The obesity pandemic is a global public health threat that requires urgent action to reverse its alarming increase in prevalence. According to current data from the Centers for Disease Control and Prevention1, obesity rates have approximately tripled in the past two decades, with over one-third of American adults and 17% (12.5 million) of children and adolescents classified as obese. Furthermore, an additional 8.6 million children in the USA are hypothesized to be at risk of becoming overweight2. Obese children have a higher probability of becoming obese adults, and have an increased risk for negative, short-term and long-term obesity-related health outcomes3-8. For example, a longitudinal study of 2392 children (aged 13 ± 2 years) observed that 70% of overweight children had at least one and 39% had two or more risk factors for cardiovascular disease (CVD)6.
Children raised in rural communities are at a higher risk of being overweight and/or obese than children in urban settings. It is estimated that rural children have 30-55% greater risk of becoming obese than their urban counterparts9,10. This trend holds true even after adjusting for 'obesogenic' environmental factors that are common in rural settings10,11. Increased risk is due, in part, to rural parents' unique set of barriers to sustaining healthy lifestyles for their children12. Citizens living in rural settings are also at an increased risk of developing CVD compared to individuals residing in non-rural areas13-15. This can be explained by a higher prevalence of CVD risk behaviors (eg cigarette smoking, obesity, physical inactivity, high lipid diet), which are prevalent in rural communities. Challenges presented in rural settings include the lack of availability of fresh fruits and vegetables and accessibility to exercise facilities and hospitals/clinics9. Another barrier to maintaining child healthy environments for rural families is lower family income, which is often due to seasonal incomes and is commonly associated with lack of family health insurance9,12.
Literature has documented that parents often misperceive their children's risk. When this happens, parental misperceptions can create additional barriers to care. Skinner et al discovered that type 2 diabetic adolescences experienced unhealthy diet behaviors and greater perceived barriers with regard to weight loss efforts when having parents who underestimated their weight16. According to Vanhala et al's 2011 Finland study, parents' recognition of their child being overweight was inversely related to the child's health eating habits and physical activity17. In overweight or obese adults the association between weight loss efforts was inversely related to misperception of their body mass index (BMI)18. Therefore, adults who correctly recognize their BMI are more apt to welcome a healthy behavior change. However, it is not known how parents' interpretation of their child's fasting lipid profiles and their perception of their child's body composition are associated with CVD risk factors, and in turn can foster a successful intervention.
To better understand parents' perceptions of their child's weight and related health effects, the current study tests the hypothesis that parents who misclassified their child, by over- or underestimating their child's BMI category, have children with higher lipid levels compared to their correctly classified peers. To approach this question, researchers analyzed retrospective cohort data from the Coronary Artery Risk Detection in Appalachian Communities (CARDIAC) Project to determine the direct association between parents' perception and presence of their children's CVD risk factors. To the authors' knowledge, this is the first study to connect parents' perceptions of their children's weight status to actual lipid values that represent children's coronary risk-related factors.
Participants
The current study incorporated a 4-year subsample of the fifth grade CARDIAC screening data (2008-2011). CARDIAC is a statewide child CVD screening project, which was initiated in 1998 as a means of reversing the high rates of CVD in rural Appalachia. Data were collected from the state of West Virginia (central eastern USA), which is the only state entirely covered by the Appalachian region. Comprehensive in design, CARDIAC has two components: a school-based surveillance and intervention initiative, and a targeted individualized approach toward identification and referral of treatment to those individuals with the most severe genetic cause of death from premature CVD, familial hypercholesterolemia19. Another mission of CARDIAC involves supporting the clinical and community-based research. This research is established on CARDIAC screening outcomes and related research programs that improve the current understanding for the causes and impact of obesity, metabolic disease, and associated risk factors among children and adolescents.
A total of 161 families participated in both the fifth grade screening and Active 8 follow-up survey between 2008 and 2011. This study excluded children of parents who reported any medical conditions or disabilities that limited their child's physical activity, resulting in 147 participants, between the ages of 9 and 13 years.
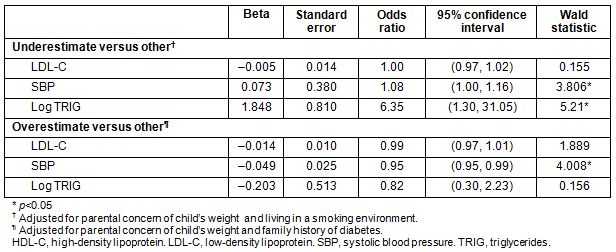
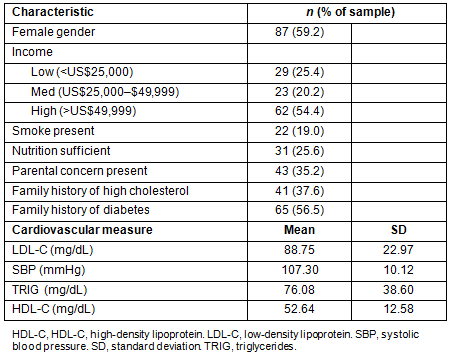
Demographics: Basic family demographic information included parents' report of their children's gender, race, BMI, and annual household income. Annual household income was stratified into three categories utilized by CDC20: low socioeconomic status (SES) ( Family history and environmental risks: Child's smoke exposure was assessed by parental report of smoking occurrence in the home ('present' if a parent or sibling smokes, and 'absent' if it is unknown or there is not smoking in the household). Family history of diabetes and high cholesterol was collected from the parents by asking whether the child's biological mother or father ever had diabetes or high cholesterol. The children's diet was evaluated according to the current CDC guidelines: sufficient (versus insufficient) nutritious diet if they consumed at least five servings of fruit and vegetables daily21. Parental concern: Parental concern was measured by the question 'Please indicate how concerned you are about your child's weight?' and responses were dichotomized into 'present' (very or little concerned) versus 'absent' (non-concerned). Child's actual body composition: Child's BMI status was calculated for each participant using recorded weight and height values (kg/m2) from the CARDIAC Project school screenings using CDC Epi Info NutStat v9.1 software (CDC; http://wwwn.cdc.gov/epiinfo/html/prevVersion.htm). This software was also used to calculate age- and-sex specific BMI percentiles derived from the CDC 2000 growth charts that were classified as follows: underweight: BMI<5th; normal: 5≤BMI<85, overweight: 85≤BMI<95; obese: BMI≥9522. Parent perceptions of child's body composition: Parent perceptions of their child's BMI were analyzed by comparing responses to the question 'How would you describe your child's weight?' to the child's actual BMI. Parents' perceptions were reported on a five-point Likert scale, with response options 'very underweight', 'slightly underweight', 'normal', 'slightly overweight' and 'very overweight'. Parents' responses 'very underweight' and 'slightly underweight' were combined to equate against children's underweight BMI. For the purpose of this study, weight status was dichotomized into 'under and normal weight' versus 'overweight and obese'. Parents who labeled their child's weight status higher than the actual were categorized as overestimating; this group was compared against 'others' (ie children of parents who accurately or underestimated their child's BMI). Likewise, parents who labeled their child's weight status lower than actual were categorized as underestimating. CVD risk factors: Child's CVD risk factors utilized in this study included high-density lipoprotein (HDL-C), low-density lipoprotein (LDL-C), triglycerides (TRIG), and systolic blood pressure (SBP). Procedures Detailed procedures for the CARDIAC Project have been presented elsewhere23,24. All screenings were conducted by trained health professionals and health science students in order to administer the blood pressure and anthropometrical testing with compliance to CARDIAC screening methodologies. The SECA Road Rod stadiometer (78'/200 cm) and SECA 840 Personal Digital Scale instruments were used to measure the participants' heights without shoes (cm) and weight (kg) respectively25. Participants were asked to rest for 5 minutes before giving a blood pressure reading, which used the fifth Korotkoff sound for the diastolic pressure measurement. Volunteer phlebotomists and local Lab Corp laboratories followed standard procedure to conduct blood draws and analysis for lipids. Lipid analyses conducted included total cholesterol (TC), HDL-C, LDL-C, very low density lipoprotein (VLDL-C), and TRIG. Participating families received a health report, with a fasting lipid profile, that included information outlining the importance of each test, results, interpretation of their results, and instructions on how to follow up with medical referrals if necessary. Parents were also offered access to a free healthcare hotline to obtain answers if they had additional questions regarding their results. In eight counties, parents were given the opportunity to participate in a follow-up questionnaire following their receipt of the screening results. For this study, only parent-reported questionnaire results were used, and only one parent from each family reported on the outcomes. These surveys were matched to the child screening results for analysis. Statistical analyses All statistical analyses are performed using the Statistical Package for the Social Sciences v18.0 (SPSS Inc.; http://www.spss.com). Normality of continuous variables and potential outliers were detected and addressed as follows: variables not conforming to normality assumptions had the appropriate statistical transformations conducted, extreme outliers found to be impossible values were omitted, and missing data was treated with pairwise deletion. To determine the demographic characteristics of the participants, means and standard deviations of continuous variables, and frequencies using valid responses of categorical variables, were calculated. Consistent with state demographics, over 96% of the participants reported being Caucasian; therefore child's race was not further included in the analyses. TC and VLDL-C were also not included in the analyses because their values were computed by manipulating other variables of interest, and their exclusion allowed researchers to resolve multicollinearity issues26-28. Two multivariable logistic regression models were used to test the hypothesis that groups ('overestimators versus other' and 'underestimators versus other') differ, with respect to CVD risk factors, while controlling for significant independent variables. To determine the associations between independent variables and parental estimates of their child's weight status, cross-tabulations were conducted using χ² tests for the categorical variables (covariates) and t-tests for the continuous variables (CVD risk factors). Significant covariates adjusted for in the 'underestimated children' multivariable model included parental concern and living in a smoking environment. The 'overestimated children' model controlled for parental concern and family history of diabetes. All of the key independent variables (ie CVD risk factors) were included in the models. Covariates were entered first, and then children's fasting lipid profile values were entered last into the model to explain parental estimates. Omnibus testing was assessed looking at the model fit; p<0.05 was considered significant. The Hosmer and Lemeshow test was also examined for goodness of fit; p>0.05 was considered good fit. Nagelkereke R2 was examined for a pseudo R2 assessment of effect. After model fit was assessed and deemed appropriate, individual predictors were examined. Wald statistic was considered significant if p<0.05, and all tests were two-sided. Ethics approval Ethics approval was not required for the current study because all identifiers were removed from the dataset prior to initiation of research. Therefore, the researchers could not identify study participants. Descriptive statistics Demographic characteristics of the sample are depicted in Table 1. The sample included 147 fifth grade public school children and parents (97.6% female parents; mean age 39.3 ± 6.45 years). More than half (64.2%) of children had underweight or normal BMI levels (2.8% were underweight), followed by 14.5% overweight, and 21% obese. Less than half of the parents accurately accessed their child's BMI (41.4%), while nearly 21% and 38% underestimated and overestimated their child's BMI, respectively. Children in the sample exhibited other factors that put them at an increased risk for obesity and obesity-related health outcomes. Participants predominantly did not meet the CDC's recommended nutritional guidelines, more than half reported a family history of diabetes, and more than a third reported having a family history of high cholesterol. HDL-C was strongly correlated with TRIG (r = -0.52), which provided a less powerful model when compared to TRIG, thus it was not included as a predictor due to collinearity. Table 1: Demographic, descriptive and cardiovascular characteristics of participants (n=147) Multivariable logistic regression Table 2 shows the adjusted associations between child CVD risk factors with parental estimates of their child's weight status. In the final block of the underestimated group, the model χ² was significant (5) = 30.19, p<0.001. Hosmer and Lemeshow χ² (8) was not significant (p=0.551) and the Nagelkerke R2 was 0.421. Children of parents who underestimated their BMI were over three times more likely to have parents who reported very or little concern about their child's weight (odds ratio (OR): 4.3; 95% confidence interval (CI): 1.08, 17.16). These children were nearly seven times more likely to live in a smoking environment (OR: 7.97; 95% CI: 1.86, 34.07). Parental underestimation was positively associated with a child's TRIG (OR: 6.35; 95% CI: 1.30, 31.05). In the final block of the overestimated group, the model χ² was significant (5) = 25.885, p<0.001. Hosmer and Lemeshow χ² (8) was not significant (p=0.547) and the Nagelkerke R2 was 0.298. Children of parents who overestimated their BMI were 67.4% less likely to have parents who were concerned about their child's weight (OR: 0.33; 95% CI: 0.11, 0.93). These children were nearly four times more likely to have a family history of diabetes (OR: 4.9; 95% CI: 1.87, 12.98). Parental overestimation was inversely associated with child SBP. These children had lower SBP (OR: 0.95; 95% CI: 0.91, 0.99) compared to those children whose parents accurately or underestimated their BMI. Table 2: Association between child lipid profiles and parent estimates of child's body mass index (n=103) Discussion The results of this study confirm that even after parents reviewed their child's health profiles, the majority of parents inaccurately assessed their offspring's weight status. The key findings suggest that children of parents who underestimated their BMI had higher SBP and TRIG values than children of parents who accurately or overestimated their weight status. Lipid levels are indicators in which the National Cholesterol Education Program (NCEP) observes to detect CVD risk factors in children29. Therefore, parents' underestimation of their child's BMI is associated with health consequences for the child. Existing literature supports the common occurrence of parents' inaccurate assessment of their child's weight. These inaccuracies most commonly occur with parents underestimating their BMI, for example saying that their overweight or obese child has a normal BMI30. In the current study parents observed their child's fasting lipid profiles prior to estimation; therefore, researchers hypothesized that most parents would accurately perceive their child's BMI and the majority who were inaccurate would have underestimated. The findings were inconsistent with the hypothesis; instead, most inaccurate parents overestimated their child's weight status. This result could be explained by the recency effect, which states one's actions, attitudes, and beliefs reflect recent experiences31. Parents reviewed their child's health profiles prior to estimating offspring's BMI, and therefore participants could have been hypervigilant to possible health issues resulting from participation in the CARDIAC Project. While comprehending the negative health consequences of children whose weight is underestimated by parents, one needs to consider the social mechanisms that could influence why parents would underestimate their child's weight status. These children had higher CVD risk factors, largely lived in a smoking environment, and had parents who reported concern about their child's weight. This finding is in contrast with the trans-theoretical model of behavior change, which states that parents who are aware and concerned about their child's weight are more prepared to take action about reversing the issue32. The contrast could result from a stigma parents feel while disclosing information about their child's health, which could reflect their parenting33. The current study shows disconnect between parental actions (ie misperceiving child's BMI and raising a child in a smoking environment) and attitudes (ie higher concern). Due to the fact that these children have higher than average SBP and TRIG values, reporting parental concern might not be enough to foster a child healthy environment. Higher level of concern could indicate that parents are in a state of readiness to take action against a weight issue, but in the presence of potential social barriers, parents may be unable to influence their child's healthy behaviors and environments34. Raising a child in a smoking environment is one of the previously addressed unhealthy behaviors that was positively associated with underestimation of a child's BMI. This finding is indirectly supported in current literature. It is known that mothers who smoke during pregnancy, or those who are exposed to environmental tobacco, are more likely to give birth to low-weight babies35,36. Low birth weight infants have an increased risk of disease onset later in life37. This association is evident in Johnson and Schoeni's 2011 study, which observed low birth weight babies to have increased health risks later in life after controlling for sociodemographic factors corresponding to birth weight. Their study found that low birth weight babies were more than two times more likely to have hypertension and over seven times more likely to have a stroke, heart attack, or heart disease later in life37. A second key finding of the current study is that children with parents who overestimated their BMI had lower SBP levels compared to their accurately and underestimated counterparts. Childhood high blood pressure is associated with the occurrence of high blood pressure later in life38. Therefore, future research should explore whether overestimating a child's weight status is protective against developing hypertension. The overestimated subgroup was more likely to have a family history of obesity-related chronic conditions (eg diabetes) and less likely to be concerned about their child's weight status. A family history of diabetes could influence parents' perception of cardiovascular health in general. The presence of an obesity-related disease brings about knowledge and awareness of its etiology and consequences. A reason that parents in this subgroup overestimated their child's BMI could be due to hypervigilancy about their child's overall health. Greater overall health consciousness may lead to parents practicing health-related behaviors, resulting in lower SBP values in children. Although the parents who overestimated their child's weight status possess hypervigilant characteristics, they reported being less concerned about their child's weight. This could be due to prior parental actions taken to fill a potential void of concern. These children are healthier (ie have lower SBP), which could suggest they have health-conscious parents. If the question about parental concern was targeted to address concern about future presence of chronic disease, then the researchers would expect a positive relationship between concern and parental estimation. The aforementioned findings have practical implications in a clinical and rural health realm. Although children's average lipid levels did not yet exceed the CDC's CVD at-risk cutoff points, over a third of these children were overweight or obese and the vast majority of them did not meet the guidelines for adequate levels of nutrition, which is associated with developing CVD risk factors39. The sample is considered an at-risk population for developing obesity-related conditions because of the children's weight status, the majority of their guardians being overweight or obese, and the rurality of the sample40 . It is important for childhood obesity interventions to target young children, who are not yet above the CVD at-risk cutoff points, in order to understand and reverse the trajectory of developing these risks and therefore CVD later in life. After parents reviewed their child's fasting lipid profiles, 58.6% still inaccurately estimated their child's weight status, which is a public health concern because this research demonstrates the children of parents who underestimated their weight had higher SBP and TRIG levels. Also, parental perceptions are known to affect children's success41. These parents may need more than just health-related information (ie review of their child's health profile) to accurately assess and then address treatment needs. Specific interventions with this parental subgroup should focus on increasing motivation, concern, and knowledge pertaining to obesity-related health issues and ways of overcoming barriers. Rather than assuming that the parents have the skills and understanding necessary to promote healthy change, appropriate interventions could help parents learn to provide a home environment that fosters success for weight loss interventions33,42. Limitations After accounting for outliers and missingness, the sample size was small. Therefore, researchers were unable to test the independent associations between a three-group comparison of children whose parents overestimated, correctly estimated, or underestimated their offspring's BMI status. Because most of the children were classified as normal or overweight (only two were underweight and 29 were obese), underweight and normal BMI categories were grouped and overweight and obese were combined. A potential limitation is that it is impossible to overestimate an obese child and underestimate an underweight child, and therefore this method of analysis helps to explain the results. Despite this limitation, it shows underlying differences between underestimated and overestimated children. This finding is important because it indicates researchers should analyze these groups separately, versus the common practice of comparing 'inaccurate' to 'accurate' estimated groups. The average level of physical activity the child experienced and maternal education level are variables that are associated with both CVD risk predictors and maternal estimates of a child's BMI, but researchers were unable to test these factors due to the variable's low response rate and the small sample size43-48. Parental concern had missing responses (17% of the responses were missing) and more than half of the completed respondents indicated being 'not concerned'. Despite the limitation, parental concern was categorized for analytic and conceptual reasons (ie the researchers were interested in separating parents who had indicated any concern versus no concern). Common limitations of a secondary analysis and cross-sectional study design were present in this study. Researchers could only use existing data and examine differences of parent perceptions and lipid profiles taken at one point in time; therefore, causal implications cannot be observed. Generalization of results to other populations is also a limiting factor because the sample consisted of fifth grade children in a predominantly rural, Appalachian region. It would be ideal to prospectively collect data and repeat the current study with a larger sample size. Although public health efforts have focused on childhood obesity prevention, many parents still are not aware and/or do not report being concerned with resolving their child's weight issues. The current study shows that many parents are inaccurately assessing their child's weight, even after reviewing their children's health profiles. Also, children of parents who underestimate their weight tend to have higher SBP and TRIG values. This finding is relevant because it supports the study of whether underestimated children are at a higher risk for developing obesity-related CVD risk factors and whether they are more in need to partake in an intervention than their correctly classified peers. To the researchers' knowledge, this is the first study that examines the direct association between accuracy of parental estimates of child's weight status and the presence of child CVD risk factors, particularly after parental review of their child's fasting lipid profiles. Future studies should continue to observe this relationship to help public health professionals better understand alternative explanations for the presence of health risk markers in children. Known associations of parental perceptions and adverse child health outcomes can channel public health efforts in rural areas to use tailored methods to appropriately educate parents of their child's weight status and weight-related risk factors. This can enable them to take action against childhood obesity. Acknowledgements The authors thank the RHEP coordinators, school nurses, and CARDIAC team for help with data collection and analysis. This study was supported by funds from the WV Bureau of Public Health, the Benedum Foundation, the Centers for Disease Control and Prevention, and the Robert Wood Johnson Foundation. References 1. Centers for Disease Control and Prevention. Childhood overweight and obesity (Online) 2012. Available: http://www.cdc.gov/obesity/childhood/index.html (Accessed 23 August 2012). 2. Georgetown University, Institute for Healthcare Research & Policy. Childhood obesity: a lifelong threat to health (Online) 2002. Available: http://ihcrp.georgetown.edu/agingsociety/pubhtml/obesity/obesity.html (Accessed 23 August 2012). 3. Dattilo AM, Birch L, Krebs NF, Lake A, Taveras EM, Saavedra JM. Need for early interventions in the prevention of pediatric overweight: a review and upcoming directions. Journal of Obesity 2012: 1-18 (Online) 2012. Available: http://www.hindawi.com/journals/jobe/2012/123023 (Accessed 7 March 2014). 4. Biro F, Wien M. Childhood obesity and adult morbidities. The American Journal of Clinical Nutrition 91(5): 1499S-1505S (Online) 2010. Available: http://ajcn.nutrition.org/content/91/5/1499S.abstract (Accessed 21 June 2013). 5. Freedman D, Khan L, Dietz W, Srinivasan S, Berenson G. Relationship of childhood obesity to coronary heart disease risk factors in adulthood: the Bogalusa Heart Study. Pediatrics 108(3): 712 (Online) 2001. Available: http://pediatrics.aappublications.org/content/108/3/712.full.pdf (Accessed 21 June 2013). 6. Freedman D, Mei Z, Srinivasan S, Berenson G, Dietz W. Cardiovascular risk factors and excess adiposity among overweight children and adolescents: the Bogalusa Heart Study. The Journal of Pediatrics 150(1): 12-17.e2 (Online) 2007. Available: http://www.ncbi.nlm.nih.gov/pubmed/17188605 (Accessed 21 June 2013). 7. Whitlock E, Williams S, Gold R, Smith P, Shipman S. Screening and interventions for childhood overweight: a summary of evidence for the US Preventive Services Task Force. Pediatrics 116(1): e125-e144 (Online) 2005. Available: http://www.ncbi.nlm.nih.gov/pubmed/15995013 (Accessed 21 June 2013). 8. Han J, Lawlor D, Kimm S. Childhood obesity. Lancet 375(9727): 1737-1748 (Online) 2010. Available: http://www.sciencedirect.com/science/article/pii/S0140673610601717 (Accessed 21 June 2013). 9. Lynch WC, Martz J, Eldridge G, Bailey SJ, Benke C, Paul L. Childhood obesity prevention in rural settings: background, rationale, and study design of '4-Health', a parent-only intervention. BMC Public Health 2012; 12: 255. 10. Liu JH, Jones SJ, Sun H, Probst JC, Merchant AT, Cavicchia P. Diet, physical activity, and sedentary behaviors as risk factors for childhood obesity: an urban and rural comparison. Child Obesity 2012; 8(5): 440-448. 11. McMurray RG, Harrell JS, Bangdiwala SI, Deng SB. Cardiovascular disease risk factors and obesity of rural and urban elementary school children. Journal of Rural Health 1999; 15(4): 365-374. 12. Melvin CL, Corbie-Smith G, Kumanyika SK, Pratt CA, Nelson C, Walker ER, et al. Developing a research agenda for cardiovascular disease prevention in high-risk rural communities. American Journal of Public Health 2013; 103(6): e1-e11. 13. Ingram D, Gillum R. Regional and urbanization differentials in coronary heart disease mortality in the United States, 1968-85. Journal of Clinical Epidemiology 42(9): 857-868 (Online) 1989. Available: http://www.ncbi.nlm.nih.gov/pubmed/2778467 (Accessed 21 June 2013). 14. Brown JR, O'Connor GT. Coronary heart disease and prevention in the United States. New England Journal of Medicine 2010; 362(23): 2150-2153. 15. Cosby A, Neaves T, Cossman R, Cossman J, James W, Farrigan T, et al. Preliminary evidence for an emerging nonmetropolitan mortality penalty in the United States. American Journal of Public Health 98(8): 1470-1472 (Online) 2008. Available: http://www.ncbi.nlm.nih.gov/pubmed/18556611 (Accessed 21 June 2013). 16. Skinner A, Weinberger M, Mulvaney S, Schlundt D, Rothman R. Accuracy of perceptions of overweight and relation to self-care behaviors among adolescents with type 2 diabetes and their parents. Diabetes Care 31(2): 227-229 (Online) 2008. Available: http://care.diabetesjournals.org/content/31/2/227.full (Accessed 21 June 2013). 17. Vanhala M, Keinanen-Kiukaanniemi S, Kaikkonen K, Laitinen J, Korpelainen R. Factors associated with parental recognition of a child's overweight status - a cross sectional study. BMC Public Health 11(665): 1-7 (Online) 2011. Available: http://www.biomedcentral.com/1471-2458/11/665 (Accessed 21 June 2013). 18. Duncan D, Wolin K, Scharoun-Lee M, Ding E, Warner E, Bennett G. Does perception equal reality? Weight misperception in relation to weight-related attitudes and behaviors among overweight and obese US adults. International Journal of Behavioral Nutrition & Physical Activity 8(1): 20-28 (Online) 2011. Available: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3073863/ (Accessed 21 June 2013). 19. CARDIAC VW Project. The CARDIAC project - celebrating over 100,000 WV kids screened since 1998 (Online) 2010. Available: http://www.cardiacwv.org/ (Accessed 15 October 2012). 20. Abeyta I, Tuitt N, Byers T, Sauaia A. Effect of community affluence on the association between individual socioeconomic status and cardiovascular disease risk factors, Colorado, 2007-2008. Preventing Chronic Disease 9: 110305 (Online) 2012. Available: http://www.cdc.gov/pcd/issues/2012/11_0305.htm (Accessed 21 June 2013). 21. Centers for Disease Control and Prevention. 5 a day works! Atlanta: U.S. Department of Health and Human Services, 2005. 22. Kuczmarski RJ, Ogden CL, Guo SS, Grummer-Strawn LM, Flegal KM, Mei Z, et al. 2000 CDC growth charts for the United States: methods and development. Vital Health Statistics 2002; 11(246): 1-190. 23. Neal W, Demerath E, Gonzales E, Spangler E, Minor V, Islam S, et al. Coronary Artery Risk Detection in Appalachian Communities (CARDIAC): preliminary findings. The West Virginia Medical Journal 97(2): 102-105 (Online) 2001. Available: http://europepmc.org/abstract/MED/11392187 (Accessed 21 June 2013). 24. Demerath E, Muratova V, Spangler E, Li J, Minor V, Neal W. School-based obesity screening in rural Appalachia. Preventive Medicine 37(6): 553 (Online) 2003. Available: http://www.ncbi.nlm.nih.gov/pubmed/14636788 (Accessed 21 June 2013). 25. Ice C, Murphy E, Cottrell L, Neal W. Morbidly obese diagnosis as an indicator of cardiovascular disease risk in children: results from the CARDIAC Project. International Journal of Pediatric Obesity 6(2): 113-119 (Online) 2011. Available: http://www.ncbi.nlm.nih.gov/pubmed/20545480 (Accessed 21 June 2013). 26. Friedewald WT, Levy RI, Fredrickson DS. Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clinical Chemistry 1972; 18(6): 499-502. 27. McNamara JR, Cohn JS, Wilson PW, Schaefer EJ. Calculated values for low-density lipoprotein cholesterol in the assessment of lipid abnormalities and coronary disease risk. Clinical Chemistry 1990; 36(1): 36-42. 28. Abudu N, Levinson SS. Calculated low-density lipoprotein cholesterol remains a viable and important test for screening and targeting therapy. Clinical Chemistry Laboratory Medicine 2007; 45(10): 1319-1325. 29. NIH Heart, Lung, and Blood Institute, U.S. Department of Health and Human Services. National Cholesterol Education Program: program description (Online) 2012. Available: http://www.nhlbi.nih.gov/about/ncep/ncep_pd.htm (Accessed 15 August 2012). 30. Towns N, D'Auria J. Parental perceptions of their child's overweight: an integrative review of the literature. Journal of Pediatric Nursing 2009; 24(2): 115-130. 31. Miller N, Campbell D. Recency and primacy in persuasion as a function of the timing of speeches and measurements. The Journal of Abnormal Psychology 59(1): 1-9 (Online) 1959. Available: http://www.ncbi.nlm.nih.gov/pubmed/13664403 (Accessed 21 June 2013). 32. Rhee K, De Lago C, Arscott-Mills T, Mehta S, Davis R. Factors associated with parental readiness to make changes for overweight children. Pediatrics 116(1): e94-e101 (Online) 2005. Available: http://www.ncbi.nlm.nih.gov/pubmed/15995022 (Accessed 21 June 2013). 33. Thorn J, DeLellis N, Chandler J, Boyd K. Parent and child self-reports of dietary behaviors, physical activity, and screen time. The Journal of Pediatrics 162(3): 557-561 (Online) 2013. Available: http://www.ncbi.nlm.nih.gov/pubmed/23058292 (Accessed 21 June 2013). 34. Mathieu M-E, Drapeau V, Tremblay A. Parental misperception of their child's body weight status impedes the assessment of the child's lifestyle behaviors. International Journal of Pediatrics 2010 (Online) 2010. Available: http://www.hindawi.com/journals/ijped/2010/306703/ (Accessed 21 June 2013). 35. Knopik V. Maternal smoking during pregnancy and child outcomes: real or spurious effect? Developmental Neuropsychology 34(1): 1-36 (Online) 2009. Available: http://www.ncbi.nlm.nih.gov/pubmed/19142764 (Accessed 21 June 2013). 36. Salmasi G, Grady R, Jones J, McDonald S. Environmental tobacco smoke exposure and perinatal outcomes: a systematic review and meta-analyses. Acta Obstetricia Et Gynecologica Scandinavica 89(4): 423-441 (Online) 2010. Available: http://www.ncbi.nlm.nih.gov/pubmed/20085532 (Accessed 21 June 2013). 37. Johnson R, Schoeni R. Early-life origins of adult disease: national longitudinal population-based study of the United States. American Journal of Public Health 101(12): 2317-2324 (Online) 2011. Available: http://www.ncbi.nlm.nih.gov/pubmed/22021306 (Accessed 21 June 2013). 38. Morrison J, Glueck C, Wang P. Childhood risk factors predict cardiovascular disease, impaired fasting glucose plus type 2 diabetes mellitus, and high blood pressure 26 years later at a mean age of 38 years: the Princeton-lipid research clinics follow-up study. Metabolism, Clinical and Experimental 61(4): 531-541 (Online) 2012. Available: http://www.ncbi.nlm.nih.gov/pubmed/22001337 (Accessed 21 June 2013). 39. Center for Disease Control and Prevention. Nutrition and physical activity: helping people choose healthy eating and active living, at a glance. CDC: Atlanta, GA, 2011. 40. Lutfiyya M, Inpanbutr-Martinkus M, Wisdom-Behounek J, Lipsky M. Is rural residency a risk factor for overweight and obesity for U.S. children? Obesity Research 15(9): 2348-2356 (Online) 2007. Available: http://www.ncbi.nlm.nih.gov/pubmed/17890504 (Accessed 21 June 2013). 41. Kitzmann K, Dalton W, Stanley C, Beech B, Reeves T, Midgett E, et al. Lifestyle interventions for youth who are overweight: a meta-analytic review. Health Psychology 29(1): 91-101 (Online) 2010. Available: http://psycnet.apa.org/?fa=main.doiLanding&doi=10.1037/a0017437 (Accessed 21 June 2013). 42. Singer JB (producer). Prochaska and DiClemente's Stages of Change Model for social workers. Episode 53, 10 October 2009. Social Work Podcast (audio podcast). Available: http://socialworkpodcast.com/2009/10/prochaska-and-diclementes-stages-of.html 43. Andersen L, Harro M, Sardinha L, Froberg K, Ekelund U, Anderssen S, et al. Physical activity and clustered cardiovascular risk in children: a cross-sectional study (The European Youth Heart Study). Lancet 368(9532): 299-304 (Online) 2006. Available: http://www.sciencedirect.com/science/article/pii/S0140673606690752 (Accessed 21 June 2013). 44. Eckstein K, Mikhail L, Ariza A, Thomson J, Millard S, Binns H. Parents' perceptions of their child's weight and health. Pediatrics 117(3): 681-690 (Online) 2006. Available: http://pediatrics.aappublications.org/content/117/3/681 (Accessed 21 June 2013). 45. Genovesi S, Giussani M, Faini A, Vigorita F, Pieruzzi F, Valsecchi M, et al. Maternal perception of excess weight in children: a survey conducted by paediatricians in the province of Milan. Acta Paediatrica 94(6): 747-752 (Online) 2005. Available: http://www.ncbi.nlm.nih.gov/pubmed/16188779 (Accessed 21 June 2013). 46. Manios Y, Kondaki K, Kourlaba G, Vasilopoulou E, Grammatikaki E. Maternal perceptions of their child's weight status: the GENESIS study. Public Health Nutrition 12(8): 1099-1105 (Online) 2009. Available: http://www.ncbi.nlm.nih.gov/pubmed/19105868 (Accessed 21 June 2013). 47. Jain A, Sherman S, Chamberlin L, Carter Y, Powers S, Whitaker R. Why don't low-income mothers worry about their preschoolers being overweight? Pediatrics 107(5): 1138-1146 (Online) 2001. Available: http://www.ncbi.nlm.nih.gov/pubmed/11331699 (Accessed 21 June 2013). 48. Reifsnider E, Flores-Vela A, Beckman-Mendez D, Nguyen H, Keller C, Dowdall-Smith S. Perceptions of children's body sizes among mothers living on the Texas-Mexico border (La Frontera). Public Health Nursing 23(6): 488-495 (Online) 2006. Available: http://www.ncbi.nlm.nih.gov/pubmed/17096773 (Accessed 21 June 2013).
 >
>