On 6 January 2005, an improperly aligned railway switch led to the collision of two freight trains near the Avondale Mills textile plant in Graniteville, a small, rural, unincorporated town in South Carolina. The collision culminated in the rupture of a tank car and release of an estimated 60 tons of chlorine gas into the sleeping community1-3. Nine people died, and at least 550 residents sought immediate medical attention1-3. Approximately 5400 residents within a 1.5 km radius of the spill were subject to a mandatory evacuation the following day and were not permitted home until 2-3 weeks later. With damages in excess of US$6.9 million4-6, the Graniteville train disaster was one of the worst chlorine gas exposures in US history3,7-9.
At the time of the accident, the social and economic landscape of Graniteville was similar to that of many small rural towns, with limited access to resources and reliance on local manufacturing industry as a primary economic source. The Gregg division plant in Graniteville, one of several Avondale Mills plants, had a 160-year history of employing generations of families in the town of 7000 residents10. In the years leading up to the train disaster, the US textile manufacturing industry, concentrated in the south-east, began to reduce employment - a loss of more 900 000 jobs between 1990 and 200511. The accident and the corrosive effects of chlorine gas were devastating for Avondale Mills12: less than 2 years after the disaster, the company closed, and more than 1600 of the 4000 jobs lost were held by Graniteville area residents13.
The Graniteville chlorine spill was a technological disaster which, unlike natural disasters, are often unpredictable and result from human error or negligence6,7,14. Recent technological disasters include the 2010 Deepwater Horizon oil spill in the Gulf of Mexico15, the failure of the Fukushima Daiichi Nuclear Power Station following the earthquake and tsunami in Japan in 201116, and the April 2013 West Fertilizer Company explosion in West, Texas17.
The impacts of natural and technological disasters are many and can include psychological, physical, and social implications18. For example, a 70-year mining operation that began in 1919 left residents of the Libby, Montana community exposed to asbestos for several decades, resulting in chronic health and social impacts19. In cases where people were exposed to noxious chemicals, long-term post-disaster effects have included frequent reports of physical ailments such as cancer20,21; congenital anomalies22;cardiovascular outcomes20; endocrine immune system dysfunction20,23; and respiratory disorders such as asthma, emphysema, and chronic obstructive pulmonary disease (COPD)20.
The intersection of economic insecurity and toxic exposure impacted the already fragile state of health care in rural Graniteville. According to the Health Resources and Services Administration's Index of Medical Underservice, Graniteville qualified as a medically underserved, health professional shortage area, even prior to the chlorine spill24. Conceivably, the train disaster added additional stressors to a community with limited health resources25-27. As such, healthcare professionals provide a unique and important perspective to help understand the impact of the disaster on the community's health.
Few studies document the long-term effects of technological disasters on communities' health and access to health services, and even fewer do so from the perspectives of those responsible for care, such as healthcare providers. To better understand the long-term health effects of the Graniteville disaster, a thematic analytic approach was employed to explore healthcare providers' perspectives on the long-term effects of the disaster on community health, healthcare access, and wellbeing.
Research context and setting
The data collection team consisted of six research team members who were trained in qualitative interview procedures. A protocol was developed to maintain standardization of interview questions and procedures used. Eligible participants were healthcare providers located in Graniteville and the surrounding areas. This included towns in Aiken County (where Graniteville is located) as well as nearby Georgia (the Georgia state line is less than 20 km from Graniteville). Participants were invited to be interviewed at times and in private locations that were convenient to them (eg in person, by phone, or via Skype).
Recruitment
To be eligible to participate in the study, healthcare providers must have worked in Graniteville, Aiken County, or nearby Georgia during the time of the 2005 Graniteville train disaster, and have patients from the Graniteville area who were impacted by the disaster. This purposive sample was recruited in a number of ways:
- Community residents who participated in another phase of the project28 were asked to provide referrals.
- A community advisory board was organized, and members assisted with participant recruitment through their personal and social networks and knowledge of the community and local providers.
- Two community members were enlisted who had grown up and lived in the Graniteville area and were members of the research team assisted with direction to potential participants and visited local healthcare provider offices to invite them to participate in the study.
- Local healthcare provider networks (eg physician directories and professional associations) were accessed.
- Referrals from healthcare providers who agreed to participate were requested.
After potential participants were identified, invitation letters were mailed (via email or US postal service) and in-person contacts were made. Follow-ups were made with phone calls to describe the study and solicit participation. People who identified themselves as potential participants were screened using the aforementioned eligibility criteria. Those who met the criteria were then scheduled to conduct an interview at a time and in a location that was convenient to them.
Instrument
The research team developed an interview guide with questions and accompanying probes related to how the providers perceived that the disaster impacted the community's health, healthcare access, and wellbeing. The interview guide was pretested on a sample of four healthcare providers who were not included in the study, and no concerns were noted. The guide included questions such as, 'How has the disaster impacted the community's health' with probes such as 'How has the disaster positively impacted the community's health', 'How has the disaster negatively impacted the community's health' and 'Have there been any segments of the population more impacted than others'? Additionally, participants completed an interviewer-administered demographic survey developed by the research team prior to each interview. Items included age, gender, race, employment status, job title, and perceived level of chlorine exposure as a result of the disaster.
Procedure
Before any data were collected, participants underwent an informed consent process. Participants who conducted the interview in person were provided an informed consent document to review while the interviewer reviewed the document aloud. Participants were invited to ask any questions about the study and were asked to provide verbal consent to participate before the interview could commence. For participants who conducted interviews by phone, the consent process was documented by audio recording and saved to a file separate from their interview. Phone participants were emailed a copy of the consent document at least 24 hours before their scheduled interview. The interviewer reviewed the document aloud as with face-to-face interviews. No participants selected the Skype interview option.
Interviews were approximately 30 minutes in length and were conducted between October 2012 and March 2013. Six interviewers were trained to conduct the interviews using the interview guide. Participants chose to be interviewed either in person (in our study office or the participant's office) or via phone. It was essential that each interview setting was private so as not to disrupt the interview process. Interviewers conducted interviews using the interview guide and recorded field notes as appropriate. Interviews were audio recorded and transcribed verbatim by an independent professional transcription firm. Upon completion, each participant received a $50 cash incentive.
Data analysis
An essentialist, inductive thematic analytic approach was utilized in the data analysis29. The transcribed interviews were managed using NVivo v10 (QSR International; http://www.qsrinternational.com). The analysis team included five members; four were academic researchers and program staff whose work focus on community health and health disparities, and one who was a community investigator whose participation was beneficial in providing insight from the community perspective as well as building community capacity for qualitative data analysis. One team member was the primary coder, two team members were secondary coders, and two team members oversaw the analysis process and helped ensure the process was translated accurately from the methodological process into report and manuscript development.
Following the phases of thematic analysis29, the analysis team members began the process of reading and re-reading the transcribed data to become familiar with details and patterns. Using knowledge of the data and the interview questions as a guide, initial codes were generated to inform the development of the codebook and coding scheme30. The codebook was finalized after analysis team members identified no new codes, thus establishing the master codebook used to code the remainder of the interview transcripts. Using the master codebook, each interview transcript was coded by at least two research team members. Coding discrepancies were resolved by consensus. As the iterative process of analysis continued, codes were combined into overarching themes and evaluated by the first three authors to ensure that they were adequately supported by the data.
Ethics approval
All study procedures were reviewed and approved by the principal investigator's Institutional Review Board (University of South Carolina Institutional Review Board registration number 00000204).
Sample characteristics
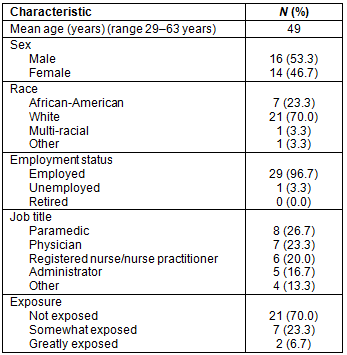
Thirty healthcare providers (n=16 females; n=14 males) participated in the study. Ages ranged from 29 to 63 years with a mean age of 49 years. The majority of participants were white (70%; n=21), and were primarily employed as paramedics (27.0%; n=8), physicians (23.3%; n=7), and registered nurses/nurse practitioners (20.0%; n=6). In terms of perceived level of chlorine exposure, 30% (n=9) of providers reported that they had been exposed (Table 1).
Table 1: Socio-demographic characteristics of study participants (N=30)
Qualitative themes
Four themes emerged regarding the disaster's long-term impact on community health: effects of chlorine exposure on physical health, issues with healthcare access, residual effects of the disaster on personal and community wellbeing, and improving health and community wellbeing.
Effects of chlorine exposure on physical health: Healthcare providers identified numerous and expected immediate post-disaster effects including respiratory complications and dermatologic ailments linked to the direct inhalation of and exposure to chlorine gas. However, they also identified lingering and at times devastating physical symptoms for both the exposed community members and healthcare providers themselves.
Patients The chlorine gas exposure occurred within the context of a community that already had health vulnerabilities. Many community members had ongoing lung issues related to working in the textile mill, which were exacerbated by inhaling the chlorine gas:
Most of the people who grew up and worked in those mills from the time they could work until they were old have lung problems. And now they have lung problems of a different nature. You know, most of these people couldn't breathe in the first place and now they really can't. So, you know, you go from a brown lung situation to a scarred lung situation.
The healthcare providers observed that, for some of their patients, the chlorine exposure resulted in long-term physical disability. As one provider noted:
... they are still feeling very devastating effects of it, simply because they can't work, they can't have what I feel is a full and complete life, simply because they physically cannot do what they used to be able to do.
These providers were very familiar with the patients in their community who had recurrent issues related to their exposure, and were resigned to the inevitability that their patients' health would never improve:
There's a zone of calls that you run that you know their age and everything else and you know that they were here when it happened and you know what their complaints are, and it's a couple times a month, you know. Weather will change and they'll exacerbate and get bad and it's gonna be that way until their last day. It's just a fact. You see it on a daily basis and you feel for them but they're going on so we go on.
Healthcare providers Some healthcare providers were also directly exposed to the chlorine gas, either as they entered the scene, or from the victims' clothing as they underwent decontamination. Descriptions of personal exposure were more evident among paramedics than other healthcare providers as they were more likely to report being first responders in close proximity to ground zero. For one paramedic who briefly inhaled the toxic gas when he left a decontamination area to go back to rescue another victim, exposure had long-term effects:
That short period of time that I was breathing all the chlorine gas off of my protective gear, has in some subsequent years, created - I already had some minimal respiratory problems, but this is really exaggerated them to the point where I cannot be around Clorox right now. I can't even spray bathroom cleaner without having difficulties breathing. I have since developed asthma. I've since developed a worse case of COPD.
Even if not directly impacted, every provider knew a colleague who had been exposed and suffered long-term physical complications.
Issues with healthcare access: Healthcare providers offered disparate responses concerning the disaster's impacts on access to healthcare services. Initially, some healthcare providers stated that the disaster did not affect access to healthcare services. However, when probed for further details, providers also identified changing access over time, and community barriers and negative perceptions of available health care that hindered access.
Initial increased access Several providers highlighted the increase in the number of people accessing healthcare services post-disaster. One healthcare provider stated:
You know, initially it had a huge impact on access ... I actually remember like the first two or three weeks we didn't close right at closing time like we traditionally did ... There was still a waiting room full of patients. So we accommodated those patients by seeing them the day that they came in, but of course we also opened up our access ... seeing more walk-ins.
Some healthcare providers noted that access to healthcare services improved as a result of research activities following the accident:
... overall it seems like all the different programs that have become available in the area with USC [University of South Carolina] doing what they're doing, with the free clinics coming about, with Margaret Weston [local community health center] expanding and having more access, I think that more people have better access to care now.
Negative impact on access Healthcare providers highlighted several negative impacts on access to services including closing of local businesses, loss of employment, and subsequent loss of health insurance coverage. Specifically, the accident had a significant, adverse impact on the town's economy due to the subsequent closing of the textile mill that had been a major employer for town residents. One healthcare provider stated: 'The mill closes, people [are] unemployed now. They don't have the money; they don't have healthcare. And you know there's Medicare/Medicaid, it still is a lot of people who don't qualify, and still don't have insurance.' Additionally, the loss of income had a direct impact on patients' ability to access transportation:
Transportation is a really big problem for a lot of people around here. They don't own a car or they have to try and get a relative and there's the price of gas. Some of the places for them to get into a doctor's ... it could be an hour ride.
Local clinics accommodated the increase in patients in the immediate aftermath of the disaster, but the providers interviewed were unaware of any long-term financial assistance. Coupled with the dramatic increase in demand, and the absence of ongoing aid, one provider described how their clinic became overwhelmed:
They lost their jobs and didn't have money, and so they came here. And what that did to us is put a strain on us, because we get a fixed amount of money every year to see all populations. And when you're accustomed to seeing - I believe we did 6000 in 2009, and now we're serving 10,000 with the same amount of federal dollars in terms of our grant.
Community suspicions Several providers noted perceptions of community residents that the health care available in the community prior to the disaster was, in some ways, inferior to what they could access in other areas. One provider stated: 'They think that they're not getting the best healthcare services.' It was common practice for community residents to go to surrounding larger cities to access services, and this distrust of the quality of services carried over to the care provided in the aftermath of the disaster. Even the motives behind opening the new clinics were seen by some residents as suspicious:
I don't think there's really been any what I would consider a true medical clinic open up that wasn't trying to get data, that was strictly here, 'We're just concerned about you, making sure you're healthy' kind of deal and stuff. It was more - most of the stuff I've seen is, in some way, they can get some help, services but they're more or less just a data collection to try and research what this has done.
Some providers highlighted the scarcity of mental health resources when they wanted to refer their patients, a problem that existed before the disaster and was exacerbated afterward due to the marked increase in mental health disorders. Compounding this problem, the providers observed that many patients were suspicious of health care services for mental health issues, and often did not want the referral anyway:
I think the majority of them were given the opportunity for counseling. But then you got a lot of people that say, 'I don't need it. I can take care of my own'.
Residual effects of the disaster on personal and community wellbeing: The intersections of chronic illnesses, financial insecurity, and an uncertain future impacted the community's perceptions of their town; one provider stated: '[they say] "My town is no longer my town. My town died when the train hit." And you can feel when you drive through there.' The poor and elderly were disproportionately affected by the disaster as they were more likely to live closer to ground zero. They lost more, and had less ability to recover:
That house that their grandfather lived in and their father lived in and they live in, you know, now all the wiring is rotted out and all the iron plumbing is rotted out because of the corrosiveness of the chlorine and it's almost inhabitable and, here again, some of them have to live in it, you know, still.
And even less ability to leave:
I think for them and the ones who owns property in those areas, I think that they - a lot of people start to feel trapped; they can't - they wanna get out, but they cannot afford to get out. They're stuck. And a lot of them wanted to give up, I think, because of being in close proximity to the tracks and knowing that maybe - I mean, it's not impossible for that to happen again. But I think a lot of people in that area know that they can't afford to go anyway anywhere.
'Being stuck' was related to an increase in mental illnesses including depression, post-traumatic stress disorder, fear, and anxiety in the long-term aftermath of the disaster. The providers linked these issues to the traumatic nature of the disaster, the death of community members, loss of beloved pets, and the negative environmental and physical health effects. As stated by one provider, 'Well, in a small percent of the population, they still have some depression or depression issues related to seeing others die in the incident.'
Even if some were not directly affected, the ongoing responsibility of caring for sick family and community members could be difficult:
And again, some haven't lost their lives, and the impact that has on who's left and who's left to care for the one that's now disabled who may be having some problems social[ly] as well as health problems of their own; still residual-type issues from that.
Improving health and community well-being: Even with the overwhelming adversity experienced by this community, healthcare providers also identified long-term positive impacts to the community's health related to a heightened awareness of health needs. One healthcare provider stated:
Well, I think positively one of the things that it did was that it made people more aware of their health. You know, when they started having side effects, maybe headaches, they were more likely to come into the doctor because they may have thought it was from the chlorine exposure and it could have actually been an underlying issue like blood pressure issues or their thirstiness may have been attributed actually to them being a diabetic.
According to another healthcare provider:
There were a lot of people that were impacted that were uninsured and underinsured. A lot of those people came here, did receive healthcare services, and are still receiving healthcare services today. In a way, it could have ... caught some preexisting health conditions that they already had, or that they didn't know that they had, like diabetes, hypertension, things like that.
The first responders noted that the disaster had caused the emergency response community to 'come together and support each other':
So in a positive way, we learned to work better with each other. We have now better communications. We know how to handle some of these things. Our equipment and funding that we received following the Graniteville disaster increased.
And finally, the healthcare providers noted how the disaster was part of the community's history, and something that they had begun to overcome:
The local fire department built kind of a shrine right there near the accident site, to honor those nine people that died that morning, and the others that were injured. So there were definitely some things made as far as not only safety, but as far as community improvement to try to - to not try to hide the fact that that accident happened there, but to recognize it, and to honor it, in as much as they did have people that died.
Discussion
The purpose of this study was to determine the long-term impact of the Graniteville train disaster on the community's health, healthcare access, and wellbeing from the perspective of local healthcare providers. Regarding the disaster's impact on the community's health, healthcare providers identified noted physical and mental health consequences. These results are comparable to other studies of technological disaster impacts on community health. For example, researchers found chronic cases of stress31 and identified long-term negative physical health impacts such as chronic high blood pressure and impaired immune system functioning among individuals in the aftermath of the Three Mile Island nuclear plant disaster32. They also identified increased negative mental health impacts such as anxiety, depression and somatic distress among individuals at least 6 years post-disaster33. Other researchers are increasingly relaying the presence of long-term psychological disorders, typically after natural disasters23,33-35. It is evident and reflective of extant literature that physical and mental health effects abound in this community post-disaster. These results suggest a need to focus on interventions to mitigate the negative physical and mental health impacts immediately post-disaster, in addition to ensuring that resources are readily and consistently available in the long term.
Regarding the impact of the disaster on the community's healthcare access, healthcare providers noted an increased opportunity to receive medical attention immediately following the train disaster. However, while there was increased access immediately after the disaster with the increase in acute medical issues, the secondary surge, or the increased need for long-term healthcare services following a disaster, drained an already medically resource-poor community36. A number of healthcare providers referred to the sole healthcare facility in Graniteville and stated that that the majority of community residents had to seek health care in neighboring counties, a major inconvenience for many residents. The present study's findings are comparable to other researchers who have noted that the secondary surge can lead to a sudden increase in the need for long-term healthcare services as well as add additional financial and resource burden, particularly in rural, underserved communities25-27. As such, addressing the long-term impacts of technological disasters should be a critical component of disaster response planning and a public health priority.
An interesting finding is that healthcare providers did not solely identify negative health consequences from the disaster. They also noted a positive impact on community wellbeing in the form of heightened health awareness, namely how community members were more aware of their health post-disaster compared to the time pre-disaster. While this may have been a factor that healthcare providers viewed as a positive effect of the disasters, this is a notable contrast to literature highlighting the grave, adverse impact of disasters, particularly on vulnerable communities23,28,31-35. This perspective is a unique contribution and perhaps indicative of the landscape of the rural community and the scarcity of health resources pre-disaster.
While the results of this study have limited generalizability, as findings are specific to the study population in Graniteville, South Carolina, the authors are confident that these findings are an important contribution to the body of knowledge about the long-term health impact of disasters on underserved, rural communities. These study findings could be useful in identifying areas of intervention post-disaster to address community health and access to healthcare services in communities with similar socio-demographic characteristics.
Despite this limitation, the present study has several strengths. First, the involvement of the community advisory board and community investigators was integral to the success of our project. Board members helped plan and approve each step of the study protocol and community investigators conducted interviews and provided contextual information that made for a meaningful and collaborative process. Furthermore, the semi-structured interviews provided in-depth data about healthcare providers' perspectives following a technological disaster. The healthcare providers represented a diverse cadre of nurses, paramedics, doctors, and other health professionals who provided their points of view regarding the health and healthcare challenges present in a community in the long-term aftermath of a disaster. Their ongoing access to place and persons directly affected by the events offered a unique perspective in understanding the long-term effects of toxic exposure in an already vulnerable rural community, and to identify examples of community resilience and opportunities for optimal recovery.
More than a decade later, the repercussions of the Graniteville disaster continue to impact the health and wellbeing of the local residents. The findings from this study help illustrate that disaster recovery should not be considered solely an acute event - potentially chronic physical health, mental health, healthcare access, and wellbeing consequences need to be addressed, particularly in underserved, rural communities. The study findings are relevant for researchers, practitioners, policy makers, and others who are concerned with improving the service delivery and availability of resources post-disaster. The perspectives provided by the healthcare providers in this community should be considered as future disaster response strategies are developed, and can be used as a model for other communities locally and globally.
References
1. Wenck MA, Van Sickle D, Drociuk D, et al. Rapid assessment of exposure to chlorine released from a train derailment and resulting health impact. Public Health Reports 2007; 1: 784-792.
2. Van Sickle D, Wenck MA, Belflower A, et al. Acute health effects after exposure to chlorine gas released after a train derailment. The American Journal of Emergency Medicine 2009; 27(1): 1-7. http://dx.doi.org/10.1016/j.ajem.2007.12.006
3. Dunning A, Oswalt J. Train wreck and chlorine spill in Graniteville, South Carolina: transportation effects and lessons in small-town capacity for no-notice evacuation. Transportation Research Record 2007; 26 December. http://dx.doi.org/10.3141/2009-17
4. Anon. 2005 Labor profile for Graniteville, SC. (Internet) 2005. Available: http://www.statelibrary.sc.gov/scedocs/Em735M/000888.pdf (Accessed 8 December 2015).
5. USA City Facts. Graniteville, SC income and economy. (Internet) 2015. Available: http://www.usacityfacts.com/sc/aiken/graniteville/economy/ (Accessed 8 December 2015).
6. Noji EK. The nature of disaster: general characteristics and public health effects. In EK Noji (Ed). The public health consequences of disasters. Oxford University Press, 1997; 3-20.
7. Sulkowski ML, Lazarus PJ. Five essential elements of crisis intervention for communities and schools when responding to technological disasters. International Journal of School & Educational Psychology 2013; 1(1): 3-12. http://dx.doi.org/10.1080/21683603.2013.780192
8. Abara W, Wilson S, Vena J, et al. Engaging a chemical disaster community: lessons from Graniteville. International Journal of Environmental Research and Public Health 2014; 11(6): 5684-5697. http://dx.doi.org/10.3390/ijerph110605684
9. National Transportation Safety Board. Collision of Norfolk Southern freight train 192 with standing Norfolk Southern local train P22 with subsequent hazardous materials release. (Internet) 2005. Available: http://www.ntsb.gov/investigations/AccidentReports/Reports/RAR0504.pdf (Accessed 8 October 2015).
10. WRDW-TV, Augusta, GA. 'Highly likely' that Avondale Mills will close its entire operation. (Internet) 2006. Available: http://www.wrdw.com/home/headlines/2845626.html (Accessed 8 January 2016).
11. United States Department of Agriculture Economic Research Service. U.S. textile and apparel industries and rural America. (Internet). Available: http://www.ers.usda.gov/topics/crops/cotton-wool/background/us-textile-and-apparel-industries-and-rural-america.aspx (Accessed 28 December 2015).
12. The Augusta Chronicle. Avondale Mills' electronic records destroyed in wreck (Internet) 2005. Available: http://chronicle.augusta.com/stories/2005/01/12/met_439678.shtml#.VoH9ohUrLjY (Accessed 28 December 2015).
13. Fretwell S. Graniteville: five years later, a town trying to heal. (Internet) 2010. Available: http://www.thestate.com/news/local/article14371367.html (Accessed 28 December 2015).
14. Chua AY. A tale of two hurricanes: comparing Katrina and Rita through a knowledge management perspective. Journal of the American Society for Information Science and Technology 2007; 58(10): 1518-1528. http://dx.doi.org/10.1002/asi.20640
15. Kujawinski EB, Kido Soule MC, Valentine DL, Boysen AK, Longnecker K, Redmond MC. Fate of dispersants associated with the Deepwater Horizon oil spill. Environmental Science & Technology 2011; 45(4): 1298-1306. http://dx.doi.org/10.1021/es103838p
16. Ohnishi T. The disaster at Japan's Fukushima-Daiichi Nuclear Power Plant after the March 11, 2011 earthquake and tsunami, and the resulting spread of radioisotope contamination. Radiation Research 2011; 177(1): 1-4. http://dx.doi.org/10.1667/RR2830.1
17. Johnson J. Deadly fertilizer explosion. Chemical and Engineering News. (Internet) 2013; 91(16): 8. Available: http://cen.acs.org/articles/91/i16/Deadly-Fertilizer-Explosion.html (Accessed 28 December 2015).
18. Goldsteen R, Schorr JK. The long?term impact of a man?made disaster: an examination of a small town in the aftermath of the Three Mile Island Nuclear Reactor Accident. Disasters 1982; 6(1): 50-59. http://dx.doi.org/10.1111/j.1467-7717.1982.tb00744.x
19. Cline RJ, Orom H, Berry-Bobovski L, Hernandez T, Black CB, Schwartz AG, Ruckdeschel JC. Community?level social support responses in a slow?motion technological disaster: the case of Libby, Montana. American Journal of Community Psychology 2010; 46(1-2): 1-8. http://dx.doi.org/10.1007/s10464-010-9329-6
20. Bertazzi PA, Consonni D, Bachetti S, et al. Health effects of dioxin exposure: a 20-year mortality study. American Journal of Epidemiology 2001; 153(11): 1031-1044. http://dx.doi.org/10.1093/aje/153.11.1031
21. Hatch M, Ron E, Bouville A, Zablotska L, Howe G. The Chernobyl disaster: cancer following the accident at the Chernobyl nuclear power plant. Epidemiologic Reviews 2005; 27(1): 56-66. http://dx.doi.org/10.1093/epirev/mxi012
22. Hoffmann W. Fallout from the Chernobyl nuclear disaster and congenital malformations in Europe. Archives of Environmental Health 2001; 56(6): 478-484. http://dx.doi.org/10.1080/00039890109602895
23. Mishra P, Samarth R, Pathak N, Jain S, Banerjee S, Maudar K. Bhopal gas tragedy: review of clinical and experimental findings after 25 years. International Journal of Occupational Medicine and Environmental Health 2009; 22(3): 193-202. http://dx.doi.org/10.2478/v10001-009-0028-1
24. US Department of Health and Human Services. Health professional shortage areas: designation criteria and guidelines. (Internet). Available: http://bhpr.hrsa.gov/shortage/hpsas/designationcriteria/index.html (Accessed 28 December 2015).
25. Davis JR, Wilson S, Brock-Martin A, Glover S, Svendsen ER. The impact of disasters on populations with health and health care disparities. Disaster Medicine and Public Health Preparedness 2010; 4(1): 30-38. http://dx.doi.org/10.1017/S1935789300002391
26. Hsu CE, Mas FS, Jacobson HE, Harris AM, Hunt VI, Nkhoma ET. Public health preparedness of health providers: meeting the needs of diverse, rural communities. Journal of the National Medical Association 2006; 98(11): 1784.
27. US Department of Health and Human Services, Office of Rural Health Policy. Rural communities and emergency preparedness. (Internet) 2002. Available: ftp://ftp.hrsa.gov/ruralhealth/ruralpreparedness.pdf (Accessed 28 December 2015).
28. Annang L, Wilson S, Tinago C, et al. Photovoice assessing the long-term impact of a disaster on a community's quality of life. Qualitative Health Research 2016; 26(2): 241-251. http://dx.doi.org/10.1177/1049732315576495
29. Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology 2006; 3(2): 77-101. http://dx.doi.org/10.1191/1478088706qp063oa
30. Saldaña J. The coding manual for qualitative researchers. 2nd ed. London: Sage, 2013.
31. Davidson LM, Baum A. Chronic stress and posttraumatic stress disorders. Journal of Consulting and Clinical Psychology 1986; 54(3): 303. http://dx.doi.org/10.1037/0022-006X.54.3.303
32. Baum A. Implications of psychological research on stress and technological accidents. American Psychologist 1993; 48(6): 665. http://dx.doi.org/10.1037/0003-066X.48.6.665
33. Yule W, Bolton D, Udwin O, Boyle S, O'Ryan D, Nurrish J. The long?term psychological effects of a disaster experienced in adolescence: I: The incidence and course of PTSD. Journal of Child Psychology and Psychiatry 2000; 41(4): 503-511. http://dx.doi.org/10.1111/1469-7610.00635
34. Davidson JR, McFarlane AC. The extent and impact of mental health problems after disaster. Journal of Clinical Psychiatry 2006; 67(suppl 2): 9-14.
35. Abramson D, Stehling-Ariza T, Garfield R, Redlener I. Prevalence and predictors of mental health distress post-Katrina: findings from the Gulf Coast Child and Family Health Study. Disaster Medicine and Public Health Preparedness 2008; 2(2): 77-86. http://dx.doi.org/10.1097/DMP.0b013e318173a8e7
36. Runkle JR, Zhang H, Karmaus W, Brock-Martin A, Svendsen ER. Long-term impact of environmental public health disaster on health system performance: experiences from the Graniteville, South Carolina chlorine spill. Southern Medical Journal 2013; 106(1): 74. http://dx.doi.org/10.1097/SMJ.0b013e31827c54fc









