full article:
The World Health Organization defines palliative care as an approach that improves the quality of life of patients with life-threatening illness and their families1. Family caregivers are important to the support and care of dying persons, yet providing this care can result in a decrease in their own quality of life2. This decrease in caregiver quality of life is compounded by the paucity of health services available to some caregivers, particularly those in rural areas3,4. The majority of research on caregivers has focused on those living in urban areas, without considering the influence of geographic location on family caregivers' quality of life5.
Hope has a positive influence on quality of life for family caregivers of persons with advanced cancer6 and lower hope scores are significantly related to higher levels of caregiver strain7. Moreover, family caregivers of persons at the end of life experience lower levels of hope than the person for whom they are caring8.
Hope is an important psychosocial resource among family caregivers of persons with advanced cancer that helps them to manage and deal with the caregiver experience9-12. Hope is defined by these caregivers as the inner strength to achieve a better future and to continue caregiving10. Although there are multiple definitions and conceptualizations of hope, very little research has focused on understanding the hope of family caregivers of persons with advanced cancer11. Moreover, no studies have examined what factors influence the hope of rural women caregivers. The purpose of this study is to explore the factors that influence hope in rural women caring for a person with advanced cancer. Understanding these factors is important for the development of strategies to foster hope and support this vulnerable population. To contribute to this knowledge base, this study analyzed baseline data from a hope intervention study among rural women caregivers of persons with advanced cancer13.
Background
While there can be benefits to caregiving2, there are also risks. In Canada, the majority of informal caregivers are women14. The literature identifies that women who provide end-of-life care can experience caregiver burden, reduced health, depression, and anxiety15. Family caregivers in rural areas may not have the same access to palliative services, including counseling and bereavement services, as those in urban centers16. Thus, this study focuses on rural women caregivers because of their increased vulnerability to the risks of caregiving.
Hope may be an important resource to mitigate the negative effects of caregiving for rural women caregivers. In a recent metasynthesis study of the hope experience of caregivers of persons with chronic disease, the importance of hope to the caregivers was well substantiated12. The metasynthesis included the findings from 14 studies of caregivers of persons with life-threatening illness, of which three studies focused on caregivers of persons with advanced disease. Hope was described as dynamic, occurring within uncertainty and influenced by internal and external factors. However, research on hope and family caregivers of persons with advanced cancer has been descriptive and exploratory in nature and as such has not examined the factors influencing hope. These factors could include physical and mental health, loss and grief, general self-efficacy, and demographic variables.
Physical and mental health: Hope of family caregivers of persons with advanced disease is experienced within the context of fatigue and distress10,11. Research suggests that caregiver fatigue, distress, and reduced physical and mental health results in the loss of hope for family caregivers of persons receiving palliative care6,8,9. Borneman et al6 described how their participants experienced fatigue and distress, became overwhelmed with caregiving and lost hope. Similarly, Herth9 reported levels of caregiver fatigue, health status, and interference with sleep as significantly related to levels of hope: hope decreased with increasing fatigue and decreased health status. Significant negative relationships between fatigue and hope were also found in a study of hope, hopelessness, and fatigue in patients and family members in palliative care8. In this study, the family caregivers had lower levels of hope than the palliative patients and the relationship between hope and fatigue was significant for family caregivers but not for palliative patients. This difference may be related to caregiver strain, as caregiver strain has been found to have a significant inverse relationship with hope7; higher levels of caregiver strain lead to lower levels of hope. These findings suggest that the physical and mental health of family caregivers of persons with advanced cancer may influence hope. However, none of these studies specifically measured physical and mental health and examined its association with hope.
Loss and grief: Qualitative studies of the hope of family caregivers of persons receiving palliative care suggest that loss and grief (a response to loss17) may influence hope9-11. In these studies, participants described a number of losses, including the loss of time to spend with the person, loss of relationships, and loss of their own health. These losses resulted in feelings of overload and overwhelming grief. High levels of grief were reported in a study examining the relationships among hope, coping style, and grief in 61 family caregivers of persons receiving palliative home care18. Hope was found to be a significant factor in despair, loss of control and coping. Although the relationship of grief and hope was not studied, it is possible that grief could be a significant factor influencing hope in these family caregivers.
General self-efficacy: Self-efficacy is the confidence in the ability to complete challenging tasks or to cope with difficult situations19. There are reasons to believe that a sense of self-efficacy may be particularly important in caregiving situations. Rural women caregivers require confidence to care for a family member with advanced cancer and the ability to control some aspect of their situation. Family caregivers of persons receiving palliative care often describe uncertainty and loss of control as part of their hope experience9,10. In Holtslander et al's10 study of hope in family caregivers, self-efficacy or feelings of control was a major theme that participants described as influencing hope. Although the influence of self-efficacy has not been studied in our target population, it has been found to have a significant positive relationship with the hope of male spouses of women with breast cancer20. As such, self-efficacy may be a factor influencing hope in family caregivers of persons with advanced disease.
Demographic variables: Published studies on hope in family caregivers of persons with advanced disease have identified several variables that may influence hope: age, sex, spousal relationship, and service use. The research is inconclusive for age. For example, age and hope were inversely correlated (older caregivers had less hope) in a study of 85 caregivers of persons with advanced cancer8. This is in contrast to a significant positive correlation of age and hope (older participants had more hope) in a study of 61 family caregivers of persons receiving palliative care18. In another study of hope and caregiver strain in 112 family caregivers, no significant correlations between age and hope were found7.With respect to sex (male or female), female caregivers of persons with advanced disease have reported more anger/despair and lower levels of hope than male counterparts14. Spousal relationships may also affect hope. A mixed methods study found that the relationship of family caregivers to the terminally ill person for whom they were caring was significantly associated with levels of hope6. Moreover, spousal caregivers had less hope compared to parents or children. Finally, whether or not family caregivers are using formal supportive services (ie service use) is an important consideration. Family caregivers who do not have access to services, including counselling and bereavement services, are in need of more support than other populations3. Other variables have unknown relationships with caregivers' hope. These include caregiver years of education; marital status; ethnicity; religion; income; receiving informal (unpaid) help; length of time caregiving; and patient age, gender, and type of cancer.
Conceptual framework
The conceptual framework guiding this study was developed utilizing the main concepts from (a) a grounded theory study by Holtslander et al10, (b) social cognitive theory21, and (c) empirical findings (described above). Taken together, this work suggests that potential factors influencing family caregivers' hope includes their grief, feelings of self-efficacy, and physical and mental health. Hope is conceptualized as a psychosocial resource that is more likely present when self-efficacy is high and grief is low. Hope can have a positive effect on physical and mental health12. Thus, both physical and mental health were expected to have positive associations with hope in this study. The conceptual framework also includes caregiver age, spousal relationship, and service use to reflect the findings from other research on hope for family caregivers.
Purpose
The purpose of this study was to determine which factors are associated with (and may predict) hope for rural women caregivers of persons with advanced disease, by examining the relationship of hope with demographic variables, self-efficacy, grief, and caregiver physical and mental health.
This study was conducted using a cross-sectional correlational design. This design is utilized to test measures of association among variables22. Baseline data from an intervention study were analyzed. The purpose of the intervention study was to evaluate a Living with Hope Program whose intent was to foster hope in rural women caring for a person with advanced cancer13.
Sample/setting
Inclusion criteria for the study were: (a) female, (b) 18 years of age or older, (c) caring for a person who is diagnosed with advanced cancer, (d) home address has a rural postal code, and (e) English-speaking. Using convenience sampling, participants were recruited through mail-out invitations by the Alberta and Saskatchewan Cancer Registries. Mail-out invitations were sent to all stage 4 cancer patients over 18 years of age, diagnosed between June 2007 and 2010, with rural postal codes, and who had indicated that they had a female family caregiver. Patients were asked to pass the study invitation letter on to their caregiver. Rural postal codes in Saskatchewan include anyone who lives in a community of 9999 or fewer, the definition of 'rural' used by Saskatchewan Health23. Rural postal codes in Alberta include anyone who does not live in the two tertiary or five regional centers24 where populations range from 55 032 to 1.1 million25 Alberta and Saskatchewan are both large provinces. Rural areas range from very remote settings, to mid-size communities which may have large neighboring cities. Regardless of the type of rural setting, in rural Alberta and Saskatchewan settings, there is a little access to palliative care services. Any services are delivered by home care nurses.
Cohen's26formula was used to determine the appropriate sample size. With a moderate effect size (f=0.13), power of 0.80, alpha of 0.05, and with a regression equation of six independent variables (general self-efficacy, grief, physical health, mental health, and demographic variables), the total required sample size was estimated to be 98.
Data collection
Using a revised Dillman27 technique, 780 surveys were mailed by the Alberta and Saskatchewan Cancer Registries between September 2010 and January 2011. A follow-up reminder postcard was mailed out approximately 4 weeks later. Dillman technique includes a second reminder postcard, but this step was omitted to prevent burdening the recipients with an additional request for study participation. The surveys included a letter of invitation to persons with stage 4 cancer instructing them to ask their caregiver to participate. A caregiver was defined as a family member who was supporting them (ie patients identified their own caregivers according to their own criteria about those providing them with support). It was deemed inappropriate to pre-determine which specific supportive activities (eg assistance with bathing or making meals) were meaningful to individual patients with advanced cancer, since each will have their own unique experience of receiving support. Caregivers were asked to complete the Herth Hope Index (HHI; measure of hope), General Self-Efficacy Scale (GSES; measure of general self-efficacy), Non-Death Revised Grief Inventory (NDRGEI; measure of grief), and the Short Form Health Survey Version 2 (SF-12v2; measure of physical and mental health).
Demographic information was also collected. A prepaid postage envelope was included in the study package and participants were asked to return completed surveys by mail. Return of the surveys indicated implied consent. Individuals who were invited to participate in the study were offered a small incentive (a $5 Tim Horton's Cafe and Bake Shop card), regardless of their choice to complete the survey, and were given the option of participating in an intervention study intended to foster hope. The contact information for an experienced palliative care nurse was provided in the study invitation letter for individuals who wanted more information.
Measures
Demographic variables: Caregiver information collected included years of education, marital status, spousal relationship to patient, use of formal services, ethnicity, religion, income, receiving informal help from other caregivers, and length of time caregiving. Patient information included age, gender, and type of cancer.
Herth Hope Index28: The HHI provides a summative hope score and scores for three sub-scales of hope: temporality and future, positive readiness and expectancy, and interconnectedness28. It is a 12-item Likert response scale (1-4) with summative scores ranging from 12 to 48, with a higher score denoting greater hope. It has reported reliability (test-retest r=0.91, p<0.05) and validity (concurrent validity, r=0.84, p<0.05; criterion, r=0.92, p<0.05; divergent, r = -0.73, p<0.05)28. The HHI has been used in studies with family caregivers6,8.In this study Cronbach's alpha was r=0.87.
General Self-Efficacy Scale19: This Likert-type scale has 10 items which produce a total perceived general self-efficacy score. It has a maximum score of 40; the higher the score, the higher participant feelings of self-efficacy. The GSES has been found to be a reliable and valid measure in many populations and countries19 and has been used in a study of hope and family caregivers of women with breast cancer20. Reliability ranges from r=0.76 to r=0.90 and criterion-related reliability was r=0.80, p<0.0519. In this study Cronbach's alpha was r=0.88.
Short Form Health Survey Version 2: The SF-12v2 was developed as a shorter yet valid alternative to the SF-36 as a measure of quality of life29. The SF-12v2 produces a physical component summary (PCS) score and a mental component summary (MCS) score , but not a total summary score. The SF-12v2 PCS and MCS scores correlate very highly (r=0.95 and 0.96 respectively) with the SF-36 and have reported test-retest reliability of r=0.89 and 0.76 respectively30. In this study Cronbach's alpha for the PCS score was r=0.83, and for the MCS score r=0.72.
Non-Death Revised Grief Experience Inventory31: The NDRGEI is a 22-item scale measuring four domains of the grief experience for people who are not bereaved (item examples are in brackets): (1) existential concerns (eg 'I feel lost and helpless'), (2) depression (eg 'I cry easily'), (3) guilt (eg 'I have feelings of guilt'), and (4) distress (eg 'My arms and legs feel very heavy') . The NDRGEI contains items nearly identical to those of the revised grief experience inventory (RGEI), which is used for people who are bereaved. Just two items on the NDRGEI differ from the RGEI in that they do not specify that feelings of guilt or having frequent headaches are linked to the death of the person they were caring for. Responses are scored on a six-point scale, ranging from slight disagreement to strong agreement, with a higher total score indicating more grief and loss. The scale has established reliability (internal consistency of alpha =0.93) and validity (internal structure and criterion p=0.01)31. The non-death version of the RGEI has been used in a study of hope and caregivers6. In this study Cronbach's alpha was r=0.824.
Data analysis
The Statistical Package for the Social Sciences v19 (SPSS; http://www.spss.com) was used for all analysis. Data entry was completed using a standardized code-book, and data cleaning was conducted to identify data entry errors (eg by checking outliers). Mean imputation was used to handle missing data for the GSES and NDRGEI; missing data on the SF-12v2 was imputed using the Quality Metric software algorithms (http://www.qualitymetric.com)30. Univariate analysis included descriptive statistics for all demographic data, hope, self-efficacy, physical and mental health, and grief, in order to describe the sample. SF-12v2 summary scores were calculated using Quality Metric software30 and compared to US population norms based on Quality Metric calculations. Univariate analysis was conducted for each independent variable (all demographics, GSES, total NDRGEI, the four NDRGEI subscales, and SF-12v2 PCS and MCS scores) separately with hope as the dependent variable. The total hope score was used as the dependent variable; hope subscales were not used. Generalized linear modeling (GLM) was utilized to determine significant factors associated with hope. Variables were entered into the multivariate generalized linear model if they were significant at the p<0.10 level in the bivariate analysis to determine significant factors associated with the total hope score. GLM is an extension of linear regression and provides the flexibility to handle categorical, count, and continuous data as response variables32.
Ethics approval
This study received ethics approval from the Alberta Cancer Research Ethics Committee, the University of Saskatchewan Behavioral Research Ethics Board and the Regina/Qu'Appelle Health Region Ethics Board; ethics approval number 25209.
Sample
A total of 122 participants completed the surveys (15.6% response rate). Demographic characteristics of the whole sample (n=122) are presented in Table 1. The mean age of caregivers was 59.0 years (standard deviation (SD) =11.5), and the mean years of education was 13.0 (SD=2.4). The majority of caregivers were married (76%), and were caring for their spouse (66%). Length of caregiving was an average of 38.0 months (SD=77.3). The persons for whom they were caring had a mean age of 64.7 years (SD=11.6) and the majority were male (73%).
Table 1: Demographic characteristics of participants (N=122)
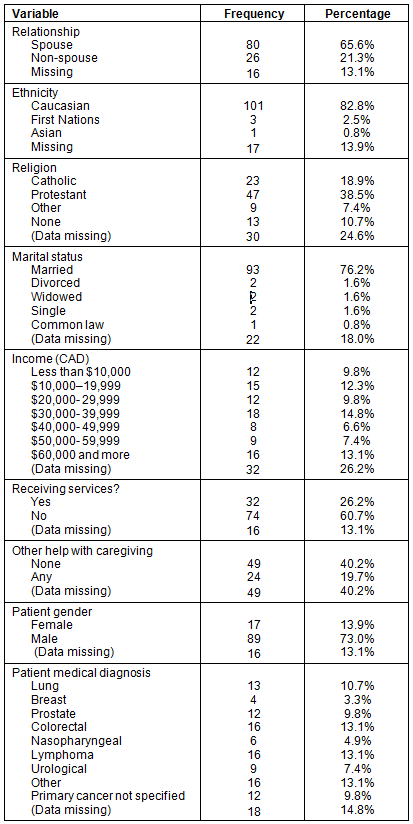
Main variables
The mean, standard deviation, and internal consistency of the HHI, total NDRGEI, four NDRGEI subscales, GSES (all with n=122) and SF-12v2 PCS and MCS scores (n=119, due to missing data) are presented in Table 2. The SF-12v2 mean PCS score of 43.30 (SD=4.63) is below the 25th percentile (46.53) of US population norms. The SF12v2 mean MCS score of 45.24 (SD=5.98) is just above the 25th percentile US population norms (45.13).
Significant factors influencing HHI at the univariate analysis level were receiving other services (p=0.023), GSES (p≤0.0001), NDRGEI (p≤0.0001), SF-12v2 PCS score (p≤0.0001) and MCS score (p≤0.0001). These were entered into the multivariate model for analysis. The total NDGREI was also significant in univariate analysis but, because no other subscales of the NDRGEI were significant, the NDRGEI-guilt subscale was entered into the model instead of the total score. No other demographic variables, such as age or spousal relationship to the patient, were significant.
Using GLM (n=105), significant factors influencing HHI scores for study participants (Table 3) were GSES (p≤0.0001), NDRGEI (p=0.001) and SF-12v2 MHS score (p=0.002). Participants with higher HHI scores had higher GSES, lower NDRGEI and higher SF-12v2 MHS scores. Although the scales are designed to measure distinct constructs, some of the individual items in the SF-12v2 and the NDRGEI appear to have some conceptual overlap. This could cause collinearity issues in the final model. However, all Pearson correlation coefficients were examined and were well below the 0.8 cut-off, which indicates that collinearity was not a concern in the final model.
Table 2: Mean scores of main variables
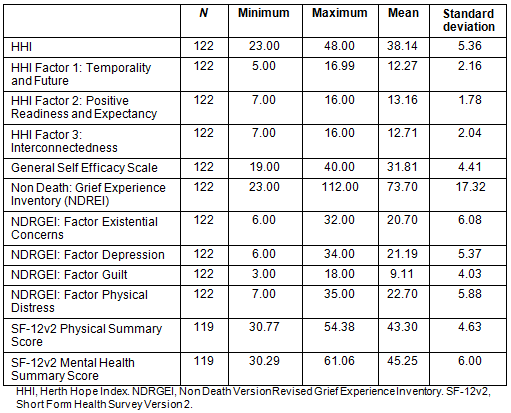
Table 3: Multivariate analysis results (n=105)
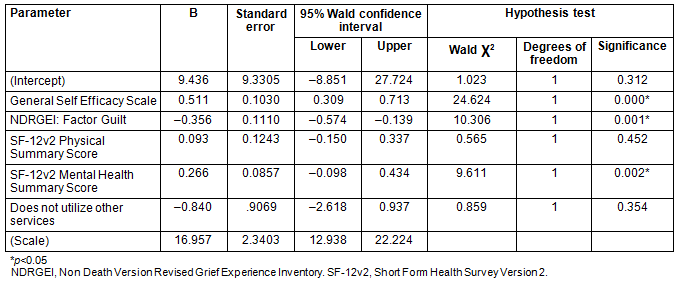
Discussion
The mental health, general self-efficacy, and perceptions of guilt of rural women caregivers of persons with advanced cancer were associated with (and may be considered predictors of) their levels of hope. Participants with higher hope scores had higher mental health scores, lower perceptions of loss and grief scores, and higher scores in their confidence in their ability to deal with difficult situations (self-efficacy). Grief, physical health and other demographics (eg relationship to patients (spouse or other), service use) were not found to be significant.
Mental health
Mental health or wellbeing was found to be a predictor of hope for rural women caregivers of persons with advanced cancer. It is an important aspect of quality of life for family caregivers. Although hope is considered a factor in quality of life for persons with advanced cancer33, this is the first study to find mental health as a significant factor influencing hope in rural women caregivers. By contrast, physical health was not significant. Qualitative studies of hope in family caregivers of persons receiving palliative care support the association between hope and mental health, with participants describing how hope helped them deal with their distress and anxiety9,10. In other studies of cancer patients, hope has been found to be inversely related to psychological distress34 and anxiety35,36. In psychology students, hope has been found to have a significant positive relationship with the following six aspects of mental health: autonomy, environmental mastery, personal growth, positive relations with others, purpose in life and self-acceptance37. However, the specific aspects of mental health associated with the hope of rural women caregivers of persons with advanced cancer is unknown.
The mental and physical health of the participants of this study, when compared to US population norms, were at or below the 25th percentile. Although this is a Canadian study, this finding suggests that the health of the rural women participants was poor. The US population SF-12v2 physical and mental health comparison data are not delineated by rural or urban geographic areas, therefore determining if the low physical and mental health summary scores are related to the rural location of the participants is not possible. The findings from a study comparing urban and rural caregivers of persons receiving palliative care found no significant differences in the participants' perceived health status and caregiver burden based on geographic location5; however, rural Canadians have reported poorer health status than their urban counterparts38. This study's findings clearly show that the women participating reported poorer physical and mental health than US population norms, but more comparative research is needed to determine if rural women caring for persons with advanced cancer have poorer physical and mental health than their urban counterparts.
General self-efficacy
General self-efficacy was a significant factor predicting hope in the participants. Self-efficacy has been found to be significantly and positively correlated with quality of life of caregivers of breast cancer patients16 and formal caregivers33. People with higher general self-efficacy may have more confidence in their ability to deal with difficult situations and have some control in their lives, and this is important to the hope of the rural women caregivers of persons with advanced cancer and to other caregiver populations as well. General self-efficacy (confidence in the ability to deal with difficult situations) is a different concept than caregiver self-efficacy (confidence in caregiving ability). Future research should explore whether caregiving self-efficacy would share the same association with hope as general self-efficacy, because the nature of an intervention to improve general self-efficacy and caregiving self- efficacy could differ in important ways.
The conceptual model for the study suggests that grief is a significant predictor of hope. Our results did not find grief itself to be a predictor; only guilt, one component of grief, was a predictor. This is similar to the findings of spouses of women with breast cancer20. Guilt has been found to be an important factor contributing to burden, depression, and distress in family caregivers of cancer survivors39 and persons with Alzheimer's disease40. Caregivers felt guilt when they could not deal with the demands of caregiving and when they felt they had not done enough for their family member41. Future research should explore the nature of the relationship between guilt and hope, in order to identify the reasons for perceptions of guilt and how this may influence hope in rural women caregivers of persons with advanced cancer.
Demographic variables
Relationship, defined as a spouse or other, was not found to be significantly associated with hope. This is in contrast to a previous study that included both male and female caregivers and that found that spouses had lower levels of hope than others6. The differences in the results could be related to whether the caregiver was living with the person with advanced cancer. Lohne et al7 found that caregivers that lived with the person for whom they were caring had less hope. The present study did not collect data on living arrangement, and this cannot be directly inferred from the reported formal relationship (ie spouse or other). In addition, formal relationship may not be as important as the supportive quality of the relationship. Qualitative studies of hope in family caregivers of palliative care patients suggest that supportive relationships, rather than formal relationships, are critical to maintaining hope9,10. Therefore, future research should utilize measures of relationship that extend beyond formal relationship, and distinguish between supportive and non-supportive relationships.
Implications for health professionals
This study's findings identify that rural women caregivers are a group with lower physical and mental health than US population norms. Thus, this is a group who may benefit from increased support. Overall, the findings highlight several areas that healthcare professionals could focus on in their practice. Rather than limiting focus to the more observable physical health issues, this study indicates that there are important associations between various mental and emotional needs of rural women family caregivers and their hope. While more research is needed to establish whether these associations are causal, the findings from this study support the importance of asking caregivers about their experiences in relation to their hope, self-efficacy, and guilt in order to identify people at risk for lower levels of mental health.
Limitations
This study has several limitations related to the sample and study design. The study was cross-sectional in nature, so it captured a one-time description of the factors associated with hope. Hope is dynamic in nature and fluctuates over time, so future research should also consider longitudinal study designs. Also, while the cross-sectional design matches with the intent of the study to determine associations between selected factors and hope, it does not test the direction of the relationships and so cannot establish cause and effect. Because the present design focused on examining the predictors of hope, whether hope was a predictor of other factors, or if there are interconnections between the factors, is unknown. More research is needed to determine the interrelationships between the factors evaluated here and hope, and to determine whether hope can influence the factors.
The low response rate (15.6%) limits the generalizability of the study findings. Using a modified Dillman technique may have resulted in a poorer response rate. The SF-12v2 PCS and MCS scores suggest that this population has very poor physical and mental health, which is a barrier to participation in any study. While generalizability remains a concern, a sample size that resulted in adequate power to prevent a type I error was achieved, despite the low response rate.
As no published population norms describe rural women caregivers of persons with advanced cancer, it is difficult to determine if the demographic characteristics of the participants in the study were representative of the population as a whole. The sample comprised rural women caregivers in two western Canadian provinces. The majority were married, well-educated and Caucasian. Research with rural women caregivers of lower levels of education and different ethnic groups may return different findings. More research is needed with rural women caregivers with more diverse demographic characteristics.
The sample included caregivers who reported widely varying lengths of time caregiving (from less than 1 month to more than 500 months). Because the caregiving experience may shift over time, it is reasonable to expect that the effects of caregiving on hope may also change over time. Length of time caregiving was tested in univariate analysis and was not significantly associated with hope. However, studies that collect sufficient data on subgroups of caregivers at different stages are warranted to better understand the specific factors that affect hope for caregivers at different points in the caregiving trajectory. The present study did not have enough participants to perform this subgroup analysis.
The findings of this study add to the knowledge about the concept of hope, in particular in an understudied area of rural women caring for persons with advanced cancer. The poor physical and mental health of these women is of grave concern and reinforces the need to find strategies to support them, as they care for their family member. The finding of significant relationships between hope and mental health, general self-efficacy, and perceptions of guilt provides a foundation for future research and underscores the importance of hope to rural women caregivers. The specific nature of the relationships of mental health, general self-efficacy and perceptions of guilt with hope require more study to inform effective strategies to foster hope in this population.
Acknowledgements
This study was funded by a Canadian Institutes of Health Research Operating Grant. The authors acknowledge co-investigators Dr Mary Hampton and Dr David Popkin, the Alberta and Saskatchewan Cancer Registries for their assistance and the study participants.
References
1. World Health Organization. WHO definition of palliative care. (Online) 2013. Available: http://www.who.int/cancer/palliative/definition/en/ (Accessed 30 January 2013).
2. Stajduhar K, Funk L, Toye C, Grande G, Aoun S, Todd C. Part 1: Home-based family caregiving at the end of life: a comprehensive review of published quantiative research (1998-2008). Palliative Medicine 2010; 24(6): 573-593.
3. Robinson C, Pesut B, Bottorff J, Mowry A, Broughton S, Fyles G. Rural palliative care: a comprehensive review. Journal of Palliative Medicine 2009; 12(3): 253-258.
4. Donovan R, Williams A. Shifting the burden: the effects of home-based palliative care on family caregivers in rural areas. In: J Kulig, A Williams (Eds) Health in rural Canada. Vancouver: UBC Press, 2012; 316-333.
5. Brazil K, Kassalainen S, Williams A, Rodriguez C. Comparing the experiences of rural and urban family caregivers of the terminally ill. Rural and Remote Health 13: 2250. (Online) 2013. Available: www.rrh.org.au (Accessed 3 February 2014).
6. Borneman T, Stahl C, Ferrell BR, Smith D. The concept of hope in family caregivers of cancer patients at home. Journal of Hospice and Palliative Nursing 2002; 4(1): 21-33.
7. Lohne V, Miaskowski C, Rustoen T. The relationship between hope and caregiver strain in family caregivers of patients with advanced cancer. Cancer Nursing 2012; 35(2): 99-105.
8. Benzein EG, Berg A. The level of and relation between hope, hopelessness and fatigue in patients and family members in palliative care. Palliative Medicine 2005; 19(3): 234-240.
9. Herth K. Hope in the family caregiver of terminally ill people. Journal of Advanced Nursing 1993;18(4): 538-548.
10. Holtslander L, Duggleby W, Williams A, Wright K. The experience of hope for informal caregivers of palliative patients. Journal of Palliative Care 2005; 21(4): 285-291.
11. Revier S, Meiers SJ, Herth K. The lived experience of hope in family caregivers caring for a terminally ill loved one. Journal of Hospice and Palliative Care Nursing 2012; 14(6): 438-446.
12. Duggleby W, Kylma J, Holtslander L, Duncan V, Hammond C, Williams A. Metasynthesis of the hope experience of family caregivers of persons with chronic illness. Qualitative Health Research 2010; 20(2): 148-158.
13. Duggleby W, Williams A. Living with hope: developing a psychosocial supportive program for rural women caregivers of persons with advanced cancer. BMC Palliative Care 2010; 9: 3.
14. Turner A, Findlay L. Informal caregiving for seniors. (Online) 2012. Available: http://www.statcan.gc.ca/ (Accessed 3 January 2013).
15. Cranswick K. Canada's caregivers. Canadian Social Trends 1997; 47(4): 2-6.
16. MacLean M, Kelley M. Palliative care in rural Canada. Rural Social Work 2001; 6(3): 63-73.
17. Parkes CM. Bereavement: studies of grief in adult life. London: Tavistock Publications, 1972; 2012.
18. Chapman KJ, Pepler C. Coping, hope, and anticipatory grief in family members in palliative home care. Cancer Nursing 1998; 21(4): 226-234.
19. Schwarzer R, Jerusalem M. Generalized Self-Efficacy scale. In: J Weinman, S Wright, M Johnston (Eds). Measures in health psychology: a user's portfolio. Causal and control beliefs. Windsor, UK: NFER-NELSON, 1995; 35-37.
20. Duggleby W, Doell H, Cooper D, Thomas R, Ghosh S. The quality of life of male spouses of women with breast cancer: hope, self-efficacy and perceptions of guilt. Cancer Nursing 37(1) E28-E35. (Online) 2014. Available: http://www.ncbi.nlm.nih.gov/pubmed/23348665 (Accessed 19 February 2014).
21. Bandura A. Self-efficacy: the exercise of control. New York: Freeman, 1997.
22. Cresswell J. Research design: qualitative, quantitative, and mixed methods approaches. 3rd edn. Thousand Oaks, CA: Sage, 2008.
23. Statistics Canada. Population counts for Canada, province, and territory and census division by urban and rural, 2001 Census-100% data. Ottawa, ON: Government of Canada, 2002.
24. Alberta Health Services. Community and rural health planning. Edmonton, AB: Government of Alberta 2012.
25. Statistics Canada. Population and dwelling counts for Canada and census subdivisions (municipalities) with 5,000-plus populations, 2011 and 2006 censuses. (Online) 2013. Available: http://www12.statcan.ca/census-recensement/2011 (Accessed 18 February 2014).
26. Cohen J. Statistical power analysis for the behavioral sciences. New York: Academic Press, 1977.
27. Dillman D, Smyth JD. Mail and internet surveys: the tailored design method. New Jersey: John Wiley and Sons, 2009.
28. Herth K. Abbreviated instrument to measure hope: development and psychometric evaluation. Journal of Advanced Nursing 1992; 17(10): 1251-1259.
29. Ware J, Kosinski M, Keller SD. A 12 item Short-Form Health Survey: construction of scales and preliminary tests of reliability and validity. Medical Care 1996; 34(3): 220-233.
30. Ware J, Kosiniski M, Keller S. SF-12. How to score the SF-12 physical and mental health summary scale. 3rd edn. Lincoln, RI: Quality Metric Incorporated, 1998.
31. Lev E, Hazard Munro B, McCorkle R. A shortened version of an instrument measuring bereavement. International Journal of Nursing Studies 1993; 30(3): 213-226.
32. Nelder JA, Wedderbirm RWM. Generalized linear models. Journal of the Royal Statistical Society - Series A (General) 1972: 370-384.
33. Duggleby W, Williams A, Wright K, Cooper D, Popkin D, Holtslander L. Living with hope: initial evaluation of a psychosocial hope intervention for older palliative home care patients. Journal of Pain and Symptom Management 2007; 33(3): 247-257.
34. Rusteon T, Cooper B, Miaskowski C. The importance of hope as a mediator of psychological distress and life satisfaction in a community sample of cancer patients. Cancer Nursing 2010; 33(4): 258-267.
35. Vellone E, Rega ML, Galletti C, Cohen M. Hope and related variables in Italian cancer patients. Cancer Nursing 2006; 29(5): 356-366.
36. Utne I, Miaskowski C, Bjordal K, Paul SM, Rusteon T. The relationships between mood disturbances and pain, hope and quality of life in hospitalized cancer patients with pain on regularly scheduled opioid analgesic. Journal of Palliative Medicine 2010; 13(3): 311-318.
37. Gallagher MW, Lopez SJ. Positive expectancies and mental health: identifying the unique contributions of hope and optimism. Journal of Positive Psychology 2009; 4(6): 548-556.
38. Canadian Institutes of Health Information. How healthy are rural Canadians? A component of the initiative 'Canadian rural communities: Understanding rural health and its determinants'. Ottawa, ON: Canadian Institutes of Health Information, 2006.
39. Spillers R, Wellisch D, Kim Y, Matthews A, Baker F. Family caregivers and guilt in the context of cancer care. Psychosomatics 2008; 49(6): 511-519.
40. Losada A, Marquez-Gonazles M, Penacoba C, Romero-Moreno R. Development and validation of the caregiver guilt questionnaire. International Psychogeriatrics 2010; 22(4): 650-660.
41. Erlingsson CL, Magnusson L, Hanson E. Family caregivers' health in connection with providing care. Qualitative Health Research 2012; 22(5): 640-655.





