The unequal geographical distribution of physicians in Australia, Canada and the USA has been a major challenge for policy developers1. Over the past 50 years, numerous attempts, including financial incentives, tuition fee reimbursement, and increased rural learning opportunities have been made to recruit and retain doctors in rural and remote areas. Clear evidence that students with rural backgrounds are more likely to choose rural practice2-4 has led to recruitment efforts being focused primarily on rural origin learners1,5. Subsequent to medical school admission, there is a substantial published literature on the effects of rural training programs on students that seek to motivate them to practice in rural areas6,7. These rural training programs may include shadowing experiences, short mandatory or elective rotations, and rural longitudinal integrated clerkships ranging from 3 months to a complete year7-9.
The pool of rural-origin students entering medical school is diminishing8,10-12. This trend aggravates the persistent shortage of physicians in rural and underserved communities and undermines the traditional program or governmental response. In addition, there is a trend amongst rural origin physicians to relocate to urban areas and establish practice13-15 supporting the need to study factors that motivate urban-origin students in choosing rural practice.
According to Arksey and O'Malley, a scoping review is a specific literature review in which emphasis is placed on techniques to rapidly map key concepts in pertinent literature in the field of interest. The purpose of a scoping review generally is to highlight the key concepts supporting a research area and the main sources and types of evidence available. Such reviews may be undertaken as an independent project especially when the research area has not been previously reviewed extensively16. Since quality of evidence is not accessed, it cannot be established whether particular studies provide robust or generalizable findings. A strong scoping statement, as well as definite inclusion and exclusion criteria applied to each paper identified, are prerequisites to prevent irrelevant material from being included within the study and to certify that the results meet the needs of the research question. The results of the review are summarized by thematic construction in order to present a narrative account of existing literature. The paucity of number of articles does not influence development of themes and each article can have multiple themes. Each step is documented and the results are listed to ensure repeatability of the study17.
Our research question was, 'What factors are responsible for rural recruitment and retention of urban-origin students?' The present article is a scoping review of the existing literature that specifically considers factors that promote urban-origin students to choose medical practice in a rural community. This allows the development of potential research questions for future studies targeting urban-origin students who choose a career in rural medicine.
Ovid Medline (Appendix I) and PubMed (Appendix II) databases were searched for articles nationally and internationally. MeSH terms, keywords and truncations were used with titles and abstracts for the search. The search was limited by date and language. Only articles published in the English language between 1 January 1970 and 30 November 2014 were included. The PubMed database was searched initially with the broad theme of 'rural retention of physicians' to retrieve a maximum number of articles on the topic. It resulted in 249 articles in total under this theme. The Medline database was searched in a similar way, but with the more specific terms listed in the appendix in the advanced search option. The themes under which the search was narrowed were:
- determinants for urban-origin students practicing in rural community (25 articles)
- determining factors for rural retention of doctors (31 articles)
- determinants of Manpower in rural community (171 articles).
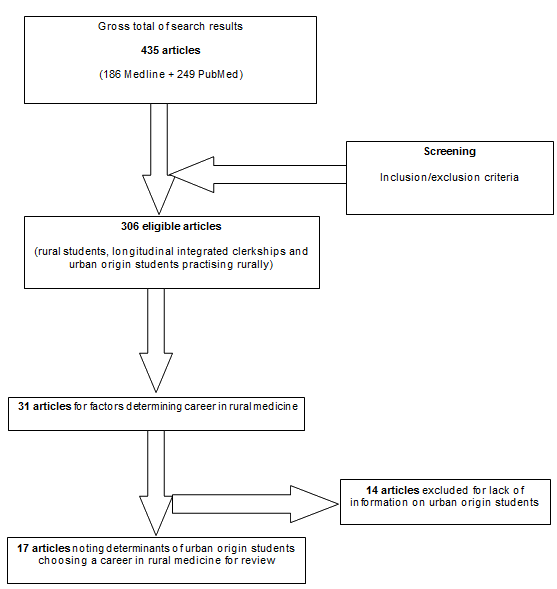
EndNote X7 was used to import references from Medline and PubMed databases. The articles were grouped together and duplicates removed. In combining lists from both databases, and after removing duplicates, 435 articles were identified; 186 articles were shortlisted from Medline and 249 from PubMed.
An Excel spreadsheet was designed with Microsoft Excel 2013 and used for screening the searched articles. The sheet was designed so that it contained the required information on inclusion and exclusion criteria noted below. Each article was required to pass the mandatory screening requirements to be included in the review study. Of these, articles that discussed factors influencing urban-origin students to choose rural practice were extracted for further review.
The following questions were the basis of the inclusion/exclusion criteria (Appendix III):
- Does the paper contain information regarding rural retention/rural practice of physicians?
- Was the paper published between 1 January 1970 and 30 November 2014?
- Is the paper from a peer-reviewed journal?
- Does the article have an abstract?
- Is the paper written in English?
Once a paper was determined to have met the criteria, it was screened further (Appendix III) for information about:
- urban-origin physicians
- factors related to urban-origin physicians choosing rural practice
- factors that led to retention of an urban-origin physician to stay in rural practice for longer than 5 years
- trends in rural migration of physicians.
Based on the inclusion criteria, 306 articles were identified. Two researchers worked separately and independently to complete the screening process. These results were subsequently compared and discrepancies were resolved by revisiting the inclusion criterion.
Applying exclusion criteria, 31 articles were identified discussing factors that potentially lead urban-origin students to choose rural practice. Further analysis excluded 14 more articles due to lack of specific information addressing the research question; 17 articles were finally accepted for the scoping review.
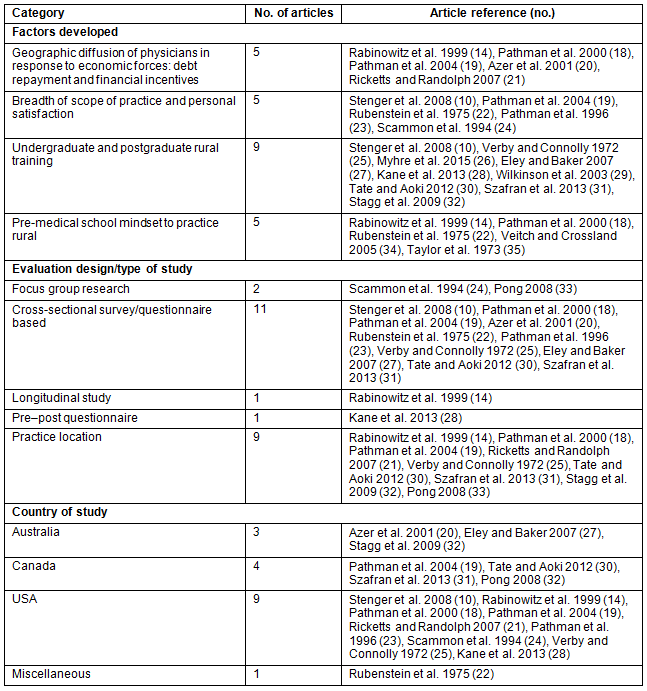
Table 1 shows the geographic distribution and type of studies conducted. Four themes were developed to summarize the information. These themes, in a broader sense, encompass the potential driving forces that may influence the choice of a rural career by urban-origin students. The total number of articles is greater than 17 studies because some measured more than one outcome (Table 1).
Table 1: Types of studies and the country where research was done10,14,18-35
1. Geographic diffusion of physicians in response to economic forces: debt repayment and financial incentives
One factor that motivates urban-origin students to choose a rural career is the taut competition they face in an urban location after completing their medical education. Both rural- and urban-origin students often acquire significant debt during medical school with approximately 80% of medical students in the USA carrying loans from $100 000 to $150 000 at the time of graduation18. High debt load and the risk of establishing a practice in a competitive market promote the movement of physicians to locations where economic opportunities are more apparent. This debt stress may then be aggravated upon graduation as competing financial priorities such as home mortgages, practice costs, and family expenses build. Some urban-origin students may choose rural practice to ease this financial burden. Provincial, state and federal governments, in an attempt to lure physicians to rural or underserved communities, may provide loan repayment options, which are frequently combined with direct financial incentives such as fee-for-service rural surcharges18. Debt repayment policies such as a waiver of full or partial tuition fees or in-kind benefits from the rural community/town council act as instant financial relief for urban-origin students19. Although the burden of work is greater in rural and underserved communities, these loan repayment options and higher fees for service motivate urban-origin students to relocate rurally14. Migration has been seen to rural areas that are located near an urban or suburban center, possibly to reap the benefits of both worlds. Frequent travel is possible when a physician lives in close proximity to a major urban center20. The decision to choose rural practice may also be seen to generate higher and more secure compensation21.
2. Breadth of scope of practice and personal satisfaction
New graduates tend to move to rural locations to gain valuable experience and confidence. Family physicians who choose to practice in rural locations are those who feel satisfied in their professional life due to opportunities available in those areas22. Physicians have reported that closer contact with patients in a rural setting establishes better doctor-patient relationships, thereby increasing role satisfaction22. The fact that fewer specialists work in rural areas may broaden the scope of practice for generalist/family physicians, leading to overall high job satisfaction in rural physicians19. The increased spectrum of services a rural family physician provides often exceeds that of their urban counterpart, leading to a challenging career that may be attractive to urban-origin students. Furthermore, it has been reported that rural physicians feel more appreciated in the community they serve, which results in increased satisfaction in spite of the increased workload10. Broader scope practices and the ability to become integrated into the local community appear to ultimately help urban-origin physicians to achieve their professional goals23,24.
3. Undergraduate and postgraduate rural training
The concept of medical education in a rural setting was introduced in the 1970s in the USA in an attempt to bridge the gap between demand and supply of physicians in rural areas25. Since implementation, various rural medical education programs have proven their effectiveness26. Rural undergraduate or postgraduate training broadens the horizons of urban-origin students who have never explored beyond the boundaries of their urban centers. Learners begin to appreciate the diversity of patients they treat and feel more valued in their profession. The success of rural medical education/training depends on factors that include quality of teaching, level of student-preceptor contact, dedicated patient panels and accommodation arrangements27. Subsequent to completing their rural training, students have been reported to show more interest in working in rural areas. Urban-origin students who participate in rural training are more inclined to choose family medicine residencies and become generalists28. The duration of rural postgraduate training in a rural area is positively correlated with the choice of rural practice by that physician29. Moreover, rural training facilitates an urban-origin student's understanding of the cultural aspects of rural practice, which further promotes amalgamation within the community10,30-32.
4. Premedical school mindset to practice rurally
A small number of studies identified an important, yet under-recognized, consideration that some urban-origin students enter medical school with the intention of practicing in a rural community. These urban-origin students may be an untapped resource in the effort to resolve the problem of shortage of physicians in rural areas. Their choice for rural practice should be reinforced by frequent exposures to rural rotations22. Little is known about the factors that lead to this predetermined career preference22.
According to Rabinowitz et al14, the existing intent to practice rurally at matriculation is clearly an independent predictor of rural retention. As depicted in their analysis, even after three decades of graduation from medical school, urban-origin physicians who intended to practice rurally at the time of matriculation continued to practice in rural and underserved communities. Furthermore, urban-origin physicians who have a partner of rural origin at time of matriculation have a higher chance of having a mindset to practice rurally19,34,35.
Discussion
External factors promoting rural practice to urban-origin students are identified in two of the four themes. Market and economic forces observed in the last decade along with government-based loan repayment and financial incentives play a role in the redistribution of physicians. These economic drivers do not simply apply to the physician alone, but at times are equally important for their partner19. It appears that physicians who are retained in a rural practice for a longer duration are those whose spouse/partner is able to find work in a rural community.
Rural medical education and rural postgraduate training have had a positive impact in changing the attitudes of urban-origin students in the consideration of a rural practice34. Those urban-origin students who have had a successful experience may also motivate peers to enroll in rural clerkships/rotations to enrich their experience and explore opportunities26. These rural training opportunities should be longer in duration to create a more meaningful experience for the learner26.
Two of the four themes consider factors that are not under the control of training programs, institutions or governments. An individual physician determines the value that a broad scope of practice and procedural opportunities holds. This breadth of practice does appear to be linked with the sense of fulfillment or value the physician appreciates. The theme does suggest that those undergraduates who value this practice characteristic could be offered such an opportunity in a smaller community as they are increasingly rare in urban centers.
Finally, those that have developed a mindset to practice rurally at the pre-medical school stage should be identified early in their career with the intent to reinforce this interest. One explanation for this mindset may be that urban-origin students possibly engage in trend analyses of supply and demand of physicians before the start of their medical education. Clearly, further studies should be done to identify this group of students early and to understand their motivation and decision process.
In addition to these themes that reflect primary factors promoting a career in rural medicine, our process also identified many obstacles for urban-origin students to practice in a rural setting. Some of the obstacles identified include career and job opportunities for spouses, educational and recreational opportunities for children, and continuing medical education for the physicians20,22. Other factors that may form a barrier to choosing rural medicine are feelings of isolation, remoteness from an urban area and lack of coverage for vacations. Potential solutions to these problems might lie in the development of remote continuing medical education and faculty development programs. Policies should be developed by governing bodies to address the issue of coverage for vacations by arranging for replacement physicians13. Further research should be conducted specifically to find solutions to these obstacles faced by urban-origin students.
This scoping review has identified themes for consideration in addressing the potential of urban-origin medical undergraduates to help address the maldistribution of physicians in rural communities. Further research to clarify the factors that promote a rural focus in urban-origin students prior to beginning training, and to support them through their education, may uncover a means to add a new pool of rural recruits and therefore help to bridge the gap between demand and supply of physicians in rural and underserved communities.
References
1. Heng D, Pong RW, Chan BT, Degani N, Crichton T, Goertzen J, et al. Graduates of northern Ontario family medicine residency programs practise where they train. Canadian Journal of Rural Medicine 2007; 12(3): 146-152.
2. Yeganeh-Arani E, Chandratilake M, Muula AS. Factors affecting career preferences of medical students at the College of Medicine, Malawi. South African Medical Journal 2012; 102(4): 249-251.
3. Beauchamp J, Belanger M, Schofield A, Bordage R, Donovan D, Landry M. Recruiting doctors from and for underserved groups: does New Brunswick's initiative to recruit doctors for its linguistic minority help rural communities? Canadian Journal of Public Health 2013; 104(6 Suppl 1): S44-S48.
4. de Vries E, Reid S. Do South African medical students of rural origin return to rural practice? South African Medical Journal 2003; 93(10): 789-793.
5. Alexander C, Fraser JD. Education, training and support needs of Australian trained doctors and international medical graduates in rural Australia: a case of special needs? Rural and Remote Health 7(2): 681. (Online) 2007. Available: www.rrh.org.au (Accessed 20 November 2014).
6. Acosta DA. Impact of rural training on physician work force: the role of postresidency education. Journal of Rural Health 2000; 16(3): 254-261.
7. Verby JE. The Minnesota Rural Physician Associate Program for medical students. Journal of Medical Education 1988; 63(6): 427-437.
8. Kassebaum DG, Szenas PL. Rural sources of medical students, and graduates' choice of rural practice. Academic Medicine 1993; 68(3): 232-236.
9. Myhre DL, Hohman S. Going the distance: early results of a distributed medical education initiative for Royal College residencies in Canada. Rural and Remote Health 12: 2151. (Online) 2012. Available: www.rrh.org.au (Accessed 20 November 2014).
10. Stenger J, Cashman SB, Savageau JA. The primary care physician workforce in Massachusetts: implications for the workforce in rural, small town America. Journal of Rural Health 2008; 24(4): 375-383.
11. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R, et al. Rural background and clinical rural rotations during medical training: effect on practice location. Canadian Medical Association Journal 1999; 160(8): 1159-1163.
12. Lu DJ, Hakes J, Bai M, Tolhurst H, Dickinson JA. Rural intentions: factors affecting the career choices of family medicine graduates. Canadian Family Physician 2008; 54(7): 1016-1017.
13. Mateen FJ. Future practice location and satisfaction with rural medical education: survey of medical students. Canadian Family Physician 2006; 52(9): 1106-1107.
14. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. Journal of Rural Health 1999; 15(2): 212-218.
15. Davies P. A comparison of rural and non rural RACGP training program trainees. Royal Australian College of General Practice. Australian Family Physician 1994; 23(7): 1330-1333, 1336.
16. Arksey H, O'Malley L. Scoping studies: towards a methodological framework. International Journal of Social Research Methodology 2005; 8(1): 19-32.
17. Landa AH, Szabo I, Le BL, Owen I, Fletcher G, Hill M. An evidence-based approach to scoping reviews. Electronic Journal of Information Systems Evaluation 2011; 10(4): 173-175.
18. Pathman DE, Konrad TR, King TS, Spaulding C, Taylor DH. Medical training debt and service commitments: the rural consequences. Journal of Rural Health 2000; 16(3): 264-272.
19. Pathman DE, Konrad TR, King TS, Taylor DH, Jr, Koch GG. Outcomes of states' scholarship, loan repayment, and related programs for physicians. Medical Care 2004; 42(6): 560-568.
20. Azer SA, Simmons D, Elliott SL. Rural training and the state of rural health services: effect of rural background on the perception and attitude of first-year medical students at the University of Melbourne. Australian Journal of Rural Health 2001; 9(4): 178-185.
21. Ricketts TC, Randolph R. Urban-rural flows of physicians. Journal of Rural Health 2007; 23(4): 277-285.
22. Rubenstein LZ, Rubenstein L, Elkin P, Elkin SP. Determinants of the choice of rural practice: a study of Yugoslav general practitioners. Journal of Medical Education 1975; 50(6): 615-623.
23. Pathman DE, Williams ES, Konrad TR. Rural physician satisfaction: its sources and relationship to retention. Journal of Rural Health 1996; 12(5): 366-377.
24. Scammon DL, Williams SD, Li LB. Understanding physicians' decisions to practice in rural areas as a basis for developing recruitment and retention strategies. Journal of Ambulatory Care Marketing 1994; 5(2): 85-100.
25. Verby JE, Connolly JP. Rural physician's associate program. Journal of Medical Education 1972; 47(11): 907-908.
26. Myhre DL, Adamiak PJ, Pedersen JS. Specialty resident perceptions of the impact of a distributed education model on practice location intentions. Medical Teacher 2015; 37(9): 856-861.
27. Eley DS, Baker PG. Will Australian rural clinical schools be an effective workforce strategy? Early indications of their positive effect on intern choice and rural career interest. Medical Journal of Australia 2007; 187(3): 166-167.
28. Kane KY, Quinn KJ, Stevermer JJ, Porter JL, Webb WD, Williamson HA Jr, et al. Summer in the country: changes in medical students' perceptions following an innovative rural community experience. Academic Medicine 2013; 88(8): 1157-1163.
29. Wilkinson D, Laven G, Pratt N, Beilby J. Impact of undergraduate and postgraduate rural training, and medical school entry criteria on rural practice among Australian general practitioners: national study of 2414 doctors. Medical Education 2003; 37(9): 809-814.
30. Tate RB, Aoki FY. Rural practice and the personal and educational characteristics of medical students: Survey of 1269 graduates of the University of Manitoba. Canadian Family Physician 2012; 58(11): e641-e648.
31. Szafran O, Crutcher RA, Woloschuk W, Myhre DL, Konkin J. Perceived preparedness for family practice: does rural background matter? Canadian Journal of Rural Medicine 2013; 18(2): 47-55.
32. Stagg P, Greenhill J, Worley PS. A new model to understand the career choice and practice location decisions of medical graduates. Rural and Remote Health 9(4): 1245. (Online) 2009. Available: www.rrh.org.au (Accessed 20 November 2014.).
33. Pong RW. Strategies to overcome physician shortages in northern Ontario: a study of policy implementation over 35 years. Human Resources for Health 2008; 6: 24.
34. Veitch C, Crossland LJ. Medical family support needs and experiences in rural Queensland. Rural and Remote Health 2005; 5(4): 1-11. (Online) 2005. Available: www.rrh.org.au (Accessed 20 November 2014).
35. Taylor M, Dickman W, Kane R. Medical students' attitudes toward rural practice. Journal of Medical Education 1973; 48(10): 885-895.
____________________________________
Appendix I: Search strategy for articles from Medline

Appendix II: Search strategy for articles from PubMed

Appendix III: Flowchart for screening of articles