full article:
Introduction
The Rural Physician Associate Program (RPAP) of the University of Minnesota Medical School is a 36-year-old program that provides third year medical students with a nine-month community-based, clinical continuity care experience1-3. Students are mentored by a primary preceptor over a period of months.
Historically, the students' 2 day orientation included introductions to the RPAP experience and coursework, communication skills, and resuscitation training. In recent years, student feedback indicated dissatisfaction with resuscitation training during orientation. A review of the literature revealed a paucity of published curricula directed to orienting students to long-term community rotations. However, literature in community-based learning recognized the challenges for new students with undifferentiated clinical problems and the emotional nature of the patient's world view. A prior sensitization experience was posited to ease students' adaptation to a community setting4.
In response, faculty considered the types of clinical skills that might be most useful for students who were starting in apprentice roles. The Interprofessional Education and Resource Center (IERC), a clinic setting designed for teaching and testing health professions students on clinical skills through the use of standardized patients and human patient simulators, presented creative learning opportunities. The orientation was restructured to include a day of clinical skills training in 2005 using the objective structured clinical examination (OSCE) for teaching as opposed to testing5. To date two classes of RPAP students have participated in this experience.
Methods: Clinical skills day description
Objectives
The learning objectives of the full-day experience included to:
- Distinguish urgent from non-urgent clinical presentation.
- Use clinical guidelines for making decisions.
- Communicate effectively in stressful situations.
- Uncover a significant clinical issue with a different presenting complaint.
Orientation
Prior to the day, faculty received an on-line presentation orienting them to the IERC, and the teaching model and the scenario assigned to them. Evidence-based guidelines were provided for context and to share with the students as resources to utilize during their RPAP experiences. A brief face-to-face orientation session was held before the students arrived.
Students reviewed an on-line audio-visual presentation orienting them to the IERC and outlining the learning expectations for the day. Otherwise, students were not expected to prepare for the day because this was an immersion learning experience.
Evaluation
Evaluations were completed at the end of the day by both students and faculty. The final evaluation completed by students at the end of the 9 month RPAP experience also enquired about the value of the clinical skills day. Analyses of these data included simple descriptive statistics (quantitative) and written comments organized into representative themes (qualitative). The University of Minnesota Institutional Review Board granted exemption from formal review.
Case scenarios
Cases scenarios were written for a variety of diagnoses in patients of differing ages. Less complex primary care problems were given 20 min. Complex problems including acute abdomen, labor and delivery management, and two urgent cases (chest pain and major trauma) were allocated 45 min. All experiences occurred in the IERC which offers 18 fully-equipped ambulatory examination rooms with a computer for accessing data and a video camera for central monitoring. The IERC also oversees the University of Minnesota's health sciences simulations and Standardized Patient Program, which recruited and trained the patients participating in this event.
Faculty recruited from the department of family medicine and community health and the department of emergency medicine supervised the stations. They were present in each room as observers, facilitators and educators. Their roles were more active or passive, depending on the case scenario and the presence of simulated or standardized patient. Each station, except the radiology station, involved a debriefing at the end for final questions, distribution of educational resources or summary teaching points. Standardized patients also gave the students feedback.
Students were randomly assigned to small groups of three to four students that rotated through the stations as a unit. Groups were combined for the longer cases. The students were encouraged to take turns leading the interview among stations. The schedule was monitored centrally with overhead announcements informing students when to begin and when 5 minutes remained. After completing the interview the student performed a directed examination, as appropriate, for the content of the station. The lead student could ask the other students to assist him/her as needed. The faculty member observed and taught at appropriate junctures. Near the end of the time period, the standardized patient and faculty debriefed the students on the salient issues, provided directed feedback to the students and shared the evidence-based guidelines provided for the station.
Primary care cases (20 min each): Anaphylaxis After receiving an influenza vaccination, a middle-aged patient had an anaphylactic response. The objectives of the station were to recognize the symptoms and signs of acute anaphylaxis, to understand the basic treatment, and to educate the patient in the use of appropriate avoidance and protection from anaphylaxis in a situation of a known allergen. The Diagnosis and Management of Anaphylaxis: an Updated Practice Parameter guideline was used6.
Pediatric upper respiratory infection A young mother presented with her screaming 15 month old baby, requesting antibiotics for an uncomplicated upper respiratory infection. The challenge for the student was dealing with an exhausted and difficult parent. The objectives were to assess presenting symptoms and decide whether the case was urgent or non-urgent. Then the student educated the parent on the child's status and provided appropriate educational resources (ie the difference between bacterial vs viral illness, appropriate antibiotic usage). Further, she/he practiced effective communication in the setting of a crying infant and a demanding parent. The Institute for Clinical Systems Improvement (ICSI) Health Care Guideline: Viral Upper Respiratory Infection in Adults and Children was used7.
Knee injury A middle-aged man presented with knee pain after a weekend of playing football. The objectives of this station included the ability to gather information about the nature of the injury and to make a decision about whether or not to order an X-ray with the assistance of the Ottawa guidelines, and to inform the patient on basic assessment and plan8.
Heartburn and depression A 30-year-old female patient presented with symptoms of heartburn with an underlying significant depression. The objectives of this station were: to recognize the signs and symptoms of depression in a clinical presentation of unrelated complaints; to communicate with the patient about the diagnosis of depression; to recognize the need for urgent psychological/psychiatric intervention; and to develop a contract with the patient should she become suicidal. The Institute for Clinical Systems Improvement healthcare guideline: Major Depression in Adults in Primary Care' was utilized9. The Patient Healthcare Questionnaire 9 was discussed as tool for assessing depression10. The standardized patient played a critical role in providing feedback to the students about which interviewing skills were productive in eliciting her information.
Radiology This station was the only one without role-play by a standardized patient. Instead, a series of different X-rays were presented based on brief case scenarios with the following objectives: to review an X-ray in an organized approach and to find basic abnormalities on X-ray assisted by clinical details.
Complex cases (45 min each): Acute abdomen The acute abdomen station included two scenarios involving standardized patients. One was a 24 year old with right lower quadrant abdominal pain and delayed menses. In this scenario students thought through the differential and management of a young woman who might be pregnant, have a sexually transmitted disease or an appendicitis. The second scenario was a 70 year old woman with left lower quadrant abdominal pain. Guidelines about the appropriate imaging for abdominal pain were available11-13. The learning objectives for the acute abdomen stations were: to obtain presenting complaints and perform a limited physical examination; to develop a differential diagnosis considering the four quadrants; and to understand when surgery might be indicated for the acute abdomen.
Labor and delivery management Two scenarios dealt with issues related to labor and delivery using a patient simulator and a standardized patient. The learning objectives for the station on prolonged labor with a patient simulator included: exposure to a labor curve and fetal monitoring strips; assessment of prolonged labor/failure to progress; identification and management of failure to progress; and performance of uncomplicated vertex vaginal delivery. This station also involved the APGAR scoring of the newborn and the management of post-partum hemorrhage. The second labor station featured the early presentation of labor with a standardized patient and the following learning objectives: obtain presenting symptoms and pregnancy history and to decide on urgency or non-urgency; to understand how to perform the basic tests required to assess labor and fetal health; and to educate the patient on expectations for labor and delivery.
Urgent stations Both urgent scenarios (chest pain and major trauma) used a patient simulator. The objectives were that students articulate, not answer, four to five questions from the following list: What basic emergency equipment does my facility have? Where is it kept? How does it work? Who knows how to use it? Where can I find quick references for emergency interventions? Who is on our emergency care team? What are the critical care capabilities of this facility? What management and transfer protocols exist at this facility? What are our referral centers and mechanisms of transfer?
The chest pain scenario consisted of an inferior myocardial infarction with bradycardia and pulseless electrical activity (PEA) arrest. Students conducted a basic resuscitation for this rhythm, including airway management, and discussed the elements of effective communication with patient families and medical colleagues/consultants. At the conclusion of this station, students were provided with the Handbook of Emergency Cardiovascular Care for Healthcare Providers and familiarized themselves with the resource using a scavenger hunt format14.
A major trauma scenario involved the victim of an all terrain vehicle accident. Managing this patient with abdominal trauma and shock, students verbalized understanding of major sources of morbidity in major trauma. These included airway/breathing abnormalities, shock and neurotrauma, and how to prioritize trauma care in order to address these concerns. Students conducted a basic secondary survey for trauma and formulated a diagnostic, treatment and disposition plan consistent with the patient's condition and the facility's capabilities.
Results
Seventy-seven students have participated in the clinical skills day. Evaluations were collected from 76 medical students (30 from 2005 and 46 from 2006). One student did not hand in any evaluations. Students completed three evaluations: one for the 45 min stations, one for the 20 min stations, and one administered at the end of the day evaluating the experience as a whole. In 2005, the evaluation for each station type used four general, summary items to assess the students' perceptions of the event, the degree to which it reinforced or improved their skills and knowledge, and their confidence as student practitioners. In 2006, students were asked to evaluate learning objectives more specifically (eg their ability to recognize symptoms of depression or to find abnormalities on an X-ray). Responses to all items used a 5 point Likert scale (strongly disagree to strongly agree). Students were also asked for open-ended written comments at the end of each evaluation form. The final evaluation completed after the 9 month rotation also included three questions about the day. One questions asked about the helpfulness of the experience, using a 5 point Likert response scale. The second question asked how the experience could be improved, and the third listed the four objectives and asked for written comments about how the student applied the learning at the RPAP site. Fifty-nine students completed this evaluation.
Table 1 shows the overall mean for each station. Table 2 presents the day's evaluation immediately after the event. Students rated the stations and overall day positively, with means well above four on the 5 point scale.
Table 3 includes qualitative data from written comments at the end of the experience organized in themes. Quotations representing each topic area for a theme are presented. Overall, student comments were positive. Several students in both classes recommended expansion of this type of simulation throughout the medical school curriculum. In 2005, one deficit noted by students, faculty and staff was the need for greater preparation of both students and faculty instructors. Not all instructors were able to practice scenarios with the equipment (especially the patient simulators) before the event, and logistics made it difficult for an on-site orientation the day of the event. In 2006, several students complained about the length and intensity of the day. This may have been due to incorporating two scenarios into the longer stations which was done in order to address the 2005 staff and faculty's perceptions that the longer stations needed more content.
On the evaluation 9 months later, the majority (71%) thought the orientation was very helpful (15%) or helpful (56%). A quarter rated the experience as adequate (24%) and 5% did not think the experience was helpful. Table 4 summarizes the written comments 9 months later about how to improve the day and how the learning was applied. A few could not remember the specifics of the day, but had retained a positive impression of it.
Table 5 presents the evaluations by all 2006 faculty performed immediately after the experience. Responses were on a 5 point Likert scale (strongly disagree to strongly agree). Written comments were also encouraged. Formal faculty evaluation was not made in 2005. The experience caused some to reflect on their teaching, the content of the scenarios, and the medical school curriculum in general. For example, one faculty member at an acute care station wrote, 'I felt like I scared the students a bit'. Several others indicated that they left with a strong sense of the need to incorporate more of this kind of content and more active learning strategies into the curriculum.
Table 1: Mean for each urgent and non-urgent station for two Rural Physician Associate Program classes, 2005 and 2006

Table 2: Summary evaluations for the entire clinical skills day for two Rural Physician Associate Program classes, 2005 and 2006

Table 3: Student comments about the clinical skills day two Rural Physician Associate Program classes, 2005 and 2006
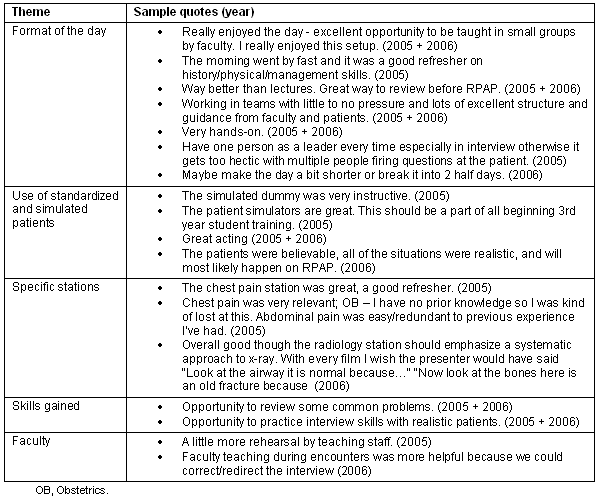
Table 4: Summary of themes of student comments about how learning from the clinical skills day was applied during the Rural Physician Associate Program rotation, and suggestions about improving the day

Table 5: 2006 Faculty summary evaluation (n = 15)

Discussion
Student feedback about the limited usefulness of resuscitation skills training as orientation to a rural longitudinal clerkship encouraged faculty to develop an active, learner-centered experience with broader and more appropriate objectives. Using the OSCE format for teaching as opposed to testing has been done by others and, as our evaluations suggest, it was well received by the students15. Students learned eagerly in a non-competitive and supportive environment. The increased content and the intensity of the urgent care stations may have led to the complaints about the length of the day. In the future, RPAP faculty will continue to use student and faculty feedback to make improvements for the following year. While evaluations immediately after the event are essential, enhanced longitudinal assessment following the students' RPAP community experiences will impact the design and support of the teaching experience.
The RPAP students are immersed in their settings, working with 'experts', physicians who have been in practice for several years16. They can use intuition where empirical knowledge does not yet exist. 'Learning for mastery' or outcome-focused and competency-based teaching objectives that encourage students to acquire skills at the level of a practicing physician, enables students to put all their skills together17. Introducing them to this early in a realistic, facilitated experience is the value of the OSCE format5.
Conclusions
The clinical skills day experience immersed students into situations that they would be facing in their settings. This provided them with opportunities to begin to understand the complex skills that they would need before they learned them step by step. Building a bridge between skills-laboratory learning and real-life communities of practice using faculty-assisted simulated clinical learning is valuable18. Evaluations were positive both immediately after the experience and 9 months later. As we ponder how to improve medical education19, the evaluations for this clinical skills day support the value of learning that is realistic, active and faculty facilitated.
References
1. Halaas GW. The rural physician associate program: Successful outcomes in primary care and rural practice. Rural and Remote Health 5: 453. (Online) 2005. Available: http://www.rrh.org.au (Accessed 30 August 2007).
2. Verby JE, Feldman B. The rural physician associate program (RPAP). A righton program for all participants. Minn Medicine 1983; 66:181-185.
3. Verby JE, Newell JP, Andresen SA, Swentko WM. Changing the medical school curriculum to improve patient access to primary care. JAMA 1991; 266: 110-113.
4. Howe A. Twelve tips for community-based medical education. Medical Teacher 2002; 24: 9-12.
5. Harden RM, Gleeson FA. Assessment of clinical competence using an objective structured clinical examination (OSCE). Medical.Education 1979; 13: 41-54.
6. Lieberman P, Kemp SF, Oppenheimer J Lang DM, Bernstein IL, Nicklas RA et al. The diagnosis and management of anaphylaxis: an updated practice parameter. Journal of Allergyand Clinical Immunology 2005; 115: S483-S523.
7. Institute for Clinical Systems Improvement. Viral upper respiratory infection in adults and children. (Online) 2004. Available: http://www.icsi.org (Accessed 3 February 2007).
8. Tandeter HB, Shvartzman P, Stevens MA. Acute knee injuries: use of decision rules for selective radiograph ordering. American Family Physician 1999; 60: 2599-2608.
9. Institute for Clinical Systems Improvement. Major depression in adults in primary care. Health care guidelines. (Online) 2007. Available: http://www.icsi.org (Accessed 30 August 2007).
10. Spitzer R, Kroenke K, Williams J. Validation and utility of a self-report version of PRIME-MD: the PHQ primary care study. JAMA 1999; 282: 1737-1744.
11. AHRQ, National Guideline Clearinghouse. Evaluation of acute lower right quadrant pain. American College of Radiology - Medical Specialty Society. NGC: 004780. (Online) no date. Available: www.guidelines.gov (Accessed 31 January 2007).
12. AHRQ, National Guideline Clearinghouse. Evaluation of left lower quadrant pain. American College of Radiology - Medical Specialty Society. NGC:004773. (Online) no date. Available: www.guidelines.gov (Accessed 31 January 2007).
13. AHRQ, National Guideline Clearinghouse. Evaluation of patients with acute right upper quadrant pain. American College of Radiology - Medical Specialty Society. NGC:004781. (Online) no date. Available: www.guidelines.gov (Accessed 31 January 2007).
14. American Heart Association. Handbook of emergency cardiovascular care for healthcare providers 2006. Dallas Tx: American Heart Association, 2005.
15. Austin Z, Gregory P, Tabak D. Simulated patients vs. standardized patients in objective structure clinical exams. American Journal of Pharmaceutical Education 2006; 70: 119.
16. Eraut M. Developing professional knowledge and competence. London: Falmer Press, 1994.
17. Benbassat J, Baumal R. A proposal for teaching basic clinical skills for mastery: the case against vertical integration. Academic Medicine 2007; 82: 83-91.
18. Kneebone RL, Scott W, Darzi A, Horrocks M. Simulation and clinical practice: strengthening the relationship. Medical Education 2004; 38:1095-1102.
19. Irby DM, Wilkerson L. Educational innovations in academic medicine and environmental trends. Journal of General Internal Medicine 2003; 18: 370-376.



