Introduction
Despite declining mortality rates for the last four decades, cardiovascular disease remains the foremost cause of death in wealthy countries. Once considered primarily a disease of affluence, cardiovascular disease is of increasing global concern as disease risk factors such as overweight/obesity and smoking become more common in low- and middle-income countries1. Within countries as diverse as the USA2 and Australia3, cardiovascular disease prevalence also shows a gradient along the urban-rural continuum, with rural areas having higher disease rates.
Coronary heart disease (CHD) accounts for the majority of cardiovascular disease deaths, predominantly through its devastating end result, myocardial infarction (MI)4. Heart failure (HF), a complex medical syndrome in which the heart fails to pump sufficient blood to meet the body's needs, can be caused by a variety of cardiovascular abnormities. Because it is primarily a disease of the elderly, and because people who survive MI are at risk to develop HF5, the number of hospitalizations for HF has grown steadily in wealthy counties as the population has aged and treatment of MI has improved4.
Heart failure and CHD share important risk factors including hypertension, obesity, smoking, and diabetes mellitus. Indeed, having CHD is itself a risk factor for developing HF4,5. Consequently, we might expect that CHD and HF would have similar geographic distributions of relative prevalence. However, additional factors such as access to ambulatory care and patient or provider behavior may play a role in determining hospitalization rates6.
Access to ambulatory care and patient/provider behaviors may impact HF and MI hospitalizations differently. Heart failure is an ambulatory care sensitive condition, defined as a condition for which hospitalization rates can be reduced by timely and high quality ambulatory care7. By contrast, MI is often used as a marker condition - a diagnosis that all medical practitioners agree requires hospitalization without delay and for which ambulatory care is unlikely to greatly reduce hospitalization rates8. However, it is also known that some patients, particularly those living in rural areas, do delay in seeking health care, even when they are experiencing symptoms of MI9. Thus, a low hospitalization rate at the town level may be an indicator of good general health or an indicator that the town's residents are not seeking appropriate hospitalization.
To further understand how living in a rural area and living in an area that is remote from health care impacts on health and health behavior we constructed a geographic information system (GIS) to study the factors that impact HF and MI hospitalization rates at town level in the state of Maine, USA. Our results may be of interest to those who provide health care in rural areas remote from health services, whether they work in wealthy counties that currently have a high prevalence of heart diseases, or in less affluent countries whose populations are now experiencing increasing risk for these conditions.
Methods
Data sources
The data sources included the following:
- digital Maine map layers obtained from Maine Office of GIS10
- census blocks, towns, primary care analysis areas (PCAA), and counties
- hospital locations
- census blocks, towns, primary care analysis areas (PCAA), and counties
- 2000 Census tables at the census block level for Maine obtained from Maine Office of GIS10
- socioeconomic status variables at the town level for Maine
- unemployment rate, poverty rate, and family income obtained from the Maine State Planning Office11
- educational attainment obtained from 2000 census long-form12
- unemployment rate, poverty rate, and family income obtained from the Maine State Planning Office11
- CHD prevalence at the county level for Maine determined from Centers for Disease Control and Prevention Behavioral Risk Factor Surveillance System (BRFSS) survey tables that we obtained from Maine Office of Health Data and Program Management13
- number of primary care physicians at PCAA level for Maine obtained from Maine Office of Rural Health and Primary Care14
- number of hospitalizations for HF and MI by patients' town of residence for all Maine hospitals, determined from restricted hospital discharge inpatient datasets that we obtained from the Maine Health Data Organization15
- rurality codes at the PCAA level for Maine determined with the use of zipcode approximation files and available from the WWAMI Research Center at the University of Washington16.
Generation of variables
The dependent variables in this study are the average, yearly, age-corrected hospitalization rates for MI and HF for 1998-2002 for each town in Maine. International Classification of Disease, 9th revision (ICD-9) codes of 410.x at the time of discharge were used to identify MI hospitalization and ICD-9 codes of 428.x at the time of discharge were used to identify HF hospitalization. These rates, which included people who died in hospital, were aggregated by town of residence, and normalized to the population of that town. We chose this 5 year period because it is distributed across the year 2000 - the most recent census year from which we drew population numbers for the normalization. Thus, any consistent population change trend would tend to average out over this period. Hospitalization files for the state of Maine are arranged by date of discharge from, rather than date of admission to the hospital. We use the term 'hospitalization' here to indicate cases in which a person was discharged from an acute care hospital in the study period.
We queried the inpatient data sets for the 5 year study period to obtain tables of raw hospitalization counts for MI and HF aggregated by town and stratified into the same age categories as the census data. Then, in a GIS environment, we joined these tables and 2000 census data to the map layer of Maine towns. Finally, we performed an age correction using the direct age correction method17. The units of the resultant variables are hospitalizations per 1000 population per year for each town.
Because lower socioeconomic status (SES) is associated with higher risk for heart disease and heart disease deaths18-20 this study includes four independent variables that relate to SES - the fraction of workers unemployed, the fraction of families living in poverty, median family income, and educational attainment. We generated these variables by joining tables with unemployment, poverty, income, and educational attainment values aggregated at the town level to the map layer of Maine towns in the GIS environment. As a measure of educational attainment, we determined the fraction of adults 25 years of age or older who had education beyond high school for each town. We chose this variable to represent educational attainment because high school graduation rates in Maine are uniformly high while college attendance is much more variable in different Maine communities.
Two independent variables in this study relate to access to health care. Working in the GIS environments, we joined the number of full-time equivalent primary care physicians, aggregated on the PCAA level, to the PCAA-level Maine map and normalized the physician count per 1000 people in the population to produce a primary care physician density variable (primary care physicians per 1000 population). Maine has 62 PCAAs, the boundaries of which were assigned by the Maine Office of Rural Health and Primary Care14. We also used the GIS to compute the linear distance from the centroid of each town to the closest hospital. This distance variable may not be directly related to access to primary care because most people do not receive primary care at a hospital. Rather, it addresses the likelihood that a population will travel long distances for health care, particularly if this travel necessitates that they leave their normal activity space21.
The remaining independent variable in this study relates to rurality. To obtain this variable, we joined a table of rural urban commuting area codes at the PCAA level (coded 1-10) to the PCAA-level map in the GIS environment.
Data analysis
We assigned values for independent and dependent variables to each town within the GIS and output the resultant table into a spreadsheet. For independent variables aggregated at units of area larger than a town (eg PCAA), each town was assigned the variable value for the larger unit of area in which it was located.
Of the 663 Maine towns with population at the time of the 2000 census, 486 had a complete set of independent variables. After checking variables for distribution normality, univariable linear regression analysis and multiple linear regression analysis were conducted for these towns to determine which of the independent variables predicted either of the two dependent variables. Pearson correlation coefficients were used to examine correlations among independent variables and significant interactions were tested for among the independent variables. A p-value of < 0.05 was considered significant. Variable values are reported as mean ± SD unless otherwise noted.
The 177 towns that were eliminated from the analysis due to missing values were predominantly sparsely populated. They represented almost 20% of Maine's land area, but less than 1% of Maine's population. To gain an understanding of the characteristics of these towns, a comparison was performed of the included with the eliminated towns for MI and HF hospitalization rates, rurality, physician density, and distance from the closest hospital (the variables for which data was available for all 663 towns) using a Mann-Whitney test.
This protocol was approved by MHDO and the USM Institutional Review board.
Results
Descriptive statistics - towns included in predictive analysis
During the 5 year study period there were 24 452 hospitalizations of Maine residents to Maine hospitals for MI and 20 330 for HF. Hospitalizations of non-Maine residents to Maine hospitals were excluded from this study and hospitalizations of Maine residents to hospitals outside the state were not captured in the available datasets. Age corrected hospitalization rates at the town level ranged from 0 to 14.71/year/1000 population (mean = 3.65 ± 2.46) for MI, and from 0 to 28.77/year/1000 population (mean = 2.74 ± 2.20) for HF. The spatial distribution of age-adjusted hospitalization rates for MI and HF is shown (Figs1,2). The descriptive statistics for the independent variables are also shown (Table 1).
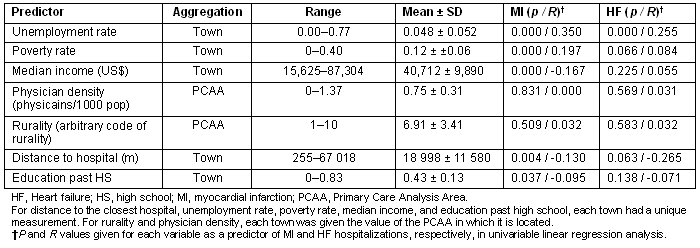
Table 1: Independent variables descriptive statistics and univariable regression for the 486 towns included in the predictive analysis
Predictors of MI and HF hospitalizations
In univariable linear regression analysis the following variables were significant (p < 0.05) predictors of higher MI hospitalization rate: higher poverty rate, lower median family income, higher unemployment rate, less distance from place of residence to the closest hospital, and lower educational attainment. The only significant univariable predictor of higher HF hospitalization rates was higher unemployment rate. There are trends toward high poverty rate and distance from place of residence to the closest hospital as univariable predictors of high HF hospitalization rates (Table 1).
Results of the multiple linear regression analysis of predictors of MI and HF hospitalization rates are shown (Table 2). At the p <0.05 level of significance, high MI hospitalization rates are predicted for towns that have a higher unemployment rate, a higher poverty rate, and are closer to a hospital. High hospitalization rates for HF are predicted (p <0.05) for towns that have a higher unemployment rate and are closer to a hospital. A model that includes just these significant independent variables explains 19.1% of the variability in MI hospitalization rates and 8.4% of the variability in HF hospitalization. As would be expected for variables related to rurality and socioeconomic status, the significant independent variables in this study all correlate significantly with each other. These variables also interact significantly to predict the dependent variables. A model that included the significant independent variables and the interactions between them explains 23.1% of the variability in MI hospitalization rates and 9.2% of the variability in HF hospitalization rates suggesting that the factors that contribute to hospitalization rates for these two forms of heart disease in Maine are varied and complex. To provide a cartographic representation of the relationship between MI and HF hospitalization rates versus the distance of each town from the closest hospital (a significant predictor of both MI and HF hospitalization rates in multiple regression analysis) the locations of Maine's hospitals have been added to Figures 1 and 2.
Table 2: Myocardial infarction and heart failure hospitalization rates - multiple linear regression
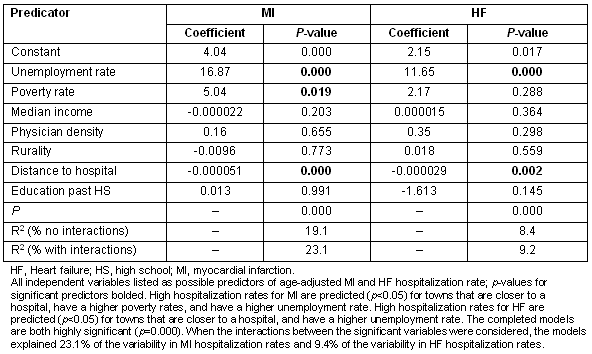
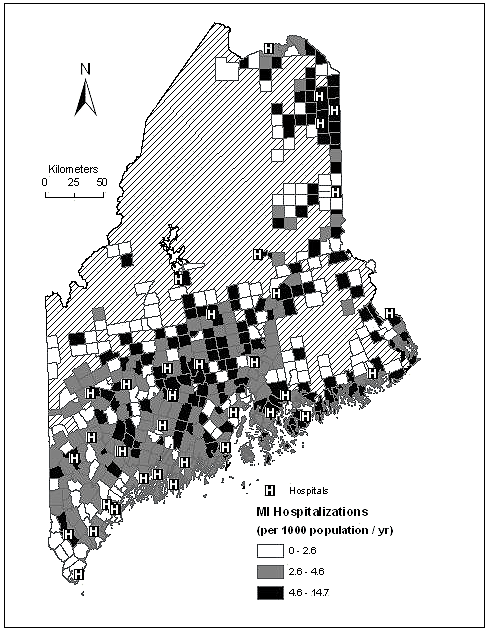
Figure 1: Map of the state of Maine showing the age-adjusted hospitalization rates for myocardial infarction from 1998 to 2002 displayed as hospitalizations/1000 population/year by town and symbolized by quantiles. Areas excluded from the analysis (due to zero population or an incomplete set of independent variables) are shown cross-hatched and without town boundaries. The locations of the acute care hospitals are marked 'H'.
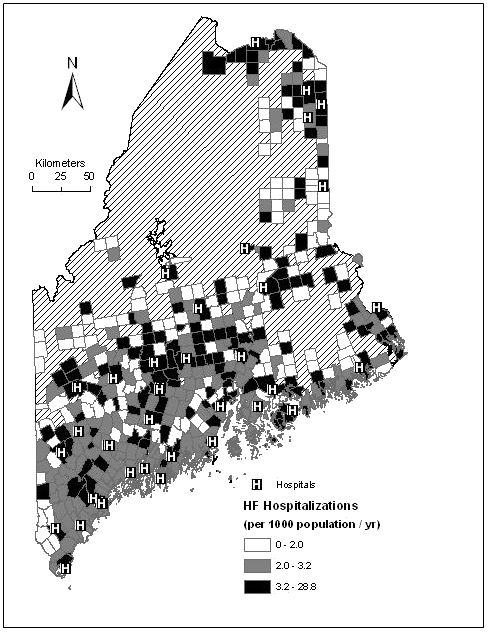
Figure 2: Map of the state of Maine showing the age-adjusted hospitalization rates for heart failure from 1998 to 2002 displayed as hospitalizations/1000 population/year by town and symbolized by quantiles. Areas excluded from the analysis (due to zero population or an incomplete set of independent variables) are shown cross-hatched and without town boundaries. The locations of the acute care hospitals are marked 'H'.
Towns eliminated from predictive analysis
Although Maine does have several population centers, mostly in the southern one-third of the state, much of its area is quite rural and parts of the state are remote from any population center, particularly in the winter when travel is difficult. Of Maine's 83 703 km2 of land area, the 663 towns that were populated at the 2000 census made up 60 586 km2 (72%). The 486 towns included in the predictive analysis of this study make up only 44 971 km2 or 54% of Maine's land area. However, the 177 towns that were eliminated from the predictive analysis because they had one or more missing values for independent variables have a total population of only 9509. Thus, 99.25% of Maine's 2000 census population of 1 274 923 is captured in the predictive analysis. When we compared the eliminated with the included towns on the basis of those variables for which full data was available, it was found that the eliminated towns had significantly lower hospitalization rates for both MI (p = 0.000) and HF (p = 0.000), were located further from the closest hospital (p = 0.000), were more rural (p = 0.000), and had fewer primary care physicians (p = 0.002).
Discussion
Socioeconomic status and heart disease
Low SES predicts high cardiovascular disease mortality risk at the individual level22. This impact partially reflects the fact that individuals with low income and less education are more likely to have heart disease risk factors such as hypertension, diabetes, and smoking23,24. However, even after correcting for individual risk factors, people who live in neighborhoods with low SES, as measured by average income and education, have a higher risk for 'coronary events' (eg MI) and heart disease death18-20.
The impacts of income and/or income disparity (indicators or SES) on heart disease mortality seen at the neighborhood level25 are generally observed at the city26 and the county27,28 levels as well in the US, and similar findings have been reported for stroke risk in New Zealand29. These disparities may reflect unequal distribution of health resources, the impact of the community on health-related behaviors (walking and diet for example), or stress-induced health effects (eg the impact of job insecurity)29.
Unemployment shows a pattern of effects on heart disease similar to other measures of SES in that it is both a risk factor for MI and cardiac death at the individual level in Italy30 and a predictor of higher all-cause mortality at the community level across a range of European countries and the US31. Socioeconomic status indicators also have an impact on ambulatory care sensitive hospitalization rates. Higher rates of poverty32 and lower average income33 in communities are associated with higher rates of hospitalization for ambulatory care sensitive conditions in the US and in Canada34.
In this study, high unemployment rate was a predictor of high hospitalization rate for both MI and HF while high poverty rate also predicted high MI hospitalization rate (Table 2). Thus, these results are in agreement with previous work showing that low SES negatively impacts health and probably reflect a community effect.
Rurality and access to healthcare
Living in a rural community is generally associated with a lower consumption of healthcare35, poorer health2, and an increased rate of ambulatory care sensitive hospitalizations6 in countries as different as the USA and Australia3,36. However, no significant relationship was found in the present study between rurality and hospitalization rates for either MI or HF in multiple regression analysis. This is striking because a positive, although not significant, correlation was found between the fraction of people in Maine who answer in the affirmative when asked by BRFSS questioners if they have ever been told that they have heart disease, and the rurality code of their county of residence (data not shown). This suggests that the prevalence of heart disease is at least as high, if not higher, in rural Maine communities as in non-rural areas.
The link between rurality and poor health is almost certainly multi-facetted6, but a simple lack of health providers may play a role by limiting access to health care37,38. However, the relationship between ambulatory care sensitive hospitalization rate and physician supply is often difficult to demonstrate32,33, particularly in rural areas39, and may not be monotonic36,40. That is, hospitalization rates may be high both in areas where physician supply is very low and where it is very high.
Our inability to demonstrate a correlation between rurality code and hospitalization rates for MI or HF shows that, in this instance, the rurality code did not add predictive value to a model that contained multiple more specific measures of SES and access to health care. Our inability to demonstrate a correlation between physician density and the hospitalization rates for either HF or MI may suggest that primary care physician density in Maine is high enough so that it does not present a barrier to ambulatory care access. However if it is true in Maine, as elsewhere, that people who live in rural areas tend to be less healthy, then our results may also suggest that rural Mainers may be less likely than those who live in more urban areas to seek health care or to be hospitalized appropriately. This conclusion is in general agreement with the finding that rural Australians delay in seeking healthcare for MI symptoms9 and evidence from rural southwest Virginia, US showing that people feel that they should 'make do' or 'suffer it out' when they are sick, rather than seeking healthcare41. In rural Maine, the phase 'tough it out' is used to refer to similar ideas.
Distance from the hospital
Because hospitals are often situated in population centers, rural communities tend to be further from hospitals in Maine (data not shown), and elsewhere. However, distance from a hospital impacts ambulatory care sensitive hospitalization rates in a manner that is opposite that of rurality. People who live further from the locations of healthcare delivery have fewer regular checkups42, which should result in them being less healthy, but they are still less likely to be hospitalized for ambulatory care sensitive conditions, at least in rural USA32. This may reflect the reluctance of primary care physicians to admit patients to distant hospitals among other factors.
For a condition such as MI for which hospitalization is mandatory, one might expect little or no effect of distance of residence from the hospital on hospitalization rate43. One might even propose that emergency room physicians would be more likely to admit a person who lived further from the hospital when they presented with equivocal but possibly cardiac symptoms, out of concern that sending the patient home would pose too great a risk. This sort of concern may indeed impact admitting practices, as evidenced by findings from Italy showing that people who live further from hospitals are more likely to be hospitalized inappropriately44. However, contrary to these expectations, greater travel time to the hospital is associated with lower rather than higher admission rates for ischemic heart disease (including MI) in England43.
In this study, greater distance between town of residence and the closest hospital predicted lower hospitalization rates for both HF (an ambulatory care sensitive condition) and MI (a condition for which hospitalization is mandatory) in the multiple regression analysis (Table 2). Inappropriate hospitalization probably has little impact on our results, at least for MI, because the data set analyzed was based on diagnosis at the time of discharge, not at admission. Thus, patients admitted with possible MI symptoms that were subsequently determined to be non-cardiac in origin would not appear in this study. Our striking finding of a negative relationship between distance to a hospital and hospitalization rate suggests that the patients themselves are not presenting for care that they suspect will include hospitalization.
To explain such behavior, it is useful to evoke the concept of 'experience of place' that describes distance as a socially constructed phenomenon that has different meanings for different people21. In relation to health care, this may mean that people are reluctant to utilize healthcare that is located outside their normal activity space, the area in which they travel to work, recreate, and perform other life tasks. This idea is supported by evidence that, for elderly residents of rural areas of Vermont in the US, the number of physician visits is predicted by whether or not the physician's office is in the patient's normal activity space - not by distance to the office21. In contrast, for adults in rural areas of North Carolina in the USA, a smaller number of primary care providers in an individual's normal activity space was associated with fewer acute care visits but not chronic care visits or regular check-ups; while people who lived closer to their primary care provider were more likely to have regular checkups without consideration of normal activity space42.
One possible reason for differences between the North Carolina and Vermont findings is that the Vermont study focused on older (> 65 years of age) people with incomes < $50,000 per year21, while the North Carolina study included all adults over the age of 18 years and had no income criteria42. The findings from rural North Carolina and rural Vermont may not be as different as they initially appear, however. In Vermont, researchers used the number of primary care physician visits as the dependent variable without regard for whether these visits were for regular checkups, acute conditions, or chronic conditions21 - and given the elderly patient population in this study, many visits for regular checkups undoubtedly included elements of chronic disease management as well. By contrast, the North Carolina workers elicited the reason for the physician visits in their questionnaire, and were thus able to distinguish among visits for acute conditions, chronic conditions, and regular checkups42. Thus, both studies reinforce the point that geographic barriers may impact healthcare utilization.
Clearly, healthcare seeking behavior is influenced by geography in complex ways. There is also evidence from rural western Maine, US that it is not uncommon for people to travel outside their self-reported 'reasonable travel limit' to receive general medical care45. However, regardless of whether location outside of an individual's normal activity space or distance alone is the deterrent to seeking healthcare, this behavior may have important consequences. Given the risk of cardiac arrest from arrhythmia during an MI, an event that may be treated effectively in hospital but will almost certainly result in fatality if it occurs at home, it is vital that individuals experiencing MI be hospitalized without delay. Thus, as previously suggested for rural residents of Australia9, the findings presented here suggest that patient education about the importance of a person experiencing MI symptoms accessing the healthcare system, be directed in particular to rural residents who live at greater distances from hospitals.
Study limitations
This study has several limitations. First, there are two independent variables (physician density and rurality) that were aggregated at the level of the PCAA. Because there are 62 PCAAs in Maine, and because people readily travel to neighboring towns to visit a physician, this may not be a large a limitation for physician density. However, it does point to variables for which greater resolution of area (eg variables aggregated to smaller geographic units) might alter our conclusions.
The fact that the total predictive power of our models was low shows that many other individual and community attributes contribute to the rate of hospitalization of the town's residents for MI and HF. Some previous studies have shown much higher power for SES and access to health care as predictors of ambulatory care sensitive hospitalization rates8,36. However, these studies were conducted in more homogeneous urban settings. There is also interesting evidence that the ability of models based on community variables to predict hospitalization rates is higher in urban, compared with rural areas32 and that the predictive ability of these models is greater for younger compared with older people33. Much of Maine is rural and both MI and HF preferentially strike older people.
Finally, hospitalizations of Maine residents to facilities outside of the state (eg in Canada, New Hampshire, and Massachusetts) were not captured in the present data set. This might preferentially impact areas of the state near these borders.
Conclusion
In conclusion, in multivariable analysis we have found that:
- higher unemployment rates predicted higher hospitalization rates for both MI and HF
- higher poverty rate predicted higher hospitalization rates for MI
- neither rurality nor physician density significantly predicted hospitalization rates for MI or HF
- hospitalization rates for both MI and HF fell as the distance between the town of residence and the closest hospital increased.
The findings about poverty and unemployment demonstrate that the well known impact of low SES on health is operating in Maine, as elsewhere. The negative relationship between distance to the closest and hospitalization rates probably reflects patient and/or provider behavior. This suggests that healthcare systems that serve communities at a greater distance from hospitals may benefit from patient education addressing the importance of seeking immediate hospitalization for MI, and also from particularly close scrutiny of physician admitting patterns.
Acknowledgements
The authors thank the personnel from the Maine Health Data Organization for help with the process of application to use Maine inpatient hospitalization data; personnel from the Maine Office of Health Data and Program Management for their help in obtaining BRFSS data sets; and personnel from the Maine Office of Rural Health and Primary Care for supplying information about physician density aggregated by PCAA. Also thanked are Andrea Small and Rosemary Mosher for technical suggestions about data analysis techniques.
References
1. Ezzati M, Hoorn SV, Lawes CMM, Leach R, James WPT, Lopez AD et al. Rethinking the 'diseases of affluence' paradigm: Global patterns of nutritional risks in relation to economic development. PLOS Medicine 2005; 2(5): 404-411.
2. Weeks WB, Wallace AE, Wang S, Lee A, Kazis LE. Rural-urban disparities in health-related quality of life within disease categories of veterans. Journal of Rural Health 2006; 22(3): 204-211.
3. Clark RA, McLenna S, Eckert K, Dawson A, Wilkinson D, Stewart S. Chronic heart failure beyond city limits. Rural and Remote Health 5: 443. (Online) 2005. Available: http://www.rrh.org.au (Accessed 18 January 2008).
4. American Heart Association Statistics Committee. Heart disease and stroke statistics - 2007 update. (Online) 2007. Available at: http://www.americanheart.org/presenter.jhtml?identifier%012007 (Accessed 24 June 2008).
5. ACC/AHA Task Force on Practice Guidelines. ACC/AHA 2005 guideline update for the diagnosis and management of chronic heart failure in the adult. Circulation 2005; 112: 1853-1887.
6. Silver MP, Babitz ME, Magill MK. Ambulatory care sensitive hospitalization rates in the aged Medicare population in Utah, 1990 to 1994: a rural-urban comparison. Journal Rural Health 1997; 13(4): 285-294.
7. Sanderson C, Dixon J. Conditions for which onset of hospital admission is potentially preventable by timely and effective ambulatory care. Journal of Health Services Research and Policy 2000; 5(4): 222-230.
8. Billings J, Zeitel L, Lukomnik J, Carey TS, Blank AE, Newman L. Impact of socioeconomic status on hospital use in New York City. Health Affairs 1993; Spring:162-173.
9. Finn JC, Nick Bett JH, Shilton TR, Cunningham C, Thompson PL. Patient delay in responding to symptoms of a possible heart attack: can we reduce time to care? Medical Journal of Australia 2007; 187(5): 293-298.
10. Maine Office of GIS. GIS Data Catalog. (Online) 2007. Available: http://megis.maine.gov/catalog/ (Accessed 15 February 2007).
11. Maine State Planning Office. Maine Planning Office. (Online) 2007. Available: http://www.maine.gov/spo/index.shtml (Accessed 23 June 2007).
12. US Census Bureau. Census Atlas of the United States. (Online) 2007. Available: http://www.census.gov/ (Accessed 15 February 2007).
13. Office of Health Data and Program Management. Behavioral Risk Factor Surveillance System. (Online) 2007. Available: http://www.maine.gov/dhhs/bohodr/brfss.htm (Accessed 15 February 2007).
14. Maine Office of Rural Health and Primary Care. Office of Rural Health and Primary Care. (Online) 2007. Available: http://www.maine.gov/dhhs/boh/orhpc/ (Accessed 15 February 2007).
15. Maine Health Data Organization. Maine Health Data Organization . (Online) 2007. Available: http://mhdo.maine.gov/imhdo/ (Accessed 15 February 2007).
16. Hart LG. Rural urban commuting areas, version 2.0. WWAMI Rural Health Research Center. (Online) 2006. Available: http://depts.washington.edu/uwruca/ (Accessed 15 February 2007).
17. Buescher PA. Age-adjusted death rates. (Online) 1998. Available at: http://www.schs.state.nc.us/SCHS/pdf/primer13.pdf (Accessed 15 February 2007).
18. Diez Roux AV, Merkin SS, Arnett D, Chambless L, Massing M, Neito FJ et al. Neighborhood of residence and incidence of coronary heart disease. New England Journal of Medicine2001; 345(2): 99-106.
19. Borrell LA, Diez Roux AV, Rose K, Catellier D, Clark BL. Neighborhood characteristics and mortality in the arthrosclerosis risk in communities study. International Journal of Epidemiology 2004; 33: 398-407.
20. Diez Roux AV, Borrell LN, Hann M, Jackson SA, Schultz R. Neighborhood environments and mortality in an elderly cohort: results from the cardiovascular health study. Journal of Epidemiology and Community Health 2004; 58: 917-923.
21. Nemet GF, Bailey AJ. Distance and health care utilization among the rural elderly. Social Science & Medicine 2000; 50: 1197-1208.
22. Kaplan GA, Keil JE. Socioeconomic factors and cardiovascular disease: a review of the literature. Circulation 1993; 88: 1973-1998.
23. Alter DA, Iron K, Austin, PC, Naylor, CD. Influence of education and income on atherogenic risk factors profiles among patients hospitalized with acute myocardial infarction. Canadian Journal of Cardiology 2004; 20(12): 1229-1228.
24. Banks J, Marot M, Oldfield Z, Smith JP. Disease and disadvantage in the United States and in England. JAMA 2006; 295(17): 2037-2045.
25. Cohen DA, Farley TA, Mason K. Why is poverty unhealthy? Social and physical mediators. Social Science & Medicine 2003; 57: 1631-1641.
26. Cooper RS. Social inequality, ethnicity and cardiovascular disease. International Journal of Epidemiology 2001; 30: S48-S52.
27. Massing MW, Roseamond WD, Wing SB, Suchindran CM, Kaplan BH, Tyroler HA. Income, income inequality, and cardiovascular disease mortality: relations among county populations of the United States, 1985 to 1994. Southern Medical Journal 2004; 97(5): 475-484.
28. Shi L, Macinko J, Starfield B, Politzer R, Wulu J, Xu J. Primary care, social inequalities, and all-cause, heart disease, and cancer mortality in US counties. American Journal of Public Health 2005; 95(4): 674-680.
29. Brown P, Guy M, Broad J. Individual socio-economic status, community socio-economic status and stroke in new Zealand: A case control study. Social Science & Medicine 2005; 61: 1174-1188.
30. Petrelli A, Ganvi R, Marinacci C, Costa G. Socioeconomic inequalities in coronary heart disease in Italy: a multilevel population-based study. Social Science & Medicine 2006; 63: 446-456.
31. van Lenthe FJ, Borrell LN, Diez Roux AV, Kauppinen TM, Marinacci C, Martikainen P et al. Neighborhood unemployment and all cause mortality: a comparison of six countries. Journal of Epidemiology and Community Health 2005; 59: 231-237.
32. Schreiber S, Zielinski T. The meaning of ambulatory care sensitive admissions: urban and rural perspectives. Journal of Rural Health 1997; 13(4): 276-284.
33. Ricketts TC, Randolph R, Howard HA, Pathman D, Carey T. Hospitalization rates as indicators or access to primary care. Health & Place 2001; 7: 27-38.
34. Roos LL, Walld R, Uhanava J, Bond R. Physician visits, hospitalizations, and socioeconomic status: ambulatory care sensitive conditions in a Canadian setting. Health Services Research 2005; 40(4): 1167-1185.
35. Chan L, Hart G, Goodman DC. Geographic access to health care for rural Medicare beneficiaries. Journal of Rural Health 2006; 22(2): 140-146.
36. Ansair X, Laditka JN, Laditka SB. Access to heath care and hospitalization for ambulatory care sensitive conditions. Medical Care Research and Review 2006; 63(6): 719-743.
37. Shi L, Macinko J, Starfield B, Politzer R, Wulu J, Xu J. Primary care, social inequalities and all-cause, heart disease, and cancer mortality in US counties: a comparison between urban and non-urban areas. Public Health 2005; 119: 699-710.
38. Zhang W, Mueller KJ, Chen L, Conway K. The role of rural health clinics in hospitalization due to ambulatory care sensitive conditions: a study in Nebraska. Journal of Rural Health 2006; 22(3): 220-223.
39. Laditka JN, Laditka SB, Probst JC. More may be better: evidence of a negative relationship between physician supply and hospitalization for ambulatory care sensitive conditions. Health Services Research 2005; 40(4): 1148-1166.
40. Laditka, JN. Physician supply, physician diversity, and outcomes of primary health care for older persons in the United States. Health & Place 2004; 10: 231-244.
41. Huttlinger K, Schaller-Ayers J, Lawson T, Ayers J. Suffering it out: Meeting the needs of healthcare delivery in a rural area. Online Journal of Rural Nursing and Health Care 2003; 3(2): 17-28.
42. Arcury TA, Gesler WM, Preisser JS, Sherman J, Spencer J, Perin J. The effects of geography and spatial behavior on health care utilization among residents of a rural region. Health Services Research 2005; 40(1): 135-155.
43. Twigger JP, Jessop EG. Small area variation in hospital admission: random or systematic? Public Health 2000; 114: 328-329.
44. Angelillo IF, Ricciardi G, Nante, N, Boccia, A. Appropriateness of hospital utilization in Italy. Public Health 2000; 114: 9-14.
45. Shannnon G, Lovett J, Bashshur R. Travel for primary care: expectations and performance in a rural setting. Journal of Community Health 1979; 5(2): 113-125.

