The Centers for Disease Control and Prevention (CDC) Diabetes report card 20121 notes that both the incidence of newly diagnosed diabetes as well as the prevalence of diabetes increased dramatically beginning in the early 1990s. Numbers of new cases almost tripled between 1990 and 2010. One projection indicates that at least one out of every three adults could have diabetes by 2050 if current trends prevail1.
Diabetes results in other major medical conditions, due to complications, resulting in increased healthcare costs1. In March 2013, the American Diabetes Association (ADA) reported that diabetes costs increased from US$174 billion in 2007 to US$245 billion by 2012, a 41% increase. This accounts for US$176 billion in direct medical costs and US$69 billion in lost productivity. People with diabetes experience more than twice the average medical expenses and have higher rates of work loss than individuals with other chronic diseases1-3. The ADA reports that those with diabetes spend about US$13,700 annually on healthcare costs, with about US$7,900 of that amount attributed to diabetes. Persons with diabetes are more likely to experience stroke, heart disease, and other serious complications including vision loss, kidney failure, limb amputation and high blood pressure1,2.
A pathway for a public health approach to diabetes prevention and diabetes management has been adopted by the CDC's National Diabetes Prevention Program. The Diabetes Prevention Program demonstrated success using a cognitive behavioral approach in a variety of settings and formats to prevent diabetes for those at risk4. Program findings indicate that modest behavior changes, such as improving food choices, increasing physical activity to 150 minutes per week, and losing 5-7% of body weight reduces risks of developing type 2 diabetes by 58% in individuals with pre-diabetes5. Additionally, self-management strategies such as daily glucose monitoring, controlling high blood pressure and cholesterol levels, lifestyle changes in terms of nutrition and physical activity, daily foot exams, and medical management including annual physical, eye and feet exams by a healthcare professional, regular A1c (blood glucose) tests and recommended immunizations can reduce diabetes risks and complications6. Finally, there is broad recognition that the obesity increase across the population is linked to increased diabetes7,8.
The various factors linked with diabetes suggest a three-pronged strategy to address diabetes at the community level. Primary prevention aims to reduce obesity rates through increased awareness of the risks of diabetes, education about the importance of healthy nutrition and daily physical activity, and opportunities to engage in healthy lifestyle choices. Secondary prevention targets individuals who have been diagnosed or determined to be at-risk along with their family members, promoting regular screening and targeting those diagnosed and at-risk with effective programs to help make healthy food choices, increase physical activity, and make modest weight reductions. Tertiary prevention targets individuals diagnosed with type 2 diabetes and helps them effectively manage the disease through self- and medical management.
Long-recognized health disparities among populations related to diabetes exist. African-Americans, Native Americans, Asian Pacific Islanders and Hispanic populations are known to be adversely affected by diabetes compared with other population groups6. Diabetes has been found to be particularly serious for those residing in the geographic region of Appalachia. Using data from the National Health and Nutrition Examination Survey (NHANES) and the Behavioral Risk Factor Survey, the states with Appalachian counties have been identified as areas with the highest diabetes prevalence9,10. Furthermore, people living in distressed or at-risk Appalachian counties tend to be diagnosed with diabetes 2-3 years earlier than peers in non-Appalachian counties11.
Background
The Appalachian region is a large geographic region that extends along the Appalachian Mountain range from southern New York to counties in Alabama, Georgia, and Mississippi. Counties from 12 states and all of West Virginia, 420 counties in total, cover an area of 330 000 km212. This mountainous region differs somewhat from the surrounding areas, especially in the northern and central region, as its population is primarily Caucasian. Many inhabitants have not only multiple generations of ancestors from the region, but also extended families living nearby, often within a short distance and in the county where they were born and raised12,13. Although much of the region is rural, Appalachian people are not isolated, but choose to live where life is less harried by progressive change. Past traditions still influence the present. Many residents choose these long-valued places near extended family members and friends despite obstacles of high unemployment, extended poverty, lowered educational opportunities, and other disparities. Shared local history and linkages to family and friends hold great sway over residents' daily lives13,14.
This rural area is a 'diabetes belt,' an area with high rates of type 2 diabetes similar to those of the nation's minority groups15. Those living in rural Appalachia have limited access to hospitals, physicians, specialists such as endocrinologists, certified diabetes educators, and dietitians16. Lack of health insurance, long distances to healthcare services, and competing financial needs that outweigh spending money for medical expenses also delay seeking care16,17. Social networks often have greater influence over daily life than health professionals14. Many regional residents view type 2 diabetes as commonplace, expected, and not as bad as conditions like cancer or heart disease. Lack of education and support for disease management, inadequate knowledge about high risks for complications linked to poor self-management, and poor understandings about healthy lifestyles and prevention often mean the condition is ignored, under-treated, and poorly managed16,18.
Beginning in 2009, with support from the CDC's National Diabetes Education Program, a community-based effort using a family-focused approach was initiated. Diabetes: A Family Matter is an intervention that focuses on citizen action, culturally sensitive education, support and the mobilization of family, friends, neighborhoods, and community resources to increase diabetes awareness9. The Family Health Model19 guided the creation of an intervention aimed at local coalition development. Using a train-the-trainer model, local health providers and community volunteers were prepared. A culturally relevant toolkit employed an 'edutainment' approach to diabetes education20. The toolkit materials included ideas about family care and fun, entertainment, rural perspectives, personal stories, and low health literacy.
The toolkit employs images and stories that depict families living in the rural Appalachian region. It includes an online and print version of the Family Matters diabetes educators manual for coalition leaders and health professionals, a SUGAR helpers manual for community volunteer training, brochures and handouts, posters, and photo novellas. The website www.diabetesfamily.net included functionality to encourage social networking.
In a 2-year pilot, 11 Appalachian counties, in Ohio, West Virginia, and Kentucky, with diabetes rates among the highest in the nation, were selected to participate. Each county was invited to develop a local coalition of health professionals and designate a local coordinator. Eight Ohio counties were recruited in the first year and seven additional counties from Ohio, West Virginia and Kentucky were recruited in the second year. Using a train-the-trainer model, the investigators conducted 2 days of trainings each year with representative team members from the county coalitions. The trainings covered diabetes topics, prevention, ways to use the materials in the toolkit, and how to recruit and train a group of local volunteers. Those trained were asked to recruit and train a group of community volunteers, incorporate them into the coalitions' work, and develop plans for community engagement. At the end of each year, representatives of the coalitions attended a networking event where they shared their successes, challenges, and plans for the coming year.
Data collection
This study was a non-randomized prospective mixed-methods study that used a one-group design to test the effectiveness of the model to:
- engage and train local health professionals
- utilize culturally appropriate tools
- put to use a train-the-trainer model with health professionals enabling them to recruit and train community volunteers
- establish local coalitions whose focus is on increasing awareness and promoting healthy lifestyle changes.
At the initial training, coalition participants completed a knowledge test to examine understandings of the diabetes disease process, family roles in healthy eating, active living, diabetes management, and prevention. Additionally, efficacy questions about abilities to engage others in diabetes prevention and awareness were included. The same knowledge test with efficacy questions was also administered to volunteers at the beginning of the volunteer training that each coalition conducted. The knowledge test was re-administered later to all coalition participants, volunteers and health professionals.
Two measures and qualitative findings from focus groups and open-ended survey response questions examined the usefulness of the print material and online tools. The unique number of website visits and total numbers of visits were monitored throughout the project and beyond. Additionally, coalition members, health professionals, and trained volunteers were asked to rate the tools in terms of how often components were used and how useful, accurate, interesting, and comprehensible components appeared to be. The tools were rated initially at the end of training sessions when they were introduced and then near the close of the project after participants used them. Finally, three focus groups were held at the final event at the end of years one and two with county liaisons, health professionals, and with volunteers. Questions about the utility of the tools and approach were included.
Evidence of the coalition development and training of local volunteers was gathered through coalition and project reports, focus groups held at the end of each year, and annual interviews with coalition coordinators. Evidence of community engagement was collected qualitatively through coalition reports, end-of-year presentations, coordinator interviews, artifacts from events, and focus group findings from the final event.
Ethics approval
This study was approved by Ohio University's Office of Research Compliance, Approval #14EO30.
Coalition members' knowledge and self-efficacy
In all, 43 individuals (16 health professionals and 27 volunteers) completed pre- and post-knowledge tests. Thirty-nine of them also completed the efficacy assessment, which included questions about their ability to talk with others about diabetes, lifestyle changes and healthy nutrition. Using a paired samples t-test, the analysis showed the change in perceived efficacy was significant, and knowledge about diabetes and information about diabetes and families approached significance (Table 1). Based on the pre-test scores, the results show that these participants possessed a high degree of knowledge about diabetes and diabetes prevention prior to participation (Table 2).
Table 1: Difference scores from pre- and post-test of knowledge and self-efficacy among coalition members
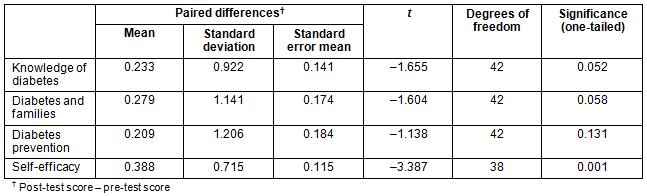
Table 2: Pre- and post-test means by topic
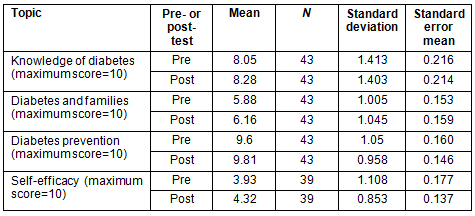
Website utilization and toolkit assessment
Between the first and second year, the technician managing the website changed, and different website statistics were provided. In the first year, the average number of daily visits were calculated, while in the second year and after the project was completed, monthly statistics on the number of unique visitors was also provided. In all 3 years, the total number of website visits per month was recorded. In the first year, website use nearly doubled between the third and fourth month and then doubled again between the fourth and fifth month. This was when local coalitions were recruiting and training volunteers. The total number of visits then vacillated until July and August when the end-of-year training events were held. Website use decreased somewhat in the first four months of the second year as new coalitions were brought on, but increases appeared again around month five and remained until the end of the project. Data from 2 years post-project demonstrated that website use remained fairly steady even after the project's formal completion, as many of the county coalitions continue their activities and others gain access to the website (Fig1).
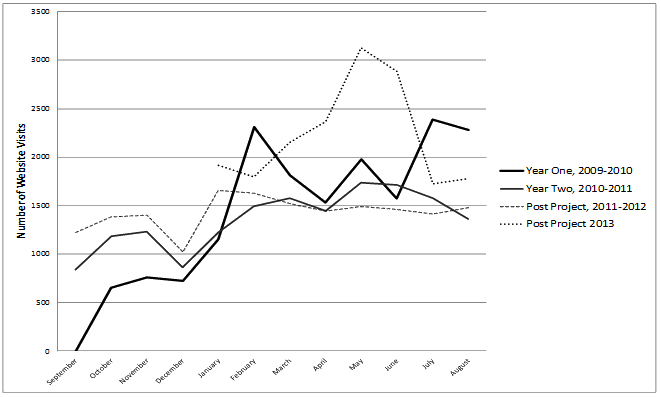
Figure 1: Monthly website usage rates by year.
Toolkit materials
In the first year, 30 health professionals were asked to rate the materials in the toolkit, using a scale of 1-5 (5='strongly agree') between the first and second initial training, after the materials had been reviewed with them. At the end of the project, 31 participants, 20 health professionals and 11 trained community volunteers again rated the tools in the Family Matters Toolkit. Table 3 indicates that most tools were highly rated initially and the ratings decreased slightly after participants had the opportunity to use the tools. Most respondents agreed the tools were useful, easy to understand, presented in an interesting way, and possessed accurate information.
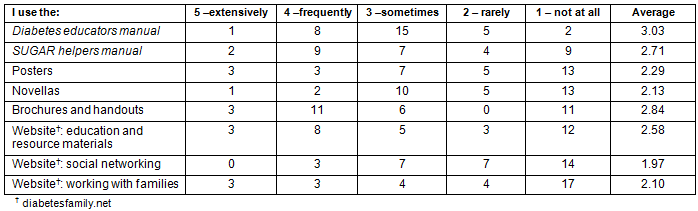
In the final assessment, participants were asked how often they used each tool. As Table 4 indicates, the Diabetes educators manual was most often used, followed by the SUGAR helpers manual. 'Sugar' is the term often used to refer to diabetes in the Appalachian region. Thus, SUGAR (Support to Unite Generations in the Appalachian Region) Helper became the acronym used to refer to participating volunteers. Most materials were put to use in their print form. The website was most often used for education and resources. The website was not substantially employed as a social networking tool or when working directly with families.
The responses from the focus groups at the closing event echo the quantitative findings. Participants generally had positive comments about the tools. Brochures, posters, and the pyramid plate were most frequently noted. Comments included, 'these [tools] are very relevant to the area we serve' and 'information on diabetes is presented in a way that people can relate to and it doesn't seem so clinical.' Others commented on how the brochures were used: 'The family brochures are also great with their story telling approach. I also use these with SUGAR Helpers training and encourage them to use them to start diabetes discussions. We used the brochures at our Hike for Health last year to educate participants.' Participants reported that the brochures, novellas and posters were frequently used during awareness-raising events they attended throughout the year such as health fairs and other events the teams organized.
Opinions of the manuals were roughly divided between coordinators and community volunteers. Some coordinators reported using the manuals less often, reasoning that people were resistant to so much reading material, while others integrated the manuals into their volunteer training. 'I have used it [SUGAR helper manual] for training sessions and for talks that I give. It gets to the point and is easy to understand by lay individuals.' Several volunteers reported an appreciation for the manuals, citing the consistency and common knowledge base it provided for all team members. It was suggested that materials with fewer words and more visual qualities, such as online videos, would be better for the focus audience of community members. Participants reported that the brochures, photo novellas, and posters were frequently used during awareness-raising events they attended throughout the year - health fairs and other events the teams organized.
Table 3: Family Matters Toolkit ratings
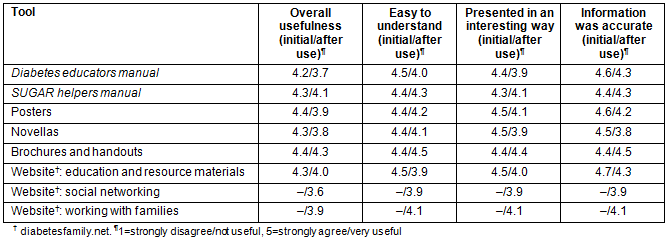
Table 4: Family Matters Toolkit: use of materials by type
Coalition development and volunteer training
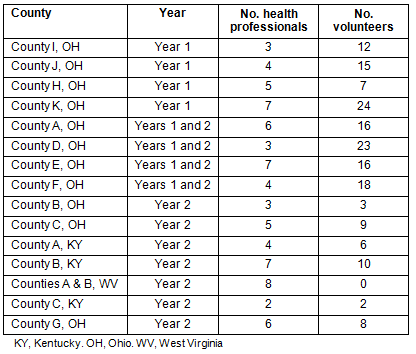
Records reflect that in the first year, 38 healthcare professionals participated in the initial training and 29 returned for the second training session 1 month later. In the second year, 30 participants, including both volunteers and health professionals, attended a 2-day training session. Coalition reports indicated that all but one of the coalitions successfully recruited volunteers. Four of the coalitions participated across both years, continuing to recruit volunteers. Table 5 indicates the number of participants who completed at least one assessment tool, usually the pre-assessment administered at the beginning of volunteer training.
Focus groups and interview findings all support the challenges of recruiting volunteers. Some coordinators noted that while they felt well prepared to discuss diabetes and conduct training, they did not feel confident in their ability to recruit volunteers. Several strategies were identified including word of mouth, personal invitation and partnering with other efforts. For example, partnering with an established program through the university extension services to teach people how to prepare healthy food was useful. Identifying individuals with diabetes or family members experiencing diabetes was often identified by coordinators as a strategy to obtain passionate and interested volunteers.
Coalition reports indicated that 14 of the 15 participating coalitions held volunteer trainings. Most coalitions conducted four or five training sessions, although one coalition conducted only one session and two coalitions conducted seven or eight sessions. Reports reflect that training sessions typically focused on the problem of diabetes in the region, health risk factors, healthy eating, and active living. The goal of the training sessions was to encourage volunteers to talk informally with friends, family, neighbors and church members about diabetes as well as the value of healthy eating and active living. Increasing the visibility of the problem was a major aim of the toolkit project. Coalition members who were health professionals expressed concerns about volunteers providing medical guidance: 'We made it clear to them in the beginning, we didn't expect them to be experts, we just wanted them to talk about making healthy life choices.'
Local coordinators noted the lifestyle changes that occurred among coalition members, especially community volunteers. 'We had a volunteer who used the education from her training to help her husband, who has diabetes, lose 63 pounds, and get better control of his blood sugar.' There were numerous reports of volunteers forming walking groups. Several volunteers discussed the value of the information they received on healthy nutrition. Thirty-one of the volunteers in the second year completed a questionnaire about changing their own behavior and influencing others to make changes. Most were more willing to make a change in personal behavior, with 97% indicating they had increased their physical activity and 94% reporting eating a healthier diet. Eighty percent said they had made suggestions to family members about increasing physical activity and/or health nutrition.
Table 5: Number and type of coalition participant by county and year
Community engagement
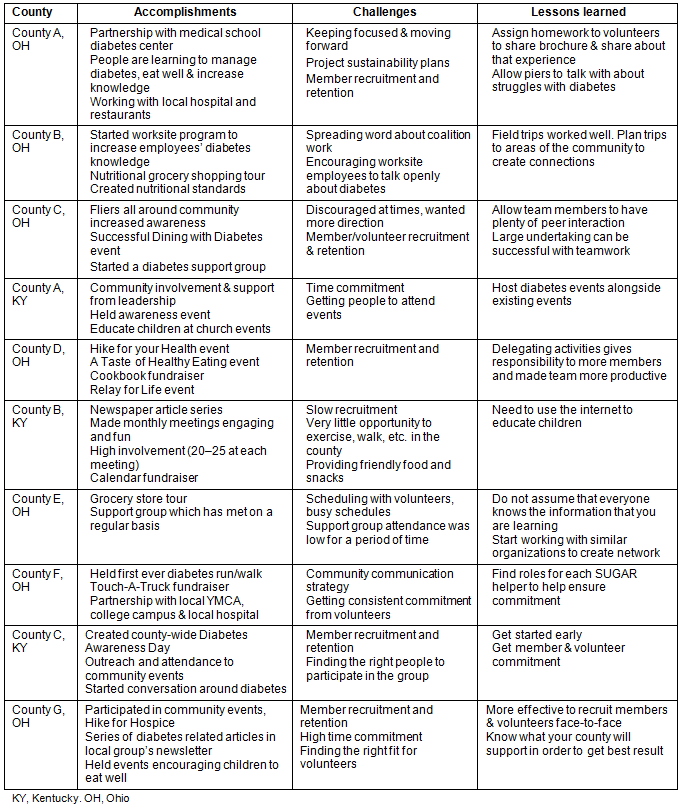
Year-end reports from the eight coalitions engaged in year one indicated that five of the coalitions were successful in their efforts to recruit, train, and engage volunteers, and implement a team strategy in their communities (Table 6). Two of the coalitions struggled with recruitment and training and one coalition participated minimally after the initial training. Four of these teams elected to continue in year two and seven new coalitions were added. Ten of the eleven coalitions in year two reported some degree of success with recruitment, training and community engagement.
Many coordinators noted that the recruitment and training of volunteers served as an important initial task for engaging coalition members. During interviews with county coordinators, the majority stated they worked to make training sessions as interactive as possible. In some counties, volunteers studied a subject in the manual and presented the information to the rest of the group. Such a hands-on approach was used whenever possible to create in students a sense of responsibility and control over their learning. Health professional presentations were a common part of most county trainings. Physicians, dietitians, podiatrists, and pharmacists frequently attended and shared information relevant to diabetes and prevention. Most of the coalitions had a number of health professionals who had participated in the initial training. Local coordinators engaged these professionals in the recruitment and design of the volunteer training.
Besides recruiting and training volunteers, the coalitions participated in a number of community awareness activities. The initiative did not prescribe the kinds of activities the coalitions should engage in and some were challenged by the breadth of opportunities. During the initiative, most of the coalitions participated actively in local health fairs and county fairs. They gave presentations at churches, schools, and places of work. Materials from the toolkit, especially brochures, handouts and novellas, were distributed to local health departments, social service agencies, recreational facilities and other public venues. Sponsoring one-time or ongoing walk/run events was another popular activity. Many offered nutrition and cooking classes/demonstrations, sometimes successfully partnering with ongoing diabetes management efforts by the local extension service.
Coalition leaders noted that open discussion of diabetes is not common in the Appalachian culture. This unwillingness to discuss the disease posed a challenge for the coalitions. To begin conversations, several teams turned to newspapers or organization newsletters. Teams submitted series of articles highlighting individuals in their community who have diabetes, which not only provided education about diabetes, but also raised awareness of a common issue in their community.
A number of coalitions developed some unique efforts. One coalition worked with local restaurants to offer healthier menu options. Another conducted grocery store tours, highlighting the nutritional information found on packaging and promoting health eating. A partnership with a large employer was a strategy undertaken by one coalition. Identifying a way to provide inexpensive or free diabetic medical supplies to people already dealing with type 2 diabetes was a focus of one coalition. Many of the successful coalitions noted that they partnered with other community groups or organizations with a vested interest in preventing diabetes. Partnerships with local health departments, universities, local businesses, schools, YMCAs, pharmacies, and healthcare organizations were established.
During the concluding focus groups, participants were asked where they believe the greatest community affect was made. One county saw the biggest change in children's activities dealing with healthy living and diabetes. Other coalitions mentioned the growing change seen as partnerships were made with private-sector companies and industries. Mentioned most often was the overall change in openness in discussing diabetes and healthy lifestyles. Participants attributed this change to increased awareness in their communities, educating the public about the disease, prevention strategies, and the existing network of support.
Several coalitions discussed plans for continued efforts after the project concluded. Some had designed products or events for fundraising for sustaining their work. One coalition created and sold a calendar that highlighted local people affected by diabetes and included information about healthy eating, while another published and sold a recipe book. One Kentucky coalition organized an event around basketball called Dribbling for Diabetes. Another coalition partnered with local restaurants and held Dining out with Diabetes fundraising events.
Table 6: Accomplishments, challenges, and lessons learned by coalitions
Discussion
The Diabetes: A Family Matter initiative was successful in the development of local coalitions with a variety of health professionals and lay volunteers in 14 counties. The coalitions participated in and then conducted training about diabetes and diabetes prevention using the materials from the Family Matters Toolkit. A number of the coalitions sponsored or participated in various community events and activities promoting diabetes prevention messages. Many customized materials from the toolkit to provide unique local products. These developing coalitions directly influenced the volunteers and coalition members in terms of providing increased education and awareness about diabetes and diabetes prevention.
The initial training focused on the crisis of diabetes and the information about diabetes management and prevention. Results showed increases in knowledge and self-efficacy. Feedback from coalition coordinators and key coalition members identified the importance of training and support for the recruitment, engagement, and retention of volunteers. Additionally, opportunities for coalitions to come together, share results of their activities, and exchange ideas with other teams was valuable. This provided insights and inspiration as well as opportunities for support and recognition.
Providing resources and tools that were user-friendly, accurate and appropriate to the culture of the communities was an important step. Results suggest that the coalitions used the materials provided and customized them for local use based on the information provided. Arming local coalition members with relevant and accurate materials and information, and encouraging them to engage family, neighbors, church members, and communities, is a model worth exploring, especially in rural areas. Informal social networks have a powerful impact on lifestyle choices, including healthy nutrition and active living of these rural Appalachian residents.
Using modest initial resources, providing training, support, and good materials and tools, is an economical approach to a community- and family-level prevention strategy. Using the coalition structure within a local community provides significant opportunities for ongoing sustainability beyond the initiative.
Type 2 diabetes and its complications are great risks for those living in the Appalachian region. However, relevant resources through usual treatments and traditional medical establishments seem inadequate to address growing problems. Innovative community programs and creative solutions that can reach people where they live, learn, work, play, and pray are still needed to combat the growing problem. Training local volunteers using culturally sensitive materials and working through social networks appear to be ways to educate residents of Appalachian communities about the risks and help support lifestyle changes. Culturally sensitive programs, such as Diabetes: A Family Matter, seem to be useful ways to address the problem.
References
1. Centers for Disease Control and Prevention. Diabetes Report Card 2012. Atlanta, GA: Centers for Disease Control and Prevention, US Department of Health and Human Services, 2012.
2. Yang W, Dall T, Halder P, Gallo P, Kowal S, Hogan P. Economic costs of diabetes in the U.S. in 2012. Diabetes Care 2013; 36(4): 1033-1046.
3. Egede L, Zheng D, Simpson K. Comorbid depression is associated with increased health care use and expenditures in individuals with diabetes. Diabetes Care 2002; 25: 464-470.
4. Kramer M, Kriska A, Venditti E, Miller R, Brooks M., Burke L, Siminerio L, et al. Translating the Diabetes Prevention Program: a comprehensive model for prevention training and program delivery. American Journal of Preventive Medicine 2009; 37(6): 505-511.
5. National Center for Chronic Disease Prevention and Health Promotion. National Diabetes Prevention Program. (Online) 2010. Available: http://www.cdc.gov/diabetes/prevention/about.htm (Accessed 10 December 2013).
6. Centers for Disease Control and Prevention. National diabetes fact sheet: national estimates and general information on diabetes and prediabetes in the United States. (Online) 2011. Available: http://www.cdc.gov/diabetes/pubs/pdf/ndfs_2011.pdf (Accessed 7 December 2013).
7. Ford E, Williamson D, Liu S. Weight change and diabetes incidence: findings from a national cohort of US adults. American Journal of Epidemiology, 1997; 146: 214-222.
8. Mokdad A, Ford A, Bowman B, Dietz W, Vinicor F, Bales V, et al. Prevalence of obesity, diabetes, and obesity-related health risk factors, 2001. Journal of the American Medical Association 2003; 289(1): 76-79.
9. Denham S. Diabetes and its management. In RL Ludke, PJ Obermiller (Eds). Appalachian health and well-being. Lexington, KY: University Press of Kentucky, 2012; 131-148.
10. Danaei G, Friedman A, Oza S, Murray C, Ezzati M. Diabetes prevalence and diagnosis in the U.S. states; analysis of health surveys. Population Health Metrics 7(16). (Online) September 2009. Available: http://www.pophealthmetrics.com/content/7/1/16 (Accessed 30 October 2013).
11. Barker L, Gerzoff R, Crespo R, Shrewsberry M. Age at diagnosis of diabetes in Appalachia. Population Health Metrics 9(54). (Online) September 2011. Available: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3203846/ (Accessed 30 October 2013).
12. Appalachian Regional Commission. The Appalachian region. (Online) 2014. Available: http://www.arc.gov/appalachian_region/TheAppalachianRegion.asp (Accessed 12 January 2014).
13. Billings DB, Norman G, Ledford K. Back talk from Appalachia: confronting stereotypes. Lexington, KY: University Press of Kentucky, 2000.
14. Denham SA, Manoogian M, Schuster L. Managing family support and dietary Routines: type 2 diabetes in rural Appalachian families. Families, Systems, & Health 2007; 25(1): 36-52.
15. Centers for Disease Control and Prevention. CDC identifies diabetes belt. (Online) 2011. Available: http://www.cdc.gov/diabetes/news/docs/diabetes_belt.htm (Accessed 12 January 2014).
16. O'Brien T, Denham SA. Diabetes care and education in rural regions. The Diabetes Educator 2008; 34(1): 334-347.
17. Denham SA, Remsberg K, Wood L. Diabetes education in the Appalachian region: providers' views. Rural and Remote Health 10: 1321. (Online) 2010. Available: www.rrh.org.au (Accessed 12 January 2014).
18. Denham SA, Wood L, Remsburg K. Diabetes care: provider disparities in the US Appalachian region. Rural and Remote Health 10: 1320. (Online) 2010. Available: www.rrh.org.au (Accessed 12 January 2014).
19. Denham S. Family health: a framework for nursing. Philadelphia, PA: FA Davis, 2003.
20. New World Encyclopedia. Edutainment. (Online) 2013. Available: http://www.newworldencyclopedia.org/entry/Edutainment (Accessed 12 January 2014).

