The nutritional transition that has accompanied the process of global development has resulted in a demographic change in the profile of health and illness1,2. Undernutrition is considered by the World Health Organization (WHO) to be one of the principal causes of death in children and a threat to public health because of long-term consequences in childrenŽs physical and mental development3. On the other hand, overnutrition associated with development and 'progress' is also recognized by WHO as a public health problem because of its link to various chronic diseases such as diabetes, heart disease, stroke, and cancer. Thus, the process of development has not eliminated nutritional problems but, rather, has changed the demographic profile of nutritional deficiencies1,4,5.
Brazil has undergone immense development in the past 50 years, and the accompanying nutritional transition is evidenced by a 72% decrease in undernutrition (measured by height for age) among children over the past 25 years6-8. However, the development process has not affected all regions of the country equally. The most evident division in terms of socioeconomic development is the contrast between the industrialized south-eastern macro-region and the rural, remote, and far less developed north-eastern macro-region9,10. The northern region of Minas Gerais is a frontier between these macro-regions. Its political borders situate it within the south-eastern macro-region. Its indices of development are more similar to those of the north-eastern macro-region. It is the most remote region of the south-east, and more than 60% of the population of the region is rural11.
Many Brazilians are still living in degrading conditions of misery and hunger12. To address the needs of socially excluded Brazilians, the Brazilian government has implanted income transfer programs to assist poor families and help the nutritional status of low-income individuals. One such program, implemented in 2003, is called Bolsa Família (the Family Grant)13-15.
Through income transfer policies, the Family Grant program strives to positively impact the development of individuals by decreasing familial poverty and reinforcing the guaranteed rights of all to health, education, and social assistance. Recipient families are selected from a register of low-income families called Cadastro Único (the Single Register for Federal Social Assistance)13,15,16. This register is used to identify and characterize families whose income is less than half of the minimum wage or less than three minimum wages per household. Not all families registered in the Cadastro Único qualify for inclusion in the Family Grant program. The income level cutoff for inclusion in the program is currently less than half the cutoff level for inclusion in the register: $R140 (approximately equal to US$70) in per-person monthly income13,17,18.
Once a family is included in the Family Grant program, they receive a stipend of between R$80 (approx. US$40) and R$400 (approx. US$200) per month based on the number of people residing in the household. All members of the qualifying household must participate in health and education programs or the family may lose the funding. This approach to eradicating poverty and extreme poverty has garnered international attention13,16,18.
The Brazilian government also maintains the System for Alimentary and Nutritional Oversight (SISVAN), databanks aimed at promoting health by collecting ongoing information regarding the nutritional conditions of the population and factors that influence nutrition. SISVAN databanks dating back to the year 2008 are publicly available on the Internet using free government software (TabNet), and, using this program, it is possible to select SISVAN data for all recipients of the Family Grant program19-21.
The ongoing processes of social and economic development in Brazil between the years 2008 and 2012 are well documented. While the average income adjusted for purchasing power (PPP) of the Brazilian population has increased by nearly 20%, the Gini coefficient, that measures level of inequality, has decreased and the percentage in the lower classes has decreased12,14,18. The objective of the current study is to evaluate the change in nutritional status from 2008 to 2012 as per body mass index (BMI) standards. In this way the authors hope to add to understandings of how children included in the Family Grant program have been affected by the development process and consider how the health and educational aspects of the program may need to adjust to meet the changing needs of the recipient population.
This analysis of secondary data of the nutritional status of children in governmental databases was transversal, descriptive, and retrospective.
The sample was made up of children between the ages of 5 and 10, residing in the northern and north-eastern regions the state of Minas Gerais, Brazil, who were registered in the SISVAN databank as recipients in the Family Grant program in the years 2008 and 2012. The year 2008 was chosen because it was the first year with complete regional information on BMI available in the databank, and 2012 was chosen because it was the most recent with complete BMI data sets for the selected regions.
Considering that, in Brazil, public health is organized in networks with mid-level cities serving as administrative centers, data was selected from cities serving as micro-regional centers of care in the most rural and remote regions of the state of Minas Gerais listed in the SISVAN databank: Januária, Pirapora, Montes Claros, Diamantina, Pedra Azul, and Teófilo Otoni.
The weight-for-height statuses (BMI) of the participants were evaluated in comparison to five cutoff points established by the Brazilian Ministry of Health5: severely underweight (<-3), underweight (>-3 and <-2), ideal weight (>-2 and +1), obese (>+1 and <+3) and severely obese (>+3). For the purposes of this study these variables were reorganized into three categories: underweight (incorporating severely underweight and underweight), ideal weight (maintaining the original grouping), and overweight (incorporating severely obese and obese).
Data from 2008 and 2012 were collected directly from the SISVAN site (via http://nutricao.saude.gov.br) in February 2013. The data were entered into Statistical Package for the Social Sciences software v17 (SPSS; http://www.spss.com), and the following analyses were applied: descriptive statistics, confidence intervals (CI 95%) and χ2 tests (p<0.05).
Table 1 describes the distribution of underweight, ideal weight, and overweight children by municipal network in the years of interest. Figure 1 demonstrates the relative frequency of underweight, ideal weight, and overweight children in the overall study sample. The overall tendency evidenced in these data is a minimal reduction of underweight children and a much larger tendency towards movement from the ideal to overweight category.
Table 1: Weight status among children in select city networks in 2008 and 2012
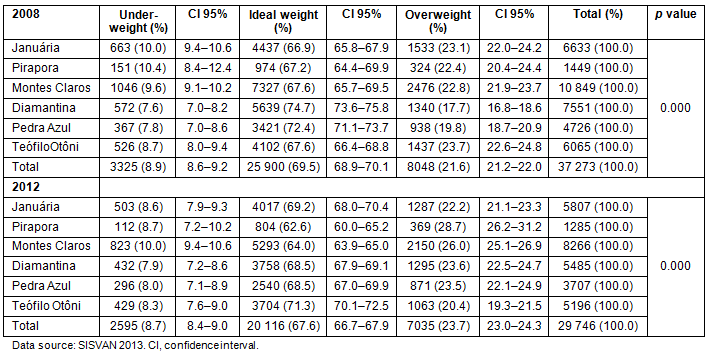
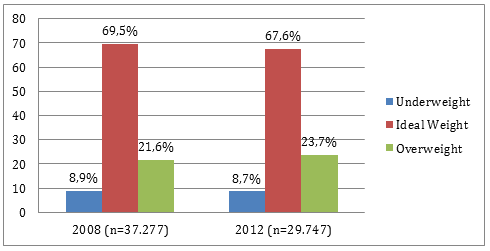
Figure 1: Underweight, ideal weight, and overweight children in northern and north-eastern Minas Gerais in 2008 and 2012.
(Data source: System for Alimentary and Nutritional Oversight databanks)
Discussion
With the implementation of SISVAN, the Brazilian government has demonstrated its concern regarding the collection of reliable and up-to-date information on the nutritional status of its citizens. This study, along with other similar published studies, demonstrates the importance of SISVAN and points out its value in recognizing tendencies in the population and giving direction to government programs, such as the health and educational components of the Family Grant program10,12,14.
The present study demonstrates variations in the frequencies of overweight, ideal weight, and underweight Family Grant program children between the years 2008 and 2012, with the overall tendency being an insignificant reduction of underweight children, and a movement of 2% from the ideal weight category to the overweight category. This result is consistent with other studies in developing regions of Brazil that have found similar changes in the BMI index7,9,13.
Both scientific and governmental studies in Brazil have demonstrated that the Family Grant program is reducing hunger in Brazil, especially in the poor regions that are frequently isolated from Brazil's large industrial centers. Poor families tend to use a major part of their limited resources to buy food, and food spending has been shown to be directly proportional to the financial situation of poor families13,22. These families tend to spend the majority of their food allowance on high calorie, inexpensive foods that offer a greater sensation of being full and more energy for physically demanding labor14,18.
The Brazilian Ministry of Health has also noted a significant increase in overweight children between the years 2008 and 2012, which has been evidenced in this study and in other similar studies1,3,5,11,18. These studies, realized after the initiation of the Family Grant program and the implantation of SISVAN, indicate that there is an overall trend towards increased weight among Brazilian children, especially in socially and economically excluded regions. The association of childhood obesity with increased risk for lifelong chronic disease is well documented in the international literature1,10,20. Therefore, programs directed at diminishing hunger among poor families must include nutritional education programs that address the need to choose foods that are nutritionally balanced10,13,22.
The Family Grant program already has mandatory health and education requirements. If children do not attend school regularly or if they do not have regular doctorŽs visits, the family may become disqualified from the program. Considering this existent infrastructure, the program may be particularly well suited to include mandatory health education regarding economical and balanced nutrition.
With the implementation of SISVAN, the Brazilian government has facilitated a close monitoring of how the current development processes are affecting its citizens' nutritional status. This monitoring can potentially help the government to avoid the pitfalls that have occurred in more developed countries where development has caused a transition from undernutrition to overnutrition.
However, this study shows that undernutrition among socially marginalized children living in this rural and remote region of Brazil has not been significantly changed by the Family Grant program. On the other hand, the incidence of overnutrition has increased. In order to ensure the best possible health outcomes later in life for the children targeted by this program, it may be necessary to consider how educational programs can better prepare recipient families to make healthy nutritional choices with new sources of income.
References
1. Winichagoon P. Thailand nutrition in transition: situation and challenges of maternal and child nutrition. Asia Pacific Journal of Clinical Nutrition 2013; 22(1): 6-15.
2. Carmen N, Ricardo H. The role of life events in mothers of malnourished children: the other side of malnutrition. Ciência & Saúde Coletiva 2011; 16(3): 1993-1999.
3. Martins IS, Marinho SP, de Oliveira DC, de Araújo EAC. Poverty, malnutrition and obesity: interrelationships among the nutritional status of members of the same family. Ciência & Saúde Coletiva 2007; 12(6): 1553-1565.
4. Sarturi JB, das Neves J, Karen Glazer Peres KG. Obesity in adult people: a population based study in a small town in South of Brazil, 2005. Ciência & Saúde Coletiva 2010; 15(1): 105-113.
5. Coutinho JG, Gentil PC, Tora N. Malnutrition and obesity in Brazil: dealing with the problem through a unified nutritional agenda. Cadernos de Saúde Pública 2008; 24(2): 332-340.
6. Souto TS, Oliveira MN, Casoy F, Machado EHS, Juliano Y, Gouvêa LC, et al. Anemia and per capita income in children enrolled in a childhood education center in São Paulo, Brazil. Revista Paulista de Pediatria 2007; 25(2): 161-166.
7. Oliveira FCC, Cotta RMM, Ribeiro AQ, Sant'Ana FR, Priore SE, Franceschini SCC. Nutritional status and determinants of short stature in children enrolled in the Bolsa Família Program. Epidemiologia e Serviços de Saúde. 2011; 20(1): 7-18.
8. Burlandy L. Transferência condicionada de renda e segurança alimentar e nutricional. Ciência & Saúde Coletiva. 2007; 12(6): 1441-1451.
9. Justo GF, Callo GQ, Carletti L, Molina MC. Nutritional extremes among school children in a rural Brazilian municipality. Rural and Remote Health 12(4): 2220. (Online) 2012 Available: www.rrh.org.au (Accessed 22 February 2013).
10. Custódio MB, Yuba TY, Cyrillo DC. Food and nutrition security policy in Brazil: an analysis of resource allocation. Revista Panamericana de Salud Publica 2013; 33(2): 144-150.
11. Freitas DA, Moreira G, Jones KM, Caldeira AP. Social exclusion and myiasis of the upper lip in a Brazilian rural resident. Rural and Remote Health 12: 2188. (Online) 2012. Available: www.rrh.org.au (Accessed 25 February 2013).
12. Oliveira FCC, Cotta RMM, Sant'Ana LFR, Priore SE, Franceschini SCC. Bolsa Família Program and child nutritional status: strategic challenges. Ciência & Saúde Coletiva 2011; 16(7): 3307-3316.
13. Silva DAS. Sobrepeso e obesidade em crianças de cinco a dez anos de idade beneficiárias do programa bolsa família no estado de Sergipe, Brasil. Revista Paulista de Pediatria 2011; 29(4): 529-535.
14. Traldi DRC, Almeida LMMC, Ferrante VLSB. Repercussions of the Bolsa Familia Program in the city of Araraquara, SP: a look at food security and nutritional status of beneficiaries. Interações 2012; 13(1): 23-37.
15. Ministério do Desenvolvimento Social e Combate a Fome. Normas e diretrizes para execução do Programa Bolsa Família. Brasilia: Brazilian Ministry of Health, 2012.
16. Simões P, Soares RB. Efeitos do Programa Bolsa Família na fecundidade das beneficiárias. Revista Brasileira de Economia 2012; 66(4): 445-468.
17. Senna MCM, Burlandy L, Monnerat GL, Schottz V, Magalhães R. The family grant program: new institutionalism in Brazilian social policy. Revista Katálysis 2007; 10(1): 86-94.
18. Santos LMP, Pasquim EM, dos Santos SMC. Cash transfer programs in Brazil: a multidimensional study of Bolsa Escola, Bolsa Alimentação and Cartão Alimentação Program implementation. Ciência & Saúde Coletiva 2011; 16(3): 1821-1834.
19. Damé PK, Pedroso MR, Marinho CL, Gonçalves VM, Duncan BB, Fisher PD, et al. Food and Nutritional Surveillance System (SISVAN) in children from Rio Grande do Sul State, Brazil: coverage, nutritional status, and data reliability. Cadernos de Saúde Publica. 2011; 27(11): 2155-2165.
20. Felisbino-Mendes MS, Campos MD, Lana FC. Nutritional assessment in children under 10 in Ferros, Minas Gerais. Revista da Escola de Enfermagem USP 2010; 44(2): 257-265.
21. Ministério da Saúde. Vigilância Alimentar e Nutricional - SISVAN: orientações básicas para a coleta, o processamento, a análise de dados e a informação em serviços de saúde. Brasilia: Ministério da Saúde, 2012.
22. Oliveira Fde C, Cotta RM, Sant'Ana LF, Priore SE, Franceschini Sdo C. Bolsa Família Program and child nutritional status: strategic challenges. Ciência &Saúde Coletiva. 2011; 16(7): 3307-3316.


