The United States Department of Agriculture (USDA) describes a food desert as an urban neighborhood or rural town without ready access to fresh, healthy, and affordable food1. Food deserts are further defined by meeting at least one of two criteria: (1) low-access communities where at least 500 persons and/or at least 33% of the census tract's population live more than 1.6 km (1.0 mile) from a supermarket or large grocery store in urban tracts, or 16 km (10 miles) in rural tracts; and (2) low-income communities with a poverty rate of 20% or greater, or a median family income at or below 80% of the area median family income1. Instead of supermarkets and grocery stores, these food desert communities may have no food access or are served only by fast food restaurants and convenience stores that offer few healthy, affordable food options1.
Living in a food desert brings upon its residents a unique set of health-related challenges. Limited access to healthy food and the food insecurity caused by food deserts are significant contributors to obesity and chronic disease1-5. Travel distance to a grocery store is associated with higher rates of obesity in children and adults3,6. Ghosh-Dastidar and colleagues predicted that for every 1.6 km (1.0 mile) traveled to purchase food the odds of being obese increase by 5.0%3. The prevailing logic also says that if you cannot buy healthy food, you cannot remain healthy. Food insecurity causes people to experience hunger, reduced food intake, disruption of eating patterns, and poor health2,5. Most of these health-related problems associated with food deserts are thought to be a result of poor diet quality5-8. People who live in food deserts spend less money on fresh fruits and vegetables and more money on poor quality food items6,8,9.
An estimated 2.3 million rural Americans live in food deserts1. With this reality, the goal is to eliminate food deserts in the USA1. Consequently, the USDA, Department of the Treasury, and Department of Health and Human Services have given priority funding to projects and interventions that establish healthy food outlets and distribution centers in identified food deserts1. Some examples of general project categories supported by this initiative include farmers' markets, direct-to-consumer marketing of food, food value chains, food hubs, wholesale markets, and local food directories to help people find locally grown and raised healthy food1. The USDA provides some 'success stories' or anecdotal evidence that food deserts are being eliminated, but the USDA does not provide any data about the number of food deserts that have been eliminated or the number of Americans who are no longer living in a food desert environment1.
At a point when it seems like food deserts are being eliminated, hundreds of grocery stores are closing across the USA. At least 291 US grocery stores closed during the year 2015. The most common reason for closure was weak economic performance or bankruptcy10. The closure of so many grocery stores must certainly cause rise to more food deserts, particularly in rural communities where there were previously no competitive food markets.
It appears that much of the effort of the USDA to eliminate food deserts is offset by the current reality of food marketing economics. Amidst this back-and-forth of food availability, it would be important to know the net effect of the opposing forces for food availability on American food deserts. Even if the net effect is that the total number of food deserts is being reduced, it would be important to know how communities adapt to an emerging food desert, where previously there was none.
There is a void in both the scientific literature and the popular press on how a community could adapt to an impending or foreseeable food desert. The available literature focuses solely on how food desert communities currently survive their existing food insecurity, how food desert communities have eliminated their local food desert, or on descriptive and intervention studies on food desert community member shopping and dietary behaviors.
If a rural community is facing a forthcoming food desert, due to a grocery store closure(s) and/or an economic downturn that increases the community's poverty level, how does the community adapt? The answer to this question, whether the community adaptations produced negative or positive outcomes, would be meaningful. The answer would help other communities facing a similar situation as well as provide insight that may help the USDA in its struggle with food deserts. The purpose of this study was to investigate how a small rural community in the south-eastern USA adapted to an impending food desert - proactive adaptations and reactive adaptations. This is particularly important because rural Appalachian food deserts have some of the highest rates of cardiovascular disease and mortality in the USA4, and it is well known that poor nutrition is a risk factor for cardiovascular disease11.
Research setting and significance
Alderson is a small rural town in the south-eastern part of the state of West Virginia, which sits in the center of the Appalachian region of the USA. Appalachia is a region that follows the spine of the Appalachian Mountains, from southern New York State in the north-eastern USA to the northern part of the state of Mississippi in the southern USA. Appalachia includes the entire state of West Virginia and parts of 12 other states12. The Appalachian economy depends upon mining, forestry, agriculture, chemical industries, and heavy industry, with limited manufacturing and service industries. Appalachia is a region of widespread economic contrasts, with 17% of Appalachia living in poverty12.
The Appalachian town of Alderson, West Virginia, has 1184 persons who make up 315 family units13,14. Alderson West Virginia's population is made up of 91% Caucasians, 5% African Americans, 3% Hispanics or Latinos, and 1% other. The town is unique in that it sits on the Greenbrier River, with half of the city on the Greenbrier County side of the river and half on the Monroe County side. Nonetheless, the city is unified and run by one city government13,14.
Alderson recently became a food desert, by all definitions, when its only grocery store closed its doors on 31 December 2014. The closest grocery store for Alderson residents is now 17.7 km (11 miles) away. The closing of the grocery store left Alderson residents served by four fast food restaurants and two convenience stores. In addition, the poverty rate in Alderson had just reached 22.9%, with 52% of its children living in poverty13,14. This rate of poverty is much higher than the national poverty rate of 14.8%15. Part of the rise in Alderson's poverty is the lack of economic development and the failure of income levels to rise, causing a relative drop in per capita income of 16% over a 3-year period8. All of these changes, with the final one being the closing of Alderson's only full-service grocery store, left Alderson unquestionably in a food desert. Alderson is now on the USDA list of food deserts16.
News in October 2014 of the impending grocery store closure alerted the community members that Alderson would soon become a food desert. Alderson community members rallied together to proactively face this impending food desert. Community members organized themselves by creating a food hub, a business or organization that actively manages the collection, distribution, and marketing of food products. These food products are generally produced locally, and their distribution and sale in local markets benefits local businesses as well as individual community members. The Alderson Community Food Hub includes the Alderson Community Market, a community garden, and the Alderson Green Grocer. The Alderson Community Market is the local name for what others usually refer to as a farmers' market. The Alderson community garden is a tract of land, within the city limits, where any community member can rent a plot of land to grow a garden. The Alderson Green Grocer is a small grocery cooperative that was initiated as the Alderson community became a new food desert. The new Green Grocer has a store front where residents can make food purchases.
The purpose of this study was to learn how the Alderson Food Hub responded to the creation of the new food desert, when the town's only grocery store closed. Because the Alderson Community Market and garden already existed prior to the closing of the grocery store, this study was able to monitor how the community market and garden were affected by the grocery store closure. The Green Grocer opened its doors on 1 April 2015, 3 months after the full-service grocery store closing. The sales activities of the Green Grocer were monitored for 3 months to see which food desert needs were being met or unmet by this food hub cooperative.
It is beyond the scope of this article and out of context with this research project to present all the legal work and organizational issues that had to be overcome in order to make the Alderson Food Hub functional. This study is focused on two aspects of response to the impending food desert - community member behaviors and business activities. The research agenda was categorized into survey activities regarding individual community member food shopping behaviors before and after the food desert; restaurant activities before and after the food desert, community market response to the food desert, and the Green Grocer sales activities within the food desert.
Procedures
The Center for Rural and Community Health (CRCH) at the West Virginia School of Osteopathic Medicine was contacted by the president of the Alderson Community Food Hub about the impending food desert and opening of the Alderson Green Grocer. This led to the development of a community-based participatory research effort. Members of the CRCH research team met with the president and other members of the Alderson Community Food Hub Board of Directors various times to organize the study. (Details of the community meetings are irrelevant to the focus of this article.) An open-forum meeting was also held for any lay member of the community to attend. The study was designed so that all of the community stakeholders would be surveyed about their behaviors and business activities related to the emerging food desert. Details for each facet of survey and data collection follow.
Data collection
Community member survey: A 17-item survey was designed to investigate individual community member food acquisition behaviors before and after the emergence of the food desert. The survey contained questions relevant to participant demographics, use of the national Supplemental Nutrition Assistance Program (SNAP), use of the Women, Infants, and Children (WIC) program, shopping at the new Alderson Green Grocer, local restaurant use, gardening, and reliance on the Alderson Food Pantry. (Food pantries are non-profit charitable organizations that store and distribute food locally to people who, without their help, would experience hunger and/or malnutrition. Food pantries distribute food freely or at a nominal cost to low-income residents and often the homeless. Many food pantries in the USA are run by faith-based organizations.) The Alderson Food Pantry is run by the Alderson Ministerial Association, represented by six Christian religious denominations.
The community member survey was delivered to community members through several mechanisms. Four members of the research team went door-to-door one Saturday to gather community survey data. Surveys were placed in businesses most frequented by Alderson community members. These included the Alderson pharmacy, the family restaurant, the community market, the food pantry, and the newly established Green Grocer. One adult family member completed the survey for their respective family unit. The survey was administered 2-3 months after the opening of the Food Hub's Green Grocer. The survey was also administered to local church congregations.
Food price comparison: When the full-service grocery store in Alderson closed, the nearest grocery store was 17.7 km (11 miles) distant. One of the study questions was to determine how competitive the new Green Grocer was compared to large grocery stores in the nearest neighboring city. The research team constructed a list of 27 commonly purchased food items (eg milk, eggs, bread, lettuce, cheese, ground beef) and manually performed a price comparison among the new Alderson Green Grocer, the nearest large national supermarket chain store, a discount grocery warehouse, and an independent grocery chain store. The independent grocery store chosen is part of the Independent Grocers Alliance. The large national supermarket was selected because it is the nearest grocery superstore to Alderson. The discount food warehouse was chosen because it was the closest discount grocery warehouse. The independent grocery store was selected because it is part of the same independent grocery store chain as the store that closed in Alderson. The selection of the independent grocery store allowed the research team to determine how competitive pricing between the Green Grocer and the Alderson independent grocer would be if the Alderson independent grocer had not closed. The large national supermarket, discount warehouse, and independent grocer are all within 2.4 km (1.5 miles) of each other.
In addition, price comparisons were made to include the cost of gas/petrol for travel to the grocery stores. Estimates were calculated in US dollars at the cost when the survey was taken (US$0.63 per liter or US$2.40 per gallon). The rate of 8.5 km per liter (20 miles per gallon) was used, because this is the rate of the average American pick-up truck and sport utility vehicle, the most popular two vehicles in Alderson. The distance of a radius of 4.8 km (3.0 miles) was used to include the distance Alderson residents would travel to the Green Grocer.
Green Grocer survey: Data for the new Green Grocer were obtained through a survey that was completed by the store manager and through procurement of sales receipts that were provided by the store manager (cash register receipts). The main data obtained from the Green Grocer were daily customer count, average amount spent per purchase, best-selling items, worst-selling items, requested items, and percentage of sale items obtained from local producers.
Restaurant survey: Alderson has four fast food restaurants: a family restaurant, a sandwich shop, a smokehouse bar and grill, and a fast food restaurant. An eight-item survey was designed to determine the food acquisition and customer sales for the restaurants. The survey determined how much of the restaurant food was supplied from local producers, and if this changed with the closing of the grocery store. The survey also determined if customer food sales changed with the grocery store closure, and if customers requested healthier foods due to the grocery store closing.
Community garden: The Greenbrier Catholic Church and Federal Emergency Management Agency provide community garden plots, at two city locations, for any community member. Each garden plot is 3 m by 3 m (10 ft by 10 ft) in size and costs US$10 per year. The research team surveyed how many community garden plots and home garden plots were planted before and after the closure of the Alderson grocery store.
Community market: The Alderson Community Market is made up of various vendors who sell their wares every Saturday morning from 8.30 am until 12.30 pm at the market square in the town center. Approximately 12 vendors participate each week, but not every vendor participates during any given week. Some vendors are farmers and some are craft persons. The market runs from May through October. An extension of the community market is the mobile food unit. The mobile food unit distributes locally produced food on a monthly basis to Alderson Manor, which is a community housing project for the elderly and the economically disadvantaged. The community member survey, previously described, questioned community members about use of the community market. One researcher traveled with the mobile food unit during the months of July and August 2015, to record its food distribution activities.
Data analysis
All data were compiled into spreadsheet format and analyzed using the Systat v13.1 statistical software program (Systat Software, Inc.; http://www.systatsoftware.com). Demographic and descriptive data were compiled and analyzed using basic statistics (means, median, range, standard error of the mean, percentages, and ratios). Group comparisons for numerical data were conducted using an independent t-test for separate group comparisons and a dependent t-test for within-group pre- and post-comparisons. An analysis of variance (ANOVA) was used for multiple group mean comparisons. Group-by-group comparisons for response rates or ratios were made by testing the equality of two proportions test. Categorical data were analyzed by the use of the χ2 test, the equality of two proportions test, or frequency distribution analysis. Group averages are reported as mean ± standard error of the mean (SEM). Significance for all analyses was set at the p<0.05 level.
Ethics approval
The study protocol was submitted to the West Virginia School of Osteopathic Medicine Institutional Review Board for research involving human subjects (approval number WVSOM IRB #2015-7). The study met the 45 CFR 46.101 (b) (2) research involving the use of educational tests (cognitive, diagnostic, aptitude, achievement), survey procedures, interview procedures or observation of public behavior criteria for Exempt status.
There are 315 families residing in Alderson. The community member survey was completed by 155 of these families. According to sample size calculations, this family response rate of 49% was a large enough sample size to accurately represent the Alderson family population17. Accordingly, a 5% margin of error was calculated for the community survey response17.
One adult (≥18 years) answered the community member survey for his/her respective family. The responders were 30% men (n=46) and 70% women (n=109). The average age of the community member survey respondent was 56.7±2.2 years for men and 52.5±1.8 years for women (mean±SEM). There was no significant difference in age between the men and women respondents (p=0.17). Of the respondents, 25% (n=39) were using SNAP, and only 4% (n=6) were using the WIC program.
Almost all of the respondents (97%, n=150) were aware of the new Food Hub Green Grocer, and 91% (n=141) had shopped at the Green Grocer. Table 1 shows the sample population's frequency of shopping at the Green Grocer. Even though a majority of the sample population regularly shopped at the Alderson Green Grocer, 77% (n=120) of them did most of their grocery shopping at a store more than 17.7 km (11 miles) from Alderson. The number of long-distance grocery shopping trips families made after the food desert (3.3±0.4 trips per month) did not change significantly (p=0.16) from the number that were made before the food desert (2.8±0.3 trips per month).
The price comparisons for the 27 food items at the four grocery stores are shown in Table 2. The estimated cost savings to travel to the nearest grocery store outside of Alderson to buy these 27 common food items would be US$18.77. The costs of the 27 food items at the Green Grocer would be US$5.42 more than they would have been if the Alderson grocery store had not closed.
The Green Grocer is open for business from 10.30 am until 7.00 pm Monday through Saturday. The store hours for the discount warehouse and independent grocer are 8.00 am to 10.00 pm, while the national supermarket store is open 24 hours each day. These three stores are all open 7 days a week. The Green Grocer survey revealed that the store has an average of 97 customers a day, and that the average transaction amounts to US$13.03. The top selling items at the Green Grocer are tomatoes, eggs, bananas, watermelon, and ground beef. The Green Grocer is not a full-service grocery store. The following items were frequently requested by customers: toilet paper, bottled water, aluminum foil, and plastic ware. Stocked items at the Green Grocer that did not sell were baby food and breakfast cereal. Between 18% and 32% of the Green Grocer products were supplied by local producers.
When community members who shopped at the Green Grocer monthly or less were asked why they do not shop there more often, 44% (n=21) said the store had limited items, and 36% (n=17) said the store was too expensive. The remaining 20% reported various other reasons.
The community survey also revealed that the emergence of the food desert did not change the frequency of customer visits to the four local restaurants in Alderson (p=0.85). Families frequented local restaurants at the rate of 2.98±0.54 times a month before the food desert and 3.05±0.51 times a month after the food desert. Table 3 shows the distribution of favoritism for restaurant business shared by the local restaurants.
Restaurant managers reported that the emergence of the food desert did not significantly affect their business. The new food desert did not affect restaurant menu prices, customer patronage, food costs from wholesale suppliers, or volume of sales. However, the Smokehouse restaurant reported that the closed Alderson grocery store had previously supplied them with hot dogs and buns, which now had to be purchased from another supplier. The family restaurant, the Smokehouse, and the sandwich shop reported that during the time between the closure of the Alderson grocery store and the opening of the Green Grocer, customers frequently requested non-menu items for use in home meal preparation. The requested items were eggs, milk, tomatoes, onions, peppers, potatoes, and fruit. There were no significant changes in restaurant visits for those who were on the SNAP or WIC program (data not shown).
The Alderson Food Pantry was used by 44% (n=68) of the community members surveyed. Of those that used the food pantry, 43% (n=29) said they rely on the food pantry more now than they did when the Alderson grocery store was in business. Several community members reported getting food items from the food pantry that they would have otherwise purchased from the Alderson grocery store before it closed. Eighteen percent (n=12) of food pantry users said they now rely on the food pantry for fruits, vegetables, and meats. Fifteen percent (n=10) said they now rely on the food pantry for dairy products, while 13% (n=9) say they now rely on the food pantry for canned or bottled food.
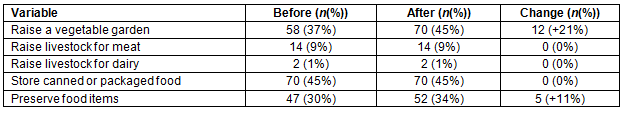
Home food production and storage was also recorded in the community member survey. Table 4 shows how home food production and preservation changed due to the emergence of the food desert. Although 12 families began gardening and 5 families began preserving food after the food desert, the change in proportions for these variables was not statistically significant (p=0.16, p=0.54 respectively). Nonetheless, the practical significance is that 17 families changed their food acquisition and storage practices due to the food desert.
Sales at the community market or the number of vendors at the community market did not change due to the food desert. A new mobile food unit distributed food from community market vendors to 13 families in the Alderson Manor. Cost of fresh produce distribution was US$36 per week for a minimal commitment of 6 weeks. The food distribution for June included strawberries, watermelon, green beans, cantaloupe, and lettuce. July's distribution included strawberries, green beans, kale, cucumbers, potatoes, beets, squash, zucchini and onions. August food included cucumbers, squash, zucchini, tomatoes, apples, peaches, and corn.
Table 1: Frequency of Green Grocer shopping
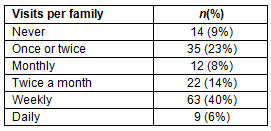
Table 2: Food price comparisons
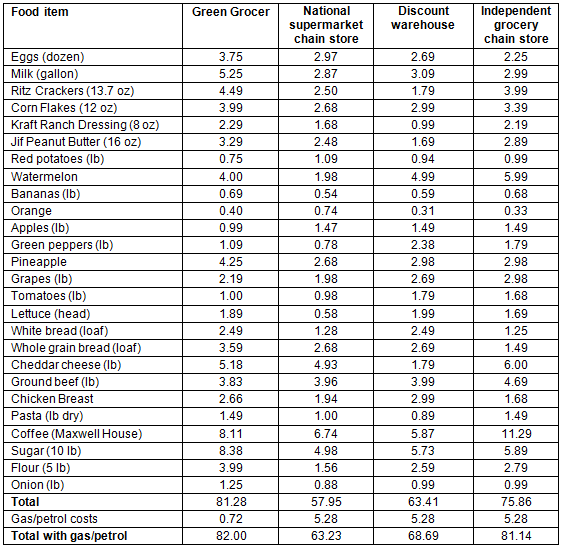
Table 3: Alderson residents' favorite restaurant

Table 4: Home food production and storage before and after the food desert
Discussion
At a time when many food deserts are being eliminated across the US, new food deserts are emerging due to hundreds of grocery store closures10. The irony extends even further in that many people think the solution to the food desert problem is opening grocery stores in the midst of existing food deserts2. When the community of Alderson, West Virginia, was faced with an impending food desert, one of its reactions was to open a new grocery store or cooperative (Green Grocer). Data from this study show that 86% of the Alderson community shop at the Green Grocer, but that 77% do a majority of their grocery shopping at a supermarket more than 16 km (11 miles) from home. The Green Grocer sales receipts confirm this, showing the average purchase amount of only US$13.03, clearly not enough to feed a family. A similar study, conducted in an urban setting, showed that opening a grocery store in a food desert was not a guaranteed success2. Community members in this city did not embrace the new grocery store, and it closed its doors after only 18 months of operation. Other related studies show that placement of a grocery store in an urban food desert does not ensure its success or that dietary behaviors improve with better food access2,3,18-20. Therefore, food access is not the entire answer to the food desert problem.
Many residents in urban and rural areas drive distances further than the nearest grocery store to purchase foods at the best price2,3,18-21. The most common barrier to obtaining food in rural areas is cost18,21. The food price comparison in this study supports this behavior, showing people made significant savings by traveling greater than 17.7 km (11 miles) to purchase common food items. If the Official USDA Food Plans are used to estimate food costs22 and the calculated 30% increase in common food costs between the Green Grocer and the national supermarket chain store for this study were assumed to be consistent storewide, a family of four could save US$44.82 per week or US$179.28 per month by traveling the further distance to buy food at the large supermarket22.
On the other hand, traveling long distances to buy cheaper groceries can have negative effects on health. The prevalence of obesity, cardiovascular disease and mortality rise with increased traveling distance to buy groceries1-5. People with poor access to healthy foods may spend less money by traveling long distances to buy food, but their low-cost food purchases are less healthy than comparable higher cost items8. Furthermore, when cost is the primary force behind distant food purchases, as seen in rural food deserts, people buy less fresh fruits and vegetables at these distant markets than they would otherwise6,7,9. These postulates are somewhat confirmed by the purchases that were made at the local Green Grocer. The four most popular food items bought at the Green Grocer (tomatoes, eggs, bananas, and watermelon) were more expensive than found at the distant supermarket. This means that the Alderson community valued these healthy fresh food items enough to purchase them locally at a higher price, and that unhealthy food items or 'junk food' purchases were not the most popular in the local market.
Another factor affecting healthy dietary behaviors in rural food deserts is marketing. Research shows that low-price supermarkets promote unhealthy food or 'junk food' sales more than healthy food3. In this study, fruits and vegetables dominated the view from the main entrance in 71% of the high-price stores and only 14% of the low-price stores. In contrast, 'junk food' dominated the entrance view in 67% of the low-price stores. The low-price stores averaged eight displays to promote healthy foods, while high-price stores averaged 20 displays of healthy foods3.
The emergence of the Alderson food desert did not affect patronage to fast food restaurants, but it did cause an interesting change. During the interim between the closing of the Alderson full-service grocery store and the opening of the Green Grocer, community members requested that fast food restaurants sell them fresh fruits, vegetables, and dairy products. Furthermore, many of the food pantry patrons also relied more heavily on the food pantry for fruits, vegetables, meat, and dairy products after the emergence of the food desert. All of this data parallel the Green Grocer sales data: the top-selling items at the Green Grocer were fruits, vegetables, dairy, and meat. Thus, the Green Grocer seems to be meeting some of the food desert needs of Alderson community members, but not the bulk of their needs. A less immediate adaptation to the food desert was the 21% increase in home gardening and 11% increase in food preservation practices.
The rural Appalachian US town of Alderson, West Virginia, recently became a food desert. This elevated disease risk, because rural Appalachian food deserts have some of the highest cardiovascular disease and mortality rates in the country4. Community members organized a food hub to negate or minimize the effects of the food desert on food security. The opening of the Green Grocer played a part in offsetting only some of the effects of the food desert, because community members do not use the Green Grocer as a one-stop shop for groceries. The patrons of the Green Grocer seem to use it as a convenience store to purchase fresh fruits, vegetables, and dairy products that families may lack before their next long-distance trip to a supermarket. Alderson's low-income residents now rely more heavily on food pantry assistance, while a small number of others have turned to gardening and food preservation.
It seems like the answer to the food desert problem in rural Appalachia is similar to that reasoned by a conglomerate of research on existing food deserts in urban areas. The first factor governing food acquisition behavior is food pricing, with the proximity of food access coming in second2,3,16,17,19,23. How to overcome these two major barriers in the midst of current economics and marketing in rural America remains to be answered.
Acknowledgements
This study was supported by the Center for Rural and Community Health at the West Virginia School of Osteopathic Medicine and the West Virginia Clinical and Translational Science Institute. Research reported in this publication was supported, in part, by the National Institute of General Medical Sciences of the United States National Institutes of Health under award number U54GM104942. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
References
1. United States Department of Agriculture. Food deserts. (Internet). Available: https://apps.ams.usda.gov/fooddeserts/fooddeserts.aspx (Accessed 15 January 2016).
2. Sadler RC, Gilliland JA, Arku G. A food retail-based intervention on food security and consumption. International Journal of Environmental Research and Public Health 2013; 10: 3325-3346. http://dx.doi.org/10.3390/ijerph10083325
3. Ghosh-Dastidar B, Cohen D, Hunter G, Zenk SN, Huang C, Beckman R, et al. Distance to store, food prices, and obesity in urban food deserts. American Journal of Preventive Medicine 2014; 47(5): 587-595. http://dx.doi.org/10.1016/j.amepre.2014.07.005
4. Harden-Fanning F. Adherence to a Mediterranean diet in a rural Appalachian food desert. Rural and Remote Health (Internet) 2012; 13: 2293. Available: www.rrh.org.au (Accessed 15 March 2015).
5. Tolzman C, Rooney B, Duquette D, Rees K. Perceived barriers to accessing adequate nutrition among food insecure households within a food desert. Wisconsin Medical Journal 2014; 113: 139-143.
6. Ver Ploeg M. Food environment, food store access, consumer behavior, and diet. Choices 2010; 25(3): 1-5.
7. Laraia BA, Siega-Riz AM, Kaufman JS, Jones SJ. Proximity of supermarkets is positively associated with diet quality index for pregnancy. Preventive Medicine 2004; 39: 869-875. http://dx.doi.org/10.1016/j.ypmed.2004.03.018
8. Williamson SH. Seven ways to compute the relative value of a U.S. dollar amount, 1774 to present. (Internet) 2016. Available: https://www.measuringworth.com/uscompare/ (Accessed 15 March 2016).
9. Rose D. Food store access and household fruit and vegetable use among participants in the US Food Stamp Program. Public Health Nutrition 2004; 7(8): 1081-1088. http://dx.doi.org/10.1079/PHN2004648
10. Farfan B. Store Closings Index 2015 of largest US brick-and-mortar retail chains. (Internet) 2016. Available: http://retailindustry.about.com/od/USRetailStoreClosingInfoFAQs/fl/All-2015-Store-Closings-Stores-Closed-by-US-Retail-Industry-Chains_4.htm (Accessed 15 March 2016).
11. World Heart Federation. Cardiovascular disease risk factors. (Internet) 2016. Available: http://www.world-heart-federation.org/cardiovascular-health/cardiovascular-disease-risk-factors/ (Accessed 20 August 2016).
12. Appalachian Regional Commission. The Appalachian region. (Internet). Available: http://www.arc.gov/appalachian_region/TheAppalachianRegion.asp (Accessed 15 March 2016).
13. City-data.com. Alderson, West Virginia (WV) poverty rate data. (Internet). Available: http://www.city-data.com/poverty/poverty-Alderson-West-Virginia.html (Accessed 15 March 2016).
14. United States Census Bureau. Community facts. (Internet). Available: http://factfinder.census.gov/faces/nav/jsf/pages/index.xhtml (Accessed 15 March 2016).
15. United States Census Bureau. Income and poverty in the United States: 2014. (Internet) 2016. Available: http://www.census.gov/library/publications/2015/demo/p60-252.html (Accessed 20 August 2016).
16. United States Department of Agriculture. Designated food desert census tracts. (Internet). Available: https://apps.ams.usda.gov/fooddeserts/TractBreakdown.pdf (Accessed 15 January 2016).
17. Raosoft. Sample size calculator. (Internet) 2004. Available: http://www.raosoft.com/samplesize.html (Accessed 15 March 2016).
18. Yousefian A, Leighton A, Fox K, Hartley S. Understanding the rural food environment - perspectives of low-income parents. Rural and Remote Health (Internet) 2011; 11: 1631. Available: www.rrh.org.au (Accessed 15 March 2016).
19. Chung C, Myers Jr SL. Do the poor pay more for food? An analysis of grocery store availability and food price disparities. Journal of Consumer Affairs 1999; 33(2): 276-296. http://dx.doi.org/10.1111/j.1745-6606.1999.tb00071.x
20. Dubowitz T, Zenk SN, Ghosh-Dastidar B, Cohen DA, Backman R, Hunter G, et al. Healthy food access for urban food desert residents: examination of the food environment, food purchasing and practices, diet and BMI. Public Health Nutrition 2015; 18(12): 2220-2230. http://dx.doi.org/10.1017/S1368980014002742
21. Haynes-Maslow L, Parsons SE, Wheeler SB, Leone LA. A qualitative study of perceived barriers to fruit and vegetable consumption among low-income populations, North Carolina, 2011. Preventing Chronic Disease (Internet) 2013; 10: 120206. Available: http://dx.doi.org/10.5888/pcd10.120206 (Accessed 15 March 2016). http://dx.doi.org/10.5888/pcd10.120206
22. United States Department of Agriculture Center for Nutrition Policy and Promotion. USDA food plans: cost of food. (Internet) 2015. Available: http://www.cnpp.usda.gov/USDAFoodPlansCostofFood/reports (Accessed 15 March 2016).
23. Liese AD, Weis KE, Pluto D, Smith E, Lawson A. Food store types, availability, and cost of foods in a rural environment. Journal of the American Dietetic Association 2007; 107: 1916-1923. http://dx.doi.org/10.1016/j.jada.2007.08.012
