Introduction
There is major maldistribution of physicians in the Democratic Republic of the Congo (DRC). While 70% of Congolese live in rural areas, relativley few doctors practice there1,2. Until recently all three Congolese medical schools were publicly funded and located in large cities. In 1989 the government authorized the establishment of additional medical schools throughout the country, partially to address the need for physicians in rural areas. This policy also allowed for private orgainisations to develop medical schools, especially religious organizations in rural areas. The Catholic University of Graben (UCG) Medical School at Butembo was one of the first rural medical schools established in the DRC.
Of the 1989 total of 25 DRC medical schools, 11 are privately funded and only one is located in a rural area. All 14 publicly funded schools are located in urban areas. This is consistent with the Congolese system where religious (catholic and protestant) services and activities in education and medicine are generally localized in rural areas, while public enterprises are dominant in urban areas.
Uneven urban-rural distribution of healthcare services and medical personnel is a concern in many countries3,4, often leading to poorer access to good health care and services for rural populations. The situation is magnified in Africa5,6 and compounded by the massive migration of medical personnel to other well-resourced countries7-9. Because medical studies are fully self-funded in DRC, graduation practice location is self-determined, and the government is unable to prevent the loss of new graduates to foreign countries.
Although in developing countries approximately 80% of the population live in rural areas (as opposed to 20% in such countries as the USA and Canada10,11), entire-country decisions are often determined by urban policy-makers, to the disadvantage of rural populations. Multiple factors increase the uneven distribution of resources to rural areas, including difficult rural living conditions, a lack of amenities such as shops and educational opportunities, and inadequate access to medical equipment12.
Bowman13 suggested four factors are pivotal in reversing this maldistribution: (i) selecting medical students who have rural birth origins; (ii) selecting medical students who are older than 29 years on graduation; (iii) changing curriculum and policies to increase the likelihood that graduates will choose family practice; and (iv) increasing the number of 'distributional' medical schools located in rural and underserved areas. The latter factor supports the hypothesis that the uneven distribution medical personnel is related to an urban-location bias for faculties of medicine.
To overcome this problem, several strategies have been suggested14-17, and Hays suggested the following17:
- Organize rotation programs for medical students to work in resource poor and neglected rural areas.
- Develop a rural hospital or clinic for each faculty of medicine and rotate all students there.
- Create faculties of medicine in rural areas where a complete curriculum of adapted training is available.
At the end of the 1980s, DRC policy development led to the establishment of a rural-located medical school, as recommended by Hays17. In this article, the initial outcomes of this newly established rural-located medical school are reported, and compared with an urban-located medical school, both located in east DRC. The movement of early career doctors from each institution was tracked.
Definition of rural and urban areas
In DRC the term 'urban' is related to a town environment which has a legally designated mayor. However, rural or non-urban areas include small settlements, villages and other areas distant from towns, lacking in human and material resources (eg no running water, electricity). Currently in DRC, both urban and rural areas lack facilities so the presence of a mayor (urban) is an important distinction, as is the reduced availability of drinking water, electricity, medical services, public transportation and sanitation of rural areas.
Methods
The two medical schools
Two recently established private medical schools located in east DRC (Fig1) were studied: the rural Catholic University of Graben (UCG) and the urban located Université Evangélique en Afrique (UEA). Both follow the national curriculum for DRC medical schools and there is no emphasis on primary health care at the rural school. According to Congolese higher education policy, student admission is according to the performance of students in their last year of high school and rural background characteristics are not considered.
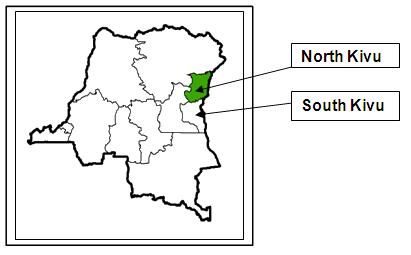
Figure 1: Map showing the locations of the medical schools in the eastern provinces of the Democratic Republic of the Congo.
The Faculty of Medicine of UCG is located in an eastern rural area in Butembo in North-Kivu (NK) Province. This province covers 59 000 km2 and has a population of 5 million (Fig1). In 1989 when the medical school was established, Butembo was a village with less than 74 000 inhabitants and no running water or electricity. The UCG was created by the Catholic church at the request of the local community. It consists of 6 faculties (veterinary science, agriculture, economic sciences, social, political and administrative sciences, law and medicine), as well as several study and research centers. The first doctors graduated from the seven-year curriculum during the academic year 1997-1998.
The School of Medicine UEA is located in an urban area at Bukavu in South Kivu, a neighboring province of NK (Fig1). This province covers 65 070 km2 and has a population of 2 837 779. The chief town Bukavu has 245 000 inhabitants. The UEA is a Protestant university founded in 1991 and has 4 faculties: agriculture, economic sciences, medicine and theology. The first doctors graduated from the seven-year curriculum during the academic year 1997-1998.
Records from the academic services offices of both institutions were analysed to establish matriculation and graduation rates of the first 6 classes of both schools. At UCG the first 6 graduation classes included 43 doctors; at UEA of 120 graduating doctors two were lost to death, reducing the follow-up number to 118. Practice location of the graduates was obtained by direct contact with alumni and from provincial medical offices. No information was available for 11 UEA graduates, so the final UEA study population was 107.
The data were analyzed using SPSS for Windows v12.0.1 (SPSS; Chicago, IL, USA). Descriptive statistic (percentage, means and standard deviation), t-test and χ2 were used for comparison.
Results
Number of the matriculating and graduating physicians
At both universities, less than 6% of matriculated students finished their studies within the planned seven-year curriculum period. At the rural UGC medical school, 43 doctors graduated over the 6 classes from 1997 to 2004. This represents an annual average of 7.2 graduating doctors or 3.9% of all matriculated students. At the urban UEA medical school, a total of 120 doctors graduated over the 6 classes, representing an annual average of 20 doctors but only 5.7% of all matriculated students.
Table 1: Number of doctors matriculated and graduated at the Catholic University of Graben rural medical school and Université Evangélique en Afrique urban medical school
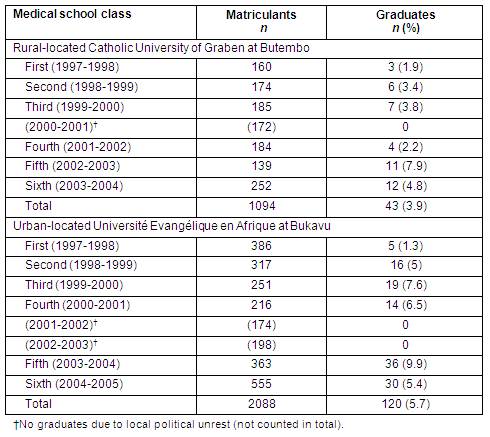
Location of employment for the graduating physicians from the Catholic University of Graben rural medical school and Université Evangélique en Afrique urban medical school
Among the 43 rural UCG graduates, almost all (97.7%) worked in the NK Province where they were trained (Table 2). Of these, 81.4% were located in a rural area (Fig2). One graduate (2.3%) had left the area for further training. In contrast, less than half the urban UEA graduates (46/107, 43.0%) were employed in the South Kivu Province where they were trained. Of these, 61% were employed in a rural area while 39% worked in urban Bukavu; 15.9% (17/107) were employed in urban areas in other DRC provinces.
Of the 107 UEA graduates, 25 (23.4%) were employed in other African countries. In contrast with the rural-trained doctors, a substantial number of these urban-school graduates (15.9%) were pursuing advanced study in the DRC (n = 1), in other African countries (14) or outside Africa (3).
Table 2: Location of employment or advanced study of graduates from the Catholic University of Graben rural medical school and Université Evangélique en Afrique urban medical school (2006)
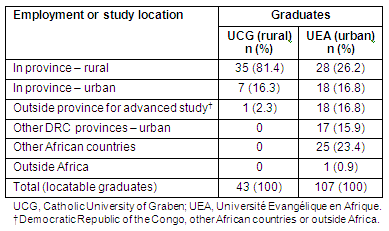
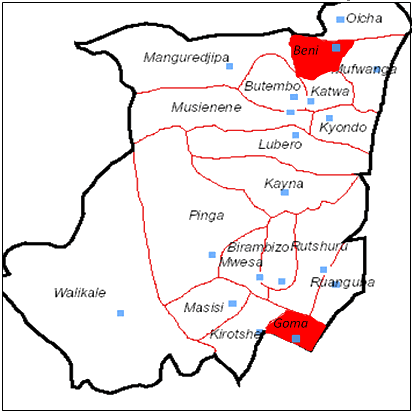
Figure 2: Map showing North Kivu health zones and the location and number of graduates from the rural Catholic University of Graben Medical School. The two North Kivu towns (Beni and Goma) are shaded.
For location of employment or advanced study, the difference was highly significant between rural and urban areas (χ2 = 653.28, df = 5, p<0.00001).
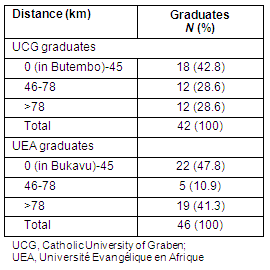
All 42 doctors who graduated from rural UCG and practising in NK were located between 0 km (in Butembo) and 355 km from Butembo (Table 3). The mean distance from their place of training was 88 km. The majority (71.4%) worked within a radius of 78 km of their medical school, or 3 hours travel by motorcycle. A similar pattern was found for the 46 urban graduates from UEA who were practising in the South Kivu Province. All were located between 0 km (in Bukavu) and 340 km from Bukavu, the majority (68.7%) within a radius of 78 km of their medical school.
Table 3: Distance between place of employment and their medical school for medical graduates of the rural Catholic University of Graben (at Butembo) and urban Université Evangélique en Afrique (at Bukavu)
Type of employment for the rural and urban graduating doctors in the province
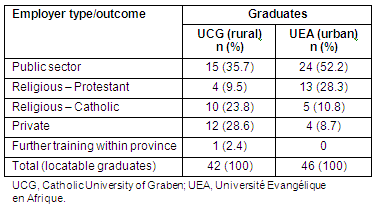
The public sector was the largest single employer of graduate doctors practising in the province: 35.7% of rural UCG graduates (15) and 50% of urban UEA graduates (23%) (Table 4). The second largest employing sector was private healthcare in facilities sponsored by religious organisations, at 33.3% of UCG graduates (14) and 39.1% of UEA graduates (18). The remainder were employed in other private facilities.
Table 4: Type of employment of graduates practising in their original province
Discussion
This study provides evidence that rural-located medical schools can increase the distribution of practising physicians to rural areas in the DRC. Similar results have been found in other countries. In Canada 30.7% of graduates from a rural-based medical school practised in rural areas18. Similarly, in China 34% of graduates from a rural-based medical school practised rurally19. Visiting health academics in Thailand reported that doctors trained in rural areas tended to remain and work there20. These 'successful' examples all fell far short of the 81.3% rural practitioners produced by UCG.
In the present study, the contrast between rural UCG and urban UEA students was striking, with 81.4% versus 26.7%, respectively, working in a rural zone on graduation, and this difference was highly significant (χ2 = 38.41, df = 1, p<0.00001). These data confirm other studies that found graduates from urban settings tend to remain and work there13,21,22. Hays17 and Bowman13 concluded that a major strategy to increase the distribution of doctors to rural areas is the existence of rural medical schools.
While the data on enhanced distribution of doctors to rural postings is encouraging, the present study highlights a number of troubling issues. First, the yield of graduates was low from both schools. This appears to be related to student change of faculty and/or university and is currently being investigated. At the time of the study both schools were newly established in an era of political unrest, and were subject to national and local (community) pressure to admit more students than the faculty could educate. Other likely factors include inadequate preparation of students for higher education; inadequate faculty numbers and preparation for their roles; and inadequate equipment for effective teaching (in common with Indian studies23,24). It may also be necessary to define rural medical schools by including rural-specific subjects to supplement to the national curriculum25.
Second, the already low proportion of graduates from both schools was far lower than that of other African universities for the period 1990-2004 (423 at Kisangani, DRC; 1721 at Ibadan, Nigeria; 2196 at Lagos, Nigeria; 2214 at Cape Town, South Africa; 1375 at Makerere, Uganda9) and this merits additional study. The contributing factors already discussed and the lack of scholarships and facilities such as campus restaurants for students may play a greater role in the low graduation rate than location. However, with more than 100 students matriculating from UEA, an increase of even 10%, would triple the graduating doctors available for heath service.
Third, the rural-trained graduates were less likely to access post-graduate training, with only one UCG doctor (2.5%) undertaking residency training, compared with 18 UEA doctors (16.8%). This emphasizes the worth of providing rurally relevant postgraduate training for those committed to remaining in a rural setting25.
The relatively close location of practising graduates to their parent institutions offers an opportunity to provide continued professional development (CPD) from the medical schools, which other studies have shown to be important in retaining doctors in rural areas21,26,27. The contribution of the medical schools to CPD is important in the present setting, where poor roads and communication systems make ongoing education difficult for graduates. Moreover, medical-school based CPR creates the possibility of rural-based practitioners playing a role in undergraduate training28.
The limitations of the present study are that only two schools were investigated, and that both were new so only early outcomes of medical practice could be measured. The study focused only on the location of medical schools and there were a low number of graduating students. Other factors reported to increase rural-based medical practitioners (such as the rural origin of medical students, increased age of students, and increased emphasis on family medicine in the curriculum13) were not explored. These other factors, in addition to following newly graduated medical practitioners for longer periods, and investigating other rural and urban located medical schools should be investigated before making major recommendations for policy changes. This and a previous study9 strongly recommend developing better tracking systems to follow students before, during and after graduation from medical schools in Africa.
The present results shows that all medical sectors within the province (government, private and religious/denominational) benefit from the services these young doctors provide, and that doctors produced by private medical schools associated with religious bodies mainly serve in the public sector where they are desperately needed. With a DRC doctor : population ratio of 1:10 0002, it is encouraging to see positive results from policy that promotes the decentralization of faculties of medicine.
Conclusion
This study provides five key messages: (i) a rural-located medical school in the DRC provides the majority of its graduates to the rural workforce; (ii) rural graduates work in all sectors where doctors are needed; (iii) attention must be paid to improving the yield of graduates; (iv) very few rural graduates appear to have the opportunity of advanced training; and (v) the majority of graduates work close to their medical school, and this offers universities a relatively easy opportunity to provide CPD, and also increase faculty capacity by recruiting graduates to academic staff.
Acknowledgements
The author thanks the Foundation for the Advancement of International Medical Education and Research (FAIMER) for its support in the form of fellowships that included graduate education at Maastricht University. The author also thanks Page Morahan, PhD, for her careful review of the manuscript.
References
1. Kongolo LS. Rapport National, Ministère du Plan et de la Reconstruction (République Démocratique du Congo). Rapport présenté à la quatrième Réunion du Comité de suivi de la mise en oeuvre de la Déclaration de Dakar/NGOR (DNN) et du Programme d'Action de la Conférence Internationale sur la Population et le Développement; 28-31 Janvier 2002; Yaoundé (Cameroun), 2002.
2. WHO. World health statistics 2008. (Online) 2008. Available: http://www.who.int/whosis/whostat/EN_WHS08_Full.pdf (Accessed 21 April 2009).
3. WONCA Working Party on Rural Practice. Policy on rural practice and rural health. Melbourne, VIC: Monash University School of Rural Health, 2001.
4. Hays R. Rural medical education in Europe: the relevance of the Australian experience. Rural and Remote Health 7: 683. (Online) 2007. Available: http://www.rrh.org.au (Accessed March 2008).
5. De Vries E, Reid S. Do South African medical students of rural origin return to rural practice? South African Medical Journal 2003; 93(10): 789-793.
6. Onwujekwe O, Uzochukwu B. Socio-economic and geographic differentials in costs and payment strategies for primary healthcare services in Southeast Nigeria. Health Policy 2005; 7(1): 383-397.
7. Haagopian A, Thompson MJ, Fordyce M, Johnson, Hart LG. The migration of physicians from sub-Saharan Africa to the United States of America: measures of the African brain drain. Human Research in Health 2004; 2(1): 17.
8. Cooper R.A. Physician migration: a challenge for America, a challenge for the world. Journal of Contininuing Education for Health Professionals 2005; 25(1): 8-14.
9. Longombe AO, Burch V, Luboga S, Mkony C, Olapade-Olaopa EO, Otieno-NyunyaB et al. Research on medical migration from Sub-Saharan medical schools: usefulness of a feasibility process to define barriers to data collection and develop a practical study. Education and Health 2007; 20(10): 1-6.
10. Ng E, Wilkins R, Pole J, Adams OB. How far to the nearest physician? Rural and Small Town Canada Analysis Bulletin 1999; 1(5): 1-7.
11. Blumenthal SJ. The effects of socioeconomic status on health in rural and urban America. JAMA 2002; 287(1): 109.
12. Kumar D, Verma A, Sehgal VK. Neonatal mortality in India. Rural and Remote Health 7: 833. (Online) 2007. Available: http://www.rrh.org.au (Accessed 4 March 2008).
13. Bowman RC. They really do go. Rural Remote Health 8: 1035. (Online) 2008. Available: http://www.rrh.org.au (Accessed 27 December 2008).
14. Rourke J. Strategies to increase the enrollment of students of rural origin in medical school: recommendations from the Society of Rural Physicians of Canada. Canada Medical Association Journal 2005; 172(1): 62-65.
15. Schoo AM, McNamara KP, Stagnitt KE. Clinical placement and rurality of career commencement: a pilot study. Rural Remote Health 8: 964. (Online) 2008. Available: http://www.rrh.org.au (Accessed 27 December 2008).
16. Inoue K, Hirayama Y, Igarashi M. A medical school for rural areas. Medical Education 1997; 31(6): 430-434.
17. Hays R. Developing health education to address recruitment and retention issues. In: Proceedings, World Rural Health, International Conference; 1-3 May 2002; Melbourne, VIC; 2002. Available: http://abc.net.au/rural/worldhealth/papers/84.htm (Accessed 16 June 2007).
18. Mathews M, Rourke JTB, Park A. National and provincial retention of medical graduates of Memorial University of Newfoundland. Canada Medical Association Journal 2006; 175(4): 357-360.
19. Wang L. A Comparison of metropolitan and rural medical schools in China: Which Schools Provide Rural Physicians? Australian Journal of Rural Health 2002: 10(2): 94.
20. The University of New England (UNE). Thai health academics visit UNE. News and Events. (Online) 2007. Available: http://www.une.edu.au/news/archives/000396.html (Accessed 17 November 2008).
21. Kamien M. Staying in or leaving rural practice: 1996 outcomes of rural doctors' 1986 intentions. In: Proceedings, 5th National Rural health Conference; 14-17 March 1999; Adelaide SA, 1999.
22. Dunbabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available: http://www.rrh.org.au (Accessed 21 April 2008).
23. Sood R. Medical education in India. Medical Teaching 2008; 30: 585-591.
24. Singh T, Bansal P, Sharma M. A need and necessity for faculty development: the role of medical education units in the Indian context. Southeast Asian Journal of Medical Education 2008; 2: 2-6.
25. Palsdottir B, Neusy A-J, Reed G. Building the evidence base: networking innovative socially accountable medical education programs. Education and Health 2008; 2: 1-6.
26. White CD, Willet K, Mitchell C, Constantine S. Making a difference: education and training retains and supports rural and remote doctors in Queensland. Rural and Remote Health 7: 700. (Online) 2007. Available: http://www.rrh.org.au (Accessed 29 July 2008).
27. Hoyal FM. 'Swallowing the medicine': determining the present and the desire modes for delivery of continuing medical education to rural doctors. Australian Journal of Rural Health 1999; 7: 212-215.
28. Somers GT. Do rural mentors, rural undergraduate clubs and rural rotations increase the medical student's intention to practise in the country? (Online) 2002. Available: http://www.rrh.org.au/journal/article/706 (Accessed 14 September 2008).
