Introduction
The geographic distribution of physician in the United States of America has been often described as unbalanced or maldistributed1. This is the result of multiple factors, one of them being the migration. There are articles in the literature comparing distribution of physicians between urban and rural places, and between different regions2-4, but not much is written about the migration of physicians during the course of their professional career. There are multiple studies on attraction of physicians to a rural/underserved area5-8, as well as on dissatisfaction as a potential cause for leaving the area9,10. However, less attention has been paid to understanding the actual migration physicians make over the span of their careers and whether their moves are based on economic or professional considerations. One of the recent studies used a national sample of physicians to discover the reasons physicians moved from one area to a different one. These could be professional satisfaction/dissatisfaction, changes in interests, or changes in local/regional health policies11.
A Canadian study aiming at to characterizing physicians' migration based on their specialty and their practice location, showed that specialists were more prone to move into areas where income rose and where primary care physicians were leaving; while primary care physicians were more prone to migrate to areas where there were recent increases in the number of specialists12. A similar analysis of organizational factors was conducted on US physicians between 1985 and 1994, and showed that 'hospital consolidation' and managed care penetration were associated with an increase in supply of primary care physicians but with a decrease among specialists13. Jiang et al also put forward the idea of carrying capacity and revealed the existence of a competition phenomenon among specialized physicians. More precisely he showed that a change in the number of specialists has a significant negative relationship with the initial number of physicians in the specialty13. That study looked only at absolute changes in supply, not in the dynamics of change, using a national sample of young physicians (aged less than 40 years). Other studies found that up to one-third of physicians change their practice arrangements within 5 years of the start of their careers14, and that the average tenure of primary care physicians in any practice location beyond residency was 4.5 years15.
In summary, three types of factors could be associated with the migration of physicians: those related to the physicians, those related to the region of origin and those related to the region of attraction. Questions remained unanswered for the three types of factors. Among them, we were mainly interested in exploring the difference in the migration pattern, according to the region of origin. Thus, this study aimed to examine the geographic migration of physicians over a 22 year period (1981-2003), into and out the four US census regions (Northeast, Midwest, South and West). Specific objectives of this study were to: (i) describe physician and counties of origin characteristics of migrant physicians compared with counties of non-migrant physicians; (ii) describe the migration flow (origins and destinations) across US census regions taking into account the rural/urban status of the county of practice in 1981; (iii) evaluate determinants of migration; and (iv) to sketch specific profiles of migrants according to the four US census regions. We chose to compare clinically active primary care physician (CAPCP) migration across the four US regions instead of the 52 states, in order to provide enough physicians in each group to perform comprehensive tree-based analysis.
Methods
This is a two points in time observational cohort study using secondary data analysis. The studied population includes non-federal clinically active patient care physicians. All CAPCP in 1981 who were still active in 2003 entered the cohort. Federal, military and resident physicians were excluded as well as physicians with data missing from their file. The physician location data were drawn from the American Medical Association Physician Masterfile. The full files for 1981 and 2003 were merged and the data for each physician were matched across years. The matching process used an algorithm to match names, then other non-varying data such as medical school, gender and date of birth. The addresses for all of the physicians were verified and a common geocode was given for assignment into county classifications. This process was also subject to a priority protocol with values assigned to the accuracy of the matching process from exact street address for practice locations to match according to an assigned ZIP code centroid.
For the analyses, counties were classified according to the four US census regions. The main variable was the migration status of the CAPCPs, namely whether they were non-migrants, internal migrants or external migrants. Non-migrants were defined as CAPCPs with practice address in the same county in 1981 and 2003; internal migrants as CAPCPs with practice address in different counties in 1981 and 2003, but in the same census region; and external migrants as CAPCPs with practice address in different census regions in 1981 and 2003. Covariates used in the analyses were physicians' personal attributes as well as attributes related to the counties of the practice location in 1981. Physicians' covariables were gender and age (in 1981). Counties' covariables included the mean per capita income, the percentage of non-white population, the number of primary care physician per 1000 inhabitants, the number of hospital beds per 1000 inhabitants, as well as the rural/urban status of the county (LM, large metropolitan area or adjacent; SM, small metropolitan area or adjacent; or NA, non-adjacent to metropolitan areas). This former variable was defined using the 1993 Urban Influence Codes of the Economic Research Service, US department of Agriculture.
Descriptive analyses provide CAPCP characteristics and involve summary parameters such as means and proportions. The predictive models focus on the probability, for a given physician, of changing region of practice between 1981 and 2003 (external migration). The modeling process involves the usual logistic regression and the regression tree approach used by Zhang et al16-18. The tree-based method recursively partitions the population based on the explanatory variables and forms a number of more homogeneous sub-populations in which subjects are at the same level of risk. The first step is to split the entire sample (root node) into two groups on the basis of splits in the covariates and using a homogeneity function. All covariates are candidate for splitting. If the covariate is ordinal, then the split is performed according to whether it is less than a constant c and if it is nominal, the split is based on whether it is included in a subset B. The homogeneity function is calculated for all possible c and B, and the split which maximizes the homogeneity is selected. The second step consists of applying the same algorithm to the daughter nodes, each node taking the role of the root node, and the splitting process continuing until no more partition is possible. The resulting tree is then pruned by a backward deletion process (p value < 0.0001 for this study).
Results
Our analysis identified 83 383 non-federal primary care physicians who were registered as clinically active in both of the 1981 and the 2003 Masterfiles, and whose location could be geocoded to a county. When looking at the CAPCP migration at the US level for the 22 year follow-up period, 49 470 (59.3%) were practicing in the same county in 2003 as in 1981; and 33 913 (40.7%) had changed county, among which only 11 043 (13.2%) moved from one region to another (Table 1). Even though most CAPCPs were male, it was apparent that women were proportionally more prone to migrate during their career. Younger CAPCPs were also more inclined to change from one county to another in the same region (internal migrant), as well as from one region to another (external migrant). Gender repartition, mean age and proportion of migrant and non-migrant CAPCPs differed significantly between regions. CAPCPs were younger in the Midwest as the proportion of females is greater in the Northeast. The external migration rate in the Midwest region was almost double that of the West and South regions (Table 2).
Table 1: Characteristics of CAPCP according to the migration status at the region level
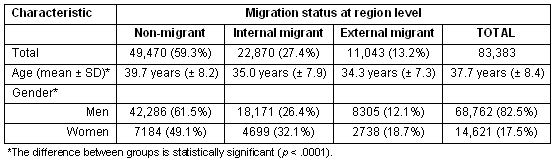
Table 2: Studied population characteristics by region
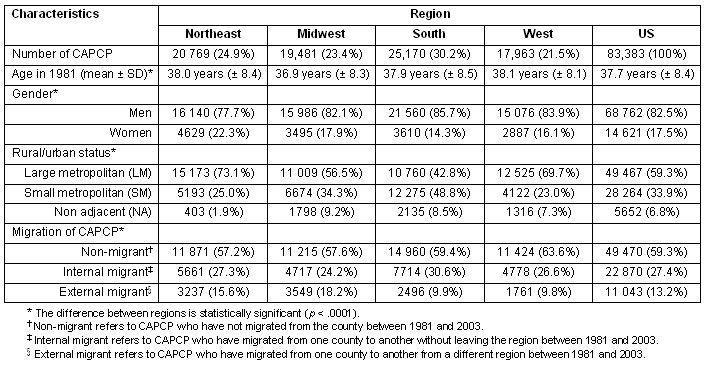
Figure 1 presents the flow of CAPCPs across and within the four US regions, and the net change observed. There is a greater outflow for the Northeast and Midwest regions with 16% and 18% of the 1981 workforce, respectively, compared with 10% for both the West and South regions. When taking into account the total flow (in and out) for each region, the West and the South 'benefited' from CAPCPs' migration with a 1.10 and 1.07 increase, respectively, in 2003 when compared with 1981; while the Midwest and the Northeast regions ended with 0.90 and 0.92 decrease in 2003. There is a clear Southwestern direction of CAPCPs' migration over the 22 year period (Fig1).
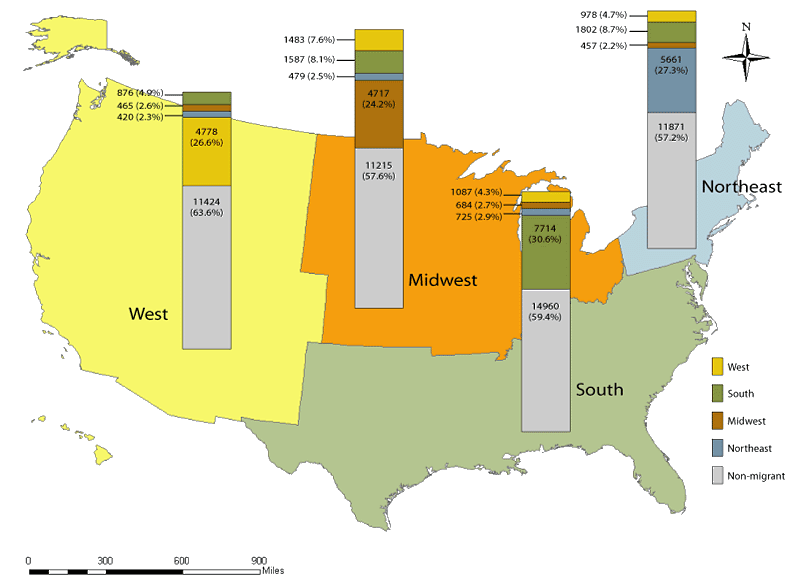
Figure 1: Migration of CAPCPs from one region to another between 1981 and 2003 (n = 83 383). #, Number of.
Table 3 presents the distribution of internal and external migrants according to their practice census region and rural/urban status. This table reveals that the two-thirds of migrant CAPCPs practicing in an LM in 1981 remained in an LM area in 2003; more than half of those practicing in an SM in 1981 remained in a SM area in 2003; while less than a quarter of those practicing in a county NA in 1981 remained in an NA area in 2003. These rates vary according to regions, particularly in the Northeast region, compared with the others.
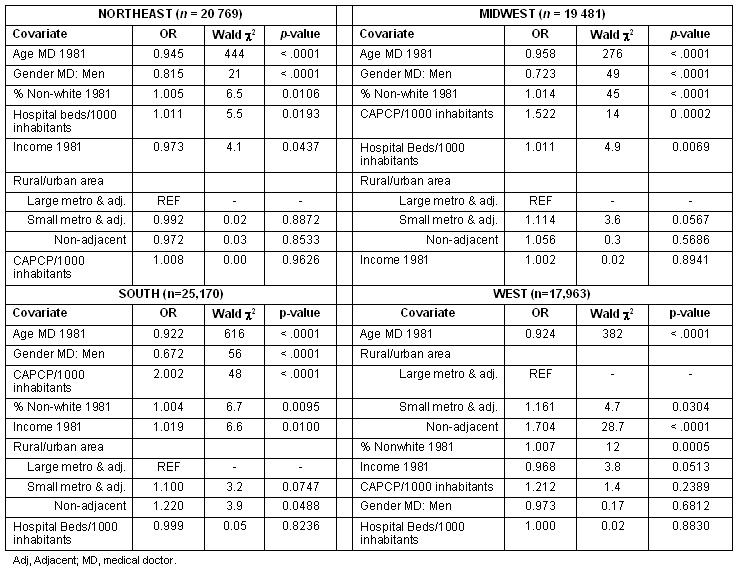
Results from the logistic regression analyses are presented (Table 4) and show that for all regions, physician's age and percentage of non-whites of the county of origin are statistically associated with external migration. Rural/urban status of the county of origin is related to external migration only in the West region. Another result is that female CAPCPs are more prone to migrate than males, except in the West region where no significant gender difference is noted for external migration.
Table 3: Migration distribution according to census region and rural/urban status (n = 33 913)
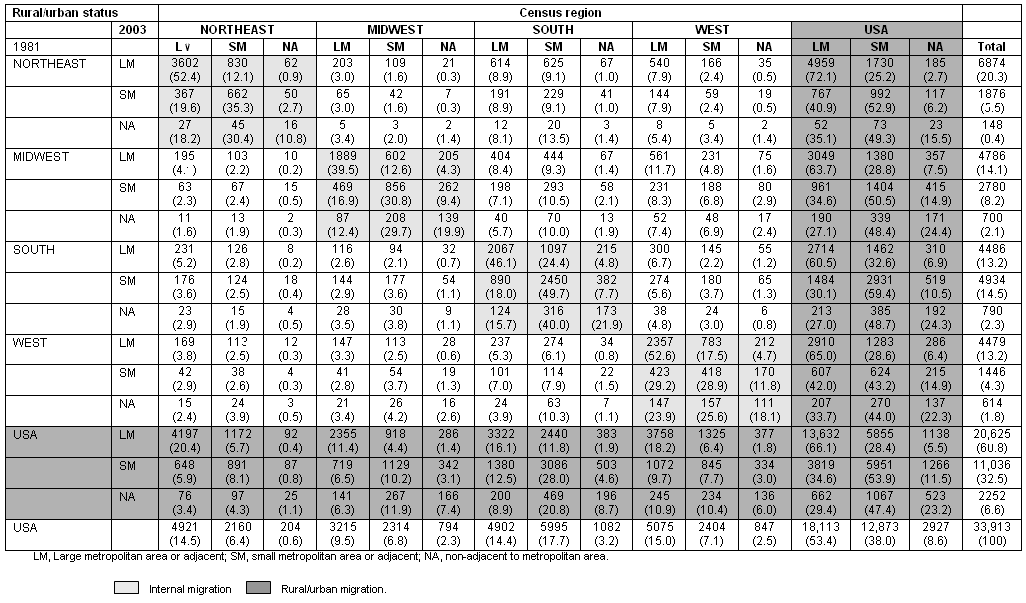
Table 4: Determinants of external migration: logistic regressions by region
Tree-based analyses (Fig2) provide complementary information to sketch the different profiles of external migrant CAPCPs for each region. The tree-based regression results were interpreted as follows. For all regions, age is the covariate that maximizes the homogeneity of the two daughter nodes with cutoff values varying from 32 years in the Midwest region to 38 years in the South, demonstrating that maximization appears at different cutoff points, depending on the region. Not only does the cutoff value differ among the four regions but so does risk. For example, in the Northeast region, the risk of migration associated with CAPCPs younger than 37 years is 21.1%, compared with 9.9% for those older; while the risk for younger migration is 25.9% compared with 14.6% in the Midwest, 14.1% vs 4.7% in the South, and 14.8% vs 6.3% in the West. Physicians' age, percent of non-white population in the county of practice in 1981, and the number of CAPCPs per 1000 inhabitants in the county of practice in 1981 appear at the second level of the trees, and thus constitute the second most important explanatory variables. The highest migration risk profile is generally presented on the left side and the lowest risk is presented on the right side. As an example, the highest migration risk profile for CAPCPs practicing in the Northeast region in 1981 was 27.0% and belongs to young CAPCPs (< 32 years old) practicing in a county with more than 8.6% non-white population. The lowest migration risk (8.8%) belongs to older physicians (≥42 years old). Table 5 summarizes the profile of those most at risk of migration and those least at risk for every Census region, as deduced from the tree-based analysis. The systemic pictures sketched by the tree-based analyses are different from one region to another, and the urban/rural attribute of the county of practice in 1981 only entered the model for middle-aged physicians practicing in the West region.
Table 5: CAPCPs' profiles for lowest and highest risk of external migration by region of practice in 1981
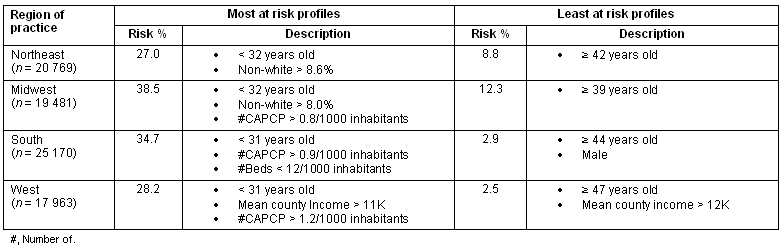
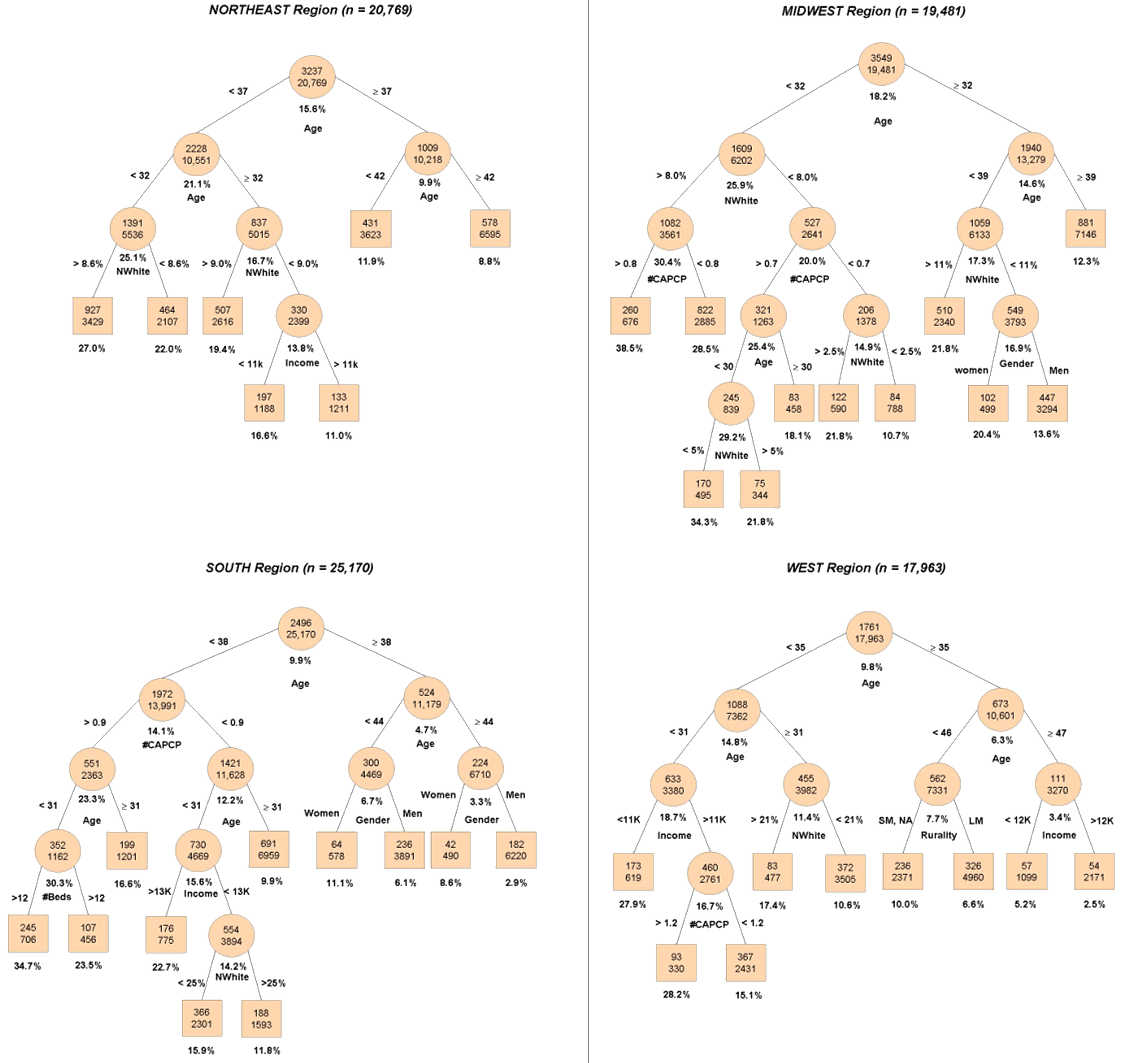
Figure 2: Determinants of external migration: regression trees analyses by region. Inside each circle and box, the number of migrants (first number) is given along with the sample size (bottom number). The risk associated with a node appears under the node along with the splitting rule. Pruned trees at level p = 0.0001.
Discussion
This cohort study looked at the net movement of CAPCP across the US regions from 1981 to 2003. It may provide an approximate idea of the factors related to a change in practice regions. The pattern shows a relative stability across regions. However, despite only 13.2% of all matched primary care physicians moving from one region to another over a 22 year period, as many as 27.4% moved and relocated to another county, but within the same region. Others studies8,19,20 have reported different migration rates; however these cannot be compared with those reported in this study due to major differences in the population studied and in the definition of migration and the time period of observation. However, the migration magnitude observed in the present study is similar to that reported by West et al19, where two out of three family physicians will practice at the same location throughout their career.
Other findings show that the absolute change across regions generally 'advantages' the South and West regions with the Midwest region being the most 'disadvantaged' by the migration flow. To our knowledge, the direction of the migration of the medical workforce has not been studied; however, a western and southern migration pattern has been reported for the general population between 1990 and 200421. In this period, the average annual domestic net migration rate was negative for the Northeast (-6.1? for 1990-2000, and -4.6? for 2000-2004) and the Midwest (-1.2? for 1990-2000 and -2.5? for 2000-2004) and positive for the South (4.1? for 1990-2000 and 3.4? for 2000-2004) and the West (0.1? for 1990-2000 and 0.8? for 2000-2004)21.
Seifer22 and Henderson4 studied the link between the state of medical training and the choice of location of practice, in order to quantify the capacity of medical training and retention among states. Using their data (at the state level), we calculated the average proportion of physicians practicing and trained in each region. We observed that Northeast, Midwest and South have higher proportions of physicians practicing in the same region they were trained, with respectively 47.2%, 42.8% and 40.5% retention rates. That can raise the hypothesis that West, with a retention rate of only 29.3%, will 'import' a higher proportion of their physicians to compensate.
Considering the determinants and the profiles of external migrant CAPCPs at the professional level, logistic and tree-based regressions clearly showed that age was a major factor. For all four regions, the age threshold generated by tree-based analysis was mid-30s, the younger CAPCPs being more prone to migrate. This is consistent with some previously published studies19,20,23. Logistic regression showed that female gender was a significant determinant of migration for all regions except for the West region. However, when taking into account interactions between covariates using tree-based analyses, gender seems to be mostly relevant for older CAPCPs in the Midwest and South regions. Other authors19,20 have also reported gender as a significant risk factor of migration, but with different effect according to the context (rural vs non rural). Conversely, Seifer finds that female gender is a significant predictor of physicians remaining to practice in the same state of their graduate medical education22. In Canada, gender is not a significant predictor of the probability of a physician moving to another province23. The explanation of why female CAPCPs show a higher risk of migration than males remains unclear. We can hypothesized that, at the considered time period (1981-2003), women were more prone to follow spousal career location. Further studies are needed to confirm or invalidate this hypothesis.
In the logistic model, the percentage non-white population in the county was a significant and positive factor for external migration for all four census regions, which is consistent with a previous study by Komaromy24. This factor also appears in all four trees, especially in Midwest, were the factor appears in many branches. Interestingly, in our study, the rural/urban status of the county of practice does appear to be a contributing factor only in the West for middle-aged physicians. Carpenter and Neun found that rural status is not a significant predictor in the choice of place of practice for the young primary care physicians25. Conversely, Benarroch and Grant found that the rural status is a negative predictor of interprovincial physician migration in Canada26.
Another expected variable, the mean per capita income, was a less important factor in external migration. Although previous studies25,27,28 have found a positive relationship between economic variables and concentration of physicians, Bach29 found that the supply of physicians was more strongly associated in areas with the proportion of black and Hispanic population than with income. In addition, because the non-white population is generally poorer27, it is possible that this variable partially expresses the level of poverty of the county.
The major strength of this study is probably its naturalistic approach, which aimed at building an exhaustive observational cohort study that enhanced external validity. Other strengths are the duration of the follow-up period (22 years) and the use of both logistic and tree-based regression analyses, which allow a comprehensive understanding of CAPCP long-term migration, and the factors associated with migration at both personal and the county levels. One of the disadvantages of the logistic regression approach is that some variables may exert their effect on the whole population while others may be relevant only in specific subgroups (global and local effects). This drawback was overcome using a more systemic approach, the tree-based analysis, which summarizes information by dividing the population into several homogeneous subgroups which are also distinct with respect to the parameters they predict. The subgroups are identified by a tree-structured figure of binary value on the predictors. Tree-growing techniques are particularly suited to handling a large number of variables and to investigating the interactions between the variables. They can also be useful in setting thresholds for predictive variables. To our knowledge, no previously published study has used tree-based analysis to refine predictive logistic models of physicians' migration pattern. In fact, not only do the results present significant factors relating to migrant status, but they also show the interaction between such factors, as well as their splitting thresholds.
The present study has some limitations. It was hypothesized that physicians who were in the same county in 1981 and 2003 did not move between these years, and we defined them as non-migrant physicians. This is not necessarily so, although it is possible that a small part of the total primary physician workforce will leave a county and return to practicing in to the same county 22 years later. In addition, some potential predictors were used relating to the county of origin in 1981, representing the satisfaction/dissatisfaction factor involved in the migration process. It is acknowledged that the attraction factors of the county of destination were not part of our analysis and that this would represent a new dimension to include in a future analysis on physician migration. Predictors relating to the county of origin in 1981 may be a limitation, considering the fact that a county's characteristics (such as the percent non-whites and average income) may have changed between 1981 and the actual year where migration occurred. In addition, using secondary data analysis presents some threats to the internal validity of the results; however, the nature of the professional and census database, which was used to build the cohort and their previous utilizations in other observational studies, limit this possibility. This study also presents some limitations to transposition of its conclusion to countries other than the USA. However, it underscores the importance of performing specific regional analysis in large countries where socio-demographical and geographical heterogeneities can be observed. It also provides methodological improvement in workforce analysis, with the complementary use of tree-based analysis to produce a more systemic picture of the risk of migration in different census regions.
Conclusions
This study looked at the net movement of the CAPCPs across census regions in the USA between 1981 and 2003, and underscores the importance of performing specific regional analysis in large countries where socio-demographical and geographical heterogeneities can be observed. Overall, 13.2 % CAPCPs moved from one region to another in the 22 year period, mostly benefiting the South and West regions. Age was the major determinant factor of migrant CAPCP. Logistic regression and regression tree models also showed that the percent of non-whites within counties is another major determinant. Tree-based analysis produced a more systemic picture of the risk of migration in different census regions. Other studies are needed to assist in understand the complex movement of primary care physician workforce in the USA. For example, studying physicians' migration across large metropolitan areas, small metropolitan areas and counties non-adjacent to metropolitan areas would be of interest. Another important direction would be to study both the satisfaction/dissatisfaction factor and the attraction factor in a tree-based analysis, in order to better understand the relevant sub-population and location involved in the migration of physicians.
Finally, the exploration of physicians' spatial and temporal trajectories represents a challenging methodological approach with potential to provide enlightening results in the quest to understand the evolution of the rural and wider medical workforce.
Acknowledgements
The Office of Rural Health, HRSA, US DHHS (Cooperative agreement number 5 U1CRH03714-03-00), subsidized this project. The Department of Family Medicine, Université de Sherbrooke; the Clinical Research Center, Sherbrooke University Hospital; and the Fonds de Recherche en Santé du Québec also supported the principal investigator.
References
1. Fowkes VK, Campeau P, Wilson SR. The evolution and impact of the national AHEC program over two decades. Academic Medicine 1991; 66: 211-220.
2. Dartmouth Medical School. Center for the Evaluative Clinical Sciences, The Dartmouth Atlas of Health Care 1998. In: JE Wennberg (Ed.). The Dartmouth Atlas of Health Care in the United States. Chicago: American Hospital Publishing, 1998.
3. Goodman DC, Fisher ES, Bubolz TA, Mohr JE, Poage JF, Wennberg JE. Benchmarking the US physician workforce. An alternative to needs-based or demand-based planning. JAMA 1996; 276: 1811-1817. Comments; Erratum: JAMA 1997 277: 277; 966
4. Henderson T, Farmer C, Szwarc S. Practice location of physician graduates: do states function as markets? Washington, DC: National Conference of State Legislatures Institute for Primary Care and Workforce Analysis, 2003; 1-15.
5. Rabinowitz H. Recruitment and retention of rural physicians: how much progress have we made? Journal of the American Board of Family Practice 1995; 8: 496-499.
6. Rabinowitz HK, Paynter NP. The role of the medical school in rural graduate medical education: pipeline or control valve? Journal of Rural Health 2000; 16: 249-253.
7. Pathman DE, Riggins TA. Promoting medical careers in underserved areas through training. Family Medicine 1996; 28: 508-510.
8. Rosenblatt RA, Saunders G, Shreffler J, Pirani MJ, Larson EH, Hart LG. Beyond retention: National Health Service Corps participation and subsequent practice locations of a cohort of rural family physicians. The Journal of the American Board of Family Practice 1996; 9: 23-30.
9. Pathman DE, Konrad TR, Williams ES, Scheckler WE, Linzer M, Douglas J. Physician job satisfaction, dissatisfaction, and turnover. Journal of Family Practice 2002; 51: 593.
10. Pathman DE, Williams ES, Konrad TR. Rural physician satisfaction: its sources and relationship to retention. Journal of Rural Health 1996; 12: 366-377.
11. Landon BE, Reschovsky J, Blumenthal D. Changes in career satisfaction among primary care and specialist physicians, 1997-2001. JAMA 2003; 289: 442-449.
12. Krishnan V. A macro model of change in specialty and spatial distribution of physicians. Socioeconomic Planning Sciences 1992; 26: 111-127.
13. Jiang HJ, Begun JW. Dynamics of change in local physician supply: an ecological perspective. Social Science & Medicine 2002; 54: 1525-1541.
14. Willke RJ. Practice mobility among young physicians. Medical Care 1991; 29: 977-988.
15. Horner RD, Samsa GP, Ricketts TC. Preliminary evidence on retention rates of primary care physicians in rural and urban areas. Medical Care 1993; 31: 640-648.
16. Zhang H, Bracken MB. Tree-based risk factor analysis of preterm delivery and small-for-gestational-age birth. American Journal of Epidemiology 1995; 141: 70-78.
17. Zhang H, Bracken MB. Tree-based, two-stage risk factor analysis for spontaneous abortion. American Journal of Epidemiology 1996; 144: 989-996.
18. Zhang H, Holford T, Bracken MB. A tree-based method of analysis for prospective studies. Statistics in Medicine 1996; 15: 37-49.
19. West PA, Norris TE, Gore EJ, Baldwin LM, Hart LG. The geographic and temporal patterns of residency-trained family physicians: University of Washington Family Practice Residency Network. The Journal of the American Board of Family Practice 1996; 9: 100-108.
20. Li H. Physician migration in non-metropolitan counties of the United States from 1887 to 1990. Chapel Hill: Department of Health Policy and Administration, University of North Carolina at Chapel Hill, 1995; 182.
21. Perry MJ. Domestic Net Migration in the United States: 2000 to 2004. In: MJ Perry (Ed.). Current Population Reports. Washington: US Census Bureau, 2006; 16.
22. Seifer SD, Vranizan K, Grumbach K. Graduate medical education and physician practice location: implications for physician workforce policy. JAMA 1995; 274: 685-691.
23. Basu K, Rajbhandary S. Interprovincial migration of physicians in Canada: what are the determinants? Health Policy 2006, 76: 186-193.
24. Komaromy M, Grumbach K, Drake M, Vranizan K, Lurie N, Keane D et al. The role of Black and Hispanic physicians in providing health care for underserved populations. The New England Journal of Medicine 1996; 334: 1305-1310.
25. Carpenter BE, Neun SP. An analysis of the location decision of young primary care physicians. Atlantic Economic Journal 1999; 27: 135-149.
26. Benarroch M, Grant H. The interprovincial migration of Canadian physicians: does income matter? Applied Economics 2004; 36: 2335-2345.
27. Freed GL, Nahra TA, Wheeler JRC. Relation of per capita income and gross domestic product to the supply and distribution of pediatricians in the United States. The Journal of Pediatrics 2004; 144: 723-728.
28. Chang RKR, Halfon N. Geographic Distribution of Pediatricians in the United States: An Analysis of the Fifty States and Washington, DC. Pediatrics 1997; 100(2): 172-179.
29. Bach P, Pham H, Schrag D, Tate RC, Hargraves JL. Primary care physicians who treat Blacks and Whites. The New England Journal of Medicine 2004; 351: 575-584.





