Rural acute care nursing has been described as a form of multi-specialist practice requiring registered nurses to have an extensive breadth and depth of practice knowledge1,2. Working in an environment with minimal medical or ancillary support3, rural registered nurses (RNs) may be required to draw on specialty nursing knowledge and skills that are sporadically used4,5. Furthermore, contextual knowledge, that is knowledge of the people and the resources at hand, must be mobilized by rural nurses to safeguard patients during hospitalization6.
Hence, rural RNs must be nimble and responsive in their reasoning and clinical decision-making abilities if they are to deal with a wide range of practice and work environment issues that can potentially have an impact on patient outcomes7,8. Nurses who are new to rural practice environments and their employers, however, have raised concerns related to patient safety during their transition to rural nursing practice3,9. They have also suggested that feeling unprepared for the rigors of rural hospital nursing practice is a central issue influencing RN recruitment and retention9,10.
While the nature of rural nursing practice has been studied2, significantly less is known about how rural RNs reason through clinical problems. Understanding how rural RNs reason through a problem to its solution is a key element for identifying professional development needs, and may support the recruitment and retention of skilled rural nurses.
Purpose
Rural nursing practice requires RNs to access, use and assess in a meaningful way multiple types of information from a variety of sources at a moment's notice. Deciding on which possible course of action is often made without medical, collegial or ancillary support. Furthermore, they must reflect in the moment whether or not they are choosing the right course of action given the situation at hand. The purpose of this study was to explore how rural RNs reason through the complex clinical problems they encounter.
Literature review
Theoretical underpinnings of clinical reasoning: In her seminal work with novice to expert practitioners, Benner found that novice practitioners made decisions using context-free rules; that is, they make decisions using linear processes while disregarding the tacit dimensions of the problem11. Extending this work, Dyess and Sherman found that novice and advanced beginner RNs (nurses with less than 2 years of work experience) take longer to work through complex critical situations and need more time to reach sound clinical decisions12. These nurse researchers proposed that the main difference between novice and expert practitioners relates to their use of intuitive judgement. O'Neill et al13 concluded that novice RNs differed in their reasoning from experienced nurses in that they were less able to home in on salient cues and make clinical decisions quickly. In a qualitative study of 12 RNs working in critical access hospitals in the USA, Seright14 examined the cues used by novice rural RNs to make clinical decisions and the sources of feedback that influenced cue processing and subsequent decision making. The findings suggest that when novice RNs encountered unfamiliar patient situations but sensed a need to take action, they were frequently unable to articulate what the cues for taking action were or to state their rationale for the decisions they made. To cope, the participants compared the cues they observed with patients they had encountered in previous practice situations and drew on the knowledge they had gained during their nursing education program. When confronted with subtle or ambiguous cues, participants turned to co-workers to confirm their suspicions and to help them identify appropriate actions. Seright14 concluded that novice RNs can come to understand and utilize effective patterns of clinical reasoning and decision making through situational learning that cultivates curious, creative and reflective minds.
Clinical decision making: The process of clinical reasoning with clinical decision making forms a symbiotic relationship15. While the ability to think critically is considered to be at the heart of good clinical nursing practice, the literature remains unclear about what constitutes clinical decision making and its specific relationship to critical thinking. An early definition suggests clinical decision making includes identifying, prioritizing, establishing a plan of care, and evaluating the outcome of the care provided16, resulting in the generation of reasoned judgements17. Extending this definition, Rashotte and Carnevale suggest that complex decisions about the patient's status are contextually situated within the human social phenomena that affect the person's response to nursing care18. Oliver and Butler15, however, suggest that the influence of the context on clinical decision making is dependent on the practitioner's evaluation of its importance.
In two recent studies, factors that influence RNs' decision making processes were explored. In the first study, differing levels of foreground knowledge (knowledge required for day-to-day performance) and background knowledge (facts about underlying conditions and diseases) had an impact on the quality of heart specialist nurses' decision making19. In the second study, the researchers discovered that more experienced pediatric nurses used different clinical decision-making processes than novice pediatric RNs20. Highly experienced pediatric nurse specialists used forward thinking where they gathered data first and then offered a diagnosis. Conversely, more novice pediatric nurse specialists frequently used backward thinking: they would identify the established nursing diagnosis and collect data to confirm the diagnosis.
In the present study, clinical reasoning and decision making were understood as 'mindful doing'21. As such, RNs must practise their cognitive and metacognitive skills in order to engage in effective clinical reasoning and decision making22. Clinical reasoning and decision-making was conceptualized as not an exclusively cognitive function but included significant social, psychological, cultural and contextual influences18.
An exploratory approach using observation in a simulated environment followed by a semi-structured interview was used. Consequently, the research approach for this study does not fit within traditional positivist or naturalistic paradigms23, nor is it a typical mixed-methods approach24. Rather, the recreation of a simulated rural nursing unit followed by a semi-structured interview format using a substantive approach to critical thinking25 offered a melding of a more controlled approach to content than conventional ethnographic approaches, while still offering a sufficiently natural context.
Participants
The aim of this study required the recruitment of rural RNs with a wide range of work experience. Recruitment was expected to be problematic because of the time commitment (approximately 2.5 hours including travel time to the research site). Rural nurses who were committed to professional development, and who worked in at least one of the nine rural hospitals across the health region where the university was located, were approached. For this study, 'rural' included any geographical area situated outside of the two large tertiary centers and five regional centers within the province of Alberta, Canada26.
Fifteen RNs aged 22-61 years volunteered to participate in this study. Five RNs had less than 5 years of rural hospital work experience post-graduation, three RNs had 5-10 years of rural hospital work experience, and seven RNs had more than 10 years of experience. The average number of years of work experience within this group of participants was 25 years. Six RNs were diploma prepared, eight RNs had undergraduate degrees, and one participant held a graduate degree. The majority of the participants reported having completed a variety of courses they believed were necessary for the provision of safe, efficient and effective nursing care (for example Advanced Cardiac Life Saving and Newborn Resuscitation Program). Although the sample size was small, its size and the heterogeneity of the group were considered acceptable for an in-depth, exploratory study. No participants withdrew from the study.
Data generation
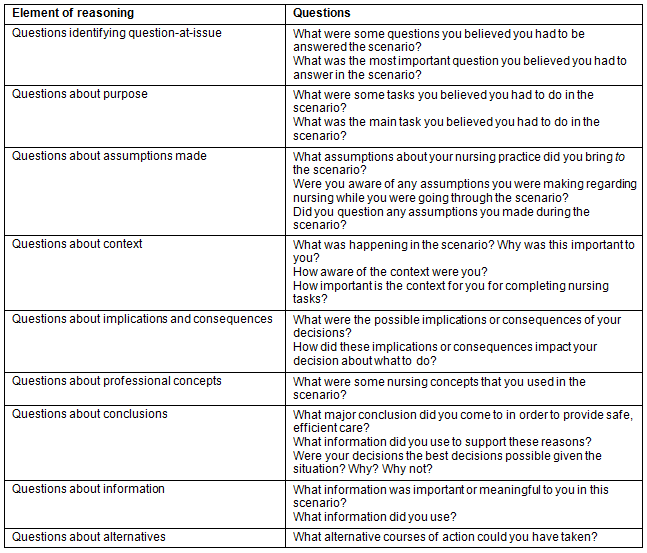
Data were generated over a 1-month period. Data consisted of interview transcripts and observation. Specifically, the participants worked through a 30-minute scenario where they interacted with high- and medium-fidelity mannequins as well as real-life actors. Using the simulated environment is discussed in detail elsewhere27. At the completion of the scenario, the participants were interviewed by one of the researchers. The interview had a semi-structured format where questions based on elements of reasoning21 were asked (Table 1). All of the interviews were recorded and transcribed verbatim for analysis. Interview duration was 90-120 minutes.
Table 1: Interview questions
Data analysis
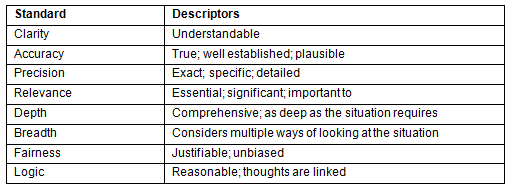
A template that included Nosich's21 standards of reasoning (Table 2) was created. Each interview was analyzed line by line. To ensure that analysis was consistent across the three researchers, three interviews were randomly selected and analyzed by each researcher. When individual analysis was completed, as a group the analyses were discussed until consensus was reached and there was common understanding of the standards of reasoning. The remaining interviews were divided amongst the researchers and individually analyzed. After an interview was completely analyzed, the analysis was circulated to the other two researchers for the purpose of receiving feedback regarding accuracy and consistency of the analysis. After all of the interviews were analyzed, the researchers met and reviewed the analysis within and across all of the transcripts to identify common themes and trends.
Table 2: Nosich's standards of reasoning
Establishing reliability and validity
Recreating a rural hospital setting and scenario for the participants to work through provided comparable data sets for data analysis, and several strategies were used to ensure the reliability and validity of the data. First, the 30-minute scenario the participants worked through was developed with the help of expert rural practitioners. Their involvement was intended to enhance the credibility and validity of the scenario and to bridge practice and research. The practitioners evaluated the scenario to determine how well it captured the patient conditions and nursing care requirements rural RNs might expect to encounter during a typical shift. They also evaluated the sequencing and timing of the cues embedded within the scenario.
Second, because the aim of the study was to explore how rural RNs reason through diverse problems with conflicting demands, a constructed natural environment that was similar to the participants' 'real practice setting' was created. Once again, advice from the expert practitioners was sought to ensure that the created environment - including patients with various physiologic and psychological needs, physical equipment, and real people entering and exiting the unit - reflected the typical rural nursing environment. Because the types of patient conditions that could be used in the scenario were dictated by the functional capabilities of the mannequins, the assistance of a simulation laboratory coordinator became central in determining the physiologic patient conditions that participants would encounter. In consultation with the expert practitioners and the simulation coordinator, a high-fidelity mannequin was programmed to recreate a diabetic ketoacidosis event, a newborn high-fidelity mannequin was programmed to move its legs and arms and produce crying sounds, and a medium-fidelity mannequin was programmed to produce deteriorating vital signs. Three low-fidelity mannequins represented patients with more chronic but stable conditions.
Third, the scenario was written in such a way as to elicit verbal and physical responses from participants. Thus, actors were used. An RN with a graduate nursing degree took the licensed practical nurse and emergency personnel roles. Another RN with an undergraduate nursing degree took on the 'voice' of the mannequins as well as the lab/x-ray technician role. A laboratory assistant who did not have any formal nursing education took on the roles of mother and sister-in-law. In preparation for engaging in their roles, the actors were instructed to respond to the participants' directions and actions. Thus, the credibility of the simulation greatly depended on the ability of the actors to get into their role and to respond to the participant accordingly25. To assist the actors in taking on these roles, several run-throughs of the scenario were undertaken under the direction of the research team.
Fourth, for the purposes of identifying scenario inaccuracies, scripting difficulties, identifying equipment malfunctions, and ensuring the interview questions were clear and logically ordered, an RN not part of the sample group but who had 15 years of rural hospital nursing practice experience was invited to run through the study procedures. Using her feedback, minor modifications were made to the scenario.
Ethics approval
Ethics approval was received from the Human Subject Research Committee at the researchers' university. Participation was voluntary and participants could withdraw at any time. Written informed consent was obtained from each participant at the beginning of the data collection session. Participants were assigned pseudonyms. All project documents were kept in a locked cabinet in the researchers' offices.
The scenario for this study was designed to have three acute in-hospital patients who were displaying changes in their health status as well as more stable patients with chronic conditions. It was also designed in such a way as to capture the concepts of 'we're a team' and 'we're a family'28, where nurses know not only their nurse colleagues but also other members of the healthcare team (eg a licensed practical nurse, laboratory/x-ray technician, emergency medical service personnel and physician). Having developed this type of scenario, in the conceptual phase of this study, assumptions about the phenomenon under study and the participants were identified.
Under the influence of Benner's work with novices to experts11, the first assumption that needed to be addressed was that more experienced RNs would display greater ability to engage in clinical reasoning and decision making. Analysis of the data revealed that the number of years of practice experience did not seem to be directly linked to the ability to engage in clinical reasoning. For instance, Debra (real names have been changed throughout), an RN with 26 years of practice experience, seemed to prioritize her nursing care using a relatively discrete piece of information, disregarding much of what was unfolding around her. That is, Debra's focus was at the micro-level. She seemed unable to reconcile the palliative patient's needs with the needs of the unit as a whole. This participant also stated that she felt overwhelmed because she understood she had many tasks to complete but was unable to complete them.
I was quite concerned about the fellow with the spinal cancer because I think he had had a fairly rough evening without telling us, and I wanted to find out from him what we could do to bridge that gap so that he wouldn't be laying there trying to visit with people and having a lot of pain. I guess I wanted to know specifically what was going on with him. The thought quickly raced through my mind I have all these things to do, maybe this should be dealt with later. But then I quickly decided, I'm here now.
In comparison, Lana, an RN with 2 years of practice experience, begins at the macro-level and quickly narrows her focus to individual patient needs. From within a broad perspective, she efficiently identifies her priorities. She also provides a rationale that is clear and accurate. Last, and what is perhaps most striking, is that she also asks herself if her most important question is in fact the 'right' one. She was able to assess the relevance of a specific question in the immediate context. Questioning whether or not this is the right question in the context at hand demonstrates an ability to consider potential patient responses to interventions taken or not taken29.
My biggest question was patient status. Where is everyone at this point, because I had been off the floor for several hours and when you're responsible for that many patients you need to know, okay, where are they right now and what do they need? I was trying to think, okay, what's the most important thing to do right now? Okay, so what should be my next step? Should I do this or do that?
The second assumption identified by the research team was that clinical reasoning and decision making would be a function of the interpersonal characteristics of rural nursing practice. Rural nurses identify one another as their most important single source of information and education, and because they share close intimate knowledge of one another, there is a great sense of accountability30. Consistent with Seright's findings14, the participants in this study with less than 5 years of practice experience demonstrated that their relationship with more experienced healthcare professionals influenced their clinical reasoning and decision making. For example, the most important question that Diane, an RN for only 3 months, developed was based on her colleague's patient assessments.
Once the LPN [licensed practical nurse] said that our DKA [patient with diabetic ketoacidosis] wasn't doing very good that was like a ting-ting in my mind because we know what can happen if they're not treated. So the priority to go and assess his blood sugar, the medications he was on, how long he's been on it and whether or not it was working.
Other junior nurses reported that their interpersonal relationships with the more experienced nurses were also positive. Working with more experienced nurses provided them with the opportunity to learn clinical reasoning and decision making through observation and reflection.
I'm constantly watching the older RNs and saying, okay, why did they do that and not do this, or why when this happened did they kind of go hum but then jumped when this happened. (Catherine, 4 years practice experience)
The interpersonal characteristics of rural nursing practice meant that the less experienced participants in this study would confer with families to gather information that would then be used in their reasoning and decision making.
You get to know the patients and the family really well, and it is actually nice because then you can utilize the family and say, hey, how's his pain? He's not going to tell me. You know, he's trying to hold it in. You know him best, what do you see? Oh, he's in a lot of pain. Okay, good to know. (Rena, 9 months practice experience)
It has been reported in the literature that RNs believe that when they know the patients personally, they provide better care30. The more experienced participants in this study, however, acknowledged that while knowing the patient and family was helpful, this knowledge did not play a central role in their reasoning and decision making.
I never try and treat anybody more special than another person. It's like, we're all sick people here and you might be number three on my list. I've got two more that are a little sicker and I have to spend my time with them also. Just because this person was the mayor or is the wife of a pharmacist or is the coach you have those relationships but that doesn't make them any more important than the next patient sitting beside them who just moved into town. (Letty, 17 years practice experience)
The research team's last assumption was that being able to engage in deep clinical reasoning was dependent on being able to think creatively. According to Gillespie and Paterson creative thinking acknowledges the reality of present-day nursing practice31 - increasing patient acuity and complexity, and the growing scarcity of resources, requires nurses to find creative solutions to patient situations. Many of the participants in this study clearly indicated that the need to be creative in problem solving was necessary for the provision of care.
The security guards are usually around. They will look after Alzheimer patients in the middle of the night that are starting to crawl out of bed and you just don't have time - we've had them sit there with them before. (Claire, 3 years practice experience)
According to Thompson et al19 nurses vary in their decision-making ability despite being given identical clinical information. Analyses of the present study data revealed that clinical reasoning and problem solving was context-specific31: sophistication of reasoning varied depending on the moment and what was occurring within that moment. In this study, each participant demonstrated reasoning that at times was more clear, accurate, and relevant than at other times. For example, one participant stated, 'it's important to know what other patients you have and what you're dealing with'. While this comment was not particularly clear or precise, it was accurate in that nurses do need to have a breadth of perspective while performing specific tasks. In short, they need a holistic view of what is happening on the unit, especially when the unit is short staffed and they are on shift when support is limited.
Consequently, deep clinical reasoning and decision making is a function of reflection and self-correction that requires a critical self-awareness: awareness of the need to seek out the best possible solution. For example, through reflection in the act of providing nursing care, Halley (an RN with 3 years of work experience) was able to self-correct her initial course of action.
I knew the bag was empty and I ran a TKVO [to keep a vein/vessel open] for a short time just to give me time to mix a bag so the line didn't go dry. So I knew I had to do that before carrying on with anything otherwise I was going to have a pain crisis on my hands. I kind of put it off for a minute, and then I'm like, no, I have to do this. I wouldn't have wanted to deal with a pain crisis on top of everything else.
Deep clinical reasoning and effective decision making is more about how nurses think then what they think32.
Discussion
Rural RNs' ability to engage in deep clinical reasoning varied considerably despite RNs being given the same information under the same circumstances. The results highlight the dangers of assuming that quantity of clinical experience is a proxy for engaging in sound clinical reasoning in a given domain of clinical practice19. The findings of this study suggest the degree of sophistication in reasoning of experts and novices is at times equivalent in that the reasoning of both can be somewhat limited and focused primarily on human physicality and less on conceptual knowledge33. It would seem then, that practice is necessary to become proficient in any skill, including clinical reasoning. Van Gelder suggests that not only is deliberate practice required but also that the exercises used need to focus on the enhancement of reasoning skills34. Evidence is accumulating suggesting that using clinical simulation and reflective interviewing that emphasize how clinical decisions are made enhances reasoning skills and confidence35-37.
The findings of this study support the notion that clinical knowledge in the rural setting is socially embedded and that the social context that includes interpersonal relationships plays a pivotal role in the clinical reasoning and decision making of novice RNs14,28. In this study, less experienced RNs were able to pay attention to obvious cues gathered from patients such as vital signs and verbal comments. More importantly, they relied heavily on others in their decision making to ensure they were making the right decision13. Indeed, to engage in efficacious decision making, the less experienced participants in this study depended on what they knew about the patient, being able to engage the patient in a discussion about his/her needs, and their ability to engage other healthcare providers31,38.
Of particular interest and importance is that, consistent with Seright's findings14, regardless of level of education or experience, the participants in this study did not reference hospital policies, decision trees or algorithms. Whether or not these participants engaged in evidence-based practice remains unclear.
While the less experienced RNs in this study engaged their colleagues in making decisions about patient care regardless of the acuity of the patient, all of the participants relied on their colleagues when patient status began to deteriorate. This is in keeping with the notion that when decision making is critical in situations where patient status is highly volatile, such as in emergency situations, cue recognition becomes less reliable and depending on others to help with decision making is essential11,31,38. In rural hospitals where patient census and acuity is variable and coupled with less frequent exposure to high acuity patient conditions, and where novice RNs may be working alone, development of good clinical skills and pattern recognition is essential for positive patient outcomes14,35. Recognizing the need to collaborate and engage others in sound reasoning and decision making may be supported through the use of simulation and feedback offered through debriefing sessions such as was used in this study.
There is substantial support in the literature for linking critical thinking and creativity39-41. Paul and Elder suggest that critical thinking and creativity are inextricably linked and develop in parallel40. In this study, the more experienced RNs discussed times when they used creative solutions to address a problem they had encountered. While the participants with less than 5 years of work experience did not indicate that they had generated creative solutions to difficult problems, they were able to clearly describe solutions they identified as creative that their more experienced colleagues had engaged in.
Reflection and self-corrections are other cornerstones to developing high-quality reasoning. Metacognition, thinking about thinking, supports critical reasoning: monitoring and evaluating one's own thought processes help to deepen the quality of reasoning. Furthermore, the ability to evaluate one's own arguments and the reasoning producing them is necessary for self-correction41. However, the participants in this study seldom engaged in self-correction. Indeed, many participants had difficulty identifying potential alternative courses of action in resolving the problems they identified during the scenario. So while the rural hospital practice setting is recognized as a complex environment in which sound clinical reasoning and decision making are required, it is possible that the pace at which nurses must make decisions and deliver care in this setting does not provide opportunity for reflection on practice and self-correction. Collaborative partnerships are needed among nurse educators, rural RNs, rural hospital administrators and educational institutions and educators for the development of programs that focus of critical reasoning and decision making42,43.
Implications
Nursing education: There seems to be a need for a healthier balance between teaching procedural skills and critical thinking pedagogy. Without doubt, it is necessary that nurses learn and master a variety of clinical procedures. It is also the case that they need to be able to contextualize those procedures, knowing when to apply them and when to be critical of their application. In order to nurture such a reflective stance, nursing education needs to have the twin foci of teaching procedural knowledge and critical thinking.
Not having enough time in nursing curricula and in professional development opportunities within the practice setting to teach for a deeper, critical understanding of course material is not the issue at hand. It is a matter of infusing basic elements of reasoning and their related, intellectual standards into the daily activities of clinical instruction. Nurse educators can ask students and nurses a variety of questions, prompt them to seek alternative solutions to the presenting clinical problem, and encourage examination of the accuracy and relevance of the information gathered.
Practice policy: Rural healthcare can no longer be sustained by nurses who remain at the beginner level in their clinical reasoning ability44 or who focus solely on mastery of procedural knowledge. Thus, during professional development opportunities, explicit instruction in specifics basic to both clinical procedures and critical thinking must become compulsory. As such, reporting professional development opportunities that incorporate critical thinking elements can be linked to performance evaluations.
Research: A limitation of this study was the wide range of years of experience of the participants. Furthermore, the participants' practice experiences were varied and may have influenced their ability to engage in deep clinical reasoning and decision making. Last, the scenario represented only a brief segment of a shift. However, the findings of this study suggest that simulation combined with a post-simulation interview has the potential for exploring complex concepts including reasoning processes rural RNs engage in during a typical shift. Further research in the use of simulation and post-simulation interviewing is needed.
Rural nurses who demonstrate metacognitive self-awareness are more purposeful and focused in their reasoning. They are aware of the need to deepen the quality of their reasoning by appealing to criteria or intellectual standards when deciding what to do in a nursing context. They see relevance in the need to think deeply and broadly, making decisions when evidence is present and revisiting them in the presence of counter-evidence.
Conversely, nurses who are not metacognitively self-aware do not consistently demonstrate the skills and attitudes basic to sound and deep clinical reasoning. They have difficulty prioritizing tasks, posing clear and relevant questions within a specific context and revisiting working answers to those questions. They rely less on their own reasoned judgement under stress, often deferring to more experienced colleagues.
The participants in this small exploratory study demonstrated that engaging in clinical reasoning and decision making was variable across participants, across moments in time, and dependent on the perceived acuity of the situation. Whether or not these participants engaged in evidence-based practice is a question that remains open11 and will require further investigation. Studying the influence of the social climate and context of the rural hospital setting may provide further insight into how rural RNs reason and make clinical decisions.
References
1. Kenny A, Ducket S. Educating for rural nursing practice. Journal of Advanced Nursing Education 2003; 44(6): 613-622.
2. MacLeod M, Martin Misener R, Banks K, Morton AM, Vogt C, Bentham D. 'I'm a different kind of nurse': advice from nurses in rural and remote Canada. Nursing Leadership 2008; 21(3): 40-53.
3. MacKinnon K. Learning maternity: the experiences of rural nurses. Canadian Journal of Nursing Research 2010; 42(1): 38-55.
4. Paliadelis PS, Parmenter Parker V, Giles M, Higgins I. The challenges confronting clinicians in rural acute care settings: a participatory research project. Rural and Remote Health 12: 2017. (Online) 2012. Available: www.rrh.org.au (Accessed 31 August 2013).
5. Squires A. New graduate orientation in the rural community hospital. The Journal of Continuing Education in Nursing 2002; 33(5): 202-239.
6. MacKinnon K. Rural nurses' safeguarding work: re-embodying patient safety. Advances in Nursing Science 2011; 34(2): 119-129.
7. Bushy A. The rural context and nursing practice. In D Molinari, A Bushy (eds). The rural nurse: transition to practice. New York, NY: Springer Publishing, 2012; 3-22.
8. Molinari D. Rural nurse transition-to-practice programs. In D Molinari, A Bushy (eds). The rural nurse: transition to practice. New York, NY: Springer Publishing, 2012; 23-34.
9. Spector N, Silvestre J. Quality of care and patient safety: the evidence for transition-to-practice programs. In D Molinari, A Bushy (eds). The rural nurse: transition to practice. New York, NY: Springer Publishing, 2012; 35-46.
10. Pine R, Tart K. Return on investment: benefits and challenges of a baccalaureate nurse residency program. Nursing Economics 2007; 25(1):13-18, 39.
11. Benner P. From novice to expert: excellence and power in clinical nursing practice. Upper Saddle River, NJ: Prentice Hall, 2001.
12. Dyess S, Sherman R. The first year of practice: new graduates nurses' transition and learning needs. The Journal of Continuing Education in Nursing 2009; 40(9): 403-410.
13. O'Neill E, Dluhy N, Hansen A, Ryan J. Coupling the N-Codes system with actual nurse decision-making. CIN: Computers, Informatics, Nursing 2006; 24(1): 28-34.
14. Seright TJ. Clinical decision-making of rural novice nurses. Rural and Remote Health 11: 1726. (Online) 2011. Available: www.rrh.org.au (Accessed 31 August 2013).
15. Oliver M, Butler J. Contextualising the trajectory of experience of expert, competent and novice nurses in making decisions and solving problems. Collegian 2004; 11(1): 21-27.
16. Grossman S, Campbell C, Riley B. Assessment of clinical decision-making ability of critical care nurses. Dimensions of Critical Care Nursing 1996; 15(5): 272-279.
17. Tanner C, Benner P, Chesla C, Gordon D. The phenomenology of knowing the patient. Image 1993; 25: 273-280.
18. Rashotte J, Carnevale FA. Medical and nursing clinical decision making: a comparative epistemological analysis. Nursing Philosophy 2004; 5: 160-174.
19. Thompson C, Spilsbury K, Dowding D, Pattenden J, Brownlow R. Do heart failure specialist nurses think differently when faced with 'hard' or 'easy' decisions: a judgement analysis. Journal of Clinical Nursing 2008; 17: 2174-2184.
20. Andersson N, Klang B, Petersson G. Differences in clinical reasoning among nurses working in highly specialised paediatric care. Journal of Clinical Nursing 2012; 21: 870-879.
21. Nosich GM. Learning to think things through: a guide to critical thinking across the curriculum. 4th edn. New York, NY: Pearson, 2012.
22. Chaboyer W, Creamer J. Intellectual work of the critical care nurse: applications from a qualitative study. Australian Critical Care 1999; 12(2): 66-69.
23. Loiselle CG, Profetto-McGrath J. Canadian essentials of nursing research. 3rd edn. Philadelphia, PA: Wolters Kluwer Health, Lippincott Williams & Wilkins, 2011.
24. Ostlund U, Kidd L, Wengstrom Y, Rowa-Dewar N. Combining qualitative and quantitative research within mixed method research designs: a methodological review. International Journal of Nursing Studies 2011; 48: 369-383.
25. Bryans A, McIntosh J. The use of simulation and post-simulation interview to examine the knowledge involved in community nursing assessment practice. Journal of Advanced Nursing 2000; 31(5): 1244-1251.
26. Alberta Health Services. Community & rural planning framework, strengthening communities: a rural health strategy for Alberta. Draft 7. (Online) 2010. Available: http://www.albertahealthservices.ca (Accessed 5 September 2013).
27. Sedgwick M, Dersch S, Grigg L. The creation of a simulated rural hospital nursing unit for the purpose of conducting research. Journal of Nursing Education and Practice 4(9): 27 (Online) 2014. Available: http://dx.doi.org/10.5430/jnep.v4n9p27 (Accessed 20 August 2014).
28. Sedgwick M, Yonge O. 'We're it', 'we're a team', 'we're family' means a sense a sense of belonging. Rural and Remote Health 8: 1021. (Online) 2008. Available: www.rrh.org.au (Accessed 31 August 2013).
29. Tanner C. Thinking like a nurse: a research-based model of clinical judgment in nursing. Journal of Nursing Education 2006; 45(6): 204-212.
30. Ellis Scharff J. The distinctive nature and scope of rural nursing practice: philosophical bases. In CA Winters (ed). Rural nursing concepts, theory, and practice. 4th edn. New York, NY: Springer, 2013; 241-258.
31. Gillespie M, Paterson BL. Helping novice nurses make effective clinical decisions: the Situated Clinical Decision-Making Framework. Nursing Education Perspective 2009; 30(3): 164-170.
32. Wilson Mulnix J. Thinking critically about critical thinking. Educational Philosophy and Theory 2012; 44(5): DOI: 10.1111/j.1469-5812.2010.00673.x
33. Greenwood J, King M. Some surprising similarities in the clinical reasoning of 'expert' and 'novice' orthopaedic nurses: report of a study using verbal protocols and protocol analyses. Journal of Advanced Nursing 1995; 22: 907-913.
34. Van Gelder T. Teaching critical thinking: some lessons from cognitive science. College Teaching 2005; 53: 41-46.
35. Endacott R, Scholes J, Cooper S, McConnell-Henry T, Porter J, Missen K, et al. Identifying patient deterioration: using simulation and reflective interviewing to examine decision making skills in a rural hospital. International Journal of Nursing Studies 49: 710-717. (Online) 2012. Available: http://www.elsevier.com/ijns (Accessed 31 August 2013).
36. Kaddoura MA. New graduate nurses' perceptions of the effects of clinical simulation on their critical thinking, learning, and confidence. The Journal of Continuing Education in Nursing 2010; 41(11): 507-516.
37. Wolf L. The use of human patient simulation in ED triage training can improve nursing confidence and patient outcomes. Journal of Emergency Nursing 2008; 34(2): 169-171.
38. Cioffi J. A study of the use of past experiences in clinical-decision making. Computers, Informatics, Nursing 2001; 24(1): 591-599.
39. Bailin S. Critical thinking and science education. Science & Education 2002; 11(4): 361-375.
40. Paul R, Elder L. Critical thinking: the nature of critical and creative thought. Journal of Developmental Education 2006; 30(2): 34-35.
41. Lai ER. Critical thinking: a literature review. Pearson's Research Report Series. (Online) 2011. Available: http://www.pearsonassessments.com/research (Accessed 15 August 2013).
42. Dyess S, Sherman R. The first year of practice: new graduates nurses' transition and learning needs. The Journal of Continuing Education in Nursing 2009; 40(9): 403-410.
43. Tobin B. Development of a post-basic critical care program for registered nurses: a collaborative venture between education and practice. The Journal of Continuing Education in Nursing 2007; 38(6): 258-261.
44. Galloway S. Simulation techniques to bridge the gap between novice and competent healthcare professionals. Online Journal of Issues in Nursing 2009; 14(2): 1-9.


