Pain is an international concern. National and international health surveys indicate that the majority of adults experience pain on a regular basis1. According to a US Gallup survey2, 89% of Americans experience pain each month, and a Canadian National Population Health Survey (NPHS) reported 65% of Canadians had taken some type of over-the-counter (OTC) and/or prescription medication for pain relief during the course of a month3. Yet, there is evidence that indicates most individuals are reluctant to seek professional care for their pain2. Consumer reports suggest that today's health trend is moving more towards self-care4 and that an increasing number of individuals are self-treating their pain without informing their primary healthcare practitioner2,5-7. This may be due to many factors, such as changes in primary healthcare cost, long waiting periods for non-urgent medical care, and general consumer dissatisfaction with overall health care8,24.
Pain has been defined by the International Association for the Study of Pain as 'An unpleasant sensory and emotional experience normally associated with tissue damage or described in terms of such damage'9. Research findings indicate that increasing numbers of individuals are using non-prescription drugs in addition to prescriptive medications to relieve their pain10 and that the potential for adverse drug reactions are also increasing11,12. These findings may be related to reports that suggest individuals are seeking non-prescriptive OTC medications, complimentary/alternative therapies (CAM) such as herbal therapies for pain in order to manage not only the physical discomforts of pain but also the psychological and emotional experience of pain10,13-15. The combination of treatment modalities poses a potential for serious health problems, such as drug interactions between prescription, OTC and CAM therapies. Thus, the study of self-treatment modalities for pain is warranted.
Self-treatment has been viewed as similar to self-care. According to the World Health Organization self-care is:
The activities individuals, families and communities undertake with the intention of enhancing health, preventing disease, limiting illness, and restoring health. These activities are derived from knowledge and skills from the pool of both professional and lay experiences. Lay people on their own behalf undertake them, either separately or in participative collaboration with professionals14,25.
Factors that may affect self-care treatment choices include income, ethnicity, educational level and age. Cultural forces among other social forces such as health perspectives have also been identified as powerful determinants of health related behaviors16. At present, little is known about the pain self-treatment modalities individuals in rural communities choose to relieve pain that exceeds everyday kinds of pain such as minor headaches and toothaches. There are differences in health perspectives between rural and urban communities4. Those living in rural communities value independence and self-reliance. The availability of primary health care and hesitancy to seek treatment related to the belief that professional consultation may lead to prolonged periods away from work are factors that are common to rural health perspectives4,17. Although urban residents also view self-reliance on managing health related concerns, the degree of importance is different from that of rural residents. Comfort and life-prolonging aspects of health are more frequently the focus for urbanites4. Self-treatment modalities may also be used by urbanites to manage their pain, however, for reasons such as lack of medical insurance, ethnic versus traditional health care practices, and lack of transportation services to accessible healthcare facilities4.
The purposes for this descriptive/exploratory study were twofold:
- To explore the occurrence of pain that exceeds everyday kinds of pain (such as minor headaches or toothaches), pain intensity ratings, interference.
- To report on the modalities of self-treatment of pain used by rural Canadian adults.
The widespread promotion of pain self-treatment products to consumers through media and the Internet, gives rural Canadian adults a false sense of confidence about using these products without their understanding the health precautions of each product18. Health care practitioners caring for people with pain need to be aware of the different pain self-treatment modalities used by their patients, in order that they may provide effective and comprehensive pain management. The information from this study describes pain self-treatment modalities used by rural adults to control everyday kinds of pain. Another purpose of the present study is to compare this Canadian data with results from a US rural cohort study5. Although self-treatment has been studied in various populations, a comparison between the influences of diverse healthcare systems has not been made.
Methods
Design
The present study replicated the descriptive/exploratory research design, procedure and sample recruitment used by Vallerand, Fouladbakhsh and Templin5, which entailed rural community participants. Participants were recruited who had experienced acute or chronic pain that exceeded everyday headaches or toothaches in the previous 2 weeks. They were asked to complete three survey questionnaires about their self-treatment of pain.
Sample recruitment
A convenience sample of 105 participants was recruited for this study from two Canadian rural communities. A rural community is defined as one that has less than 150 people per km219. For this study, participants were selected from rural communities located outside the commuting zone of an urban center with a population density of 400 or more people per km2. The average population of the rural communities ranged from 13 000 to 46 00020.
Sample selection: Rural community sources for sample recruitment included local businesses, such as a corporate financial institution, a physical therapy clinic and a local fitness center, church/community organizations such as the Knights of Columbus, a women's group, senior centers and a pain support group. The principal investigator contacted each group's site director by phone to explain the study and request an invitation to give out the survey at a group meeting. Upon receipt of an invitation to address the group, the principal investigator explained the purpose of study to the potential participants. The eligibility criteria for participation were that all participants were 18 years of age or older, English or French speaking, and have had experienced pain that exceeded everyday kinds of pain (such as minor headaches or toothaches) in the previous 2 weeks. Pain could originate from acute or chronic conditions. Those participants who met the eligibility criteria and agreed to fill out the questionnaires were included in the study.
Informed consent was obtained from each participant following the guidelines for Human Subjects. The participants were asked to complete the questionnaires given to them. The principal investigator was available to answer any questions they had. Educational pamphlets outlining pain management for acute and chronic pain and a pain resource list were made available to all participants. Questionnaires were translated into French by the principal investigator for the approximately 1% of French-speaking participants.
Instrumentation
Pain intensity and pain interference were measured using the Brief Pain Inventory: Short Form (BPI-SF), an internationally accepted pain assessment tool21. The BPI-SF uses a 10-point numerical rating scale (NRS) and consists of seven questions that assess level of pain, degree of pain relief and amount of pain interference with functional and psychosocial factors. A question also asks participants to identify the location of pain on a diagram of a human body. Pain intensity was measured by summing four of the BPI - SF's questions that asked participant to rate the intensity of their worst, least, average and current pain using the 10-point NRS (0 = 'no pain' and 10 = 'pain as bad as you can imagine') yielding a possible total score of 40. Internal reliability for this measure yielded a satisfactory alpha of .86. Pain interference was measured by summing seven questions from the BPI-SF that yielded a possible total score of 70. These questions asked participants to rate how much the pain interfered with their general activities, mood, sleep, walking, normal work, relationship with others and enjoyment in life using the 10 point NRS (0 = 'does not interfere' and 10 = 'completely interferes'). Internal reliability for this measure yielded an alpha of .91. Participants were also asked to identify the percentage of pain relief their pain treatments and medications provided in the past 24 hours on a scale from 0 = 'no relief' and 10 = 'complete relief'.
The self-treatment of pain in the community Questionnaire, developed by Vallerand, Fouladbakhsh and Templin1 was used to describe the self-treatment modalities participants used to relieve their pain. It consisted of four open-ended questions, asking the participants to list any prescription medications they took to relieve their pain; any OTC product; any herbal and CAM; and any other treatments other than medications they were using to treat their pain. Participants were also asked to list the medications and/or herbal and vitamin supplements they were taking to treat disorders other than pain. No medications or modalities were suggested; participants described the modalities they were using for self-treatment. Finally, participants were asked to indicate 'yes' or 'no' to the question: 'Is your primary care practitioner aware of the modalities you listed in questions 1 through 4'. Demographic data was collected using an investigator-designed questionnaire.
Statistical analysis
Demographics, pain intensity, pain interference and percentage of pain relief were summarized using descriptive statistics. Data on self-treatment of pain were grouped into four categories:
- Primary practitioner prescribed pharmacological non-opioid, opioid, and/or adjuvant medication.
- Non-prescription medications (OTC).
- CAM therapies such as vitamins and herbal therapies.
- Non-pharmacological modalities such as relaxation, heat/cold, and massage.
Frequencies were performed for each group and c2 tests of significance were computed to test differences between Canadian data and US data. Differences in mean scores between Canadian data and US data on demographics, pain intensity, pain interference, pain relief and types of self-treatment of pain were determined through independent t-tests. Bivariate correlations were conducted to determine the relationships between demographic characteristics, pain intensity, pain interference and self-treatment choices of pain relief.
Results
Sample
A convenience sample (n = 103) of adults from two rural communities, in two Canadian provinces was used. Approximately half (48%) of the participants came from a rural community in Northern New Brunswick and the other half (52%) came from a rural community in Central Ontario. Participants were mostly women (70%), Caucasian (94%), with at least some post secondary education (84%). The majority of the participants were married (55%), employed full time or part time and living with another family member.
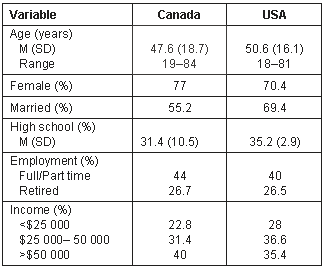
The Canadian sample (n = 103) and the US sample (n = 100) were found to be comparable in both demographic and socioeconomic characteristics through independent t-tests. The sample characteristics of both the USA and Canadian participants are shown (Table 1). Both the Canadian and US study participants have similar distribution of annual household income (Table 1).
Table 1. Participant characteristics for Canadian (n = 103) and US (n = 100) samples
Descriptive analysis
Pain intensity and pain relief: Canadian study participants identified their worst, average, and least pain during the past 2 weeks, as well as their current pain level. On average, participants reported worst pain to be of moderate to severe intensity on a scale of 0-10 (M = 6.0), and average pain to be of moderate intensity on a scale of 0-10 (M = 4.1). Current pain was reported to be of minimal intensity and less than average pain (M = 3.1) on a scale of 0-10 in the past 2 weeks. Participants were also asked to identify the percentage relief they received from their current self-treatment regimen. Canadian participants reported an average of only 43% pain relief with their current self-treatment regimen.
Results of independent t-tests comparing Canadian and US mean pain levels indicated that there were no significant differences between the two countries for worst pain (t = -.85, p = .9), average pain (t = .6, p.11), least pain (t = 1.6, p.1) or current pain (t = .32, p.2). However, the results of independent t-tests showed a significant difference between Canadian and US scores on the relief from pain they received by using their current self-treatment pain modalities (t = 13.7, p.00).
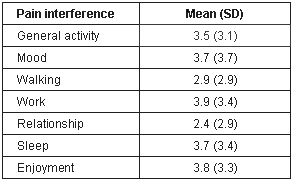
Pain interference: Table 2 presents Canadian reports of the extent to which pain interfered with the functional and psychosocial aspects of daily activities such as, general activity, mood, walking, normal work, relationships with other people, sleep and enjoyment in life. Findings indicated that activities most affected by pain were mood, work and sleep.
Overall pain interference was measured by summing the composite of these scores to yield a total possible score of 70. The mean overall pain interference for Canadians was 24 (SD = 18.7). Results of independent t-tests comparing Canadian and US mean pain interference scores indicated that there were no significant differences between the two countries for overall pain interference (t = .91, p = .11).
Table 2: Canadian mean pain interference with daily activities (on a scale of 1-10)
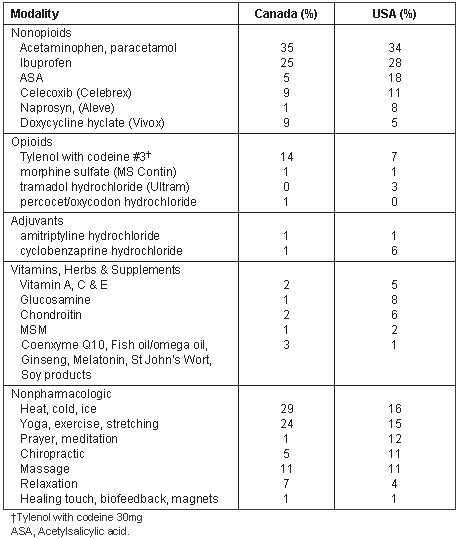
Self-treatment of pain: US participants reported using significantly more physician prescribed medications (60%) to treat their pain than did Canadians (48%) (c2 = 4.8, p = .03). These included non-opioid, and opioid analgesics, such as Celecoxib (Celebrex), and tramadol hydrochloride (Ultram), and adjuvants, such as tricyclic antidepressants and muscle relaxants. US participants also reported using significantly more OTC medications (74%) to treat pain than did the Canadians (62%) (c2 = 8.1, p = .004). These included acetaminophen, ibuprofen, and other non-steroidal anti-inflammatory drugs (NSAIDs). Although both Canadian and US participants reported using pain treatments other than medications, there was no significant difference between the two countries in the percentage of CAM therapies such as vitamins, herbal therapies and supplements taken for pain relief (USA = 16%, Canada = 11%). Canadians, however, reported choosing significantly more non-pharmacological pain treatments such as heat/cold, exercise/stretching and massage (61%) than did US participants (41%), (c2 = 7.6, p = .006)(Table 3).
Table 3: Self-treatment modalities used by rural participants
Bivariate analysis
Pharmacological self-treatment modalities: Canadians with greater pain intensity used significantly more pharmacological self-treatment modalities (r = 0.29, p <.01). Similarly, Canadians who reported having greater pain interference also used significantly more pharmacological self-treatment modalities (r = 0.28, p <.01).
Non-pharmacological self-treatment modalities: Findings indicated that Canadian rural adults under 55 years of age used significantly more non-pharmacological self-treatment pain modalities (68%) than Canadians 55 years and older (36%) (r = -.27, p < .01). Furthermore, the use of non-pharmacological self-treatment modalities was significantly higher in those Canadians who reported greater pain intensity (r = 0.24, p < .05), as well as, greater pain interference (r = .25, p <.05).
Practitioner awareness of self-treatment of pain: The number of reports of practitioner awareness increased significantly as the age of the Canadian rural adult increased, (r = 0.196, p <.05). Similarly, Canadians who were married reported significantly greater practitioner awareness than those who were single or unmarried (r = 0.22, p <.05).
Discussion
The findings from the present study indicate that pain is a common experience among Canadians living in rural communities in northeastern New Brunswick and southeastern Ontario. The majority of Canadians were using some form of self-treatment for their pain. Average pain intensity levels, while self-treating were reported as being moderate (4 on a scale from 1-10), and pain interfered most often with mood, sleep and work. The results of this study also indicated that the percentage of relief that pain self-treatments provided, as reported on the BSI-SF, was on average lower for Canadian participants than US5 participants. Despite the use of self-treatment modalities such as prescription medication, OTC medication, herbs and vitamin supplements and other non-pharmacological modalities, Canadian participants reported an average of 43% pain relief, whereas their US cohorts, who although did not receive complete relief (100%) with self-treatment, reported an average of 52% pain relief.
Patterns of the use of self-treatment modalities also differed between the US and Canadian samples. Canadians used 9% less prescription and OTC pain medication, and 23% more non-pharmacologic modalities than the US cohorts5. Canadians reported using more traditional non-pharmacologic self-treatment pain modalities such as heat, cold, exercise/stretching and massage than the US cohorts5.These findings are consistent with previous research looking at the choices of pain treatments for non-cancer chronic pain suffers in Canada1. In their investigation, Moulin et al.1 found that despite 80% prevalence of moderate to severe pain, only 22% of patients reported using major analgesic medication along with some kind of non-pharmacological treatment. These findings are of interest because anecdotal evidence suggests that pharmacological products, including prescription and OTC medications, are more available to Canadians due to differences between the two countries' federal drug administration policies. Further study is needed to discern reasons for differences in utilization of prescription and non-prescription analgesics for Canadians suffering from moderate to severe chronic pain.
Reports from the present study also indicate that Canadian participants used 5% less of the modalities identified as CAM, such as vitamins and herbal treatments, to relieve their pain than did the US cohort study5. However, findings showed that similarities between the countries existed in the characteristics of CAM users. In both studies, increased age reduced the likelihood of using CAM modalities and CAM choices of self-treatment of pain were used when pain intensity was high.
Although the present study did not examine cultural factors, such as cultural beliefs and attitudes toward pain, the authors acknowledge that these variables may play a role in the experience of pain, pain perception, the management of pain, and in fact may influence whether practitioners as well as patients address pain as a serious health concern1. When one deals with pain as a clinical problem, perceptions of the experience of pain are of utmost importance. Many still hold the view that pain is an aversive sensory response to a physiological problem and the most effective way to reduce this response is to change or turn off the sensory response through opioids or other drugs22,23. However, this level of understanding is incomplete, because research has shown that pain clearly affects more than physiological processes. Research has shown that pain can appear and persist without evidence of tissue trauma, enveloping the whole of the person who experiences it24. Because persistent pain causes true suffering, clinical intervention should focus on pain needs that address the entire person and family to protect functional capability, psychological wellbeing and overall health25.
Although, the limited sample size makes it inappropriate to generalize the results of this study to all rural communities in Canada, findings from this study, as well as the US cohort study, indicate that the potential for adverse interactions exist. Data from this comparative study indicate that a majority of participants used some form of non-prescribed pain self-treatment modality to treat their pain, yet over 33% of Canadian participants and 20% of US participants reported that they had not informed their primary care practitioner of their self-treatment choices. This is of great concern to the authors, because it indicates that individuals may not be receiving accurate information about how to treat their pain effectively and avoid the potential for harmful drug interactions and under-treatment of pain. Numerous studies have documented the seriousness and life-threatening potential of drug-drug and drug-herb interactions12,15. Similarly, research has shown that the under-treatment of pain, especially in older adult populations, has become a community health problem that can lead to the potential for long-lasting negative effects on ones perception of control over pain25.
Recent worldwide changes indicating the paradigm shift in healthcare across health systems, with a continually increasing focus on the use of CAM, has further added to the complexity of pain self-treatment5. Individuals all over the globe are able to purchase herbal products and supplements over the counter or on the Internet, further increasing self-treatment options. Research has indicated that use of these may not be reported to healthcare providers under the misguided assumption that they are 'natural products' and hence, not harmful7,26. Further research is needed on the marketing of non-prescription herbal and vitamin therapies and potential risks to consumers when combining these products.
The findings from comparative data from both cohort studies indicate the need for increasing the knowledge of rural Canadians in self-treatment of pain in order to manage their pain effectively. Although the Canadian group reported using more non-pharmacologic modalities than was associated with increased pain intensity, the percent of pain relief was less than in the US cohort who reported using more prescription medications, OTC products and herbal products/supplements in conjunction with non-pharmacologic modalities. Educational interventions that include information about how to combine both pharmacologic and non-pharmacologic modalities into self-treatment regimens, and the importance of sharing self-treatment practices with primary practitioners and community health nurses should be considered for rural Canadian residents. This education in turn may facilitate the proper use of OTC medications, awareness of potential adverse drug-herb interactions, and prevention of inappropriate self-treatment choices. Innovative educational strategies that recognize the needs of rural populations are essential in bringing this knowledge to community residents. Rurality presents concerns such as distance from healthcare providers, availability of places of learning (schools, libraries etc), and hesitancy to seek treatment related to the rural work ethic17. Information could be disseminated through small community support groups, and through pamphlets available at pharmacies, clinics and medical offices. Web-based pain management tutorials could also be valuable information sources for rural communities in remote areas.
Summary
Pain is a common experience for many individuals and as self-care becomes more prevalent in rural communities4,16, Canadians need to be more aware of self-treatment options of pain control. Examining and comparing the self-treatment practices of rural US and Canadian residents has increased the understanding of pain interference, self-treatment choices of pain control and potential for harmful consequences in this population. Significant findings included that Canadians, who used more non-pharmacologic self-treatment modalities of pain control, had less pain relief than US participants by their self-treatment choices. In addition, 33% had not informed their primary-care practitioner of their self-treatment choices. Further study is indicated to examine whether the cultural factors and the current healthcare systems influence self-treatment choices of pain control in rural populations.
Acknowledgements
Dr Cheryl Riley-Doucet, Assistant Professor, is a faculty at The Oakland University School of Nursing, Rochester, Michigan. This study was funded by a Sigma Theta Tau, Chapter Iota, small research grant, Madonna University, School of Nursing.
References
1. Moulin DE, Clark AJ, Speechley M. Chronic pain in Canada: prevalence, treatment, impact and the role of opioid analgesia. Pain Res Manage 2002; 7: 179-184.
2. Arthritis Foundation. Pain in America. Arthritis Foundation. (Online) 2000. Available: http://www.arthritis.org/conditions/pain_center/default.asp (Accessed 14 July 2004).
3. Statistics Canada. Catalogue 82-003. Health Reports 2000; 12: 33-39.
4. American Medical Student Association. Health care delivery: rural vs urban communities. (Online) 2004. Available: http://www.amsa.org/programs/gpit/ruralurban.cfm (Accessed: June 2004)
5. Vallerand AH, Fouladbakhsh J, Templin T. Self-treatment of pain in a rural community. Journal of Rural Health 2004; 20: 166-172.
6. Chambers CT, Reid GJ, McGrath PJ, Finley GA. Self-administration of over-the-counter medication for pain among adolescents. Archives of Pediatric and Adolescent Medicine 1997; 151: 449-455.
7. Fautrel B, Adam V, St Pierre Y, Joseph L, Clarke AE, Penrod JR. Use of complementary and alternative therapies by patients self-reporting arthritis or rheumatism: results from a nationwide Canadian survey. Journal of Rheumatology 2002; 29: 2435-2441.
8. Ross MM, Carswell A, Hing M, Hollingworth G, Dalziel WB. Seniors' decision making about pain management. Journal of Advanced Nursing 2001; 35: 442-451.
9. International Association for the Study of Pain. IASP pain terminology. (Online) 2003. Available: http://www.iasp-pain.org/terms-p.html (Accessed 14 July 2004).
10. Musil CM. Gender differences in health and health actions among community-dwelling elders. Journal of Gerontological Nursing 1998; 24: 30-38.
11. Sheftell FD. Role and impact of over-the-counter medication in the management of headache. Neurologic Clinics 1997; 43: 893-898.
12. Kuhn MA. Drug interactions with medications and food. Nursing Spectrum 1998; 8: 12-14.
13. Harrison P. A pain primer. Canadian Living 2003; May: 64-70.
14. Lowe NK, Ryan-Weinger NM. Over-the-counter medications and self-care. Nurse Practitioner 1999; 24: 34-44.
15. Hensrud DD, Engle DD, Scheitel SM. Underreporting the use of dietary supplements and nonprescription medications among patients undergoing a periodic health examination. Mayo Clinic Proceedings 1999; 74: 443-447.
16. World Self-Medication Industry. About self-medication. (Online) 2004. Available: http://www.wsmi.org/aboutsm.htm (Accessed 14 July 2004).
17. Bushy A. Rural determinants in family health: considerations for community nurses. Family Community Health 1990; 12: 29-38.
18. Torrible SJ, Hogan DB. Medication use and rural seniors: who really knows what they are taking? Canada Family Physician 1997; 43: 893-898.
19. Ehrensaft P, Beeman J. Distance and diversity in non-metropolitan economies. In: RD Bollman (Ed.). Rural and small town Canada. Toronto: Thompson Educational, 1992.
20. Statistics Canada. Community profiles 2001. (Online) 2001 http://www.statcan.ca (Accessed 14 July 2004).
21. Daut RL, Cleeland CS, Flanery RC. Development of the Wisconsin Brief Pain Questionnaire to assess pain in cancer and other diseases. Pain 1983; 17: 197-210.
22.WHO Drug Information. General policy issues. (Online) 2000. Available: http://www.who.int/druginformation/vol14num1_2000/voume14-1.pdf (Accessed 14 July 2004).
23. Stoller EP, Forster LE, Portugal S. Self-care responses to symptoms by older people. A health diary study of illness behavior. Medical Care 1993; 31: 24-42.
24. Chapman CR, Stillman M. Pathological pain, handbook of perception: pain and touch. L Krueger (Ed.). New York: Academic Press, 1996; 315-340.
25. Riley-Doucet C. Congruence in family dyadic perceptions of pain controllability between older adult cancer patients and family caregivers (Doctoral dissertation, Wayne State University, 2002). Dissertation Abstracts International; AAT 3071826.
26. Morrissey J. Triage for the ER. Modern Healthcare 2003; 33: 65-66, 75.


