Obesity has become an epidemic in the USA and throughout the world1-3. Obesity is associated with increased incidence of many chronic conditions, including cardiovascular disease, type 2 diabetes mellitus, dyslipidemia, osteoarthritis, and cancers4-7. Costs associated with obesity in the USA are estimated to exceed $147 billion per year8. Obesity is one of the biggest challenges facing public health in the 21st century. Physical inactivity that includes lack of leisure-time physical activity or a sedentary lifestyle, and an unhealthy diet that is high in calories, has low servings of fruits and vegetables, high servings of sugar-sweetened beverages and high servings of meat, and includes skipping breakfast, are the important modifiable behavioral risk factors for obesity9-15.
Prevalence of obesity may differ by urban or rural residence because of differences in cultural, socioeconomic, and environmental conditions. In many developing countries, such as India16 and China17, urbanization and its associated lifestyle changes, such as increased sedentary behavior and a Westernized high-fat diet, are considered important risk factors for obesity. In contrast, studies from developed countries such as the USA18-20, Canada21,22, and Sweden23 found a higher prevalence of obesity in rural areas. This has been attributed to a built-in environment that offers limited opportunities for physical activity24,25, access to healthy diet26,27, and access to medical services28.
In the USA, where approximately 20% of the population lives in rural areas, published studies have consistently reported a higher prevalence of obesity among rural residents18-20. Previous studies have mainly examined the differences in sociodemographic characteristics of residents and have limited ability to explore the role of individual obesity-related behaviors such as diet and physical activity between these two populations. The objectives of the present study were to compare the differences in the obesity-related health behaviors across rural and urban populations in the USA, and further examine how these differences account for the observed disparity (if any) in the prevalence of obesity. Better understanding of rural-urban differences in obesity-related behaviors and their contribution to rural-urban differences in obesity will be beneficial to the design of evidence-based programs and policies targeting rural populations in the USA.
Data source
Data were obtained from the 1999-2006 continuous National Health and Nutrition Examination Survey (NHANES), an ongoing, nationally representative study conducted by the National Center for Health Statistics that includes both an interview and a follow-up physical examination. Multiple years of NHANES observations were combined to allow an adequate number of observations from rural residents. The response rate for years 1999-2006 for home interviews was 81%, and 95% of respondents interviewed at home had a follow-up examination at a mobile examination center (MEC). The study methods of NHANES are described in detail on the study website29. The 1999-2006 NHANES interviewed 20 294 adults who were ³20 years. For obesity prevalence estimates, data were restricted to 17 302 participants aged ³20 years, after excluding 1323 participants who were not interviewed at MEC follow-up visits, 1097 pregnant subjects, and 572 participants with missing values for weight and height measurements. For analyses addressing obesity-related behavioral factors, data were further restricted to 14 039 participants, after additional exclusions for respondents with unreliable dietary recall (837), those requiring special equipment such as wheelchair and cane (1365), and those with missing values for main covariates (1061).
Measures
Urban and rural residence: Urban and rural residence were defined using the Rural-Urban Commuting Area (RUCA) definition developed by the University of Washington's Rural Health Research Center and the Economic Research Service at the US Department of Agriculture30. RUCA categories are based on the size of settlements and towns as delineated by the Census Bureau and the functional relationships between places as measured by track-level work-commuting data30. Urban areas were defined as RUCA codes between 1 and 3, and rural areas as RUCA codes between 4 and 1031. This protected Census track information was accessed through the Research Data Center at the National Center for Health Statistics.
Measure of obesity: At MEC visits, trained examiners took height and weight measurements from each subject. This information was used to calculate body mass index (BMI), by dividing weight in kilograms by height in meters squared (kg/m2). Consistent with the definition of major health organizations, such as the US Department of Health and Human Services and the World Health Organization, obesity was defined as BMI³30 kg/m232.
Sedentary behavior and physical activity: Sedentary behavior and physical activity levels (assessed from self-reported and validated questions) were categorized in two ways - total daily TV/computer screen time (<2, ≥2 to <4, ≥4 hours/day33) and leisure-time physical activity levels - as per the four categories for physical activity recommended by the American College of Sports Medicine: (1) no leisure-time physical activity levels; (2) less than minimum goal (<450 metabolic equivalent (MET) min/week); (3) meeting the minimum goal (450 to <750 MET min/week); (4) overachievers (>750 MET min/week)34.
Diet: NHANES collected diet data through a one-day, 24 hour dietary recall interview. This information was used to calculate the following dietary variables to assess dietary intake and behavior: breakfast consumption ('have breakfast' vs 'skip breakfast'), sugar-sweetened beverage intake (<230, 230-680, >700 mL/day), fruit intake (0, <1, 1-2, >2 cups/day), vegetable intake (<1, 1-3, >3 cups/day), dairy product intake (<1, 1-2, 2-3, >3 cups/day), meat and bean consumption (<2, 2-4, >4 servings/day), daily total energy (continuous), and fiber intake (continuous). Breakfast skipping was defined as no energy intake before 10.30 hours.
Other control variables: Number of covariates was considered as possible confounders for the association between residence and obesity. These included sociodemographic variables such as age, sex, race/ethnicity, household's poverty status, education level, region of residence, self-reported health status, health insurance, and marital status. The racial/ethnic categories were Mexican-American, non-Hispanic Black (hereafter, Black), non-Hispanic White (hereafter, White), and other racial/ethnic groups. Economic status was divided into five categories: <100%, 100-199%, 200-399%, 400% federal poverty level or above and a proxy category for missing values.
Statistical methods
Statistical Analysis Software v9.3 (SAS Institute, Cary, NC) and SUDAAN v10 (Research Triangle Park, NC) were used to perform all statistical analyses, incorporating sample weights and adjusting for cluster and strata of the complex sample design in NHANES. The prevalence rates of obesity, and obesity-related risk factors (physical activity, sedentary behaviors, and diet) for urban and rural residents were calculated. Age-, gender- and race-specific prevalence of obesity were also calculated by residence. The χ2 test was used to assess whether urban and rural differences were statistically significant.
Multiple logistic regression analysis was used to evaluate the independent association between obesity and residence after adjusting for differences in population characteristics. First, crude odds ratios (OR) for obesity were calculated by residence, and then by obesity-related behaviors, including physical activity levels, screen time, and diet, without adjusting for any covariates. Then, an adjusted model was run, which included residence, obesity-related behaviors, and all above-mentioned other control variables, to examine the independence association between residence and obesity. Since the interaction term between gender and urban-rural residence was not significant at the 0.05 level, the analysis was not stratified by gender.
Ethics approval
The study was approved by the Office of Research Compliance at the University of South Carolina (HSA5892). All information collected from participants by NHANES is kept confidential. Details of informed consent and data confidentiality can be found on the study website29.
Sociodemographic characteristics and obesity-related behaviors of the sample population are summarized in Table 1 and Table 2, respectively. In comparison to urban residents, rural residents were more likely to be older, White, and married or have a partner, and had lower self-perceived health status, household income, and educational attainment (Table 1). Rural residents were more likely to report no physical activity at all, and were also less likely to meet recommended goals for leisure-time physical activity (Table 2). Scant differences were also found for daily screen time, with a higher percentage of rural residents reporting more than 4 hours of daily screen time. In terms of diet, rural residents had higher intakes of sweetened beverages, and lower intakes of fruit and total daily dietary fiber. Rural residents were also more likely to skip breakfast (Table 2).
Approximately 31.6% of the sample population was obese. The prevalence of obesity was higher among rural than among urban adults (35.6% vs 30.4%, p<0.01). The prevalence of obesity was higher for rural than urban men (37.7% vs 32.5%, p<0.01), and also higher for rural than urban women (33.4% vs 28.2%, p<0.01) (Table 3). Among rural residents, the prevalence of obesity was the highest among Black adults (49.6%), and lowest among White adults (34.2%). Within each racial subgroup, rural residents had a significantly higher prevalence of obesity than urban residents (Table 3).
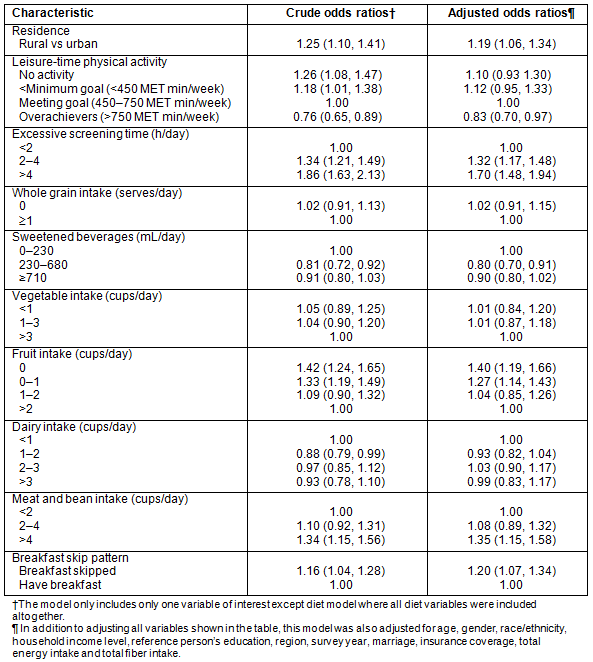
In crude analysis (Table 4), rural residents had 1.25 times higher odds of being obese than urban residents (95% confidence interval [CI]: 1.10, 1.41). On examining the crude association of obesity-related behavioral risk factors on obesity, it can be seen that lower levels of physical activity, excessive screen time, lower fruit consumption, higher meat and bean intake, and skipped breakfast patterns were associated with increased obesity risk. In adjusted analysis, where residence, sociodemographic variables and all obesity-related behaviors (physical activity, sedentary behavior, and diet) were simultaneously adjusted for, rural residents still had higher odds for obesity (OR 1.19, 95% CI 1.06-1.34). Among the sociodemographic variables included in the adjusted analysis, male gender, being in age group 40-59 years, and Black race/ethnicity were associated with increased odds of obesity, and never being married and having no insurance coverage were associated with reduced odds of obesity (data not shown). Among obesity-related behaviors in this model, not meeting physical activity recommendations, high screen time, low fruit consumption, high meat and bean intake, and skipping breakfast were associated with increased odds of obesity.
Table 1: Sample characteristics of US adults, by urban/rural residence, National Health and Nutrition Examination Survey 1999-2006
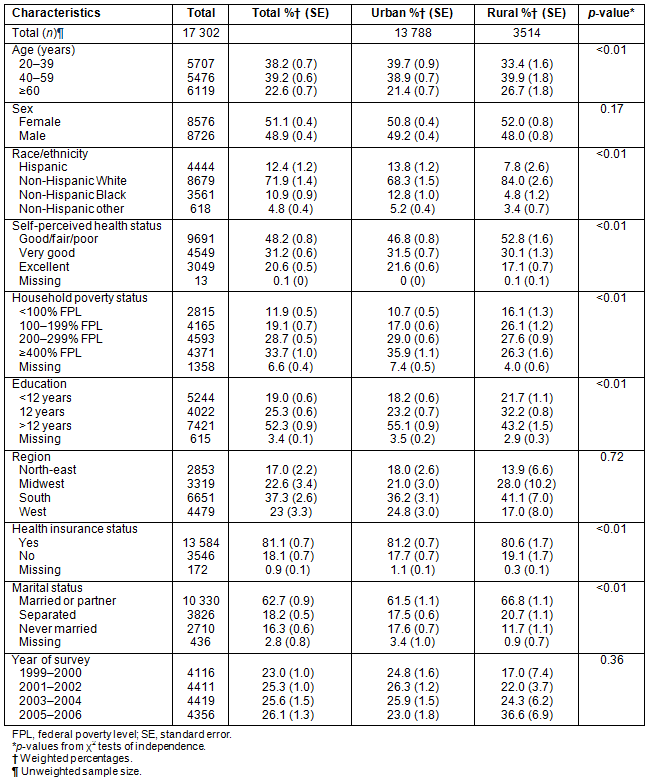
Table 2: Obesity-related behaviors among US adults by residence, National Health and Nutrition Examination Survey 1999-2006 (n=14 039)
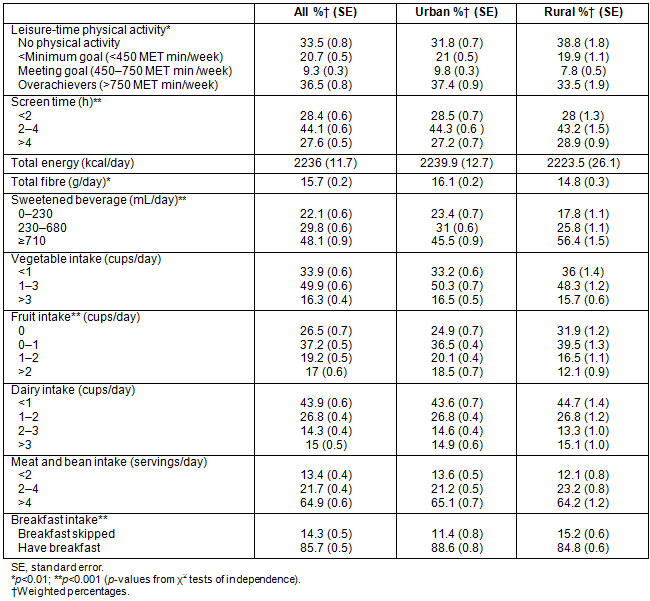
Table 3: Proportion of US adults who were obese by residence, age, gender, and race 1999-2006 (n=17 302)
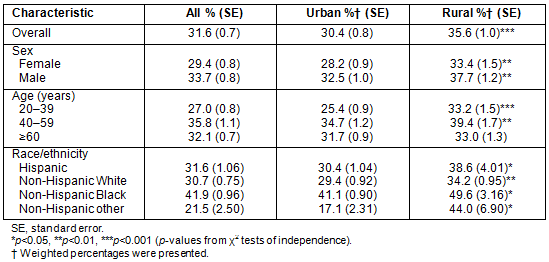
Table 4: Residence and obesity-related behaviors as risk factors for obesity among US adults, National Health and Nutrition Examination Survey 1999-2006 (n=14 039)
Discussion
This study advances previous research findings by providing a detailed description of obesity and obesity-related health behaviors (leisure-time physical activity, screen time, and dietary intake) in rural USA by using a nationally representative data set. Previous research into these topics provided limited information on obesity-related health behaviors among rural populations18-20. A better understanding of the modifiable determinants of obesity among high-risk populations such as rural Americans is important for the design of effective public health strategies to prevent obesity and associated comorbidities.
This research confirms findings from previous epidemiological studies that adults living in rural areas across the USA have a higher prevalence of obesity than urban residents do. In addition, findings from this study also indicate that rural residents are more likely to be physically inactive and have unhealthy diets in many aspects when compared to urban residents. To promote and maintain good health, the American College of Sports Medicine recommends at least 150 minutes per week of moderate exercise or 60 minutes per week of vigorous exercise (or a combination of moderate and vigorous activity34). The results from this study indicate that in comparison to their urban counterparts, higher proportions of rural residents do not meet recommended levels of leisure-time physical activity. Along with being physically active, having a healthy and balanced diet is an important lifestyle behavior that can help an individual manage healthy body weight. The results from this study suggest rural residents have a higher intake of sweetened beverages, a lower intake of fruits, and a lower intake of daily dietary fiber, and were more likely to skip breakfast. All these dietary behaviors have been well documented in the literature as 'pro-obesogenic'10,12-15.
When compared to their urban counterparts, rural populations have a higher representation of less-educated and low-income residents. Earlier studies have documented associations between obesity and low socioeconomic status35,36. Multiple mechanisms have been suggested, including the relationship of low education levels, low income, and other markers of low socioeconomic status to lower levels of recreational physical activity, unhealthy diet, and certain psychosocial behaviors leading to increased risk for obesity37. Thus, lower socioeconomic status may partly explain the higher prevalence of obesogenic behaviors among rural residents37.
This study has several noteworthy strengths. First, previous studies on rural-urban obesity disparities provided either none18 or limited information19,20 for the differences in obesity-related behaviors among these two populations. Patterson et al19 included physical activity (inactive vs active) and Befort et al20 considered physical activity (inactive vs active) and dietary variables (daily energy intake, and percent kilocalories from fat) in their analyses. However, their measurements on obesity-related behaviors were not as comprehensive as in this study, thus explaining none or little significant differences in the rural-urban context. Second, the use of measured height and weight in this study helps to avoid misclassification of the outcome when compared to the use of self-reported height and weight in many previous studies. To the authors' knowledge, with the exception of one recent study20, all previous studies on rural-urban obesity disparities have used self-reported height and weight to calculate BMI and classify obesity status, which may underestimate obesity prevalence38. Third, this study used ZIP code-approximated RUCA codes to have a precise definition of rural residence, which is more precise than the definition of rurality based on county of residence used in the previous studies18-20, as the large geographical area of counties often obscures intracounty differences30.
This study is limited by its reliance on self-reported leisure-time physical activity as the quantitative measure of physical activity. Work-related activity, household activity, and transportation-related physical activity were not considered, which could be relevant considering the differences in the working environment of urban and rural residents. However, the agriculture, forestry, and fishing sectors constitute only about 6% of employment in high-density rural areas and about 12% of employment in low-density rural areas in the USA39. Thus, it is unlikely that the working environment in rural areas is conducive to a more physically active lifestyle. In the adjusted analysis, even after including all the sociodemographic factors, obesity-related behaviors and other covariates, rural residence is still associated with higher odds of obesity than urban residence. This could suggest either other unmeasured factors are at work, or possible measurement errors in the study's covariates. Future studies may consider including variables such as stress levels40, sleep time40, social support41, and access to primary care services, factors that are known to affect an individual's weight and overall health through different mechanisms and can be important when considering socioeconomic differences in urban-rural populations.
Obesity is an ever-increasing problem in the USA and across the globe. The association between obesity and rural residence in industrialized countries such as the USA is evident and robust. A study using more recent data (2005-2008) reported that obesity prevalence is as high as 40% in rural areas in the USA20. Thus, it is important to understand that obesity reduction is much more challenging in rural areas, where both cultural and environmental factors contribute to a higher prevalence. Emphasis must be given to developing evidence-based programs that can be successful in diverse rural environments, which can range from the forests of New England to the deserts of Nevada. Strategies keyed to an urban environment, such as convenient access to public transportation or increases in the availability of paved sidewalks42, are irrelevant in rural USA. Examples of obesity interventions that have been effective in rural areas are a community-based health promotion program that relied on community group discussions, educational presentations, health fairs and screenings43, and continued medical education for rural physicians to integrate physical activity and diet counseling in their clinical practice44.
The built environment in rural USA plays a role in promoting unhealthy behaviors conducive to obesity. For example, rural residents have limited access to healthy food choices45,46, and the limited recreational resources such as parks and exercise facilities is an impediment to physical activity47,48. Additional research is needed to identify low-cost, sustainable changes that can improve built environments in rural areas. Techniques that empower rural communities to increase the availability of quality food markets and recreational resources need to be identified and disseminated.
The national epidemic of obesity is particularly acute in rural USA and demands prompt public health action. The disparities in rural versus urban health issues including obesity are complex and based on sociodemographic, environmental, and lifestyle differences. Future research, community-based interventions and structural changes are needed to get rural populations moving towards a healthier future.
References
1. Wang Y, Beydoun MA. The obesity epidemic in the United States - gender, age, socioeconomic, racial/ethnic, and geographic characteristics: a systematic review and meta-regression analysis. Epidemiologic Reviews 2007; 29: 6-28.
2. Kelly T, Yang W, Chen C, Reynolds K, He J. Global burden of obesity in 2005 and projections to 2030. International Journal of Obesity 2008; 32(9): 1431-1437.
3. Swinburn B, Sacks G, Hall K, McPherson K, Finegood D, Moodie M, et al. The global obesity pandemic: shaped by global drivers and local environments. Lancet 2007; 378(9793): 804-814.
4. Guh D, Zhang W, Bansback N, Amarsi Z, Birmingham C, Anis A. The incidence of co-morbidities related to obesity and overweight: a systematic review and meta-analysis. BMC Public Health 2009; 9(1): 88.
5. Alwan A. Global status report on noncommunicable diseases 2010. Geneva: WHO, 2011.
6. Nejat E, Polotsky A, Pal L. Predictors of chronic disease at midlife and beyond-the health risks of obesity. Maturitas 2010; 65(2): 106-111.
7. Pischon T, Nöthlings U, Boeing H. Obesity and cancer. Proceedings of the Nutrition Society 2007; 67(2): 128-145.
8. Hammond RA, Levine R. The economic impact of obesity in the United States. Diabetes Metabolic Syndrome and Obesity: Target and Therapy 2010; 3: 285-295.
9. Pietilainen KH, Kaprio J, Borg P, Plasqui G, Yki-Jarvinen H, Kujala UM, et al. Physical inactivity and obesity: a vicious circle. Obesity (Silver Spring) 2008; 16(2): 409-414.
10. Newby PK, Muller D, Hallfrisch J, Qiao N, Andres R, Tucker KL. Dietary patterns and changes in body mass index and waist circumference in adults. American Journal of Clinical Nutrition 2003; 77(6): 1417-1425.
11. He K, Hu FB, Colditz GA, Manson JE, Willett WC, Liu S. Changes in intake of fruits and vegetables in relation to risk of obesity and weight gain among middle-aged women. International Journal of Obesity and Related Metabolic Disorders 2004; 28(12): 1569-1574.
12. Wang Y, Beydoun MA. Meat consumption is associated with obesity and central obesity among US adults. International Journal of Obesity 2009; 33(6): 621-628.
13. Malik V, Popkin B, Bray G, Després J, Hu F. Sugar-sweetened beverages, obesity, type 2 diabetes mellitus, and cardiovascular disease risk. Circulation 2010; 121(11): 1356-1364.
14. Deshmukh-Taskar P, Nicklas T, Radcliffe J, O'Neil C, Liu Y. The relationship of breakfast skipping and type of breakfast consumed with overweight/obesity, abdominal obesity, other cardiometabolic risk factors and the metabolic syndrome in young adults. The National Health and Nutrition Examination Survey (NHANES): 1999-2006. Public Health Nutrition 2013; 16(11): 2073-2082.
15. Liebman M, Pelican S, Moore SA, Holmes B, Wardlaw MK, Melcher LM, et al. Dietary intake, eating behavior, and physical activity-related determinants of high body mass index in rural communities in Wyoming, Montana, and Idaho. International Journal of Obesity and Related Metabolic Disorders 2003; 27(6): 684-692.
16. Ebrahim S, Kinra S, Bowen L, Andersen E, Ben-Shlomo Y, Lyngdoh T, et al. The effect of rural-to-urban migration on obesity and diabetes in India: a cross-sectional study. PLoS Medicine 2010; 7(4): e1000268.
17. Weng X, Liu Y, Ma J, Wang W, Yang G, Caballero B. An urban-rural comparison of the prevalence of the metabolic syndrome in Eastern China. Public Health Nutrition 2007; 10(2): 131-136.
18. Jackson JE, Doescher MP, Jerant AF, Hart LG. A national study of obesity prevalence and trends by type of rural county. Journal of Rural Health 2005; 21(2): 140-148.
19. Patterson PD, Moore CG, Probst JC, Shinogle JA. Obesity and physical inactivity in rural America. Journal of Rural Health 2004; 20(2): 151-159.
20. Befort CA, Nazir N, Perri MG. Prevalence of obesity among adults from rural and urban areas of the United States: findings from NHANES (2005-2008). Journal of Rural Health 2012; 28(4): 392-397.
21. Reeder BA, Chen Y, Macdonald SM, Angel A, Sweet L. Regional and rural-urban differences in obesity in Canada. Canadian Heart Health Surveys Research Group. Canadian Medical Association Journal 1997; 157(Suppl 1): S10-6.
22. Kettle SM, Roebothan BV, West R. Prevalence of specific cardiovascular disease risk factors in young Newfoundland and Labrador adults living in urban and rural communities. Canadian Journal of Rural Medicine 2005; 10(2): 81-85.
23. Rasmussen F, Johansson M, Hansen HO. Trends in overweight and obesity among 18-year-old males in Sweden between 1971 and 1995. Acta Paediatrica 1999; 88(4): 431-437.
24. Parks SE, Housemann RA, Brownson RC. Differential correlates of physical activity in urban and rural adults of various socioeconomic backgrounds in the United States. Journal of Epidemiology and Community Health 2003; 57(1): 29-35.
25. Wilcox S, Castro C, King AC, Housemann R, Brownson RC. Determinants of leisure time physical activity in rural compared with urban older and ethnically diverse women in the United States. Journal of Epidemiology and Community Health 2000; 54(9): 667-672.
26. Morton LW, Blanchard TC. Starved for access: life in rural America's food deserts. Rural Sociology Society 2007; 1(4): 1-10.
27. Walker RE, Keane CR, Burke JG. Disparities and access to healthy food in the United States: a review of food deserts literature. Health & Place 2010; 16(5): 876-884.
28. Eberhardt MS, Ingram DD, Makuc DM, et al. Urban and rural health chartbook. Health, United States, 2001 Hyattsville, MD: National Center for Health Statistics (Online) 2001. Available: www.cdc.gov/nchs/data/hus/hus01cht.pdf (Accessed 9 December 2009).
29. Centers for Disease Control and Prevention. National Health and Nutrition Examination Survey (Online). Available: www.cdc.gov/nchs/nhanes.htm (Accessed 5 December 2013).
30. Hart LG, Larson EH, Lishner DM. Rural definitions for health policy and research. American Journal of Public Health 2005; 95(7): 1149-1155.
31. US Department of Agriculture, Economic Research Service. Measuring rurality: rural-urban commuting area codes 2005. (Online). Available: www.ers.usda.gov/data-products/rural-urban-commuting-area-codes.aspx (Accessed 5 January 2015).
32. Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organization Technical Report Series 2000; 894: i-xii, 1-253.
33. Weiss EC, Galuska DA, Kettel Khan L, Gillespie C, Serdula MK. Weight regain in US adults who experienced substantial weight loss, 1999-2002. American Journal of Preventive Medicine 2007; 33(1): 34-40.
34. Haskell WL, Lee IM, Pate RR, Powell KE, Blair SN, Franklin BA, et al. Physical activity and public health: updated recommendation for adults from the American College of Sports Medicine and the American Heart Association. Circulation 2007; 116(9): 1081-1093.
35. Albright CL, Pruitt L, Castro C, Gonzalez A, Woo S, King AC. Modifying physical activity in a multiethnic sample of low-income women: one-year results from the IMPACT (Increasing Motivation for Physical ACTivity) project. Annals of Behavioral Medicine 2005; 30(3): 191-200.
36. Ball K, Crawford D. Socioeconomic status and weight change in adults: a review. Social Science & Medicine 2005; 60(9): 1987-2010.
37. Gearhart RF GD, Vanata DF. Obesity in the lower socio-economic status segments of American society. Forum on Public Policy 1 (Online). 2008. Available: www.forumonpublicpolicy.com/archivespring08/gearhart.pdf (Accessed 30 January 2014).
38. Gorber SC, Tremblay M, Moher D, Gorber B. A comparison of direct versus self-report measures for assessing height, weight, and body mass index: a systematic review. Obesity Reviews 2007; 84: 307-326.
39. White House Council of Economic Advisors. Strengthening the rural economy - the current state of rural America. (Online). Available: www.whitehouse.gov/administration/eop/cea/factsheets-reports/strengthening-the-rural-economy/the-current-state-of-rural-america (Accessed 5 July 2013).
40. Elder CR, Gullion CM, Funk KL, Debar LL, Lindberg NM, Stevens VJ. Impact of sleep, screen time, depression and stress on weight change in the intensive weight loss phase of the LIFE study. International Journal of Obesity 2012; 36(1): 86-92.
41. Anderson ES, Winett RA, Wojcik JR. Self-regulation, self-efficacy, outcome expectations, and social support: social cognitive theory and nutrition behavior. Annals of Behavioral Medicine 2007; 34(3): 304-312.
42. Khan LK, Sobush K, Keener D, Goodman K, Lowry A, Kakietek J, et al. Recommended community strategies and measurements to prevent obesity in the United States. MMWR Recommendations and Reports 2009; 58(RR-7): 1-26.
43. Vadheim L, Brewer K, Kassner D, Vanderwood K, Hall T, Butcher M, Harwell T. Effectiveness of a lifestyle intervention program among persons at high risk for cardiovascular disease and diabetes in a rural community. Journal of Rural Health 2010; 26(3): 266-272.
44. Tai-Seale T, Chandler C. Nutrition and overweight concerns in rural areas: a literature review. Rural Healthy People 2010; 187-198.
45. Sharkey JR, Johnson CM, Dean WR. Food access and perceptions of the community and household food environment as correlates of fruit and vegetable intake among rural seniors. BMC Geriatrics 2010; 10: 32.
46. Renee W, Keane C, Burke J. Disparities and access to healthy food in the United States: a review of food deserts literature. Health & Place 2010; 16(5): 876-884.
47. Kegler MC, Escoffery C, Alcantara I, Ballard D, Glanz K. A qualitative examination of home and neighborhood environments for obesity prevention in rural adults. International Journal of Behavioral Nutrition and Physical Activity 2008; 5: 65.
48. Casey AA, Elliott M, Glanz K, Haire-Joshu D, Lovegreen SL, Saelens BE, et al. Impact of the food environment and physical activity environment on behaviors and weight status in rural US communities. Preventive Medicine 2008; 47(6): 600-604.

