full article:
Since the World Health Organization (WHO) launched the Global Age-Friendly Cities project in 20061, there has been considerable interest on the part of policy-makers in the concept of 'age-friendliness'2. The interest in making communities and cities better places to live for older adults is, to a large extent, driven by the recognition that the world's older population is growing. Population aging is a global phenomenon that affects both developed and developing countries3. In Canada, for example, the population aged 65 or older is expected to increase from the current 14% to 23% by 20364,5.
Presented as an approach to dealing with global aging, the WHO1defines an age-friendly city as one that provides supports and opportunities in the physical and social environment in order to enable older adults to age actively. Active aging, in turn, is a broad concept defined in terms of health, participation, and security6. Specifically, a range of domains are considered important in an age-friendly city, including housing, transportation, community supports and health services, communication and information. The Age-Friendly Cities project was designed to identify, via focus group research, features within each of these domains that can either present challenges for older adults, or foster healthy, active aging. Features identified were subsequently compiled in a guide to help make cities around the world more age-friendly1,7. For example, within the domain of transportation, a few of the specific features identified were affordable public transportation, specialized transportation for disabled people, and traffic signs and intersections that are visible and well-placed1.
Although the WHO introduced the notion of age-friendliness in the context of cities, the concept has been expanded to include rural communities. The emphasis on rural communities is particularly evident in Canada where, in parallel with the WHO Age-Friendly Cities project, the Federal, Provincial, Territorial (F/T/P) Ministers Responsible for Seniors sponsored a project designed to identify specific features that make Canadian rural and remote communities age-friendly8. As in the WHO project, focus groups were conducted, with findings used to develop a guide to help rural and remote communities become more age-friendly8.
Many features identified in the Canadian rural communities project were similar to those in cities (eg having accessible buildings; affordable housing); however, unique issues also emerged8. For example, transportation issues are magnified in rural areas and there may be a lack (or limited number) of healthcare providers, such as physicians or home support workers8. This is consistent with other research that shows the challenges that rural communities face in providing social and healthcare services9-11. For instance, attracting and retaining healthcare providers is an ongoing challenge in rural areas around the globe, and many approaches are being used to try to remedy this problem12-14.
The concept of age-friendliness has been garnering a great deal of attention from policy-makers in recent years. In Canada, several provinces have launched age-friendly initiatives, including the Province of Manitoba, the setting of the present study. In Manitoba, the provincial government launched its Age-Friendly Manitoba Initiative in 2008 as a way to promote healthy aging. Empirical literature in the area of age-friendly communities is only starting to emerge, however15,16. The present study addresses two major gaps in the literature.
First, although much research has focused on specific aspects of the environment and health-related outcomes, there is a paucity of research that has examined community characteristics from a broader perspective. For instance, there is a large literature that shows that features like the presence of footpaths, mixed land use, neighborhood walkability, and the presence of green space are related to various health-related outcomes such as walking, disability, functional capacity, and obesity17-19. Besides examining aspects of the physical environment, some studies have included features of the social environment, such as crime17,20.
The neighborhood characteristics examined in these studies are quite consistent with some of the features that have been identified as making a city age-friendly. However, a hallmark of the conceptualization of age-friendliness is its holistic nature, with a wide range of domains identified as being important in older adults' lives1,8,21-23. Thus, there is a need to examine a wider range of community features than has been the case in previous studies. In the present study, age-friendliness is conceptualized in terms of the broad range of domains that have been identified1,8,21-23 , including the physical environment, housing, social environment, opportunities for participation, informal and formal community supports and health services, transportation options, and communication and information.
Second, age-friendliness is viewed here through an ecologic theory lens24-26. Ecologic theory provides a general framework for understanding human behavior, health, or wellbeing, and makes explicit the importance of viewing the individual as being impacted by a broad range of influences within the environment. Best outcomes are achieved when there is a fit between the characteristics of the individual and those of the environment in which he or she lives24-26. With its focus on adapting communities or cities to the needs and resources of older adults, the concept of age-friendliness aligns well with ecologic theory23.
Ecologic theory also suggests that broader contextual factors, such as rural/urban, need to be taken into account when examining age-friendliness in relation to the health and wellbeing of older adults. The primary objective of the present study was, therefore, to examine this issue in a rural context. As such, the study addresses the second major gap in the literature, namely that the discourse around age-friendliness has tended to focus on cities, consistent with the WHO's original conceptualization of the topic. Similarly, literatures on the physical and social environment and health-related outcomes are heavily urban-centered17-19. Thus, much less is known about how the range of community features subsumed under the notion of age-friendliness relate to health-related outcomes in rural settings.
Examining age-friendliness in a rural context is important, given that the proportion of older adults tends to be higher in rural than in urban areas in most regions of the world, with rural areas growing older at faster rates than urban areas27,28. In Canada, 33% of older adults live in rural areas28. Moreover, rural-urban health disparities have been found within and outside of Canada29,30, although a great deal of heterogeneity across rural regions is also evident30,31. This suggests that solutions to enhancing health, such as making communities more age-friendly, are particularly needed in rural areas.
Data source
Data used in the present study were collected as part of a larger program of research (the Age-Friendly Community-University Research Alliance), which created a partnership between researchers and the Province of Manitoba's Age-Friendly Manitoba Initiative. Since its launch, municipalities throughout the province have been formally invited by government to join the initiative and become more age-friendly. At the time this article was prepared, 86 municipalities were part of the initiative, representing over 80% of the population of the province.
As part of the partnership with the provincial government, a protocol was developed by this research team to conduct needs assessments in communities that have joined the Age-Friendly Manitoba Initiative. Needs assessment consultations were designed to start a dialog about age-friendliness in the community and identify priorities for action. They were, thus, an integral part of the initiative. Because needs assessments were part of a larger public policy initiative, a protocol was developed that was easy to implement, while at the same time yielding as much information for communities as possible to help them initiate the process of becoming more age-friendly. As such, assessments involved bringing together community residents for a meeting that was facilitated by the research team. Participants first completed a brief survey developed for this purpose to measure aspects of age-friendliness (see details below). After this, there was a facilitated group discussion that allowed participants to identify priorities that should be addressed to make the community more age-friendly. The present study is based on the survey data only.
Communities
This study included 29 communities that are part of the Age-Friendly Manitoba Initiative that had needs assessment consultations completed between May 2010 and May 2012. Data from these communities were used because starting in May 2010 questions pertaining to life satisfaction and self-perceived health were added to the consultation survey. The 29 communities are a subset (52%) of communities that had a needs assessment consultation since the initiative was first launched.
A comparison of characteristics of the 29 communities included in this study with the communities that had a needs assessment but were not included showed no differences in population size and sociodemographic characteristics (eg percentage of residents 65 years or older, median income). Moreover, the 29 communities did not differ from communities that were part of the Age-Friendly Manitoba Initiative but did not have a needs assessment. Thus, the 29 communities were generally similar to other communities that are part of the Age-Friendly Manitoba Initiative. Relative to communities that are not part of the initiative to date, however, the populations in the 29 communities were somewhat older, with on average of 21% of residents being aged 65 years or older, compared to 16.4% in the communities that have not yet joined.
It must be noted here that the Age-Friendly Manitoba Initiative is implemented via municipalities. Two types of municipalities are officially recognized as legal entities in Manitoba: single settlements (villages, towns, or cities) and 'rural municipalities'. Rural municipalities refer to geographic areas with low density that may contain one or more very small villages. Rural municipalities are treated the same way as single settlement municipalities in the context of the Age-Friendly Manitoba Initiative. Both types of municipalities are referred to as 'communities' in this article for simplicity.
In one rural municipality that was part of the present study, separate needs assessment consultations were held in two small villages, on request of the municipality's Age-Friendly Advisory Committee. In this case, survey responses from the two villages were combined and treated as responses in one 'community'. Age-Friendly Advisory Committees lead the initiative at the local level and are composed of a range of stakeholders, including elected officials (municipal councilor or mayor), older adults at large (ie who did not represent an organization); representatives of organizations serving older adults or senior centers, town employees, representatives of governmental organizations (eg recreation departments) and non-profit organizations, business, clergy, and educators (eg school principal).
Participants
Participants were invited to the consultations by the communities' Age-Friendly Advisory Committees. Committees used a variety of approaches to invite community residents, such as word of mouth and local newspaper notices. Participants were thus not invited by this research team, although recommendations were made about the kinds of individuals to invite to ensure that a diversity of perspectives was represented.
A total of 646 individuals participated in needs assessment consultations in the 29 communities. Of these, 593 individuals had complete data on all age-friendly questions and the life satisfaction measure; 592 individuals had complete data for the analysis involving self-rated health. Thus, the number of participants included in analyses differs slightly depending on which outcome measure is used.
Measures
'Seniors' versus younger adults: As needs assessment consultations were part of the Age-Friendly Manitoba Initiative, asking personal questions would not have fitted with their overall goal of identifying community priorities. As such, no demographic information was collected from participants. Participants were asked only which of the following best described them: senior, caregiver to a family member or friend who is a senior, service provider; representative of a governmental organization, representative of a non-governmental organization, representative of municipal government, or business person/merchant. A total of 371 (62.6%) individuals identified themselves as a 'senior', 214 (36.1%) participants checked off another category, and 8 (1.3%) individuals did not answer the question. Among the participants that checked off another category, the following groups were represented: service provider (30.4%), caregiver to an older adult (23.4%), representative of a non-governmental organization (22.9%),representative of municipal government (22.9%), representative of a governmental organization (15%), and business person/merchant (17.3%). (These percentages do not add up to 100% as about a third of participants (31.3%) checked off more than one category.)
Individuals who did not self-identify themselves as seniors are referred to as 'younger adults', although it is recognized that some of them might have been classified as 'older' had an age cut-off been used, such as age 65. Thus, the seniors/younger adult measure was based on individuals' perceptions, which fits with the idea that a person's self-definition is more important than her or his age per se32. In this respect, research indicates that although organizations serving older adults in Manitoba typically define 'seniors' as those aged 55 years or older, many older individuals do not perceive themselves as seniors until much older and as a result prefer not to access these services32.
Age-friendly domains: Although instruments exist that measure certain aspects of age-friendly domains, there is no one instrument that captures the full range of domains. An Age-Friendly Survey was therefore developed for the purposes of the needs assessment consultations. Items were derived based on the work by the WHO1 and Federal, Provincial, Territorial Ministers Responsible for Seniors8, as well as other research15. Given that the survey was designed in the context of the Age-Friendly Manitoba Initiative's needs assessments, it had to be short and user-friendly.
The Age-Friendly Survey included 54 items that map onto seven age-friendly domains23,33:
- physical environment (12 items; eg 'Local parks or walking trails in my community are accessible and easy to use for seniors'; 'Most or all businesses in my community are readily accessible to seniors')
- housing (4 items; eg 'There is enough housing that meets the needs of seniors in my community'; 'Housing for seniors is affordable in my community')
- social environment (9 items; eg 'Seniors serve in an advisory role to municipal government in my community'; 'Crime and vandalism are a problem in my community')
- opportunities for participation (8 items; eg 'There are enough recreation programs specifically for seniors in my community'; 'The job opportunities in my community accommodate the needs of seniors')
- informal and formal community supports and health services (8 items; eg 'The home care services that support seniors in their own home (eg meal preparation, nursing care) are sufficient in my community'; 'The health care services that are provided in my community meet the needs of seniors (eg hospital, physicians, eye care)')
- transportation options (8 items; eg 'The transportation that is available for individuals with disabilities is sufficient in my community'; 'There are enough parking spaces close to services and stores in my community')
- communication and information (5 items; eg 'Information about community events is readily available to seniors in my community'; 'Official, written information, such as forms or brochures is easy to read and understand').
To simplify responding, a yes/no/don't know response format was used. An overall Age-Friendly Index was created by summing 'yes' responses (coded as 1) across all 54 items. Responses that were negatively worded were re-coded, so that higher scores on the questions reflect more positive ratings. The scale showed good internal reliability with a Cronbach's alpha of 0.88 (0.87 for seniors; 0.86 for younger adults). Separate indices for each of the seven age-friendly domains were also created by summing 'yes' responses on relevant items.
Community characteristics: Key community characteristics were identified using public access, 2006 census data, including two population-related measures (population size and the percentage of residents aged 65 or older) and two socioeconomic status indicators (percentage of residents with less than high school education, and median income). These measures were chosen for two reasons: their possible association with either age-friendliness or self-rated health and life satisfaction, and their relatively large variation across communities. Other characteristics, such as visible minorities, were not included because percentages were very low across all communities, whereas others (eg median age) would have been too highly correlated with other variables to allow inclusion in analyses.
There is no one universally accepted definition of 'rural' in Canada34. A useful definition introduced by Statistics Canada allows classifying municipalities on an urban-rural continuum by taking into account both population size and proximity (commuting patterns) to larger centers (metropolitan influenced zones, MIZ)35. This definition has been shown to meaningfully differentiate between types of rural communities in terms of health outcomes31.
The definition of MIZ35 assigns each municipality to a category: census metropolitan areas (CMA) are urban core areas with a population of at least 100 000, and census agglomerations (CA) are urban areas populations between 10 000 and 100 000. Municipalities outside a CMA or CA are then categorized into MIZ depending on the percentage of employed residents that commute to work in a CMA or CA. Strong MIZ municipalities are those in which at least 30% of the employed labor force commute to a CMA or CA; moderate MIZ municipalities include those in which between 5% and 30% of the employed labor force commute to a CMA or CA; in weak MIZ more than 0% but less than 5% of labor force participants commute; and no MIZ municipalities have no commuters.
Manitoba has a population of about 1.2 million. About two-thirds of the population is concentrated into one city (Winnipeg), located in the south of the province. Winnipeg is the only city in Manitoba that has a population of more than 100 000, and is, thus, classified as a CMA. The Winnipeg CMA also includes several small 'bedroom' communities that are close to Winnipeg. The 29 communities in the present study include several of these small communities, albeit not Winnipeg itself. This study, therefore, does not include a larger urban centre per se.
The 29 communities were first assigned to one of the six urban-rural categories. Given the small number of communities in some categories, CMA, CA, and strong MIZ communities were subsequently combined. As such, four groups were created: CMA/CA/strong MIZ (5 communities), moderate MIZ (11 communities), weak MIZ (9 communities), and no MIZ (4 communities).
Outcome measures: Two outcome variables were included: life satisfaction and self-perceived health. Both were measured with single items: 'How would you describe your satisfaction with life in general at present? Would you say it is ...' and 'In general, would you say your health is ...' In both cases the response scale was 'excellent' (coded as 5), 'very good' (coded as 4), 'good (3), 'fair' (2), and 'poor' (1). The 'fair' and 'poor' categories were subsequently combined because very few participants described their life satisfaction or health as poor. The two questions were asked immediately after those pertaining to age-friendliness.
These measures have been used extensively in previous research36,37. Single-item measures are useful because they are easy to administer, which was particularly important in the context of the needs assessment consultations, as it was not possible to add long scales to the Age-Friendly Survey. The measures have been shown to have good psychometric properties, such as good reliability38 and good validity, with high correlations with multi-item scales36. Furthermore, predictive validity is excellent. For example, self-perceived health has been shown to be related to mortality in numerous studies, even when controlling for more objective measures of health32.
Analytic approach
Three sets of analyses were conducted. First, t-tests were calculated to determine if there were any differences between seniors and younger adults on ratings on the overall Age-Friendly Index and the seven subscales, respectively. Second, multi-level regression analyses using SAS v9.3 PROC MIXED (SAS Institute; http://support.sas.com/documentation/cdl/en/statug/63962/HTML/default/viewer.htm#statug_mixed_sect001.htm) were conducted to examine the relationship between age-friendliness, measured using the Age-Friendly Index and the seven subscales, respectively, and life satisfaction and self-perceived health. In all analyses community characteristics were controlled. Third, multi-level regressions for seniors versus younger adults, respectively, were conducted to examine if similar patterns would emerge in the two groups. Again, analyses were run with either the overall Age-Friendly Index in the model or one of the seven subscales, while controlling for community characteristics. Multi-level regression with a random intercept was used to reflect the fact that individuals (Level 1) were nested within communities (Level 2).
Ethics approval
This project received ethics approval from the Health Research Ethics Board at the University of Manitoba; ethics approval number HS11795.
Table 1 shows descriptive results for ratings of age-friendliness. The mean rating on the Age-Friendly Index was 21.6 (median=21) out of a possible total of 54. Scores were the lowest for housing with a mean rating of just under 1 (median=1).
Descriptive statistics for community characteristics are displayed in Table 2. The population sizes of the 29 communities were small, reflective of rural Manitoba as a whole, ranging from 432 individuals in the smallest community to 13 446 in the largest, with a mean of 2501. Considerable variation is also evident in terms of the percentage of residents aged 65 or older, percentage residents with less than high school education, and communities' median income, which ranged from about $28 000 to $75 500 (Canadian dollars).
Responses on the Age-Friendly Index and seven age-friendly subscales provided by seniors versus younger adults were compared next. None of the eight t-tests were significant, indicating that ratings did not differ between the two groups.
Regression results for the overall Age-Friendly Index (top panel) and individual age-friendly subscales (bottom panel) are shown in Table 3. As can be seen, none of the community characteristics were related to life satisfaction and self-perceived health. Seniors did not differ from younger adults on life satisfaction, but did report being less healthy. Significant effects emerged for the overall Age-Friendly Index, with higher ratings being associated with greater life satisfaction and better perceived health.
When conducting separate analyses for the seven age-friendly subscales, with the exception of housing, all subscales were positively related to life satisfaction (Table 3). For self-perceived health, significant positive effects emerged for the physical environment, social environment, opportunities for participation, and transportation options.
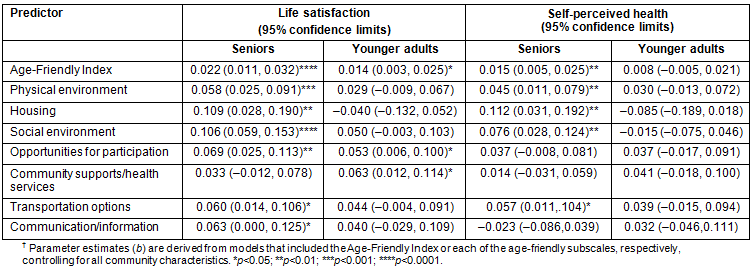
Lastly, separate analyses for seniors versus younger adults were conducted (Table 4). Community characteristics were taken into account in all the analyses. With the exception of community supports/health services, all age-friendly measures were related to life satisfaction among seniors, whereas only the overall Age-Friendly Index, opportunities for participation, and community supports/health services were significant for younger adults. Similarly, several age-friendly measures were related to self-perceived health among seniors (the overall Age-Friendly Index, physical environment, housing, social environment, transportation options), whereas no significant effects emerged for younger adults.
Table 1: Descriptive statistics of ratings of age-friendliness
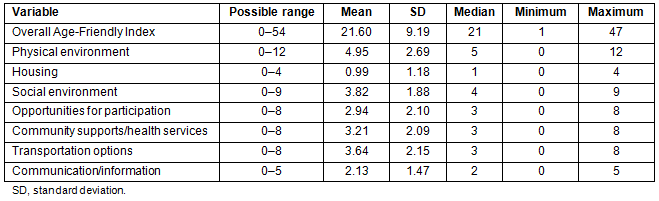
Table 2: Descriptive statistics of community characteristics (29 communities)
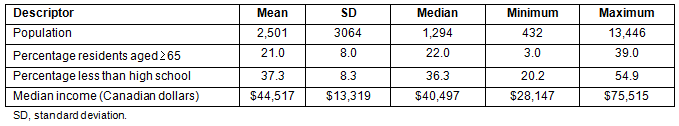
Table 3: Predictors of life satisfaction and self-perceived health: multi-level regression analysis for total sample
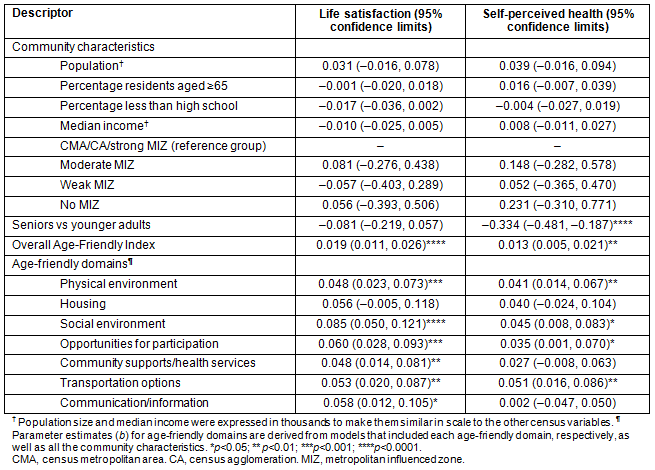
Table 4: Predictors of life satisfaction and self-perceived health: multi-level regression analysis for 'seniors' versus 'not seniors'?
Discussion
The concept of age-friendliness is clearly appealing to policy-makers, and a rapidly growing number of jurisdictions around the world are trying to make cities and communities more age-friendly2. The interest the concept has been garnering is, in part, due to the aging population, but may also be due to the recognition that in order to promote healthy, active aging, a wide range of factors within the community environments need to be considered and enhanced. Much research has focused on certain aspects of the environment, such as in the built environment, and how they relate to health and wellbeing17-19. A large literature also exists on the relationship between the social environment and health outcomes, including for example income39 and social capital40. There is a paucity of studies, however, that have simultaneously examined the range of age-friendly domains that older adults identify as being important in their lives1,8,15,21,22. The present study thus contributes to the literature by examining a diversity of age-friendly domains and their relationship to life satisfaction and self-perceived health in a rural context.
The overall Age-Friendly Index was positively related to both life satisfaction and self-perceived health. Moreover, all age-friendly domains, with the exception of housing, were related to life satisfaction. Thus, higher ratings regarding the physical environment, social environment, opportunities for participation, community supports/health services, transportation options, and communication/information were associated with greater life satisfaction. This is reminiscent of previous research in an urban context that shows that the quality of the neighborhood, defined in terms of a range of factors including access to public transportation, access to shops and services, and having clean footpaths and streets, was related to life satisfaction among older adults41. In contrast, only perceptions of the physical environment, social environment, and transportation options were related to self-perceived health.
Making communities more age-friendly is first and foremost thought to benefit older adults1. However, is it assumed that those same community supports and features would also be beneficial to younger individuals42. For instance, a safe environment is thought to be good for both young and old, as are barrier-free streets42. For example, having well-maintained footpaths should help older adults with their mobility, but presumably also benefits a parent navigating the environment with a child in a stroller. Although the argument seems logical, the present findings suggest that benefits of age-friendly features were predominantly restricted to older adults. As such, all but community supports/health services were related to life satisfaction among individuals who self-identified themselves as 'senior', and four of the age-friendly domains (physical environment, housing, social environment, and transportation options) were related to self-perceived health. In contrast, few significant effects emerged among individuals who did not identify themselves as seniors.
That the benefits of age-friendliness are generally restricted to older adults makes sense, given the nature of the questions contained in the age-friendly survey, most of which were very much focused on older adults, such as whether there is enough housing that meets the needs of older adults or whether housing for older adults is affordable. Presumably, having more opportunities in this respect would impact older adults, but not necessarily younger individuals.
The findings regarding community supports/health services warrant discussion. This was the only domain that was significant for younger adults, but not seniors. Indeed, it produced one of only two significant effects among younger adults. It is possible that the positive relationship for younger adults is due to the impact community supports and health services have on informal caregivers, such as spouses, daughters, or sons. For instance, having home care services should reduce the burden that is placed on informal caregivers. Consistent with this interpretation, previous research has demonstrated that there is a relationship between caregiver burden and unmet service needs in rural settings43.
Why community supports and health services were not related to seniors' life satisfaction is not clear. Similarly, this domain was not related to self-perceived health. The lack of significant relationships may be due to a confound with health status. Individuals who are less healthy may be more likely to use and be aware of community supports and health services. Thus higher ratings on this domain would not be expected to be associated with higher life satisfaction or self-perceived health; if anything, one might expect the opposite effect.
The findings for community characteristics are also noteworthy. None of the characteristics included in the present study were related to life satisfaction and self-perceived health, nor were the urban-rural categories. This is to some extent consistent with previous research, which shows that the effects for rurality in a Canadian context are small, with substantial heterogeneity in health among rural areas31. Similarly, a review of studies on rural health conducted in a range of countries shows a great deal of inconsistency in findings, with rural residents not necessarily being disadvantaged health-wise, relative to their urban counterparts30.
In the present study, even though 29 communities were included, there may not have been enough variability to find any health discrepancies across degrees of rurality. Moreover, both outcome measures were subjective in nature, which may minimize any differences among communities. For instance, individuals would likely stay in a community if they are satisfied with their lives there; if they were not, they may choose to move elsewhere. On the positive side, the findings suggest that residents are equally satisfied with their lives and equally healthy regardless of the size of the community, its average income or its location (closer or further away from a larger urban center).
The present study has several limitations that must be acknowledged. First, this is a cross-sectional study. As such, it cannot be inferred that age-friendliness leads to greater life satisfaction and better self-perceived health. It is possible that individuals who rated themselves higher on these two measures were generally more positive and therefore also rated their community as more age-friendly. The fact that life satisfaction and self-rated health were assessed immediately after participants completed the Age-Friendly Survey may also have inflated the correlation between these measures. Second, only very limited information on participants' sociodemographic characteristics was available. In developing the needs assessment consultations from which the data for the present study were derived, it was important to have a short instrument, which could not contain too many personal questions. It is therefore not known if participants represented a diversity in terms of gender, socio-economic status, mobility, etc. Moreover, participants were not randomly chosen and it is not known to what extent they reflect the sociodemographic make-up of the community as a whole.
Third, although the Age-Friendly Survey was developed with the aim to measure a range of age-friendly features within a number of domains, the number of items that could be included was necessarily limited because the survey had to fit into the needs assessment consultation process. Also, the simple, dichotomous response format does not provide as nuanced an assessment of age-friendly features as one might like. However, despite these limitations, the present findings show consistent, meaningful relationships between age-friendly domains and life satisfaction in particular, and to a lesser extent with self-perceived health. Moreover, the differences in results obtained for participants who self-identified as seniors versus younger adults provide support for the validity of the survey.
The present study represents a first step in examining the relationship between communities' age-friendliness and health-related outcomes in a rural context. The overall Age-Friendly Index and more specifically the ratings of the physical environment, housing, social environment, opportunities for participation, transportation options, and communication/information were all positively related to life satisfaction among seniors. The effects were less consistent for younger adults. Moreover, the Age-Friendly Index, as well as several domains (physical environment, housing, social environment, and transportation options) were positively related to self-perceived health. As such, the findings generally support the idea that age-friendliness is related to healthy, active aging1.
Further research is needed to examine whether these effects are causally related. For example, comparisons of communities that have implemented age-friendly projects versus those that have not and measuring health-related outcomes longitudinally would be useful. Qualitative studies that provide an in-depth understanding of how older adults view their communities and how that relates to healthy aging would also provide important information. From a policy perspective, the present findings point to the potential benefits of making communities more age-friendly, as well as the need to focus on a range of domains that are important in older adults' lives. The findings further suggest that province-wide policy initiatives, such as the Province of Manitoba's Age-Friendly Initiative, may be one approach to enhancing healthy aging in rural settings.
References
1. World Health Organization. Global age-friendly cities: a guide. Geneva: World Health Organization, 2007.
2. Plouffe LA, Kalache A. Making communities age friendly: State and municipal initiatives in Canada and other countries. Gaceta Sanitaria 2011; 25(Suppl. 2): 131-137.
3. United Nations Population Fund and HelpAge International (UNFPA). Ageing in the twenty-first century: a celebration and a challenge. New York, NY: UNFPA, 2012.
4. Statistics Canada. Population projections for Canada, provinces and territories: 2009 to 2036. Catalogue no. 91-520-x. Ottawa, ON: Minister of Industry, 2010.
5. Statistics Canada. The Canadian population in 2011: age and sex. Catalogue no. 98-311-X2011001. Ottawa, ON: Minister of Industry, 2012.
6. World Health Organization. Active aging: a policy framework. Madrid: Second United Nations World Assembly on Ageing, 2002.
7. Plouffe LA, Kalache A. Towards global age-friendly cities: determining urban features that promote active aging. Journal of Urban Health 2010; 87(5): 733-739.
8. Federal, Provincial, Territorial Ministers Responsible for Seniors. Age-friendly rural and remote communities: a guide. Ottawa, ON: Minister of Industry, 2007.
9. Hanlon N, Halseth G. The greying of resource communities in northern British Columbia: implications for health care delivery in already-underserviced communities. The Canadian Geographer 2005; 49(1): 1-24.
10. Ryser L, Halseth G. Resolving mobility constraints impeding rural seniors' access to regionalized services. Journal of Aging and Social Policy, 2012; 24(3): 328-344.
11. Winterton R, Warburton J. Models of care for socially isolated older rural carers: barriers and implications. Rural and Remote Health, 11(3): 1678 (Online) 2011. Available: www.rrh.org.au (Accessed 19 February 2013).
12. Strasser R, Neusy AJ. Context counts: training health workers in and for rural and remote areas. Bulletin of the World Health Organization 2010; 88(10): 777-782.
13. Weeks WB, Wallace AE. Rural-urban differences in primary care physicians' practice patterns, characteristics, and incomes. Journal of Rural Health 2008; 24(2): 161-170.
14. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health, 9(2): 1060 (Online) 2009. Available: www.rrh.org.au (Accessed 19 February 2013).
15. Novek S, Menec VH. Older adults' perceptions of age-friendly communities in Canada: a photovoice study. Ageing & Society. (Online) 2013. http://dx.doi.org/10.1017/S0144686X1200150X (Accessed 6 December 2013).
16. Smith RJ, Lehning AJ, Dunkle RE. Conceptualizing age-friendly community characteristics in a sample of urban elders: an exploratory factor analysis. Journal of Gerontological Social Work 2013; 56(2): 90-111.
17. Ding D, Gebel K. Built environment, physical activity, and obesity: what have we learned from reviewing the literature? Health and Place 2012; 18(1): 100-105.
18. Rosso AL, Auchincloss AH, Michael YL. The urban built environment and mobility in older adults: a comprehensive review. Journal of Aging Research, doi:10.4061/2011/816106. (Online) 2011. Available: http://pubmedcentralcanada.ca/pmcc (Accessed 15 August 2011).
19. Saelens BE, Handy SL. Built environment correlates of walking: a review. Medicine & Science in Sports & Exercise 2008; 40(7): S550-S566.
20. Foster S, Giles-Corti B. The built environment, neighborhood crime and constrained physical activity: an exploration of inconsistent findings. Preventive Medicine 2008; 47(3): 241-251.
21. Alley D, Liebig P, Pynoos J, Banerjee T, Choi IH. Creating elder-friendly communities: preparing for an aging society. Journal of Gerontological Social Work 2007; 49(1/2): 1-18.
22. Lui CW, Everingham JA, Warburton J, Cuthill M, Bartlett H. What makes a community age-friendly: a review of the international literature. Australasian Journal on Aging 2009; 28(3): 116-121.
23. Menec VH, Means R, Keating N, Parkhurst G, Eales J. Conceptualizing age-friendly communities. Canadian Journal on Aging 2011; 30(3): 479-493.
24. Bronfenbrenner U. Ecological models of human development. In T Husen, T Poslethwaite (Eds.). International Encyclopedia of Education (2nd ed., Vol. 3). New York, NY: Elsevier Science, 1994; 1643-1647.
25. Stokols D. (1992). Establishing and maintaining healthy environments: toward a social ecology of health promotion. American Psychologist 1992; 47(1): 6-22.
26. Stokols D. Translating social ecological theory into guidelines for community health promotion. American Journal of Health Promotion 1996; 10(4): 282-298.
27. United Nations. World population aging. New York, NY: United Nations, 2009.
28. Dandy K, Bollman RD. Seniors in rural Canada. Rural and Small Town Canada Analysis Bulletin, Catalogue no. 21-006-X. Ottawa, ON: Statistics Canada, 2008.
29. Pong RW, Desmeules M, Lagacé C. Rural-urban disparities in health: how does Canada fare and how does Canada compare with Australia? Australian Journal of Rural Health 2009; 17(1): 58-64.
30. Smith KB, Humphreys JS, Wilson MG. Addressing the health disadvantage of rural populations: how does epidemiological evidence inform rural health policies and research? Australian Journal of Rural Health 2008; 16(2): 56-66.
31. Lavergne MR, Kephart G. Examining variations in health within rural Canada. Rural and Remote Health, 12, 1848 (Online) 2012. Available: www.rrh.org.au (Accessed 19 February 2013).
32. Bell S, Menec VH. 'You don't want to ask for the help'. The imperative of independence: is it related to social exclusion? Journal of Applied Gerontology. (Online) 2013. http://dx.doi.org/10.1177/0733464812469292 (Accessed 6 December 2013).
33. Menec VH, Hutton L, Newall N, Nowicki S, Spina J, Veselyuk D. How 'age-friendly' are rural communities and what community characteristics are related to age-friendliness? The case of rural Manitoba, Canada. Ageing & Society. (Online) 2013. http://dx.doi.org/10.1017/S0144686X13000627 (Accessed 6 December 2013).
34. duPlessis V, Beshiri R, Bollman RD. Definitions of rural. Rural and Small Town Canada Analysis Bulletin 2001; 3(3): 1-17.
35. McNiven C, Puderer H, Janes D. Census Metropolitan Area and Census Agglomeration Influenced Zones (MIZ): a description of the methodology. Catalogue no. 92F0138MIE2000002. Ottawa, ON: Statistics Canada, 2000.
36. McDowell I. Measures of self-perceived well-being. Journal of Psychosomatic Research 2010; 69(1): 69-79.
37. Idler EL, Benyamini Y. Self-rated health and mortality: a review of twenty-seven community studies. Journal of Health and Social Behavior 1997; 38(1): 21-37.
38. Lucas RE, Donnellan MB. Estimating the reliability of single-item life satisfaction measures: results from four national panel studies. Social Indicators Research 2012; 105(3): 323-331.
39. Berkman LF, Kawachi I (Eds.). Social epidemiology. New York, NY: Oxford, 2000.
40. Elgar FJ, Davis CG, Wohl MJ, Trites SJ, Zelenski JM, Martin MS. Social capital, health and life satisfaction in 50 countries. Health and Place 2011; 17(5): 1044-1053.
41. Oswald F, Jopp D, Rott C, Wahl HW. Is aging in place a resource for or risk to life satisfaction? Gerontologist 2011; 51(2): 238-250.
42. World Health Organization. Global age-friendly cities project. Geneva: World Health Organization, 2006.
43. Li H, Kyrouac GA, McManus DQ, Cranston RE, Hughes S. Unmet home care service needs of rural older adults with Alzheimer's disease: a perspective of informal caregivers. Journal of Gerontological Social Work 2012; 55(5): 409-425.
