full article:
Breastfeeding an infant provides complete nutrition necessary for its full physical and mental development1-3. The American Academy of Pediatrics advises exclusive breastfeeding for the first six months and continued breastfeeding for at least a year4. Introduction of complementary foods should not happen before the sixth month, and breastfeeding should continue at least until 12 months of age4. According to the Centers of Disease Control and Prevention (CDC), 74.6% of babies are ever breastfed in USA, 44.3% breastfeeding at 6 months and only 23.8% continuing to breastfeed to 12 months5. In Nebraska, the numbers of ever breastfed and exclusively breastfed babies at 6 months stay below the national average5. Healthy People 2020 (HP2020) aims to increase the proportion of ever breastfed babies to 81.9%, 60.6% at 6 months, and 34.1% at 12 months6.
Disparities in breastfeeding practices exist across different groups7,8. There is a need for more research on culturally tailored interventions to achieve established breastfeeding goals9. Among Hispanic mothers, perceptions of infant rejection to breastfeeding and milk insufficiency are often reported10, and formula supplementation is practiced among one in three mothers11. Previous research has shown initiation of breastfeeding may be more frequent among urban (59%) than among rural women (49%)12. There is a lack of research on breastfeeding initiation and continuation among Hispanic women in rural areas13-19 and the factors that influence breastfeeding are unknown.
The purpose of this pilot study was to explore factors that influence breastfeeding initiation and continuation among Hispanic women living in rural settings.
A convenience sample of 12 Hispanic women, age 19 years or older, was enrolled from the Regional West Medical Center, Scottsbluff, a rural setting in Nebraska, during October 2012. Two focus groups of six individuals, with sessions lasting for one to two hours each were conducted20. Individuals were excluded if they were not of Hispanic origin. A multimethod approach was used to gather both quantitative and qualitative data. All questionnaires were in Spanish and English, and a certified Spanish translator was present to assist participants.
Sociodemographics, maternal history, health literacy, and computer and internet use were gathered to describe the population. The previously validated Breastfeeding Self-Efficacy Scale Short Form (BSES-SF) was used to (i) identify breastfeeding mothers at high risk, (ii) identify breastfeeding behaviors and cognitions to individualize confidence-building strategies, (iii) evaluate effectiveness of various interventions and (iv) guide program development21. The revised Breastfeeding Attrition Prediction Tool (BAPT) questionnaire was used to determine women's intention, attitudes toward breastfeeding, and likelihood to discontinue breastfeeding22-24.
The qualitative data included a series of open-ended questions about (i) decisions to breastfeed, (ii) challenges of breastfeeding, (iii) timing of breastfeeding, (iv) benefits of breastfeeding, and (v) overall experience with breastfeeding. The focus group questions were developed on the basis of Predicting and Changing Behavior Theory (PCBT)25. The sessions were moderated by a certified Spanish translator and were audio recorded. The recordings were transcribed into written format, and translated into English when appropriate. Each study participant was given a $50 gift card.
Data analysis
For the quantitative portion, descriptive analysis was performed using univariate statistics to report means and standard deviations for the continuous variables and frequency distributions for the categorical variables. The open-ended questions were analyzed in order to identify themes and their relationships as they emerged from the data. The audio files were listened to and the notes were transcribed to quotes. Framework analysis approach was employed, using thematic analysis, charting and indexing, which provided the flexibility to explore the meaning of narrative data while following a rigorous methodology. All data were analyzed using Statistical Analysis Software v9.1 (SAS Institute, www.sas.com).
Ethics approval
The Institutional Review Board (IRB) at the University of Nebraska Medical Center approved this study (IRB protocol #430-12-EP).
Study population characteristics
The majority of women were in the age group 19-24 years old (58%, n=7), married (75%, n=9), not employed (58%, n=7), and had 12 or more years of education (58%, n=7) (Table 1). The average number of children was 2 (standard deviation (SD)=2), with average previous history of pregnancies of 2 (SD=2). The average age of the children was 24 months old (SD=10), ranging from 14 to 48 months. Less than half of the mothers had breastfed for at least 6 months (42%, n=5). The majority did not take prenatal breastfeeding classes and did not intend to (83%, n=10). The average health literacy score was 6.75 (SD 2.8) with a range of 3-10. Four participants (33%) scored 10 and above, reflecting poor health literacy scores (Fig1).
Table 1: Study population characteristics
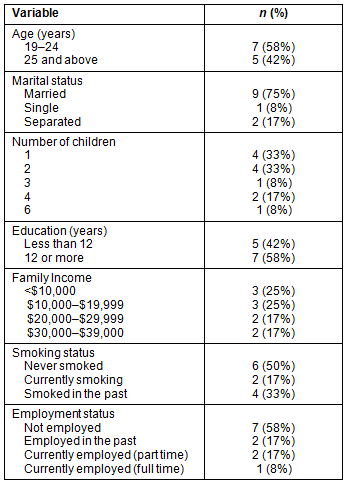
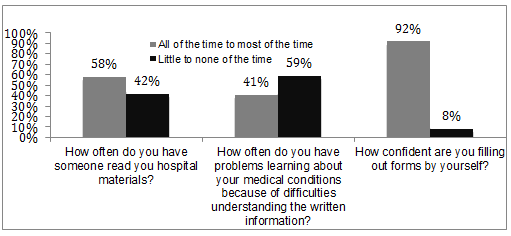
Figure 1: Frequency of participants' responses to health literacy assessments.
Family (83%, n=10) was reported as the main source of breastfeeding information, followed healthcare professionals (42%, n=5), and friends (25%, n=3). The majority reported having a computer at home (58%, n=7), and less than half (42%, n=5) used the computer on a daily basis. Internet use was reported by 75% (n=9) of the study participants, while 42% (n=5) of them indicated using it daily. Ninety-two percent (n=11) reported rarely or not at all using internet for finding breastfeeding information. Only one participant indicated that the internet met her needs to find appropriate breastfeeding information.
Breastfeeding Self-efficacy and Breastfeeding Attrition Prediction Tool
The average BSES-SF score was 55, with the scores ranging from 36 to 67 (Fig2). Thirty-three percent (n=4) had BSES-SF scores of 50 or less, indicating a higher risk for early discontinuation of breastfeeding. Mothers who breastfed for 6 months or more had a higher mean score (mean=61, SD=5) than mothers who breastfed for less than 6 months (mean=47, SD=17). BAPT results indicated an above-average intention to breastfeed with an average of 31 (SD=4). Mothers who breastfed for 6 months or more had a higher average BAPT scores (mean=32, SD=2) than mothers who breastfed for less than 6 months (mean=26, SD= 3).
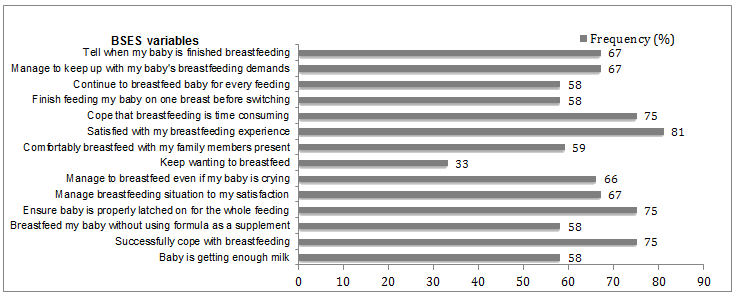
Figure 2: Frequency of participants who answered 'Always or usually confident' in the Breastfeeding Self-efficacy Scale Short Form.
Qualitative analysis
I. Decisions to breastfeed: Half of the participants decided at the time of pregnancy to breastfeed their children (50%, n=6), 25% (n=3) planned before pregnancy to breastfeed, and 25% (n=3) decided after giving birth. The majority (67%, n=8) decided to breastfeed because of the perceived benefits for the health of the baby, or as one mother replied '[the babies] grow healthier and are sick less often.' Other factors are summarized in Table 2.
II. Challenges of breastfeeding: The most common discomforts of breastfeeding reported were sore nipples (92%, n=11), severe engorgement (58%, n=7), and plugged ducts (50%, n=6). One mother stated 'I first started, my nipples were very sore and my baby had a time latching on, but once the soreness went away it was fine.' Twenty-five percent (n=3) reported supplementing water along with breast milk, or giving some other supplement. However, less than half reported problems with breastfeeding (42%, n=5). The reported reasons for discontinuing breastfeeding are summarized in Table 2. One mother stated, 'After 3 months of fighting with latching, I gave him the bottle.'
Family interference was identified as a problem, a very important issue as one mother stated, and 'I wasn't producing enough milk so my grandma would make my son herbal teas.' The majority received help from their mothers to continue breastfeeding (67%, n=8). Other influential figures for breastfeeding continuation are summarized in Table 2. On average, solid foods were introduced in the baby's diet at 5.8 months (SD=2.9), ranging from 3 to 12 months. Fruits and cereal were the most common foods introduced (50%, n=4, each), followed by baby food and vegetables (37%, n=3, each).
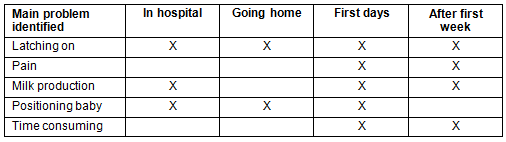
III. Timing of breastfeeding: The results showed that the main problems throughout the first weeks of breastfeeding included latching on and milk production. One mother had problems remembering the doctor's instructions, 'I was alone and to position the baby I couldn't remember the doctor's instructions so I could not get him positioned just right.' Other problems reported at different stages after giving birth are reported in Table 3.
Table 2: Summary of most important challenges faced while breastfeeding
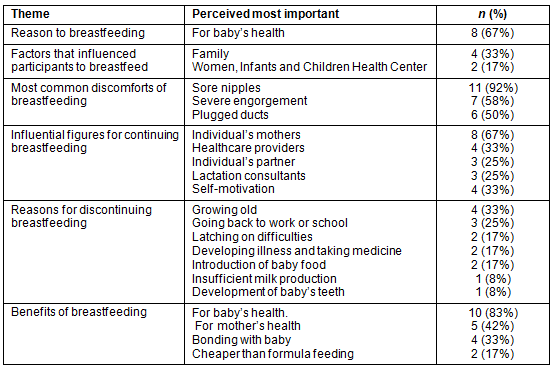
Table 3: Problems identified by mothers in different stages of breastfeeding
IV. Benefits of breastfeeding: The most common benefit of breastfeeding perceived by the participants was the health of the child (83%, n=10). Less than half perceived benefit to mother's health (42%, n=5), including losing weight acquired during pregnancy (33%, n=4), re-establishing a regular menstrual cycle (33%, n=4), and bonding between mother and baby (33%, n=4). Another benefit reported was that breastfeeding is a cheaper option than formula supplementation or baby foods (17%, n=2). Table 2 summarizes the most important factors perceived by the mothers among various themes.
V. Overall experience with breastfeeding: Participants were asked to share their experience with breastfeeding. The most common themes that emerged included benefits to the baby (33%, n=4) and overall greater satisfaction. One mother stated, 'I threw in the towel when my oldest one got jaundice and it stressed me out because I thought she wasn't getting enough nutrients.' Another mother declared that '[...] I felt good to know that I was giving my kids the best ... [the milk] comes from me and I know what I ate and what I consume, versus giving them something that who knows where it came from and what it is made of...' The results of the study showed that benefits to the baby and family influence can play a pivotal role in helping participants whether they want to breastfeed or not.
Discussion
Only 41% of participants breastfed for at least 6 months, and only one mother breastfed for 12 months. The Hispanic rural mothers most often recognized the health of the baby as a decisive factor to initiate breastfeeding. Only two mothers had previously taken prenatal breastfeeding classes, or planned to attend them in the future. This reflects a need to educate local Hispanic rural mothers about the importance of prenatal breastfeeding classes, as research has shown their effectiveness in increasing breastfeeding initiation and duration26,27.
The study results were similar to previous research that identified familial and cultural issues for breastfeeding practices, and the perceptions of general social disapproval28. The results have shown that the majority of the participants considered their mothers to be the most important help in continuing breastfeeding, similar to the results of a study done in urban Hispanic women29. Mothers should be presented with relevant information about the advantages of breastfeeding to improve the health of mother and child. Four participants (33%) had BSES-SF scores of 50 or less. Prior studies have shown that lower BSES-SF scores help identify mothers at high risk for early discontinuation of breastfeeding21,30,31. BAPT results indicated an above-average intention to breastfeed (average 30.5, SD=4.3), which is consistent with a previous study that reported similar results in a sample of 143 Hispanic mothers24.
Among Hispanic rural mothers, early introduction of solid foods or formula, eventually substituting breast milk, is an important issue. Two out of the 12 mothers had introduced solid foods before 6 months. High priority should be given to educating them on related health risks to their babies. Previous research has shown that solid foods introduced before 4 months of age was associated with a sixfold increase in obesity at 3 years of age32; and one study established that early exposure to formula is a risk factor for the development of childhood type 1 diabetes33. Family interference was identified by mothers in the focus groups and indicates that educating family members may be as relevant as educating mothers. Nutrition teaching should be provided to Hispanic rural mothers and grandmothers. Interventions to improve outcomes should be culturally sensitive and directed at the populations of specific geographic areas34.
The feedback obtained during the focus groups guided the development of the breastfeeding educational content. The educational program included information on nine major themes including: (i) basics of breastfeeding, (ii) how to breastfeed, (iii) mother and child benefits, (iv) other breastfeeding benefits, (v) normal feeding signs, (vi) problems during breastfeeding, (vii) formula feeding, (viii) coping with situations, and (ix) getting pregnant while breastfeeding. A touch-screen enabled, bilingual, interactive breastfeeding educational program is being developed.
The study describes the factors that impact on breastfeeding practices among Hispanic rural women. Further, assessment of BSES and BAPT scales facilitates the development of the breastfeeding educational content. The study highlights the importance of identification of behavioral and cultural factors that might be essential to increase adoption of breastfeeding among Hispanic rural women.
Acknowledgements
The current study was funded by the Agency for Healthcare Research Quality (AHRQ) #HS021321 01A1. The authors would like to thank Lupe Salazar, who helped the researchers with the facilitation and Spanish communication during the focus groups, and conducted the transcription of sessions.
References
1. Clark SGJ, Bungum TJ. The benefits of breastfeeding: an introduction for health educators. Californian Journal of Health Promotion 2003; 3(1): 158-163.
2. Dewey KG, Heinig MJ, Nommsen-Rivers LA. Differences in morbidity between breast-fed and formula-fed infants. Journal of Pediatrics 1995; 126(5): 696-702.
3. Duffy LC, Faden H, Wasielewski R, Wolf J, Krystofik D. Exclusive breastfeeding protects against bacterial colonization and day care exposure to otitis media. Pediatrics 1997; 100(4): e7.
4. Gartner LM, Morton J, Lawrence RA, Naylor AJ, O'Hare D, Schanler RJ, et al. Breastfeeding and the use of human milk. Pediatrics 2005; 115: 496-506.
5. Centers for Disease Control and Prevention. Breastfeeding report card 2011. Atlanta, GA: Division of Nutrition, Physical Activity, and Obesity, 2011. Available: www.cdc.gov/breastfeeding/pdf/2011breastfeedingreportcard.pdf (Accessed 21 January 2013).
6. US Department of Health and Human Services. Maternal, infant and child health, objectives new to healthy people 2020. Developing Healthy People 2020. (Online) Available: http://healthypeople.gov/2020/topicsobjectives2020/overview.aspx?topicid=26 (Accessed: 5 October 2012).
7. Kloeblen-Tarver AS, Thompson NJ, Miner KR. Intent to breast-feed: the impact of attitudes, norms, parity, and experience. American Journal of Health Behavior 2002; 26(3): 182-187.
8. Wells KJ, Thompson NJ, Kloeblen-Tarver AS. Intrinsic and extrinsic motivation and intention to breast-feed. American Journal of Health Behavior 2002; 26(2): 111-120.
9. Chapman DJ, Pérez-Escamilla R. Breastfeeding among minority women: moving from risk factors to interventions. Advances in Nutrition 2012; 3(1): 95-104.
10. Hurley KM, Black MM, Papas MA, Quigg AM. Variation in breastfeeding behaviours, perceptions, and experiences by race/ethnicity among a low-income statewide sample of Special Supplemental Nutrition Program for Women, Infants, and Children (WIC) participants in the United States. Maternal and Child Nutrition 2008; 4(2): 95-105.
11. Centers for Disease Control and Prevention. Provisional formula supplementation of breast milk rates by socio-demographic factors, among children born in 2007. National Immunization Survey, 2007. Available: www.cdc.gov/breastfeeding/data/NIS_data/2007/sociodemographic_formula.htm (Accessed: 21 January 2013).
12. Li R, Ogden C, Ballew C, Gillespie C, Grummer-Strawn L. Prevalence of exclusive breastfeeding among US infants: the Third National Health Examination Survey (Phase II, 1991-1994). American Journal of Public Health 2002; 92: 1107-1110.
13. Chatterji P, Brooks-Gunn J. WIC participation, breastfeeding practices, and well-child care among unmarried, low-income mothers. American Journal of Public Health 2004; 94: 1324-1327.
14. Kurinij N, Shiono PH, Ezrine SF, Rhoads GG. Does maternal employment affect breast-feeding? American Journal of Public Health 1989; 79: 1247-1250.
15. Kuan LW, Britto M, Decolongon J, Schoettker PJ, Atherton HD, Kotagal UR. Health system factors contributing to breastfeeding success. Pediatrics 1999; 104: e28.
16. Ertem IO, Votto N, Leventhal JM. The timing and predictors of the early termination of breastfeeding. Pediatrics 2001; 107: 543-548.
17. Taveras EM, Capra AM, Braveman PA, Jensvold NG, Escobar GJ, Lieu TA. Clinician support and psychosocial risk factors associated with breastfeeding discontinuation. Pediatrics 2003; 112: 108-115.
18. Taveras EM, Li R, Grummer-Strawn L, Richardson M, Marshall R, Rêgo VH et al. Opinions and practices of clinicians associated with continuation of exclusive breastfeeding. Pediatrics 2004; 113: e283-e290.
19. Flower KB, Willoughby M, Cadigan RJ, Perrin EM, Randolph G. Understanding breastfeeding initiation and continuation in rural communities: a combined qualitative/quantitative approach. Maternal and Child Health Journal 2008; 12(3): 402-414.
20. Krueger RA and Casey MA. Focus groups: a practical guide for applied research, 3rd edn. Thousand Oaks, CA: Sage Publications, 2000.
21. Dennis CL. The breastfeeding self-efficacy scale: psychometric assessment of the short form. Journal of Obstetric, Gynecologic, and Neonatal Nursing 2003; 32(6): 734-744.
22. Dick MJ, Evans ML, Arthurs JB, Barnes JK, Caldwell RS, Hutchins SS, et al. Predicting early breastfeeding attrition. Journal of Human Lactation 2002; 18(1): 21-28.
23. Evans ML, Dick MJ, Lewallen LP, Jeffrey C. Modified breastfeeding attrition prediction tool: prenatal and postpartum tests. Journal of Perinatal Education 2004; 13(1): 1-8.
24. Gill SL, Reifsnider E, Lucke JF, Mann AR. Predicting breastfeeding attrition: adapting the breastfeeding attrition prediction tool. Journal of Perinatal and Neonatal Nursing 2007; 21(3): 216-224.
25. Fishbein M, Ajzen I. Predicting and changing behavior: the reasoned action approach. New York, US: Psychology Press, 2010.
26. Sikorski J, Renfrew MJ, Pindoria S, Wade A. Support for breastfeeding mothers (Cochrane review). In: The Cochrane Library, Issue 3, 2003. Oxford: Update Software, 2003.
27. Wambach KA, Aaronson L, Breedlove G, Domian EW, Rojjanasrirat W, Yeh HW. A randomized controlled trial of breastfeeding support and education for adolescent mothers. Western Journal of Nursing Research 2011; 33(4): 486-505.
28. Wilhelm SL, Rodehorst TK, Stepans MB, Hertzog M, Berens C. Influence of intention and self-efficacy levels on duration of breastfeeding for Midwest rural mothers. Applied Nursing Research 2008; 21(3): 123-130.
29. Bunik M, Clark L, Zimmer LM, Jimenez LM, O'Connor ME, Crane LA, et al. Early infant feeding decisions in low-income Latinas. Breastfeeding Medicine 2006; 1: 225-235.
30. Wells KJ, Thompson NJ, Kloeblen-Tarver AS. Development and psychometric testing of the prenatal breast-feeding self-efficacy scale. American Journal of Health Behavior 2006; 30(2): 177-187.
31. Gregory A, Penrose K, Morrison C, Dennis CL, MacArthur C. Psychometric properties of the Breastfeeding Self-Efficacy Scale-Short Form in an ethnically diverse UK sample. Public Health Nursing 2008; 25(3): 278-284.
32. Huh SY, Rifas-Shiman SL, Taveras EM, Oken E, Gillman MW. Timing of solid food introduction and risk of obesity in preschool-aged children. Pediatrics 2011; 127(3): e544-e551.
33. Hyppönen E, Kenward MG, Virtanen SM, Piitulainen A, Virta-Autio P, Tuomilehto J, et al. Infant feeding, early weight gain, and risk of type 1 diabetes. Childhood Diabetes in Finland (DiMe) Study Group. Diabetes Care 1999; 22(12): 1961-1965.
34. Philipp BL, Malone KL, Cimo S, Merewood A. Sustained breastfeeding rates at a US baby-friendly hospital. Pediatrics 2003; 112: e234-e236.

