In Canada and internationally, a crisis of sustainability is being faced by rural maternity and surgical health services1-5. This is evidenced most clearly by the closure of rural services, particularly maternity and small surgical6. An often drawn-out process involving instability of local providers, consequent diversion of patients to other communities, and attendant provider and community stress culminate into this lack of sustainability7. Closures across administrative or electoral regions may prompt system responses that do not address the root causes of the unsustainability, often in the form of increased payments to care providers or other fiscal incentives to revive the services, which may be effective only in the short term, with long-term effects unknown.
This article was generated as part of a larger review commissioned by the provincial Ministry of Health and Perinatal Services British Columbia (BC), Canada. The larger review was used to investigate centralized or decentralized care as the optimal model of perinatal surgical care for rural women. The immediate context for the review included the recognition of the importance of cesarean section (C-section) services in preserving small maternity services8. The high number of rural maternity service closures and the care provider and community response, manifest in local efforts to sustain or reinstate services9, provided the broader context10. A common community response, rooted primarily in a social imperative for services closer to home, is in parallel to the growing need for a health services response to combat poor maternity and newborn outcomes. At least in part, distance to services is shown by emerging research to be the basis for these worsening outcomes1,11-13.
There has not been a comprehensive review on the satisfaction with and sustainability of decentralized rural surgical services, despite the current threats to such services seen both in Canada14 and internationally15,16. In this article, literature was reviewed through a realist lens as part of a larger review to contribute to an understanding of these entwined concepts. The larger review was conducted as a starting place for interventive policy development, setting out to answer the question, 'can the perinatal surgical needs for rural women be met more effectively through an optimally centralized or optimally decentralized model of care?' The review question was operationalized through considering safety and outcomes, costs and cost-effectiveness, sustainability and satisfaction. Further, each of these areas of consideration was examined according to the model(s) of care involved, including generalist models supported by general practitioners (GPs) with enhanced surgical and/or anesthesia skills and/or general surgeons, specialist models and mixed models. Summative findings from this larger report have also been reported elsewhere17.
There is a growing appetency from health policy makers and planners to glean insights from best practice models for health services delivery from other jurisdictions. The findings reported here on satisfaction and sustainability are interpreted through the lens of health policy in Canada broadly, and BC specifically.
Background - the local context
In 2012, a draft of the Primary Maternity Care Framework for BC was released by Perinatal Services BC and the Ministry of Health to address the salient action items that provincial consultations had raised. Due to high attrition of services, there was a particular focus on rural settings7:
Rural maternity services show system stresses early and are particularly vulnerable to shifts in provider supply or availability for intra-partum care. Several consultations have pointed to the importance of sustained availability of C-section capacity in preserving the small maternity services. The availability of general practitioners with C-section (or general surgery) skills or anaesthesia skills could play a significant role outside of urban areas. There are tensions within the medical community that make it difficult to develop a concrete next step with regard particularly to GP Surgery but also GP Anaesthesia7.
The imperative of birthing 'closer to home' has been noted in recent BC policy directives7,18,19. Alongside the policy directions, this has led to the growing recognition of the need to address challenges in sustaining rural perinatal surgical care.
Realist reviews
A realist review is a systematic way of looking for health services interventions with particular detail to 'what works for whom in what circumstances . . . and why'20. This approach accounts for the contextual factors embedded in health policy and suggests strategies to account for them through attention to context, mechanisms, and outcomes21. A realist approach was deemed most suitable for the contextually embedded health services issue of decentralized perinatal surgical services, of which satisfaction and sustainability are key attributes.
The RAMESES quality standard for realist reviews guided application of the methodology20 with the present study meeting an excellent standard by most criteria (ie feasible topic, appropriately structured question, understanding and application of realist philosophy, rigor of appraisal process).
The larger study
The larger study responded to the question jointly constructed between review commissioners and the research team:
Can the perinatal surgical needs of rural women be met more effectively through an optimally centralized or optimally decentralized model of care?
The larger review examined issues related to the optimal level of (de)centralization in the BC context by operationalizing the concept to include issues of safety, sustainability, and cost-effectiveness of surgical services for rural women. Findings suggest that centralized models of perinatal surgical care were assumed safe, sustainable, satisfactory, and cost effective. The burden of proof of safety and efficacy was borne by services that deviated from this model, such as rurally distributed services. This has resulted in studies using centralized care as a benchmark in evaluation and comparison. Scant research attention was paid to rural maternity care prior to 1990 in developed nations and technological and social changes for both the patient (eg lower costs of travel) and the system (eg an increasing role for specialists) strained contextual comparison beyond 25 years. However, these limitations are in keeping with a realist tradition in which the relevance of the data to the phenomenon under consideration is paramount.
Findings from the larger study have demonstrated the relative safety of decentralized models of perinatal surgical services within the context of supported care providers and efficient transport17. The literature directly referencing interrelated concepts of sustainability, provider satisfaction, and client or patient satisfaction of rural maternal surgical care is the focus of the present article.
Inclusion criteria
A wide variety of plausible issues, relevant to the centralization of maternal surgical care, were captured by an intentionally broad primary search structure. While search terms were intended to maximize sensitivity, search limiters were used on language (English) and year (1990), in keeping with a rapid review tradition as well as a realist review approach. MEDLINE, PubMed, EMBASE, CINAHL, EBM Reviews, NHS Economic Evaluation Database, and PAIS International for literature were searched. Keywords associated to each search area as well as the reasoning behind the search strategy are summarized in Table 1.
Database searching resulted in 2049 total resources, of which 735 were duplicate records across different databases. Manual abstract exclusion eliminated a further 1060 as from developing settings (n=699) or irrelevant (n=361) (Fig1). Of the remaining 254 resources, 192 were included for full article review after literature on best practice evidence for specific conditions (eg HIV, pre-eclampsia or diabetes) (n=27), and on defensive medicine and litigation concerns (n=35) were excluded.
Inclusion criteria at the full article review stage included direct discussion of maternal surgical care, including but not limited to safety of practice models, governance of care models, and sustainability of service delivery; and consideration of the relative centralization of care modeling (intentional and non-intentional), including but not limited to centralization of decision making, ways of incorporating specialist care, and optimal geography and/or level of service delivery. Of the 192 articles under full article review, 84 were excluded based on these criteria. Seven resources could not be obtained through the authors' resources by the report deadline for full article review. A further 59 resources were added through pearling and 13 grey literature reports were added on recommendation from the commissioners. Of the total 175 resources included in the full realist review, 42 were included on the subject of satisfaction and sustainability specifically and are included in this article (Fig1).
Although literature from low-resource settings was excluded from this review, all other jurisdictions were considered. Those that were deemed most relevant to the BC context included Scotland, the United Kingdom, Norway, Finland, Sweden, the Netherlands, Germany, New Zealand, the USA, Australia, and the rest of Canada.
The majority of studies found through this review were descriptive in nature, either through case studies and reviews or practice-based outcomes. When considered together and in the broader context of international rural maternity care, the similarities in the findings indicate a good strength of evidence. Finally, a few thoughtful editorials were included and considered in the case the author(s) spoke directly to the subject area, and several grey literature reports were found with the help of policy and service programming experts in both Canada and Australia.
Table 1: Key words associated to primary search areas, and reasoning for inclusion
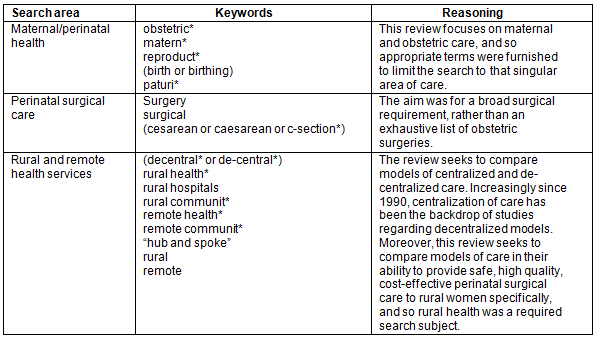
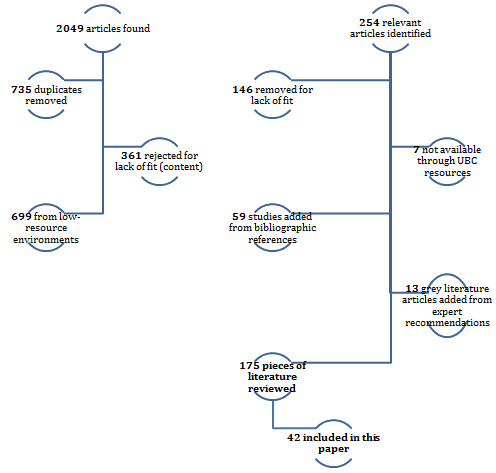
Figure 1: Inclusion and exclusion screening stages to identify literature.
Ethics approval
Ethical review was not sought for this study as it involved no human participants and involved only a secondary analysis of data.
Procedural or surgical care was found to directly influence rural providers' satisfaction and has been named as the lynchpin of sustainability22,23, guarding against a cascading loss of practitioners and the services they provide. Findings are grouped into the following themes: workforce issues (shortage of providers and challenges with recruitment and retention), educational programs (the role of exposure to rural practice and access to continuing medical education), and workforce training and case mix (the nuances of rural practice compared to urban and how these nuances can be approached in medical education). While provider satisfaction is a subject throughout these findings, the essential relationship between procedural practice and contextual support is addressed by the theme of 'provider satisfaction with practice'. The broader scope of rural practice and what it means for performing procedures inconsistently or intermittently is considered under the theme of 'practice thresholds'. Each of these themes is explicated below.
Workforce: shortage of providers
The reality of the declining rural workforce was common to all jurisdictions covered in this review24 including Canada25 and the USA26-29. The shortage in general surgeons is pointed to specifically in research from the USA27-29. Additionally, maldistribution of providers weighted towards over-representation in larger urban centres at the cost of smaller rural settings was reported as challenging by several jurisdictions22,23,29-34. This process is predicted to intensify with further centralization, leading to rural patients facing the greatest surgeon shortages and distance to care35.
Effective patient care is undermined by the attrition of services. In a study by Larimore and Davis36 it was found that the availability of perinatal surgical care in rural Florida accounted for 17.6% of variation in the rate of infant mortality. The mathematical model that measured impact of service availability predicted that the loss of a single family physician performing maternal care in a rural county would account for a 2.3% increase in infant mortality in that county, and the loss of an obstetrician/gynecologist would account for a 9.6% increase. Similar variations have been observed in other jurisdictions37.
Workforce: recruitment and retention of rural providers
In an effort to understand how to recruit and retain more general surgeons into rural practice, one study attempted to determine motivations for practice location and found that rural providers were less motivated than urban providers by income, professional growth, availability of hospital facilities, quality of surgical community, and quality of medical community38. Rural providers were, however, motivated equally by quality of life. Conclusions stated that exposure to rural areas may have improved the opinions of graduates about the quality of life in rural settings and led them to choose a rural path.
A qualitative study of the training experiences of GP surgeons in BC and Alberta conducted by Kornelsen et al identified further motivations for rural practice, including the desire to respond to community needs, enhance professional competence, and gain personal satisfaction39. These findings are congruent with a study done with 22 rural GPs in California and Nevada40. Positive predictors of rural practice were familiarity, sense of place, community involvement, and self-actualization. A focus on retention that built specifically on these themes would effectively improve recruitment as well, raising the standard of living and making interactions with rural practice more positive. Exposure to rural environments as brief as summer camps, recreational activities, and rural service projects were found to impact choice of practice location40.
The Australian Rural Clinical School initiative has sought to increase exposure to rural environments and research through more general and rural practice placements in medical schools, financial incentives for graduates to move into rural practice, and regionalized Australian General Practice Training for specific geographic health systems41. Taken together, these strategies led to increases in the number of rural GPs41. However, findings indicate that only 29% of rural pathway graduates have remained in rural practice upon graduation and the number of rural pathway registrants entering surgical obstetric training remains insufficient to meet the current needs of rural communities.
A qualitative study42 considering the motivations of 70 GPs practicing obstetric, surgical, or anesthetic procedures in the Bogong region of Australia distinguished between the motivations for choosing rural practice and the reasons for staying with rural practice from an administrative perspective. Lifestyle, cultural fit, spousal employment, secondary schooling options and a sense of belonging were reasons stated as being important to GP attraction to rural general practice. However, it was the diversity and challenge of general and procedural medicine that both attracted and kept GPs in rural settings42.
Educational programs
Educational programs are a viable means of attracting GPs to rural practice through exposure, although predictors of long-term program success are limited in the literature, perhaps because the initiatives are somewhat new or simply understudied. A study by Eley et al43 found that only 40% of graduates from the Australian Rural Clinical School initiative were in rural practice between 2 and 9 years after their graduation. Surgical educational programs with a rural component report higher rates of graduates taking up rural practice, general practice, and primary care practice40,43-45. Further examples include a study by Crump et al, which found that practitioners who graduated from a rural program in Kentucky were more likely to stay in Kentucky upon graduation, work in a rural setting, and choose general practice45. A study by Anderson found that a rural program near Buffalo, New York, attracted faculty physicians and improved access to and quality of care in the area immediately, even though the goal of the program was to train rural practitioners for long-term workforce replenishment44. These positive indicators confirm existing recruitment strategies based on the belief that those from rural backgrounds are more likely to practice there, and those with positive experiences in rural communities are similarly more inclined to work there43.
With the recognition that generalists often fill care gaps in rural communities, research by Campbell et al argues that rural training should be more expansive than a single list of procedural competencies - general surgeons should be trained to meet community needs not met by regional specialists46. This argument is supported in research by Pollett and Harris47.
Continuing medical education was noted to be important, although upgrading skills as a rural provider is not straightforward. Work by Glazebrook and Harrison identified barriers including lack of training opportunities, lack of locum relief, and the distance to training48. Additionally, the costs associated with maintaining procedural skills were identified as a deterrent, underscoring the need to bring continuing medical education to rural providers.
Workforce: training and case mix
Education programs that increase exposure for the strategic aim of recruitment and retention also need to be tailored to train practitioners for the nuances of rural practice. There is an acceptance in the descriptive literature from all jurisdictions in this review that rural providers have a broader case mix than their urban or semi-rural colleagues45,49-57.
Specific to perinatal surgical care, 90% of Iowa's rural general surgeons report routinely doing C-sections52, while just 11% of non-rural general surgeons reported the same. In rural Western Australia in the mid-1990s, 62% of GPs reported providing obstetrical care, and 46% had performed a C-section in the previous year58. Similar rates of C-section participation were found in the rural areas of southern Australia (43%)59 and in the Australia state of New South Wales (41%)60. In a study of family practice graduates in Alberta from 1985 to 1995 it was found that 78% of those practicing in rural areas performed deliveries, compared to just 53% of graduates in metropolitan practice61. As well, 11% were performing C-sections in those rural areas, versus just 1.8% in metropolitan areas. Caseload and case mix, as well as referral patterns of rural GPs, were found to depend partly on the proximity and availability of local specialists62,63 .
Provider satisfaction with practice
The cornerstone of rural provider satisfaction appears to rest in the ability to practice to the full extent of generalist procedural scope within a broad case mix. When not properly supported, however, this extended role can also lead to frustration and the sense of vulnerability from being 'in too deep'. In a survey of rural and urban general surgeons in the USA it was found rural providers had lower satisfaction with specialist support, access to technology, recruiting and retaining assistants, vacation, and on-call schedules38. A study by Humphreys et al examined the retention of rural providers in Australia and found similar satisfaction concerns64. However, the variety of their work, including procedural care, was found to be the recurring reason given by rural GPs regarding their choice to practice rurally.
These findings were reinforced in an editorial by Darrell Baker about the challenges and rewards of rural surgical practice in Canada65. Lack of contact with colleagues, difficulty accessing consultants and specialists in emergencies, poor locum coverage, long on-call hours, distant continued medical education, and lifestyle issues are all listed as serious problems. 'So, why would anyone want to be a rural surgeon in Canada?' Baker asks. 'The rewards far outweigh all of the drawbacks. The sincere gratitude of the patients, the exciting variety of the caseload, financial incentives, and the camaraderie of the staff of a small hospital are just a few of the things that make it all worthwhile (p. 1632)'65. Likewise, in a study of rural general surgical practice in British Columbia by Humber and Iglesias it was found that the variety of caseload is a key part of satisfaction among rural providers66, reinforcing the planning principal of using providers to their broadest scope of practice.
Practitioners who also experienced diminishing local resources, both infrastructural and human resources, reported feeling extended beyond a usual scope of practice22. In a survey of rural GPs in New South Wales, Australia, it was found that they valued procedural work such that closure of surgical facilities may lead them to leave rural areas67.
Practice thresholds
A small set of research was found that attempted to examine the role of procedural volume in maintaining competency and/or comfort. In a study of 167 GPs practicing obstetrics in southern Australia, it was found that the 'self-reported comfort with obstetrics' was 7.46 on a 10 cm visual analogue scale59. Comfort was correlated significantly with length of obstetric training and number of deliveries per year. The study reports that those with more than 12 months training were more confident, and those who had conducted fewer than 10 deliveries annually were less comfortable. Number of years of experience had no correlation with comfort.
The practice threshold number found in a study by Watts et al59, although low, was not found in a study by Norris et al68 of 86 rural GPs practicing obstetrics (including C-section) in Washington State. Instead, it was found that comfort with procedures was based on the number of procedures performed in residency and not on number of deliveries during practice68.
A study by Tucker et al found there was a confound between competency and comfort69. Interviews with a purposive, representative sample of rural maternity providers in Scotland (n=70) were supplemented with a survey (n=125), for which 42% of respondents agreed with the statement, 'it's like riding a bicycle - once you have delivered babies, you don't forget how'. Asked specifically about how many births per year were required for a competency threshold, answers varied wildly and were frequently left blank. One respondent (questionnaire open comment, midwife 0081, p. 37) wrote, 'I find number of cases difficult to answer. It would depend on your previous experience and additional training'69.
No other direct evidence was found regarding thresholds of care to maintain competency; in each study cited, obstetrically specific medical school and residency training was essential for GPs to feel confident providing obstetric care.
There is clear evidence on the merits of rural practice as a site to actualize personal goals and values by participating in community level health improvement to a broad scope of practice. This is juxtaposed, however, with feelings of being 'in too deep' due to lack of redundancies in health human resources, compromised access to specialist support and technology and lifestyle needs (locum relief and manageable on-call schedules). Compromised satisfaction with practice is directly linked with higher levels of burn-out and attrition, making urgent the need to address conditions that impede sustainability.
The body of literature on the satisfaction and sustainability of rural perinatal surgical services focuses primarily on the challenges incurred in providing such services, particularly in the face of diminishing system support. This is a reflection of the system assumptions towards centralized care and the lack of evaluation of this model from the perspective of rural women and care providers. Although the growing international attention to sustaining rural health services may be motivated in part by the crisis in providing equitable access for rural residents, a by-product has been the nascent attention given to rural health and emerging efforts towards understanding the preconditions to sustainability.
Consistent throughout much of the literature on sustainability, studies identified perinatal surgical services as the lynchpin for robust rural health services, one of the attributes differentiating rural from urban services. The recognition of different levels of care patterns is crucial for administrative and decision-making bodies, to prevent incidental centralization. The antidote is to privilege the experience of rural communities in health services planning.
Acknowledgements
The authors would like to gratefully acknowledge support from the Michael Smith Foundation for Health Research and the editorial expertise of Lana Newton.
References
1. Allen VM, Jilwah N, Joseph KS, Dodds L, O'Connell CM, Luther ER et al. The influence of hospital closures in Nova Scotia on perinatal outcomes. Journal of Obstetrics and Gynaecology Canada 2004; 26: 1077-1085.
2. Hutten-Czapski P. Decline of obstetrical services in northern Ontario. Canadian Journal of Rural Medicine 1994; 4(2): 72-76.
3. Hutten-Czapski P. Abridged version of the Society of Rural Physicians of Canada's discussion paper on rural hospital service closures. Canadian Journal of Rural Medicine 2009; 14(3): 111-114.
4. Mungall IJ 2005. Trend towards centralisation of hospital services, and its effect on access to care for rural and remote communities in the UK. Rural and Remote Health (Internet) 2005; 5: 390. Available: www.rrh.org.au (Accessed 9 December 2013).
5. Rourke JTB. Trends in small hospital obstetrical services in Ontario. Canadian Family Physician 1998; 44: 2117-2124.
6. Grzybowski S, Stoll K, Kornelsen J. The outcomes of perinatal surgical services in rural British Columbia: a population-based study. Canadian Journal of Rural Medicine 2013; 18(4): 123-129.
7. British Columbia Ministry of Health. Rural health services in BC: a policy framework to provide a system of quality care. Vancouver, BC: British Columbia Ministry of Health, 2015.
8. Applied Policy Research Unit. Optimal perinatal surgical services for rural women: a realist review. Vancouver, BC: Applied Policy Research Unit, 2014.
9. Miller KJ, Couchie C, Ehman W, Graves L, Grzybowski S, Medves J. Rural maternity care. Journal of Obstetrics and Gynaecology Canada 2012; 34(10): 984-991.
10. BC Perinatal Database Registry. British Columbia deliveries by maternal residence and delivery hospital highest level of service/care. Vancouver, BC: BC Reproductive Care Program, 2000-2007.
11. Grzybowski S, Stoll K, Kornelsen J. Distance matters: a population based study examining access to maternity services for rural women. BMC Health Services Research 2011; 11: 147.
12. Nesbitt TS, Larson EH, Rosenblatt RA, Hart LG. Access to maternity care in rural Washington: its effect on neonatal outcomes and resource use. American Journal of Public Health 1997; 87(1): 85-90.
13. Nesbitt TS, Connell FA, Hart LG, Rosenblatt RA. Access to obstetric care in rural areas: effect on birth outcomes. American Journal of Public Health 1990; 80(7): 814-818.
14. Harris SJ, Janssen PA, Saxell L, Carty EA, MacRae GS, Petersen KL. Effect of a collaborative interdisciplinary maternity care program on perinatal outcomes. Canadian Medical Association Journal 2012; 184(7): 1885-1892.
15. Kildea S, Stratigos S. Rural birth index for Australia? The Australian Journal of Rural Health 2010; 18(2): 85-86.
16. Lynge DC, Larson EH, Thompson MJ, Rosenblatt R, Hart LG. A longitudinal analysis of the general surgery workforce in the United States, 1981-2005. Archives of Surgery 2008; 143(4): 345-350.
17. Kornelsen JK, McCartney K, Williams K. Centralized or decentralized perinatal surgical care for rural women: a realist review of evidence on safety. BMC Health Services Research 2016 (in press).
18. British Columbia Royal Commission on Health Care and Costs. Closer to home: the report of the British Columbia Royal Commission on Health Care and Costs. Victoria, BC: British Columbia Royal Commission on Health Care and Costs, 1991.
19. BC Ministry of Health Services. Standards of accessibility and guidelines for provision of sustainable acute care services by health authorities. Victoria, BC: BC Ministry of Health Services, 2002.
20. Wong G, Greenhalgh T, Westhorp G, Buckingham J, Pawson R. RAMESES publication standards: realist syntheses. BMC Medicine 2013; 11(1): 21.
21. Pawson R, Greenhalgh T, Harvey G, Walshe K. Realist review - a new method of systematic review designed for complex policy interventions. Journal of Health Services Research Policy 2005; 10(1): 21-34.
22. Swayne A, Eley DS. Synergy and sustainability in rural procedural medicine: views from the coalface. Australian Journal of Rural Health 2010; 18(1): 38-42.
23. Klein MC, Christilaw J, Johnston S. Loss of maternity care: the cascade of unforeseen dangers. Canadian Journal of Rural Medicine 2002; 7(2): 120-121.
24. Chiasson PM, Roy PD. Role of the general practitioner in the delivery of surgical and anesthesia services in rural western Canada. Canadian Medical Association Journal 1995; 153(10): 1447-1452.
25. Roos N, Black C, Wade J, Decker K. How many general surgeons do you need in rural areas? Three approaches to physician resource planning in southern Manitoba. Canadian Medical Association Journal 1996; 155(4): 395-400.
26. MacDowell M, Glasser M, Fitts M, Nielsen K, Hunsaker M. A national view of rural health workforce issues in the USA. Rural and Remote Health (Internet) 2010; 10(3): 1531. Available: www.rrh.org.au (Accessed 9 December 2013).
27. Heneghan SJ, Bordley J, Dietz P, Gold MS, Jenkins PL, Zuckerman RJ. Comparison of urban and rural general surgeons: motivations for practice location, practice patterns, and education requirements. Journal of the American College of Surgeons 2005; 201(5): 732-736.
28. Lynge DC, Larson EH. Workforce issues in rural surgery. Surgical Clinics of North America 2009; 89(6): 1285-1291.
29. Inglis F. Surgical care in rural Canada: training and planning for the future - editorial. Canadian Medical Association Journal 1995; 153(10): 1453-1454.
30. Belsky D, Ricketts T, Poley S, Gaul K, Fraher E, Sheldon G. Surgical deserts in the US: places without surgeons. (Internet) 2009. Available: http://www.acshpri.org/documents/ACSHPRI_FS2.pdf (Accessed 9 December 2013).
31. Humber N, Frecker T. Delivery models of rural surgical services in British Columbia (1996-2005): are general practitioner-surgeons still part of the picture? Canadian Journal of Surgery 2008; 51(3): 173-178.
32. Williams TE, Ellison EC. Population analysis predicts a future critical shortage of general surgeons. Surgery 2008; 144(4): 548-554.
33. Borgstrom DC, Heneghan SJ. Bassett Healthcare rural surgery experience. Surgical Clinics of North America 2009; 89(6): 1321.
34. Williams Jr. TE, Satiani B, Ellison EC. A comparison of future recruitment needs in urban and rural hospitals: the rural imperative. Surgery 2011; 150(4): 617-625.
35. Thompson MJ, Lynge DC, Larson EH, Tachawachira P, Hart LG. Characterizing the general surgery workforce in rural America. Archives of Surgery 2005; 140(1): 74-79.
36. Larimore WL, Davis A. Relation of infant mortality to the availability of maternity care in rural Florida. Journal of the American Board of Family Practice 1991; 8(5): 392-399.
37. Allen DI, Kamradt JM. Relationship of infant mortality to the availability of obstetrical care in Indiana. Journal of Family Practice 1991; 33(6): 609.
38. Heneghan SJ, Bordley J, Dietz P, Gold MS, Jenkins PL, Zuckerman RJ. Comparison of urban and rural general surgeons: motivations for practice location, practice patterns, and education requirements. Journal of the American College of Surgeons 2005; 201(5): 732-736.
39. Kornelsen J, Iglesias S, Humber N, Caron N, Grzybowski S. GP surgeons' experiences of training in British Columbia and Alberta: a case study of enhanced skills for rural primary care providers. Canadian Medical Education Journal 2012; 3(1): 33-41.
40. Hancock C, Steinbach A, Nesbitt TS, Adler SR, Auerswald CL. Why doctors choose small towns: a developmental model of rural physician recruitment and retention. Social Sciences and Medicine 2009; 69(9): 1368-1376.
41. Campbell DG, Greacen JH, Giddings PH, Skinner LP. Regionalisation of general practice training: are we meeting the needs of rural Australia? Medical Journal of Australia 2011; 194(11): S71:S74.
42. Robinson M, Slaney GM, Jones GI, Robinson JB. GP proceduralists: "the hidden heart" of rural and regional health in Australia. Rural and Remote Health (Internet) 2010; 10(3): 1402. Available: www.rrh.org.au (Accessed 9 December 2013).
43. Eley DS, Synnott R, Baker PG, Chater AB. A decade of Australian rural clinical school graduates -where are they and why? Rural and Remote Health (Internet) 2012; 12: 1937. Available: www.rrh.org.au (Accessed 9 December 2013).
44. Anderson G. The effect of a rural track residency program with an emphasis on obstetrics on physician shortage areas. Journal of Rural Health 2000; 16(3): 230-231.
45. Crump WJ, Fricker RS, Ziegler C, Wiegman DL, Rowland ML. Rural track training based at a small regional campus: equivalency of training, residency choice, and practice location of graduates. Academic Medicine 2013; 88(8): 1122-1128.
46. Campbell NA, Kitchen G, Campbell IA. Operative experience of general surgeons in a rural hospital. Australia New Zealand Journal of Surgery 2011; 81(9): 601-603.
47. Pollett W, Harris K. The future of rural surgical care in Canada: a time for action. Canadian Journal of Surgery 2002; 45(2): 88-89.
48. Glazebrook RM, Harrison SL. Obstacles and solutions to maintenance of advanced procedural skills for rural and remote medical practitioners in Australia. Journal of Rural Health 2006; 6(4): 502.
49. Buck ST, Trauba V, Christensen RG. Minnesota physician workforce analysis: rural supply and demand. Minnesota Medicine 2004; 87(9): 40-43.
50. Glasser M, Peters K, Macdowell M. Rural Illinois hospital chief executive officers' perceptions of provider shortages and issues in rural recruitment and retention. Journal of Rural Health 2006; 22(1): 59-62.
51. Callaghan J. A twenty-five year survey of a solo practice in rural surgical care. Journal of the American College of Surgeons 1994; 178(5): 459-465.
52. Breon TA, Scott-Conner CEH, Tracy RD. Spectrum of general surgery in rural Iowa. Current Surgery 2003; 60(1): 94-99.
53. Baker E, Schmitz D, Epperly T, Nukui A, Miller CM. Rural Idaho family physicians' scope of practice. Journal of Rural Health 2010; 26(1): 85-89.
54. Buser KB. Laparoscopic surgery in the pregnant patient: results and recommendations. Journal of the Society of Laparoendoscopic Surgeons 2009; 13(1): 32-33.
55. Buser KB. Laparoscopic surgery in the pregnant patient - one surgeon's experience in a small rural hospital. Journal of the Society of Laparoendoscopic Surgeons 2002; 6(2): 121-124.
56. MacDowell M, Glasser M, Fitts M, Fratzke M, Peters K. Perspectives on rural health workforce issues: Illinois-Arkansas comparison. Journal of Rural Health 2009; 25(2): 135-140.
57. Smith DW, Murphy NJ. Alaska's obstetrical delivery systems: a descriptive epidemiologic study. Alaska Medicine 2000; 42(3): 78-84.
58. Welch R, Power R. General practitioner obstetric practice in rural and remote Western Australia. Australia New Zealand Journal of Obstetrics and Gynaecology 1995; 35(3): 241-244.
59. Watts RW, Marley JE, Beilby JJ, MacKinnon RP, Doughty S. Training, skills and approach to high-risk obstetrics in rural GP obstetricians. Australia New Zealand Journal of Obstetrics and Gynaecology 1997; 37(4): 424-426.
60. Woollard LA, Hays RB. Rural obstetrics in NSW. Australia New Zealand Journal of Obstetrics and Gynaecology 1993; 33(3): 240-242.
61. Chaytors RG, Szafran O, Crutcher RA. Rural-urban and gender differences in procedures performed by family practice residency graduates. Family Medicine 2001; 33(10): 766-771.
62. Tulloh B, Clifforth S, Miller I. Caseload in rural general surgical practice and implications for training. Australia New Zealand Journal of Surgery 2001; 71(4): 215-217.
63. Gruen RL, Knox S, Britt H. Where there is no surgeon: the effect of specialist proximity on general practitioners' referral rates. Medical Journal of Australia 2002; 177(2): 111-115.
64. Humphreys JS, Jones MP, Jones J, Mara PR. Workforce retention in rural and remote Australia: determining the factors that influence length of practice. Medical Journal of Australia 2002; 176(10): 472-476.
65. Baker DK. Rural surgery in Canada. World Journal of Surgery 2006; 30(9): 1632-1633.
66. Humber N, Iglesias S. Position paper on training for family physicians in general surgery. Shawville, Quebec: Society of Rural Physicians of Canada, 1999.
67. Alexander C. Why doctors would stay in rural practice in the New England health area of New South Wales. Australia Journal of Rural Health 1998; 6(3): 136-139.
68. Norris TE, Reese JW, Pirani MJ, Rosenblatt RA. Are rural family physicians comfortable performing cesarean sections? Journal of Family Practice 1996; 43(5): 455-460.
69. Tucker J, Hundley V, Kiger A, Bryers H, Caldow J, Farmer J, et al. Sustainable maternity services in remote and rural Scotland? A qualitative survey of staff views on required skills, competencies and training. Quality Safety Health Care 2005; 14(1): 34-40.



