There is great disparity between the health status of Aboriginal and non-Aboriginal peoples in Canada. Of particular concern to the pediatric population are alarmingly high rates of early childhood caries (ECC). Early childhood caries is defined by the presence of tooth decay in one or more primary teeth in children younger than 6 years1. The prevalence of ECC typically ranges between 50% and 100% across Aboriginal communities2. Prevalence rates are generally higher in rural communities compared to urban areas2.
The development of ECC requires the biologically based triad of host susceptibility: the condition of tooth enamel; a diet containing fermentable carbohydrates such as glucose, fructose and lactose, where prolonged exposure (eg through bottle-feeding) poses a great risk for ECC3; and exposure to cariogenic bacteria such as Streptococcus mutans. Hygiene practices are important, especially in overcrowded households where poor hygiene may promote the spread of S. mutans amongst household members4-6. Many of these factors are affected by socioeconomic status (SES), which broadly encompasses the greatest risk factor for ECC5.
At an individual level, ECC may cause great physical pain and social distress to a child7. Early childhood caries may also adversely affect child growth and development leading to caregiver burden and stress7,8. Severe ECC, left untreated, usually requires tooth extraction by surgical intervention under general anesthesia. Not only does surgical intervention under general anesthesia carry its own set of health risks, but also it may displace children and their caregivers from their communities to distant hospitals9. This treatment carries significant financial cost for families and insurance companies for the procedure itself as well as costs related to travel and lodging. Early childhood caries also increases the risk of tooth decay in permanent teeth10 as well as periodontal and cardiovascular disease in later life11. Given the range and severity of the consequences of ECC, a number of strategies have been developed to prevent the development and recurrence of ECC through oral health promotion and hygiene.
Strategies to prevent ECC in Aboriginal communities
Health Canada implemented the Children's Oral Health Initiative (COHI) in 2004 to help prevent dental disease and promote oral health in Aboriginal children12. COHI services target mothers during the prenatal period and children younger than 7 years. COHI services are usually offered by a dental hygienist who visits rural communities regularly to provide dental screening and oral health counseling.
In addition to COHI, several community-based interventions have been designed for Aboriginal women during the antenatal period to help prevent ECC. One such intervention took place in an Ontario First Nations community13. This program distributed oral health information brochures in English and Oji-Cree along with toothbrushes and tippee cups to mothers with infants between 6 months and 12 months, and offered guided grocery shopping sessions with nutritionists. Health workers also provided oral hygiene information, such as toothbrushing technique, during visits with children and throughout local media. An evaluative study revealed outcomes such as increased knowledge about child oral health; unfortunately, night-time use of baby bottles persisted13.
Another community-based intervention in a First Nations community in British Columbia specifically sought to decrease bottle-feeding with sugary beverages14. Whereas willow cradles had been traditionally used to soothe crying children, this tradition was replaced by bottle-feeding. Local mothers and health workers collaborated with researchers to create and distribute willow cradles to parents to soothe their children. Community advertising about ECC prevention and individual counselling with a community nurse were also part of the intervention. Findings included slight improvement in child oral health, fewer reports of night-time bottle-feeding and greater community awareness about ECC risks.
Oral hygiene teaching alone was not enough to decrease the pervasive and harmful practice of night-time bottle-feeding in the former study13; in the latter study, an intervention targeting local beliefs resulted in decreased night-time bottle-feeding and also directly implicated local community members in improving their children's health in a culturally appropriate manner14. The present study builds on these findings by exploring a wider range of oral health beliefs pertaining to school-age children.
One school- and community-based intervention, the Brighter Smiles Initiative, was designed to reduce ECC and took place in the First Nations community of Hartley Bay, British Columbia15. This intervention was developed in collaboration with university dentistry faculty members, community elders and community health workers and targeted children, pre-kindergarten to grade 12, and their parents. Supervised toothbrushing sessions and weekly fluoride washes with incentive for participation based on draws for prizes were main elements of intervention. Presentations about nutrition, oral health, and related topics were also offered to children at the local school. Key outcomes at 3 years included increased dental visits for preventative dental care as well as increased community capacity, especially of community health workers to organize other prevention programs at school15,16.
Although the Brighter Smiles initiative was successful in improving the oral health of school-age children15,16, community beliefs about oral health were not explored in this study. Exploration of such beliefs can lead to better understanding of common practices harmful to children's health and can ultimately help in designing culturally adapted interventions to reduce harmful practices.
The Algonquin community of Rapid Lake, Quebec
As in many other rural Aboriginal communities, ECC is of concern in the Algonquin community of Rapid Lake, a semi-isolated community located in the Outaouais region of western Quebec. Examination by a dental hygienist in 2011 revealed high rates of ECC, with greater than 50% of the children in the community having had surgery for ECC. The McGill Ingram School of Nursing (ISoN) has collaborated with this community to conduct community-based research over the past 6 years17-19. The community requested collaboration with the McGill ISoN to design a culturally adapted activity to promote oral health in school-aged children in their community.
Rapid Lake is the home to the Algonquin of Barriere Lake, a community of 680 registered community members, over half of whom live in Rapid Lake. Community services include a daycare, an elementary school that also teaches Algonquin language, and a youth center offering activities after school, staffed by a youth coordinator and two youth workers. Health services are provided at the Kitiganik Health Clinic, which is funded by Health Canada. At the time of the study, the clinic was staffed by four nurses, a community health representative (CHR), a local maternal child worker, a drug and alcohol counselor as well as several support staff. The clinic hosted a dentist part-time, and a hygienist a few days per month as part of the COHI program already described.
This research project was conducted between September and December 2012 as part of the student researcher's requirements for a Masters of Nursing degree. The purpose of the project was to learn about local beliefs and practices regarding oral health and to use this knowledge to design and implement a culturally adapted activity to promote oral health among school-age children in the community. A community-based participatory research (CBPR) design was used given its link to positive outcomes for community oral health promotion10,14. For instance, the CBPR framework takes into account the power imbalances that have resulted from a long and devastating history of colonialism and forced assimilation. This power differential is today reinforced by ongoing government disputes with Aboriginal peoples regarding rights to self-government, land, and economic resources. The main tenets of CBPR include developing community strengths and resources; supporting co-learning and empowerment, taking social inequalities into account; using knowledge and action for the benefit of all partners; disseminating findings to all partners; and long-term committed relationships20.
Conceptual frameworks
Two conceptual frameworks were used to guide this study's understanding of oral health in Rapid Lake: Aboriginal understandings of health, and components of the PRECEDE-PROCEED framework. The first framework, Aboriginal understandings of health, was used to ground the study's design, analysis and interpretation in understandings of Aboriginal worldviews, particularly the local culture of Rapid Lake. According to this framework, the health of Aboriginal children is linked to culturally based practices that promote the use of Indigenous languages; oral teachings from elders about traditional life; interrelationships between the land, tribes, families, and ancestors; and holistic views of well-being and health based on spiritual, emotional, mental and physical dimensions21,22.
The second conceptual framework was adapted from the PRECEDE-PROCEED framework. PRECEDE refers to Predisposing, Reinforcing and Enabling Constructs in Educational/Environmental Diagnosis and Evaluation23. Watson et al. used this model in a community-based oral health program in a low socioeconomic community, for which they identified predisposing constructs (eg knowledge, attitudes, and beliefs about oral health and caries), reinforcing constructs (eg support from family and healthcare providers), and enabling constructs related to access to dental care (eg language spoken, insurance coverage) to play a role in the oral health of participants24. This model was used to help conceptualize factors affecting oral health in the current study, especially during the design of the interview guide.
Project design
Focused ethnography was used in this project, a methodology adapted from cultural anthropology and based upon a constructivist framework that assumes multiple realities are co-created through interactions amongst participants and between researchers and participants25. Focused ethnography is a type of ethnography that lends itself to a relatively short timeframe and answers questions more specific than may be the case in traditional ethnography26.
This project consisted of four phases (Fig1). Participant observation was a key method of data collection throughout each phase, for which data were recorded through a series of detailed field notes after interaction with participants. The goal of phase 1 was to learn about child oral health and hygiene practices from a range of community members. Six key informants were recruited for individual semi-structured interviews based upon an interview guide (Appendix I). Purposive sampling ensured a range of participants27: three participants were Algonquin community members and three were non-Algonquin workers from the Kitiganik Health Clinic; two of the six participants were men and overall age range was 22-58 years. Together, the six participants represented various community positions including healthcare worker (n=3), school staff (n=1), mother with infants (n=1), and elder (n=1). Given the influential role of elders in the community and their knowledge of traditional practices, a local elder was sought to participate in the study, in accordance with an Indigenous school health promotion framework22.
Following this, two convenience samples27 were recruited: children between 9 and 11 years from Cycle 3 (grades 3-5) at Rapid Lake School (n=7), and their parents (n=8). The goal of working with children of this age was to facilitate dialog about oral health as well as to promote oral health with children who could later act as role models for younger children. A focus group was organized at the day center for parent participants, the goal of which was to generate discussion amongst participants and explore oral health beliefs in general. The focus group used an interview guide similar to the one used during interviews with community members. A group interview was then organized with the child participants at the youth center based on further adaptation to the interview guide (Appendix II). The group interview was more structured than the focus group, because its goal was to inquire about specific topics, knowledge, and behaviors and thus was more about information gathering than a group conversation. The local youth coordinator and youth workers helped facilitate the interview and all further activities with the child participants.
The goal of phase 2 was to build and pilot test an activity to promote oral health amongst local children. Two activities were created, each tested with child participants from phase 1 and their peers in Cycle 3 (n=14). Written and verbal feedback about the activities was sought from child participants.
The goal of phase 3 was to revise the activities based on participant feedback and observations. The re-designed activities were retested in the Cycle 3 class (n=14) and feedback was again gathered.
The goal of phase 4 was to disseminate findings among community members (children and adults) through an interactive presentation. Anonymous written feedback was requested from all attendees.
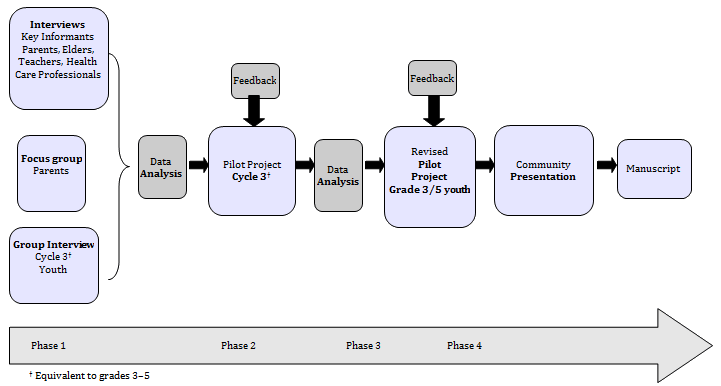
Figure 1: Schematic overview of study design
Data analysis
Interview data were audio-recorded and then transcribed for thematic content analysis; participant-observation data were recorded via fieldnotes. During phase 1, data was analyzed sequentially: transcripts and field notes from the first interview were read and coded for emergent concepts, the codes were then used for subsequent interviews, with additional new codes added as they emerged. This process was repeated for all key informant interviews, after which codes were grouped into broader concepts. This analysis was then used to build the focus group interview guide. Transcripts and field notes from the focus group were analyzed in a similar manner, building upon the codes and concepts derived from previous data; a similar process was used for the group interview with children.
Preliminary findings were shared with on-site co-researchers and community members working with youth. Discussion amongst co-researchers (including off-site supervisors) resulted in the organization of concepts into categories, subcategories, and overarching themes. Feedback from participants and community members pertaining to the activities and the community presentation were compiled and analyzed for convergence and divergence with previously identified concepts and themes.
Methodological rigor was ensured through three key processes: reflexivity, triangulation, and transferability26. The student researcher sought to be reflexive by documenting personal thoughts, feelings, and concerns, and corresponding regularly with McGill supervisors. Data and investigator triangulation were ensured by seeking multiple data sources, using several methods of inquiry, and by including multiple investigators. Contextual descriptions of the setting and participants in Rapid Lake were sought to facilitate assessment of transferability of results to other rural Aboriginal communities27.
Ethics approval
Ethical approval was obtained from the McGill Institutional Review Board (IRB) prior to commencement of the project (IRB Assurance Number FWA 00004545). The project followed guidelines for research pertaining to Aboriginal peoples outlined in the Tri-Council policy statement: 'Ethical conduct for research involving humans'28. The student researcher's entry into the community was facilitated by the long-standing partnership between the McGill Ingram School of Nursing and the Rapid Lake community. Project approval was sought from staff at Kitiganik Clinic and the local CHR prior to project commencement. The local youth coordinator was an active project collaborator throughout all phases of the research and thus has been included as an author.
This analysis identified three main themes, which together illustrate the state of child oral health in Rapid Lake as well as influencing factors and the importance of parental involvement in promoting child oral health.
Theme 1: The gap between oral health knowledge and practice
According to local community health workers, oral health knowledge in the community has increased in the 3 years since the dentist and hygienist began providing monthly services in Rapid Lake. For example, participants in the focus group attributed poor oral health in infants to bottle-feeding sugary beverages instead of breast-feeding, a message often expressed by the dental hygienist during maternal/child workshops in the community. Yet, despite this knowledge, parents were often observed giving their infants and children bottles of juice or sugary water to drink. In some extreme cases, staff at the health clinic observed children awaiting surgical intervention for decayed teeth drinking sugary beverages by bottle, despite extensive oral hygiene teaching to the family. Thus, although parents were aware of causes of tooth decay and the harm associated with bottle-feeding sugary beverages, this practice continued.
In addition, when child participants of the group interview were asked about the causes of tooth decay, they unanimously answered 'candy' and other foods and drinks that are high in sugar content. They also agreed that brushing their teeth after eating sugary foods would help to prevent cavities. Yet, when asked about how often they ate candy and how often they brushed their teeth, it became clear that candy is popular while toothbrushing is not. When children were asked if they would brush their teeth at home that evening, only about half said they would.
Although oral health knowledge has increased in many areas, important misconceptions about oral health remain unchallenged. For example, few child participants associated juice with tooth decay, despite its acidity and high sugar content. Also, a few parents mentioned that brown sugar is a healthier food and beverage additive than white sugar.
Theme 2: Challenges for oral health promotion
Challenges for oral health promotion in Rapid Lake can be broadly classified into attitudes and beliefs, access, and priorities.
Attitudes and beliefs: A common childrearing practice in Rapid Lake that challenges oral health promotion is the practice of feeding babies sugar water in a bottle. While exploring beliefs related to this practice, a healthcare worker noted that some parents believe that sugar water helps babies sleep soundly. Further, one young mother reported that some parents in the community believe that their infants will simply not drink sugar-free liquids. Another belief that challenges oral health promotion is local understandings of baby teeth: since primary teeth fall out, explained one mother, parents believe it is not important to take care of them. Also, parent participants described 'laziness' as an important challenge to oral health promotion. During the focus group, almost all parents used this term to describe local barriers to oral hygiene practices. For example, they attributed laziness to parents not brushing their children's teeth, or their own teeth. When asked to elaborate, a wide range of nuances emerged. For example, one parent exemplified laziness as 'being hung over from drinking or using drugs' while another talked about laziness related to being 'sick with diabetes'. Some parents described being lazy as 'just because', and a mother who worked at the school said that she felt 'lazy' in the evenings after work.
Access issues: Participants identified a number of issues related to access to the resources needed to promote oral health. For example, parents discussed the challenges of buying healthy foods in the community. As told by one parent:
There are no stores, grocery stores, in the reserve. And when your baby is hungry and you have no milk, powdered juice is fast. It's not because you don't know [that powdered juice is bad for oral health].
Indeed, the closest grocery store and health supply store are located at least 45 minutes away from Rapid Lake by car. While makeshift convenience stores open from time to time in the community, they have limited healthy options, focusing instead on chips, pop (soft drink) and candy. There are no stores with health supplies in Rapid Lake, and so children without a toothbrush often wait for the hygienist to bring supplies. While some supplies are available at the health clinic and school, they are limited. Two child participants reported that they cannot brush their teeth at home because they do not have toothbrushes.
In addition, many community members have limited income and this challenges their access to healthy foods and health supplies. Many homes in Rapid Lake lack the basic infrastructure to store healthy food. According to one community worker, non-perishable items like 'powdered juice, peanut butter, jelly and bread, cornflakes [with powdered milk or water] with sugar' are popular because many homes lack the plumbing and electricity required to power a freezer or fridge. For one mother, these poor living conditions combine with the realities of overcrowding to seriously limit oral hygiene practices. In her words: 'Here [there is] one small bathroom for 12 people in the same house. A small bathroom and you put 12 toothbrushes, where?'
Finally, impeded access to oral health professionals was seen as a barrier to oral health. Most months during the project, a dentist visited the community for 1 day per month. Those who missed the visit would have to wait until the following month or travel hours to an adjacent city to see a dentist. As of 2013, no dentist was visiting the community.
A hierarchy of priorities: Community members identified a number of key priorities that superseded oral health. These priorities included addressing drug and alcohol use, physical and sexual abuse, and unemployment. Such challenges had already led to social services removing some children from homes and placing them in foster care. Such disruption was seen to fundamentally challenge the overall health and stability of the community. An elder spoke about the ongoing land struggles that directly threaten the health and wellbeing of the Algonquin; land provides a sacred ground for cultural wellness and healing. According to this elder, oral health cannot be seen in isolation from cultural and community health and wellness.
Theme 3: The importance of parents in health promotion strategies
There are multiple local strategies in place to promote children's oral hygiene practices. These strategies are largely based on the COHI dental hygienist's work along with clinic staff and teachers. Parents also play a crucial role in oral health promotion, a point made clear by community workers and parents alike during interviews and the focus group. The problem, as expressed by one parent participant, is that many parents do not feel themselves to be strong role models in this respect. For example, parents who were residential school survivors did not learn about oral hygiene as children and consequently have poor oral health. It was suggested that access to oral health education workshops for parents would help to promote oral hygiene for the entire family.
From this analysis, two key outcomes were inspired and enacted: the development of activities to promote oral health among local children, and the increased capacity of community members and researchers to address local health.
The first outcome was the development of a life-sized Eagles & Otters board game (approximately 180 × 270 cm) built using Snakes & Ladders as a model (Appendix III). An eagle was chosen by community members as a symbol of flying high and therefore moving up on the game board and an otter was chosen for being playful and sliding down the game board. Both animals are found locally in Rapid Lake and have significance in local culture. The game included question squares linked to cards with questions based on areas of learning that emerged from interviews. While playing the game and answering oral health related questions, children engaged in active debate with their teammates; they played repeatedly, improving their scores as they played. Teachers requested the game be adapted to include questions about other health concerns (eg overall hygiene).
The second activity was designed to move beyond health knowledge to healthy oral hygiene practices. It involved a toothbrushing calendar and a checklist to be filled out at home (Appendix IV). Each completed activity sheet would be returned to the school for a small prize. The children were actively engaged and eager to win a prize.
After each activity was developed and implemented, the student researcher organized a final event at the local community center. All participants and collaborators were invited to attend. The presentation included interactive educational material from SipSmart, a program designed for use in classrooms by Quebec Heart & Stroke Foundation29. The material included an exhibit with eggs soaked in various sugary beverages displaying the negative effects of sugar and acid on the shell of an egg, which was likened to tooth enamel. Attendees of all ages were engaged throughout the presentation, asking questions and responding to questions posed, reinforcing knowledge acquired. Prizes were distributed and all child attendees received dental supplies.
A final outcome of this study was increased capacity of community members to address local health needs. For example, the youth coordinator, teachers and school nurse were eager to further develop the activities created to promote oral health and overall health. The dental hygienist and the student researcher both gained hands-on experience implementing culturally adapted health interventions. Additionally, children and parents acquired new knowledge to share with others and apply at home in the promotion of oral health.
Discussion
This project used community-based participatory research (CBPR) to explore oral health and hygiene practices with community members in Rapid Lake. CBPR made it possible to build upon the long-term relationship between Rapid Lake and McGill's Ingram School of Nursing as well as to draw on community strengths and resources to improve children's oral health knowledge and practices.
The authors found that general knowledge of oral hygiene was considerable among parent and child participants; this finding is particularly important given that knowledge has been identified as one of several predisposing constructs affecting oral health behaviors24. Yet it was also found that knowledge alone was not sufficient to motivate changes in oral health practices. For example, while parents were aware that feeding infants with sugary beverages causes tooth decay, many continued this practice. One reason cited for feeding infants sugary beverages was limited access to milk and healthy alternatives. The practice of breastfeeding could help ameliorate these access issues; however, rates of breastfeeding in Rapid Lake are low30. Importantly, a recent study in the community focused on identifying and alleviating barriers to breastfeeding30.
Another reason cited for feeding infants and children sugary beverages was the belief that it would soothe them. This finding is similar to that of a study mentioned above that established infant feeding as a comfort practice among First Nations people14. Beliefs have been identified as another key predisposing construct24; greater understanding of these beliefs can lead to successful culturally based interventions. For example, the use of willow cradles as an alternative comforting practice resulted in a decrease of bottle-feeding14. A similar infant comforting practice could be explored for use in Rapid Lake where the practice of wrapping a baby in a birch bark cradleboard was traditionally used in the community to soothe infants.
The notion that 'laziness' is a common barrier to oral health can be explored through the concept of motivation. For example, a prior study examining oral health outcomes in patients with diabetes linked laziness to lack of motivation31. Further, interventions based on motivational interviewing targeting an individual's motivation to change have been used with parents to increase child oral hygiene practices32,33. These interventions involved counselors working with parents to increase their motivation to adopt health practices, for example by using a non-confrontational style to point out discrepancies between parent-stated health goals and their behaviors. This type of support from healthcare workers could represent a reinforcing construct for oral health behaviors24.
Importantly, laziness may itself point to deeper issues than just motivation. Persons with low SES have been found to interpret mental health problems as personality traits such as laziness34. The promotion of mental wellness may be relevant for persons in the community complaining of laziness given that, in general, approximately 30% of First Nations persons have experienced depression, sadness or feeling blue for extended periods35. Addressing mental wellness may help to promote overall health in Rapid Lake.
Access to the resources needed to promote oral health was an important issue brought up by the study participants, a factor that may be considered as enabling oral health behaviors. Access to healthy foods and health supplies such as toothbrushes is limited because of geographic isolation and limited income; access to junk foods, by comparison, is quite easy. According to Sherman et al., promoting consumption of traditional foods such as moose, beaver and partridge - foods accessed directly from the land instead of from a grocery store - may help improve overall health18. Restricted access to stores could be mitigated by the local health clinic carrying toothbrushes and toothpaste in larger quantities. Further, community-based initiatives that distribute healthy meals to families, as well as community gardens, could help address issues of access while promoting food security at the local level36. Broader interventions aimed at improving access to grocery stores and health supply stores, as well as interventions to increase economic opportunities and ensure adequate housing, are essential components to the promotion of oral health37.
The final theme identified a need for parental involvement in oral health initiatives. In particular, facilitating opportunities for parents to learn about oral health through outreach programs was suggested as a way to promote parents' own oral health as well as their children's. This could be facilitated through a newly developed parent-teacher association which aims to foster collaboration between parents and teachers. This type of support could help reinforce oral health behaviors and increase parental capacity. Other barriers to oral health included lack of role models and priorities that supersede oral health. A lack of positive role models may be particularly relevant for families in which parents are residential school survivors. Moving forward a generation, these parents may face challenges with caring for their own children given their own experience and lack of role models21. Outreach using incentive gifts, positive phone calls and newsletters may help improve engagement38.
Following the tenets of CBPR, the activities created through this study drew directly from local culture and experience. The Eagles & Otters game incorporated an Aboriginal worldview that linked health with the local cultural environment21,22. In Rapid Lake, connecting with the land is associated with general health and wellbeing17. Incorporating animals native to the land as symbols in the game promoted discussion and awareness amongst the children about the significance of these animals in local culture. The children demonstrated enhanced knowledge of oral health after playing the game, and showed a keen desire to engage in health-promoting activities; this enthusiasm concurs with findings from prior studies in the community17,18. Similarly, the activity sheet with prize rewards was based upon local experience using prizes to motivate behavior change. This strategy had previously been found successful during an influenza vaccination campaign at the local clinic, resulting in the highest number of 'flu vaccinations in recent memory.
As with any study, there are limitations to be considered in interpreting the findings. First, while participants were community members chosen for their ability to speak about oral health experiences, their views do not necessarily represent those of the entire community. Second, because of a concurrent study in the community, it was not possible to work more directly with the maternal-child program. Prenatal women and their infants postpartum were therefore not directly involved in this study. Finally, the student researcher spent only 4 months in the community, which limited the level of rapport that could be established with research participants. Notwithstanding these limitations, this study has several strengths. Using CBPR, the authors were able to build upon a 5-year collaboration with Rapid Lake to promote oral health among local children as well as to develop capacity-building with parents, local community workers and the nursing student.
Through community-based participatory research, this study explored oral health and hygiene beliefs and practices among children in Rapid Lake and developed culturally based activities for healthy engagement. The findings demonstrate that children can be actively engaged in oral health promoting activities, and that parents, essential to children's oral hygiene and health, need and seek outreach initiatives to help enhance their own capacity with their children. Systemic factors that affect oral health in the community, such as access to healthy foods and health supplies, stem from geographic isolation and limited income. While local interventions, such as the distribution of healthy meals or stocking the local clinics with toothbrushes, may help address some of these challenges, broader interventions addressing substance abuse, crowded housing, and land resources remain essential to enable the necessary conditions to promote and sustain oral health and overall community wellness.
Acknowledgements
The authors acknowledge funding from Health Canada throughout the project. The authors are grateful for the support of Rapid Lake School staff, community youth workers, and staff at Kitiganik Clinic. The authors especially thank the Cycle 3 class for their participation and enthusiasm throughout the project. Finally the authors would like to acknowledge the expertise and input of Denise Chief, dental hygienist.
References
1. American Academy of Pediatric Dentistry. Definition of early childhood caries (ECC). Pediatric Dentistry 2005; 27(7): 13.
2. Schroth R, Smith W. A review of repeat general anesthesia for pediatric dental surgery in Alberta, Canada. Pediatric Dentistry 2007; 29(6): 480-487.
3. Davies GN. Early childhood caries - a synopsis. Community Dentistry and Oral Epidemiology 1998; 26(S1): 106-116.
4. Gussy MG. Early childhood caries: current evidence for aetiology and prevention. Journal of Paediatrics and Child Health 2006; 42(1-2): 37-43.
5. Gibson S, Williams S. Dental caries in pre-school children: associations with social class, toothbrushing habit and consumption of sugar and sugar-containing foods. Further analysis of data from the National Diet and Nutrition Survey of children aged 1.5-4.5 years. Caries Research 1999; 33(2): 101-113.
6. Lewis CW, Riedy CA, Grossman DC, Domoto PK, Roberts MC. Oral health of young Alaska Native children and their caregivers in Southwestern Alaska. Alaska Medicine 2002; 44(4): 83-87.
7. Filstrup SL, Briskie D, da Fonseca M, Lawrence L, Wandera A, Inglehart MR. Early childhood caries and quality of life: child and parent perspectives. Pediatric Dentistry 2003; 25(5): 431-440.
8. Irvine JD, Holve S, Krol D, Schroth R, Canadian Paediatric Society, First Nations, Inuit and Métis Health Committee. Early childhood caries in indigenous communities: a joint statement with the American Academy of Pediatrics Society. Pediatric Child Health 2011; 16(6): 351-357.
9. Schroth RJ, Harrison RL, Moffatt ME. Oral health of indigenous children and the influence of early childhood caries on childhood health and well-being. Pediatric Clinics of North America 2009; 56(6): 1481-1499.
10. Manitoba Institute of Child Health. Oral health and the Aboriginal child: a forum for community members, researchers and policy-makers. Executive summary of forum proceedings. (Online). Available: http://oralhealth.circumpolarhealth.org/files/2009/07/Dental_ExecutiveSummaryofForumProceedings-Nov27-2007.pdf (Accessed 18 September 2013).
11. de Oliveira C, Watt R, Hamer M. Toothbrushing, inflammation, and risk of cardiovascular disease: results from Scottish Health Survey. British Medical Journal 2010. 340: c2451.
12. National Aboriginal Health Organization. Children's oral health initiative overview. Presented at Our People, Our Health conference; 24-26 November, Crowne Plaza Hotel, Ottawa, Canada, 2009.
13. Lawrence HP, Romanetz M, Rutherford L, Cappel L, Binguis D, Rogers JB. Effects of a community-based prenatal nutrition program on the oral health of Aboriginal preschool children in northern Ontario. Probe 2004; 38(4): 172-190.
14. Harrison RL, White LA. A community-based approach to infant and child oral health promotion in a British Columbia First Nations community. Canadian Journal of Community Dentistry 1997; 12(1): 7-14.
15. Harrison RL, MacNab AJ, Duffy DJ, Benton DH. Brighter smiles: service learning, inter-professional collaboration and health promotion in a First Nations community. Canadian Journal of Public Health 2006; 97(3): 237-240.
16. Macnab AJ, Rozmus J, Benton D, Gagnon FA. 3-year results of a collaborative school-based oral health program in a remote First Nations community. Rural and Remote Health 8(2): 882. (Online) 2008. Available: http://www.rrh.org.au/journal/article/882 (Accessed 18 September 2013).
17. Lang C, Macdonald ME, Carnevale F, Lévesque MJ, Decoursay A. Kadiminekak kiwabigonem: barriers and facilitators to fostering community involvement in a prenatal program in an Algonquin community. Pimatisiwin: a Journal of Aboriginal and Indigenous Community Health 2010; 8(1): 55-80.
18. Sherman J, Macdonald ME, Carnevale F, Vignola S. The development and implementation of a type 2 diabetes prevention program for the youth in the Algonquin community of Rapid Lake, Quebec. Pimatisiwin: a Journal of Aboriginal and Indigenous Community Health 2011; 9(1): 219-243.
19. Kooiman H, Macdonald ME, Carnevale F, Pineda C, Nottaway W, Vignola S. Minododazin: translating an Algonquin tradition of self-respect into youth well-being in Rapid Lake, Quebec. Pimatisiwin: a Journal of Aboriginal and Indigenous Community Health 2012; 10(1): 1-15.
20. Israel BA, Schulz AJ, Parker EA, Becker AB. Review of community-based research: assessing partnership approaches to improve public health. Annual Review of Public Health 1998; 19: 173-202.
21. Blackstock C, Bruyere D, Moreau E. Many hands, one dream: principles for a new perspective on the health of First Nations, Inuit and Métis children and youth. Summary of the conference of the same title held in Victoria, BC, 3 December 2005. (Online) 2006. Available: http://www.fncaringsociety.com/sites/default/files/manyhands-principles.pdf (Accessed 18 September 2013).
22. Tagalik S. A framework for indigenous school health: foundations in cultural principles. (Online) 2010. Available: http://www.nccah-ccnsa.ca/docs/nccah%20reports/nccah_cash_report.pdf (Accessed 18 September 2013).
23. Green L. The PRECEDE-PROCEED model of health program planning and evaluation. (Online). Available: http://www.Igreen.net/precede.html (Accessed 20 September 2013). Green, LW, Kreuter MW. Health program planning: an educational and ecological approach. New York: McGraw-Hill, 2005.
24. Watson MR, Horowitz AM, Garcia I, Canto MT. A community participatory oral health promotion program in an inner-city Latino community. Journal of Public Health Dentistry 2001; 61(1): 34-41.
25. Roper JM, Shapira J. Ethnography in nursing research. Thousand Oaks, CA: Sage Publications Inc., 2000.
26. Knoblauch H. Focused ethnography. Forum: Qualitative Social Research 2005; 6(3): Art. 44.
27. Polit DF, Beck CT. Essentials of nursing research: appraising evidence for nursing practice. 7th edn. Philadelphia, PA: Lippincott, Williams & Wilkins, 2009.
28. Canadian Institute of Health Research, Natural Sciences and Engineering Research Council of Canada and Social Sciences and Humanities Research Council of Canada. Tri-Council policy statement: ethical conduct for research involving humans. (Online) 2010. Available: http://www.pre.ethics.gc.ca/pdf/eng/tcps2/TCPS_2_FINAL_Web.pdf (Accessed 18 September 2013).
29. Heart and Stroke Foundation. Sip Smart: quick start overview of resource guide. (Online). Available: http://boissante.soisfute.ca/en/demarrage/survol_du_manuel#introduction-survol (Accessed 20 September 2013).
30. Levesque MJ, Dumas L, Lepage M. L'influence des grand-mères dans les décisions liées à l'alimentation des jeunes enfants en milieu autochtone (MSc thesis). Quebec: Université du Québec en Outaouais, 2013.
31. Kneckt MC, Syrjälä AH, Knuuttila ML. Attributions to dental and diabetes health outcomes. Journal of Clinical Periodontology 2000; 27(3): 205-211.
32. Freudenthal JJ, Bowen DM. Motivational interviewing to decrease parental risk-related behaviors for early childhood caries. Journal of Dental Hygiene 2010; 84(1): 29-34.
33. Weinstein P, Harrison R, Benton T. Motivating mothers to prevent caries: confirming the beneficial effect of counseling. Journal of the American Dental Association 2006; 137(6): 789-793.
34. Horwitz AV. Help-seeking processes and mental health services. New Directions for Mental Health Services 1987; 36: 33-45.
35. First Nations Centre. First Nations Regional Longitudinal Health Survey (RHS) 2002/03: results for adults, youth and children living in First Nations communities. First Nations Centre, 2005.
36. Dieticians of Canada. Individual and household food insecurity in Canada: position of Dieticians of Canada. Canadian Journal of Dietetic Practice and Research 2005; 66: 43-46.
37. Reading CL, Wien F. Health inequalities and social determinants of Aboriginal peoples' health. (Online) 2009 Available: http://www.nccah-ccnsa.ca/docs/social%20determinates/NCCAH-loppie-Wien_report.pdf2009 (Accessed 20 September 2013).
38. Kavanagh B. Teaching in a First Nations school: an information handbook for teachers new to First Nations schools. (Online) 2006. Available: http://www.fnesc.ca/wordpress/wp-content/uploads/2011/05/Teaching%20in%20a%20FN%20School.pdf (Accessed 18 September 2013).
__________________________
Appendix I: Sample questions for interviews with key informants and parents in focus groups

Appendix II: Sample questions for group interview with children

Appendix III: Eagles & Otters game

Appendix IV: Oral health calendar: 1-week example