Introduction
Alzheimer's disease (AD) has become an increasingly prevalent and dreaded affliction as the population ages. Since the 1980s the number of people diagnosed with the disease has more than doubled, with approximately 4.5 million cases reported in the US1. The impact is such that one in ten Americans has a family member with the disease and one out of every three people in the USA knows someone with Alzheimer's2. The growth in cases accompanies the aging population (50% risk over age 85) across the nation, with some of the highest projected increases falling in the Western region of the USA. Currently, Colorado has approximately 62 000 residents with the disease (Alzheimer's Association, pers. comm., 2004); this state is expected to see a 124% increase by the year 2025, making it the third highest projected increase in the nation3.
Alzheimer's and other dementias are particularly problematic in rural communities. As younger family members move to larger population centers, the remaining rural population is increasingly older. Census data collected in Colorado in 2000 indicate that statewide 13% of the population is over 60 and 9.7% over 65, but in some rural counties 20% or more of the population is over 65, and that proportion is growing faster than in urban areas4. Research has shown that rural elderly are not only likely to be older, but also to have a lower income and be less educated than those in more urban environments5,6. Non-farm rural elderly have lower incomes compared with farming elderly, poorer housing, fewer family members to provide assistance, and poorer reported health7. These hardships can be extremely taxing when an elderly individual has AD. Because children of rural elderly often leave home and settle in more urban areas, the responsibility for taking care of the rural elder falls to the spouse or a single child living in the area. Help for the caregiver in the form of respite services such as adult day care and in-home health care is not readily available in rural areas because the population density (1.0 to 2.0 per square mile in some Colorado counties) makes it unlikely that an economically viable respite service would be feasible.
As AD progresses, certain behavioral, affective, and cognitive losses make caring for an elder with AD more difficult than caring for loved ones with other chronic conditions and disabilities8. Although self-management of chronic illnesses is a growing trend9, dementing illnesses are not amenable to management by the afflicted individual, but quality of life can be enhanced by supporting the family caregiver. The US Congress Office of Technology Assessment10 found that 7 out of 10 people with AD live at home, where family and friends provide approximately 75% of their care. The experience of being a caregiver can cover as long as 20 or 30 years, but the length, amount, and intensity of care can vary depending on family circumstances.
While caregiving can be a fulfilling and rewarding experience, often it comes with associated stressors for the caregiver. In general, many AD caregivers experience increased depression and anxiety symptoms in addition to perceiving their health to be somewhat poorer than non-caregivers or community samples11. These increases in psychosocial stressors may also contribute to physical deterioration, as a recent meta-analysis showed that caregiving stressors are also associated with higher levels of stress hormones and lower levels of antibody responses compared to non-caregivers12. Interventions have resulted in findings that successful coping can minimize the burden of caregiving and make the experience more positive13,14. Factors that play a role in influencing how well the caregiver handles the experience, include social support from others, perceived control, supportive relief services such as respite care and adult day care, and education and training for caregiving tasks and strategies15-17.
One intervention designed to increase caregiver skills and confidence, create reliable and accessible networks of support for caregivers, and increase access to supportive services is the Savvy Caregiver Program (SCP). The SCP was modeled on the Minnesota Family Workshop (MFW) and was designed to offer organizations a means of implementing a successful and academic-based caregiver psycho-educational program. The training consists of approximately 12 hours of sessions that involve accomplishing various objectives for the caregivers (eg acknowledge the disease, developing emotional tolerance, taking control) in addition to providing them with a caregiver manual and educational CD-ROM18. The manual contains educational material for the caregivers to review at their own pace. The 6 sections include: (i) introduction to dementing disorder; (ii) caregiver self-care; (iii) the anchors of enjoyable involvement; (iv) levels of thinking and performance; (v) strengthening the family as a resource for caregiving; and (vi) review and integration of the previous sections.
The training sessions help caregivers develop a clearer picture of their new role, give them an understanding of the disease, help them deal with difficult behavior, and teach them how to take control. Tests of the program's effectiveness found favorable results showing that caregivers report substantial increases in skill, knowledge, and confidence after completing the training18. The SCP should have advantages for rural caregivers since those trained in the program can subsequently use the manual and CD-ROM to build skills and obtain advice regardless of the presence of other community resources.
In 2002 a collaborative effort with affiliates from the Alzheimer's Association Colorado Chapter, Colorado State University, the Area Agencies on Aging of Colorado, and the state Aging and Adult Services (the unit operating Older Americans Act programs) was initiated using the SCP in order to increase training and services to caregivers of the elderly, with special emphasis on those living in remote rural areas. The project was funded as part of the AD Demonstration Grants to States (ADDGS) program of the Administration on Aging. Here we report the initial impact of the program on caregivers in rural areas of the state.
Method
Participants
The participants in this study consisted of caregivers of persons with Alzheimer's living in rural areas (ie, fewer than 2500 people; n = 27), or small cities or towns (ie, fewer than 50 000 people; n = 27) in Colorado. Their participation in the Savvy Caregiver workshop was voluntary and free of charge. The mean age of the caregivers was 62 years, with 8 male and 22 female participants (gender was not reported for every participant). The mean age of the person with dementia was 78, with 21 males and 33 females. Of the caregivers, 17 were a spouse/domestic partner, 26 a child/child-in-law, three a sibling, three a friend/neighbor, and one other relative. A sample (n = 42) that resided in larger urban communities served as a comparison group (ie, 50 000 to 100 000 people; n = 22; more than 100 000; n = 20). Demographic characteristics (ie, age of person with dementia, degree of impairment, gender of participant, and relationship with person with dementia) of the rural and urban samples were compared and no statistically significant differences were found between the two groups.
Materials
Client intake form (OMB#: 0985-0013): This standard ADDGS form contains questions regarding demographic information of the caregiver and the client in addition to various scales assessing the patient and the caregiver's current status, including the Epidemiological Studies Depression Scale19. This is a 20 item self-report scale with coefficient alpha of .85 to .92, high correlations with other measures of depression, and proven applicability to elderly populations20,21. The questionnaire also inquires about amount of time the caregiver provides care, the employment status of the caregiver, and a self-report measure of their overall health.
Caregiver's manual and CD-ROM: The SCP manual, as described previously, provided a written version of the skill-building information conveyed in the training. Included on the CD along with educational information for the caregivers was a cognitive performance estimation procedure, and video clips of experts providing suggested interventions for behavioral problems at multiple stages of dementia.
SCP questionnaire: This questionnaire was given to our main participant sample during 6 month follow-up phone interviews. Questions pertaining to the effectiveness of the SCP training and the use of the materials were asked (eg. 'Since completing SCP I have used the manual for reference', 'Using the manual helped me to structure meaningful household activities for the person with dementia'), with a 5 point response format.
Procedure
Participants were recruited through the seven area offices of the Alzheimer's Association. To accommodate the needs of each community, the training program was adapted to either 1 day, 2 day, or 3 day formats. (The small sample size for the various community sizes makes meaningful comparison of the impact of the alternative 1, 2, or 3 day training formats impractical. However, in a study of this question with a larger sample, Scharf22 found no differences in the outcomes for length of training format.). Once participants contacted their local Alzheimer's Association, the staff understood their unique situation and the desire to receive assistance was great enough that traveling to training sites was not seen as a huge obstacle by participants. Training was provided in 25 communities, with 2 to 18 family members per community. Participants signed informed consents, and then completed the Client Intake Form (consistent with Human Research Committee approval) at the beginning of the training and again approximately 6 months later in a telephone interview. Participants were also offered a voucher-type respite grant for up to $1000 per family through the Alzheimer's Association as reimbursement for use of community-based respite services.
Results
The frequencies for the 6 month follow-up responses to the SCP Questionnaire are presented (Figs 1-4). The responses by the rural participants show that 88% of the participants used the SCP manual with some frequency since completing the training, 69% found the manual helpful in structuring meaningful household activities for the person with AD, 38% used the CD-ROM since completion of the training, and 35% used the CD-ROM to help them determine their loved one's level of functioning. The urban participants showed similar frequencies.
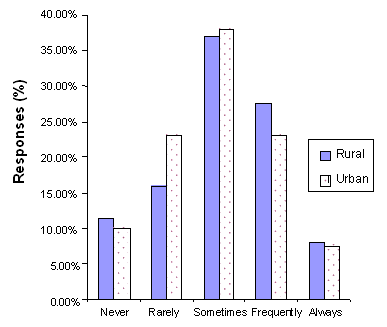
Figure 1: Use of SCP manual at 6-month follow-up (rural n = 51, urban n = 40).
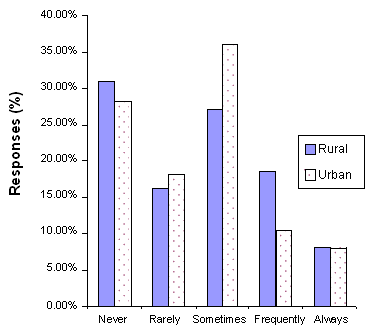
Figure 2: The manual helped to structure meaningful household activities for the AD patient (6 month follow up). (Rural n = 49, urban n = 39).
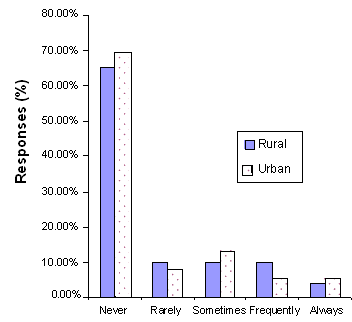
Figure 3: Use of the CD-ROM given at the SCP at the 6 month follow up (rural n = 48, urban n = 40).
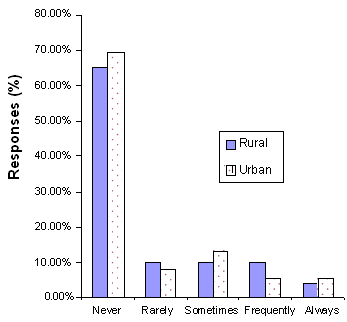
Figure 4: Using the CD at home helped in determining the AD patient's level of functioning (6-month follow-up). (Urban n = 48, Rural n = 39).
The depression scores and total support services used (both from the Client Intake Form) for baseline and 6 month follow up were analyzed using an analysis of variance (ANOVA) with repeated measures, with rural versus urban as a between-groups factor (ie, comparing the means of rural vs urban groups). The two groups did not differ in depression scores at baseline (p > .05), nor was there a group main effect or interaction (ie, the differences between the two groups did not change from baseline to follow up). However, the change in depression score from baseline to follow up was statistically significant, F(1,68) = 6.00, p< .05. For ease of understanding, this change was examined for both groups in the form of simple effects analyses. Specifically, the rural group's depression scores (pre- M = 2.42, post- M = 2.12) declined significantly, F(1,40) = 5.69, p< .05, but the urban group's depression scores (pre- M = 2.25, post- M = 2.10), did not, F(1,28) = 1.40, p > .05. As shown in Figure 5, as would be expected, some caregivers' depression scores improved while others' worsened.
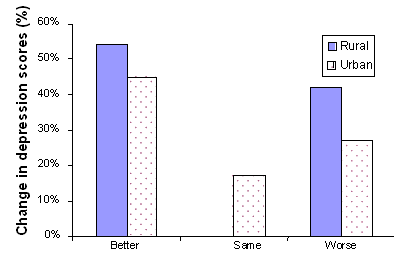
Figure 5: Change in caregiver's depression scores from baseline to 6-month follow up (Rural n = 41, urban n = 29).
For total support services used, the rural and urban groups did not differ at baseline (p > .05). There were also no significant main effects or interactions.
Due to the dichotomous nature of the support group use data a c2 McNemar test was run, finding a significant difference between the rural (17% usage) and urban (47% usage) groups at baseline (Fig 6), c2 (1, N = 89) = 9.48, p = .002. There was also an overall increase from baseline to follow up, c2 (1, N = 76) = 7.04, p < .05. However, due to smaller sample size, tests of change for the rural and urban groups separately showed no significant increase: rural support group use pre- M = 17%, post- M = 45%, c2 (1, N= 42) = 2.22, p = .13; urban support group use pre- M = 47%, post- M = 61%, c2 (1, N = 34) = 3.11, p = .08).
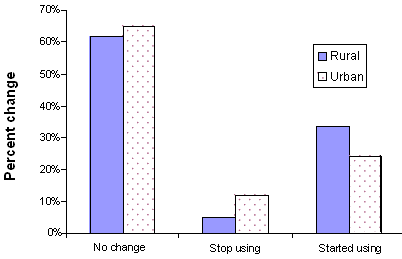
Figure 6: Changes in support group use between baseline and 6 month follow up (Rural n = 42, urban n = 34).
Discussion
The SCP encompasses many of the suggestions made by others for rural dementia caregiver training. For example, Zarit and Leitsch23 include designing an intervention that encompasses reasonable goals for the participants, initially engaging in dialogue, and specifically informing the caregivers about activities for the person with dementia, and Buettner and Langrish24 found that rural caregivers were especially interested in learning new coping strategies.
The results of the current study found overall support for the effectiveness of the SCP. The rural and urban participants not only used the training manual approximately 6 months after the training, but were able to apply the content of the manual by structuring meaningful household activities for the person with dementia. These findings have significant implications as research has found that therapeutic activities can sustain or improve function in people with dementia, in addition to reducing problem behaviors25. Lack of education about the disease has been shown to lead caregivers to attribute negative behaviors as being in the control of the person with dementia, resulting in possible confusion and frustration26. Also, many of the SCP participants were able to utilize the educational CD-ROM in order to determine their loved one's level of functioning, although use of this relatively new technology was substantially lower than use of the printed manual. Giving rural caregivers access to this type of information has desired benefits in terms of caregiver effectiveness and wellbeing.
The results for the depression measure in the current study found that the rural group had a significant improvement in their depression scores, whereas the urban group did not. Unlike previous research that has shown a worsening of depression scores across time for AD caregivers27, this study shows that over a 6 month time period, depression scores significantly improved. Here the training that was received by the rural participants may have played a role in helping to improve their depression levels. In addition to education, information about support services and making possible contacts at the training could have also aided in this overall improvement of depression.
In addition to education, social support has been found to decrease caregiver burden and depressive symptoms14. The rural caregivers in this study were more likely to start than stop attending a support group. A floor effect could explain this finding, since the rural group had only 17% support group use at baseline. Services such as support groups for caregivers of persons with dementia have been found to have numerous positive outcomes. Researchers have found that many caregivers report positive statements regarding support group usage and that simply being around others was an invaluable experience28. A study conducted by Millan-Calenti et al.29 found that AD caregivers who participated in a help program with a social component had improved wellbeing, improved health status, and reported taking comfort in knowing that they had 'back up'. Increasing the support group use for the rural participants can be particularly beneficial because many rural communities are small and may lack other services that caregivers can use to establish supportive relationships.
Limitations of this study include small sample size and constraints in the format of the Client Intake Form questions required by the ADDGS program. In addition, future caregiver interventions should include ample questions relating to issues regarding caregiver efficacy and skills related to caregiving. This particular study had a loss to follow up of approximately 30%, mostly due to death of the person with dementia or to the clients moving without leaving new contact information. The small sample size required dichotomizing community sizes into those smaller or larger than 50 000 population, which may disguise the different circumstances between caring for someone in a community of 2500 and a community of 49 999, and the associated services available in these different size communities. Future analyses with this growing dataset will be able to look at multiple waves of data to address these and other issues. For exploratory purposes, we did compare the 27 participants from communities of fewer than 2500 people ('very small') with the 27 participants from communities of 2500 to 50 000 population ('small town'). Baseline to follow-up declines in mean depression scores were present for both groups (Ms = 2.3 to 2.25 and 2.46 to 2.04), but significant for only the small town (p = .43 vs p = .02). Support group use increased for both groups (4% to 40% and 31% to 50%), but significantly only for the very small group (p = .002 vs p = .62).
This current study gives initial data on the effectiveness of the SCP in rural communities. As this is an ongoing study, more rural and urban participants will take part in the SCP and their data will be available to further assess the progress of the intervention. Additional follow-up interviews are planned with the current sample. The evidence to date does suggest that targeting rural communities for caregiver training can have very desirable outcomes.
References
1. Hebert LE, Scherr PA, Binenias JL, Bennett, D.A. Evans DA. Alzheimer disease in the US population: Prevalence estimates using the 2000 Census. Archives of Neurology 2003; 60: 1119-1122.
2. Alzheimer's Association. Growth of Alzheimer's disease through 2025. Chicago, IL: Alzheimer's Association, 2004; 1-2.
3. Hebert LE, Scherr PA, Bienias JL, Bennett DA, Evans DA . State-specific projections through 2025 of Alzheimer disease prevalence. Neurology 2004; 11: 1645.
4. US Census Bureau. Colorado QuickFacts. (Online) 2000. Available: http://quickfacts.census.gov/qfd/states/08000.html (Accessed 5 September 2005)
5. Clifford WB, Lilly SC. Rural elderly: Their demographic characteristics. In: CN Bull (Ed.). Aging in rural America Newbury Park: Sage, 1993; 3-16.
6. Hobbs FB, Damon BL. 65+ in the United States. Current population reports. Washington, DC: US Department of Commerce, US Department of Health and Human Services, 1996; 23-190.
7. Coward RT, McLaughlin DK, Duncan RP, Bull CN. An overview of health and aging in rural America. In: RT Coward, CN Bull, G Kukulka, JM Galliher (Eds). Health services for rural elders. New York: Springer, 1994; 1-32.
8. Light E, Niederehe G, Letowitz B (Eds). Stress effects on family caregivers of Alzheimer's patients. New York, NY: Springer, 1994
9. Bolin J, Gamm L, Kash B, Peck M. Chronic disease management in rural and underserved populations: Innovation and system improvement help lead to success. Managed Care Interface 2005; 18: 37-41.
10. Office of Technology Assessment, US Congress. Losing a million minds: Confronting the tragedy of Alzheimer's disease and other dementias. Washington, DC: US Government Printing Office, 1987.
11. Schulz R, Newsom J, Mittelmark M, Burton L, Hirsch C, Jackson S . Health effects of caregiving: the caregiver health effects study, an ancillary study of the cardiovascular health study. Annals of Behavioral Medicine 1997; 19: 110-116.
12. Vitaliano PP, Zhang J, Scanlan JM. Is caregiving hazardous to one's physical health? A meta-analysis. Psychological Bulletin 2003; 129: 946-972.
13. Barber CC, Pasley K. Family care of Alzheimer's patients: The role of gender and generational relationship on caregiver outcomes. Journal of Applied Gerontology 1995; 14: 172-192.
14. Clyburn LD, Stones MJ, HadjistaV, Ropoulos T, Tuokko H. Predicting caregiver burden and depression in Alzheimer's disease. Journal of Gerontology 2000; (Suppl): S2-S13.
15. Karlin NJ, Bell PA. Self-efficacy, affect, and seeking support between caregivers of dementia and non-dementia patients. Journal of Women and Aging 1992; 4: 59-77.
16. Mittelman MS, Ferris SH, Shulman E, Steinberg G, Levin B. A family intervention to delay nursing home placement of patients with Alzheimer disease: A randomized controlled trial. JAMA 1996; 276: 1725-1731.
17. Schulz R, O'Brien AT, Bookwala J, Fleissner K. Psychiatric and physical morbidity effects of dementia caregiving: Prevalence, correlates, and causes. The Gerontologist 1995; 35: 771-791.
18. Hepburn KW, Lewis M, Sherman CW, Tornatore J. The savvy caregiver program: Developing and testing a transportable dementia family caregiver training program. The Gerontologist 2003; 43: 908-915.
19. Radloff LS. The CES-D scale: A self-report depression scale for research in the general population. Applied Psychological Measurement 1977; 1: 385-401.
20. Hertzog C, Van Alstine J, Usala PD, Hultsch DF, Dixon R . Measurement properties of the Center for Epidemiological Studies Depression Scale (CES-D) in older populations. Psychological Assessment 1990; 2: 64-72.
21. Radloff LS, Teri L . Use of the Center for Epidemiological Studies-Depression scale with older adults. Clinical Gerontologist 1986; 5: 119-136.
22. Scharf L. Evaluation of formats of one, two, or three sessions for Alzheimer's Savvy Caregiver training. Senior Honor's Thesis, 2004, Colorado State University, CO.
23. Zarit SH, Leitsch SA. Developing and evaluating community based intervention programs for Alzheimer's patients and their caregivers. Aging & Mental Health 2001; 5: S84-S98.
24. Buettner LL, Langrish S. Rural vs urban caregivers of older adults with probable Alzheimer's disease: perceptions regarding daily living and recreation needs. Activities, Adaptation & Aging 1999; 24: 51-65.
25. Buettner L, Ferrario J. Therapeutic recreation-nursing team: A therapeutic intervention for nursing home residents with dementia. Annual in Therapeutic Recreation. 1998; 7: 21-28.
26. Paton J, Johnston K, Katona C, Livingston G . What causes problems in Alzheimer's disease: Attributions by caregivers. A qualitative study. International Journal of Geriatric Psychiatry 2004; 19: 527-532.
27. Hooker K, Monahan DJ, Frazier LD, Bowman SR, Shifren K. Personality counts for a lot: Predictors of mental and physical health of spouse caregivers in two disease groups. Journal of Gerontology: Psychological Sciences 1998; 53B: 73-85.
28. Karlin NJ, Bell PA, Noah JL. Long-term consequences of Alzheimer's caregiver role: a qualitative analysis. American Journal of Alzheimer's Disease and Other Dementias 2001; 16: 177-182.
29. Millan-Calenti JC, Gandoy-Grego M, Antelo-Martelo M, Lopez-Martinez M, Riveiro-Lopez MP, Mayan-Santos JM. Helping the family carers of Alzheimer's patients: from theory...to practice. A preliminary study. Archives of Gerontology and Geriatrics 2000; 30: 131-138.

