Dear Editor
There are limited and conflicting studies examining the quality of health care in rural versus urban settings1-4. This research is even more limited when it pertains to pediatrics care5. To date, no studies have examined quality as it relates to healthcare costs within the United States.
We conducted a retrospective study to compare the quality and costs of care among rural and urban hospitals for low severity pediatric bronchiolitis admissions. The Agency for Healthcare Research and Quality 2009 Kids' Inpatient Database provided the data for analysis. Diagnosis and severity of illness levels were based on All Patient Refined Diagnosis-Related Groups (APR-DRG) of 138: bronchiolitis and respiratory syncytial virus pneumonia. We included the lowest severity of illness, as defined by APR-DRG severity classification, comprising 58.8% of all pediatric bronchiolitis discharges. The Institutional Review Boards of Sanford Health and Sanford School of Medicine approved this study (Sanford Health Project Number 03-12-001, meets exempt status; Sanford School of Medicine Project Number 2011.210; meets exempt status).
Rural and urban status was based on Core Based Statistical Area codes. Additional variables included hospital ownership, National Association of Children's Hospitals and Related Institutions status, and teaching versus non-teaching designations. Hospital costs were determined by using hospital specific cost-to-charge ratios as obtained from each hospital's accounting reports.
Weighted statistical analyses were conducted using STATA/IC 12.1 (http://www.stata.com/stata12/). Given the complex sampling survey data present, we utilized the weighted analysis function ('syv' command) to determine the mean and 95% confidence intervals. Adjusted Wald tests assessed statistical significance across populations.
In 2009, there was a total of 11,161 patients admitted to rural hospitals and 54,654 admitted to urban hospitals (Table 1). Comparing patients admitted to rural versus urban hospitals, we found statistically different but clinically comparable age (0.5 vs 0.4 years, p<0.001) and gender (42.1 vs 40.7% females, p=0.03) with similar number of chronic conditions (0.12 vs 0.12 conditions, p=0.15) (Table 2). Number of procedures received was lower in rural hospitals (0.04 vs 0.13, p<0.001). Daily hospital costs were 10.9% lower ($1,136 vs $1,259, p<0.001) and total hospital costs were 19.5% lower ($2,401 vs $2,868, p<0.001) in rural hospitals with similar mortality rates (0% for both) and statistically different but clinically comparable lengths of stay (2.3 vs 2.4 days, p<0.001).
Table 1: Comparison of rural and urban hospitals
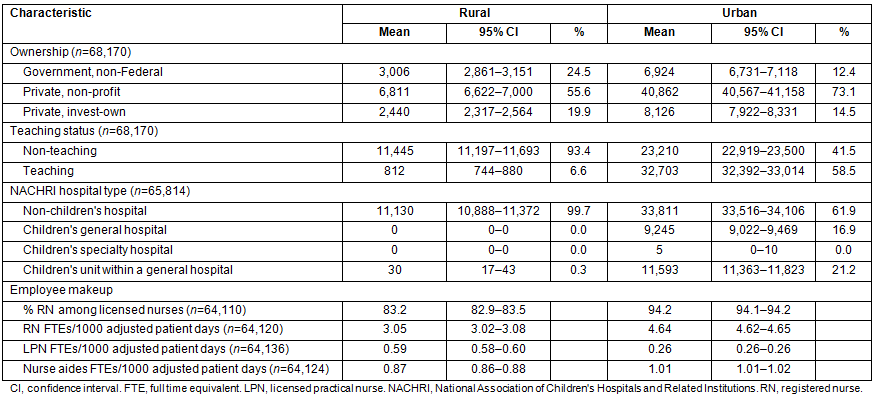
Table 2: Comparison of discharges from rural and urban hospitals
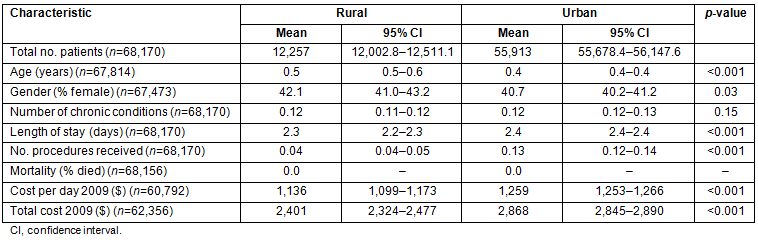
For pediatric inpatients with low severity bronchiolitis, we found that costs of care were higher in urban versus rural centers. Additionally, we found that care in urban hospitals did not improve quality outcomes, as mortality and length of stay were comparable.
These findings suggest that medical care for routine, low severity, pediatric diagnoses such as bronchiolitis may be more cost effective in rural versus urban centers. As previous studies focused primarily on quality of care, this is the first study we know of that documented lower costs of care in rural settings versus urban settings with comparable quality and outcomes.
We hypothesize that increased costs in urban settings may be influenced by factors including the higher proportion of teaching hospitals, greater competition for employees, and more procedures performed. This can have deep policy implications for the move toward regionalization of care within the United States.
Benson Hsu, MD, MBA, FAAP
Sanford School of Medicine, University of South Dakota
Sioux Falls, South Dakota, USA
Benjamin Meyer, BA
Sanford School of Medicine, University of South Dakota
Sioux Falls, South Dakota, USA
Saquib Lakhani, MD, FAAP
Sanford School of Medicine, University of South Dakota
Sioux Falls, South Dakota, USA
References
1. Paquette IM, Zuckerman R, Finlayson SR. Perforated appendicitis among rural and urban patients: implications of access to care. Annals of Surgery 2011; 253(3): 534-538.
2. Lynch CP, Strom JL, Egede LE. Disparities in diabetes self-management and quality of care in rural versus urban veterans. Journal of Diabetes and its Complications 2011; 25(6): 387-392.
3. Hicks PC, Bublitz Emsermann C, Westfall JM, Parnes B. Comparison of HTN management in patients with diabetes between rural and urban primary care clinics in Northeastern Colorado - a report from SNOCAP. Rural and Remote Health 10(1): 1279. (Online) 2010. Available: www.rrh.org.au (Accessed 28 October 2014).
4. Sheikh K, Bullock C. Urban-rural differences in the quality of care for Medicare patients with acute myocardial infarction. Archives of Internal Medicine 2001; 161(5): 737-743.
5. Lorch SA, Zhang X, Rosenbaum PR, Evan-Shoshan O, Silber JH. Equivalent lengths of stay of pediatric patients hospitalized in rural and nonrural hospitals. Pediatrics 2004; 114(4): e400-e408.
