Introduction
Aboriginal people in Canada have a significantly higher incidence of preventable health problems, including diabetes, heart disease, dental caries, injuries, premature labor and tuberculosis, compared with Canada's non-Aboriginal population1. The need to rectify these differences has been acknowledged by individuals, groups and all levels of government. Aboriginal communities want to ensure that their children are healthy, and are actively seeking ways to achieve that goal. Research is recognized to be an important element, perhaps the most important one, in improving the health status of Aboriginal communities1,2. However, to have impact, this research requires community-based studies, with whole communities agreeing to take responsibility for, and action in response to, the data obtained, so that health issues can become targets for community-driven interventions that most likely to be viable and sustainable3.
Well-intentioned researchers and clinicians who attempt to address identified needs must ensure their approaches are relevant and meaningful to the communities, while simultaneously appropriate and successful scientifically3-7. Without the necessary attention to establishing a collaborative relationship, projects are vulnerable to failure.
Type 2 diabetes (T2D) and its precursors impaired glucose tolerance (IGT) and metabolic syndrome are reaching epidemic proportions among Aboriginal Canadians8,9. Of particular concern is the appearance and increasing prevalence of T2D and IGT among Aboriginal youth8-10. Community screening programs are critical components in increasing awareness and willingness to undertake change3,5,6. They provide the evidence base for the development and support of viable interventions.
The history of a relationship between researchers and community
Personnel from the Department of Pediatrics, University of British Columbia (UBC) had previously established a partnership with a remote First Nations community in the context of an oral health program11. The program, which had been running for approximately 3 years, involved two pediatric residents and a pediatric faculty member attending the community monthly or six-weekly to: encourage participation in the oral health program; provide well-child clinics; follow up children with specific problems; and give health- and science-based presentations in the school. Following one of these visits, during which the team diagnosed a child with T2D, the community health director approached the principal investigator of the oral health program (AJM) to enquire about screening all their children for T2D. Because the community partnership was based on a history of listening to their concerns and mutual trust, we agreed to undertake the required screening in the community. There were significant logistical issues to be overcome to meet the community's request (Table 1).
Table 1: Logistical issues involved in undertaking the community screening project
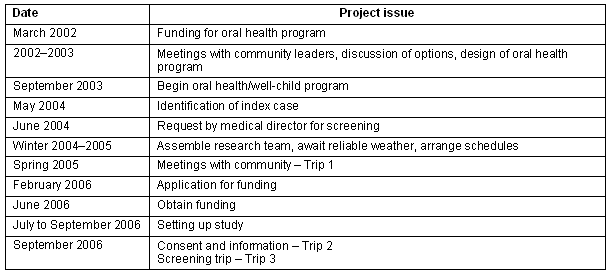
Description of the type 2 diabetes screening project:
Screening protocol
The diabetes screening protocol involved administering a 2 hour oral glucose tolerance test to children between the ages of 6 and 18 years, following a 12 hour fast. An intravenous saline lock was inserted to prevent imposing two venipunctures on the children. Blood was collected for analysis of lipid profile (total cholesterol, triglycerides, HDL and LDL) and glycosylated haemoglobin, as well as glucose and insulin (baseline and after 2 hours). Anthropometric measurements including height, weight, blood pressure and abdominal/waist hip circumferences were also collected. Several pieces of major equipment, not available in the community, were provided by the team, including an automated blood pressure machine, portable -20°C freezer, portable stadiometer, and accurate weigh scale. All were purchased for the project, with the exception of the automated blood pressure machine which was borrowed from BC Children's Hospital.
The Project
The success of the project was strongly dependent on the groundwork performed. This required two trips to the community in advance of the actual screening trip, with substantial work completed by both the university and community members between visits.
Trip 1: The objectives for this trip were to discuss the project with the community, reaffirm the commitment of community leaders to the project, and ensure community members' desire to participate in the project.
Dialogue The 'elder' investigators met with community Elders and then hosted a dinner (feast) for the community. At the dinner, the investigators gave a presentation and the Elders spoke in support of the project. It was necessary to involve and have support from leaders at all levels - traditional (Elders and hereditary Chiefs), political bodies (band council and elected chief), school leaders and community health leaders. The community health workers and Elders promoted the project to the community. Ultimately, every person in the community knew about the study through the presentations and by word of mouth, resulting in complete community support. The previously established rapport was strengthened through this community involvement.
Between Trips 1 and 2: The objective of this phase was to prepare for Trips 2 and 3.
Facilities The community health representative was asked to identify a suitable place that would have the necessary facilities and equipment (power, sinks, space, tables, chairs, audiovisual equipment) for conduct of the study. The goal was to be separate from both the school and clinic to minimize disruption to their usual operation, and to enable us to watch the children and control practical elements during the screening protocol.
Establishing understanding of test procedures and obtaining consents The community health representative distributed information letters to the parents, and scheduled parents and children to attend the clinic to have their questions answered by a team physician and to provide consent/assent.
Preparation and planning Extensive preparation was necessary to ensure that all equipment and disposable supplies were obtained and delivered to the community, as any essential items not taken in were very unlikely to be available locally. An actual run-through was conducted, noting the number of each item required to complete a single test, as it was necessary to take everything, including redundant items (in case of breakage or unexpected higher consumption than anticipated) and spare parts.
Selection of screening team The selection of the team members was critical. The five individuals needed a wide range of medical and research skills and the ability to function self-sufficiently to minimize impact on community resources. The team consisted of the principal investigator (pediatric endocrinologist), a registered nurse with over 30 years' experience in pediatric intravenous insertion, an experienced laboratory technician (doctoral student) to process blood samples in a timely fashion, a pediatric resident to assist with anthropometric measurements and blood handling, as well as an 'elder' research associate with whom the community had previously felt at ease.
Involvement of community leaders The community health director and community health representative were intimately involved in scheduling trips to mesh with school programs, arranging facilities and working with the school to arrange student absences.
Trip 2: The objectives of this trip were to explain the details of the project, ensure community support, obtain consents and assents, schedule subjects for screening and confirm access to facilities.
Involvement of community leaders The community health director and the UBC team jointly hosted an open meeting to answer final questions, ensure full understanding about the project for a population unfamiliar with clinical studies, and establish the need for children to provide written assent.
Obtaining consent/assent Parents and children were scheduled to attend the health clinic to meet with the team members, to have the study explained to them individually, and to have an opportunity to ask questions in confidence. Consent and assent forms were provided, and subjects had at least 24 hours to read them and ask questions before signing. When the forms were returned, children were assigned a time to attend for the screening procedures. A community member identified children within the same family, or cared for in the same home (eg the community health representative knew if the parents were planning to be away and the child staying with an aunt or grandparent), and ensured that they were scheduled for the same day and time if desired by the family.
Trip 3: The objectives for this trip were to transport the team and necessary equipment to the community, complete screening on all children for whom consent had been obtained, and process and return samples and the team to Vancouver.
Chartered float plane A robust but small float plane with large payload capacity (DeHavilland DH-2 Beaver) was chartered. It was necessary to ensure that the weight of passengers and equipment did not exceed the capacity of the plane and that weight could be distributed to place the majority of weight below the wings rather than in the aft storage space. Equipment was packed for flight in small individual packages to fit in the pontoons, and stay dry. The chartered aircraft was selected because it allowed the team to ensure that the freezer remained at temperature, the amount of equipment could be managed, travel time was flexible and minimized, the complexities of obtaining security clearance for our biohazardous materials were avoided, and samples remained in our possession the entire time. This process minimized the possibility of data loss through loss of sample integrity, because the study would be impossible to repeat.
Scheduling and compliance of subjects Each evening, the community health representative telephoned each child or family scheduled for the following day to remind them to fast, and to confirm the appointment time for the screening. He also rescheduled children when there were problems (no shows, failure to fast), and rearranged the schedule in real time to maximize the number of children seen on any given day.
Management of blood samples Blood samples were spun, plasma aliquoted, reagents added, and samples frozen immediately, in situ. Glucose levels were tested at the point of care using a glucometer to back up a minimal data set, in the event of loss of sample integrity before delivery to the laboratory.
Flexibility in logistics It was necessary that our schedule be flexible to accommodate the community's schedule and activities, and to allow for the possibility of delays due to adverse weather preventing teams from accessing the communities (or departing from them). On our first screening trip, the float plane arrived and was loaded. The pilot then spent almost an hour trying to discern from satellite imaging, reports of other pilots who had flown along the coastline that morning, and individuals at potential refuelling sites, whether it would be possible to make the trip. Finally, he informed the team that he could fly us approximately 1 hour northwest (to Campbell River) where he would land to check the weather farther up the coast. A subsequent return to Vancouver while paying for the travel time (without having achieved anything) was possible, but it was also possible that the fog along the coast would lift. The team decided to proceed. At the waypoint, the plane was refuelled, but the next waypoint was still fog-bound. After another hour's wait, the pilot determined that it would be possible to land at the next waypoint (Bella Bella) but a telephone call to the actual community indicated that visibility there was approximately 100 m - far less than needed for a safe landing - but that the previous day, the fog had lifted shortly after noon. Based on this information, and having learned far more about katabatic and anabatic air flow carrying fog (down and up the mountain valleys, respectively) than they ever wanted to know, the team again decided to proceed. At Bella Bella, a telephone call to the community indicated that the fog was lifting. In this stressful and potentially costly (in the event of having to abort the trip) stepwise fashion, the team finally arrived in the community, late and hungry, but safe.
Challenges and keys to success
Importance of community desire for project, comprehension, and ownership
The study was requested by the community and, consequently, the members of the community had a strong desire to ensure the successful completion of the screening. The members of the community initially had limited understanding of the need for screening or the complexity of the process and the importance of compliance with fasting procedures. It was therefore critical that the community members be given appropriate and adequate information to enable them to make decisions about supporting the program and, ultimately, to understand the results of the screening. It was also important to clarify with the community that the results would be shared with the community, and that there would be common ownership of the results, giving the community responsibility for acting on the results.
Importance of community relationship with researchers
The previously established collaborative and symbiotic relationship resulted in trust between the community and the researchers. This relationship made the screening program possible. Without it the invasiveness of the procedures and the appearance of 'parachuting in an entire medical team' would have been seen by the community as another example of externally-imposed medicine, and a violation of their community and culture. Maintenance of confidence and trust were critical aspects for conduct and interaction with community members, because sustaining the partnership was important for the health of the community, and for ongoing opportunities to investigate other health problems unique to such rural and remote communities.
Considering cultural context
It is important that investigators consider the cultural context. In our case, this included a history of paternalistic western medicine that ignored traditional medicine and approaches, and also high levels of animosity toward 'white men' and 'outsiders' because of ongoing conflict over land claims and residential school abuses12. It was necessary to address the attendant barriers and high levels of suspicion through a history of open communication and transparent behaviour, before a project as potentially invasive as pediatric diabetes screening could be undertaken. On the positive side, the remoteness of the community resulted in it being cohesive, with information traveling quickly and effectively by word of mouth.
Taking enough time
It was critical to take sufficient time to establish community involvement and support, and to work with the schedules of a remote community that does not operate at the fast pace anticipated by a project team used to conducting research in a tertiary care facility.
Addressing issues of access and travel
The pragmatic issues of getting the team, complete with equipment, to the community were challenging and required a great deal of consideration. The community is distant from our centre and remote - one hour by float plane or 4 hours by ferry from the nearest community with stores and hospital facilities (Fig1). There is no road access. Commercial travel to the community involves 2 hours by commercial airline to the nearest large community, transfer between airport and seaport, and an additional hour by float plane. Travel costs are high. This aspect of the budget was difficult for granting agencies to understand. Poor weather often prevents access to the community, and has meant teams aborting trips part of the way through (incurring cost without result) or teams being stranded in the community (incurring additional housing costs).
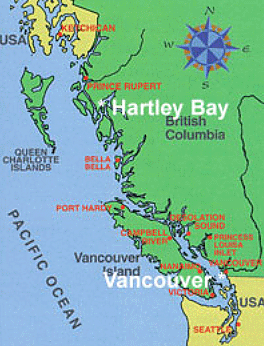
Figure 1: Location of the community on the central coast of British Columbia, Canada, 668 km north of Vancouver, the home base of the research team.
Using appropriate facilities and equipment
It was necessary to arrange appropriate facilities that would not disrupt normal health clinic function and that would avoid the potential for emergency clinic activity to disrupt the study. These facilities needed to have sufficient space with privacy for measurements, uninterrupted power, fridge, stove and audiovisual services.
Ethical considerations
When conducting research with Aboriginal populations, and particularly with Aboriginal children, ensuring that the research is conducted in an ethical manner is critical. Because of past practices and perceptions of past practices, in which data and blood samples from Aboriginal Canadians were used for research without the knowledge or permission of the individuals, our ethics process had to be completely transparent and inclusive2,13-15. However, meeting the conflicting needs of the institutional review board (IRB) and the cultural issues concerning children providing assent/consent was difficult. In particular, the community structure is such that the Elders are responsible for the welfare of the children, and the concept of a child providing informed assent was foreign to the community. In fact, some parents initially said that the children would not be allowed to provide assent, and that the parents' consent was enough. It was only after it was explained that this was a requirement of the university, and that the team could not force the children to submit to an invasive procedure such as having their blood collected, that the parents relented and allowed the research team to seek assent from the children.
Furthermore, ensuring confidentiality in a small community is a challenge, although this was considered more necessary by the IRB than by the community members. For example, after the team member obtaining consent had been very careful to maintain confidentiality when discussing one family's questions about whether their newly-pregnant daughter could safely participate in the study, the mother left the meeting room and announced in front of all of the people in the waiting room 'she's pregnant, you know'. In another example of the community's demonstration of their openness and lack of perceived need for confidentiality within the community, when the research team identified a child with impaired glucose tolerance and asked that the clinic staff arrange an appointment for the family to meet with the endocrinologist, the clinic staff immediately telephoned the school secretary to ask that the child be excused from school to meet with the doctor to discuss the results of the screening, clearly identifying the child and the reason for the meeting. It is important to note, however, that this openness is within the community where many are related by blood or marriage, and that the community members are less willing to share confidential information so openly with outsiders.
Cam Hill, member of the Eagle Clan and teacher in the community, identified the biggest challenge for the community as the issue of trust.
We didn't want to be guinea pigs, so seeing familiar faces on a regular basis helped everyone feel more comfortable and eager to do what it takes to make their community a healthier place16.
Finding funding
Obtaining sufficient funding to ensure successful completion of the screening was difficult because, from the granting agencies' perspective, the dollar rate per child screened was very high. Costs, including providing a dinner/informational meeting for the whole community and chartered travel, were seen as 'unusual' or 'excessive', but in fact were critical to the success of the project.
Summary
The measure of success of this approach is that 100% consent was obtained and data were obtained on 85% of the children. Blood samples were obtained on 29 of 33 eligible children (one failed to fast and had been scheduled for the date of departure so could not be rescheduled, two were absent from the community, and the team was unsuccessful at obtaining intravenous access in another). All plasma samples were returned to BC Children's Hospital laboratory intact and still frozen, and have since been successfully assayed. The results will be presented to the community and submitted for publication in a peer-reviewed journal. Following discussions with elders, teachers, parents and children, the team will work collaboratively to design an intervention program that the community supports and believes it can maintain with the support of the ongoing pediatric resident community visits associated with the oral health program.
Conclusions
Community-based screening for T2D of a pediatric population in a remote location is feasible. With careful preparation in the community (listening, establishing trust, understanding cultural context and meticulous attention to all aspects of ethical issues) and comprehensive logistic preparation, meaningful results that are valuable to the community's health can be obtained. The process described here can be replicated for other types of studies in other challenging or complex environments. Making optimum use of the special attributes and experience of the two halves of the team (community- and university-based) is critical to success.
Acknowledgements
The authors wish to thank the Lawson Foundation and the University of British Columbia Special Populations Fund for project funding. Also acknowledged are the Child & Family Research Institute (Clinician Scientist Career Award, CP), the Peter Wall Institute for Advanced Studies, University of British Columbia (Distinguished Scholar in Residence, AJM) and David Benton, Community Health Director.
References
1. The Standing Committee on Social Affairs, Science and Technology. The health of Canadians - the Federal role, final report. Volume 6, Recommendations for reform. Ottawa, ON: Government of Canada, 2002.
2. Assembly of First Nations. First Nations Health Research and Information Action Plan (Online) 2005. Available: http://www.afn.ca/cmslib/general/HRI2005711152443.pdf (Accessed 9 August 2007).
3. Bisset S, Cargo M, Delormier T, Macaulay AC, Potvin L. Legitimizing diabetes as a community health issue: a case analysis of an Aboriginal community in Canada. Health Promotion International 2004; 19: 317-326.
4. Fisher PA, Ball TJ. Tribal participatory research: mechanisms of a collaborative model. American Journal of Community Psychology 2003; 32: 207-216
5. Daniel M, Green LW, Marion SA, Gamble D, Herbert CP, Hertzman C et al. Effectiveness of community-directed diabetes prevention and control in a rural Aboriginal population in British Columbia, Canada. Social Science and Medicine 1999; 48: 815-832.
6. Herbert CP. Community-based research as a tool for empowerment: the Haida Gwaii Diabetes Project example. Canada Journal of Public Health 1996; 87: 109-112.
7. Macaulay AC, Ryan JG. Community needs assessment and development using the participatory research model. Annals of Family Medicine 2003; 1: 183-184.
8. Kaler SN, Ralph-Campbell K, Phar S, King M, Laboucan CR, Toth EL. High rates of the metabolic syndrome in a First Nations Community in western Canada: prevalence and determinants in adults and children. International Journal of Circumpolar Health 2006; 65: 389-402.
9. First Nations Centre. First Nations Regional Longitudinal Health Survey 2002/2003: results for adults, youth and children living in First Nations communities: Diabetes. Prince George, BC: First Nations Centre, 2005.
10. Young TK, Dean HJ, Blett B, Wood-Steiman P. Childhood obesity in a population at high risk for type 2 diabetes. Journal of Pediatrics 2000; 136: 365-369.
11. Macnab A, Rassekh R, Lai YH, Benton D, Duffy D, Gagnon F et al. Development of a symbiotic relationship with a remote First Nations community leading to a collaborative school-based oral health program. IHS Prim Care Provider 2005; 30: 230-333.
12. Indian and Northern Affairs Canada. Royal Commission on Aboriginal Peoples Report. Looking forward looking back, volume 1. (Online) 1996. Available: http://www.ainc-inac.gc.ca/ch/rcap/sg/sgmm_e.html (Accessed 9 August 2007).
13. Indian and Northern Affairs Canada. Royal Commission on Aboriginal Peoples Report. Renewal, volume 5. Appendix E: Ethical guidelines for research (Online) 1996. Available: http://www.ainc-inac.gc.ca/ch/rcap/sg/ska5e_e.html (Accessed 9 August 2007).
14. Canadian Institutes of Health Research. CIHR guidelines for health research involving Aboriginal peoples - Draft 1. Ottawa, ON: CIHR, 2005.
15. American Academy of Pediatrics. Policy statement on ethical considerations in research with socially identifiable populations. Pediatrics 2004; 113: 148-151.
16. Thomson H. Remote community engages UBC to tackle diabetes. UBC Reports 2006; 52: 4-6.


