full article:
An estimated 1.66 million Americans were diagnosed with cancer in 2015, with 5-year relative survival rates approaching 70%1. Improved survival has resulted in a growing number of survivors who must learn to cope with long-term physical and psychosocial sequelae that negatively impact their quality of life2-4. There has been increasing recognition that psychosocial support programs can play a key role in cancer survivorship care5-7 and there is significant interest in identifying ways to improve access to psychosocial care for cancer survivors, particularly for survivors who reside in rural areas8,9.
A structured, group cognitive-behavioral stress management (CBSM) intervention has been demonstrated to be effective in improving mood and quality of life in multiple cancer populations10,11. There has been increasing interest in the delivery of interventions utilizing technology in order to improve psychosocial outcomes in cancer survivors12. One of the mechanisms that has received recent attention has been the use of telehealth mechanisms, including videoconferencing, to address treatment access issues13. At our cancer center, a videoconference-based remote access educational program was developed to improve access and overcome geographic barriers to participation. This adapted CBSM14 educational program delivered by individual computer tablets loaned to participants was piloted to assess the feasibility of this novel remote access methodology.
Participants in the program were adult cancer survivors (age ≥18 years) who were not having active cancer therapy and were interested to learn how to manage stress were invited to participate in a group program. Flyers for the program were distributed in patient common areas at the main cancer center site (Dana-Farber Cancer Institute, Boston, MA) and two affiliated satellite sites (South Weymouth, MA and Londonderry, NH). To encourage within-group discussion of those diagnosed with a similar disease, three separate groups for those diagnosed with breast, prostate, and blood cancers respectively were held.
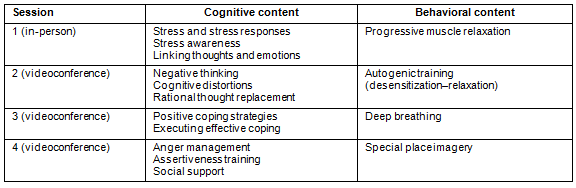
The educational program comprised four 60-minute weekly group sessions focused on the management of cognitive factors that impact stress, and the practice of relaxation exercises. All session content (Table 1) was adapted from a standardized, 10-session, in-person CBSM intervention that has demonstrated efficacy in people with cancer14. The abbreviated group program was supplemented by an ebook developed specifically for the standardized CBSM intervention. The ebook contained program-related homework and practice exercises intended to accompany each session and encouraged to be utilized by participants between sessions15.
Participants attended the first session in person at the site where they were recruited (main cancer center or two satellite sites) and were provided with a loaner tablet (iPad) and oriented to the videoconference software (Cisco WebEx) use. At the two satellite locations, staff nurses who were previously trained in tablet and software use helped to connect participants remotely to the in-person session that was being held at the main cancer center. All subsequent program sessions were conducted fully using tablet videoconference, with homework assigned in the ebook for the period in between sessions. On the day before each session, a study staff member contacted every participant individually and conducted a connection trial to ensure that they were able to successfully log in to the videoconference.
Prior to program enrollment, all participants spoke with a program facilitator by telephone. During this call, participants were asked to report the duration of their commute to the cancer center, and whether not needing to commute to program sessions had influenced their interest in enrollment in the program. Following the last program session, participants were asked to respond in writing to an open-ended query regarding what they liked and disliked about the program. Information provided during the initial telephone call and in response to the open-ended question regarding program feedback was reviewed for common themes.
In addition, all participants were asked to complete the Perceived Stress Scale (PSS), a 14-item measure assessing levels of perceived stress16, in person before the first session and by mail after the last session. The total score for the PSS was used in study analyses, with higher scores indicating more perceived stress. To evaluate the impact of the intervention on perceived stress, pre- and post-intervention scores were compared using paired-samples t-tests.
Ethics approval
The study was approved by the Dana-Farber Cancer Institute's Institutional Review Board (Protocol #14-131) and all participants signed informed consent documents allowing use of their information in research.
Table 1: Cognitive-behavioral stress management intervention pilot: session content
There are prominent barriers to the dissemination of evidence-based psychosocial interventions in oncology populations, such as the CBSM approach we utilized. This is a particularly salient issue for those residing in rural areas17. In the USA, an estimated 85.5 million Americans must travel for more than 1 hour to reach the nearest academic medical center providing cancer care18. Many evidence-based psychosocial interventions are offered at these centers, often as part of research studies, so there is a need to improve accessibility for patients with such geographic barriers to participation5.
In this pilot program, a total of 16 cancer survivors enrolled across the three groups, with 14 completing all program sessions. The two survivors who withdrew from the program both did so after the first session, indicating that they had scheduling conflicts for subsequent sessions. Findings from the 14 participants who completed all program sessions are reported on here. They were 24-70 years of age (mean=53.1; standard deviation=14.0), and a majority were women (64.3%). The participant's diagnoses were: breast (n=5), prostate (n=5), and blood (n=4) cancers.
Participants resided in four different states (Massachusetts, Rhode Island, New Hampshire, and Maine) of the New England region in north-eastern USA, and 10 of the 14 survivors who completed the program stated that not having to attend multiple program sessions in person at the cancer center played a role in their initial interest in enrolling in the intervention. Five survivors indicated that they preferred participation by videoconference instead of having to commute to their local cancer center for psychosocial support, indicative of the fact that all but one participant reported that their commute to the closest cancer center would take at least 30 minutes. Three survivors mentioned that avoiding traffic going to/from group sessions was helpful.
Qualitative program feedback, based on the open-ended question post-intervention, was positive. Ten of the 14 participants reported that they found the program to be helpful overall, and eight reported that the program content was well suited to improving psychosocial distress. Notably, five survivors stated that they found the session facilitator to be effective at communicating stress management and relaxation techniques, despite the use of a novel videoconference delivery method.
Study participants reported experiencing treatment-related barriers including difficulties with developing a connection to other group participants during the videoconference sessions, an inability to focus on content when it was presented using videoconference, and technical difficulties that impacted their ability to follow intervention content (eg wireless connectivity disruptions). In total, 6 of the 14 participants indicated that some aspect of videoconference delivery had negatively impacted their intervention experience. In addition, four participants indicated that the program duration was too brief, desiring an expanded program to better discuss the material.
Pre-post measures analysis revealed only modest improvements in perceived stress, which did not reach statistical significance: PSS total score changed from 32.6 at baseline (range 23-44) to 32.1 post-intervention (range 27-38; p=0.49).
The challenges reported by participants, coupled with a lack of statistically significant improvements in perceived stress, indicate that there are dissemination specific issues that must be addressed in future efforts. The experience with the development and delivery of this program is discussed, with a particular focus on program planning and delivery challenges experienced, and participant concerns with their intervention experience.
A CBSM educational program delivered by group-based videoconference on a tablet was piloted at a comprehensive cancer center. The lessons learned from the experiences during this pilot should contribute to recent efforts to better understand the challenges in the implementation of telehealth interventions19 and be instructive for future researchers and clinicians wishing to implement a similar model for providing psychosocial programming.
The delivery of the CBSM educational program was feasible and acceptable for the majority of participants, suggesting that some access barriers can be overcome using technology. Many participants indicated that not having to return to the cancer center for in-person intervention sessions was important. This is of consequence for regional cancer centers, including the site where this research was conducted, as it provides clinical services for patients across several New England states. Extensive travel to receive non-emergency, psychosocial services is often not desirable for patients. In cancer populations, a literature review concluded that increased travel distance for cancer treatment is not only inconvenient, but also a 'practical hardship' for many patients and can be perceived as a significant barrier to treatment20. In this pilot, which recruited patients who lived relatively long distances from the main cancer center, removal of the commute for support was clearly appreciated. There is a continuing need to improving access to psychosocial care following treatment for survivors21, and addressing travel challenges is an important consideration.
Although program feedback was generally positive, participant reports of improvements in their level of perceived stress were not statistically significant. This is hypothesized to be the result of an insufficient intervention dose (four sessions, compared to 10 sessions in the standard CBSM approach) coupled with challenges that were experienced due to the novel intervention delivery method. The cautionary feedback provided by participants included not feeling connected with other group participants through the videoconference, and struggling to focus on session content because they were more easily distracted. In addition, participants reported struggles with both their hardware and software. Although evidence suggests that the delivery of mental health care using telehealth can be effective, it may be that having in-person connections developed during the course of care delivery is important in facilitating patient-to-patient connections within the group, and between patients and the provider22,23.
Facilitator experiences in the delivery of a group-based videoconference intervention involved a steep learning curve. Future efforts to deliver programs using group-based videoconference should consider several key issues during the preparation and implementation stages.
Program preparation
- There are a variety of available software packages allowing group videoconferencing, each with unique attributes and drawbacks that require careful consideration. It is feasible to consider a range of options, including Google Hangouts, Skype, Apple FaceTime, Adobe Connect, Fuze, Zoom, and GoToMeeting. Ultimately, Cisco WebEx was selected for this research based on the size of the groups (four to six participants), its compatibility with iPad hardware, ease of incorporating presentation content, and ease of participant use. An online compendium of other web conferencing software packages is available at https://en.wikipedia.org/wiki/Comparison_of_web_conferencing_software. However, facilitators should be aware of the 'arms race' of technology, and the rate at which software packages become obsolete24.
- For hardware, all participants were loaned the same tablet device (an iPad). This ensured that all participants were on the same hardware platform, and that any troubleshooting that would need to occur could be done with a 'clean' device that had been formatted and prepared for use by study staff. In addition, the iPad was chosen because of its popularity and the belief that potential personal familiarity with the device would help to reduce the Cisco WebEx videoconference software learning curve for participants. The use of netbooks, laptops, and desktop computers was considered, but the complexity of setting up webcams and multiple software configurations across different devices was a concern.
Program implementation
- Before the first videoconference session, facilitators are strongly encouraged to conduct a trial connection with each participant to ensure that all technical concerns and enquiries are proactively addressed. In this study, a trial session was conducted the day before the group session because this allowed sufficient time to address in-home problems such as those with wireless connectivity and software problems.
- It is valuable to have an additional staff member present throughout the group sessions, supporting the facilitator. This individual can address any new onset technical issues that develop over the course of the group session, which will minimize distraction for the remaining group members. Examples of challenges that were experienced in the middle of group sessions included audio interference with other electronic devices in the participant's home, improper lighting conditions for videoconferencing, software failure, and connectivity issues.
- Purchasing headphones/earphones with a microphone built in and providing these to group participants should be considered. This simple addition to the program helped to minimize the impact of disruptive loud noises in participant's homes and improved audio clarity for the group conversations.
- Specific efforts need to be directed towards connecting group participants with one another and engaging participants in content during the session. For example, if videoconference software allows for private messaging during the group (as Cisco WebEx allows), the presence of a second group facilitator responsible for sending direct messages to check in on participant status, or to ask and answer specific questions about session content could be helpful towards engaging participants in session content.
- Facilitating group-based communication between sessions can also be considered to encourage connections between program participants. This can be accomplished by using, for example, group emails, a web forum, social networking websites, or group text messaging.
Although challenges were encountered in efforts to implement a group videoconference program, the feedback from participants indicated that they believed this delivery mechanism offered a support opportunity that they would otherwise not have been able to engage in. The study groups comprised adult survivors across a range of ages and common cancer diagnoses, which begins to capture the wide range of patients that cancer survivorship programs across the country provide care for, and who are interested in stress management. The use of videoconference and other telehealth delivery mechanisms will play an increasingly important role as cancer centers seek to support their geographically dispersed patient populations, and this discussion highlights both the promise and the challenges of such efforts.
References
1. American Cancer Society. Cancer facts and figures. Atlanta, GA: American Cancer Society, 2015.
2. Alfano CM, Rowland JH. Recovery issues in cancer survivorship: a new challenge for supportive care. Cancer Journal 2006; 12(5): 432-443.
3. Zhou ES, Penedo FJ, Bustillo NE, Benedict C, Rasheed M, Lechner S, et al. Longitudinal effects of social support and adaptive coping on the emotional well-being of survivors of localized prostate cancer. Journal of Supportive Oncology 2010; 8(5): 196-201.
4. Brinkman TM, Zhu L, Zeltzer LK, Recklitis CJ, Kimberg C, Zhang N, et al. Longitudinal patterns of psychological distress in adult survivors of childhood cancer. British Journal of Cancer 2013; 109(5): 1373-1381.
5. Stanton AL. What happens now? Psychosocial care for cancer survivors after medical treatment completion. Journal of Clinical Oncology 2012; 30(11): 1215-1220.
6. Parahoo K, McDonough S, McCaughan E, Noyes J, Semple C, Halstead EJ, et al. Psychosocial interventions for men with prostate cancer: a Cochrane systematic review. BJU International 2015; 116(2): 174-183.
7. Zhou ES, Partridge AH, Recklitis CJ. A pilot trial of brief group cognitive-behavioral treatment for insomnia in an adult cancer survivorship program. Psycho-Oncology 2016; doi: 10.1002/pon.4096.
8. Pirl WF, Jacobsen PB, Deshields TL. Opportunities for improving psychosocial care for cancer survivors. Journal of Clinical Oncology 2013; 31(16): 1920-1921.
9. Turnbull Macdonald GC, Baldassarre F, Brown P, Hatton-Bauer J, Li M, Green E, et al. Psychosocial care for cancer: a framework to guide practice, and actionable recommendations for Ontario. Current Oncology 2012; 19(4): 209-216.
10. Penedo FJ, Dahn JR, Molton I, Gonzalez JS, Kinsinger D, Roos BA, et al. Cognitive-behavioral stress management improves stress-management skills and quality of life in men recovering from treatment of prostate carcinoma. Cancer 2004; 100(1): 192-200.
11. Antoni MH, Lechner SC, Kazi A, Wimberly SR, Sifre T, Urcuyo KR, et al. How stress management improves quality of life after treatment for breast cancer. Journal of Consulting and Clinical Psychology 2006; 74(6): 1143-1152.
12. Agboola SO, Ju W, Elfiky A, Kvedar JC, Jethwani K. The effect of technology-based interventions on pain, depression, and quality of life in patients with cancer: a systematic review of randomized controlled trials. Journal of Medical Internet Research 2015; 17(3): e65.
13. Zhou ES, Vrooman LM, Manley PE, Recklitis CJ. Adapted delivery of cognitive-behavioral treatment for insomnia in adolescent and young adult cancer survivors. Behavioral Sleep Medicine 2016; 14: 1-14.
14. Penedo FJ, Antoni MH, Schneiderman N. Cognitive-behavioral stress management for prostate cancer recovery. New York: Oxford University Press, 2008.
15. Antoni MH, Ironson G, Schneiderman N. Cognitive-behavioral stress management: workbook. New York: Oxford University Press, 2007.
16. Cohen S, Kamarck T, Mermelstein R. A global measure of perceived stress. Journal of Health and Social Behavior 1983; 24(4): 385-396.
17. McHugh RK, Barlow DH. The dissemination and implementation of evidence-based psychological treatments. A review of current efforts. American Psychologist 2010; 65(2): 73-84.
18. Onega T, Duell EJ, Shi X, Wang D, Demidenko E, Goodman D. Geographic access to cancer care in the U.S. Cancer 2008; 112(4): 909-918.
19. Vassilev I, Rowsell A, Pope C, Kennedy A, O'Cathain A, Salisbury C, et al. Assessing the implementability of telehealth interventions for self-management support: a realist review. Implementation Science 2015; 10(1): 59.
20. Payne S, Jarrett N, Jeffs D. The impact of travel on cancer patients' experiences of treatment: a literature review. European Journal of Cancer Care (England). 2000; 9(4): 197-203.
21. Hewitt M, Rowland JH. Mental health service use among adult cancer survivors: analyses of the national health interview survey. Journal of Clinical Oncology 2002; 20(23): 4581-4590.
22. Bashshur RL, Shannon GW, Bashshur N, Yellowlees PM. The empirical evidence for telemedicine interventions in mental disorders. Telemedicine Journal and e-Health 2016; 22(2): 87-113.
23. Richardson LK, Frueh BC, Grubaugh AL, Egede L, Elhai JD. Current directions in videoconferencing tele-mental health research. Clinical Psychology (New York) 2009; 16(3): 323-338.
24. Palomares RS, Bufka LF, Baker DC. Critical concerns when incorporating telepractice in outpatient settings and private practice. Journal of Child and Adolescent Psychopharmacology 2016; 26(3): 252-259.
