full article:
The sustainable provision of health professionals to rural and remote regions of Australia has been an ongoing challenge1,2. While the literature on the rural and remote health workforce has focused heavily on the medical profession and, to a lesser extent, nurses, there is data to show that recruitment and retention of allied health professionals (AHPs) is also a concern3. There is a national shortage of AHPs with a mal-distribution between metropolitan centres and rural and remote communities such that access to the range of core clinical allied health services reduces significantly with increasing remoteness4. In 2005, the estimated average number of AHPs in major metropolitan areas was 2.66 per 10 000 population compared to 0.60 per 10 000 population in very remote areas, and 1.81 per 10 000 population in inner regional areas5. More recent data suggests that the ratio of allied health to population may be significantly less than this, at least in some regions of Australia6.
A considerable body of literature has accumulated investigating factors associated with recruitment and retention of health professionals. A recent WHO literature review described the factors in four categories: education interventions, regulatory interventions, financial incentives, and professional and personal support interventions7.
In Australia, governments and health services, sometimes in collaboration with university allied health departments and/or allied health organisations, have developed a raft of strategies to address the geographical mal-distribution of the AHP workforce. However there is a paucity of robustly designed studies to assess the impact of recruitment and retention interventions on the rural and remote allied health workforce. One strategy that lacks evidence is the provision of scholarships and other financial incentives. Bärnighausen and Bloom undertook a systematic review of studies published on the impact of financial incentives on recruitment and retention to rural practice8. The review included incentives for AHPs as well as nursing and medical students and found weak evidence for the effectiveness of financial incentives regarding recruitment and retention but did not identify a causal relationship. Importantly, most programs had substantial drop-out rates before the start of the service obligation period. There is a need to further assess the effectiveness of scholarships and other financial incentives in the Australian context.
The Queensland Health Rural Scholarship Scheme (Allied Health) (QHRSS-AH) has been offered since 1996 to students in physiotherapy, occupational therapy, speech pathology, social work, podiatry, psychology, pharmacy, radiography, sonography, and nutrition and dietetics. Scholarships are advertised on the Queensland Health website, through universities and rural student clubs. Applicants are short-listed and interviewed with at least one panel member being a senior rural or remote allied health practitioner or manager. Between 2000 and 2010 an average of 13 scholarships per year were awarded. Successful scholarship holders are provided with financial assistance in the final 2 years of university studies in their allied health profession ($21 000 per year). A two-year bonded service period is undertaken in a Queensland public health service that has a vacant position appropriate for a graduate coinciding with the scholarship holder's graduation. Rural or remote services are preferenced for placement by the organisation; where no appropriate vacant position is available, regional or metropolitan services may employ the scholarship holder. Program rules require repayment of scholarship funds if the service period is not completed.
In 2010, the Anton Breinl Centre for Public Health and Tropical Medicine at James Cook University was engaged by the Allied Health Workforce Advice and Coordination Unit (AHWACU) to conduct a review of Queensland Health Allied Health Pre-Entry Scholarship Programs. This project included a review of the QHRSS-AH including impacts on those engaged with the scholarship program and for the funding organisation. Specifically this part of the project aimed to examine the profile of the QHRSS-AH recipients from 2000 to 2010 including graduate recruitment outcomes and retention within the scholarship program. It also aimed to explore the influence of the QHRSS-AH on early career practice location decisions and the features of the scheme that influenced motivation to be involved as either a scholarship holder or manager, perceived barriers to employment of scholarship holders in rural or remote services, experiences of scholarship holders as new graduates in rural and remote services and views on support requirements.
Design
A mixed methods study was conducted consisting of a quantitative descriptive analysis of scholarship data and a qualitative exploratory descriptive study that collected in-depth information from scholarship holders and their managers.
Participants and sampling
A purposive criterion based sampling technique was used for the qualitative study where participants were intentionally selected for their knowledge and experience of the issue being explored9. Participants in the qualitative study were current Queensland Health employees who had been awarded a QHRSS-AH scholarship between 2000 and 2008 (including those completing their bonded service period) or managers or professional leaders of scholarship holders (from here on referred to as managers). Scholarship holders and managers were potentially employed in any of 15 Queensland Health Districts.
Scholarship holders: All scholarship holders who had commenced their service period and who appeared in Queensland Health payroll records at the time of the study were provided with an invitation to participate and information on the study by an AHWACU employee. If interested in participating, individuals were instructed to contact a member of the research team to arrange a mutually suitable time to be interviewed.
Managers of rural allied health scholarship holders: Managers were identified by AHWACU if they were in an allied health leadership role responsible for a rural or remote workforce (the target of the QHRSS-AH). This included services that commonly took scholarship holders and those that rarely did. Fifteen managers were identified and contacted by AHWACU. The process of information provision and contact was as per the scholarship holder group previously described.
Data collection
Quantitative data were compiled by AHWACU from scholarship program records and payroll data. They included scholarships awarded by year, demographic details of scholarship holders (age, gender, profession), scholarship holder status at October 2010 in relation to the stages of the QHRSS-AH, and location of employment in Queensland Health at graduation.
Qualitative data consisted of semi-structured, in-depth telephone interviews. Individuals consenting to participate were provided with the interview questions prior to the telephone interview. At the time of the interview demographic data were collected including age, gender, profession, location(s) of childhood home and location of high school completion. Interviews were taped with participants' permission. Each interview took approximately 45 minutes. The interview questions are presented in Table 1.
Table 1: Interview questions for rural allied health scholarship holders and managers

Data analysis
Scholarship data were imported from Microsoft Excel® into a Statistical Package for Social Sciences v18 data set (SPSS Inc.; http://www.ibm.com/software/analytics/spss‎) for descriptive analysis. All data were de-identified upon import.
Interviews were transcribed in note form and interview texts were then organised using QSR NVivo8 (QSR International; http://www.qsrinternational.com). The question areas guided initial organisation of categories. Scholarship holder and manager transcripts were analysed separately. The responses to the questions were read and sorted into main sub-categories, which related to the salient themes relevant to the questions. These were then reclassified into higher level categories of broader themes.
To ensure rigour and trustworthiness the interviews were conducted by two experienced qualitative interviewers with a clear interview plan. As described by Patton10, triangulation was used by applying data source triangulation, assessing the views of both scholarship holders and managers, and researcher triangulation, where two experienced qualitative researchers checked for consistency in identification of themes.
Ethics approval
Participation in the study was completely voluntary. Ethics approval was obtained prior to the commencement of the study from the JCU Human Ethics Subcommittee (H3906) and Queensland Health Human Research Ethics Committee (QTHS138).
Quantitative outcomes
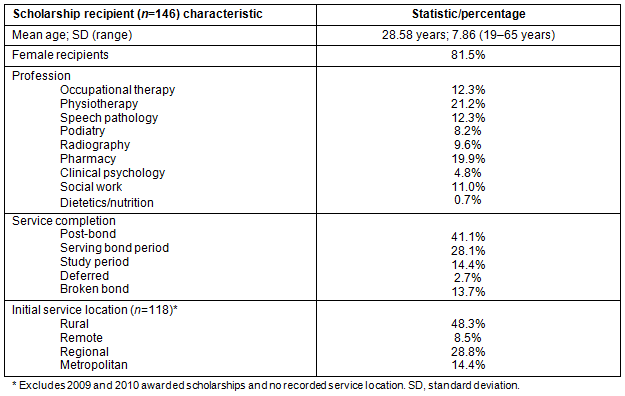
Between 2000 and 2010, 146 QHRSS-AH scholarships had been awarded. The mean age of recipients at intake to the scholarship program was 28.58 ± 7.86 years (range 19-65 years), with 81.5% being female.
Scholarship service status: In October 2010, of the 146 QHRSS-AH recipients since 2000, 41.1% had completed and 28.1% were currently completing the service period (the 2-year term of employment following graduation required in the scholarship agreement). Of the remainder, 14.4% were still completing the 2-year university study period, 2.7% had graduated university but had been approved to defer their service period for up to 1 year and 13.7% had broken service bonds (they had not fulfilled their obligations under the terms of the scholarship agreement and had exited the scholarship program either prior to graduation or before the conclusion of the service period).
Service location of scholarship holders: Of the scholarship holders who had entered their service period, the location of initial service was 48.3% rural, 8.5% remote, 28.8% regional and 14.4% metropolitan. For this study 'rural' and 'remote' were defined consistent with the Queensland Health human resources framework, 'metropolitan' as within 150 km of Brisbane and 'regional' as all other centres11. The scholarship recipient characteristics are presented in Table 2.
Table 2: Scholarship holder characteristics and service details
Qualitative interviews with scholarship holders
Seventeen past or current rural scholarship holders participated in the interviews. The majority (76.5%) of participants were female and their mean age was 30 years (SD ± 13.68.7; range 23-51). Eight different professions were represented including occupational therapy, pharmacy, physiotherapy, podiatry, psychology, radiography, social work and speech pathology. Eleven participants grew up in metropolitan or regional centres and six grew up in a rural area. Twelve participants completed high school in a metropolitan or regional centre and five completed high school in a rural area.
The main themes emerging from the scholarship holder interviews were:
- motivation to apply for scholarship
- influence of scholarship on work location choice
- reasons for leaving rural practice
- strategies to support recruitment and retention relevant to scholarship holders and new graduates.
Motivation to apply for scholarship: The main motivating influences for choosing a rural scholarship program were related to economic reasons, social reasons, work-related reasons and a desire to be in a rural location. Economic motivators were strong for the majority of respondents. Scholarship holders appreciated having financial support as it reduced the pressure of having to work and study at the same time which allowed more time to focus on their studies. Work related motivations included assurance of a position following graduation and desire for variety in their work (including desire for a generalist caseload, desire to work autonomously, quest for adventure or for something different to mainstream practice and life in a larger centre, not wanting to work in a metropolitan centre, and an overall enjoyment of rural life). Some participants felt rural communities needed more health staff and this motivated them to apply for a scholarship. Social influences such as enjoying a rural lifestyle, having a partner working in a rural area, growing up in a rural area, family experiences of rural life and practice and knowing of others who had received scholarships were also motivators. Some participants always intended to work in a rural area and had no interest in metropolitan work.
Was the decision to work rural based solely on being a scholarship holder? Most participants felt rural practice was appealing regardless of receiving a scholarship. Only three (17.6%) indicated they chose rural practice solely because of the scholarship. Other motivations for rural work included having a partner in a rural location, having always wanted to work rurally, being motivated by the professional and personal challenges, seeing rural practice as a viable professional career pathway, having family nearby or wanting to work away from the city or somewhere different.
Reasons for leaving rural practice: Most of those working in the metropolitan area at the time of interview suggested that they would consider taking up a rural position in the future, even though they had made a decision to leave previously. The most common reason for leaving was due to personal relationships and family issues. One participant stated that although she loved her time practising in a rural area she had reached a stage in life where she felt a need to reconnect with family and friends. Only one participant mentioned aspects of practice that might have impacted her decision to remain in a rural location and this included having a better orientation, being provided with more clinical support and mentoring, and having more defined career progression pathways.
Strategies to support recruitment and retention: While several respondents were very positive about the range of supports already being offered by the organisation and the existing recruitment and retention strategies in place, there were suggestions regarding further initiatives to enhance recruitment and retention of scholarship holders and new graduates more generally to rural and remote areas. These suggestions related to:
- living conditions/accommodation
- professional support
- transitional support factors
- the health service's administration context
- miscellaneous recruitment and retention issues.
Access to appropriate and affordable accommodation was important and assistance in finding accommodation was recommended as well as having access to financial support for accommodation and relocation costs.
Professional support was identified by the majority of respondents, particularly opportunities for professional development. While many scholarship holders felt well supported as a new graduate entering rural practice, others identified gaps in relation to their experiences and the support they received. It was suggested that new graduates should spend time in a larger regional centre where they could be exposed to different cases and have a different level of supervision and support before being placed in a rural area. This was seen as particularly important for those placed in more isolated centres. It was also seen as an ideal strategy for graduates to develop networks that would enhance later communication and support when the allied health professional went to their rural placement location. The level of responsibility that was placed on new graduates was an issue for a small number of respondents who expressed a need for greater professional and remunerative recognition for the amount and type of work done in these situations. Some respondents presented the view that the complexity of rural positions resulted in a quicker increase in skill levels, leading to work being conducted at a more advanced level, which should attract remuneration at the level of accountabilities demonstrated.
A comprehensive orientation when starting in new positions was seen as essential, even if the scholarship holder had undertaken the placement in the same location as a student. Participants from some professions described very good processes where they were introduced into the rural communities after spending time in the nearest larger regional centre. This allowed for confidence to be built, relationships with staff developed and the identification of skills that needed developing.
Qualitative interviews with managers
Eleven interviews were conducted with managers (73.5% response rate). All participants were in senior leadership roles that had operational or professional management responsibilities for allied health workforce in their health service. The participants were from a range of professions including medical imaging, occupational therapy, physiotherapy, social work, speech pathology, pharmacy and health administration. They were located across seven Queensland Health Districts.
Participants had been in their current positions for between 2 and 7 years with an average of 4 years and had worked in a rural and remote area during their career for between 3 and 30 years with an average of 15 years. None of the managers were rural scholarship holders themselves.
The main themes that emerged from the manager interviews were:
- advantages and issues for the work unit when new graduates (including scholarship holders) commence rural practice
- scholarship effectiveness
- recommended changes to the scholarship scheme
- support strategies to enhance recruitment and retention relevant to scholarship holders and new graduates.
Advantages and issues: Generally participants were enthusiastic and supportive of employing new graduates and saw many advantages including allowing vacancies to be filled. New graduates were viewed as enthusiastic, passionate and motivated and they injected new energy into the team. They were regarded as technically competent practitioners who brought new ideas which reflected current best practice. New graduates impacted positively on senior staff in the district who provided support and mentoring and whose knowledge and skills were improved. The mentoring relationship was seen to promote greater understanding of the rural health context and challenges in those senior staff providing the support.
Some participants felt new graduates were not always able to 'hit the ground running', were not 'work ready' and that clinical reasoning was still developing. Such graduates needed extra training, supervision and support, which put a strain on staff who had to allocate time away from usual clinical duties to provide this support.
The need for an improved transition process between graduating and commencing rural practice ('from theory to practice') was raised. One participant was concerned that not all scholarship holders had a rural placement during their undergraduate studies. Another suggested that 'in an ideal world' graduates would spend 12 months in a regional centre before being placed in a rural area. At the very least it was suggested that new graduates spend 3 months in a regional centre before commencing rural practice. Another suggestion was to have opportunities for new graduates to come into larger regional centres for short periods of time to refine clinical skills and establish networks. Supervisor training was suggested as a way of ensuring that new graduates received adequate support to assist the transition into rural practice. It was felt that support structures needed to be built into the regular operational processes of the employing health services.
Generally the positives of having new graduates were seen to mitigate negatives. The main challenge for employing work units was the provision of clinical and professional support and mentoring, either locally or through connections with larger centres.
Perceived effectiveness of the QHRSS-AH in addressing manager's workforce needs (recruitment and retention): Most participants felt that the scholarship scheme was a good recruitment strategy although some commented that recruitment was easier at the time of the study than several years earlier due to significant increases in graduate numbers. There was discussion of potential oversupply of graduates in some professions in the future and the need to target scholarships to professions where recruitment gaps continue.
Interviewees expressed that the main recruitment challenge for their service was attracting experienced allied health professionals to senior clinical and management roles, rather than recruiting graduates, and this was not addressed by the QHRSS-AH.
Retention was raised as a significant problem. For rural scholarship holders, retention issues were felt to relate to candidate selection including the importance of having the right graduate in the position and selecting a candidate that is likely to stay. One participant felt the real decider for retention was recruiting someone who had a preference and passion for rural practice regardless of whether they were a scholarship holder or not. Another stated that 'taking a scholarship holder was a risk because you didn't know what you were getting - you got what you got'. This person felt that greater involvement of the employing health service in the initial scholarship recruitment round would go some way to address this concern. The recruitment point of the scholarship program at more than 2 years before graduation limits opportunity to target selection to current vacancies. The lack of capacity for the scholarship program to be a needs-responsive recruitment strategy for health services was regarded as a key issue.
Recommended changes to QHRSS-AH
Three main themes emerged regarding how the QHRSS-AH in its current form could be changed to better meet the needs of rural services and the organisation. These were the process of recruiting scholarship holders, graduate work readiness and ongoing professional development needs, and the conditions of employment including professional support.
A number of improvements were suggested in relation to the process of recruiting scholarship holders. This included an early recruitment connection between the undergraduate and the scholarship location so that preparation and planning educationally and personally could be carried out. Another recommendation was that health services should have greater involvement in the recruitment process to influence candidate selection.
The need for increased support for new graduates and scholarship holders was discussed, particularly for sole practitioners. This was seen as a health service responsibility and one participant identified the importance of mandatory involvement of all scholarship holders in supervision or mentoring.
In regards to graduate work readiness and ongoing professional development it was recommended that universities prioritise rural placement experience for scholarship holders in areas similar to where they are likely to be placed. Universities were also seen to play key roles in providing education about the reality of rural practice. Ensuring good processes for ongoing professional support was viewed as important and it was suggested that newly graduated scholarship holders needed more structured professional development plans to support their transition to rural or remote practice.
Support strategies to enhance recruitment and retention relevant to scholarship holders and new graduates: Support strategies to enhance recruitment and retention relevant to scholarship holders and new graduates, raised by managers, were similar to those discussed by scholarship holders.
Good orientation was seen as a vital strategy to support new staff. Providing opportunities for new graduates to spend time in larger regional centres was described as a valuable strategy that allowed networking and face-to-face interaction between new graduates and staff in the regional centre who might later provide support from a distance. It was felt that this face-to-face engagement increased the likelihood of the new graduate feeling comfortable in establishing contact and seeking advice at a later time.
A number of the managers emphasised the importance of regular contact and provision of support. Where possible it was felt support should be provided by professionals from the same allied health profession. Video conferencing was seen as useful for support and professional development but could not fully replace face-to-face contact. Connectivity in locations with limited broadband capacity was an issue for some.
Buddy systems were mentioned as a useful strategy. One District had employed a new graduate support officer and this was viewed as a very successful strategy. The importance of providing good clinical supervision was also highlighted.
At a social level it was seen to be important to provide avenues for social integration. This included providing opportunities for staff to interact with the broader community to allow them time to switch off from work. The importance of providing safe and comfortable accommodation was also discussed.
Generally participants expressed that very good support strategies were already in place and that there had been significant improvements in the last 10-15 years with allied health professionals generally being well supported in rural and remote practice.
Discussion
This paper discusses the review of the QHRSS-AH. While this review is unable to show a direct relationship between the scholarship scheme and recruitment and retention outcomes of early career allied health professionals in rural and remote areas, it does provide insight regarding possible impacts of the strategy.
Of those awarded a QHRSS-AH scholarship between 2000 and 2010, 13.7% broke their service bond. However a substantial proportion (45.2%) of scholarship holders studied had an outstanding commitment to the QHRSS-AH at the time of data collection as they were completing or had deferred their service period or were in their study period. Of those who had exited the QHRSS-AH between 2000 and 2010, 25% had done so by breaking their service bonds. A review study undertaken by Bärnighausen and Bloom examined the impact of financial incentives on recruitment and retention to rural practice8. Although a range of student incentives were examined in this review (service-requiring scholarships, educational loans with service requirements, service-option educational loans), and differences exist in professions and education finance contexts between the review and this study, its findings are informative. Bärnighausen and Bloom found most programs had substantial drop-out rates before the start of the service obligation8. On average, 3 in 10 participants did not fulfill their commitment but the drop-out rate was highest among students who committed to service (eg service-requiring scholarships and educational loans with service requirements). Although lower than in the Bärnighausen and Bloom review, attrition from the QHRSS-AH was not insignificant. For funding organisations, even if scholarship funds are recouped, broken bonds represent both an opportunity cost and real monetary cost as administration and associated expenses are not recovered. The prospective, longer term nature of a scholarship program probably makes the risk of unrecouped investment greater than retrospectively applied financial incentives such as university fee recovery. However, this requires further research.
Previous research on compulsory service programs conducted by Frehywot and colleagues identified that health professionals objected to compulsory service programs with a range of reasons cited including cost, poor rural facilities and resourcing, lack of transport and basic services, and difficulty in implementing the skills learned in their training12. They concluded that high turnovers associated with many compulsory service programs needs to be seen as the reality of rural practice rather than as a weakness of the program12.
Results from the interviews indicate both scholarship holders and managers view the scholarship program positively. For scholarship holders the program provides financial support during their undergraduate degree allowing them time to concentrate on their studies as well as providing them with a graduate employment opportunity. Managers perceive a range of positives that come from employing scholarship holders including enthusiasm, passion, motivation, energy and current knowledge and skills.
Results from this study indicate that most scholarship holders would have chosen to practice in rural locations regardless of receiving a scholarship. This study was unable to explore this issue in depth although a number of studies from Canada13, the USA14-17 and Australia18-21 demonstrate that people raised in rural communities are more likely to work in rural areas. Although this may suggest that scholarships may not be a necessary recruitment strategy, the qualitative data does suggest that scholarships provide significant benefits to both the recipients and managers. Further research, including longitudinal studies of successful and unsuccessful scholarship program applicants, is required to determine the extent, if any, of the influence of scholarship programs on graduate employment destination and retention in rural and remote practice.
This study found that 56.8% of QHRSS-AH scholarship holders' initial graduate positions were in a rural or remote location. This was possibly impacted by the limited ability to target scholarship programs with long study periods to vacancies at the point of graduation. Managers expressed limited demand for graduates and graduate supervision and training requirements for some professions. Some managers expressed concern that employing scholarship holders (or any new graduates) placed additional workload pressures on existing senior staff in the early phases of new graduate tenure. This was due to new graduates not being 'work ready' and needing additional support and time to feel comfortable and confident in their role. This view on the under-preparedness of new allied health professionals to cope with the diverse clinical work load has also been identified in previous studies21,22. Regional work placements before rural practice commenced was suggested by both scholarship holders and managers as a strategy to improve work readiness for rural practice.
Support issues identified by scholarship holders and managers were similar to that previously described in the literature22-25 and reflect both professional and personal issues. Professional and clinical supervision was highlighted as being important as well as a supportive work environment and culture, mentoring and professional development. The potential for regional placements before and during rural tenure was suggested as a means of developing both skills and networks. At a personal level, support with accommodation was the most mentioned issue as well as support for social integration into communities.
Both scholarship holders and managers identified that health services play a key role in the provision of support for new graduates but responses indicated that there are differences between services regarding how well this support is provided. Some services were reported to have a structured process in place to ensure scholarship holders and new graduates are oriented and supported when commencing rural practice. Other participants suggested that this could be improved in their service.
While the mixed methods approach used in this study is a strength that has allowed an in-depth understanding of the issue this study does have some limitations. The qualitative nature of the research and diversity of professions, service settings and rural practice locations of interviewees does not allow this study to identify a definitive association between the undergraduate scholarship schemes and enhanced recruitment and retention of early career allied health professionals in rural and remote services. Seventeen scholarship holders from eight different professions and eleven managers from seven different professions participated and were spread across nine Queensland Health Districts. This diversity has made thematic saturation of the data impossible and it is possible that a range of issues are still not identified for the scholarship holders and managers.
The study design cannot exclude volunteer bias. A review of the data reveals individual respondents generally provided both positive and negative views of the scholarship program, suggesting a frank assessment of their experiences was offered. Reported themes were strongly represented in the data contributed by a professionally and geographically diverse group of interviewees. Interviews did not include scholarship recipients who did not complete their service period or those who no longer work for Queensland Health. Exploring their views would allow for deeper understanding regarding reasons for breaking service; however, this was outside the scope of the current study.
Although scholarship holders and their managers support the rural scholarship program, aspects of the scholarships in their current form require consideration in light of current workforce supply and demand issues. Targeting future scholarships to workforce shortages is required to provide any potential benefit to health services, although time-responsiveness of a scholarship program to address shortages has limitations. Concerns exist regarding the absence of rural clinical placements for some scholarship holders during their university training. Undergraduate rural placements combined with other interventions such as regional work placements before and during rural practice could play a significant role in addressing concerns of work readiness expressed by managers. While many scholarship holders felt well supported as a new graduate entering rural practice, others identified gaps in their experiences and the support they received. Opportunities exist to strengthen and standardise development and support structures across all health services, particularly for new graduates. Support structures may extend beyond the workplace and address personal support needs in areas such as accommodation and social networking.
Acknowledgements
This research was funded by Queensland Health through the Allied Health Workforce Advice and Coordination Unit. Acknowledgement is made to the following people for their assistance throughout the research: Dr Louise Roufeil and Dr Kristine Battye from Kristine Battye Consulting for their assistance with the literature review; Ms Jennifer Cox for her assistance with data collection and administrative support; Ms Julie Parison for provision of analytical support for the qualitative data. The research team is also highly appreciative of the enthusiasm shown by the Queensland Health staff who willingly agreed to participate in this project. The support received from the Allied Health Workforce Advice and Coordination Unit and Rural Health Connections is also acknowledged, in particular Sue Little and Cathy Kirkbride, who assisted in scholarship data provision.
References
1. Wakerman J, Humphreys JS, Kuipers P, Entwistle P, Jones J. Primary health care delivery models in rural and remote Australia - a systematic review. BMC Health Services Research 2008; 8: 276.
2. Australian Health Workforce Advisory Committee. The Australian Allied Health Workforce - An overview of workforce planning issues. AHWAC report. Sydney, NSW: AHWAC, 2006.
3. Best J. Rural health stocktake advisory paper to the Commonwealth Department of Health and Aged Care. Canberra, ACT: Commonwealth Department of Health and Aged Care, 2000.
4. Allen O. SARRAH: recruitment and retention of Allied Health workforce. Australian Journal of Rural Health 2005; 13(3): 198.
5. Services for Australian Rural and Remote Allied Health. Submission to the Health Workforce Productivity Commission Issues Paper. Canberra, ACT: SARRAH, 2005.
6. Smith T, Cooper R, Brown L, Hemmings R, Greaves J. Profile of the rural allied health workforce in Northern NSW and comparison with previous studies. Australian Journal of Rural Health, 2008; 16(3): 156-163.
7. World Health Organization. Increasing access to health workers in remote and rural locations through improved retention: global policy recommendation. (Online) Geneva: WHO, 2010. Available: http://www.who.int/hrh/retention/guidelines/en (Accessed 25 September 2013).
8. Bärnighausen T, Bloom DE. Financial incentives for return of service in underserviced areas: a systematic review. BMC Health Services Research, 2009; 9: 86.
9. Creswell JW, Plano Clark VL. Designing and conducting mixed methods research. California: Sage Publications, 2007.
10. Patton MQ. Qualitative research and evaluation methods. 3rd ed. California: Sage Publications, 2002.
11. Queensland Government. Human Resources Policy C15: allowances. (Online) 2010. http://www.health.qld.gov.au/qhpolicy/docs/pol/qh-pol-099.pdf (Accessed 25 September 2013).
12. Frehywot S, Mullan F, Payne PW, Ross H. Compulsory service programs for recruiting health workers in remote and rural areas: Do they work? Bulletin of the World Health Organization 2010; 88: 364-370.
13. Easterbrook M, Godwin M, Wilson R, Hodgetts G, Brown G, Pong R, et al. Rural background and clinical rotations during medical training: effect on practice location. Canadian Medical Association Journal 1999; 160(8): 1159-1163.
14. Rabinowitz HK, Diamond JJ, Markham FW, Paynter NP. Critical factors for designing programs to increase the supply and retention of rural primary care physicians. Journal of the American Medical Association 2001; 286(9): 1041-1048.
15. Fryer GE, Stine C, Vojir C, Miller M. Predictors and profiles of rural versus urban family practice. Family Medicine 1997; 29(2): 115-118.
16. Kassebaum DG, Szenas PL. Relationship between indebtedness and the specialty choices of graduating medical students. Academic Medicine 1993; 68(12): 934-937.
17. Brooks RG, Mardon R, Clawson A. The rural physician workforce in Florida: a survey of US- and foreign-born primary care physicians. Journal of Rural Health 2003; 19(4): 484-491.
18. Wilkinson D, Beilby J, Thompson D, Laven G, Chamberlain N, Laurence C. Influence of rural background on where South Australian general practitioners work. Medical Journal of Australia 2000; 173(3): 137-140.
19. Laven G, Beilby J, Wilkinson D, McElroy H. Factors associated with rural practice among Australian-trained general practitioners. Medical Journal of Australia 2003; 179(2): 75-79.
20. Playford D, Larson A, Wheatland B. Going country: rural student placement factors associated with future rural employment in nursing and allied health. Australian Journal of Rural Health 2006; 14: 14-19.
21. Lee S, Mackenzie L. Starting out in rural New South Wales: the experience of new graduate occupational therapists. Australian Journal of Rural Health 2003; 11(1): 36-43.
22. O'Toole K, Schoo A, Hernan A. Why did they leave and what can they tell us? Allied health professionals leaving rural settings. Australian Health Review 2010; 34: 66-72.
23. Struber JC. Recruiting and retaining allied health professionals in rural Australia: Why is it so difficult? Internet Journal of Allied Health Sciences and Practice 2004; 2(2).
24. Stagnitti K, Schoo A, Dunbar J, Reid C. An exploration of issues of management and intention to stay: allied health professionals in South West Victoria, Australia. Journal of Allied Health 2006; 35(4): 226-232.
25. Schoo A, Stagnitti KE, Mercer C, Dunbar J. A conceptual model for recruitment and retention: allied health workforce enhancement in Western Victoria, Australia. Rural and Remote Health 5: 477. (Online) 2005. Available: www.rrh.org.au (Accessed 25 September 2013).



