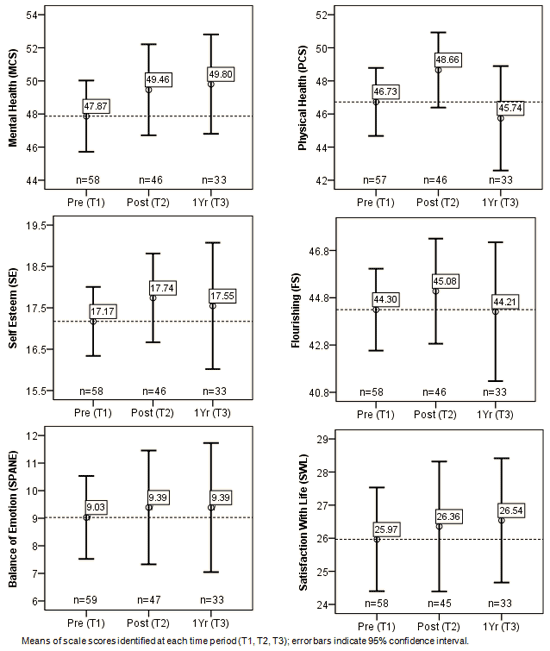 Figure 3: Scale score changes over three different time periods.
Figure 3: Scale score changes over three different time periods.
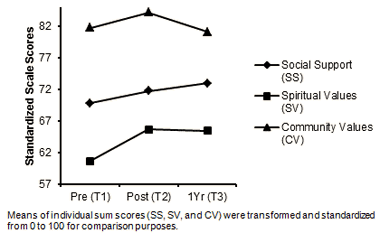 Figure 4: Social support, spiritual values and community values over three different time periods.
Figure 4: Social support, spiritual values and community values over three different time periods.
Discussion
This study demonstrated that the OALE was successful in promoting resilience over the short-term (T1 to T2). This finding was consistent with many other outdoor-related studies assessing resilience as an outcome variable in non-Aboriginal populations65-68,77-80. However, it is important to note that there were also several outdoor related studies assessing resilience that did not find statistically significant improvements64,69,81.
Wagnild suggested norms for the RS-14 were a mean of 84.4 (SD=10.2) with low resilience scores identified as 62.6 (SD=8.04) and high resilience scores identified as 94.4 (SD=2.69)47. The OALE scores at T1 had a mean of 73.65 (SD=9.78) and this increased to a mean of 77.05 (SD=9.07) at T2. Resilience scores for the OALE participants were below the norm, demonstrating low to medium resilience. The reported ES (0.36) for resilience in the OALE study was also very similar to that reported by three previous meta-analysis of outdoor adventure program outcomes (ES range=0.31-0.38)28-30. The short-term improvement in resilience identified in this study was also confirmed by qualitative results analyzed during an earlier phase of the study43.
Other studies using the RS have measured resilience immediately following the outdoor programs at T2. Researchers of outdoor program effectiveness often administer outcome measures on the last day of the program because it is more convenient and response rates are likely to be higher. However, the assessment of resilience at T2 in this study was delayed until 1 month following the experience, to avoid post-group euphoria (PGE). Marsh and colleagues coined the term PGE to describe the potential for inflated scores when outcome measures are administered immediately following the end of an impactful outdoor program82. This study was designed to avoid PGE to ensure that the youth participants were back in their home environment and well adjusted to their usual living circumstances when they completed the HWBQ following the experience. However, the lower number of respondents at T2 (n=46) reflected the challenges of tracking a dispersed group of Aboriginal participants a month later.
Results from the secondary analyses indicated a somewhat perplexing trend when the resilience scores were compared to the mental health scores. Resilience scores improved significantly between T1 and T2, but then reverted back to pre-test levels at 12 months post (T3). Conversely, mental health scores continued to improve over the three time periods. Although perplexing in this study, the RS-14 and MCS scores at T3 reflect a similar trend in other outcome studies assessing the impact of outdoor adventure experiences. The RS-14 pattern from T1 to T2 is consistent with other adventure therapy research with adolescents, which consistently demonstrates favorable outcomes for global mental health measures32-36. However, the long-term sustainability (~T3) of these outcomes is less consistent.
In adventure therapy studies involving youth at risk, both Russell83 and Harper et al84 included a 12-month post assessment using behavioral and mental health constructs. Post-test scores were higher than pre-test scores, but there was some variability in subscale scores at the 12-month post assessment83,84. The use of follow-up aftercare and support for some of the youth in these studies83,84 helped explain the positive changes in some scales over the year. In the meta-analysis of outdoor adventure programs completed by Hattie et al30, the authors found that there was an average additional increase (ES=0.17) at the 1 year post-test point compared to the post-test point immediately following the programs' completion. This suggests that improvements were not only maintained, but also improved over time. There were 96 studies included in this meta-analysis, reflecting a wide variety of adventure education programs both with and without aftercare. In comparison, the OALE results in this study were mixed, suggesting that there were intervening factors that may have impacted adolescent judgments on their self-reported scores for resilience and mental health.
The qualitative results helped to explain some of these intervening factors. Nearly all of the participants who responded to the open-ended questions at T3 (n=26) directly acknowledged that the OALE was beneficial. Yet, many of them also identified major changes in their life circumstances. The most significant comments related to changes in family living situation. In some ways, this is not surprising given that only 37.5% of the respondents at T3 reported living with both parents. Instability in family living situation is one of the most common determinants of health identified in the literature for Aboriginal populations6-8. Hence, involving families in future OALE experiences is an opportunity worth exploring.
Researchers involved in evaluating adventure therapy programs have highlighted the importance of follow-up or aftercare systems that involve participants after the initial immersive outdoor experience has been completed84,85. Introducing post-OALE programming is a future opportunity worth exploring, especially for younger males (ages 12-14), because their resilience scores decreased more dramatically from T2 to T3 (Fig2). One must exercise caution however, because the small sample size for subgroups at T3 presented difficulties in interpreting other observable differences, such as the continued increase in resilience for participants 15-18 years (n=12).
All of the HWBQ scales performed relatively well in this study as evidenced by internal consistency and mean inter-item correlations (Table 2). These scores were similar to those published by the original scale developers. Beyond resilience, every other wellbeing construct score measured in this study (mental and physical health, flourishing, balance of emotion, satisfaction with life, self-esteem, social support, community and spiritual values) demonstrated elevated scores 1 month after completion of the program (T2). The mean scores for these scales provide a unique glimpse into the self-reported health of adolescents from one First Nations reserve.
Limitations
There were several limitations to this study. The relatively small sample size available for analysis restricted the number of variables and factors that could be examined. As a result, it was not possible to adjust for demographic characteristics such as age and gender. To address this limitation, resilience was identified a priori as the primary construct (factor) examined, which was confirmed by results from a broader evaluation of mental health using the MCS. Other potential limitations related to lack of randomization, low response rates from the comparison group, and potential for sample selection bias. Study recruitment is a known challenge in this population. Nevertheless, given the small population size (N=450) of adolescents 12-18 years, it was remarkable that 59 (13.1%) available data sets were obtained at T1. Further, the ES from RS-14 change scores from T1 to T2 was evident and statistically significant. Despite the small population, it is important to note that Wikwemikong is one of the largest First Nations reserves in Ontario.
The scales included in the HWBQ were sourced from non-Aboriginal contexts, and primarily for adult populations. The results would have been strengthened by the inclusion of a measure designed for Aboriginal youth. Because the research primarily involved only one community, it is important to encourage replication of this intervention in other Aboriginal communities, to assess the generalizability of the results. It is important to note that these findings and focus on self-reported health from one First Nations community is rare in comparison to the availability of similar data for other First Nations communities. In fact, there is a compelling need to disaggregate data to provide information sources that support local decision-making within specific Aboriginal communities86.
The OALE program had a positive impact on resilience for adolescents in Wikwemikong, over the short term. Intermediate reinforcement programs are recommended to sustain benefits over time since the OALE was a summer program that was difficult to maintain through the school year. Inter-sectorial planning across departments (ie health, education, and justice) within Wikwemikong may lead to innovative ways to revise and expand the OALE, with the goal of retaining benefits and reaching specific subgroups (younger children, families, men only, and women only) and other specific clinical populations in the community.
Outcome scores from seven different wellbeing scales provide a unique glimpse into the self-reported health and wellbeing for adolescents within one First Nations community in Canada. The RS-14 seemed to function well, and is recommended for use in studies with other Aboriginal adolescent populations. However, none of the scales (including the RS-14) in the HWBQ package was developed for use with Aboriginal populations. This project identified a pressing need to develop culturally appropriate measures of health for Aboriginal children and youth in Canada. These measures could then be used to evaluate culturally appropriate programming to inform local health planning. This work has now begun87. The success and effectiveness of the OALE in Wikwemikong is encouraging. More empirical studies are required to address whether the OALE (or similar outdoor-type interventions) may be effective within other First Nations communities.
Acknowledgements
The authors would like to extend their appreciation to leaders, staff, and participants in Wikwemikong who donated their valuable time and expertise to collaborate on the development, implementation and evaluation of the OALE. In particular, they would like to acknowledge efforts of the staff at the Waasa Naabin Community Youth Services Centre, for their role in implementing and sustaining the OALE program. Rita G. Corbiere is a community Elder who was instrumental in providing oversight, support, and guidance throughout the project. Dr Brenda Restoule is a clinical psychologist who has supported the development of the project since inception. Funding for the development and implementation of the OALE came primarily through the Brighter Futures and Building Healthy Communities program from the First Nations, Inuit and Aboriginal Health Branch of Health Canada (http://www.hc-sc.gc.ca/ahc-asc/branch-dirgen/fnihb-dgspni/index-eng.php). The OALE project also received financial support from the Indigenous Health Research Development Program (http://www.ihrdp.ca) which is funded through the Canadian Institute of Health Research (http://www.cihr-irsc.gc.ca/e)‎, and resource support from the ECHO (Evaluating Children's Health Outcomes) Research Centre (http://www.echoresearchcentre.com) of Laurentian University. Nancy Young is supported by a Canada Research Chair.
References
1. Dumont-Smith C. The health status of Canada's First Nations, Métis and Inuit peoples (A background paper to accompany 'Health care renewal in Canada: accelerating change'). Toronto, ON: Health Council of Canada, 2005.
2. Government of Canada. The human face of mental health and mental illness in Canada. Ottawa, ON: Public Health Agency of Canada, 2006.
3. Mental Health Commission of Canada. Changing directions, changing lives: the mental health strategy for Canada. Calgary, AB: MHCC, 2012.
4. Canadian UNICEF Committee. Canadian supplement to the state of the world's children. Aboriginal children's health: leaving no child behind. Report no. 0-921564038-4. Toronto, ON: UNICEF Canada, 2009.
5. Health Canada. A statistical profile on the health of First Nations in Canada for the year 2000. Ottawa, ON: Her Majesty the Queen in Right of Canada, 2005.
6. National Collaborating Centre for Aboriginal Health. State of knowledge of Aboriginal health: a review of Aboriginal public health in Canada. Prince George, BC: NCCAH, 2012.
7. The First Nations Information Governance Centre. First Nations regional health survey (RHS) phase 2 (2008/10) national report on adults, youth and children living in First Nations communities. Ottawa, ON: FNIGC, 2012.
8. Loppie-Reading C, Wien F. Health inequalities and social determinants of Aboriginal peoples' health. Prince George, BC: National Collaborating Centre for Aboriginal Health, 2009.
9. Nelson S. Challenging hidden assumptions: colonial norms as determinants of Aboriginal mental health. Prince George, BC: National Collaborating Centre for Aboriginal Health, 2012.
10. Statistics Canada. Aboriginal peoples in Canada: First Nations people, Métis and Inuit. National Household Survey 2011. Analytic document - catalogue no. 99-011-x2011001. Ottawa, ON: Ministry of Industry, 2013.
11. Northeastern Ontario Local Health Integration Network. NE LHIN Aboriginal/First Nation and Métis mental health and addictions framework. North Bay, ON: NE LHIN, 2011.
12. Kirmayer LJ, Simpson C, Cargo M. Healing traditions: culture, community and mental health promotion with Canadian Aboriginal peoples. Australasian Psychiatry 2003; 11(Supplement): S15-S23.
13. Canadian Institute of Child Health. The health of Canada's children: a CICH profile. 3rd edn. Ottawa, ON: CICH, 2000.
14. Kirmayer LJ, Brass GM, Holton T, Paul K, Simpson C, Tait C. Suicide among Aboriginal people in Canada. Ottawa, ON: Aboriginal Healing Foundation, 2007.
15. First Nations Inuit and Aboriginal Health. Acting on what we know: preventing youth suicide in First Nations. The report of the Advisory Group on Suicide Prevention. Ottawa, ON: Health Canada, 2003.
16. Gibson N, LaBoucane-Benson PE. Aboriginal youth resilience research in Canada. [Special issue.] Pimatisiwin 2008; 6(2): 1-208.
17. Hunter E, Harvey D. Indigenous suicide in Australia, New Zealand, Canada and the United States. Emergency Medicine 2002; 14(1): 14-23.
18. Durie M, Milroy H, Hunter E. Mental health and the indigenous people of Australia and New Zealand. In: LJ Kirmayer, GG Valaskakis (Eds). Healing traditions: the mental health of Aboriginal people in Canada. Vancouver, BC: UBC Press, 2009; 36-55.
19. Purdie N, Dudgeon P, Walker R (Eds). Working together: Aboriginal and Torres Strait Islander mental health and wellbeing principles and practice. Barton, ACT: Australian Government Department of Health and Ageing (Commonwealth of Australia), 2010.
20. Waldram JB, Herring DA, Young TK. Aboriginal health in Canada: historical, cultural, and epidemiological perspectives. 2nd edn. Toronto, ON: University of Toronto Press, 2006.
21. Hill DL. Sense of belonging as connectedness, American Indian worldview, and mental health. Psychiatric Nursing 2006; 20(5): 210-216.
22. Isaak CA, Marchessault G. Meaning of health: the perspectives of Aboriginal adults and youth in a northern Manitoba First Nations community. Canadian Journal of Diabetes 2008; 32(2): 114-122.
23. Hart MA. Seeking mino-pimatasiwin (the good life): an Aboriginal approach to social work practice. Native Social Work Journal 2000; 2(1): 91-112.
24. Hunter LM, Logan J, Goulet J-G, Barton S. Aboriginal healing: regaining balance and culture. Journal of Transcultural Nursing 2006; 17(1): 13-22.
25. Parkes MW. Ecohealth and Aboriginal health: a review of common ground. Prince George, BC: National Collaborating Centre for Aboriginal Health, 2011.
26. Rheault DAI. Anishinaabe Mino-Bimaadiziwin (the way of a Good Life). Master's thesis. Peterborough, ON: Trent University, 1998.
27. First Nations Inuit and Aboriginal Health Branch. First Nations and Inuit health program compendium 2011-12. Ottawa, ON: Health Canada, 2012.
28. Cason DR, Gillis HL. A meta-analysis of outdoor adventure programming with adolescents. Journal of Experiential Education 1994; 17(1): 40-47.
29. Hans TA. A meta-analysis of the effects of adventure programming on locus of control. Journal of Contemporary Psychotherapy 2000; 30(1): 33-60.
30. Hattie J, Marsh HW, Neill JT, Richards GE. Adventure education and Outward Bound: out-of-class experiences that make a lasting difference. Review of Educational Research 1997; 67(1): 43-87.
31. Baker D. The effects of adventure and wilderness therapy: a meta-analytic review. Master's thesis. Townsville, QLD: James Cook University, 2011.
32. Gass MA, Gillis HL, Russell KC. Adventure therapy: theory, research, and practice. New York: Routledge, 2012.
33. Bedard RM, Rosen L, Vacha-Haase T. Wilderness therapy programs for juvenile delinquents: a meta-analysis. Journal of Therapeutic Wilderness Camping 2003; 3(1): 7-13.
34. Davis-Berman J, Berman DS. The promise of wilderness therapy. Boulder, CO: Association of Expertiential Education, 2008.
35. Marsh PE. What does camp do for kids? A meta-analysis of the influence of organized camping experience on the self constructs of youth. Bloomington, IN: Indiana University, 1999.
36. Wilson SJ, Lipsey MW. Wilderness challenge programs for delinquent youth: a meta-analysis of outcome evaluations. Evaluation and Program Planning 2000; 23(1): 1-12.
37. Walsh V, Golins G. The exploration of the Outward Bound process. Denver, CO: Colorado Outward Bound. Unpublished manuscript. 1976.
38. Disant M-J, Hébert C, Bergeron O, Bruneau S. PopHealth Notes, Issue 4: 'Aboriginal youth and social inequalities in health.' Montreal, QC: Quebec Population Health Research Network, 2008.
39. Takano T. Bonding with the land: outdoor environmental education programmes and their cultural contexts. PhD thesis. Edinburgh, UK: University of Edinburgh, 2004.
40. Ritchie SD, Enosse L, Peltier J. Frameworks for adventure: the Outward Bound process and the Medicine Wheel. Pathways: The Ontario Journal of Outdoor , Educ, ation 2013; 25(3): 12-14.
41. Fleischhacker S, Vu M, Ries A, McPhail A. Engaging tribal leaders in an American Indian healthy eating project through modified talking circles. Family & Community Health 2011; 34(3): 202-210.
42. Running Wolf P, Rickard JA. Talking circles: a Native American approach to experiential learning. Journal of Multicultural Counseling and Development 2003; 31(1): 39-43.
43. Ritchie SD, Wabano MJ, Schinke R, Peltier D, Restoule B, Russell K, et al. The Aboriginal youth resilience study: a look at promoting resilience and well-being through outdoor adventure leadership experience. In: A Prior, C Carpenter, CL Norton, J Kirchner (Eds). Emerging insights: proceedings of the 5th International Adventure Therapy Conference 2009. Prague: European Science and Art Publishing, 2012; 145-161.
44. Ritchie SD, Wabano MJ, Young N, Schinke R, Peltier D, Battochio R, et al. Developing a culturally relevant outdoor leadership training program for Aboriginal youth. Journal of Experiential Education 2010; 32(3): 300-304.
45. Fergus S, Zimmerman MA. Adolescent resilience: a framework for understanding healthy development in the face of risk. Annual Review of Public Health 2005; 26(1): 399-419.
46. Rutter M. Resilience concepts and findings: implications for family therapy. Journal of Family Therapy 1999; 21(2): 119-144.
47. Wagnild GM. The Resilience Scale user's guide for the US English version of the Resilience Scale and the 14-Item Resilience Scale. Worden, MT: The Resilience Center, 2009.
48. Kirmayer LJ, Dandeneau S, Marshall E, Phillips MK, Williamson KJ. Rethinking resilience from indigenous perspectives. Canadian Journal of Psychiatry 2011; 56(2): 84-91.
49. Ungar M. Nurturing hidden resilience in at-risk youth in different cultures. Journal of Canadian Academy of Child and Adolescent Psychiatry 2006; 15(2): 53-58.
50. Ahern NR. Adolescent resilience: an evolutionary concept analysis. Journal of Pediatric Nursing 2006; 21(3): 175-185.
51. Olsson CA, Bond L, Burns JM, Vella-Brodrick DA, Sawyer SM. Adolescent resilience: a concept analysis. Journal of Adolescence 2003; 26(1): 1-11.
52. Wright MO, Masten AS. Resilience processes in development. In: S Goldstein, RB Brooks (Eds). Handbook of resilience in children. New York, NY: Springer, 2006; 17-37.
53. Creswell JW. Research design: qualitative, quantitative, and mixed-method approaches. 3rd edn. Los Angeles, CA: Sage Publications, 2009.
54. Statistics Canada. Wikwemikong Unceded, Ontario (code3551043) (table). 2011 Census Profile. Statistics Canada catalogue no. 98-316-XWE. Ottawa, ON: Statistics Canada, 2012.
55. Jacklin K. Diversity within: deconstructing Aboriginal community health in Wikwemikong Unceded Indian Reserve. Social Science & Medicine 2009; 68(5): 980-989.
56. Ware JE, Kosinski M, Turner-Bowker DM, Gandek B. User's manual for the SF-12v2® Health Survey (with a supplement documenting the SF-12® Health Survey). Lincoln, RI: QualityMetric Incorporated, 2002.
57. Diener E, Wirtz D, Tov W, Kim-Prieto C, Choi D-W, Oishi S, et al. New well-being measures: short scales to assess flourishing and positive and negative feelings. Social Indicators Research 2010; 97(2): 143-156.
58. Rosenberg M. Society and the adolescent self-image. Princeton, NJ: Princeton University Press, 1965.
59. Pearlin LI, Schooler C. The structure of coping. Journal of Health and Social Behavior 1978; 19(1): 2-21.
60. Statistics Canada. Canadian community health survey, cycle 4.1 - 2007. Ottawa, ON: Statistics Canada, 2007.
61. Diener E, Emmons RA, Larsen RJ, Griffin S. The Satisfaction with Life Scale. Journal of Personality Assessment 1985; 49(1): 71-75.
62. Ahern NR, Kiehl EM, Sole ML, Byers J. A review of instruments measuring resilience. Issues in Comprehensive Pediatric Nursing 2006; 29(2): 103-125.
63. Wagnild GM, Young HM. Development and psychometric evaluation of the Resilience Scale. Journal of Nursing Measurement 1993; 1(2): 165-178.
64. Ewert A, Yoshino A. A preliminary exploration of the influence of short-term adventure-based expeditions on levels of resilience. Journal of Experiential Education 2008; 30(3): 262-266.
65. Gillespie E, Allen-Craig S. The enhancement of resilience via a wilderness therapy program: a preliminary investigation. Australian Journal of Outdoor Education 2009; 13(1): 39-49.
66. Luvas EL. Resilience and youth-at-risk: challenge courses as interventions. Master's thesis. Chico, CA: California State University, 2010.
67. Neill JT, Dias KL. Adventure education and resilience: the double-edged sword. Journal of Adventure Education and Outdoor Learning 2001; 1(2): 35-42.
68. Shellman A. Empowerment and resilience: a multi-method approach to understanding processes and outcomes of adventure education program experiences. PhD thesis. Indiana: Indiana University, 2009.
69. Skehill CM. Resilience, coping with an extended stay outdoor education program, and adolescent mental health. Master's thesis. Canberra, ACT: University of Canberra, 2001.
70. QualityMetric. Qualitymetric's SF Health Surveys. (Online) 2012. Available: http://www.qualitymetric.com/WhatWeDo/SFHealthSurveys/tabid/184/Default.aspx (Accessed 28 December 2012).
71. Ware JE. SF-36 Health Survey update. In: ME Maruish (Ed). The use of psychological testing for treatment planning and outcomes assessment volume 3: instruments for adults. Mahwah, NJ: Lawrence Erlbaum Associates, 2004.
72. Ungar M, Liebenberg L. Assessing resilience across cultures using mixed methods: construction of the Child and Youth Resilience Measure. Journal of Mixed Methods Research 2011; 5(2): 126-149.
73. Yazici B, Yolacan S. A comparison of various tests of normality. Journal of Statistical Computation and Simulation 2007; 77(2): 175-183.
74. Hedges LV. Distribution theory for Glass's estimator of effect size and related estimators. Journal of Educational Statistics 1981; 6(2): 107-128.
75. Cohen J. Statistical power analysis for the behavioural sciernces. Hillsdale, NJ: Erlbaum, 1988.
76. Patton MQ. Qualitative research and evaluation methods. 3rd edn. Thousand Oaks, CA: Sage Publications, 2002.
77. Bloemhoff HJ. The effect of an adventure-based recreation programme (ropes course) on the development of resiliency in at-risk adolescent boys confined to a rehabilitation centre. South African Journal for Research in Sport, Physical Education & Recreation 2006; 28(1): 1-11.
78. Ewert A, Yoshino A. The influence of short-term adventure-based experiences on levels of resilience. Journal of Adventure Education & Outdoor Learning 2011; 11(1): 35-50.
79. Ungar M, Dumond C, McDonald W. Risk, resilience and outdoor programmes for at-risk children. Journal of Social Work 2005; 5(3): 319-338.
80. Green GT, Kleiber DA, Tarrant MA. The effect of an outdoor recreation program on the resilience of low-income, minority youth. Journal of Park and Recreation Administration 2000; 18(3): 76-79.
81. Walsh MA. Wilderness adventure programming as an intervention for youthful offenders: self-efficacy, resilience, and hope for the future. Minneapolis, MN: University of Minnesota, 2009.
82. Marsh HW, Richards GE, Barnes J. Multidimensional self-concepts: the effect of participation in an Outward Bound program. Journal of Personality and Social Psychology 1986; 50(1): 195-204.
83. Russell KC. An assessment of outcomes in outdoor behavioral healthcare treatment. Child and Youth Care Forum 2003; 32(6): 355-381.
84. Harper NJ, Russell KC, Cooley R, Cupples J. Catherine Freer wilderness therapy expeditions: an exploratory case study of adolescent wilderness therapy, family functioning, and the maintenance of change. Child & Youth Care Forum 2007; 36(2-3): 111-129.
85. Russell KC. Two years later: a qualitative assessment of youth well-being and the role of aftercare in outdoor behavioral healthcare treatment. Child & Youth Care Forum 2005; 34(3): 209-239.
86. National Collaborating Centre for Aboriginal Health. Child and youth health: the importance of disaggregated data. Fact sheet. Prince George, BC: NCCAH, 2009.
87. Young N, Wabano M, Burke T, Ritchie S, Mishibinijima D, Corbiere R. A process for creating the Aboriginal children's health and well-being measure (ACHWB). Canadian Journal of Public Health 2013; 104(2): e136-e141.




