full article:
Context
Although there is a long history of research into the health of rural Canadians, as well as a long history of international research symposia and meetings on rural health issues1, the rural health research community remains small and dispersed across the country. Within the last decade, sparked largely by the new research funding opportunities created by the establishment of the Canadian Institutes of Health Research (CIHR), there has been a concerted effort to develop more substantial connections among rural health researchers from many different disciplines and parts of Canada. The Canadian Rural Health Research Society (CRHRS), created by researchers as a means to establish a robust and well-funded rural health research community, has developed as a network of researchers in the four principal areas of rural health research: (i) biomedical; (ii) clinical; (iii) health services and policy; (iv) population and public health.
The development of this rural health research networked community has not been without its challenges. The purpose of this article is to discuss the development of the CRHRS as well as the challenges and lessons learned about creating networks and building capacity among rural and remote health researchers.
Issue: research networks and networking
Health research networks have been described as, 'networks of investigators who are equipped with tools to facilitate collaboration and information sharing'2 and whole systems that 'facilitate cultural change and grass-roots participation in research' that also enable 'individual innovation, through multidisciplinary participation'3. Approaches to research networks differ, from highly coordinated endeavours to loosely coupled connections of researchers and others who maintain 'various types of contacts, co-operation and communication'4. Networks fulfil various purposes, including overcoming fragmentation of research on a particular topic5, improving multidisciplinary approaches to pressing research problems6, linking researchers and decisionmakers7, and increasing researcher competitiveness nationally and internationally6-10.
Research networks are important in building research capacity as well as influencing the development of multidisciplinary teams to address complex research questions6,8. It is not always clear what structures and processes can best enhance and sustain researcher capacity11. Key elements in successful networks include: a common, clear vision with a modest number of goals12; proven, charismatic leadership of an individual or individuals with a deep understanding of all aspects of research in the field6; a structure that suits the network's goals and purpose6,10,12; clear, effective processes of communication, coupled with mechanisms to foster and sustain researcher engagement and collaboration11,12; sufficient resources12 provided in a judicious and timely manner8; and ways of working that reflect the intent and context of the network9,11. Networks develop largely in response to contextual forces.
Rural health research
The pattern of rural health research development occurs in relation to the role of rural health in the country's health agenda, the availability of national research funding, the organization of health services, and the availability of universities and researchers to rural communities. In the USA, for instance, rural health research is largely health policy driven and focuses on access issues13. As Hartley notes, this is due primarily to three factors. First was the establishment of the Federal Office of Rural Health Policy in 1987 that provided funding and capacity-building support for research centres focused on rural issues. Second was the National Rural Health Alliance, which began in 1978 as a merger of two rural hospital and rural primary care organizations, serves as an umbrella organization, and advocates successfully for research dollars. Third was the creation of issue networks, made up of federal/state decisionmakers, clinicians and researchers, to lobby for specific issues such as rural hospital policy.
In Australia, a number of rural health units were established within state health departments in the late 1980s to focus on policy related issues. The increase in regional universities, the funding of university departments of rural health in each state and the Northern Territory, as well as the establishment of the rural clinical schools has resulted in an increase in rural health research. Most research is focused on public health and health services, however, and remains small in scale14. At the same time, funding for research that is specifically rural in nature remains limited15,16, and there are continuing needs for capacity development and communication among researchers dispersed over a vast geographic area16.
In Canada, the development of rural health research has been more researcher driven than policy driven, and hence is uneven across the country. Provinces are responsible for the provision of health and education, and interest in rural health varies from province to province. Although there is an increasing number and range of rural health research projects and programs across the country17, there are few long-term provincially-funded centres with a central mandate for rural health research, such as Ontario's Centre for Rural and Northern Health Research (CRaNHR).
Developing a Canadian Rural Health Research Network
By the late 1990s an increasing appreciation that specific knowledge was required to address rural and remote health needs in Canada18 led to the emergence of a network that has become the CRHRS. Developmental milestones, including policy and organizational influences, are outlined (Fig 1).
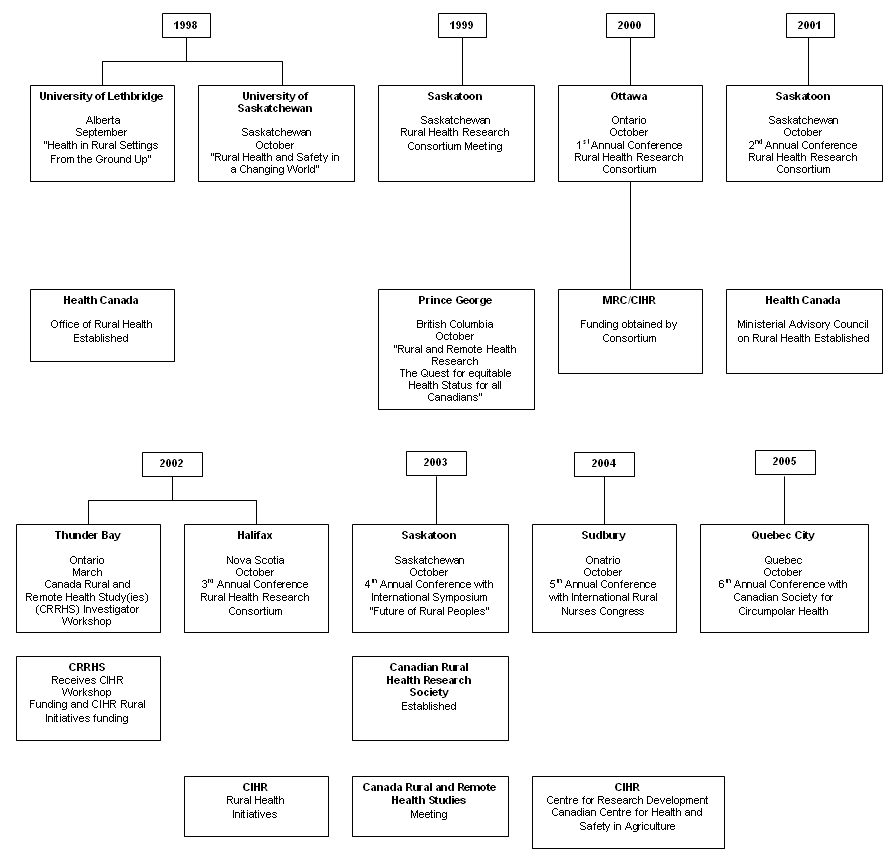
Figure 1: Milestones in Canadian Rural Health Research Society networking.
Two rural health research conferences in 1998, one at the University of Lethbridge19; the other at the University of Saskatchewan20, provided opportunities for researchers from a broad range of disciplines and research interests to meet for the first time. Also in 1998, the national department of health, Health Canada, formed the Office of Rural Health for the purpose of putting a 'rural lens' on national health issues18. Rural health research was the focus of two proposals during the consultation phase of the development of the Canadian Institutes of Health Research (CIHR)21,22.
In 1999, two national meetings served to accelerate connectedness. The University of Saskatchewan hosted a meeting of 129 researchers from a wide variety of disciplines from across Canada to explore whether specific interdisciplinary cross-university research groupings might be formed to seek funding for new research projects from the emerging CIHR and other funding venues. The outcome was the Canadian Rural Health Research Consortium (Consortium) and the emergence of research groups in nursing, the physical environment, and rural children's health. A month later, Health Canada's Office of Rural Health and the University of Northern British Columbia hosted the National Rural Health Research Summit at which researchers, rural residents and government representatives further defined the area and recommended means of supporting rural and remote health research18.
With the support of a Medical Research Council/CIHR Opportunities grant, the Consortium met in April 2000 to establish its mission, goals and 5 year targets. The Consortium held its first national scientific conference in October 2000 with 75 scientific abstracts and presentations. Workshops at this meeting resulted in the identification of nine key research areas, and requests for closer scientific connections and project development, and advocacy for increased funding for rural and remote health research.
The Canadian Rural Health Research Society: a network of networks
Rather than a single network, rural and remote health researchers have developed what can be considered a virtual network of networks, which is enabling research capacity development. The Consortium has become the Canadian Rural Health Research Society (CRHRS), annual national scientific meetings have continued, an inventory of research training in rural health research has been created23, new research groupings have emerged, and network members have worked with CIHR and other funding agencies to hold workshops and institutes, as well as to extend funding opportunities.
The Society
Between 2001 and 2003 the Consortium evolved into the CRHRS. As a national not-for-profit incorporated society, the CRHRS aims to build interdisciplinary, multidisciplinary, mutually supportive and community-focused research networks that are responsive to the needs of people living in rural and remote communities. The Society's activities are focused on researcher capacity-building, networking, increasing the availability of funding for rural health research, as well as knowledge translation24.
Connections among researchers have been fostered through annual scientific meetings. The number of abstracts and range of disciplines has increased each year. Joint conferences have identified new areas of research and expanded networks: in 2003, with the International Symposium on the Future of Rural Peoples; in 2004 with the International Rural Nurses Congress; in 2005 with the Canadian Society for Circumpolar Health (CSCH); and in 2006 with the Canadian Centre for Health and Safety in Agriculture, the National Collaborating Centre on Aboriginal Health, The National Collaborating Centre on Environmental Health, and the British Columbia Rural and Remote Health Research Network, among others. The conferences have served as the venue for research priority-setting and networking on topics such as rural women's health, definitions of rural and rurality25 working with large databases, rural health professional education, research ethics and aboriginal knowledge translation.
Research groupings
From the Consortium's earliest meetings, structured opportunities have been provided for researchers with similar interests, from various universities and disciplines to get together to explore the questions: what are the major research issues in this area? What research questions could be worked on?
One of the earliest networking results was in health services and policy research, with the nursing group's study, 'The Nature of Nursing Practice in Rural and Remote Canada'26. This Canada-wide study, was conceived when the principal researchers first met at the 1999 Saskatoon meeting, and were later supported by a Medical Research Council/CIHR Opportunities grant in 200027. The physical environment group, which also met at the 1999 meeting, was successful in its 2002 application to CIHR Strategic Training Initiative in Health Research (STIHR) Program for a multicentre training grant, Public Health and the Agricultural Rural Ecosystem Training Program (PHARE)28. In 2004, two CIHR Centres for Research Development were funded: the Centre on the Changing Physical and Social Landscape in Atlantic Rural Canada29, and the Canadian Centre for Health and Safety in Agriculture30, with its researcher network now numbering 66 scientists in 14 Canadian universities and other national and international organizations. Most research within these centres is in the areas of population and public health, and health services and policy research, although increasingly projects cross into biomedical research and genomics, on topics such as mechanisms of lung inflammation related to swine barn air31.
In March 2002, with the support of 8 CIHR Institutes, 37 researchers met in Thunder Bay, Ontario. Five additional research groupings, in addition to the ones on rural nursing, environmental health and rural children's health, were created. Subsequent proposals included a project on the links between health status and community resiliency32, and an evaluation of national information sources for developing a baseline data set on the health of rural Canadians29. Other research groupings, including one on children's mental health and a clinical research-focused group on chronic disease management have been unable to garner a sufficient critical mass of researchers to proceed.
A grant received by the Society's co-leaders33, which enabled the provision of small grants ($4000 - $5000), has added substantial value. The grants allowed investigators of varying levels of research maturity, and often with little infrastructure available to them in their home universities, to meet and prepare proposals for funding. Small grants, and the networking they have funded, have enabled researchers to achieve a critical mass across universities, to be successful in national competition, and to compete on standards of international excellence34,35.
Research training
Fostering research training has been a continuing theme. During 2001 a Canada-wide survey of training opportunities in rural and remote health research was undertaken23. The relationships built among researchers through the CRHRS and the research grant activities, have created new research training opportunities, for example, the PHARE Program through the rural health CIHR Centres for Research Development located in Nova Scotia29 and Saskatchewan30. Summer institutes have been implemented in Ontario and Newfoundland. No fewer than 22 students presented their research at the 2005 conference and, with their mentors, participated in a mentorship workshop.
Making supportive networks possible
CIHR funding has been central to fostering research groupings, networking and capacity building among rural and remote researchers27,33. The need for a Canada-wide scan of research priorities, first raised by CRHRS researchers, was taken up by the CIHR. In September 2001 a national meeting organized by CIHR resulted in a proposed strategy for rural and remote health in Canada within the context of the CIHR36,37, and led to CIHR strategic competitions in 2002, 2003 and 2004. In 2002, the CIHR created a strategic initiative across all 13 institutes, now the Special Joint Initiative in Rural and Northern Health, to provide support for the development of this strategic priority38. Funding for this initiative was discontinued in 2006.
Challenges of network development and sustainability
The challenges faced by the CRHRS are characteristic of a small research community with multiple disciplines, diverse interests, and limited capacity, dispersed over a large geographical area. Predominant among the challenges are the following:
- Sustaining communication among a small research community with a range of disciplines and research foci, spread over a vast geography.
- Addressing a range of networking and capacity-enhancing needs within the research community.
- Engendering cooperation in a research environment that rewards competition.
- Resourcing a secretariat or service centre, and other network supports.
- Balancing the demands to foster research excellence with the needs to build infrastructure and engage in advocacy action to increase research funding for rural health.
The rural health research community in Canada remains small and widely dispersed, with few senior researchers. The networking and capacity enhancing needs vary considerably within the research community, and as excellence can be defined in terms of competitive success, cooperation is sometimes stifled.
Attempts to identify gaps and set priorities in rural health research have met with limited success36,37. The list of important topics for research has been far-ranging, and researchers have been unable to reach consensus on focused research priorities because of diverse needs, interests, and disciplines. The broad range of research topics contrasts with the approach in the USA or Australia, where health services or health policy as drivers and funders of rural health research have prompted more focused research priorities13,14. In Canada, it is frequently challenging to create a critical mass of researchers around a particular topic, or to offer research training, except by finding non-traditional ways to link with others across the country or internationally. A Canadian strength however, is a multidimensional approach to understanding the determinants of rural health taken by groups of researchers examining complex issues related to the health and economic sustainability of rural communities30. The breadth of interests and disciplines among the rural health research community has been central to fostering larger multidisciplinary research groups.
Most rural and remote health researchers are located in small universities where research resources are limited. Small universities, often located in more rural or remote parts of Canada, frequently have sustained, substantive linkages with their surrounding communities. These links foster community based research, alignment of research interests, and the ability for research findings to directly impact health programs and services18,38,39. It is these abilities that provide groups of rural health researchers, often networking across provinces, with the potential to compete successfully nationally and internationally, particularly in the new funding era which increasingly emphasizes the need to work with the users of research for improved research uptake.
The targeted national support for rural health and rural health research has been short-lived: Health Canada's Office of Rural Health has been dismantled and CIHR has ceased strategic funding for rural health research. The decrease in targeted funding has made networking and capacity-building more challenging. Among the challenges is finding appropriate publication outlets. CRHRS members have edited special issues of other publications40, but efforts to create a rural health research journal in Canada have not yet been successful.
Finally, it is challenging for a small research community with few resources to develop the necessary infrastructure, while maintaining a balance between advancing the science and advocating for adequate research funding. Network members have been diligent in recommending colleagues to serve on CIHR peer review committees, and institute advisory boards, as well as regularly communicating with CIHR about rural health research needs. The CRHRS, a non-profit society funded by memberships, has sustained its leadership, and maintained its secretariat and conference planning endeavours by means of in-kind contributions by members and their universities. Without a national focus on rural health on the part of those responsible for research funding and policy development, and a more central place of rural health on provincial agendas across the country, the sustenance and growth of research excellence and funding opportunities cannot happen easily.
Lessons learned in network development
In addressing the challenges, the CRHRS has learned how to begin to support researchers with diverse interests and needs across sectors and a wide geographical area, specifically by:
- Focusing on research development through creating and supporting trusting connections among researchers.
- Building the science first, followed by infrastructure development.
- Making individual researchers the nodes in the network.
- Being inclusive by accommodating a wide variety of researchers and researcher strengths.
- Emphasizing social exchange, knowledge exchange, and mentoring in annual scientific meetings.
- Taking opportunities to develop separate projects while finding ways to link them.
- Finding a balance between advancing the science and advocating for adequate funding and appropriate peer review.
- Developing a network organizational structure that is both stable and flexible.
- Maintaining sustained visionary leadership.
Unlike research networks, designed as infrastructures for information and services8, the CRHRS has developed as a fluid channel so that researchers may find best ways of achieving their own goals of excellence in rural and remote health research. In pursuing excellence, researchers have created a variety of smaller, often overlapping knowledge networks, communities of practice and soft networks7. Building a network of networks has been an intertwined process of researchers reaching out, taking the risk to trust one another, building community-linked projects and programs of excellence, receiving funding, developing new knowledge, using the knowledge to train students, building capacity, learning how to translate our knowledge to each other and to our stakeholders and partners, and reaching out in new ways.
Conclusions
The CRHRS has made strides in enabling inclusive networks of researchers and communities to develop capacity collectively. Challenges that remain are to find new ways to link together population health, health promotion, and health services researchers with clinical and biomedical researchers to address the human and health ecosystem issues that are of such importance in rural and remote communities. New developments may see large, multidisciplinary research teams working in partnerships with communities to address the diverse health agenda of rural and remote Canada, while being connected and competitive nationally and internationally. The network of networks approach that has characterized the development of rural and remote health research in Canada may permit some innovative ways to move to this next stage.
Acknowledgements
The authors would like to acknowledge the Canadian Institutes of Health Research for funding the process leading to the formation of the Canadian Rural Health Research Society. The authors also wish to thank the efforts of colleagues from across Canada who participated in and supported the process that led to the formation and incorporation of the Society.
References
1. Dosman JA. The Fifth International Symposium ' Future of rural peoples: rural economy, healthy people, environment, rural communities'. Journal of Agricultural Safety and Health 2005; 11: 123-126.
2. National Institutes of Health. The NIH Roadmap: re-engineering the clinical research enterprise. (Online) 2003. Available: http://nihroadmap.nih.gov (Accessed 28 December 2006).
3. Thomas P, While A. Increasing research capacity and changing the culture of primary care through reflective inquiring practice: the experience of the West London Research Network (WeLReN). Journal of Interprofessional Care 2001; 15: 133-139.
4. Soderbaum F. Networking and capacity building: the role of regional research networks in Africa. The European Journal of Development Research 2001; 13: 144-163.
5. FP6 Instruments Task Force European Commission. Provisions for implementing networks of excellence. (Online) 2003. Available: http://ec.europa.eu/research/fp6/index_en.cfm?p=0_instruments (Accessed 28 December 2006).
6. Michael Smith Foundation for Health Research. Why research networking? A MSFHR backgrounder. (Online) 2004. Available: http://www.msfhr.org/docs/MSFHR_Networking_Backgrounder.pdf (Accessed 28 December 2006).
7. Canadian Health Services Research Foundation. Network notes I: what's all this talk about networks? (Online) 2005. Available: www.chsrf.ca (Accessed 28 December 2006).
8. Birdsell JM, Matthias SJ et al. Networks and their role in enhancing research impact in Alberta (working paper). Edmonton, AB: Alberta Heritage Foundation for Medical Research, 2003.
9. Bernard AK. IDRC networks: an ethnographic perspective. Evaluation Unit, International Development Research Centre. (Online) 1998. Available: www.idrc.ca/en/ev-26858-201-1-DO_TOPIC.html (Accessed 28 December 2006).
10. Holbrook JA, Wolfe DA. The Innovation Systems Research Network: a Canadian experiment in knowledge management. Science and Public Policy 2005; 32: 109-118.
11. Swepson P, Dick B, Zuber-Skerrit O, Passfield R, Carroll A-M, Wadsworth Y. A history of the Action Learning, Action Research, and Process Management Association (ALARPM): From Brisbane (Australia) to the world through inclusion and networks. Systemic Practice and Action Research 2003; 16: 237-281.
12. Hill C. Network literature review: conceptualizing and evaluating networks. Calgary: Southern Alberta Child and Youth Health Network, 2002. Available: http://www.sacyhn.ca/media/pdf/LiteratureReview.pdf (Accessed 28 December 2006).
13. Hartley D. Rural health research: building capacity and influencing policy in the United States and Canada. Canadian Journal of Nursing Research 2005; 37: 7-13.
14. Strasser R. Rural health research: have we turned the corner? Australian Journal of Rural Health 2000; 8: 249-253.
15. Patterson C. The emergence of rural health research in Australia. Australian Journal of Rural Health 2000; 8: 280-285.
16. Best J. Report on the National Health & Medical Research Council Rural Health Research Capacity Building Workshop. Alice Springs, NT: NHMRC, 2005.
17. Pong RW. Rural health research in Canada: at the crossroads. Australian Journal of Rural Health 2000; 8: 261-265
18. Watanabe M, Casebeer A. Rural, remote and northern health research: the quest for equitable health status for all Canadians. A report of The Rural Health Research Summit, October 23-25, 1999. (Online) no date. Available: http://www.unbc.ca/ruralhealth/national_research_summit.html (Accessed 28 December 2006).
19. Ramp W, Kulig J, Townshend I, McGowan V (Eds). Health in rural settings: contexts for action. Lethbridge: University of Lethbridge, 1999.
20. Dosman JA. Rural health and safety in a changing world. In: Proceedings, Fourth International Symposium, Centre for Agricultural Medicine. 18-22 October 1998; University of Saskatchewan, Canada, 1998.
21. Pong R, Atkinson AM, Irvine A, MacLeod M, Minore B, Pegoraro A et al. An institute for rural health research. A CIHR position paper prepared for the Canadian Health Services Research Foundation and the Social Sciences and Humanities Research Foundation. (Online) 1999. Available: http://www.chsrf.ca/final_research/commissioned_research/programs/hidg_e.php (Accessed 28 December 2006).
22. Kealey G, Bornstein S, Buehler S, Doyle M, Kealey L, LeFort S et al. An agency for integration and innovation in the CIHR, prepared for the Canadian Health Services Research Foundation and the Social Sciences and Humanities Research Foundation. (Online) 1999. Available: http://www.chsrf.ca/final_research/commissioned_research/programs/hidg_e.php (Accessed 28 December 2006).
23. Kulig JC, Minore B, Stewart NJ. Capacity building in rural health research: a Canadian perspective. Rural and Remote Health 4: 274. (Online) 2004. Available: http://rrh.org.au (Accessed 28 December 2006).
24. Rural Health Research News. Canadian Rural Health Research Society Newsletter. (Online) no date. Available: http://crhrs-scrsr.usask.ca (Accessed 28 December 2006).
25. Anon. Defining 'rural' and 'rurality' for health and health services research. Pre-conference workshop; October, 2002; Halifax, NS, Brandon University. (Online) no date. Available: www.brandonu.ca/rdi/publications.asp (Accessed 28 December 2006).
26. MacLeod MLP, Kulig JC, Stewart NJ, Pitblado JR, Knock M. The nature of nursing practice in rural and remote Canada. Canadian Nurse 2004; 100: 27-31.
27. Dosman JA. Consortium for Rural Health Research 2000 CIHR Opportunity Program. (Online) 2000. Available: http://www.cihr-irsc.gc.ca/e/pdf_15168.htm (accessed 28 December 2006).
28. Institute of Agricultural Rural and Environmental Health. Public Health and the Agricultural Rural Ecosystem (PHARE). (Online) no date. Available: http://iareh.usask.ca/trainingprograms.php (Accessed 28 December 2006).
29. Guernsey J. Research towards understanding rural health in Atlantic Canadian landscapes. (Online) 2005. Available: http://www.theruralcentre.com/ (Accessed 28 December 2006).
30. Dosman JA. Canadian Centre for Health and Safety in Agriculture. A CIHR Centre for Research Development. (Online) 2006. Available: http://www.cihr-irsc.gc.ca/e/30949.html (Accessed 28 December 2006).
31. Canadian Rural Health Research Society. Proceedings of the Seventh Annual Conference of the Canadian Rural Health Research Society; 19-21 October 2006; Prince George, BC. (Online) no date. Available: http://crhrs-scrsr.usask.ca (Accessed 28 December 2006).
32. Kulig J, Edge D, Guernsey J. Health status and community resiliency: what are the links. CIHR Rural Health Projects. (Online) 2003. Available: http://www.cihr-irsc.gc.ca/e/1872.html (Accessed 28 December 2006).
33. Dosman JA, MacLeod ML. The Canada Rural and Remote Health Study: progress towards project building and area identification. CIHR Strategic Initiative in Rural Health Diagnostic and Integrative Projects, 2001. (Online) 2001. Available: http://www.cihr-irsc.gc.ca/e/pdf_14435.htm (Accessed 28 December 2006).
34. Annis RC, Jeffery BL, Racher FE. Community collaboration to improve health care access of northern residents, 2004 Rural and Northern Health Research: Operating Grants. (Online) 2004. Available: http://www.cihr-irsc.gc.ca/e/24539.html (Accessed 28 December 2006).
35. MacLeod ML, Browne AJ, Moules NJ, Doane GL, Greenwood ML, Cerny LA et al. The working relationships of public health nurses and high priority families in northern communities. 2004 Rural and Northern Health Research: Operating Grants. (Online) 2004. Available: http://www.cihr-irsc.gc.ca/e/24539.html (Accessed 28 December 2006).
36. Lyons RF, Gardner P. Building a strong foundation for rural and remote health research in Canada: St. John's Rural Health Research Forum Summary Notes. Canadian Institutes of Health Research, November 2001. (Online) 2001. Available: http://www.cihr-irsc.gc.ca/e/13239.html (Accessed 28 December 2006).
37. Lyons RF, Gardner P. Strategic initiative in rural and northern health research: Canadian Institutes of Health Research, November 2001. (Online) 2001. Available: http://www.cihr.ca/e/documents/strategic_initiative_e.pdf (Accessed 28 December 2006).
38. CIHR. Canadian Institutes of Health Special Joint Initiative in Rural and Northern Health Research. (Online) no date. Available: http://www.cihr-irsc.gc.ca/e/13239.html (Accessed 28 December 2006).
39. MacLeod M, Ulrich C. Rural and northern practice and its development research program. Health Services and Policy Research Network Investigative Team Grant. Michael Smith Foundation for Health Research, 2005. (Online) 2006. Available: http://www.msfhr.org (Accessed 28 December 2006).
40. Kulig JC. Rural health research: are we beyond the crossroads? Canadian Journal of Nursing Research 2005; 37: 3-6.



