full article:
Introduction
Cervical cancer is the second leading cause of cancer death in Latin America and the Caribbean (LAC), yet prevention and control efforts have been largely unsuccessful1. A growing body of evidence suggests that a single-visit screen-and-treat approach using visual inspection with acetic acid (VIA) and cryotherapy can be more effective and may be a more suitable option for resource-constrained settings than cytology-based strategies2-4. VIA has sensitivity equal to or higher than that of cytology5, and its results are immediately available, allowing for treatment of precancerous lesions with cryotherapy on the same visit. Even if referral to another facility is needed for women to receive cryotherapy, VIA increases women's chances of being treated by eliminating the need for an additional appointment to receive screening results. Finally, VIA and cryotherapy are inexpensive and can be performed by non-physicians4,6.
The Pan American Health Organization (PAHO) Regional Strategy for Comprehensive Cervical Cancer Prevention and Control developed for the period 2008-2015 incorporates these alternative technologies as part of the overall goal of strengthening health services from primary and secondary prevention to treatment and palliative care7. In the context of a broader collaboration between PAHO and the Centers for Disease Control and Prevention (CDC), representatives from these organizations met with Ministry of Health (MOH) cancer staff from Bolivia, Barbados, Guatemala, and Trinidad & Tobago in Atlanta on April 2009 to learn about these countries' programmatic needs. Bolivia was the first country that CDC supported in its collaboration with PAHO. Cervical cancer incidence and mortality rates in Bolivia are among the highest in the LAC region (36.4/100 000 and 16.7/100 000, respectively)1. Bolivia has the commitment to address its high burden of cervical cancer and has a well-developed plan for cervical cancer prevention and control8. The plan incorporates VIA and cryotherapy and defines cytology as the primary screening strategy.
In September 2009, staff from the local PAHO office and several divisions within CDC conducted a site visit to Bolivia to assess needs for screening and precancer treatment services, education strategies, laboratories, information and monitoring systems, cancer registries, and potential for human papillomavirus (HPV) vaccine introduction. The needs assessment was conducted through informal interviews with public health officials, hospital directors, and community-based organizations. Key areas for potential collaboration with the MOH were identified:
- increased capacity to conduct colposcopy and loop electrosurgical excision procedure (LEEP), especially in areas where cytology-based screening is well-established and functioning well
- increased capacity to conduct VIA and cryotherapy, with a focus on areas where access to cytology-based services is low
- increased public awareness and community education
- technical assistance for the creation of a population-based cancer registry
- assistance with HPV vaccine introduction.
Because VIA and cryotherapy are particularly suited to constrained-resource settings, CDC, PAHO, and the Bolivian MOH decided to focus on capacity building for the use of these technologies. Some technical assistance to provide colposcopy and LEEP, which are still needed for lesions that are not suitable for cryotherapy, was also provided9. This report describes the activities undertaken to increase cervical cancer prevention efforts in Bolivia, with a focus on VIA and cryotherapy and lessons learned from such activities. Workshops conducted to increase capacity for community education and the use of colposcopy and LEEP are also briefly discussed.
VIA and cryotherapy
In an effort to promote south-to-south collaboration within the region, CDC and PAHO partnered with a regional training excellence center on VIA and cryotherapy that has been operating within the Peruvian National Cancer Institute (INEN) since 200510. The center was established by PATH, Jhpiego, and the INEN and provides a comprehensive approach for the introduction of VIA and cryotherapy in LAC11. The materials and framework utilized for capacity-building activities in Bolivia have been tested, evaluated, and validated over time through the joint work of Jhpiego, PAHO, and other organizations that have been part of the Alliance for Cervical Cancer Prevention12.
Methodology utilized for training
The workshops utilized a teaching format that was competency-based: participants' performance was emphasized; the trainer acted as a facilitator and mentor rather than an instructor; and the participants' overall evaluation was based not only on knowledge acquisition, but also on the skills and abilities developed during both classroom simulation exercises and practice in clinical settings. The workshops also incorporated adult and observational learning techniques. Lastly, anatomical models, audiovisual aids, and practice in clinical settings were used to allow trainees to gain a basic level of skill to make proper therapeutic decisions and perform procedures.
Capacity-building strategy
Peruvian trainers outlined a series of steps for capacity building: (1) the training of providers through a 5-day basic course on clinical skills to perform procedures and provide counseling, (2) the selection of no more than 10 providers to participate in a 4-day Training-of-Trainers (TOT) course, (3) the replication of basic courses by Bolivian trainers who achieved the highest level of skill and competency in the TOT course, and (4) the identification of 'master instructors' who would be in charge of providing guidance for scaling up and ensuring sustainability. Based on this framework, a basic course on VIA and cryotherapy was piloted for a small group of Bolivian physicians recruited by the MOH. This initial workshop was conducted in Peru to expose participants to the changes introduced within the Peruvian healthcare system to successfully adopt VIA and cryotherapy. Based on the expressed commitment of this prominent group of Bolivian trainees, a second basic course was conducted in La Paz, the capital city of Bolivia, targeting a separate group of providers. The participants who demonstrated the highest level of skill and knowledge in either workshop were selected for a TOT course. All participants recruited for the workshops were actively involved in the provision of reproductive health services for women in health posts, health centers, or hospitals.
Evaluation by content area: knowledge acquisition and competency
Knowledge acquisition was evaluated at pre-test and post-test in both the basic and TOT workshops. Evaluated core content areas varied by workshop. The basic course focused on influencing attitudes on the benefits and appropriate use of VIA and cryotherapy, counseling women prior to and after the procedures, developing competence to perform VIA and cryotherapy, managing side effects and preventing infections. The TOT curriculum content areas included planning and implementing basic courses for VIA and cryotherapy that emphasize a competent, dynamic, and interactive approach to the learning process; providing engaging oral presentations; proper use of standardized survey tools to evaluate providers' competency; and tutoring participants prior to and during the provision of services in clinical settings.
The purpose of the pre-test was to establish a knowledge baseline and assess group strengths and weaknesses by content area. In line with the competency-based approach, a post-test was administered midway through each of the courses to assess gained knowledge and to match trainees who did not achieve a satisfactory score on a specific content area with a trainer that would provide individualized support and mentoring.
Competency of basic workshop trainees was evaluated in classroom activities and clinical settings using standardized step-by-step lists (Appendixes A-C). In the classroom, trainees performed pelvic exams with anatomical models, identified cervical pathology using visual aids, performed cryotherapy on inanimate objects, and provided patient counseling during role-playing exercises. After these skills were acquired, trainees counseled and performed procedures on pre-selected women under supervision.
A two-phase evaluation of participants' competency was used for the TOT course: (1) level of skill demonstrated in simulation exercises and oral presentations during the duration of the TOT workshop and (2) ability to properly plan and implement a basic course on VIA and cryotherapy with the tools and guidance provided by the Peruvian experts. TOT participants were divided into three groups based on their performance in planning and implementing the basic course: group A included participants who demonstrated the highest level of skill to independently plan and implement a basic course, group B included those who were prepared to replicate basic courses only under supervision, group C included participants who still needed more training and practice in classroom activities to become instructors. The INEN designed and administered all evaluation materials. CDC received technical reports with de-identified data.
Outcomes
A total of 61 Bolivian health professionals were trained to perform VIA and cryotherapy and provide related counseling through the implementation of four basic courses (Table 1). Of these, one course was implemented by TOT Bolivian participants under the guidance of Peruvian trainers and another was implemented without supervision in the province of Beni by two Bolivian trainers who demonstrated the highest level of skill during the TOT course.
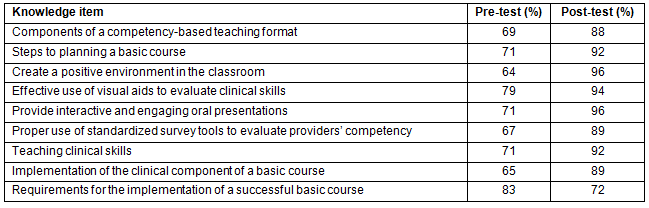
Most participants that attended basic courses received a satisfactory score at post-test (Table 1). For the two basic courses taught in La Paz, which included providers from selected provinces, the greatest improvements at post-test were in the areas of performing VIA and preventing infections (Table 2). In contrast, participants from the basic course implemented in Beni, which only included health professionals from this province, showed the most improvement in performing cryotherapy, and knowledge related to physiopathology, cancer risk factors, and HPV. Overall, familiarity with content areas was significantly lower among participants who attended the course in Beni, which included six family/general practitioners (FP/GPs) and six nurses, compared to those who attended the courses taught in La Paz which included mostly obstetricians and gynecologists. For the TOT workshop, content areas where participants were the least familiar at baseline included creating a positive learning environment (64%), implementing the clinical component of the course (65%), and using standardized tools to evaluate competency (67%) (Table 3). At post-test, however, these were some of the areas where participants showed the most improvement.
Participants from all courses provided feedback. When asked about ways to improve the basic workshop, many mentioned the need for more practice performing VIA in clinical settings. This, however, was not a problem reported in the workshop conducted in Beni, where recruitment efforts of eligible women were the most successful. Given the difficulty recruiting a high number of women who met criteria for cryotherapy, it was challenging to ensure that all trainees received proper practice to perform this procedure in a clinical setting. When asked about the hardest aspect of the basic workshop, many cited using the cryotherapy equipment properly and identifying acetowhite lesions while performing VIA.
Most of the feedback received from participants who attended the TOT course related to the planning and implementation of the basic workshop. Many stated that it was difficult to work with other trainers to plan and implement the basic workshop and that they had the most difficulty teaching trainees how to provide individual and group counseling. This finding is not surprising given that counseling is rarely emphasized during medical training; however, it highlights the need to pay special attention to the counseling component of TOT workshops to ensure that future trainers are well equipped to teach their colleagues how to properly provide this service to women. Participants' beliefs regarding the role, effectiveness, and acceptability of VIA and cryotherapy in Bolivia have been published elsewhere13.
Table 1: Participants in and outcomes of VIA and cryotherapy workshops
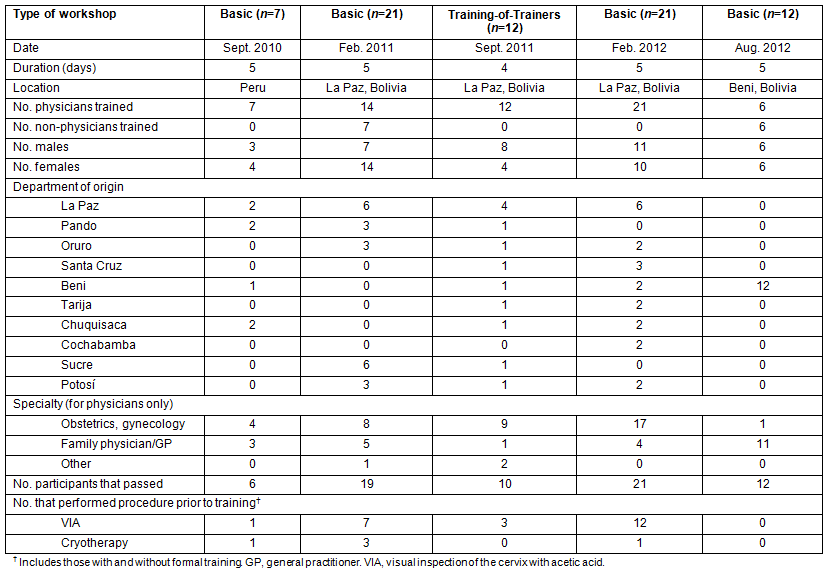
Table 2: Mean pre-test and post-test scores on knowledge items evaluated
during basic courses on VIA and cryotherapy, La Paz, Bolivia, 2010-2012 (N=61)
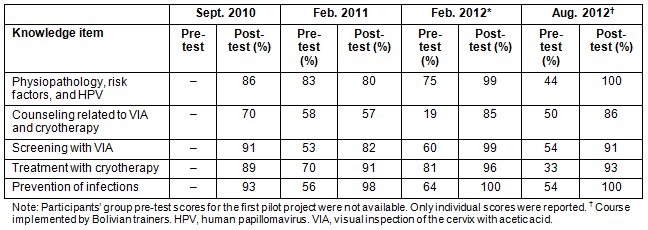
Table 3: Mean pre-test and post-test scores on knowledge items evaluated
during the Training-of-Trainers course, La Paz, Bolivia, 2011 (N=12)
Colposcopy and LEEP
CDC and PAHO partnered with the American Society for Colposcopy and Cervical Pathology (ASCCP) to support the MOH capacity-building efforts for colposcopy and LEEP. Four physicians with expertise in colposcopy and medical education from ASCCP's Committee on International Education and Humanitarian Outreach were sent to La Paz to train Bolivian physicians to perform these procedures14.
The teaching format included lectures, case reviews, interactive case presentations, and simulations. The curricula included discussion of the strengths and limitations of cytology-based screening, a review of the cytology and histology of the normal and abnormal cervix, and detailed instruction in colposcopic technique. Emphasis was placed on recognition of the colposcopic appearance of the normal and abnormal cervix as well as on management protocols for women with abnormal cytology and biopsy results. In simulations, participants practiced focusing the colposcope to conduct biopsies on inanimate objects15. LEEP was performed on chicken breasts through open-ended Styrofoam cups that simulated the cervix and vagina.
This structured training was followed by 2 days of mentored colposcopy examinations on preselected patients with abnormal cytology findings. The 2-day clinic experience at the Hospital de la Mujer in La Paz gave both trainers and learners the opportunity to work side-by-side caring for patients. Three exam rooms were set up for supervised patient exams. Each patient was examined by the ASCCP faculty mentor with two or three course participants. At each exam, technique was discussed, as were colposcopic findings and implications for management.
A total of 18 participants were trained in colposcopy and LEEP, 17 of whom indicated having performed cytology in the past and 10 of whom indicated having some prior colposcopy education. At the conclusion of the training, 94% indicated that they felt competent to perform and teach colposcopy. A total of 37 women received colposcopy examinations over 2 days. Most were biopsied, several underwent LEEP, and full spectrums of diseases were diagnosed, including cervical intraepithelial neoplasia 1, 2, and 3, as well as micro-invasive and invasive cancer. The clinic's physicians and staff arranged subsequent follow-up with the patients and management of disease identified in the clinical sessions.
Community education
Community health workers can play a pivotal role in increasing the demand for screening services and reducing cervical cancer disparities. To increase health promotion efforts a partnership with the Bolivian Cancer Foundation was formed to train lay health workers as promotoras de salud for cervical cancer prevention. The goal was to generate capacity among volunteers working in the Bolivian Cancer Foundation so that those who achieved the highest level of competency could replicate workshops in their communities.
Volunteers were exposed to two frameworks for community education: the Con Amor Aprendemos! program ('With Love We Learn'), which was developed by the Spirit Foundation in partnership with the American Cancer Society16, and a health education module developed by the Peruvian training excellence center. The curricula for both programs were developed to incorporate sociocultural values, language and literacy level issues, and communication styles specific to the Latina/Latino population. The Con Amor Aprendemos program prepares lay health workers to raise awareness about cervical cancer among both women and their male partners and has an important sexually transmitted infections component. The training excellence center health education course focuses specifically on training promotoras to provide education in their communities on VIA and cryotherapy to increase uptake of these procedures. The combination of these two complementary approaches provided the Bolivian Cancer Foundation with a wide range of tools and materials to plan and implement workshops that can be tailored to participants' needs. To date, the CDC-PAHO collaboration has supported the training of 33 promotoras affiliated with nine regional offices of the Bolivian Cancer Foundation. Plans to replicate courses are under way. More information is available at http://www.fubolcancer.com.
Discussion
The tools and evidence for the effectiveness and advantages of implementing VIA and cryotherapy in Bolivia and other LAC countries are available, but efforts are still needed to increase the visibility of these technologies and allow for their implementation through a systematic approach that ensures sustainability. With the goal of beginning a discussion to promote sustainability in the long term, PAHO convened a regional meeting in June 2011 with program managers from the MOH of 11 countries in LAC that have introduced VIA and cryotherapy, including Bolivia17. This meeting allowed program managers to share their experiences and discuss strategies to implement quality assurance mechanisms to monitor and evaluate the delivery of these services.
The experiences working in Bolivia demonstrate that capacity-building efforts for cervical cancer prevention in countries of the LAC region with the most limited infrastructure and resources are challenging but feasible. International organizations are in a strategic position to stimulate south-to-south collaborations within countries in the region. These collaborations are not only an excellent mechanism to leverage existing resources in LAC but also to increase capacity in a culturally sensitive manner, transfer knowledge and skills more successfully, increase feasibility of proposed activities, and encourage long-lasting partnerships that can contribute to the fulfillment of the millennium development goals18. The work of this multi-partner collaboration has provided valuable lessons that will be useful for the planning of the supervision and monitoring phase of this project as well as for future partnerships in the LAC region.
1. Historical allegiance to cytology-based screening is an obstacle to VIA implementation and scale-up in LAC. Coordinated action through a multi-sector platform with all stakeholders may be needed to shift attitudes concerning cervical cancer screening in the region. LAC poses unique challenges for the introduction of VIA and cryotherapy because most countries in the region have adopted a cytology-based strategy that has been in place for several decades. Increasingly, however, international organizations are discouraging low- and middle-income countries from adopting a cytology-based model given its quality assurance requirements and the workup needed for women to receive treatment19,20. Alternative technologies like VIA and cryotherapy may have an impact in Bolivia and other LAC countries if they are promoted through coordinated action and their acceptability is high, especially among physicians. Efforts are also needed to ensure that nurses receive training on VIA and cryotherapy, as these health professionals play a key role in increasing access among hard-to-reach populations. Recruiting nurses for this project was challenging due, in part, to a certain resistance within the MOH and the medical community. Historically, nurses in Bolivia and other countries in LAC have not played an active role in making therapeutic decisions or performing procedures21; however, the successful adoption and scale-up of alternative technologies for cervical cancer screening requires a shift in non-physicians' roles and responsibilities, especially in countries that need these technologies the most.
2. Countries' promotion of new technologies beyond their endorsement may play a key role in increasing acceptability of alternative technologies among physicians and allied health professionals. Bolivia's plan for cervical cancer prevention and control proposes ensuring that all facilities have the needed equipment and supplies to perform both cytology and VIA8. During the workshops, trainees often cited national norms prioritizing cytology as one of the reasons for their reluctance to perform VIA in their clinical practice. Confusion regarding the role and scope of introduction of these technologies was also common. Clear guidelines in countries' national norms about the role that alternative strategies may play if cytology remains the main screening strategy not only increase their acceptability but also facilitate their proper use. The World Health Organization is in the process of updating its guidelines for comprehensive cervical cancer control22. These guidelines may increase the visibility of VIA and cryotherapy in the region and clarify issues related to their proper use11.
3. VIA 'champions' among respected physicians may be an important step toward ensuring sustainability. Frequent changes in leadership within the MOH were a common challenge for the implementation of capacity-building activities. At different points in time, leadership at the MOH expressed different visions for this project. Some emphasized a broader scope and urgency to scale up and provide training for health professionals nationwide rather than focusing on a defined geographic location and group of trainees. Difficulty in limiting activities to a particular geographic area was also the experience of Colombia when VIA and cryotherapy were initially introduced23. Experiences of the authors and those of Colombia highlight the need to emphasize the importance of phasing projects gradually in a specific area as prerequisites to scaling up and having the wider impact that countries want and need.
The Bolivian trainers identified as 'champions' for VIA and cryotherapy provided continuity to this project during changes in leadership at the MOH. The work and commitment of these trainers allowed a focus on a specific population and defined geographic area within the province of Beni, which included the cities of Trinidad and Riveralta. Other countries that have implemented VIA, such as Zambia, provide examples of the key role that champions play to ensure successful demonstration projects in a context of political instability24.
4. 'Screen-and-treat approach' terminology may lead to confusion. Lack of capacity and resources to purchase cryotherapy equipment for primary care clinics may limit the ability of health centers and posts to perform VIA and cryotherapy during the same visit. For countries that have successfully adopted these technologies referral linkages from primary to secondary level healthcare facilities have been used within a specific geographic area for women who meet the criteria for treatment with cryotherapy11,25. Decisions on referral or a single-visit approach as the best strategy for a given area should be decided prior to the implementation of activities, to avoid confusion among stakeholders. Since many health professionals believe that VIA should only be considered as an alternative strategy if treatment with cryotherapy is provided on the same visit, emphasizing that referral to cryotherapy may be a more effective approach than adopting a cytology-based model is of equal importance. If a referral model is adopted, the optimal location of cryotherapy equipment within specific geographic areas as well as ensuring that women can access services for treatment of precancerous lesions may be important. Lastly, it should be highlighted that quality assurance mechanisms are a key requirement for VIA and cryotherapy to have an impact on cervical cancer control.
Next steps
For the third year of this project, which began on January 2013, the focus will be on supervision and follow-up in Beni. This province is working on a proposal document to conduct supervision of VIA related activities. The plan aims to achieve 60% screening coverage among a population of 21 338 women aged 30-50 years from the cities of Riveralta and Trinidad in a 3-year period. In line with the World Health Organization global monitoring framework26, the Bolivian MOH has recently approved the inclusion of VIA-related performance indicators in its surveillance system: (1) number of women screened with VIA, (2) number of women with positive VIA results, and (3) number of women with positive VIA results that received cryotherapy. At the same time, the national health authorities are improving the overall organization and quality of the national cytology-based cervical cancer program, with the technical assistance of PAHO, the MOH of Argentina, and other partners (personal communication S. Luciani, 26 February 2013). Thus, the opportunities exist in Bolivia to really scale up access to screening and treatment across the country, in order to reach more women with life-saving technologies.
Acknowledgments
This research was supported by an appointment to CDC's Research Participation Program administered by the Oak Ridge Institute for Science and Education (ORISE) through an interagency agreement between the US Department of Energy and CDC. ORISE had no involvement in the study design; collection, analysis, and interpretation of data; the writing of the manuscript; or the decision to submit this manuscript for publication.
References
1. Ferlay J, Shin HR, Bray F, Forman D, Mathers C, Parkin DM. GLOBOCAN 2008 v1.2, Cancer Incidence and Mortality Worldwide: IARC CancerBase No. 10 (Online) 2010. Available: http://globocan.iarc.fr (Accessed 11 January 2013).
2. Luciani S, Gonzales M, Munoz S, Jeronimo J, Robles S. Effectiveness of cryotherapy treatment for cervical intraepithelial neoplasia. International Journal of Gynecology & Obstetrics 2008; 101(2): 172-177.
3. Sankaranarayanan R, Esmy PO, Rajkumar R, Muwonge R, Swaminathan R, Shanthakumari S, et al. Effect of visual screening on cervical cancer incidence and mortality in Tamil Nadu, India: a cluster-randomised trial. Lancet 2007; 370(9585): 398-406.
4. Sherris J, Wittet S, Kleine A, Sellors J, Luciani S, Sankaranarayanan R, et al. Evidence-based, alternative cervical cancer screening approaches in low-resource settings. International Perspectives on Sexual and Reproductive Health 2009; 35(3): 147-154.
5. Sritipsukho P, Thaweekul Y. Accuracy of visual inspection with acetic acid (VIA) for cervical cancer screening: a systematic review. Chotmaihet thangphaet [Journal of the Medical Association of Thailand] 2010; 93(Suppl 7): S254-261.
6. Cervical Cancer Action. Progress in cervical cancer prevention: the CCA report card. (Online) 2011. Available: http://www.avac.org/ht/a/GetDocumentAction/i/33333. (Accessed 12 February 2012).
7. Pan American Health Organization (PAHO). Regional strategy and plan of action for cervical cancer prevention and control. (Online) 2007. Available: http://www.paho.org/hq/index.php?option=com_docman&task=doc_view&gid=15744&Itemid (Accessed 12 July 2010).
8. Ministerio de salud y deportes. Plan nacional de prevención, control, y seguimiento de cancer de cuello uterino 2009-2015 [in Spanish]. (Online) 2009. Available: http://es.scribd.com/doc/35745655/Plan-nacional-de-prevencion-control-y-seguimiento-de-cancer-de-cuello-uterino-2009-2015 (Accessed August 2010).
9. Santesso N, Schunemann H, Blumenthal P, De Vuyst H, Gage J, Garcia F, et al. World Health Organization Guidelines: use of cryotherapy for cervical intraepithelial neoplasia. International Journal of Gynecology & Obstetrics 2012, 118(2): 97-102.
10. Instituto Nacional de Enfermedades Neoplásicas. Escuela Latinoamericana de cáncer de cervix [in Spanish]. (Online) 2013. Available: http://esclatcc-peru.jimdo.com (Accessed 1 February 2013).
11. Cervical Cancer Action. Global advances in screening and treatment of cervical precancer. (Online) 2012. Available: http://www.cervicalcanceraction.org/multimedia/webinar11april2012/CCAwebinar_slides_11April2012.pdf. (Accessed 12 January 2013).
12. Jhpiego. ReproLine Plus: the source for technical expertise in global health practice. (Online) 2013. Available: http://reprolineplus.org/resources/trainer-educator (Accessed 10 February 2013).
13. Stormo AR, Altamirano VC, Perez-Castells M, Espey D, Padilla H, Panameno K, et al. Bolivian health providers' attitudes toward alternative technologies for cervical cancer prevention: a focus on visual inspection with acetic acid and cryotherapy. Journal of Women's Health 2012; 21(8): 801-808.
14. Waxman AG. ASCCP, moving forward. Journal of Lower Genital Tract Disease 2012; 16(3): 165-168.
15. Ferris DG, Waxman AG, Miller MD. Colposcopy and cervical biopsy educational training models. Family Medicine 1994; 26(1): 30-35.
16. Spirit Foundation, Inc. Fighting cervical cancer and other HPV diseases. (Online). Available: http://www.spiritfoundationinc.org (Accessed 20 February 2013).
17. Pan American Health Organization. Strategies for cervical cancer prevention using visual inspection with acetic acid screening and cryotherapy treatment: report of the PAHO workshops for Latin America and the Caribbean. (Online) 2011. Available: http://www2.paho.org/hq/index.php?option=com_content&view=category&layout=blog&id=3595&Itemid=3637&lang=en (Accessed 5 October 2012).
18. Pan American Health Organization. Triangular cooperation experience between the government of the Argentine Republic and the Pan-American Health Organization. (Online) 2009. Available: http://new.paho.org/sscoop/?p=2362 (Accessed 23 November 2012).
19. World Health Organization. WHO guidelines. Use of cryotherapy for cervical intraepithelial neoplasia. (Online) 2011. Available: http://whqlibdoc.who.int/publications/2011/9789241502856_eng.pdf (Accessed 5 January 2013).
20. United Nations Population Fund (UNFPA). Comprehensive cervical cancer and control: programme guidance for countries. (Online) 2011. Available: http://www.unfpa.org/public/op/preview/home/publications/pid/10413 (Accessed 12 May 2012).
21. Stormo AR, Cooper CP, Hawkins NA, Saraiya M. Physician characteristics and beliefs associated with use of pelvic examinations in asymptomatic women. Preventive Medicine 2012; 54(6): 415-421.
22. World Health Organization. Comprehensive cervical cancer control: a guide to essential practice. (Online) 2006. Available: http://whqlibdoc.who.int/publications/2006/9241547006_eng.pdf (Accessed 18 December 2012).
23. Murillo R. Approaches to cervical cancer screening in areas with unequal health services: the example of Colombia. In HPV Today 2012, 27, 12. (Online) Available: http://www.g-o-c.org/uploads/12nov_hpvtoday.pdf (Accessed 24 January 2013).
24. Mwanahamuntu MH, Sahasrabuddhe VV, Kapambwe S, Pfaendler KS, Chibwesha C, Mkumba G, et al. Advancing cervical cancer prevention initiatives in resource-constrained settings: insights from the Cervical Cancer Prevention Program in Zambia. PLoS Medicine 2011; 8(5): e1001032.
25. World Health Organization. Prevention of cervical cancer through screening using visual inspection with acetic acid (VIA) and treatment with cryotherapy: a demonstration project in six African countries: Malawi, Madagascar, Nigeria, Uganda, the United Republic of Tanzania, and Zambia. (Online) Available: http://apps.who.int/iris/bitstream/10665/75250/1/9789241503860_eng.pdf (Accessed 8 February 2013).
26. World Health Organization. Report of the formal meeting of member states to conclude the work on the comprehensive global monitoring framework, including indicators, and a set of voluntary global targets for the prevention and control of noncommunicable diseases. (Online) 2012. Available: http://apps.who.int/gb/NCDs/pdf/A_NCD_2-en.pdf (Accessed 31 January 2013).
________________________
Appendix A: Learning guide for counseling skills in visual inspection of the cervix with acetic acid (VIA) and cryotherapy
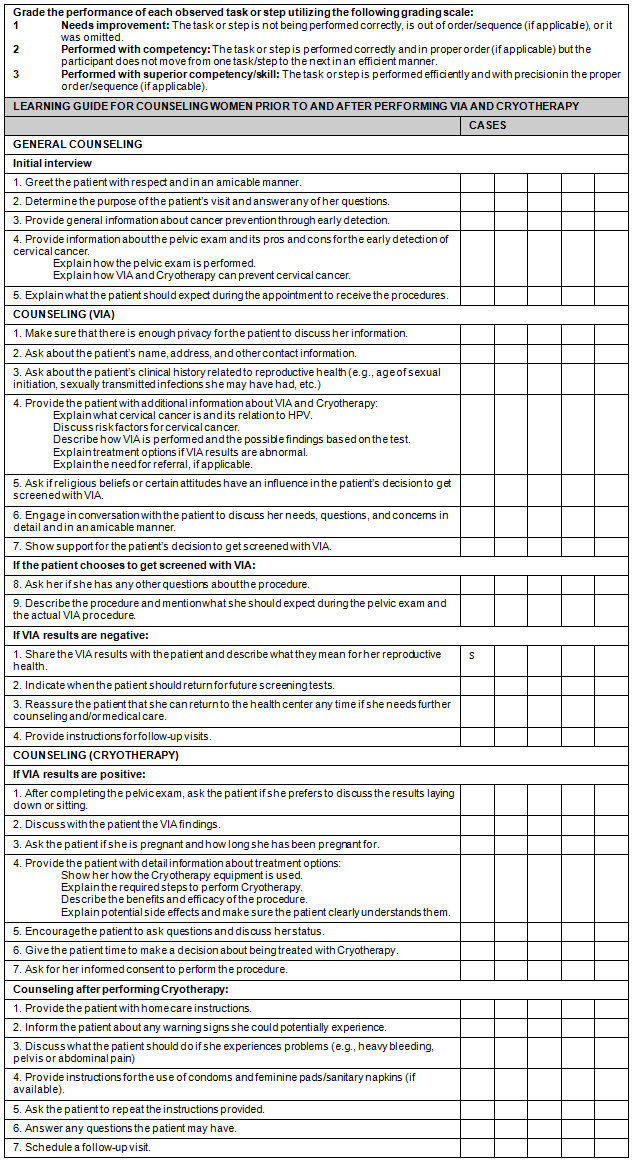
Appendix B: Learning guide for clinical skills in visual inspection of the cervix with acetic acid (VIA)
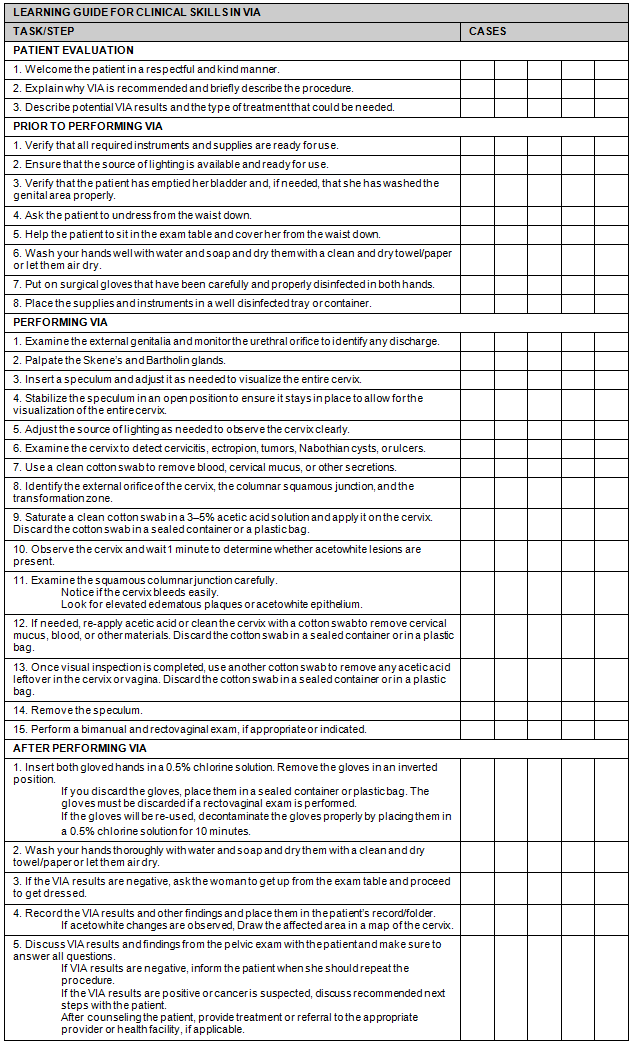
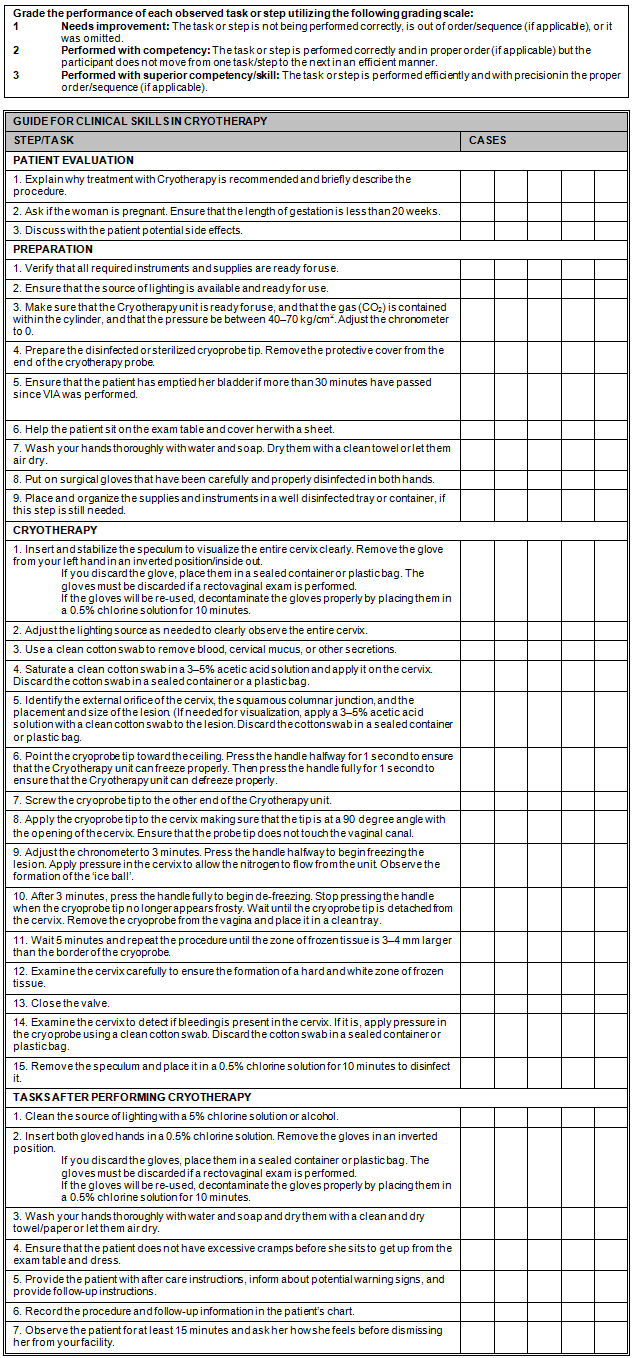
Appendix C: Guide for clinical skills in cryotherapy