Colorectal cancer is the third most common cancer worldwide and ranks fourth among cancer killers1. The highest incidence rates occur in Australia, New Zealand, Canada, the USA, and parts of Europe2. Colonoscopy is effective for screening and prevention of colorectal cancer, and colonoscopic screening has been shown to save lives3. The procedure is recommended by multiple governmental and advocacy organizations as an effective means of screening for colon cancer4-6.
Well-accepted methods of screening for colorectal cancer include annual fecal occult blood testing and endoscopic screening. Despite the consensus recommendations for colon cancer screening in general, and for colonoscopy specifically, only 65% of people in the USA are current on their colon cancer screening7. Internationally, there is inadequate capacity to screen all eligible persons8-13. As the populations in both developing and developed countries age, it is anticipated that the need for well-trained endoscopists will continue to rise.
Residents in rural areas are screened for colon cancer at lower rates than their urban counterparts14-19. Most rural physicians are generalists and are not trained in colonoscopy. In the USA and Canada the majority of colonoscopies are performed by gastroenterologists20. In the USA overall, only 2.6% of family physicians provide colonoscopy to their patients, but this rate may be higher in rural areas21,22. If colonoscopies are to be available for colon cancer screening for patients in rural areas of developed countries, then generalists will need to be able to safely and efficaciously provide this service.
There are widely accepted standards for safe and effective colonoscopy that include reach-the-cecum rate (RCR), adenoma detection rate, cancer detection rate and rates of complications. The National Bowel Cancer Screening Program (NBCSP) Quality Working Group (Australia)23, the American College of Gastroenterology/American Society of Gastrointestinal Endoscopists24, the National Health Service in England25 and the Canadian Association of Gastroenterology26 have all published guidelines.
The purpose of this article is to systematically review available studies of rural colonoscopy to determine which types of providers are performing the procedure and to assess the reported quality of these procedures. Evidence of quality and effectiveness of colonoscopies provided by rural physicians is needed to guide development of programs to increase colonoscopy capacity in rural areas.
Study selection
A systematic literature search was conducted utilizing MEDLINE from 1951 to 1 September 2013. A search strategy was developed combining medical subject headings (MeSH) and text key words (tw) for (colonoscopy[tw] OR colonoscopies[tw] OR 'colonoscopy'[MeSH Terms:noexp] OR polypectomy[tw] OR polypectomies[tw]) AND rural[tw]. The search was not restricted by language. Inclusion criteria were rural location, report of quality outcomes, or report of endoscopy workforce in rural areas. Two investigators (DE, AC) reviewed potentially relevant articles independently, with differences resolved through discussion. To ensure completeness of the literature search, citation lists for the included studies published in the previous 5 years were reviewed. Additional articles identified through review of citation lists were reviewed and included if appropriate. This study did not meet criteria for human subjects research and did not require Institutional Review Board approval.
Data abstraction and validity assessment
Two reviewers (DE, AC) independently reviewed and abstracted data from each included study using a standardized data abstraction tool (Appendix I). The following information was obtained from each study: author identification, citation, study design, source of funding, study duration and follow-up, study population, sample size, study setting, population characteristics, outcomes and results. Validity was assessed using an Agency for Healthcare Research and Quality tool for assessing the strength of scientific evidence27. Each reviewer assessed for potential bias in assigning exposure and measuring outcomes, as well as incomplete reporting or selective reporting.
The search strategy identified 121 potentially eligible articles. After reviewing the abstracts and full texts when needed, only 11 articles met inclusion criteria. Ten of the included articles measured colonoscopy quality by rural physicians28-37. One study reported on the rural colonoscopy workforce20. An additional article on colonoscopy quality38 was identified by review of a 2009 meta-analysis of colonoscopy by primary care physicians39. There were no eligible systematic reviews, meta-analyses or randomized studies. Articles were excluded if they did not report standard quality outcomes or did not report results from colonoscopies done in a rural setting. Only primary research studies, not review articles, were included.
Table 1 summarizes the characteristics of the 11 studies measuring colonoscopy quality by rural practitioners. It includes four reports from Canada, one from Australia and six from the USA. The studies encompass 8703 procedures by 25 colonoscopists. Ten of the 11 studies report on consecutive procedures. Seven collected data prospectively, three were retrospective chart reviews, and one did not report the method of data collection. Five were multi-physician studies. Colonoscopist training is summarized when available.
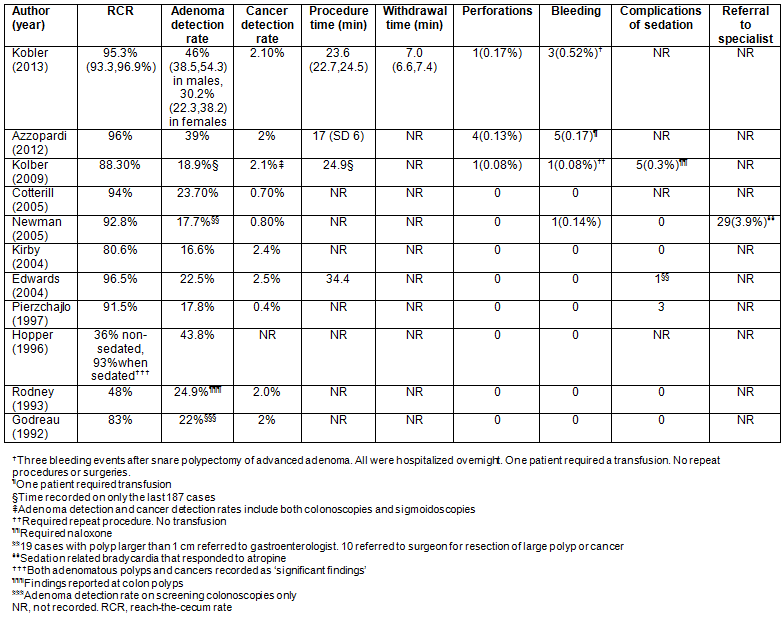
Table 2 displays the results of the 11 studies reporting colonoscopy quality measures. All studies reported RCR, adenomatous polyp detection rates and cancer detection rates. Four studies reported procedure time and one reported on scope withdrawal time. All studies reported complications of perforation and bleeding. Other reported complications included sedation complications and referrals to specialists, but there was considerable variation in how these complications were defined.
RCRs ranged from 36% to 96.5%. In studies less than 10 years old representing 6454 cases the RCR ranged from 80.6% to 96.5%. Adenoma detection rates ranged from 16.6% to 46%. Cancer detection rates ranged from 0.4% to 2.1%. Complications were uncommon. A total of six perforations, ten bleeding events and nine sedation complications were reported.
Studies focusing on the rural colonoscopist workforce studies were scarce. Hilsden et al. conducted a national study of Canadian endoscopists performing more than 100 cases per year20. In rural areas, 54% of colonoscopies were performed by general surgeons, 39% by gastroenterologists, and only 7% were performed by generalists.
Table 1: Summary of published studies reporting results of rural colonoscopy
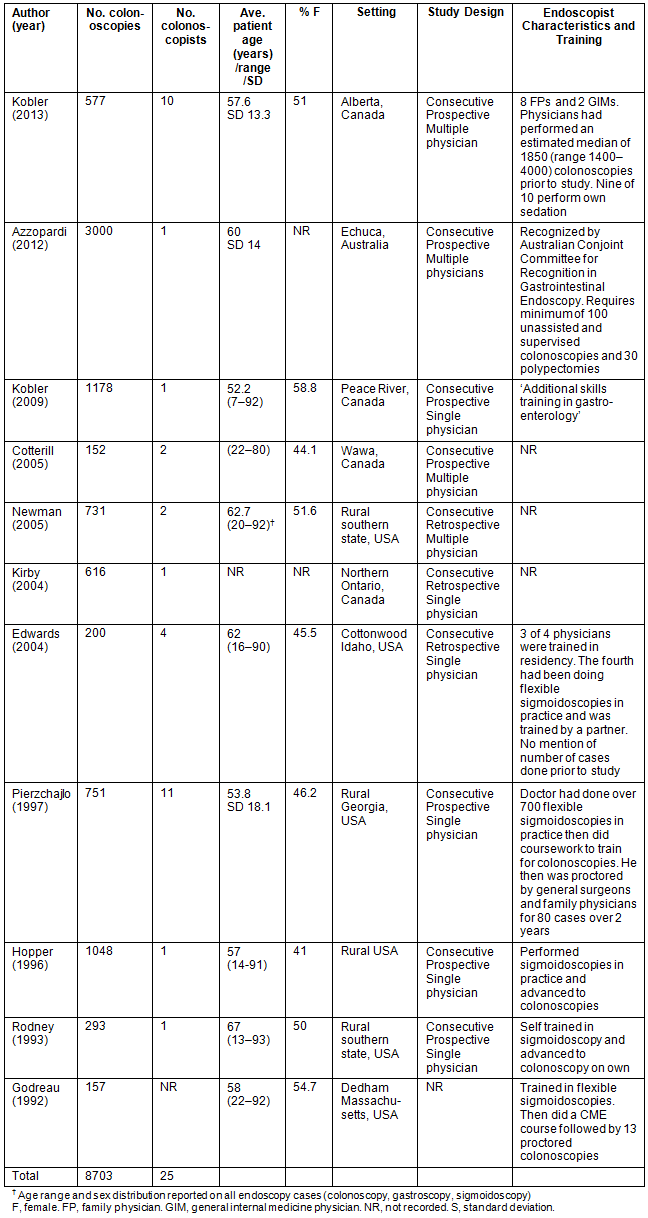
Table 2: Summary of quality of colonoscopies performed in rural areas
Discussion
This systematic review contributes to the growing body of literature that demonstrates that well-trained primary care providers can safely and effectively perform colonoscopy in rural settings. This is particularly important in developed countries where colonoscopy is the standard of care for colon cancer screening but access to colonoscopy in rural areas is limited.
Who performs colonoscopy in rural communities?
The only study meeting inclusion criteria and specifically focusing on workforce demonstrated that general surgeons perform most colonoscopy procedures in rural Canadian communities. The American Academy of Family Physicians workforce study noted that a small minority (2.6%) of US family physicians provide colonoscopy for their patients but it did not report on the rurality of these physicians. The vast majority of studies included in this review reporting quality showed cases by family physicians or general practitioners. Based on this literature review, the question of who provides colonoscopies in rural areas is unanswered. Future research to assess availability and training of colonoscopy providers in rural areas is warranted.
What, where and how well?
In contrast to the paucity of data around 'who' comprises the rural colonoscopy workforce, this review reports on 8703 colonoscopies by 25 rural physicians in three countries. Most studies report on both screening and diagnostic colonoscopies. The majority of these studies demonstrate high quality as measured by the generally accepted measures of reaching the cecum, adenoma detection and cancer detection.
Rex et al. report that 90% of all colonoscopies should reach the cecum and that the percentage should increase to 95% for screening exams40. However, a 2003 study of more than 17 000 procedures by 69 gastroenterologists in North America showed a median RCR of 88%. Only 55% of physicians had an RCR of 90% or greater41.
RCRs of rural colonoscopists are consistent with recommended standards. The present review found that 6 of 11 studies, representing 5411 of 8703 procedures, reported RCRs exceeding the 90% recommended by Rex et al29-32,34,35. One additional study of 1178 procedures exceeded 88%28. In the 1996 case series of 1048 procedures by Hopper et al36, they reported an RCR of only 36% in non-sedated patients. Using sedation the RCR increased to 93%.
The studies included in this review show variation in both cancer and adenoma detection rates. This variation is consistent with other studies of experienced colonoscopists40,42,43. Current accepted benchmarks of adenoma detection on screening of normal risk individuals are 25% in males and 15% in females23-26. Kolber et al. is the only study in this review that reported adenoma detection by gender, but included multiple indications for colonoscopy29.
While a small number of studies reported quality over time and demonstrated a training effect with respect to RCR30,32-34, other included studies did not29,31,35. Previous studies of gastroenterologists in training show improved quality with number of procedures44. There may also be improvement in performance with improvements in technology, as more recent cases show better RCRs.
A recent study from Canada reports that patients who have a negative colonoscopy performed by a gastroenterologist are less likely to develop colorectal cancer than those performed by people from other specialties45. This study reports on more than 110 000 cases but draws on data from 1992 to 1997. This finding was only significant among cases performed in a hospital and was not statistically significant among cases completed in a private/office setting. Further studies will be needed to corroborate these results.
This systematic review shows lower-than-expected rates of complications among rural colonoscopists. Frequency of colon perforation is reported at 0.14-0.65% for diagnostic procedures46,47. Perforations during therapeutic procedures in prior studies were found to be as high as 3%48. Only seven perforations were reported among the 8703 procedures (0.07%) reported here. The percentage of bleeding complications was only 0.11%. Many of the studies included here are from single providers. These solo endoscopists might have considerable influence on which patients are eligible for procedures locally and which patients require specialty referral. Referring physicians in a rural community might send more complex cases to tertiary settings as well. This could influence the low complication rate. Meyer et al. found that generalist cases are often of lower complexity than cases done by gastroenterologists49.
Limitations
This systematic review has multiple limitations. First, five of the studies reporting quality data are of cases performed by a single physician who was often the author. These cases may not be representative of rural endoscopists as a whole and may also introduce reporting bias. Second, most of the studies include multiple indications for colonoscopy or do not report specific indications as part of their data. Accepted benchmarks for cecal intubation and polyp and cancer detection are specific for screening exams. If a case series includes more repeat procedures, for example, the adenoma detection rate might be artificially high. Similarly, therapeutic procedures usually take longer and often result in higher complication rates.
This systematic review of 11 studies reporting on 8703 colonoscopies performed by rural generalists in three countries demonstrates that rural physicians can perform colonoscopies safely and effectively. These cases demonstrate cancer and adenoma detection rates consistent with generally acceptable standards and practices with correspondingly low rates of complications. Not enough data was available to draw conclusions about the specialty distribution of the rural colonoscopist workforce. However, it is clear that more rural colonscopists will be required to perform the recommended colon cancer screening on rural patients in developed countries. Training programs should be developed to address this need for high quality and effective rural colonoscopy.
Acknowledgements
The authors would like to thank Sarah Safranek, Information Management Librarian, at the University of Washington Health Sciences Library for her assistance with the literature search for this manuscript.
References
1. Wiseman M. The second World Cancer Research Fund/American Institute for Cancer Research expert report. Food, nutrition, physical activity, and the prevention of cancer: a global perspective. Proceedings of the Nutrition Society 2008; 67(3): 253-256.
2. Boyle P, Langman JS. ABC of colorectal cancer: epidemiology. BMJ 2000; 321(7264): 805-808.
3. Zauber AG, Winawer SJ, O'Brien MJ, Lansdorp-Vogelaar I, van Ballegooijen M, Hankey BF, et al. Colonoscopic polypectomy and long-term prevention of colorectal-cancer deaths. New England Journal of Medicine 2012; 366(8): 687-696.
4. Levin B, Lieberman DA, McFarland B, Andrews KS, Brooks D, Bond J, et al. Screening and surveillance for the early detection of colorectal cancer and adenomatous polyps, 2008: a joint guideline from the American Cancer Society, the US Multi-Society Task Force on Colorectal Cancer, and the American College of Radiology. Gastroenterology 2008; 134(5): 1570-1595.
5. ACOG Committee Opinion No. 384, November 2007: colonoscopy and colorectal cancer screening and prevention. Obstetrics and Gynecology 2007; 110(5): 1199-1202.
6. Colorectal cancer screening. Recommendation statement from the Canadian Task Force on Preventive Health Care. Canadian Medical Association Journal 2001; 165(2): 206-208.
7. Vital signs: colorectal cancer screening, incidence, and mortality - United States, 2002-2010. Morbidity and Mortality Weekly Report 2011; 60(26): 884-889.
8. Brown ML, Klabunde CN, Mysliwiec P. Current capacity for endoscopic colorectal cancer screening in the United States: data from the National Cancer Institute Survey of Colorectal Cancer Screening Practices. American Journal of Preventive Medicine 2003; 115(2): 129-133.
9. Armstrong D, Barkun ANG, Chen Y, Daniels S, Hollingworth R, Hunt RH, et al. Access to specialist gastroenterology care in Canada: the practice audit in gastroenterology (PAGE) wait times program. Canadian Journal of Gastroenterology 2008; 22(2): 155-160.
10. Leddin D, Armstrong D, Barkun ANG, Chen Y, Daniels S, Hollingworth R, et al. Access to specialist gastroenterology care in Canada: comparison of wait times and consensus targets. Canadian Journal of Gastroenterology 2008; 22(2): 161-167.
11. Centers for Disease Control and Prevention. A survey of endoscopic capacity (SECAP I). (Online) 2000. Available: http://www.cdc.gov/cancer/colorectal/what_cdc_is_doing/screening_capacity.htm.(Acessed 6 October 2013).
12. Yeoman A, Parry S. A survey of colonoscopy capacity in New Zealand's public hospitals. New Zealand Medical Journal 2007; 120(1258): U2632.
13. Fernando SA, Duggan AE, Dent OF, Eikli MC. Colonoscopy capacity in selected New South Wales hospitals. Medical Journal of Australia 2007; 187: 249-250.
14. Bennett KJ, Pumkam C, Bellinger JD, Probst JC. Cancer screening delivery in persistent poverty rural counties. Journal of Primary Care and Community Health 2011; 2(4): 240-249.
15. Cole AM, Jackson JE, Doescher M. Urban-rural disparities in colorectal cancer screening: cross-sectional analysis of 1998-2005 data from the Centers for Disease Control's Behavioral Risk Factor Surveillance Study. Cancer Medicine 2012; 1(3): 350-356.
16. Coronado GD, Thompson B, Chen L. Sociodemographic correlates of cancer screening services among Hispanics and non-Hispanic whites in a rural setting. American Journal of Health Behavior 2009; 33(2): 181-191.
17. Coughlin SS, Thompson TD. Colorectal cancer screening practices among men and women in rural and nonrural areas of the United States, 1999. Journal of Rural Health 2004; 20(2): 118-124.
18. Rankin SL, Hughes-Anderson W, House AK, Heath DI, Aitken RJ, House J. Costs of accessing surgical specialists by rural and remote residents. ANZ Journal of Surgery 2001; 71(9): 544-547.
19. Anderson AE, Henry KA, Samadder NJ, Merrill RM, Kinney AY. Rural vs urban residence affects risk-appropriate colorectal cancer screening. Clinical Gastroenterology and Hepatology 2013; 11(5): 526-533.
20. Hilsden RJ, Tepper J, Moayyedi P, Rabeneck L. Who provides gastrointestinal endoscopy in Canada? Canadian Journal of Gastroenterology 2007; 21(12): 843-846.
21. American Academy of Family Physicians. AAFP practice profile 2011. (Online). Available: http://www.aafp.org/about/the-aafp/family-medicine-facts/table-12.html (Accessed 6 October 2013).
22. American Academy of Family Physicians. Colonoscopy (position paper). (Online). Available: http://www.aafp.org/about/policies/all/colonoscopy.html (Accessed 21 October 2013).
23. Cancer Council Australia Colonoscopy Surveillance Working Party. Clinical Practice Guidelines for Surveillance Colonoscopy - in adenoma follow-up; following curative resection of colorectal cancer; and for cancer surveillance in inflammatory bowel disease. (Online) 2011. Available: http://wiki.cancer.org.au/australia/Guidelines:Colorectal_cancer/Colonoscopy_surveillance (Accessed 6 October 2013).
24. Faigel DO, Pike IM, Baron TH, Chak A, Cohen J, Deal SE, et al. Quality indicators for gastrointestinal endoscopic procedures: an introduction. American Journal of Gastroenterology 2006; 101(4): 866-872.
25. Chilton A, Rutter M (Eds). Quality assurance guidelines for colonoscopy. (Online) 2011. Available: http://www.cancerscreening.nhs.uk/bowel/publications/nhsbcsp06.pdf (Accessed 6 October 2013).
26. Leddin DJ, Enns R, Hilsden R, Plourde V, Rabeneck L, Sadowski DC, et al. Canadian Association of Gastroenterology position statement on screening individuals at average risk for developing colorectal cancer: 2010. Canadian Journal of Gastroenterology. 2010; 24(12): 705-714.
27. Agency for Healthcare Research and Quality. Systems to rate the strength of scientific evidence. Available: http://archive.ahrq.gov/clinic/epcsums/strengthsum.htm (Accessed 1 October 2013).
28. Kolber M, Szafran O, Suwal J, Diaz M. Outcomes of 1949 endoscopic procedures performed by a Canadian rural family physician. Canadian Family Physician 2009; 55(2): 170-175.
29. Kolber MR, Wong CKW, Fedorak RN, Rowe BH, Phys AP-ES. Prospective study of the quality of colonoscopies performed by primary care physicians: the Alberta Primary Care Endoscopy (APC-Endo) Study. Plos One 2013; 8(6).
30. Azzopardi J, DeWitt DE. Quality and safety issues in procedural rural practice: a prospective evaluation of current quality and safety guidelines in 3000 colonoscopies. Rural and Remote Health 12(3) (Online) 2012. Available: www.rrh.org.au (Accessed 6 October 2013).
31. Cotterill M, Gasparelli R, Kirby E. Colorectal cancer detection in a rural community. Development of a colonoscopy screening program. Canadian Family Physician 2005; 51: 1224-1228.
32. Newman RJ, Nichols DB, Cummings DM. Outpatient colonoscopy by rural family physicians. Annals of Family Medicine 2005; 3(2): 122-125.
33. Kirby E. Colonoscopy procedures at a small rural hospital. Canadian Journal of Rural Medicine 2004; 9(2): 89-93.
34. Edwards JK, Norris TE. Colonoscopy in rural communities: can family physicians perform the procedure with safe and efficacious results? Journal of the American Board of Family Practice 2004; 17(5): 353-358.
35. Pierzchajlo RP, Ackermann RJ, Vogel RL. Colonoscopy performed by a family physician. A case series of 751 procedures. Journal of Family Practice 1997; 44(5): 473-480.
36. Hopper W, Kyker KA, Rodney WM. Colonoscopy by a family physician: a 9-year experience of 1048 procedures. Journal of Family Practice 1996; 43(6): 561-566.
37. Rodney WM, Dabov G, Cronin C. Evolving colonoscopy skills in a rural family practice: the first 293 cases. Family Practice Research Journal 1993; 13(1): 43-52.
38. Godreau CJ. Office-based colonoscopy in a family practice. Family Practice Research Journal 1992; 12(3): 313-320.
39. Wilkins T, LeClair B, Smolkin M. Screening colonoscopies by primary care physicians: a meta-analysis. Annals of Family Medicine 2009; 7(2): 56-62.
40. Rex DK, Petrini JL, Baron TH, Chak A, Cohen J, Deal SE, et al. Quality indicators for colonoscopy. American Journal of Gastroenterology 2006; 101(4): 873-885.
41. Cotton PB, Connor P, McGee D, Jowell P, Nickl N, Schutz S, et al. Colonoscopy: practice variation among 69 hospital-based endoscopists. Gastrointestinal Endoscopy 2003; 57(3): 352-357.
42. Barclay RL, Vicari JJ, Doughty AS, Johanson JF, Greenlaw RL. Colonoscopic withdrawal times and adenoma detection during screening colonoscopy. New England Journal of Medicine 2006; 355(24): 2533-2541.
43. Chen SC, Rex DK. Endoscopist can be more powerful than age and male gender in predicting adenoma detection at colonoscopy. American Journal of Gastroenterology 2007; 102(4): 856-861.
44. Marshall JB. Technical proficiency of trainees performing colonoscopy - a learning-curve. Gastrointestinal Endoscopy 1995; 42(4): 287-291.
45. Rabeneck L, Paszat LF, Saskin R. Endoscopist specialty is associated with incident colorectal cancer after a negative colonoscopy. Clinical Gastroenterology and Hepatology 2010; 8(3): 275-279.
46. Nelson DB, McQuaid KR, Bond JH, Lieberman DA, Weiss DG, Johnston TK. Procedural success and complications of large-scale screening colonoscopy. Gastrointestinal Endoscopy 2002; 55(3): 307-314.
47. Dafnis G, Ekbom A, Pahlman L, Blomqvist P. Complications of diagnostic within a defined population and therapeutic colonoscopy in Sweden. Gastrointestinal Endoscopy 2001; 54(3): 302-309.
48. Putcha RV, Burdick JS. Management of iatrogenic perforation. Gastroenterology Clinics of North America 2003; 32(4): 1289-1309.
49. Meyer GS, Cheng EY, Elting J. Differences between generalists and specialists in characteristics of patients receiving gastrointestinal procedures. Journal of General Internal Medicine 2000; 15(3): 188-194.
_________________________
Appendix I: Individual studies abstract form?


