full article:
The recruitment of healthcare practitioners, including rehabilitation professionals, to practise in rural and/or remote (rural/remote) areas has been a well-documented challenge for many years1-4. Recent studies have continued to demonstrate an ongoing shortage of occupational therapists, physiotherapists, and speech-language pathologists in rural/remote areas. For example, while 25% of the Canadian population lives in a rural/remote area, only 8% of physiotherapists and 5% of occupational therapists practise in these areas5,6. In Ontario, there are 4.1 occupational therapists per 10 000 people in urban areas but only 0.3 per 10 000 people in rural/remote areas6. Similarly in Ontario, there are 6.0 physiotherapists per 10 000 people in urban areas but only 1.3 per 10 000 people in rural/remote areas5. Among Ontario speech-language pathologists, 95.6% practice in an urban area while only 4.4% practice in a rural area7,8.
Research, primarily amongst physicians, has demonstrated that exposure to rural learning increases the likelihood of choosing to practise in a rural area postgraduation9-11. With respect to the rehabilitation professions of occupational therapy (OT), physiotherapy (PT), speech-language pathology (SLP), and audiology, data have shown that rural recruitment appears to be positively influenced by length of time immersed in rural training12 as well as proximity to family, leisure/recreation access, and spousal influence13,14.
In response to the persistent challenge to recruit and retain rehabilitation professionals, the Northern Studies Stream (NSS) program was created in 1990 as an integral part of McMaster University's PT and OT new baccalaureate degree programs15. Part of the NSS program's mandate is to:
- increase students' awareness and knowledge of the determinants of health unique to northern and rural communities
- increase students' awareness of health concerns and practices unique to First Nations peoples
- provide students with the skills required for the unique practice of rural health care
- facilitate the recruitment and retention of rehabilitation professionals in Northern Ontario
- facilitate postgraduate professional networking and professional development among rehabilitation providers in Northwestern Ontario16,17.
Through the NSS program, McMaster OT/PT students have the opportunity to complete either a clinical placement or a complete academic semester (including clinical placement) in Northern Ontario, with the program based at the campus of the Northern Ontario School of Medicine (NOSM) at Lakehead University (LU) in Thunder Bay. In addition, the Rehabilitation Studies (RS) program, established in 1996 and also administered through NOSM, provides clinical education opportunities to PT, OT, SLP as well as audiology students from other universities in Ontario. In this context, 'academic semester' refers to classroom-based education on foundational knowledge relevant to OT or PT practice and is of 8 or 9 weeks duration. Class-based learning takes place on the campus of LU/NOSM in Thunder Bay, Ontario. Clinical placements consist of fieldwork rotations of 5 or 6 weeks duration and are completed anywhere in Northern Ontario.
The NSS and RS programs are administered jointly through NOSM with approximately 75% of all participating students enrolled through McMaster University (NSS) and the remaining 25% enrolled through other host universities (RS).
Previous work has demonstrated the positive relationship between participation in the NSS and recruitment to northern, rural, and remote practice sites12. Furthermore, when students participated in both the academic component and clinical placement this relationship was stronger12. In a previous cross-sectional study of Northern Ontario rehabilitation practitioners, 82% of individuals who reported having participated in the NSS program indicated that their participation in the program was either a 'somewhat' or 'extremely' important factor in their decision to move to Northern Ontario upon graduation14.
While this information provides some level of evidence to support the effectiveness of the NSS/RS programs, there exists no data on the actual number of NSS/RS graduates who choose to live and work in a rural or remote area. Indeed, from a program evaluation perspective, there is limited data examining the outcomes of the NSS/RS programs, both in terms of the recruitment rate of graduates, as well as to what extent participation in either the NSS/RS programs or other factors contributed to this decision.
The purpose of this study was to determine the rate of recruitment of NSS/RS graduates to rural/remote areas of practice by gathering information from previous students who participated in either the NSS or RS programs between 2002 and 2010. Secondary research questions included the identification and quantification of any other factors (eg personal, demographic, lifestyle) that contributed to an individual's likelihood to move to a remote or rural region for professional practice. Information regarding personal, demographic, and lifestyle factors was gathered from individuals who either did not choose to move to a rural/remote region upon graduation or those who did move to such a region and subsequently left.
Participants
The population of interest consisted of NSS and RS program participants who graduated between the years 2002 and 2010, inclusive (n=641). Information regarding previous participants in the NSS/RS programs was gathered via records retained within the NSS/RS programs as well as from the records at the School of Rehabilitation Science (SRS) at McMaster University. Limited availability of data for NSS/RS program participants between the years 1990 and 2001 precluded the inclusion of these individuals in the present study. For those individuals enrolled between 2002 and 2010, up-to-date contact information was then sought using databases maintained by NSS/RS and the McMaster SRS as well as searching regulatory college databases, social media (Facebook, LinkedIn), and through personal contacts of the study investigators. Of these 641 individuals, a current email address was obtained for 536 individuals (83.6%) who were subsequently invited to participate in the survey.
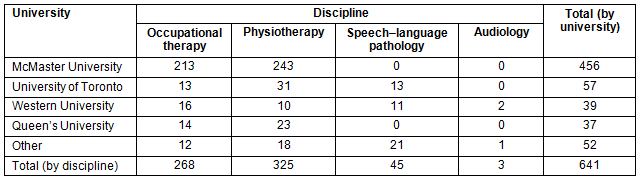
For additional information on NSS/RS program participants, see Table 1.
Table 1: Northern Studies Stream and Rehabilitation Studies program participants 2002-2010 by university and discipline (n=641)
Design overview
This study was retrospective in nature. Data were collected by means of an internet-hosted survey (SurveyMonkey) consisting of 48 questions; the actual number of questions for each participant varied depending on the responses given. The survey required approximately 15 minutes to complete and collected demographic information (eg profession, sex, year, and school of graduation), when the individual participated in the NSS/RS program, whether the individual moved to a rural or remote region after graduation and, if so, the duration of their stay. Individuals were asked to both identify and rate, using a five-point Likert scale (1='not at all important', 5 ='critically important') which factors (personal or professional) affected their decision to:
- move to a rural/remote region
- not move to a rural/remote region
- move to, but subsequently leave, a rural/remote region
- move to, and stay, in a rural/remote region.
Individuals were also asked if they were primarily raised in an area that could be considered rural, remote, both rural and remote or neither rural nor remote. A consensus definition for both 'rural' and 'remote' has historically proven challenging and various definitions for each exist18,19. For the purposes of this study, the following definitions were used:
- rural: community population density of less than 150 people per square kilometer20
- remote: restricted community access to health, education, and consumer services and/or geographical isolation.
Examples of representative communities that satisfied the definition of 'rural' were provided. Additionally, all communities within Northern Ontario were identified as satisfying the definition of 'remote'.
The survey link was distributed to 536 individuals in June 2011 and remained open for 4 weeks. Two reminder emails were sent during this 4-week period.
Ethics approval
Ethics approval for this study was obtained from the McMaster University Faculty of Health Sciences Research Ethics Board (project number 11-073).
Descriptive and frequency statistics were used to analyze demographic information as well as personal and professional factors affecting recruitment and retention. Tests for statistical significance of recruitment and retention factors were completed using χ² analysis or the Mann-Whitney U-test. A p value of less than 0.05 was considered to indicate statistical significance.
Due to sample size considerations, the categories of rural upbringing (n=62) and remote upbringing (n=37) were collapsed for data analysis. Therefore all results as they are described pertain to rural/remote reflect geographic locations that could be considered either rural, remote or both (n=82).
Data were analyzed using Statistical Package for the Social Sciences v18.0 (SPSS; http://www-01.ibm.com/software/analytics/spss/).
Respondent information
Of the 536 potential participants, 282 individuals responded to the survey; two of these individuals answered only a few demographic questions and discontinued the survey at that time. These two individuals were therefore excluded. Thus 280 survey respondents were included in the data analysis (response rate 52.2%).
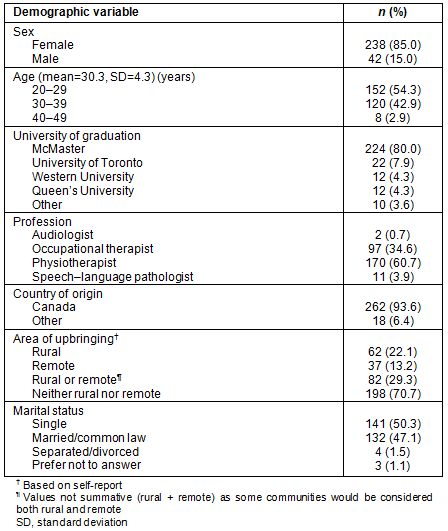
Demographic information of survey respondents (n=536) is included in Table 2.
Table 2: Demographic information about survey participants
Overall rate of recruitment to rural/remote area
The primary research question was to determine the rate of recruitment among NSS/RS program graduates to rural/remote areas of practice following graduation. Results of the survey indicated that overall, 33.9% (n=95) of survey respondents reported moving to a rural/remote region following graduation. Of those 95 individuals who moved to a rural/remote region, 65 (68.4%) reported moving to Northern Ontario while the remaining 30 individuals moved to a different rural/remote area either in Canada (n=29; 30.4%) or another country (n=1; 1.2%). Of those who did move to a rural/remote region upon graduation, a significant majority (n=78; 82.1%) did so immediately upon graduation from their university program.
Effect of rural/remote upbringing
Of the individuals who indicated they were raised in a rural/remote community (n=82), 53.7% moved to a rural/remote area after graduation. For those who were not raised in a rural/remote community (n=198), 25.8% moved to a rural/remote community after graduation. This difference was statistically significant (χ²(1)=20.1, p<0.001). Expressed as an odds ratio, individuals who indicated they moved to a rural/remote area after graduation were 3.3 times more likely to have been raised in a rural/remote area than those who did not move to a rural/remote region (95% confidence interval(CI)=1.95-5.72, p<0.001).
Effect of rural/remote academic training
Of the individuals who participated in the NSS academic semester and clinical component (n=126), 35.7% moved to a rural/remote area after graduation. For those NSS participants who did not participate in the academic component and only completed one or more clinical placements (n=98), 14.3% moved to a rural/remote community after graduation. This difference was statistically significant, indicating that individuals completing academic studies in addition to clinical components were 3.3 times more likely to move to a rural/remote area after graduation than those completing one or more clinical placements without the academic semester (95%CI=1.70-6.53, p<0.001).
Effect of number of rural/remote clinical placements
Amongst the entire survey group (participants of NSS academic plus clinical, NSS clinical-only, and RS) individuals who completed a greater number of clinical placements in Northern Ontario were more likely to move to a rural/remote community after graduation. Across the entire survey group, 27.4% of individuals who completed only one clinical placement in Northwestern Ontario chose to move to a rural/remote area following graduation. For those individuals who completed two or more clinical placements, the rate of recruitment was 64.0% (χ²(1)=24.6, p<0.001; Fig1).
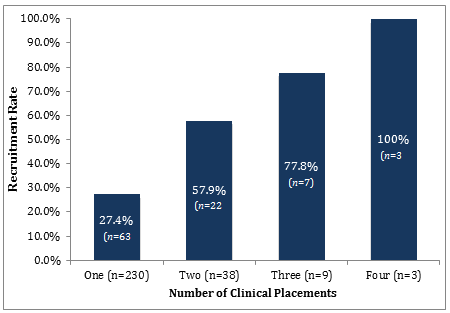
Figure 1: Recruitment rate by number of clinical placements.
To examine whether the improved recruitment rate with increasing number of clinical placements was confounded by rural/remote upbringing (ie individuals originally from a rural/remote area may have been more likely to complete more than one clinical placement), additional analyses were completed to control for location of upbringing. These results indicated that:
- among those originally from a rural/remote area, 41.8% of individuals who completed only one clinical placement moved to a rural/remote area following graduation; for those originally from a rural/remote area who completed more than one clinical placement, the recruitment rate was 77.8% (χ²(1)=9.4, p=0.002)
- among those not originally from a rural/remote area, 22.9% of individuals who completed only one clinical placement moved to a rural/remote area following graduation, for those individuals not from a rural/remote area who completed more than one clinical placement, the recruitment rate was 47.8% (χ²(1)=6.6, p=0.01; Fig2).
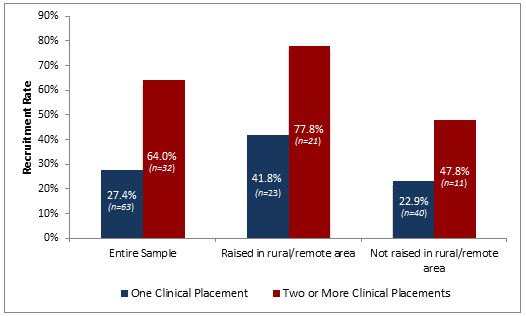
Figure 2: Recruitment rate by number of clinical placements (categorized by area of upbringing).
Thus, the data indicates that both rural/remote upbringing and increasing numbers of clinical placements in rural/remote settings during educational experiences are both positively and independently associated with an individual's decision to practise in a rural/remote location after graduation.
Personal and/or professional factors influencing recruitment
Personal and professional factors impacting decision to move (or not move) to a rural/remote area upon graduation are presented in Tables 3 and 4, respectively.
For those who did move to a rural/remote area upon graduation, 'job availability' and 'lifestyle options' were factors rated highly as part of their decision to do so, both by those originally from a rural/remote area and those who were not. Subgroup analysis revealed that for those individuals originally from a rural/remote area (n=44), rural/remote origin was the highest rated decision factor in their decision to move to a rural/remote area after graduation (mean Likert score 4.1/5.0, standard deviation(SD)=0.93).
While an attraction to the unique employment inherent in a rural/remote practice area and a preference to live in small communities were both rated more highly by individuals originally from a rural/remote area compared to those individuals who were not, the difference between groups for both of these factors was not statistically significant (data not shown).
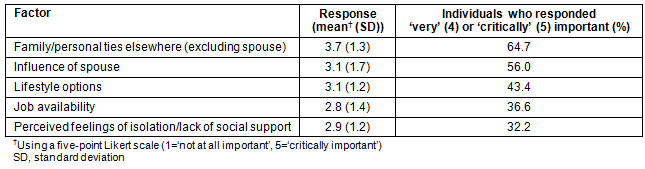
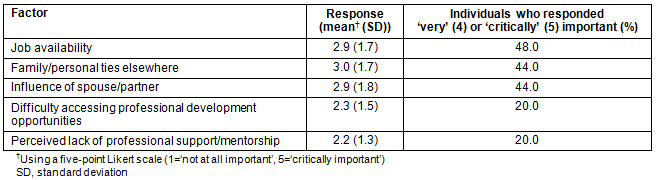
For those who did not move to a rural/remote area following graduation, 'family/personal ties elsewhere' was the highest rated factor. In a subgroup analysis (data not shown), influence of spouse/partner as a decision criterion for not moving to a rural/remote area upon graduation was highly rated by both those originally from a rural/remote area and those who were not.
Table 3: Reasons for moving to a rural/remote area (n=94)
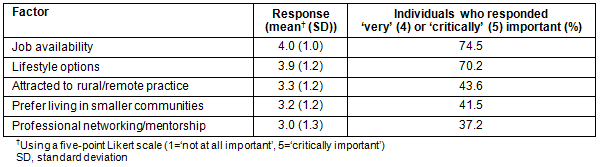
Table 4: Reasons for not moving to a rural/remote area (n=184)
Retention
Information pertaining to personal or professional factors impacting the decision to remain in a rural/remote area upon graduation is presented in Table 5. Personal and professional factors that had an impact upon individuals' decisions to leave a rural/remote area are summarized in Table 6.
Amongst those who continued to live in a rural/remote area, 'job satisfaction', 'lifestyle options' and 'prefer living in smaller communities' were factors rated highly both by individuals originally from a rural/remote area and those who were not, with no statistically significant differences noted between groups (data not shown).
In a subgroup analysis of those individuals originally from a rural or remote area, such individuals did perceive their rural upbringing as an important factor in retention, with it being the second highest rated factor in their decision to continue living in such an area (mean Likert score 4.0/5.0, SD=1.2, n=33).
In a subgroup analysis, amongst those individuals who moved to, but subsequently moved away from, a rural/remote area, there were no statistically significant differences in factors impacting this decision between those originally from a rural/remote area and those who were not (data not shown).
Of the individuals who indicated they were raised in a rural/remote community and who moved to such a community following program graduation (n=44), 75.0% indicated that they continued to live in a rural/remote area at the time of survey completion. For those who were not raised in a rural/remote community and who did move to a rural/remote community following program graduation (n=50), 72.0% indicated that they continued to live in a rural/remote area at the time of survey completion. This 3% difference was not statistically significant (χ²(1)=0.108, p=0.743).
Among those respondents currently living in Northwestern Ontario (the region serviced by the NSS program), 83% of respondents indicated that networking opportunities (such as the workshops delivered in part by the NSS program) are 'moderately', 'very' or 'critically' important factors in their decision to continue living and working in the region.
Of the 25 people who moved to a rural/remote region after graduation and then subsequently moved away, the average length of stay in the region was 1.4 years (SD=0.7) with 64% of these individuals remaining for 1 year or less. Of the 69 individuals who continued to reside in a rural/remote area, 26% reported definite plans to move away within the next 10 years, while 44.8% reported they were unsure if they would move away or remain over the next 10 years. Twenty nine percent of survey respondents currently residing in a rural/remote area reported no plans to move away during any timeframe.
Table 5: Reasons for staying in a rural/remote area (n=69)
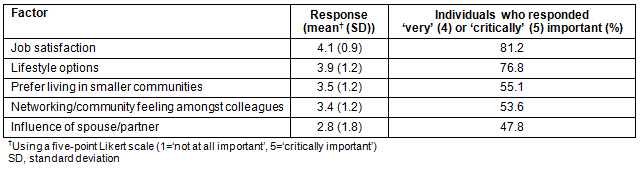
Table 6: Reasons for leaving a rural/remote area (n=25)
Discussion
Recruitment
With an overall recruitment rate of 33.9%, the NSS and RS programs appear to be adequately meeting their recruitment mandate. Consistent with previous literature in the healthcare field10,11,21,22, this study found that rural/remote upbringing was a strong and consistent factor influencing both recruitment and retention to underserviced areas.
Irrespective of rural/remote upbringing status, factors such as job availability/job satisfaction, lifestyle options, and a preference for living in a smaller community were important factors for both recruitment and retention.
As identified in odds ratio analysis, the relationship between rural/remote upbringing and moving to a rural/remote area following graduation was particularly strong; this was corroborated via the subgroup analysis of self-identified factors amongst those originally raised in a rural/remote area, which demonstrated that rural/remote upbringing was the most important personal or professional factor in the decision to move to a rural/remote area following graduation.
Individuals not originally from a rural/remote area placed greater emphasis than their rural/remote-raised colleagues on professional networking opportunities as an important retention factor. Interestingly, individuals not originally from a rural/remote area cited spousal ties as a moderately important retention factor (mean Likert score 2.1/5.0, SD=0.9, n=36), suggesting that such relationships were formed after moving to the region.
It is interesting to note that Likert scale ratings for the factors affecting an individual's decision to move away from a rural/remote area were generally lower than the ratings for factors affecting one's decision to move to, not move to, or to stay in the region. This incongruity is evidenced by both the lower response means and the smaller percentage of individuals who responded 'very' or 'critically' important to each factor affecting their decision to move away from a rural/remote area. It is also possible that there were other factors, not specifically identified in the survey, of greater importance in an individual's decision to move away from a rural/remote area.
Previous research has demonstrated that exposure to rural curriculum has a positive impact on intention to practise in a rural area2,23. In this study, recruitment to rural/remote areas increased both with participation in the NSS academic semester and with the total number of clinical placements completed by the student in rural/remote areas. The lengths of the academic semester are 8 and 9 weeks for PT and OT, respectively. Clinical placement length varies, but is almost always either 6 or 8 weeks duration for all NSS and RS learners (OT, PT, SLP, and audiology). Thus, if the total number of clinical placements is used as a proxy for the length of time immersed in the rural/remote practice setting during the student's education, the finding that higher numbers of clinical placements was also associated with an increased likelihood to move to a rural/remote region upon graduation provides some evidence to support the value of increased duration of rural training.
Indeed, longer immersion in rural training provides students with greater exposure to educational, personal, and professional variables such as professional networking, personal socialization, employment opportunities, and lifestyle options. Ultimately, it is likely that an individual's decision to move to a rural/remote area upon graduation is based on multiple factors and not any single factor in particular.
Retention
While the data for recruitment is encouraging, retention of rehabilitation providers in rural/remote areas continues to be a challenge. Of the 94 individuals who moved to a rural/remote area after graduation, only 73.4% continued to live in the area at the time of survey completion. Of those who moved away, the average length of stay was less than 2 years. An oft-cited reason for moving away was 'job availability'; however, it is unknown whether this refers to a lack of employment opportunities in rural/remote areas, or instead to the prospect of more appealing jobs elsewhere.
Retention was also adversely affected by family/spousal influence, two factors that the NSS and RS programs have little to no control over. Two additional reasons for relocation away from a rural/remote practice area were professional isolation and difficulty accessing professional development opportunities, which are both consistent with previous research2,24. Although the NSS and RS programs have funding allocated for professional development and networking opportunities targeted to practising rehabilitation professionals, these funds are limited when compared to funding allocated to the entry-to-practice initiatives within NSS and RS. The extremely large geographic size of the Northern Ontario region (larger than France) also presents significant challenges to provide professional development and networking opportunities in an effective yet cost-efficient manner.
Study limitations and benefits
A key limitation of this study includes the possibility of recall bias due to the study's retrospective nature.
In addition, respondents who participated in the NSS/RS programs and subsequently moved to a rural/remote region after graduation may have felt a greater imperative to respond to the survey, thereby increasing the recruitment percentage relative to the potential survey respondents. However, it is noteworthy that the 33.9% recruitment rate to a rural/remote area amongst NSS/RS program graduates far exceeds the percentage of physiotherapists (8.3%), occupational therapists (5.7%), and speech-language pathologists (4.4%) currently working in these areas in Canada. Additionally, if an assumption is made that of the 256 individuals who did not respond to the survey, none chose to move to a rural/remote area after graduation, the overall recruitment rate would still be 17.7% (95/536), a value two to four times higher than the current percentage of occupational therapists, physiotherapists and speech-language pathologists currently working in Canadian rural/remote areas.
Another study limitation is the lack of clarity about whether the higher recruitment rate observed amongst individuals who completed the NSS academic semester and clinical placement compared to clinical placement alone was due to the academic curriculum itself (focusing on rural/remote practice and First Nations culture), the greater length of time spent by the student immersed in a rural/remote setting during their education, or a combination.
As previously mentioned, for statistical analysis purposes the two groups of individuals raised in a rural area or a remote area were collapsed into one group, 'rural/remote'. While allowing for a greater ability to detect statistically significant differences between the rural/remote group and individuals not primarily raised in either a rural or remote area, this precludes the ability to detect whether the results reported may have differed between individuals primarily raised in a rural area and those primarily raised in a remote area. However, it is worthy to note that of the 99 individuals who reported being raised in either a rural or remote area, for 82 of these individuals (82.8%), their home community would have been considered both rural and remote by the definitions used in this study.
Although the study conclusions use the total number of clinical placements completed as a proxy for overall length of rural/remote training, the authors concede that this represents a possible limitation of the study: while clinical placement length is consistent across professions and semesters of study for NSS and RS, the study data do not establish a definitive link between length of immersion in rural/remote education and the study findings.
Strengths of this study include the 8-year time frame for follow-up, allowing for a potential pool of over 500 individuals, of which more than 50% responded to the survey. Additionally, this study collected information from individuals who moved to, and did not move to, a rural/remote area following graduation, as well as those who moved to, and subsequently left, a rural/remote area. This allowed for more robust data gathering from a wide range of individuals.
Part of the mandate of the NSS and RS programs is to increase the recruitment and retention of rehabilitation professionals to rural/remote areas of practice, particularly Northern Ontario. The results of this study support that both the NSS and RS programs have been successful in achieving a high level of recruitment of program graduates to such areas.
As identified previously, the NSS and RS programs provide professional supports for rehabilitation providers in Northern Ontario. This occurs, in part, in the form of workshops, mentorship, and networking opportunities. Thus, while such initiatives do target some of the factors identified in this study as negatively affecting retention (eg professional isolation and lack of professional development opportunities), it is apparent that retention of rehabilitation providers in rural/remote areas continues to be a challenge. This underscores a need to further enhance the initiatives already in place, as well as potentially addressing other identified issues such as job availability and spousal/family influences.
In light of the strong correlation between rural/remote upbringing and decision to practise in a rural/remote area upon program graduation, these findings raise the question of whether university rehabilitation programs with particular interest in rural/remote curricula should preferentially admit individuals with rural/remote origins. Other strategies that could be utilized by educational programs to enhance intention to practise in a rural/remote area upon graduation include curricula that address rural/remote practice experiences and competencies, as well as maximizing time spent in rural/remote practice settings during training.
In consideration of ongoing retention challenges, government agencies, employers, professional associations, and educational institutions should consider implementing new strategies or augmenting current initiatives to enhance job satisfaction as well as professional networking, mentorship, and continuing education in order to improve the retention of rehabilitation providers within rural/remote areas.
Acknowledgements
The authors wish to thank Ms Marie Parkkari and Ms Bronwen Thomas for their assistance with database generation and research literature support as well as Ms Esmé French, Ms Denise Taylor and Ms Kirsti Reinikka for their editorial contributions to this manuscript.
Funding for this study was granted through the McMaster University School of Rehabilitation Science's Education Research Grant.
References
1. Ng E, Wilkins R, Pole J, Adams OB. How far to the nearest physician? Rural and Small Town Canada Analysis Bulletin 1(5): 1-7. (Online) 1999. Available: http://www.publications.gc.ca/Collection/Statcan/21-006-X/21-006-XIE1998005.pdf (Accessed 14 August 2011).
2. Beggs CE, Noh S. Retention factors for physiotherapists in an underserviced area: an experience in northern Ontario. Physiotherapy Canada 1991; 43(2): 15-25.
3. Polatajko H, Quintyn M. Factors affecting occupational therapy job site selection in underserviced areas. Canadian Journal of Occupational Therapy 1986; 53(15): 1-157.
4. Romanow R. Building on values: the future of health care in Canada. (Online) 2002; 162-163. Available: http://publications.gc.ca/collections/Collection/CP32-85-2002E.pdf (Accessed 14 December 2013).
5. Canadian Institute for Health Information. Physiotherapists in Canada, 2008. (Online) 2009. Available: https://secure.cihi.ca/free_products/PT_report_2008_en.pdf (Accessed 27 March 2010).
6. Canadian Institute for Health Information. Occupational therapists in Canada, 2008. (Online) 2009. Available: https://secure.cihi.ca/free_products/OT_Report_EN_Revised_Feb09_2010_web.pdf (Accessed 27 March 2010).
7. Canadian Institute for Health Information. Speech-language pathologists. (Online) 2010. Available: http://www.cihi.ca/cihi-ext-portal/internet/en/document/spending+and+health+workforce/workforce/other+providers/hpdb_slpat#demTre (Accessed 28 March 2011).
8. College of Audiologists and Speech-Language Pathologists of Ontario. College of Audiologists and Speech-Language Pathologists of Ontario. CASLPO public register of members. (Online) 2013. Available: https://members.caslpo.com/public/register.htm (Accessed 4 March 2013).
9. McCready W, Jamieson J, Tran M, Berry S. The first 25 years of the Northwestern Ontario Medical Programme. Canadian Journal of Rural Medicine 2004; 9(2): 94-100.
10. Matsumoto M, Okayama M, Inoue K, Kajii E. Factors associated with rural doctors' intention to continue a rural career: a survey of 3072 doctors in Japan. Australian Journal of Rural Health 2005; 13(4): 219-225.
11. Daniels ZM, Vanleit BJ, Skipper BJ, Sanders ML, Rhyne RL. Factors in recruiting and retaining health professionals for rural practice. Journal of Rural Health 2007; 23(1): 62-71.
12. Cano J, Foster-Seargeant E. Educational preparation for rural and remote practice: the Northern Studies Stream. In P. Solomon, S. Baptiste (Eds). Innovations in rehabilitation sciences education: preparing leaders for the future. Heidelberg, Germany: Springer-Verlag, 2005; 175-190.
13. Solomon P, Salvatori P, Berry S. Recruitment factors by therapists in Northwestern Ontario. Canadian Journal of Rural Medicine 2001; 17(3): 278-285.
14. Winn CS, Chisholm BA, Hummelbrunner JA. Factors affecting recruitment and retention of rehabilitation practitioners in northern Ontario. Rural and Remote Health 14: 2619. (Online) 2014. Available: www.rrh.org.au (Accessed 30 April 2014).
15. Salvatori P, Berry S, Solomon P. Exploring professional development opportunities in Northwestern Ontario: a profile of rehabilitation health professionals. In Minore B, Hartviksen C (Eds). Redressing the imbalance: health human resources in rural and northern communities. Proceedings from a conference hosted by the Northern Health Human Resources Research Unit, Thunder Bay, Ontario, October, 1993. Thunder Bay, ON: Northern Health Human Resources Research Unit, 1995; 275-287.
16. Perkins J, Berry S, Tryssenaar J. The Northern Studies Stream: educating health professionals in remote regions. Arctic Medical Research 1994; 53(Suppl2): 118-120.
17. McMaster University. PT program information. (Online) 2008. Available: http://srs-mcmaster.ca/pt-program-information (Accessed 15 October 2013).
18. Deaville JA, Jones LM. Health-care challenges in rural areas: physical and sociocultural barriers. Professional Nurse 2003; 18(5): 262-264.
19. Ministerial Advisory Council on Rural Health. Rural health in rural hands: strategic directions for rural, remote, northern and aboriginal communities. (Online) 2002. Available: http://www.srpc.ca/PDF/rural_hands.pdf (Accessed 18 June 2011).
20. Du Plessis V, Beshiri R, Bollman RD, Clemenson H. Definitions of rural. Rural and Small Town Canada Analysis Bulletin 3(3). (Online) 2001. Available: http://www.statcan.gc.ca/pub/21-006-x/21-006-x2001003-eng.pdf (Accessed 14 August 2011).
21. Chan B, Degani N, Crichton T, et al. Factors influencing family physicians to enter rural practice: does rural or urban background make a difference? Canadian Family Physician 2005; 51: 1247-1252.
22. Richards HM, Farmer J, Selvaraj S. Sustaining the rural primary healthcare workforce: survey of healthcare professionals in the Scottish highlands. Rural Remote Health 5(1): 365. (Online) 2005. Available: www.rrh.org.au (Accessed 30 April 2014).
23. Critchley J, DeWitt DE, Khan MA, Liaw S. A required rural health module increases students' interest in rural health careers. Rural Remote Health 7(2): 688. (Online) 2007. Available: www.rrh.org.au (Accessed 30 April 2014).
24. Williams E, D'Amore W, McMeeken J. Physiotherapy in rural and regional Australia. Australian Journal of Rural Health 2007; 15(6): 380-386.