full article:
In Canada, the term Aboriginal refers to Canada's first peoples and their descendants, including First Nations (FN), Inuit and Métis peoples1. These three distinct groups of peoples each have unique histories, cultural beliefs and practices, and languages1. Of the more than one million individuals residing in Canada who identify themselves as Aboriginal (4% of the total population), more than half (53%) identify as FN2. It is estimated that approximately 40% of Canada's FN people are living on reserves2.
Although overweight and obesity in Canadian youth is a concern, Canadian Aboriginal youth and FN youth in particular are disproportionately affected3,4. The First Nations Regional Longitudinal Health Survey (RHS) reports on the health and wellness of Canada's FN people living on reserve. The most recent RHS (2008/10) reported prevalence rates of 29.9% for overweight and 12.8% for obesity (combined prevalence of 42.7%) for on-reserve FN youth aged 12-17 years4. For children aged 0-11 years, 20.3% are overweight and 42.2% are obese4. By contrast, in 2004 it was estimated that 18% of Canadian youth were overweight and 8% were obese, for a total combined prevalence rate of 26%3. More recent data from the Canadian Community Health Survey (2009-2011) reported prevalence rates of 19.5% and 11.6% for overweight and obesity (combined prevalence of 31.1%), respectively, in youth aged 5-17 years5. Considering that nearly half (48%) of the Canadian Aboriginal population is aged less than 24 years and that obese children are more likely to become obese adults, health promoting initiatives targeting healthy weights for Aboriginal youth are required6-8.
The etiology of overweight and obesity is complex, with myriad modifiable and non-modifiable contributors9. At the most simple level, overweight and obesity develop secondary to a positive energy balance, characterized by an energy intake in excess of energy expenditure. However, many factors influence the amount of food that a person consumes and the amount of physical activity they partake in; the social ecological model of health posits that an individual's health behavior is dependent on individual (intrapersonal), social-environmental (interpersonal), physical-environmental (community settings) and macrosystem (societal) influences9,10. Of interest, research worldwide has consistently demonstrated that many youth are unable to accurately identify whether their weight falls into a healthy or less healthy weight category11-18. A person's beliefs regarding their weight and motivations to change their body size can be affected by factors spanning all levels of the social ecological model9.
Little is currently known about the weight perceptions and weight control behaviors of Canadian FN youth living on reserve. It is known, however, that weight perceptions and body image are influenced by both societal and cultural norms, and therefore body weight perceptions and body weight ideals differ across cultures14,16,17,19. It has been recognized that, in some cultures, preferences and norms for body size may be different from those shared by the general Western population and that obesity may not always be seen as problematic20. For example, research in the Oji-Cree community of Sandy Lake, Ontario, Canada found that many individuals had a preference for larger body sizes - a preference especially marked among elders - some of whom associated thinness with memories of infectious diseases like tuberculosis21. Research with Cree populations in northern Quebec, Canada, found that, in some cases, larger body sizes were looked upon positively and that higher weights were sometimes associated with robustness and strength22.
Edwards George and Franko23 reviewed research pertaining to the eating behaviors and body weight ideals of various ethnic groups, including Aboriginal groups, and found that problematic eating behaviors and body image issues affect youth from diverse ethic backgrounds. An understanding of the weight perceptions and weight control behaviors of Canadian FN youth is needed because health promoting initiatives should be relevant and sensitive to the weight norms and preferences of the communities and cultures in which they are initiated20. For example, promoting the attainment and maintenance of a healthy body mass index (BMI) in a population where thinness is not idealized and larger body sizes are preferred would not be a desirable or ideal approach to improving health. Approaches promoting healthy eating habits, being adequately physically active and feeling good about oneself, regardless of body size, may be more appropriate24.
The present study investigated the weight perceptions of grade 6-8 FN youth (aged 10-14 years) residing in northern and southern Ontario communities between 2003 and 2010 with the goal of helping the communities to support the optimal health of their youth through sustainable, culturally appropriate initiatives tailored to their specific needs. The weight perceptions of the participating youth were compared to weight categories based on International Obesity Task Force (IOTF) cut points25,26, using self-reported height and weight data to calculate BMI. The appropriateness of eating-related weight control behaviors relative to BMI was also investigated.
Community-university research collaboration
The participating FN communities wish to take an active role in preserving the health of their youth and understanding the factors that affect it. With this in mind, the communities have been collaborating with researchers at the University of Waterloo for the past 10 years to obtain baseline data about the diets, physical activity levels and weight related behaviors of their youth27-37. The communities themselves are directly involved at all stages of the research process, and decisions about what types of data are collected and how they are used are made, ultimately, by the communities.
Prior to data collection, all university-based research assistants received cultural sensitivity training and were required to successfully complete a tutorial course in ethical research practices38. Whenever possible, community-based research assistants were trained by university-based researchers and participated in the data collection process, contributing to community research capacity. The data collected are used by the communities as a basis for collaborating with university-based researchers to plan health promoting initiatives for youth, mainly at the school and community level28,29,32,33,36. As part of this collaboration, the university helps to guide data collection and analysis, provides guidance for the implementation of health promoting initiatives, and provides support for the continuation of such programs (eg grant-writing support). Ultimately, the communities themselves decide on how the data will be used and what directions the programs will take. Members of the respective participating communities play an integral role in the initiation, evaluation and continuation of health promoting initiatives in their communities, providing for community ownership of the programs as well as volunteer, leadership and economic opportunities for community members. To date, the data collected in the participating communities has been used to tailor school-based health programs, all of which were planned, initiated and maintained by the communities themselves with grant-writing, research and funding support from the university-based research team28,29,32,33,36.
Communities and participants
Data were collected from a convenience sample of FN youth attending school in grades 6-8 between December 2003 and June 2010 in five northern Ontario communities located on the Western coast of James Bay and Hudson Bay and two southern Ontario communities. Youth were eligible to participate if they were enrolled in school in grade 6, 7 or 8, and in attendance on the days of data collection. Cree interpreters were available should students not be able to read or understand English. Of the participating communities, the northern communities are remote (at a great distance from a major city), isolated (not readily accessible by land) and accessible only by air year-round, by barge during the summer months and by seasonal ice road. The most southern of the northern communities is located 315 km by air from Timmins (travel hub to the northern communities) and 850 km by air from Toronto, Ontario's capital city. The most northern of these communities is located approximately 750 km by air from Timmins and more than 1300 km from Toronto. The two southern communities are not remote, but isolated. Both are islands accessible by ferry from the mainland and are located 100-170 km from Toronto.
All students who were present at school on the days of data collection and consented to the study participated. Following approval of the local education authorities and/or principals of the participating schools, passive parental consent was used. Information letters for parents/guardians were sent home with students by the participating schools at least 1 week prior to data collection. Any parent/guardian who did not wish to have their child participate in the study were asked to contact a school representative, local community health representative or research team representative, using the contact information available within the information letter (names and local phone numbers). Trained research assistants provided students with written and oral background information and students were required to consent to the study prior to participation. Thus, consent was on two levels: parental and student.
Weight perceptions and weight control behaviors
Data on weight perceptions and eating-related weight control behaviors were collected using the self-administered Waterloo Web-Based Eating Behaviour Questionnaire (WEB-Q), developed at the University of Waterloo39. The WEB-Q includes a 24-hour dietary recall, food frequency questionnaire and questions about weight perceptions and health habits. The present study focuses on the weight perceptions and weight control questions on the questionnaire, which were collected over 7 years as part of the larger research project aimed at providing the participating communities with diet, physical activity and health-related data with which to tailor health promoting initiatives for community-dwelling youth. Data from the 24-hour dietary recall and food frequency portions of the questionnaire have been reported elsewhere30,31.
The WEB-Q has been used since 2001 to survey over 20 000 Canadian youth, and has been validated in grade 6-8 youth, including FN youth from Fort Albany, Ontario (n=25, 2004)39. The WEB-Q (http://www.uwfbq.ca), was accessed by participating youth during school hours using school-based computers. Each student was provided with a random, computer-generated username and password with which to access the survey, such that no student would be identifiable by name. Trained research assistants (either university-based, community-based or both) provided youth with oral instructions prior to data collection and remained available while participants completed the questionnaires to answer questions and provide guidance, when necessary. Further, the first page of the questionnaire provides written instructions and information about the survey, including a check box where students are asked to click to agree to partake in the study.
For the purposes of this research, 'weight perceptions' was operationalized as a participant's description of their current body weight as compared to their peers; it also pertains to a participant's belief that their weight is either too high (overly heavy) or too low (overly thin). 'Weight control measures' was operationalized as a change in eating patterns in an attempt to modify one's body weight. In order to evaluate their weight perceptions and diet-related weight control measures, participants were prompted to respond to specific statements regarding (a) perceptions of their current weight compared to their peers, (b) concerns about their current weight and (c) current dietary initiatives they are partaking in with the goal of losing or gaining weight. The specific statements and response options (in italic below) used to assess these variables were provided on the WEB-Q as follows:
- (a): I would described my weight as; 'below average', 'average' or 'above average'
- (b-1): I am concerned that my weight is too low; 'definitely not', 'not really', 'neither', 'kind of' or 'really'
- (b-2): I am concerned that my weight is too high; 'definitely not', 'not really', 'neither', 'kind of' or 'really'
- (c-1): I am eating more than usual to try to gain weight; 'definitely not', 'not really', 'neither', 'kind of' or 'really'
- (c-2): I am eating less than usual to try to lose weight; 'definitely not', 'not really', 'neither', 'kind of' or 'really'.
As previously described, the questionnaire was completed as part of a larger research project, such that the response options were not all relevant for the current investigation. For the purposes of this secondary data analysis, the responses for questions (b) and (c) were collapsed to 'no' (including 'definitely not' and 'not really') and 'yes' (including 'kind of' and 'really'). 'Neither' was recoded as a non-response because it was not meaningful for the purposes of this study.
Anthropometry and body mass index
The WEB-Q was used to collect basic demographic and anthropometric information from students including age (years), grade, height (cm) and mass (kg). With the help of a trained research assistant, students' heights were measured using a measuring tape affixed to a wall. After being informed of their height, students would enter this data into the appropriate section of the WEB-Q, with the help of a research assistant when necessary. In an effort to maintain confidentiality and in accordance with the wishes of the participating communities and ethical research protocols, students weighed themselves on a standard portable weigh scale located in a quiet hallway, outside of the room where participants were completing the survey. Students were provided with oral instructions on how to use the weigh scales and research assistants were present if students required assistance. After measuring their weight, students would enter this information into the online survey. Although errors in self-reporting of heights and weights cannot be ruled out, this method of data collection was agreed upon between the research team and the participating communities as a culturally appropriate method to measure heights and weights, and is undoubtedly more accurate than self-reported height and weight data collected without the measurement tools provided. The fact that research assistants were present to guide participants through the measurement process and help those requiring assistance, when necessary, likely improved the accuracy of the results. Further, this method of data collection assured a higher degree of privacy and confidentiality for participants, increasing the likelihood of honest responses and a reduction in social desirability bias40.
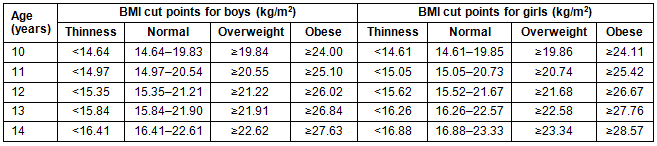
Body mass index was calculated to the nearest 0.1 kg/m2, based on the self-reported heights and weights entered into the WEB-Q. Students were classified according to four BMI categories ('thinness', 'normal', 'overweight' and 'obese') based on IOTF cut points (Table 1)25,26. These cut points are based on common BMI cut points used in adults (≤18.5 for thinness, 18.5-24.9 for normal, 25-29.9 for overweight and ≥30 for obese) and extrapolated for use in youth under 18 years of age25,26. Although not specific to FN youth, the IOTF cut points were devised from a heterogeneous, international sample25,26.
Table 1: International Obesity Task Force cut points used to classify participating youth into the body mass index (BMI) categories of 'thinness', 'normal', 'overweight' or 'obese'25,26
Data analysis
Statistical analyses were performed using the Statistical Package for the Social Sciences v21 (SPSS; http://www-01.ibm.com/software/analytics/spss/). The p value of significance for all analyses was established a priori at ≤0.05. Frequency statistics were computed in the comparison of measured BMI and weight perceptions and weight control behaviors, using cross-tabulations. Pearson Χ2 tests were used to compare the cross-tabulated categorical variables. Adjusted standardized residuals were used to determine which cells contributed to statistically significant results. Adjusted standardized residuals are preferred over the standardized residuals for checking for normality41. All analyses were stratified by sex.
Ethics approval
All research activities were carried out with approval from the Office of Research Ethics at the University of Waterloo, Ontario, Canada (#15402), in partnership with the Chiefs and Councils and local Education Authorities (local FN governing boards) in the participating communities and in accordance with the FN principles of OCAPTM42. The OCAP principles refer to the right of FN communities to own, protect and control data collection processes in their communities, allowing communities to make decisions about how, why and by whom data are collected, used and shared42.
Population demographics
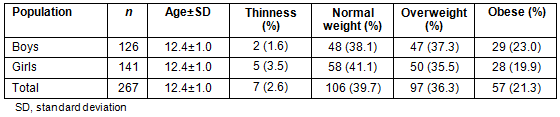
All students who attended school on the days of data collection participated in the study. No students were excluded based on parental consent or personal consent to participate. As much as possible, students who were absent on the original data collection days were provided with the opportunity to participate at a later date to optimize participation. Further, data collection days were not scheduled on days when cultural events or trips were planned. Based on the total number of students enrolled in school at the time of data collection in the respective communities, participation rates ranged from 72% to 96%31. Of the 267 participating FN youth, 47.2% were male and 52.8% were female (Table 2). Overall rates of overweight and obesity within the population were 36.3% and 21.3%, respectively (combined prevalence of 57.4%). Only 2.6% of youth fell below the BMI cut point for thinness. There were no significant differences in rates of overweight, obesity or thinness between boys and girls, or by age.
Table 2: Characteristics of the participating First Nations youth
Weight perceptions
The responses of youth to the WEB-Q questions that were related to the perceptions of their current weight are presented in Tables 3 and 4. For both boys (p=0.003) and girls (p=0.018) there was a significant relationship between perceived weight status and BMI. Notably, nearly one-quarter (23.9%) of normal weight boys reported that their weight was below average and only 6.5% reported that their weight was above average. By contrast, only 9.3% of normal weight girls reported that their weight was below average and 11.1% reported that their weight was above average. A greater proportion of overweight boys reported that their weight was average (83.0%) as compared to girls (69.4%). The same was true for boys and girls falling within the obese weight category: about half of obese boys (51.9%) felt that their weight was average as compared to only about one-third (34.6%) of obese girls. A greater proportion of obese girls believed that their weight was above average (46.2%) compared to boys (33.3%). Interestingly, 14.8% of obese boys and nearly one-fifth of obese girls (19.2%) believed that their weight was below average.
The belief that one's weight was too low was not significantly associated with BMI for either boys or girls. However, it is interesting that about one-tenth of both overweight boys (9.4%) and girls (10.8%) reported being concerned that their weight was too low. Further, 4.5% of obese boys and 5.0% of obese girls shared the same concern. Body mass index was, however, significantly associated with being concerned that one's weight was too high for both boys (p=0.003) and girls (p=0.001). Far more normal weight girls (23.9%) shared this concern as compared to boys (5.9%). For the overweight category, similar proportions of boys (26.5%) and girls (29.7%) believed that their weight was too high. In the obese category, a far greater proportion of girls (71.4%) shared this concern as compared to boys (47.8%).
Table 3: Distribution of responses on the Waterloo Web-Based Eating Behaviour Questionnaire to questions about weight perceptions and eating-related weight control behaviors by body mass index category
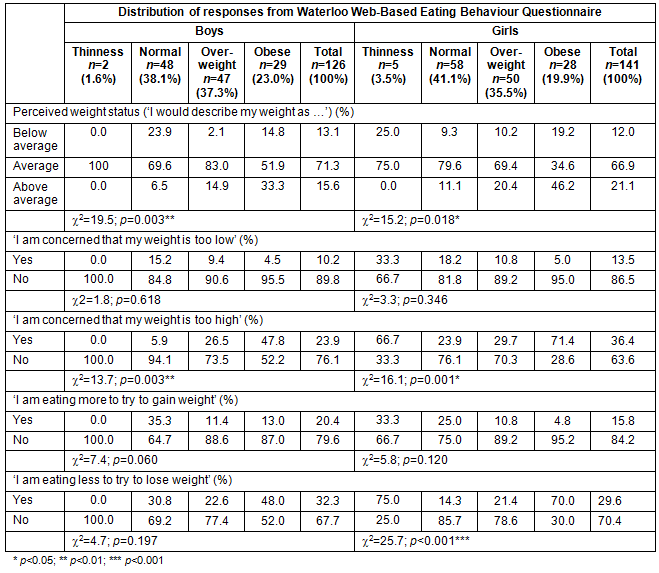 Table 4: Adjusted standardized residuals for the χ2 test of weight perceptions and weight control behaviors compared to measured body mass index category
Table 4: Adjusted standardized residuals for the χ2 test of weight perceptions and weight control behaviors compared to measured body mass index category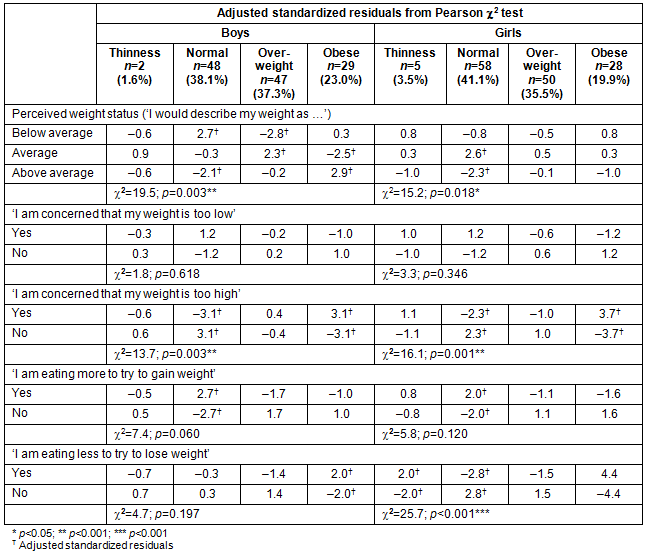
Eating-related weight control measures
There was no significant relationship between eating more with the goal of weight gain and BMI category for either boys or girls. However, it is interesting that 35.3% of normal weight boys and one quarter (25.0%) of normal weight girls reported actively trying to eat more to gain weight. Further, about one-tenth of both overweight boys (11.4%) and girls (10.8%) reported actively trying to gain weight. Of obese youth, 13.0% of boys and 4.8% of girls were trying to gain weight.
By contrast, there was a significant association between eating less to try to lose weight and BMI category for girls (p<0.001) but not boys. Of note, however, is that nearly one-third (30.8%) of normal weight boys were eating less to lose weight, compared to only 14.3% of normal weight girls. Of the girls falling into the thinness category, 75% were trying to lose weight. Similar proportions of overweight boys (22.6%) and girls (21.4%) were trying to lose weight. However, a far larger proportion of obese girls (70%) were trying to lose weight as compared to boys (48.0%).
Discussion
To the authors' knowledge, little research exists examining the weight perceptions and eating-related weight control behaviors of FN youth living on reserve in Canada. The present study adds to the available data on the topic and provides a foundation for future research. Further, this research provides new insights for the participating communities into the weight perceptions and body size ideals of their youth and may be used, in collaboration with university-based partners, to help tailor health promoting initiatives for the communities' youth. The rates of overweight and obesity in this study, although not surprising given figures reported in research with other Canadian FNs, were in excess of those reported in the most recent RHS4,43. Clearly, programs and initiatives to promote healthy weights in the youth of these communities are warranted. Although contributors to excess weight (eg diet, physical activity) may be affected by individual, social environmental, physical environmental and macrosystem influences9, it is not in doubt that these factors are amenable to change. In planning initiatives promoting healthy weights in the participating communities, taking into account the current perspectives of the targeted youth may improve the relevance, cultural sensitivity and effectiveness of such projects.
The majority of participants classified their weight as 'average'. It is notable as well that a large proportion of both overweight boys and girls considered their weights to be 'average'. Given that 60.3% of boys and 55.4% of girls were either overweight or obese, this should not be surprising. The current research only investigated whether or not youth perceived their weight as 'average' and not if they believed that heavier weights were 'the right weight' or not, nor whether these weights were healthy. It is possible, however, given the large proportion of overweight and obese youth in the sample in addition to the fact that most overweight youth believed their weight to be 'average', that heavier weights have been normalized within the populations studied. This phenomenon has been observed in other Aboriginal populations: Martin et al19 found that Native American youth were likely to perceive objectively heavier weights as 'about the right weight' or healthy. Furthermore, research by Willows et al44 found that, in a sample of Cree children from Quebec, Canada, although the majority of children were overweight or obese, most thought that their body size was 'just right'. This is concerning given that heavier body weights in youth have been shown to persist into adulthood and overweight in adults has been associated with higher rates of chronic disease11,13,17,45,46. Furthermore, it has been suggested that youth who do not recognize that they are carrying excess weight may not be motivated to make positive changes in an effort to achieve a healthy body weight11,13,47.
Across all weight categories, girls were more concerned than boys that their weight was too high. Most notably, large proportions of girls falling into the thinness or normal weight categories believed that their weight was too high, while very few boys in these weight categories felt the same. These findings suggest that FN girls in the participating communities may be more weight conscious, or prefer lower weights compared to boys. Similar findings have been observed in research with non-Aboriginal youth, where girls tend to prefer leaner body sizes as compared to boys, and normal weight and even slightly underweight girls are more likely to prefer thinner body sizes45,48. It is plausible that gender may be playing a role in the desire for a thinner figure, regardless of ethnicity. Conversely, it is particularly interesting that one-quarter of normal weight girls in the current study were attempting to gain weight. Previous qualitative research with young Aboriginal women has revealed that being 'skinny' is not necessarily accepted, and that being overweight is the acceptable traditional cultural norm49. It is possible that the participating girls are feeling differing pressures, including both traditional cultural pressures and modern media pressures that are influencing their body weight ideals.
As many FN youth from the participating communities have access to satellite television and the internet (at least at school if not at home), the fact that many girls in the thinness and normal weight categories feel their weight is too high suggests that even girls living in isolated communities may be exposed to and aware of the urban North American ideal of a slim physique, even if it is not traditionally part of their culture. Research investigating the weight ideals of youth living in the rural Appalachian region of West Virginia, USA, found that media influences (eg television, magazines) are still pervasive and have an impact on the body image of these youth, especially girls, despite the remoteness of the location in which they live50. Despite these findings, relatively few overweight boys and girls considered their weight to be too high. Fleming et al49 cited similar results in their study in which qualitative interviews with young Aboriginal women revealed feeling torn between the ideals of their own Aboriginal culture and the 'White' culture in which they lived. Also, the majority of obese girls in the current study believed that their weight was too high, while less than half of obese boys believed the same. Further, boys were more likely than girls in all weight categories to be trying to gain weight. It is possible that boys in this population prefer a larger, more robust physique. Similar findings have been reported in non-Aboriginal youth, where boys are more likely to consider themselves to be 'thin' and thus be attempting to gain weight11,12.
Evidence indicates that energy-reduced diets are appropriate for the treatment of overweight and obesity, even in youth, and are not likely to affect long-term growth51-57. In the current study, the majority of obese girls reported eating less to try to lose weight while less than half of obese boys reported the same. These results are in support of research indicating that girls are more likely than boys to be trying to lose weight12,58. Still, many overweight and obese youth did not report currently taking any dietary action to try to lose weight. This does not, however, mean that they are unaware of the risks of overweight, nor that they do not wish to adopt a healthy lifestyle. Previous research with the participating communities elucidated numerous barriers for youth to eating healthy foods and partaking in organized physical activity; it may not be easy or even possible for youth to take control of their own weight29,36,37. Recent research in one community, for example, found that the high cost, inadequate selection and poor quality of fresh vegetables and fruit and low fat dairy products at the local store were major barriers to their consumption28,36. In many remote communities, nutrient-dense foods may be up to three to four times more costly than in urban centres59. Less healthy foods are often more affordable and accessible; following a healthy diet in an effort to attain and maintain a healthy body weight may not even be a choice. Along with university-based collaborators, the communities are making strides toward providing opportunities for youth to make healthy choices through school-based health initiatives28,29,32-34,36,37.
Of particular interest is the fact that nearly one-third of normal weight boys were attempting to lose weight, a much larger proportion than observed even in girls. Research in school-aged youth has suggested that boys tend to prefer larger body sizes and/or more muscular physiques; however, it is possible that some of the boys in the present study are now feeling pressure to adopt a thin physique, similar to the pressures normally associated with girls58. These findings are converse to much of the research into the weight perceptions and body size ideals of Aboriginal youth, which report preferences for larger body sizes21,22. These youth seem to be an exception to the weight perceptions normally expected from boys based on current literature, and future investigations should focus on further elucidating the reasoning and pressures behind these perceptions.
Relevance to participating communities
As part of the ongoing research collaboration between the participating communities and the university-based research team, the knowledge gained through the present research may be used to tailor current health promoting initiatives and also to initiate relevant new initiatives aimed at providing youth with opportunities to make healthy choices. For example, the present research identified differences between the weight perceptions and weight control measures of boys and girls. This information may be used to tailor separate health messages - positive messages for girls may not be relevant for boys, and vice-versa. Further, the findings suggest that FN youth living on reserve may share some of the same weight perceptions as non-Aboriginal youth, including a preference for smaller body sizes for girls and for larger, more robust physiques for boys. Concomitantly, some of the findings suggest that Aboriginal youth may have ideals that are different from what is the typical urban Western ideal (eg normal weight boys wanting to be thinner, or normal weight youth wanting to gain weight). Current initiatives have focused on providing youth with opportunities to make healthy choices, including providing them with the chance to choose healthy foods at school and partake in structured physical activities28,29,32-34,36,60. However, providing healthy choices may not be enough. Programs need to be tailored to the views and ideals of youth, should be sensitive to these views and should promote healthy weights in a positive way. An emphasis on body size acceptance and being healthy, no matter what one's body size, may be a relevant addition to these programs, for boys and girls alike.
Limitations
It is important to note that although the BMI cut points used in this study were the result of data collected from a heterogeneous worldwide population, these may not be completely appropriate for FN youth25,26. To the authors' knowledge, there exist no specific BMI cut points for FN youth at this time. The cut points used in this study may have therefore incorrectly classified youth as overweight or obese when they were in fact not over-fat. This is a limitation of using BMI as a proxy for body fatness in any population; however, the cut points used in the current study were relatively conservative. World Health Organization cutoffs, for example, would have resulted in even higher prevalence rates of overweight and obesity in the study population compared to the IOTF cut points used61.
Because the data used in the current study were collected over 7 years, the possibility of historical bias cannot be ignored. Perceptions are likely changing over time and results may have differed should the data have been collected all at the same time point. In the context of the current research, this was not feasible. Data were collected at times that were convenient to the communities, as well as when resources allowed for travel to the communities. Future investigations should optimally aim to collect data over a much shorter time span.
The present study provides a unique investigation into the weight perceptions and weight control behaviors of on-reserve FN youth living in isolated communities in Ontario, Canada. For the participating communities, these data will help to tailor health promoting initiatives such that the messages are relevant to current perceptions and customized for both boys and girls. Because each FN communities is unique, the results may not be generalizable to all communities but may be relevant for similarly remote and/or isolated communities. The participating youth shared some of the same weight perceptions observed in non-Aboriginal youth; this may be representative of the body ideals of urban North American culture, which may be becoming more pervasive even in isolated FN communities. Some perceptions (eg a large proportion of normal weight male youth wanting to lose weight, large proportions of normal weight youth trying to gain weight), however, differed from those expected. Future research should focus on better understanding the contributors to current weight perceptions in this population, including media, parental, cultural, peer and community influences. The accuracy of the weight perceptions and health beliefs of FN youth and the pressures on both FN boys and girls to maintain a certain weight ideal are warranted.
Acknowledgements
We would like to thank the FN communities for their participation and acknowledge the contributions of those who aided in data collection, and Alex Stephen for field transportation. This research was funded by the Canadian Institutes of Health Research (CIHR), Canada's Research-Based Pharmaceutical Companies Health Research Foundation, Health Canada's First Nations and Inuit Health Branch, the Danone Institute of Canada and the Ontario Ministry of Research and Innovation. Stipend support was funded by Cancer Care Ontario and the CIHR Training Grant in Population Intervention for Chronic Disease Prevention: A Pan-Canadian Program (Grant #:53893).
References
1. Aboriginal Affairs and Northern Development Canada. Aboriginal peoples and communities. (Online) 2013. Available: http://www.aadnc-aandc.gc.ca/eng/1100100013785/1304467449155 (Accessed 13 November 2013).
2. Aboriginal Affairs and Northern Development Canada. First Nations. (Online) 2013. Available: http://www.aadnc-aandc.gc.ca/eng/1100100013791/1100100013795 (Accessed 13 November 2013).
3. Shields M. Overweight and obesity among children and youth. Health Reports 2006; 17(3): 27-42.
4. First Nations Information Governance Centre. First Nations Regional Health Survey (RHS) 2008/10: national report on adults, youth and children living in First Nations communities. Ottawa: FNIGC, 2012.
5. Roberts KC, Shields M, de Groh M, Aziz A, Gilbert J-A. Overweight and obesity in children and adolescents: results from the 2009 to 2011 Canadian Health Measures Survey. Health Reports 2012; 23(3): 37-41.
6. Freedman DS, Dietz WH, Srinivasan SR, Berenson GS. The relation of overweight to cardiovascular risk factors among children and adolescents: the Bogalusa heart study. Pediatrics 1999; 103(6 Pt 1): 1175-1182.
7. Nicklas TA, Baranowski T, Cullen KW, Berenson G. Eating patterns, dietary quality and obesity. Journal of the American College of Nutrition 2001; 20(6): 599-608.
8. Statistics Canada. Aboriginal Peoples in Canada in 2006: Inuit, Métis and First Nations, 2006 Census. (Online) 2008. Available: http://www5.statcan.gc.ca/bsolc/olc-cel/olc-cel?catno=97-558-XIE2006001&lang=eng#formatdisp (Accessed 12 November 2013).
9. Story M, Neumark-Sztainer D, French S. Individual and environmental influences on adolescent eating behaviours. Journal of the American Dietetic Association 2002; 102(3 Suppl): S40-S51.
10. Glanz K, Rimer BK, Viswanath K. Health behavior and health education, 4th edn. San Francisco, CA: Jossey-Bass, 2008.
11. Desmond SM, Price JH, Gray N, O'Connell JK. The etiology of adolescents' perceptions of their weight. Journal of Youth and Adolescence 1986; 15(6): 461-474.
12. Kilpatrick M, Ohannessian C, Bartholomew JB. Adolescent weight managements and perceptions: an analysis of the National Longitudinal Study of Adolescent Health. Journal of School Health 1999; 69(4): 148-152.
13. Strauss RS. Self-reported weight status and dieting in a cross-sectional sample of young adolescents: National Health and Nutrition Examination Survey III. Archives of Pediatrics & Adolescent Medicine 1999; 153(7): 741-747.
14. Brener ND, Eaton DK, Lowry R, McManus T. The association between weight perception and BMI among high school students. Obesity Research 2004; 12(11): 1866-1874.
15. Viner RM, Haines MM, Taylor SJ, Head J, Booy R, Stansfeld S. Body mass, weight control behaviours, weight perception and emotional well being in a multiethnic sample of early adolescents. International Journal of Obesity 2006; 30(10): 1514-1521.
16. Standley R, Sullivan V, Wardle J. Self-perceived weight in adolescents: over-estimation or under-estimation? Body Image 2009; 6(1): 56-59.
17. Edwards NM, Pettingell S, Borowski IW. Where perception meets reality: self-perception of weight in overweight adolescents. Pediatrics 2010; 125(3): 452-458.
18. Park E. Overestimation and underestimation: adolescents' weight perception in comparison to BMI-based weight status and how it varies across socio-demographic factors. Journal of School Health 2010; 81(2): 57-64.
19. Martin MA, May AL, Frisco ML. Equal weights but different weight perceptions among US adolescents. Journal of Health Psychology 2010; 15(4): 493-503.
20. Davis SP, Northington L, Kolar K. Cultural considerations for treatment of childhood obesity. Journal of Cultural Diversity 2000; 7(4): 128-132.
21. Gittlesohn J, Harris SB, Thorne-Lyman AI, Hanley AJ, Barnie A, Zinman B. Body image concepts differ by age and sex in an Ojibway-Cree community in Canada. Journal of Nutrition 1996; 126(12): 2990-3000.
22. Boston P, Jordan S, MacNamara E, Kozolanka K, Bobbish-Rondeau E, Iserhoff H, et al. Using participatory action research to understand the meanings Aboriginal Canadians attribute to the incidence of diabetes. Chronic Diseases in Canada 1997; 18(1): 5-12.
23. Edwards George JB, Franko DL. Cultural issues in eating pathology and body image among children and adolescents. Journal of Pediatric Psychology 2010; 35(3): 231-242.
24. Robison J. Health At Every Size: toward a new paradigm of weight and health. Medscape General Medicine 2005; 7(3): 13.
25. Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. British Medical Journal 2000; 320(7244): 1240-1243.
26. Cole TJ, Flegal KM, Nicholls D, Jackson AA. Body mass index cut offs to define thinness in children and adolescents: international survey. British Medical Journal 2007; 335(7612): 194.
27. Gates M, Hanning RM, Martin ID, Gates A, Tsuji LJS. Overweight and obesity in FN youth: the influences of sleep and screen time. Rural and Remote Health 2013; 13(3): 2498.
28. Gates M, Hanning RM, Gates A, Isogai A, Tsuji LJS, Metatawabin J. A pilot comprehensive school nutrition program improves knowledge and intentions for intake of milk and milk alternatives among youth in a remote First Nation. Journal of Nutrition Education and Behavior 2013; 45(5): 455-459.
29. Gates M, Hanning RM, Gates A, McCarthy D, Tsuji LJS. Assessing the impact of pilot school snack programs on milk and alternatives intake in 2 remote First Nation communities in northern Ontario, Canada. Journal of School Health 2013; 83(2): 69-76.
30. Gates M, Hanning RM, Gates A, Martin I, Tsuji LJS. Intakes of milk and alternatives and associated nutrients among on-reserve First Nation youth in northern and southern Ontario, Canada. Public Health Nutrition 2012; 16(3): 515-523.
31. Gates A, Hanning RM, Gates M, Skinner K, Martin I, Tsuji LJS. Vegetable and fruit intakes of on-reserve First Nations schoolchildren compared to national averages and current recommendations. International Journal of Environmental Research and Public Health 2012; 9(4): 1379-1397.
32. Gates A, Hanning RM, Gates M, McCarthy D, Tsuji LJS. Inadequate nutrient intakes in youth of a remote first nation community: challenges and the need for sustainable changes in program and policy. ISRN Public Health 2012; 2012, doi:10.5402/2012/504168.
33. Isogai A, Gates A, Gates M, Hanning RM, Tsuji LJS. A qualitative evaluation of a school-based environmental health educational program addressing obesity and nutrition in a remote First Nation community. Pimatisiwin 2012; 9(2): 349-362.
34. Skinner K, Hanning RM, Metatawabin J, Martin ID, Tsuji LJS. Impact of a school snack program on the dietary intake of grade size to ten First Nations students living in a remote community in northern Ontario, Canada. Rural and Remote Health 12: 2122. (Online) 2012. Available: www.rrh.org.au (Accessed 4 August 2014).
35. Skinner K, Hanning RM, Sutherland C, Edwards-Wheesk R, Tsuji LJS. Using a SWOT analysis to inform health eating and physical activity strategies for a remote First Nations community in Canada. American Journal of Health Promotion 2012; 26(6): e159-e170. doi: 10.4278/ajhp.061019136.
36. Gates A, Hanning RM, Gates M, Isogai A, Metatawabin J, Tsuji LJS. A school nutrition program improves vegetable and fruit knowledge, preferences, and exposure in First Nation youth. The Open Nutrition Journal 2011; 5: 1-6.
37. Skinner K, Hanning RM, Tsuji LJS. Barriers and supports for healthy eating and physical activity for First Nations youths in northern Canada. International Journal of Circumpolar Health 2006; 65(2): 148-161.
38. Government of Canada. Panel on Research Ethics. The TCPS 2 Tutorial Course on Research Ethics (CORE). (Online) 2013. Available: http://www.pre.ethics.gc.ca/eng/education/tutorial-didacticiel/ (Accessed 13 November 2013).
39. Hanning RM, Royall D, Toews JE, Blashill L, Wegener J, Driezen P. Web-based food behaviour questionnaire: validation with grades six to eight students. Canadian Journal of Dietetic Research and Practice 2009; 70(4): 172-178.
40. Probst YC, Tapsell LC. Overview of computerized dietary assessment programs for research and practice in nutrition education. Journal of Nutrition Education and Behavior 2005; 37(1): 20-26.
41. Noruis MJ. SPSS 15.0 guide to data analysis. Chicago, IL: Prentice Hall, 2006.
42. First Nations Information Governance Centre. The First Nations Principles of OCAPTM. (Online) 2010. Available: http://www.rhs-ers.ca/node/2 (Accessed 13 November 2013).
43. Willows ND, Johnson MS, Ball GDC. Prevalence estimates of overweight and obesity in Cree preschool children in Northern Quebec according to international and US reference criteria. American Journal of Public Health 2007; 97(2): 311-316.
44. Willows ND, Marshall D, Raine K, Ridley DC. Diabetes awareness and body size perceptions of Cree schoolchildren. Health Education Research 2009; 24(6): 1051-1058.
45. Alwan H, Viswanathan B, Paccaud F, Bovet P. Is accurate perception of body image associated with appropriate weight-control behavior among adolescents of the Seychelles. Journal of Obesity 2011; 2011: 817242, doi: 10.1155/2011/817242.
46. Powell TM, de Lemos JA, Banks K, Ayers CR, Rohatgi A, Khera A, et al. Body size misperceptions: a novel determinant in the obesity epidemic. Archives of Internal Medicine 2010; 170(18): 1695-1697.
47. Wardle J, Haase AM, Steptoe A. Body image and weight control in young adults: international comparisons in university students from 22 countries. International Journal of Obesity 2006; 30(4): 644-651.
48. Cortese S, Falissard B, Pigaiani Y, Banzato C, Bogoni G, Pellegrino M, et al. The relationship between body mass index and body size dissatisfaction in youth adolescents: spline function analysis. Journal of the American Dietetic Association 2010; 110(7): 1098-1102.
49. Fleming T-L, Kowalski KC, Humbert ML, Fagan KR, Cannon MJ, Girolami TM. Body-related emotional experiences of young Aboriginal women. Qualitative Health Research 2006; 16(4): 517-537.
50. Williams KJ, Taylor CA, Wolf KN, Lawson RF, Crespo R. Cultural perceptions of healthy weight in rural Appalachian youth. Rural and Remote Health 2007; 8: 932.
51. Epstein LH, Valoski A, Koeske R, Wing RR. Family-based behavioral weight control in obese young children. Journal of the American Dietetic Association 1986; 86(4): 481-484.
52. Valoski A, Epstein LH. Nutrient intake of obese children in a family-based behavioral weight control program. International Journal of Obesity 1990; 14(8): 667-677.
53. Eliakim A, Kaven G, Berger I, Friedland O, Wolach B, Nemet D. The effect of a combined intervention on body mass index and fitness in obese children and adolescents - a clinical experience. European Journal of Pediatrics 2002; 161(8): 449-454.
54. Saelens BE, Sallis JF, Wilfley DE, Patrick K, Cella JA, Buchta R. Behavioral weight control for overweight adolescents initiated in primary care. Obesity Research 2002; 10(1): 22-32.
55. Nemet D, Barkan S, Epstein Y, Friedland O, Kowen G, Eliakim A. Short- and long-term beneficial effects of a combined dietary-behavioral-physical activity intervention for the treatment of childhood obesity. Pediatrics 2005; 115(4): e443-e449.
56. Barbarich BN, Kubrak C, Hanning R, McCargar L. Combined diet and exercise in the treatment of pediatric overweight and obesity. 2006 Canadian Clinical Practice Guidelines on the Management and Prevention of Obesity in Adults and Children. Canadian Medical Association Journal 176(8): 87-88. (Online) 2007. Available: http://www.cmaj., ca/content/suppl/2007/09/04/176.8.S1.DC1/obesity-lau-onlineNEW.pdf (Accessed 4 August 2014).
57. Gillis L, Hussey T, Lenk J, Ball G, Jumpsen J, Hanning R, et al. Dietary intervention for the treatment of pediatric obesity. 2006 Canadian Clinical Practice Guidelines on the Management and Prevention of Obesity in Adults and Children. Canadian Medical Association Journal 176(8): 79-82 (Online) 2007. Available: http://www.cmaj.ca/content/suppl/2007/09/04/176.8.S1.DC1/obesity-lau-onlineNEW.pdf (Accessed 4 August 2014).
58. Petrie TA, Greenleaf C, Martin S. B, iopsychosocia,, , l and physical, correlates of middle scho, , , ol boys' and girls' body satisfaction. Sex Roles 2010, ; 63(9-10): 631-644.
59. Ts, uji LJS. Mandatory use of non-toxic shotshell for harvesting of migratory game birds in Canada: cultural and economic concerns. The Canadian Journal of Native Studies XVIII 1998; 1(1998): 19-36.
60. Gates A, Gates M, Hanning RM, Stephen J, Fehst A, Tsuji LJS. Diets, body composition, physical activity and fitness of First Nations youth from Kashechewan, Ontario: an opportunity for collaborative initiatives to promote healthy weights. Canadian Journal of Diabetes 2013; 37(Supplement 2): S260.
61. World Health Organization. Growth reference 5-19 years. (Online) 2013. Available: http://www.who.int/growthref/who2007_bmi_for_age/en/ (Accessed 12 November 2013).
