Attracting and retaining healthcare providers in rural locations in the USA has been an issue for more than two decades1-4. In 2010, it was estimated that 11% of physicians serve the 19% of the US population that lives in rural areas5. Many health sciences education institutions across the US have developed special programs to encourage students to become health care providers in rural locations1,6,7. One approach is the use of community-based education experiences through rural track programs. Rural track programs are designed to identify, admit and educate students with a declared interest in future rural practice, and are housed within existing schools of medicine or colleges of health sciences8. Community-based educational experiences offered through rural tracks immerse students in rural settings to provide a tangible example of practice among rural populations. As of 2013, there were approximately 38 rural track programs for medical students operating in the USA8; additionally, several institutions offer rural tracks and clerkships for physician assistant and nurse practitioner students. Rural track programs are generally small, enrolling 10 to 25 students per cohort, and many offer longitudinal experiences, wherein a student is located at one clinical site for several months8,9.
Assessment of the success of rural track programs has been conducted using retrospective questionnaires10, in-depth interviews11, and the analysis of program retention statistics. Data from these studies indicate that students who are immersed in a rural setting during training are more likely to enter practice in a rural setting compared to students following a traditional curriculum10,12. Several factors have been shown to influence this proclivity for rural practice, including increased duration of rural training period, student rural origin, and overall quality of the rural training environment8,12,13. Thus, it appears that rural tracks providing longitudinal, community-based education positively contribute to the workforce needs of rural communities. More information is needed to understand the training experiences of students who have participated in longitudinal rural training programs beyond workforce outcomes.
A limited number of studies have investigated students' perceptions of longitudinal rural training programs. Generally, these students are more satisfied with experiences at rural training sites compared to students at urban academic institutions, as they are provided with a more personalized education and increased opportunity for the practical application of clinical skills14. However, the use of researcher-designed questionnaires and interviews may not fully capture students' training experiences during a rural immersion program. To address this shortfall in the current literature, photovoice methodology was used as a novel approach for the assessment of medical and health sciences student experiences in two longitudinal rural immersion programs at an academic medical institution. The goal of the present study was to gain a better understanding of medical and physician assistant students' experiences beyond what is normally captured through testing and researcher-guided interviews.
Photovoice
Photovoice is a participatory research methodology wherein participants visually document their day-to-day lives with photographs that may be accompanied by a statement summarizing how the photograph represents their experiences. The photovoice technique was introduced in the late 1990s with three goals: (1) to enable people to record and reflect their community's strengths and concerns, (2) to promote dialog and knowledge about issues through discussion of photographs, and (3) to reach policy makers15. Since then, visual techniques have been increasingly used in public health research to integrate the knowledge of the social scientist with that of the research participant about community health16. Photovoice has been demonstrated to capture a more direct understanding of participants' experiences and their perceptions when compared to data collected solely by the researcher17.
In the present study, photographs were used to provide a visual representation of students' experiences, as well as to provide insight into what students gained from the rural immersion programs offered at their academic medical institution.
Program descriptions
The research site was an academic medical institution that offers two programs with rural clinical training: Rural Medical Education Program (RMED) and the Physician Assistant Program (PA). The RMED program places a small number of third-year medical students in rural communities full-time for 19 or 36 consecutive weeks. During this time, RMED students participate actively and extensively in continuous and comprehensive care of their preceptors' patients across the age spectrum in both ambulatory and hospital settings. The PA program is divided into two training formats: the first 15 months are dedicated to didactic training, while the final 12 months consist of 11 clinical preceptorships of 4 weeks each. All PA student preceptorships are scheduled in various rural or medically underserved communities throughout New York state. Thus, the majority of PA students underwent longitudinal training in rural locations as a function of the program structure.
Participants
All third-year medical students participating in RMED and all second-year PA students from the 2014 and 2015 student cohorts were recruited to the study during their respective program orientations. During the orientation, a research team member reviewed the consent form and provided a brief overview of the photovoice method, highlighting the types of pictures that were sought in terms of quality and content. Specifically, pictures could not violate patient privacy regulations under the Health Insurance Portability and Accountability Act. As students began their clinical rotations, they submitted their photos and vignettes to the research team via email. All photos and vignettes were submitted by the conclusion of each cohort's term.
Preliminary analysis
All members of the research team participated in the preliminary analysis of the photographs and vignettes separated by training program for the 2014 cohort. The findings of the preliminary analyses were shared with participants from each program during two separate focus group sessions. Both focus groups were conducted in July 2014. Students were recruited for focus group participation by email invitation.
Focus groups and confirmatory feedback
The goal of the focus group sessions was to obtain feedback on the preliminary analyses from the photovoice participants. The feedback received from the focus groups was used to validate the preliminary 2014 cohort results, as well as provide insight into additional themes.
After completing the focus groups, dyads within the research team were formed to conduct thematic analysis of the transcripts, with one dyad assigned to each program. Following this analysis, the research team convened to review and confirm the finalized themes and concepts. The finalized themes were summarized into a short document and shared with the 2014 cohort student participants of each program by email for confirmatory feedback.
Student photographs and vignettes obtained from the 2015 cohort were analyzed and compared to the findings from the 2014 cohort submissions and focus groups to identify new themes or concepts. Separate focus groups were not conducted with the 2015 cohort due to saturation in the themes identified through student photographs and vignettes. Results from this analysis were then summarized and shared with the 2015 cohort student participants via email for confirmatory feedback.
Ethics approval
The Institutional Review Board for the Protection of Human Subjects at SUNY Upstate Medical University granted an exemption from review for this study because it was 'conducted in (an) established or commonly accepted educational setting'.
Thirty-eight students from the RMED program and 35 students from the PA program were approached for participation; of these, five of the 2014 RMED cohort, six of the 2014 PA cohort, and 17 of the 2015 RMED cohort students enrolled in the project. In total, 163 photographs with vignettes were submitted by the 28 participants. On average, six photographs were submitted per participant. However, of the 163 photographs received, 49 either contained identifiable content and could not be accepted for analysis, or did not contain subject matter relevant to the research question (eg photographs of scenery with no explanatory vignettes). Thus, 114 photographs and accompanying vignettes were analyzed. Four students attended the 2014 RMED cohort focus group and five attended the 2014 PA cohort focus group.
The final results of the analyses, which incorporated the feedback and insights provided by student participants across both cohort years, identified two overarching themes of students' experiences training in a rural environment:
- The learning environment extends beyond direct clinical teaching.
- Sociocultural diversity impacts what students learn and how they learn it.
Each theme contained subconcepts, or subthemes (Table 1).
Theme 1: The learning environment extends beyond direct clinical teaching
Students frequently wrote and spoke about connections with both the clinical and non-clinical communities as critical aspects of their learning in the rural setting. Many students felt they were able to make deep connections with preceptors and other clinical faculty, and that the trust fostered in these relationships often translated into hands-on opportunities and engagement. Five students reflected that they felt respected by their preceptors and care teams to a higher degree than previously experienced outside of their rural training setting, and that this level of respect enhanced their training experience:
Being treated as an equal has profoundly affected my perspective of medicine, in that medical training is not all about lecturing, learning science, and evidence based therapies. Rather ... it is very humanistic and includes a great deal of social work, cultural awareness, off-label treatments, and pearls only learned with experience.
Students also discussed connecting to patients and community members through social interactions in their communities and how these encounters, outside of clinical care settings, led to increased awareness of the healthcare concerns among the population. For example, one student stated during a focus group discussion:
They taught me how to ski and they took me snowmobiling. So, it was great! By the end of the winter I felt like I really belonged and I really appreciated the community and the things that they did.
This same student took a photograph of snowmobile helmets at a restaurant and reflected on the types of injuries sustained while snowmobiling.
As students made connections with faculty and community members, they also reflected on the relationships that rural physicians have with their patients. Overall, by the end of their training, many students noticed that clinicians had deeper relationships with their patients in the rural setting due to the interconnected nature of their rural community:
There might be a little more trust because they're not just a physician and a patient, they're neighbors or they're relatives or they've taken care of grandkids, cousins, aunts, and uncles, and everything is so connected in a rural area.
The sense of community that glues these towns together comes through in your medical practice, between patients and physicians, as well as between physicians and other colleagues.
In addition to the importance of interpersonal connections, students spoke about the spaces, both physical and temporal, that rural settings provided for their reflection. Some students talked about having more space to reflect on their learning experiences in these settings; they took photos of places where they spent time and talked about journaling, hiking, running, and simply feeling at ease. This time to reflect was mentioned by seven students during the focus groups, and was echoed in 26% of the photographs. Students felt that time and space for reflection contributed to their ability to manage the stresses of medical training and the provision of medical care:
The photos I am submitting [eg Fig1] illustrate several of my favorite places where I go to refresh my mind and body so that I can be mentally and physically prepared to be the best medical provider that I can be.
Finally, students photographed and spoke about infrastructure, often comparing what they saw in rural versus urban settings. Students discussed how a lack of providers (particularly specialists), missing or outdated technology, and remote locations impacted patient care in rural settings. One student explained how they felt 'shocked' at how long patients go without receiving care:
It's shocking when you see the patients come in and they go so long without fixing things and [the patients] don't know much about their care because there's just not enough providers there.
Another student reflected on the physical barriers to receiving health care:
The connection between many people and places in rural communities can be a long road. This is an important factor in health care, as transportation becomes a significant consideration for patients needing prompt emergency care, as well as just being able to make it to their scheduled appointments.
Along with the challenges, the students also learned about opportunities to improve care. For example, one student discussed, in a photograph vignette (Fig2), the importance of new technologies, such as telemedicine, as a means of connecting patients with needed specialists:
It is hard to recruit specialists to move to a smaller town to begin with, but then to have them help patients in the surrounding smaller towns is very difficult. This [portable telemedicine system] allowed specialists to see patients in these surrounding communities without taking two hours each day just to drive there and back.
Four students described how recent changes to the healthcare system impacted the provision of care for rural communities, revealing that the rural training environment can facilitate reflection about the non-clinical aspects of healthcare provision. One student explained:
Hospital/medical politics have really forced medical care to change in a way many rural hospitals struggle to keep up with. Many smaller hospitals are being bought out by bigger organizations and they are struggling to stay afloat to continue serving their community.
Table 1: Summary of themes related to student training experiences in a rural environment
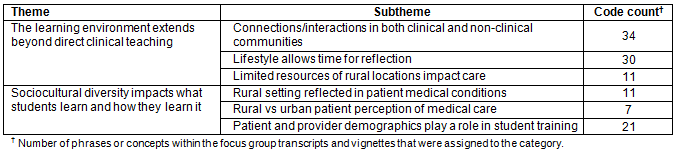

Figure 1: Time to reflect was an important theme: students felt that time and space for reflection contributed to their ability to manage the stresses of medical training and the provision of medical care.

Figure 2: Students photographed and spoke about infrastructure, often comparing what they saw in rural versus urban settings including how a lack of providers (particularly specialists), missing or outdated technology, and remote locations impacted patient care.
Theme 2: Sociocultural diversity impacts what students learn and how they learn it
Many students noted ways that sociocultural diversity, specifically diversity of occupation, education, attitude, and perception of medical care, impacted their learning in rural environments. For example, while on site, students encountered medical conditions that they had not seen in their training in urban settings. These conditions included injuries related to farming and snowmobiling accidents and diseases related to working with animals. One student explained:
Farm life involves a close relationship between farmers and animals. An understanding of potential infections, illnesses, and injuries that can result from this close interaction is important in rural medicine. [Figure 3]
Students reflected that exposure to the new variety of medical conditions seen in the rural environment helped prepare them for future practice in similar geographic settings.
Several students also stated that the lifestyle differences between rural and urban communities translated into important differences in the patients' perception of medical care. For example, one student felt that farming communities are more connected to the cycle of life and death, and patients from these communities tend to view illness and death with more acceptance than individuals from urban environments. Several other students felt that the ethos of rural communities led patients to prioritize work responsibilities above compliance with medical advice:
The work ethic and resilience of rural laborers makes for some very non-compliant patients when treatment calls for rest.
Farmers have a unique set of medical needs, as well as an impressive work ethic and deeply ingrained stoicism. Physicians treating this population often have to be creative in treatment plans. They must recognize and accept that the patient's farm duties will often come before the patient's own medical needs.
In addition, students expressed that they felt more respected and acknowledged in the rural community than they had in urban settings due to their role as medical providers. One student explained:
It's a different population and I thought I got a lot more respect as a student up there than I did here, from the patients as well as the physicians.
Students felt that this increased level of respect from both the medical community and patient community allowed them to function more as medical professionals than as students, and the higher level of trust bolstered their confidence.
The final subtheme related to sociocultural diversity focused on the patient and provider demographics that students encountered while on site. Some students talked about the farming, Mennonite (a Christian group), and refugee communities they encountered, but others felt that the patient demographics in rural areas were more homogenous than in urban settings. For some, this homogeneity made it easier to communicate with patients and reach a mutual understanding. However, three students mentioned that the low levels of education among many of their patients sometimes made it difficult to explain diagnoses and treatment plans. One student was able to leverage aspects of rural culture to contextualize medical explanations and effectively communicate with patients:
So, like, likening their body to their tractor or to a car. And then they were like, 'Oh no, yeah that makes sense.'... Not dumbing it down or putting it in layman's terms or anything like that, but putting it in a way that makes sense to them.
Students also felt that providers working in rural areas should strive to integrate themselves within the local community, especially if they are not originally from that area. One student, in observation of a local preceptor, felt that doing so fostered a deeper sense of trust between medicine and the community:
Most physicians don't grow up in the communities they practice in. Integration into the community is a process, one that can sometimes take decades, but it seems to bring great rewards, particularly in a community small enough for a physician to have an important identity.

Figure 3: Students encountered medical conditions that they had not seen in their training in urban settings.
Discussion
Qualitative investigations have provided information regarding the influence of rural training experiences on medical student education and future practice, using methods including in-depth interviews, focus groups and survey research. In this study, the photovoice method was applied to gain insight into the impact of the longitudinal rural training environment on student learning using student-generated photography and commentary. The primary strength of the photovoice method is that researchers gather real-time, visual representations of students' lived experiences, as defined by the students themselves. The use of this participatory research methodology allows us to understand which aspects of the rural training experience resonated most among students as they occurred, rather than a post-hoc exploration of researcher-generated questions about the training experience.
Several findings from this study corroborate results of previous research regarding longitudinal rural clinical training programs. Specifically, positive student reflections on increased hands-on training opportunities, higher levels of responsibility in patient care, the development of strong interpersonal skills, and increased exposure to continuity of care have been evidenced through prior investigations of longitudinal clerkship models18-20. However, the present study also presents new insights into the student experience in a rural training program regarding mentorship, self-efficacy and personal reflection. In both the photograph vignettes and the focus group discussions, most participants spoke about the professional and personal growth they experienced during their rural training. The increased responsibilities and practice of skills students experienced at their rural training sites allowed them to feel more like practicing clinicians and less like students. Most of the students used the rural environment to reflect on these training experiences and their plans for the future.
This study adds to the current body of research by suggesting that students utilize rural spaces to process the emotional development that is required as they begin to take greater responsibility in the care of patients. Twenty-six percent of the photographs returned to the study team referred to dedicated time students spent to reflect upon their experiences in training, relieve stress, and connect with their surrounding environment. The content of student photographs, coupled with the results of the focus group sessions, indicate that students value these periods of reflection for both personal and professional growth. Eight students mentioned during both the focus groups and in the photograph vignettes that these moments of reflection were unique to their rural training environment.
Findings from this study also indicate that in addition to providing a venue in which students can engage in continuity of clinical care, longitudinal rural track programs provide a structure and environment conducive to reflection and integration of these experiences into practice. As with any skill, time and practice are needed to become proficient. The students in the sample demonstrated self-reflection skills that they can carry throughout residency and their careers as physicians.
Limitations
There are limitations to this study. First, the study may have encountered selection bias, as the students who participated in this study represent a fraction of the student cohorts (33% of 2014 RMED cohort, 17% of 2014 PA cohort, and 65% 2015 RMED cohort). It is possible their experiences and opinions are different from their fellow students enrolled in the programs that did not participate in the photovoice study, as well as students participating in previous cohorts of the two programs. Additionally, the results of this investigation are not generalizable to students participating in programs at other institutions or locations.
It is also important to note that the 2014 PA cohort students were no longer in training at the university after the focus group sessions were completed. This may have contributed to their reduced participation in the final confirmatory feedback activity. Additionally, due to the discordant training schedules of the RMED and PA programs, no PA students from the 2015 cohort were recruited for participation.
Lastly, due to concerns regarding patient and clinician privacy, students were unable to submit photographs containing content that could identify individuals or training site locations. Several participants mentioned that this element of the study protocol inhibited their ability to capture important components of their training experience. While some aspects of the rural longitudinal training experience were not captured in the photographs and vignettes due to this limitation, the focus group sessions provided an opportunity for students to share and discuss those components of their rural training.
Research on alternative training programs, including longitudinal rural medical education programs, provides evidence that students are granted more hands-on experiences and greater opportunities to practice their skills in these settings; this is consistent with the findings of this study. However, less is known about how students process or reconcile experiences from this training. An important finding from this study indicates the students trained in a rural, longitudinal setting not only have the opportunity and time for reflection, but also they place a value on this reflection; these experiences reach beyond the norms of traditional academic medicine. The use of the photovoice technique illustrated the importance of these periods of reflection for the students in the study and provided them with a unique mechanism through which they could reflect on these experiences through the art of photography.
References
1. Geyman JP, Hart LG, Norris TE, Coombs JB, Lishner DM. Educating generalist physicians for rural practice: How are we doing? Journal of Rural Health 2000; 16(1): 56-80.
2. Rosenblatt RA, Hart LG. Physicians and rural America. Western Journal of Medicine 2000; 173(5): 348-351.
3. MacDowell M, Glasser M, Fitts M, Nielsen K, Hunsaker M. A national view of rural health workforce issues in the USA. Rural and Remote Health (Internet) 2010; 10(3): 1531. Available: www.rrh.org.au (Accessed 25 August 2015).
4. Arvantes J. Radical primary care changes needed to meet coming demand for health care. Annals of Family Medicine. 2013; 11(2): 184-185.
5. Rosenblatt RA, Chen FM, Lishner DM, Doescher MP. The future of family medicine and implications for rural primary care physician supply. WWAMI Rural Health Research Center; final report #125. (Internet) 2010. Available: https://www.ruralhealthresearch.org/publications/758 (Accessed 14 June 2015).
6. Wheat JR, Leeper JD, Brandon JE, Guin SM, Jackson JR. The rural medical scholars program study: data to inform rural health policy. Journal of the American Board of Family Medicine 2011; 24(1): 93-101.
7. Curran V, Rourke J. The role of medical education in the recruitment and retention of rural physicians. Medical Teacher 2004; 26(3): 265-272.
8. Deutchmann M. Medical school rural tracks in the US policy brief. Aurora, CO: National Rural Health Association, 2013.
9. University of Colorado School of Medicine, Department of Family Medicine. Rural track program list. (Internet) 2013. Available: http://ruralmeded.org/rural-tracks-program-list. (Accessed 10 June 2015).
10. Florence JA, Goodrow B, Wachs J, Grover S, Olive KE. Rural health professions education at East Tennessee State University: survey of graduates from the first decade of the community partnership program. Journal of Rural Health 2007; 23(1): 77-83.
11. Van Schalkwyk SC, Bezuidenhout J, Conradie HH, Fish T, Kok NJ, Van Heerden BH, et al. 'Going rural': driving change through a rural medical education innovation. Rural and Remote Health (Internet) 2014; 14: 2493. Available: www.rrh.org.au (Accessed 25 August 2015).
12. Sen Gupta T, Woolley T, Murray T, Hays R, McCloskey T. Positive impacts on rural and regional workforce from the first seven cohorts of James Cook University medical graduates. Rural and Remote Health (Internet) 2014; 14: 2657. Available: www.rrh.org.au (Accessed 25 August 2015).
13. Shannon CK, Jackson J. Validity of medical student questionnaire data in prediction of rural practice choice and its association with service orientation. Journal of Rural Health 2015; 31(4): 373-381.
14. Garrard J, Verby JE. Comparisons of medical student experiences in rural and university settings. Journal of Medical Education 1977; 52(10): 802-810.
15. Wang C, Burris MA. Photovoice: concept, methodology, and use for participatory needs assessment. Health Education & Behavior 1997; 24(3): 369-387.
16. Lorenz LS, Kolb B. Involving the public through participatory visual research methods. Health Expectations 2009; 12(3): 262-274.
17. Rich M, Lamola S, Gordon J, Chalfen R. Video intervention/prevention assessment: a patient-centered methodology for understanding the adolescent illness experience. Journal of Adolescent Health 2000; 27(3): 155-165.
18. Teherani A, Irby DM, Loeser H. Outcomes of different clerkship models: longitudinal integrated, hybrid, and block. Academic Medicine 2013; 88(1): 35-43.
19. Thistlethwaite JE, Bartle E, Chong AAL, Dick ML, King D, Mahoney S, et al. A review of longitudinal community and hospital placements in medical education: BEME guide no. 26. Medical Teacher 2013; 35(8): e1340-e1364.
20. Walters L, Greenhill J, Richards J, et al. Outcomes of longitudinal integrated clinical placements for students, clinicians and society. Medical Education 2012; 2012;46(11):1028- 1041.





