Introduction
Increasingly, it is recognized that adolescence is a critical time for the development of lifestyle practices, attitudes, and beliefs related to health and wellbeing1-3. Previous researchers have described many of the health-related behaviors among adolescent populations, including the use of alcohol, tobacco and other substances, weight and dietary practices, and exercise habits4-6. Yet the evidence also suggests that there may be cause for concern, not only about the current health status and behaviors of adolescents, but also about their future health status as adults.
For example, the rising prevalence among children and youths of risk factors for adult-onset conditions such as cardiovascular disease7-10 suggests that adolescents may not be receiving or implementing health promotion messages designed to contribute to optimal health throughout the lifespan11,12. Furthermore, according to Statistics Canada13, the rate of smoking among rural Canadians aged 12 years and older exceeds the national average, as do the rates of obesity and heavy drinking among young adults. It also appears that adolescents may believe that their health is better than their current health behaviors would suggest2.
In addition, there appears to be cause for particular attention to the health status of rural adolescents. The health status of rural Canadians is generally poorer than that of urban Canadians, and governments along with health researchers and practitioners have identified the need to examine rural health in greater depth4,14. Long15 has asserted that although rural dwellers in general hold certain views and beliefs that affect health-related behaviours, the perspectives of rural youth are not well researched or understood. Within the adolescent population, the majority of research on health and health behaviors has been conducted in urban settings. Only a handful of studies have explored the health behaviors and/or beliefs of adolescents in rural areas2,7,16, and typically have been conducted in the USA.
Thus, when one of the authors (NKM) originally met with students, parents and school administrators to pursue a local participatory action research project on the health of rural adolescents, little information on this topic was available in the literature. The purpose of this article, therefore, is to describe a participatory action research project, involving use of a survey, designed to elicit the health practices and beliefs of rural adolescents. This article will also address interventions that were planned and implemented by students in collaboration with parents, teachers, and the public health nurse, as well as recommendations based upon the study's findings.
Methods
Research design
A participatory action research (PAR) framework was chosen to guide the study, because the aim was to not only to construct knowledge, but also to involve the rural community members in a collaborative and empowering partnership, a goal which is congruent with the philosophical underpinnings of PAR17,18. The process of collaboration with participants was seen as the most appropriate avenue to engaging their interest in developing and implementing interventions that would be viewed as useful and acceptable. As the public health nurse (PHN) for the school, one of the authors (NKM) was charged with implementing the Comprehensive School Health Program (CSHP) at the institution. The CSHP was implemented in the province of Alberta in an attempt to work within school communities to identify needs and to collaborate in the development of strategies to enable children and youth to value their health and to work towards maintaining wellbeing. Because the program's emphasis lies in health promotion and education activities, rather than in the provision of direct medical services, it was important to orient the students, staff, and parents to the role of all participants. Through this process it was made clear that the nurse was available to facilitate the identification of health needs, and the development and implementation of actions to address those needs. Consultation with the school community led to the decision that the starting point should be a survey to determine the assets and needs of students and staff. The aim was to discover the nature of the foundation on which to build interventions, and also to avoid duplication of existing strategies or creation of unnecessary ones. As noted by Henderson19, methodological simplicity is an important principle in action research and one which guided this project in order to maintain momentum.
Several survey tools, including a Health Canada20 instrument, were originally reviewed by the PHN. The PHN drafted a survey with the assistance of a parent volunteer, school principal, and counsellor. Revisions were made and reviewed in an iterative process until all stakeholders, including the school council, were satisfied with the tool. A copy of the resulting survey is available from the authors. The group's final objective was to not only ascertain the students' evaluations of their own health status and lifestyle choices, but to learn how they felt about their lives in a more general sense. For example, one question on the original Health Canada20 survey asked for the respondent's grade point average. The item was changed to reflect the student's level of satisfaction associated with academic achievement.
The resulting survey elicited data about the following: basic demographics, physical activity, body image, nutrition, alcohol use, tobacco use, drug use, injury prevention, stress, and improving overall health. The majority of questions consisted of coded response options (eg yes/no, multiple choice, or Likert-type scales); a few items included space for written responses and some questions included a checklist of options. Students were asked to indicate specific health promotion activities that could be developed in collaboration with school personnel and public health nurses in order to improve knowledge, awareness, and strategies for enhancing personal wellbeing. The intention was to summarize the results, present them to stakeholders, and jointly develop interventions tailored to provide a health-promoting environment.
Participants and setting
Students in grades 9, 10, 11 and 12 in a rural high school in Western Canada were invited to participate in a survey on adolescent health. The completed surveys (n = 288) represented a response rate of 84.5% of the total school enrolment. The mean age of the students was 15.5 years, and slightly more males than females completed the survey (males = 53.6%; females = 46.4%). Respondents were almost equally divided according to grade (grade 9 = 22.7%; grade 10 = 25.1%; grade 11 = 25.1%; and grade 12 = 24.7%). The school was located in a town with a population of approximately 1900, which served the ranching and farming needs of the surrounding region. The town was approximately 60 km from a major urban centre of 900 000 people.
Survey procedure
Ethics approval for this study was received from the University of Lethbridge Human Subject Research Committee. Students were invited by their teachers, during regular class time, to fill out the survey. Teachers read the first page of the survey to the students, which included, as is standard with survey research, statements on anonymity, confidentiality, the voluntary nature of the research, and the fact that participation in the survey signified implied consent. Completed anonymous surveys were sealed in envelopes by students and given to the teacher, who passed them directly to one of the researchers.
Data analysis
Original survey data were analyzed using SPSS for Windows vers 11.5.0 (SPSS Inc., Chicago, IL) statistical computer package with descriptive statistics (ie, frequency counts and cross-tabulations) computed for all questions. As many of the initial descriptive results suggested significant differences in responses by gender, c2 analyses were conducted on selected variables to test for statistically significant differences in responses between males and females. The significance level for statistically significant results was set at p< 0.05.
Results
Student interests, body image, and nutrition
Students (n = 288) reported numerous interests including music (50.0% girls; 41.0% boys), art (40.0% girls; 20.5% of boys) and reading (31.5% girls; 19.2% boys). They were also interested in animals (48.5% girls; 30.8% boys), computers (29.2% girls; 38.5% boys), and having a part-time job (38.8% girls; 26.3% boys). The students reported their greatest interests to be participating in sports activities (60.8%), especially competitive sports (39.4%). Frequent involvement (at least three times per week) in a physical activity was noted by 75.9% of respondents.
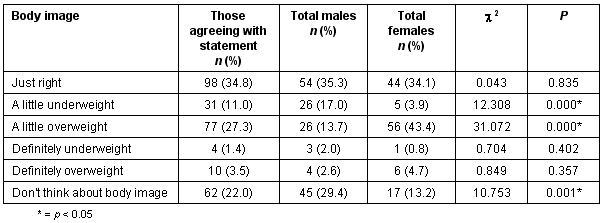
Despite their reports of a high level of activity, only 34.1% of females and 35.3% of males said their body image was 'just right'. Almost half of the females (48.1%) thought they were either 'a little overweight' or 'definitely overweight' (Table 1). Many of the adolescents (63.2%) indicated that they ate well-balanced meals, but 49.5% also noted that they ate a lot of junk food. Meals were skipped most of the time by 25.8% of the students, and 17.9% indicated that they need caffeine to get through the day. A surprisingly low percentage (9.3%) indicated they 'eat out a lot'.
Table 1: Adolescents' perceptions of body image by sex
Students' use of tobacco, alcohol, and drugs
Student use of tobacco, alcohol and drugs is summarized by sex (Table 2). Regular cigarette smoking was reported by only 14.1% of the students involved in the study, although 55.9% reported having tried smoking at one time. Of those who did smoke, more girls smoked (16.2%) than boys (12.3%).
Table 2: Adolescents' use of tobacco, illegal drugs and alcohol by sex
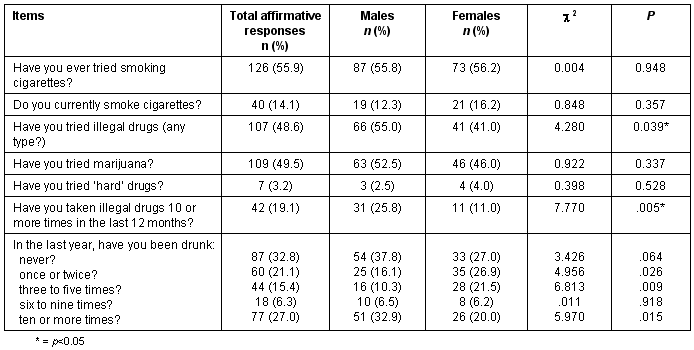
Marijuana had been used by 49.5% of the students, and 19.1% (11.0% of females and 25.8% of males) had taken drugs 10 or more times in the last 12 months. Only 3.2% of the student sampled had tried hard drugs. Of the students, 70% reported that they had been drunk at least one time in the last 12 months, with 27.1% indicating they had been drunk 10 or more times in that time period. Consumption of more than five drinks in a two to three hour period was stated to have occurred at least one time in the last 12 months by 51.5%; 20.3% said they had had more than five drinks 10 or more times. There were few gender differences in the use of tobacco or alcohol, although significantly more males (55.0%) than females (41%) had tried illegal drugs (c2 = 4.280, p<0.05).
Injuries and injury prevention
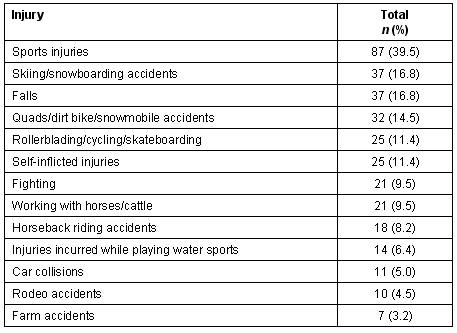
The most common injuries experienced by this sample of adolescents in the previous year is presented (Table 3). Within that time frame, 53.3% of the students noted that they had been injured, with the most common injury (39.5%) being sports-related. Seatbelts were always or usually worn by 65.3% of the teens when riding in a car, and 67.9% said they obeyed driving laws usually or always. With regard to drinking and driving, 53.0% of students indicated that they always drove sober, 7.9% said they usually drove sober, 12.0% said they have driven after drinking alcohol, and 39.8% have ridden with a driver who had been drinking alcohol.
Table 3: Most common injuries (occurring in past year) in adolescents
Student worry and stress
Students indicated that their main issues at school were: concern about grades (40.5%); managing schoolwork (35.7%); and managing their time (31.6%). Students also observed that meeting standards set by teachers (29.9%) and meeting deadlines (27.5%) were common stressors at school. Some of the least common sources of stress and worry included being physically threatened or bullied (5.8%), being sexually harassed (3.4%), and problems with drugs and/or alcohol (3.4%).
At home, the main worries or stresses mentioned were: balancing home, work, and school (33.7%); not enough money (28.9%); and pressure from parents to get good marks (20.3%). The students also indicated that having a close family member die or become ill (18.9%); conflicts with family members (18.2%); and having a close relationship end (16.8%) were among the most stressful events in their lives. Unexpected pregnancy (3.8%), birth of a child (2.4%) and sexual abuse (2.1%) were the least-mentioned sources of stress or worry.
Health promotion behaviors
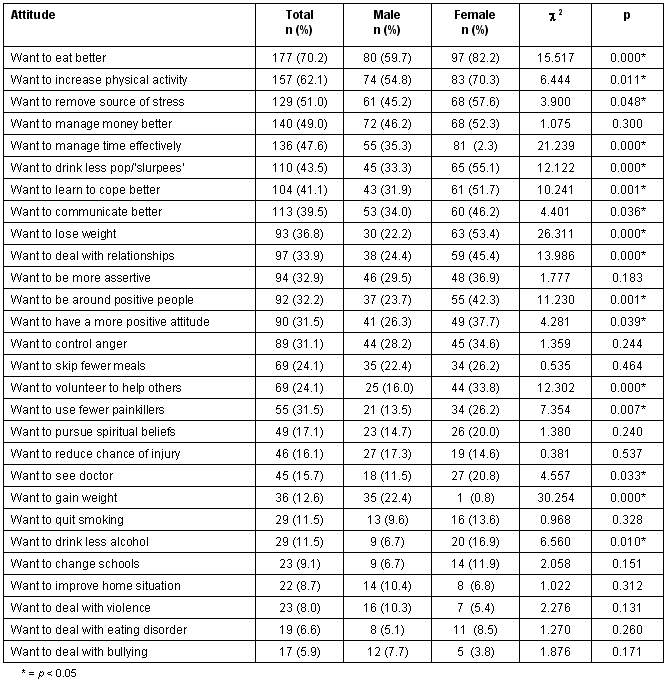
Table 4 is a representation of the various health promotion behaviors that adolescents wanted to use to improve or maintain their health. Most participants indicated that they would like to eat better (70.2%), increase their physical activity (62.1%), and remove a source of stress (51.0%) in order to improve or maintain their health. Slightly fewer than half the participants also mentioned that managing their money better (49.0%) and their time more effectively (47.6%) were ways they could improve or maintain their health in the next year. Of particular note was the gender difference in preferred health promotion strategies. That is, female respondents consistently reported a statistically greater desire to implement all of the stated health promotion behaviors, with the exception of five strategies which male adolescents reported more often: 'wanting to reduce chance of injury', 'wanting to gain weight', 'wanting to improve home situation', 'wanting to deal with violence', and 'wanting to deal with bullying'. With several of the health behaviors, females expressed at least twice as much interest as males, including 'want to lose weight', 'want to volunteer to help others', and 'want to use fewer painkillers'.
Table 4: Adolescents' attitudes towards improving or maintaining their health
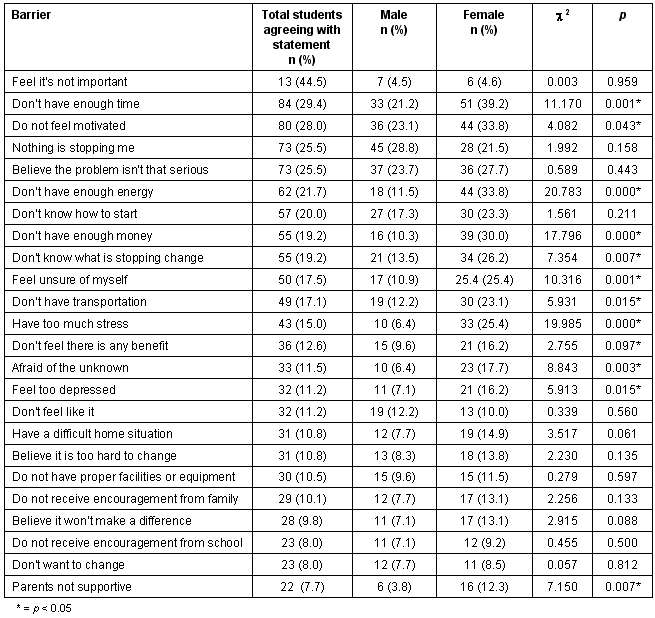
A summary of participants' perceived barriers to implementing the above health promotion behaviors is given (Table 5). The main perceived barriers were 'feel it's not important' (44.5%), 'not enough time' (29.4%), and 'do not feel motivated' (28.0%). Again, there were some significant differences in the perceived barriers between males and females, with females much more likely than males to report such barriers as 'don't have enough time', 'afraid of the unknown', and 'feel unsure about myself'. Obstacles reported especially frequently in females were the lack of energy (33.8%), lack of money (30.0%) and an overabundance of stress (25.4%).
Table 5: Barriers to making a positive change in health
Finally, students were asked what they thought the school could do to help them improve or maintain their health. Almost half (43.0%) the respondents wanted more advice from fellow students, 35.7% wanted more varied classroom activities, 32.6% wanted more access to nutritional foods, and 29.9% wanted more physical activity during school time.
Action strategy
In a PAR project, it is up to the participants to guide the choice and implementation of strategies to address the identified concerns. In general, these adolescents were aware of the need to improve their health and were able to suggest strategies to accomplish this goal. Although there were obvious problems related to alcohol and drug use, these were not issues the students chose to tackle initially. Alternatively, the students decided to arrange for general health education and awareness-raising sessions. In consultation with students, staff, and parents, a one-day 'Grade 12 Conference' was developed for members of the graduating class. Invitations were sent to students in the mail, and they were expected to take responsibility to register for the free event. Various community resource persons (including a psychologist, registered nurse, social worker, registered dietitian, and representatives from local businesses) discussed with students such topics as making smart choices, sexual and reproductive health, food choice and meal preparation, money management, job-hunting strategies, and post-secondary education options. Overall, the students felt it was important to address such topics as a health-promotion strategy, prior to leaving high school and preparing themselves for the transition into adulthood.
Other health-related spin offs have occurred as a result of the community's action strategy. Several months after the survey and the health conference, some motor vehicle collisions involving students occurred. Their peers identified the need to raise awareness and promote safer decisionmaking by the youth of the community. Consequently, the students are currently working with school, health, and emergency medical services personnel to create and implement strategies to achieve their goal of a safer community. Activities to date have included first aid and cardiopulmonary resuscitation training for students as a result of the feelings of helplessness on the part of fellow passengers in one of the car crashes. Students have implemented an orientation process for incoming classes of new students at their school to allay the fears and anxieties associated with changing schools. Parents also have decided to become more active in the health of all students in the community, and have initiated activities to identify and deal with food security issues that affect the students. Nutrition policies are being reviewed and the community dietitian has been consulted. As the key stakeholders assume more responsibility for identifying and addressing issues that affect the school community, the PHN is finding that she is able to step back from the facilitator role, and become more of a consultant and resource.
Discussion
The data obtained from the questionnaire revealed lifestyle practices and choices that could potentially be interpreted as health-compromising. For example, although sports activities were popular with many students, they were also the cause of most injuries. This finding is consistent with other reviews of adolescent statistics that suggested that most of the non-fatal injuries experienced by members of this age group were sports-related21,22. Frequent physical activity was reported by 75.9% of students in the present study, compared with 59.3% of participants in one Pennsylvania study who stated that they never exercised16, and 31.3% in another study who claimed to be very active2. Despite the comparatively high rate of physical activity found in this study, the rural female adolescents were still highly concerned about their body weight, as almost half felt they were a little or definitely overweight. In contrast, Puskar et al.16 noted that 30% of girls in a sample of rural Pennsylvania high schools noted concerns about excess body weight. Muscari et al.2 found that 41.1% of respondents felt that their weight was 'just right.' In another American study, 28% of boys and 34% of girls at a rural high school were concerned about weight, exercise, and eating8. Vingilis et al.3 noted that highly active adolescents (both urban and rural) in the Canadian National Population Health Survey rated their health more poorly than did less active individuals, a finding they described as 'counterintuitive'. These authors speculated that students who were concerned about their health and appearance were active because of their concern. Regardless of the reason, it is worrying that so many female students in this study were dissatisfied with their body weight, particularly given their reportedly high level of physical activity.
Although the reported rate of smoking among this sample of rural students (14.1%) was below both the Canadian average (22%)23 and the American average (28.5%)24 for this age group, and well below the numbers reported in some rural American studies2,7,16, the reason for the unexpectedly low rate of smoking remains unclear. The fact that more girls than boys smoked, however, is consistent with Canadian data. Several authors have noted links among the use of tobacco, dietary restraints, and self-reported concerns about body weight in rural and urban female students6,11,25. In view of the compelling evidence suggesting that this combination of factors is predictive of major eating disorders in young women6,25, the rural adolescent girls in this study may be at higher risk for starting smoking as a method to control perceived weight and body image problems.
Risk-taking behaviors - characteristic of adolescence - were commonly reported by participants in this study. Many students had experimented with tobacco, alcohol, and other drugs, consistent with the findings of other rural investigators2,7,16. Boys in particular were more likely to engage in significant alcohol use; similar findings were noted by several investigators14,16. Although there was evidence of lack of compliance with seat belt use and sobriety while driving, even less compliance has been reported in at least one other study2. Nevertheless, the combination of alcohol use and potentially dangerous driving behavior in this sample is a public health issue worthy of ongoing monitoring and health promotion initiatives26.
Students identified many stressors in their lives. Most concerns centered around school and the pressures to earn good grades, as well as the need to balance home, work, relationships, and school activities. Similarly, Puskar, Lamb, and Bartolovic27 found that the two most common causes of stress in their study of rural students in Pennsylvania were school and family issues, including fighting and loss of a family member. There is no doubt that students experience and are affected by a wide variety of stressors, both in school and in their day-to-day lives.
Students noted that the school had a role in facilitating access to information and skills that would lead to better health status. Hanson et al.28, in their investigation of the health services desired by rural Illinois high school students, reported that stress management services, weight management counselling, depression counselling, birth control advice, tests and treatment for sexually transmitted diseases, and job counselling were the most wanted services. Numerous authors have echoed the suggestion that schools provide an ideal environment in which to initiate comprehensive health services for adolescents8,28-32 and that schools and communities that work together are likely to be more successful in reducing youth risk behaviours33. Furthermore, Gådin and Hammarström11 suggested that schools may have a role in the identification of future unfavourable health behaviors among young students based on their observation that such behaviors seem to be established by the age of 12 years. In addition, Symons et al.32 pointed out that the inextricable link between student health status and academic achievement makes it imperative that resources be invested in improving the health status of adolescents.
Limitations
Despite the strengths that numerous collaborative partners - including parents, teachers, administrators, and students - brought to this project, compromises were inevitable. While the key interests of all partners were represented in the final survey, such compromises precluded the use of an existing adolescent health survey, complete with established validity and reliability. Also precluded by necessity was the ability to compare and contrast the results of this study with other studies that may have used well-tested instruments. In addition, the results of this particular study are limited in their generalizability, due to the involvement of only one rural school. Finally, the survey findings are based solely on self-reports of students, and the authors were unable to verify and substantiate these data by utilizing other potential sources, such as emergency room data on injury type and prevalence.
Implications
The need for school and health personnel to actively involve high school students in the process of developing, implementing, and evaluating health-focused initiatives cannot be overemphasized. Indeed, the adolescents in this study were able to identify clearly the status of various factors which contributed to their health, their needs and the obstacles they faced in achieving health. More importantly, they were able to engage in a community process to take action on improving their health. Engagement of participants in this kind of participatory action process not only demonstrates respect for the knowledge and abilities of community members34, but is essential in order to ensure appropriateness of assessment and intervention activities, and to facilitate their 'buy-in'. In addition, attention to the unique culture of the rural community context is vital to demonstrate understanding of and respect for the reality in which the adolescents live and function. For example, awareness of the specific needs of students and their families will facilitate implementation of relevant initiatives, thus enhancing the possibility of achieving positive outcomes.
Those involved in school health programs have an important role to play in the education and encouragement of adolescents as they make critical health and lifestyle choices. School and health personnel must continue to recognize and acknowledge the many influences to which adolescents are exposed as they develop decisionmaking skills around lifestyle and health choices and risks. A thoughtful and appropriate balance between strategies that reduce harm and those that enhance protective factors may offer an effective framework for promoting the health of adolescents. Particular attention to differences between the genders is essential in order to provide appropriate coaching and counselling services to young people4. It is essential that the architects of school health programs be familiar with local health-related curricula in order to collaborate with parents, students, education professionals, and other community resources to develop appropriate health initiatives for teenagers. Awareness of, and participation in, the process of curriculum development and its evaluation and assessment by school health nurses and other workers will facilitate the maintenance of a holistic perspective of health and its determinants. A focus on integrating health issues across the school curriculum will reinforce the concept of health as a dynamic resource for living as well as a state of wellbeing. For example, instruction in and opportunity to explore lifelong recreational activities in physical education classes would reinforce the importance of maintaining physical fitness throughout adulthood.
Further research is required to gain a more comprehensive understanding of the parameters and determinants of health among rural adolescents and of the factors which both promote and compromise the wellbeing of these students. As noted by Doerr and Wantuch35, decision-makers are more likely to respond to a problem when presented with quantified relevant information. Of equal importance, however, is the need to develop and evaluate intervention strategies that will benefit and promote health and resiliency among the youth in the context of the communities in which they live. Several authors have indicated a necessity to better understand those factors that contribute to the community's resiliency-that is, its abilities to both respond to adversity and improve functioning36,37. While this study does not directly address the notion of resiliency, it does provide an example of how a rural community can galvanize around a community issue - in this case rural adolescent health - and thereby help adolescents to gradually build their own resiliency regarding health and wellness issues.
Recommendations
This PAR project not only assisted a rural community to research and address its adolescent health issues, but also provides a foundation from which to direct future practice and research. Therefore, at this point, the authors would like to make a number of recommendations for further research and practice, stemming from this project:
- This project demonstrated that rural adolescents are enthusiastic and willing participants in the identification, design, and implementation of appropriate interventions in order to promote health behaviors when opportunities to collaborate with family and community members are presented. It is appropriate to engage students in the process of addressing their own health concerns and practices, and to solicit the support of parents and the broader community in so doing. In this way, the chances of succeeding are higher and the sense of accomplishment greater. Therefore, the kind of community development approach demonstrated in this PAR project is highly recommended as a way to address rural adolescent health issues.
- The students' choice of harm reduction activities suggested that they understand that risky behaviors among youth may never be eliminated completely. However, by providing students with the knowledge and power to make healthy choices, the potential for great harm may be mediated somewhat. Furthermore, it is vital to recognize that the problems of youth are the problems of the wider society, and that successful interventions will require implementation at a multiple levels, from the individual and family level to the policy level. Few educators, for example, would agree that the students' schools can or should bear total responsibility for the health of adolescents. Rather, collaborative efforts by students, their families and communities, and governments and other societal institutions are required in order to achieve health and well-being among rural youth.
- Although many issues were identified by students, better understanding of adolescent health antecedents and consequences would be gained by investigating other sources of information. For example, clearer knowledge about the processes used by students as they make choices and decisions about health practices would offer information helpful to the development of appropriate strategies that will facilitate better health among rural adolescents.
- A detailed investigation of the extent of drug, alcohol, and tobacco use by rural youth of all ages also would offer a more comprehensive understanding of risky adolescent health practices in rural areas. Diet, stress, nutrition, and physical activity concerns raised by these rural students would also benefit from further study. Finally, evaluation of participatory action research interventions around adolescent rural health, such as the ones implemented in this study, would provide direction for how best to allocate public adolescent health resources in rural communities.
Conclusions
Participants in this action research project were successful in achieving their goal of engaging the youth of a rural Canadian community in identifying their unique health assets and needs. A number of significant concerns were raised as a result of the survey, including use of drugs and alcohol, diet and nutrition, and risky behaviours. It was also evident that gender plays an important role in health perceptions and behaviours. As a result of their increased awareness not only of the potential threats to their health, but also of the willingness of the community to provide support, students initiated a health conference designed to help them learn about resources and topics of interest to them. In addition, students have engaged in harm reduction activities for themselves and their younger peers, while their parents have taken steps to further examine issues of health and wellbeing across a wider spectrum of the community.
References
1. Jessor R, Turbin MS, Costa FM. Protective factors in adolescent health behavior. Journal of Personality and Social Psychology 1998; 75: 788-800.
2. Muscari ME, Phillips C, Bears T. Health beliefs and behaviors in rural high school juniors. Pediatric Nursing 1997; 23: 380-389.
3. Vingilis ER, Wade TJ, Seeley JS. Predictors of adolescent self-rated health. Canadian Journal of Public Health 2002; 93: 193-197.
4. Plotnikoff RC, Bercovitz K, Loucaides CA. Physical activity, smoking, and obesity among Canadian school youth. Canadian Journal of Public Health 2004; 95: 413-418.
5. Bethell C, Klein J, Peck C. Assessing health system provision of adolescent preventive services: The young adult health care survey. Medical Care 2001; 39: 478-490.
6. Winter A-L, de Guia NA, Ferrence R, Cohen JE. The relationship between body weight perceptions, weight control behaviours and smoking status among adolescents. Canadian Journal of Public Health 2002; 93: 362-365.
7. Atav S, Spencer GA. Health risk behaviors among adolescents attending rural, suburban, and urban schools: A comparative study. Family & Community Health 2002; 25: 53-64.
8. Bracken AC, Hersh AL, Johnson DJ. A computerized school-based health assessment with rapid feedback to improve adolescent health. Clinical Pediatrics 1998; 11: 677-683.
9. Evers S, Taylor J, Manske S, Midgett C. Eating and smoking behaviours of school children in southwestern Ontario and Charlottetown, PEI. Canadian Journal of Public Health 2001; 92: 433-436.
10. Pittman KP, Wold JL, Wilson AH, Huff C, Williams S. Community connections: Promoting family health. Family & Community Health 2000; 23: 72-78.
11. Gådin KG, Hammarström A. Can school-related factors predict future health behaviour among young adolescents? Public Health 2002; 116: 22-29.
12. Walker Z, Townsend J, Oakley L et al. Health promotion for adolescents in primary care: Randomised controlled trial. British Medical Journal 2002; 325: 1-6.
13. Statistics Canada. How healthy are Canadians? Report no: 82-003-XPE. Ottawa, ON: Statistics Canada, 2002.
14. Mitura V, Bollman RD. The health of rural Canadians: A rural-urban comparison of health indicators. Rural and Small Town Canada Analysis Bulletin 2003; 4: 23.
15. Long KA. The concept of health: Rural perspectives. Nursing Clinics of North America 1993; 28: 123-130.
16. Puskar KR, Tusaie-Mumford K, Sereika S, Lamb JM. Health concerns and risk behaviors of rural adolescents. Journal of Community Health Nursing 1999; 16: 109-119.
17. Patton MQ. Qualitative research and evaluation methods. 3rd ed. Thousand Oaks, CA: Sage; 2002.
18. Wallerstein N, Duran B. The conceptual, historical, and practice roots of community based participatory research and related participatory traditions. In: M Minkler, N Wallerstein (Eds). Community-based participatory research for health. San Francisco: Jossey-Bass, 2003; 27-52.
19. Henderson I. Action research: A route to practice and professional development. Synergy 2002 (August): 18-20.
20. Health Canada. Voices and choices: Student needs assessment questionnaire. Ottawa, ON: Health Canada, 2000.
21. Ardern C, Pickett W, King MA, Boyce WF. Injury in Canadian youth: A brief report from the Health Behaviour in School-Aged Children survey. Canadian Journal of Public Health 2001; 92: 201-203.
22. Scheidt PC, Harel Y, Trumble AC, Jones DH, Overpeck MD, Bijur PE. The epidemiology of nonfatal injuries among U.S. Children and youth. American Journal of Public Health 1995; 85: 932-938.
23. Health Canada. Canadian Tobacco Use Monitoring Survey (CTUMS) summary of results for Wave 1 (February to June) 2002. (Online) 2002. Available: http://www.hc-sc.gc.ca/hecs-sesc/tobacco/research/ctums/2002/summary.html (Accessed 2 July 2 2003)
24. Grunbaum JA, Kann L, Kinchen SA, Williams et al. Youth risk behavior surveillance - United States, 2001. Morbidity and Mortality Weekly Report 2002; 51(SS04): 1-64.
25. Crocker P, Kowalski N, Kowalski K, Chad K, Humbert L, Forrester S. Smoking and dietary restraint in young adolescent women: The role of physical self-perceptions. Canadian Journal of Public Health 2001; 92: 428-432.
26. Single E. Alcohol and youth: Time for effective action. Canadian Journal of Public Health 2002; 93: 169-170.
27. Puskar KR, Lamb JM, Bartolovic M. Examining the common stressors and coping methods of rural adolescents. Nurse Practitioner 1993; 18: 50-53.
28. Hanson CL, Kittleson M, Welschimer KJ, Ritzel DO, Woehlke PL, Isberner FR. Rural school health services: An assessment of adolescents' felt needs. International Electronic Journal of Health Education 1999; 2: 18-27.
29. James TC, Cinelli B. Targeted awareness campaigns: Advocating for coordinated school health programs. American Journal of Health Education 2003; 34: 117-118.
30. Lynagh M, Knight J, Schofield MJ, Paras L. Lessons learned from the Hunter Region Health Promoting Schools Project in New South Wales, Australia. Journal of School Health 1999; 69: 227-232.
31. Rickert VI, Davis SO. Rural school-based clinics: Are adolescents willing to use them and what services do they want? Journal of School Health 1997; 67: 144-149.
32. Symons CW, Cinelli B, James TC, Groff P. Bridging student health risks and academic achievement through comprehensive school health programs. Journal of School Health 1997; 67: 220-227.
33. Martino-McAllister JM, Thompson JM, Caulkins P. Developing a community response to reduce youth risk behaviors. American Journal of Health Education 2001; 32: 298-301.
34. McAllister CL, Green BL, Terry MA, Herman V, Mulvey L. Parents, practitioners, and researchers: Community-based participatory research with Early Head Start. American Journal of Public Health 2003; 93: 1672-1679.
35. Doerr BT, Wantuch C. Cudahy High School survey and focus groups: Assessment of the needs of a teen population. A community-campus collaboration. Public Health Nursing 2000; 17: 11-15.
36. Kulig JC. Community resiliency: The potential for community health nursing theory development. Public Health Nursing 2000; 17: 374-385.
37. Larson NC, Dearmont M. Strengths of farming communities in fostering resilience in children. Child Welfare 2002; 81: 821-835.



