full article:
Previous research has established that, in comparison to their heterosexual counterparts, lesbian identified women experience a variety of health disparities, including increased risks for and/or rates of breast and gynecologic cancers, obesity, asthma, diabetes, cardiovascular disease, and multiple chronic conditions1-9, which appear to be largely associated with infrequent and/or inappropriate preventive health care1,10,11. According to the Institute of Medicine1 one of the greatest health risks for lesbians and other sexual minorities is the avoidance of routine health care. Ongoing medical care and regular physical exams help with the identification of health-related risks (such as poor eating/exercise patterns, weight concerns, unprotected sex, smoking, alcohol and drug use, and other mental health issues, all of which have been shown to be high among lesbians1-6,12-16) and provides an opportunity for early prevention/intervention efforts and the provision of appropriate referrals. Furthermore, foregoing routine gynecological appointments is particularly problematic for lesbians as they are less likely to receive regular preventive screenings that are typically a part of women's health care. Overall, this lack of preventive care reduces the likelihood of early detection of reproductive cancers, sexually transmitted infections, heart disease, and diabetes, and therefore poses a significant risk for the development of long-term and potentially life-threatening health problems that, if detected early, are more manageable and treatable17.
More specifically, research consistently demonstrates that lesbians are less likely to have a regular source of women's health care, seek medical care in general less often, and have significantly lower rates of engagement in routine preventive cancer screenings and physical exams when compared to heterosexual women6,10,13,15,18-21. For example, results from the 2010 Behavioral Risk Factor Surveillance System surveys revealed that lesbians in the USA, in comparison to their heterosexual counterparts, have more than 30% lower odds of receiving yearly routine physical exams14. In particular, recent national data suggest that approximately 38% of lesbians do not receive routine Pap tests. Although this is a decrease from past studies suggesting that 43-56% of lesbians do not receive regular Pap tests, the prevalence of non-screening among lesbians continues to be significantly higher in comparison to the general US population of women (16-25%22). Earlier research conducted by Diamant and colleagues23 suggests a disparity among lesbians with regards to regular clinical breast exams, with approximately 39% of lesbians in their sample reporting that they had not received a breast exam by a medical provider in the previous 2 years (in comparison to only 29% of heterosexual women). Likewise, Grindel and colleagues12 found that 42.3% of lesbians aged 40 years or more do not adhere to the American Cancer Society's guidelines for regular mammogram screenings, with almost 10% having never received a mammogram.
Given the magnitude of these disparities in preventive behavior among lesbians, coupled with their increased health risks, researchers have begun to explore potential explanations for the observed differences in the receipt of cancer screenings among lesbians and heterosexual women. One major factor that has been found to be associated with lower rates of preventive care among lesbians is the traditionally heterosexist nature of women's health care and the related avoidance by lesbians of regular care due to previous negative experiences with providers (ie exposure to heterosexism/homophobia-related language/paperwork, rejection, discrimination, and inappropriate care) and/or fear of future mistreatment within the healthcare setting24-26. Furthermore, fear-based avoidance of preventive healthcare may be particularly salient for more gender non-conforming lesbians whose gender presentation/identification may be in conflict with traditional femininity and typical, heteronormative women's healthcare experiences. Hiestand and colleagues27 found that 'butch'-identified lesbians, in comparison to their 'femme'-identified counterparts, report less frequent gynecological examinations due to a history of poor treatment and perceived discrimination in healthcare settings. Therefore, the experiences that lesbians have with their women's healthcare providers (WHCPs, for example obstetricians/gynecologists and/or other healthcare providers that women see for gynecologic preventive care and screenings) are crucial to their health and wellbeing. Unfortunately, many WHCPs do not have adequate training to provide appropriate care to lesbians and/or harbor their own heterosexist attitudes, beliefs, and misperceptions, both of which can result in significant mistreatment and/or subsequent avoidance of care1,24,25,28.
Although the past decade has shown a significant increase in research examining women's health-related experiences and behaviors of lesbians, the majority of that research has been conducted with primarily urban samples, with very few studies examining the potential influence of geographic context (rural or urban) on lesbians' preventive care. More specifically, due to a variety of cultural and structural related factors, rural lesbians may have more negative experiences with WHCPs and/or be less likely to receive appropriate and routine preventive care. For example, due to a greater emphasis on heteronormativity and traditional, conservative values, rural culture is often associated with higher levels of heterosexism/homophobia29-34. In addition, rural sexual minorities in the USA have been found to report increased exposure to enacted stigma35. Furthermore, the majority of rural communities are characterized by overall health professional shortages and a limited availability of women's healthcare specialists36,37, with the general population of rural women having lower rates of engagement in regular women's healthcare services in comparison to their urban counterparts36. This shortage is coupled with the likelihood that WHCPs that are knowledgeable of and sensitive to lesbian health concerns are even more scarce (if available at all) in these areas1,38.
Despite the added vulnerabilities of rural living, there is currently a dearth of research that explores aspects of women's health among rural lesbians. Only two known studies specifically examine the potential impact of living outside of an urban area on the healthcare behaviors and experiences of lesbians. First, Austin39 examined the rates of disclosure to healthcare providers among a sample of lesbians living in urban and non-urban areas in the Southern region of the USA and found that, in comparison to urban lesbians, non-urban lesbians had lower rates of disclosure (50.7% vs 61.3%, respectively). However, although this study provides some valuable information with regards to the disclosure behavior of non-urban Southern US lesbians, these results are limited in their generalizability to rural lesbians across the USA given that the study was conducted with lesbians in one region of the country and only a small portion of the 'non-urban' sample were residents of rural communities. Furthermore, Austin's39 study focused on primary health care and did not specifically assess aspects of gynecological care. Next, Tiemann and colleagues40 conducted a qualitative study involving a small (N=8), geographically limited (Midwest USA) sample of rural lesbians that was also primarily focused on disclosure to providers. Participants were asked to describe their healthcare disclosure-related behaviors and related experiences with providers in their areas. Results of these interviews highlighted a variety of negative experiences with rural medical providers if one's sexual orientation was known (eg heterosexist/homophobic reactions and/or mistreatment). Furthermore, interview responses suggested that rural lesbians may engage in a variety of disclosure-related protective strategies when interacting with healthcare providers such as screening potential providers with regards to their sensitivity/knowledge of lesbian health, discontinuing care following negative reactions to their sexual orientation disclosure, and/or avoidance of disclosure due to fears of rejection and/or mistreatment given that alternative options for safe, affirming care may not be available due to the shortage of providers in their community.
Current study
The Institute of Medicine1 has emphasized a substantial need for research that takes an intersectionality approach to examining the potential influences of rural-urban location on the health-related needs and experiences of lesbians and other sexual minorities. More specifically, there is currently no known large-scale quantitative research that examines aspects of women's health care among rural lesbians. The purpose of this study was to quantitatively compare rural and urban lesbians' access to women's health care, experiences with WHCPs, and preventive behavior (receipt of human papillomavirus (HPV) vaccination and past 3-year HIV screening, Pap test, clinical breast exam, and mammogram) using a large, diverse sample of lesbians from across the USA. It was hypothesized that, in comparison to their urban counterparts, rural lesbians would have less access to women's health care and, for those that do have access, different experiences with WHCPs (eg less likely to be asked about their sexual orientation and provided appropriate safe-sex education), in addition to having lower rates of engagement in preventive behaviors.
Participants
As part of a larger lesbian, gay, bisexual, and transgender (LGBT) health survey41, participants for the current study were recruited from across the USA through email communication to LGBT-focused organizations and a classified advertisements website. To participate in the overall study, individuals had to be aged 18 years or older and identity as a gender and/or sexual minority (lesbian, gay, bisexual, pansexual, queer, transgender, gender non-conforming/genderqueer). A total of 3279 LGBT-identified individuals participated in the overall study. For the purposes of this study, only cisgender (not transgender) women who identified their sexual orientation as lesbian were included in the analytic sample (N=895).
Procedures
Recruitment for this study was completed entirely online through email, social media, and a classified advertisement website. Over the course of the study, approximately 5000 emails and messages were sent to LGBT-related organizations and listservs in all 50 US states. To increase the sample of rural-residing gender and sexual minorities who may have limited access to formal LGBT organizations and networks29, the same recruitment message was also used to create an online advertisement that was posted in the 'community volunteer' section of each US municipality on classified advertisement websites. The hyperlink to the study was included within the recruitment advertisements. After interested and eligible participants reached the survey webpage they were initially asked to read the informed consent page and indicate their willingness to voluntarily participate in the anonymous study by clicking 'yes' at the end of the page. Following informed consent, participants were guided through the survey using skip patterns. After completing the survey, participants were redirected to a debriefing page and provided with an opportunity to voluntarily participate in a draw to win 1 of 30 gift cards valued at $50.
Measures
The parent study included 75-demographic and health-related questions created by the investigators and seven formal questionnaires. For the current study, only demographics and questions related to women's health care were used. To assess current geographic location, participants were asked 'Which best describes the area that you currently live in?' (answer choices: 'rural' and 'urban'). To examine access to women's healthcare and experiences with providers, participants were asked to complete a series of dichotomous (yes/no) questions regarding their personal experiences ('Do you have an obstetrician/gynecologist (OB/GYN) or other women's healthcare provider that you see on a regular basis for preventive care?', 'Do you feel that your women's health provider is knowledgeable and sensitive to unique lesbian and bisexual women's health issues/concerns?'). Next, with the exception of receipt of HPV vaccination, which was measured using a similar yes/no question, preventive behavior was assessed by having participants indicate when they last received an HIV/sexually transmitted infection (STI) test, Pap smear, breast exam, and mammogram using the following scale: 0='never' to 4='within the last year'. Lastly, participants were asked to indicate how many male sexual partners they have had in their lifetime (1='none' to 7='over 50').
Ethics approval
All relevant ethical safeguards were followed in relation to participant protection, and the project was reviewed by the institutional review board of Georgia Southern University (H13171).
Data preparation and analysis
According to recent updates to the cervical cancer screening guidelines, the US Preventive Services Task Force42 recommends that women receive a Pap test every 3-5 years (instead of the traditional emphasis on having annual HPV screenings). Furthermore, according to the American Cancer Society's Guidelines for Early Detection of Cancer, the recommended frequency of clinical breast exams for women aged 20-39 is also every 3 years43. To simplify the current study's interpretations, past 3-year preventive behaviors (Pap smear, breast exam, mammogram, and HIV/STI screening) were examined by collapsing responses into two categories: 'never' and 'over 3 years ago' = 'no' and all other responses = 'yes'. Similarly, responses to the question regarding previous male sexual partners were collapsed into yes/no categories ('never' = 'no' and all other responses = 'yes'). To compare rural-urban differences across dependent variables, a series of χ2 analyses were utilized for each dichotomous question. Given that, in the USA, the recommended age to begin receiving regular mammograms is 4043, only those lesbians that self-reported their age as 40 years or more (n=163) were included in the χ2 analysis examining rural-urban differences in mammography behavior.
Sample characteristics
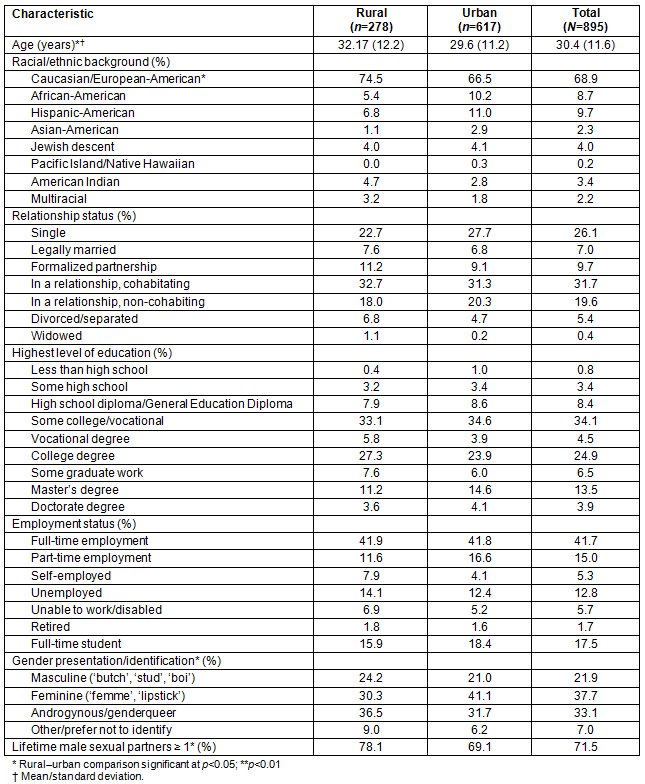
A total of 895 lesbian-identified cisgender women participated in the current study. Of the total sample, 31.1% were rural residents and 68.9% were urban residents. The mean age of the total sample was 30.4 (standard deviation (SD)=11.6), with the sample of rural-residing lesbians being significantly older than those living in urban areas (t(893)= -3.05, p=0.002). More than two-thirds (68.9%) of the total sample identified their racial/ethnic background as Caucasian/European American. However, the urban sample was significantly more racially and ethnically diverse in comparison to the rural sample of lesbians (χ2(1, N=895)=18.00, p=0.021). See Table 1 for additional sample characteristics.
Table 1: Demographic characteristics of lesbian-identified cisgender women who participated in study (N=895)
Access to women's healthcare, and experiences with providers
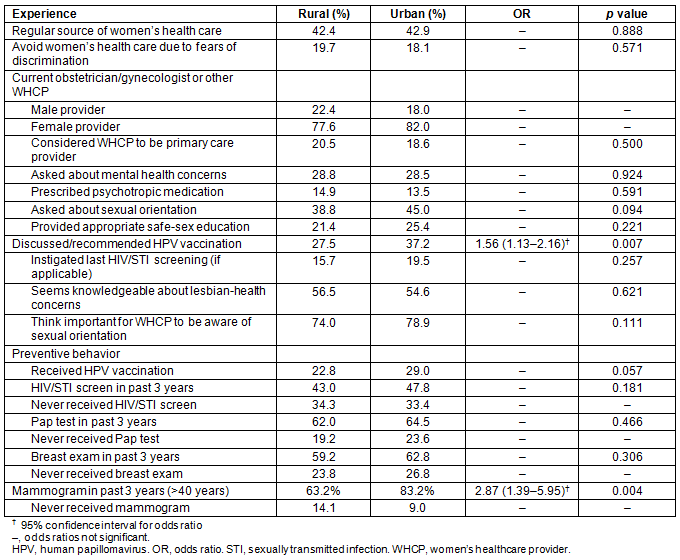
A similarly low percentage of rural (42.4%) and urban (42.9%) lesbians reported that they have a WHCP that they see on a regular basis for preventive care. In terms of experiences with WHCP providers, significantly fewer rural lesbians indicated that their current WHCP had discussed/recommended the HPV vaccination in comparison to urban lesbians (27.5% vs 37.2%, χ2(1, N=796)=7.24, p=0.007). No other rural-urban differences emerged, with a similar percentage of rural and urban lesbians indicating that they avoid/put off women's healthcare appointments due to fears of discrimination (19.7% and 18.1%, respectively) and they believe that it is important for their WHCP to be aware of their sexual orientation (74.0% and 78.9%), in addition to the following experiences with a women's healthcare provider: they consider their WHCP to be their primary care provider (20.5% and 18.6%, respectively); their WHCP has asked about mental health concerns (28.8% and 28.5%); their WHCP has prescribed psychotropic medication (14.9% and 13.5%); their WHCP has asked about sexual orientation (38.8% and 45.0%); their WHCP has provided appropriate safe-sex education (21.4% and 25.3%); their WHCP instigated their previous HIV/STI screening (if applicable; 15.7% and 19.5%); their WHPC seems knowledgeable about lesbian health concerns (56.5% and 54.6%).
Preventive behavior
An examination of preventive behavior among rural and urban lesbians revealed that significantly fewer rural lesbians aged 40 years or more had received a mammogram in the past 3 years (63.2% vs 83.2%, χ2(1, N=163)=8.36, p=0.004) when compared to their urban counterparts. No other significant differences in preventive behavior emerged. A similar percentage of rural and urban lesbians indicated that they have received the HPV vaccination (22.8% and 29.0%, respectively), had a HIV/STI screening (43.0% and 47.8%), Pap test (62.0% and 64.5%), or breast exam (59.2% and 62.8%) in the past 3 years. See Table 2 for rural-urban comparisons of experiences with providers and preventive behavior.
Table 2: Rural-urban comparisons of experiences with women's healthcare providers and preventive behavior among lesbian-identified cisgender women who participated in study (N=895)
Discussion
The purpose of the current student was to explore rural-urban differences with regards to women's healthcare-related experiences and preventive behaviors among US lesbians. Given the unique cultural and structural aspects of rural living, it was hypothesized that there would be differences across many aspects of care. Namely, it was expected that, in comparison to their urban counterparts, rural lesbians would have less access to women's health care and, for those that do have access, different experiences with WHCPs, in addition to having lower rates of engagement in preventive behaviors. Contrary to expectations, however, very few significant rural-urban differences in experiences and behavior emerged. Overall, it appears that women's healthcare-related experiences and preventive behaviors of rural lesbians are fairly similar to those of their urban counterparts (ie similarly low levels of engagement with and access to appropriate care).
The few significant rural-urban differences found in the current study are important to recognize and explore further as they have significant implications for the health and wellbeing of rural lesbians, especially with regards to HPV and cervical cancer risks. In comparison to urban lesbians, relatively fewer rural lesbians indicated that their WHCP had recommended that they receive the HPV vaccination (27.5% vs 37.2%), coupled with the finding that 22.8% of the current sample of rural-residing lesbians have actually been vaccinated for HPV. This is particularly concerning given that almost 80% of the rural-residing lesbians endorsed having at least one previous male sexual partner in their lifetime, which was significantly higher than the urban sample. This highlights an elevated risk for contracting HPV among rural lesbians, as they were less likely to receive a vaccination recommendation despite being more likely to have a history of male sexual partners. Although it is often assumed by providers and patients alike that lesbians have lower risks for contracting HPV and are less susceptible to cervical cancer given that one major risk factor is unprotected sexual intercourse with multiple male partners44,45, the current findings and previous studies (with prevalence rates ranging from 70% to 80%46-49) highlight that the majority of lesbian-identified women have had at least one male sexual partner, which adds to their risk of developing cervical cancer13,50. Furthermore, despite misconceptions about lesbians' risks, HPV infections can be sexually transmitted between women13,51,52, and HPV infections have been found among samples of women with only female sexual partners, with recent research suggesting a HPV infection prevalence rate of 34% among sexual minority women with no previous male sexual contact52.
The prevalence of HPV among the general population of both men and women in the USA is alarmingly high, with approximately 50% of sexually active Americans estimated to contract HPV over the course of their lifetime53. Furthermore, although the majority of HPV infections typically diminish over time, 40 out of the 150 strains of HPV can cause cancer54, with HPV being an underlying cause in almost all newly diagnosed cases of cervical cancer55. This is coupled with a well-documented and persistent rural-urban disparity wherein, in comparison to the general population of urban women in the USA, rural-residing women have been found to have significantly higher cervical cancer incidence and mortality rates56. Given that both lesbian-identified women and rural-residing women, in comparison to their heterosexual and urban counterparts, have increased risks for developing cervical cancer, the intersectionality of the two likely results in a greater risk for rural lesbians as well. Due to these potentially elevated risks and the higher rates of sexual activity with men among the current sample of rural lesbians, future research is needed that specifically examines HPV and cervical cancer risk factors and rates among rural lesbians.
It is important to note that the first US Food and Drug Administration-approved vaccine for HPV was released in 2006 and is currently only approved for use in older children and young adults (ie ages 9-26 years) and, although national utilization rates are not available for young women, approximately one-third of adolescent girls aged 14-19 years received the HPV vaccine between 2007 and 2010, with approximately 37.6% having received the vaccine by 201357. Therefore, given these national rates and the age range of our sample, overall rates of HPV vaccination were not expected to be high. However, the reasonably low percentage of lesbians in the current study who indicated that a WHCP had previously recommended that they receive the HPV vaccination, especially among the rural-residing lesbians, remains relatively concerning and warrants further research and clinical attention. To illustrate, post-hoc examination of age groups reveals that approximately 70% of the rural sample either are or were recently in the appropriate age range to receive the HPV vaccination (ie aged 26 years or less at the time of the study). However, only 46.6% of the rural-residing lesbians in this age range indicated that the HPV vaccination had been recommended to them by a WHCP. Therefore, the current results highlight that, despite the fact that the majority of lesbians have had heterosexual intercourse and have elevated risks for developing cervical cancer51,58, rural WHCPs may not be adequately addressing this disparity by including the HPV vaccination as part of the prevention education and recommendations that they provide to their lesbian patients.
An examination of access to women's health care highlights a major health risk among both rural and urban lesbians in the USA in that less than half of the women in both samples had a regular source of women's health care. These findings are consistent with previous studies highlighting the access to care disparity faced by lesbians and other sexual minorities in the general population10,14,59,60 and also suggest that this particular women's health-related risk is not exacerbated by rural location. This lack of a significant rural-urban difference is especially surprising given the previous research highlighting that women's healthcare providers tend to be more scarce in rural areas and rural women typically have less access to care when compared to their urban counterparts36,37,61-63. Overall, the current finding that almost 60% of both rural and urban lesbians do not have a regular source of women's health care represents a major public health concern, and future research, clinical, and policy efforts are needed to adequately address this disparity. For example, it may be helpful for future studies to examine the specific types of barriers (eg availability of providers, transportation limitations, insurance coverage, financial restrictions) that potentially restrict access to women's health care among both rural and urban samples of lesbians in order to further explore potential differences in access to care and identify specific target areas for improving access within these different geographic locations. One potential barrier highlighted in the current study is a personal avoidance of care that is specifically related to sexual orientation. Namely, rates of fear-based avoidance of women's health care was alarmingly high among rural and urban lesbians, with approximately 20% of the total sample of lesbians indicating that they delay or avoid women's healthcare appointments due to fears related to disclosure of sexual orientation and/or discrimination, rejection, and mistreatment. Therefore, the current finding adds to the growing body of literature highlighting that avoidance of preventive care due to fears of discrimination represents a considerable barrier to women's health care among lesbians in both rural and urban areas.
Given that other mental and physical health specialists may not be readily available in rural areas36,37,61-64 it was anticipated that rural lesbians would be more likely to consider their WHCP to be their primary care provider and report greater mental health service provision by their WHCP. This hypothesis was not supported by the current findings; a similar percentage of rural and urban lesbians identified their WHCP as their primary care provider (20.5% and 18.6%, respectively) and reported being prescribed psychotropic medications by their WHCP (14.9% and 13.5%). Interestingly, previous research has suggested that only about 6% of women in the general population utilize their WHCP as their primary source of medical care65. However, this rate has been found to be much higher (38.0%) among more underprivileged groups of women (those with lower incomes)66. Therefore, the current findings suggest that lesbians, like other disadvantaged groups of women, may have a great propensity to utilize their WHCP as their primary care provider. Although there is no research available that allows for a direct comparison of rates of being prescribed any type of psychotropic medications by a WHCP, previous national data examining prescription rates in a given quarter has suggested that only about 3% of antidepressants are prescribed by obstetricians/gynecologists67. Given this previous research, the current findings suggest that many lesbians (almost 15% of the current sample) are prescribed psychotropic medications by their WHCPs and rurality does not appear to increase this probability. Future research is needed to further explore the mental health-related needs and experiences among lesbians accessing women's healthcare services.
An examination of rural and urban lesbians' reported experiences related to receipt of appropriate and affirming women's health care also reveals a multitude of concerns for the treatment of both rural and urban lesbians. First, 61.2% of rural lesbians and 55% of urban lesbians had not been asked about their sexual orientation by their WHCP. These rates are disturbingly high given that knowledge of one's unique sexual identity and behavior on the part of women's healthcare providers is particularly crucial for the provision of appropriate and affirming care68-70. Given these low rates, it is not surprising that only 21.4% of rural lesbians and 25.4% of urban lesbians indicated that they had been provided with appropriate safe-sex education by their WHCP, with less than 20% of both samples reporting that their last HIV/STI screening was instigated by their provider. Furthermore, only about 55% of rural and urban lesbians felt that their WHCP seemed knowledgeable about lesbian health concerns. Taken together, these findings highlight significant experiences of inappropriate, and largely heterosexist, treatment among both rural and urban lesbians and suggest a high prevalence of inadequate care that likely contributes substantially to the health disparities faced by this population. Furthermore, this type of insensitive treatment increases the likelihood that lesbians will avoid subsequent health care71, which can drastically exacerbate their risk for poor health outcomes. Lastly, despite the American College of Obstetrics and Gynecology's72,73 guidelines recommending that women's healthcare providers address behavioral health concerns (including assessment, prevention, and treatment) as part of their regular practice and the well-documented mental health disparities among lesbians and other sexual minorities1,2,6,74,75, less than 30% of rural and urban lesbians reported that they had been asked about mental health concerns by a WHCP. This finding is consistent with previous research suggesting that WHCPs may not be adequately addressing the behavioral health needs of their patients76. Overall, the current findings highlight a significant need for both rural and urban WHCPs to engage in cultural competency training related to providing appropriate and affirming gynecological and behavioral health care to lesbian-identified women. Given that these types of training may not be readily available to providers practicing in rural areas, further research and policy efforts are needed to facilitate the creation of innovative strategies for providing lesbian health training to rural providers (ie through online training modules, live webinars, cyber-based supervision/consultation).
Rural lesbians also evidenced rates of engagement in regular preventive health behaviors that were either lower or similar to their urban counterparts, depending on the behavior. Namely, among the current sample of lesbian aged 40 years or more, those residing in rural areas were significantly less likely to have received a mammogram in the past 3 years when compared to their urban counterparts (63.2% vs 83.2%). Furthermore, rates of HIV/STI screening, Pap testing, and clinical breast exams were relatively low for both samples of lesbians and appear to be reasonably consistent with previous studies. For example, in the current study, 43.0% of rural lesbians and 47.8% of urban lesbians reported past 3-year HIV/STI screening; with previous studies demonstrating rates among lesbians of approximately 27-58%, depending on the sample4,21,77. In terms of Pap testing, 62.0% of rural lesbians and 64.5% of urban lesbians had received a Pap smear in the past 3 years (previous rates are 48-81%44). Likewise, rates of past 3-year breast exam among rural and urban lesbians were 59.2% and 62.8%, respectively (similar to the 61% found in Diamant and colleagues' 2000 study23), with almost a quarter of the total sample of lesbians indicating that they have never received a clinical breast exam.
Given the documented rural-urban disparities in the USA with regards to both cervical cancer (rural women have high incidence and mortality rates56) and breast cancer (diagnosed at later stage in rural women78) among the general population of women, coupled with the fact that lesbians experience greater gynecological cancer risks58, the risks for these types of cancer is theoretically highest among rural lesbians. Consequently, in order to adequately address these discrepancies, cancer screening rates among rural lesbians need to be higher than those for their urban counterparts. Therefore, the current finding that rural lesbians receive age-appropriate mammograms at significantly lower rates, and Pap tests and clinical breast exams at rates similar to urban lesbians despite having higher disease burden, represents an important shortcoming in addressing a recognized health disparity among rural-residing lesbians.
In response to the emerging evidence highlighting the lower health screening rates and related health risks of lesbians, there has been recent increased public health attention supporting the creation of lesbian-specific community outreach programs and prevention efforts (ie the Lesbian Breast and Cervical Health Project, the Atlanta Lesbian Health Initiative, The Stud Health Project and 'Real Bois Talk', the Lesbian Education and Health Program, and the 'Get Screened' Program) across the USA and Canada. However, the majority of these programs, in addition to LGBT-focused healthcare facilities (ie Fenway Health, the Mazzoni Center, the Howard Brown Health Center, Capitol Hill Medical), are located in large metropolitan areas and are not accessible to lesbians residing in rural areas and small communities. There is currently a dearth of women's health-related health education resources and programming that are culturally tailored to specifically target and meet the unique health needs of lesbians and other sexual minority women in rural areas of the USA. Therefore, if health promotion efforts aimed at increasing preventive behaviors among lesbians continue to be urban-centric, this will likely widen the rural-urban disparity among lesbians. Overall, the current findings highlight the need for women's health programming and outreach efforts that are uniquely designed to promote rural lesbians' engagement in preventive behaviors. Given the 'hard-to-reach' and less visible nature of this population29,79 these types of effort will require innovative and culturally sensitive recruitment and delivery strategies (ie using online-based programming, chain referrals, lesbian health resource guides that are discreet in their design and delivery) in order to be effective in promoting engagement in women's health care among rural-residing lesbians.
Limitations to the current study should be considered when interpreting the findings. First, this study relied exclusively on a convenience sampling approach to recruitment; thus, the current sample may not be representative of the experiences and behaviors of rural and urban lesbians in the general population. For example, the researchers' reliance on online postings to LGBT-focused organizations/listservs and a classified advertisements website limited the sample to those lesbians who: have access to the internet, are technologically literate and/or are connected with an LGBT-focused organization and/or a user of the classifieds website. Also, the majority of the lesbians included in the current sample were Caucasian/European-American (almost 70%). As a result, the current findings may not be generalizable to lesbians who identify as racial/ethnic minorities. Lastly, the current findings regarding rural and urban lesbians' women's healthcare-related experiences and behaviors are based solely on participant self-report and therefore may not be an exact representation of the preventive behaviors of lesbians.
The current study's findings highlight that rural lesbians in the USA, in comparison to urban lesbians, may experience elevated health risks related to being more likely to have at least one previous male sexual partner, less likely to be recommended the HPV vaccination by a WHCP, and, for those 40 or older, less likely to receive routine mammograms. Given the increased cervical and breast cancer risks associated with rural living, the current findings that rural lesbians engage in lower rates of age-appropriate mammogram screenings and similarly low rates of HPV vaccinations, Pap tests, and clinical breast exams as their urban counterparts highlight the dire need for health promotion efforts aimed at increasing rural lesbians' engagement in routine pelvic and breast exams. Lastly, based on the self-reported experiences of rural and urban lesbians, the current findings suggest that many of these women may not be receiving appropriate and affirming women's healthcare services. Overall, the current findings support the need for increased lesbian health-focused cultural competency training among WHCPs and also point to a need for future research that further explores the unique women's health-related risks and needs of rural and urban lesbians.
References
1. Institute of Medicine Committee on Lesbian, Gay, Bisexual, and Transgender Health Issues and Research Gaps and Opportunities. The health of lesbian, gay, bisexual, and transgender people: building a foundation for better understanding. Washington, DC: National Academic Press, 2011.
2. Gonzales G, Przedworski J, Henning-Smith C. Comparison of health and health risk factors between lesbian, gay, and bisexual adults and heterosexual adults in the United States: results from the National Health Interview Survey. JAMA Internal Medicine 2016; 176(9): 1344-1351.
3. Boehmer U, Bowen DJ, Bauer GR. Overweight and obesity in sexual-minority women: Evidence from population-based data. American Journal of Public Health 2007; 97(6): 1134-1140. https://doi.org/10.2105/AJPH.2006.088419
4. Conron K, Mimiaga M, Landers S. A population-based study of sexual orientation identity and gender differences in adult health. American Journal of Public Health 2006; 100(10): 1953-1960. https://doi.org/10.2105/AJPH.2009.174169
5. Zaritsky EL. Risk factors for reproductive and breast cancers among older lesbians. Journal of Womens Health 2010; 19(1): 125-131. https://doi.org/10.1089/jwh.2008.1094
6. Dilley J, Simmons K, Boysun M, Pizacani BA, Stark MJ. Demonstrating the importance and feasibility of including sexual orientation in public health surveys: health disparities in the Pacific Northwest. American Journal of Public Health 2010; 100(3): 460-467. https://doi.org/10.2105/AJPH.2007.130336
7. Struble CB, Lindley LL, Montgomery K, Hardin J, Burcin M. Overweight and obesity in lesbian and bisexual college women. Journal of American College Health 2010; 59(1): 51-56. https://doi.org/10.1080/07448481.2010.483703
8. Fredriksen-Goldsen KI, Kim HJ, Barkan SE, Muraco A, Hoy-Ellis CP. Health disparities among lesbian, gay, and bisexual older adults: results from a population-based study. American Journal of Public Health 2013; 103(10): 1802-1809. https://doi.org/10.2105/AJPH.2012.301110
9. Roberts SJ. Health care recommendations for lesbian women. Journal of Obstetric, Gynecologic & Neonatal Nursing 2006; 35(5): 583-591. https://doi.org/10.1111/j.1552-6909.2006.00081.x
10. Buchmueller T, Carpenter C. Disparities in health insurance coverage, access, and outcomes for individuals in same-sex versus different-sex relationships, 2000-2007. American Journal of Public Health 2010; 100(3): 489-495. https://doi.org/10.2105/AJPH.2009.160804
11. Mollon L. The forgotten minorities: health disparities of the lesbian, gay, bisexual, and transgendered communities. Journal of Health Care for the Poor and Underserved 2012; 23(1): 1-6. https://doi.org/10.1353/hpu.2012.0009
12. Grindel CG, McGehee LA, Patsdaughter CA, Roberts SJ. Cancer prevention and screening behaviors in lesbians. Women & Health 2006; 44(2): 15-39. https://doi.org/10.1300/J013v44n02_02
13. Marrazzo JM, Gorgos LM. Emerging sexual health issues among women who have sex with women. Current Infectious Disease Reports 2012; 14(2): 204-211. https://doi.org/10.1007/s11908-012-0244-x
14. Blosnich JR, Farmer GW, Lee JL, Silenzio VB, Bowen DJ. Health inequalities among sexual minority adults: evidence from ten U.S. States, 2010. American Journal of Preventive Medicine 2014; 46(4): 337-349. https://doi.org/10.1016/j.amepre.2013.11.010
15. Mason TB. Binge eating and overweight and obesity among young adult lesbians. LGBT Health 2016; 3(6): 472-476.
16. Jones AR, Hoyler CL. HIV/AIDS among women who have sex with women. In F Fernandez, P Ruiz, Eds. Psychiatric aspects of HIV/AIDS Philadelphia, PA: Lippincott Williams & Wilkins, 2005; 299-307.
17. Kerr S, Mathy R. Preventive health measures for lesbian and bisexual women. Binghamton, NY: The Haworth Medical Press, 2006.
18. Kerker BD, Mostashari F, Thorpe L. Health care access and utilization among women who have sex with women: sexual behavior and identity. Journal of Urban Health 2006; 83(5): 970-979. https://doi.org/10.1007/s11524-006-9096-8
19. Agénor M, Krieger N, Austin SB, Haneuse S, Gottlieb BR. Sexual orientation disparities in Papanicolaou test use among US women: the role of sexual and reproductive health services. American Journal of Public Health 2014; 104(2): e68-e73. https://doi.org/10.2105/AJPH.2013.301548
20. Wells BE, Bimbi DS, Tider D, Ora JV, Parsons JT. Preventive health behaviors among lesbian and bisexually identified women. Women & Health 2007; 44(2): 1-13. https://doi.org/10.1300/J013v44n02_01
21. Kerr DL, Ding K, Thompson AJ. A comparison of lesbian, bisexual, and heterosexual female college undergraduate students on selected reproductive health screenings and sexual behaviors. Women's Health Issues 2013; 23(6): e347-e355. https://doi.org/10.1016/j.whi.2013.09.003
22. Tracy JK, Schluterman NH, Greenberg, DR. Understanding cervical cancer screening among lesbians: a national survey. BMC Public Health 2013; 13(1): 442-450. https://doi.org/10.1186/1471-2458-13-442
23. Diamant A, Wold C, Spritzer K, Gelberg L. Health behaviors, health status, and access to and use of health care: a population-based study of lesbian, bisexual, and heterosexual women. Archives of Family Medicine 2000; 9(10): 1043-1051. https://doi.org/10.1001/archfami.9.10.1043
24. Hutchinson MK, Thompson AC, Cederbaum, JA. Multisystem factors contributing to disparities in preventive health care among lesbian women. Journal of Obstetric, Gynecologic, & Neonatal Nursing 2006; 35(3): 393-402. https://doi.org/10.1111/j.1552-6909.2006.00054.x
25. Herndandez M, Fultz SL. Barriers to health care access. In: MD Shankle, Ed. The handbook of lesbian, gay, bisexual, and transgender public health: a practitioner's guide to service. New York, NY: Routledge, 2006; 177-200.
26. Steele LS, Tinmouth JM, Lu A. Regular health care use by lesbians: a path analysis of predictive factors. Family Practice 2006; 23(6): 631-636. https://doi.org/10.1093/fampra/cml030
27. Hiestand KR, Horne SG, Levitt HM. Effects of gender identity on experiences of healthcare for sexual minority women. Journal of LGBT Health Research 2007; 3(4): 15-27. https://doi.org/10.1080/15574090802263405
28. Abdessamad HM, Yudin MH, Tarasoff LA, Radford KD, Ross LE. Attitudes and knowledge among obstetrician-gynecologists regarding lesbian patients and their health. Journal of Women's Health 2013; 22(1): 85-93. https://doi.org/10.1089/jwh.2012.3718
29. Barefoot KN, Rickard A, Smalley, KB, Warren, JC. Rural lesbians: unique challenges and implications for mental health providers. Journal of Rural Mental Health 2015; 39(1): 22-33. https://doi.org/10.1037/rmh0000014
30. Dillon M, Savage S. Values and religion in rural America: attitudes toward abortion and same-sex relations. In: The Carsey Institute reports on rural America (Issue brief no. 1). Durham, NH: Carsey Institute, University of New Hampshire, 2006.
31. Eldridge V, Mack L, Swank E. Explaining comfort with homosexuality in rural America. Journal of Homosexuality 2006; 51(2): 39-56. https://doi.org/10.1300/J082v51n02_03
32. Gottschalk L, Newton J. Rural homophobia: not really gay. Gay and Lesbian Issues and Psychology Review 2009; 5(3): 153-159.
33. Snively CA, Kreuger L, Stretch JJ, Watt J, Chadha J. Understanding homophobia: preparing for practice realities in urban and rural settings. Journal of Gay & Lesbian Social Services 2004; 17(1): 59-81. https://doi.org/10.1300/J041v17n01_05
34. Hastings SL, Hoover-Thompson A. Effective support for lesbians in rural communities: the role of psychotherapy. Journal of Lesbian Studies 2011; 15(2): 197-204. https://doi.org/10.1080/10894160.2011.521104
35. Swank E, Fahs B, Frost D. Region, social identities, and disclosure practices as predictors of heterosexist discrimination against sexual minorities in the United States. Sociological Inquiry 2013; 83(2): 238-258. https://doi.org/10.1111/soin.12004
36. American College of Obstetricians and Gynecologists, Committee on Health Care for Underserved Women. Health Disparities in Rural Women (Committee opinion no. 586). (Internet) 2014. Available: http://www.acog.org/Resources-And-Publications/Committee-Opinions/Committee-on-Health-Care-for-Underserved-Women/Health-Disparities-in-Rural-Women (Accessed 23 April 2015).
37. Meit M, Knudson A, Gilbert T, Yu ATC, Tanenbaum E, Ormson E, et al. The 2014 update of the rural-urban chartbook. (Internet) 2014. Available: http://ruralhealth.und.edu/projects/health-reform-policy-research-center/pdf/2014-rural-urban-chartbook-update.pdf (Accessed 23 April 2015).
38. Warren J, Smalley KB, Rimando M, Barefoot KN, Hatton A, LeLeux-LaBarge K. Rural minority health: race, ethnicity, and sexual orientation. In: JC Warren, KB Smalley, Eds. Rural public health: best practice and preventive models. New York, NY: Springer Publishing Company, 2014; 203-226.
39. Austin EL. Sexual orientation disclosure to health care providers among urban and non-urban southern lesbians. Women & Health 2013; 53(1): 41-55. https://doi.org/10.1080/03630242.2012.743497
40. Tiemann KA, Kennedy SA, Haga MP. Rural lesbians' strategies for coming out to health care professionals. Journal of Lesbian Studies 1998; 2(1): 61-75. https://doi.org/10.1300/J155v02n01_05
41. Warren JC, Smalley KB, Barefoot KN. Recruiting rural and urban LGBT populations online: differences in participant characteristics between email and Craigslist approaches. Health and Technology 2015; 5(2): 103-114. https://doi.org/10.1007/s12553-015-0112-4
42. U.S. Preventive Services Task Force. U.S. Preventive Services Task Force issues new cervical cancer screening recommendations. (Internet) 2012. Available: http://www.uspreventiveservicestaskforce.org/Page/Name/us-preventive-services-task-force-issues-new-cervical-cancer-screening-recommendations (Accessed 23 April 2015).
43. Smith RA, Cokkinides V, Eyre HJ. American Cancer Society guidelines for the early detection of cancer, 2006. CA: A Cancer Journal for Clinicians 2006; 56(1): 11-25. https://doi.org/10.3322/canjclin.56.1.11
44. Waterman L, Voss J. HPV, cervical cancer risks, and barriers to care for lesbian women. The Nurse Practitioner 2015; 40(1): 46-53. https://doi.org/10.1097/01.NPR.0000457431.20036.5c
45. Power J, McNair R, Carr S. Absent sexual scripts: lesbian and bisexual women's knowledge, attitudes and action regarding safer sex and sexual health information. Culture, Health & Sexuality 2009; 11(1): 67-81. https://doi.org/10.1080/13691050802541674
46. Price JH, Easton AN, Telljohann SK, Wallace PB. Perceptions of cervical cancer and Pap smear screening behavior by women's sexual orientation. Journal of Community Health 1996; 21(2): 89-105. https://doi.org/10.1007/BF01682301
47. Diamant AL, Schuster MA, McGuigan K, Lever J. Lesbians' sexual history with men: implications for taking a sexual history. Archives of Internal Medicine, 1999; 159(22): 2730-2736. https://doi.org/10.1001/archinte.159.22.2730
48. Koh AS, Gómez CA, Shade S, Rowley E. Sexual risk factors among self-identified lesbians, bisexual women, and heterosexual women accessing primary care settings. Sexually Transmitted Diseases 2005; 32(9): 563-569. https://doi.org/10.1097/01.olq.0000175417.17078.21
49. Carroll N, Goldstein RS, Lo W, Mayer KH. Gynecological infections and sexual practices of Massachusetts lesbian and bisexual women. Journal of the Gay & Lesbian Medical Association 1997; 1(1): 15-23. https://doi.org/10.1023/B:JOLA.0000007008.17392.2d
50. Rankow EJ, Tessaro I. Cervical cancer risk and Papanicolaou screening in a sample of lesbian and bisexual women. The Journal of Family Practice 1998; 47(2): 139-143.
51. National LGBT Cancer Network. HPV and cancer. (Internet) 2013. Available: http://www.cancer-network.org/cancer_information/hpv_and_cancer/ (Accessed 23 April 2015).
52. Reiter PL, McRee AL. HPV infection among a population-based sample of sexual minority women from USA. Sexually Transmitted Infections 2016, ahead of print. https://doi.org/10.1136/sextrans-2016-052536 (Accessed 13 December 2016).
53. Centers for Disease Control and Prevention. Genital HPV infection fact sheet. (Internet) 2014. Available: http://www.cdc.gov/std/hpv/hpv-factsheet-march-2014.pdf (Accessed 23 April 2015).
54. Markowitz LE, Dunne EF, Saraiya M, Chesson HW, Curtis CR, Gee J, et al. Human papillomavirus vaccination: recommendations of the Advisory Committee on Immunization Practices (ACIP). Morbidity and Mortality Weekly Report (MMWR) 2014; 63(RR05): 1-30.
55. Chaturvedi AK. Beyond cervical cancer: burden of other HPV-related cancers among men and women. Journal of Allied Health 2014; 46(4): S20-S26.
56. Singh GK. Rural-urban trends and patterns in cervical cancer mortality, incidence, stage, and survival in the United States, 1950-2008. Journal of Community Health 2012; 37(1): 217-223. https://doi.org/10.1007/s10900-011-9439-6
57. The Kaiser Family Foundation. The HPV vaccine: access and use in the U.S. (fact sheet). (Internet) 2015. Available: http://files.kff.org/attachment/fact-sheet-the-hpv-vaccine-access-and-use-in-the-u-s (Accessed 23 April 2015).
58. Brown JP, Tracy JK. Lesbians and cancer: an overlooked health disparity. Cancer Causes & Control 2008; 19(10): 1009-1020. https://doi.org/10.1007/s10552-008-9176-z
59. Kates J, Ranji U, Beamesderfer A, Salganicoff A, Dawson, L. Health and access to care and coverage for lesbian, gay, bisexual, and transgender individuals in the U.S. (Issue brief). (Internet) 2016. Available: http://kff.org/report-section/health-and-access-to-care-and-coverage-for-lesbian-gay-bisexual-and-transgender-the-lgbt-community/ (Accessed 25 August 2016)
60. Mayer KH, Bradford JB, Makadon HJ, Stall R, Goldhammer H, Landers S. Sexual and gender minority health: what we know and what needs to be done. American Journal of Public Health 2008; 98(6): 989-995. https://doi.org/10.2105/AJPH.2007.127811
61. Bennett, KJ, Lopes JE, Spencer K, van Hecke S. Rural women's health. (Policy brief). (Internet) 2013. Available: http://www.ruralhealthweb.org/index.cfm?objectid=F5A503E1-3048-651A-FE066957562D3AC7 (Accessed 23 April 2015).
62. Ziller E. Access to medical care in rural America. In: JC Warren, KB Smalley, Eds. Rural public health: best practice and preventive models. New York, NY: Springer Publishing Company, 2014; 11-28.
63. American Congress of Obstetricians and Gynecologists. The obstetrician-gynecologist distribution atlas. Washington, DC: American Congress of Obstetricians and Gynecologists, 2013.
64. Barefoot KN, Smalley KB, Warren JC. Psychological distress and perceived barriers to care for rural lesbians. Journal of Gay and Lesbian Mental Health 2015; 19(4): 347-369. https://doi.org/10.1080/19359705.2015.1041629
65. Henderson JT, Weisman CS, Grason H. Are two doctors better than one? Women's physician use and appropriate care. Women's Health Issues 2002; 12(3): 138-149. https://doi.org/10.1016/S1049-3867(02)00134-2
66. Scholle SH, Kelleher K. Assessing primary care performance in an obstetrics/gynecology clinic. Women & Health 2003; 37(1): 15-30. https://doi.org/10.1300/J013v37n01_02
67. Cascade E, Kalali AH, Halbreich U. Antidepressant prescribing by specialty and treatment of premenstrual dysphoric disorder. Psychiatry (Edgmont) 2008; 5(12): 14-15.
68. Mravcak SA. Primary care for lesbians and bisexual women. American Family Physician 2006; 74(2): 279-286.
69. American College of Obstetricians and Gynecologists, Committee on Health Care for Underserved Women. Health care for lesbians and bisexual women (Committee opinion no. 525). (Internet) 2012. Available: http://www.acog.org/Resources-And-Publications/Committee-Opinions/Committee-on-Health-Care-for-Underserved-Women/Health-Care-for-Lesbians-and-Bisexual-Women (Accessed 23 April 2015).
70. Quinn GP, Schabath MB, Sanchez JA, Sutton SK, Green BL. The importance of disclosure: lesbian, gay, bisexual, transgender/transsexual, queer/questioning, and intersex individuals and the cancer continuum. Cancer 2015; 121(8): 1160-1163. https://doi.org/10.1002/cncr.29203
71. McNair R. Lesbian health inequalities: a cultural minority issue for health professionals. The Medical Journal of Australia 2003; 178(12): 643-645.
72. American College of Obstetricians and Gynecologists, Committee on Ethics. At-risk drinking and illicit drug use: ethical issues in obstetric and gynecologic practice (Committee opinion no. 422). (Internet) 2008. Available: http://www.acog.org/Resources_And_Publications/Committee_Opinions/Committee_on_Ethics/At_Risk_Drinking_and_Illicit_Drug_Use_Ethical_Issues_in_Obstetric_and_Gynecologic_Practice (Accessed 23 April 2015).
73. American College of Obstetricians and Gynecologists, Committee on Obstetric Practice. Screening for depression during and after pregnancy. (Committee opinion no. 453). Obstetrics and Gynecology 2010; 115(2 Pt 1): 394-395.
74. Bostwick WB, Boyd CJ, Hughes TL, McCabe SE. Dimensions of sexual orientation and the prevalence of mood and anxiety disorders in the United States. American Journal of Public Health 2010; 100(3): 468-475. https://doi.org/10.2105/AJPH.2008.152942
75. King M, Semlyen J, Tai S, Killaspy H, Osborn D, Popelyuk D, Nazareth I. A systematic review of mental disorder, suicide, and deliberate self harm in lesbian, gay and bisexual people. BMC Psychiatry 2008; 8(1): 70. https://doi.org/10.1186/1471-244X-8-70
76. Poleshuck EL, Woods J. Psychologists partnering with obstetricians and gynecologists: meeting the need for patient-centered models of women's health care delivery. American Psychologist 2014; 69(4): 344-355. https://doi.org/10.1037/a0036044
77. Koh A. Use of preventive health behaviors by lesbian, bisexual, and heterosexual women: questionnaire survey. The Western Journal of Medicine 2000; 172(6): 379-384. https://doi.org/10.1136/ewjm.172.6.379
78. Rayman KM, Edwards J. Rural primary care providers' perceptions of their role in the breast cancer care continuum. Journal of Rural Health 2010; 26(2): 189-195. https://doi.org/10.1111/j.1748-0361.2010.00281.x
79. Meyer IH, Wilson PA. Sampling lesbian, gay, and bisexual populations. Journal of Counseling Psychology 2009; 56(1): 23-31. https://doi.org/10.1037/a0014587

