Abstract
Introduction: The regionally-based James Cook University (JCU) School of Medicine aims to meet its mission to address the health needs of the region by combining selection and curriculum strategies shown to increase rural career recruitment outcomes. The School has graduated 536 students in its first seven cohorts from 2005 to 2011. This paper presents the early career practice locations and the specialty training undertaken by these cohorts, and describes the association between later practice location with both hometown at application and internship location.
Methods: 'Hometown at application' data for JCU Bachelor of Medicine, Bachelor of Surgery (MBBS) graduates was retrieved from administrative databases held by the university, while postgraduate location and career data were obtained either from personal contact via email, telephone, Facebook or electronically from the Australian Health Practitioner Regulation Authority website. Practice location was described across Australian Standard Geographical Classification Remoteness Area (RA) categories.
Results: Data for the primary practice location of 536 JCU MBBS graduates across postgraduate years (PGY) 1 to 7 is 99% complete. A total of 65% of JCU graduates undertook their internship in non-metropolitan locations including 20% in RA 2 and 44% in RA 3-5, a pattern of practice different to that of other Australian clinicians. For the internship year, 'non-metropolitan-origin' JCU MBBS graduates predominantly worked in RA 2-5 locations, while 'metropolitan origin' graduates were more likely to work in major cities. However, by PGY 7, the distribution of 'rural' and 'metropolitan' origin JCU graduates across RA categories was similar. The RA category of internship location - either 'metropolitan (RA 1) or 'non-metropolitan' (RA 2-5) - was associated with the location of subsequent practice across PGY 2-7.
Conclusions: This comprehensive data set provides the first real evidence from one of Australia's new medical schools on actual postgraduate practice location, as compared to 'intent to practice'. The geographic profile by RA of JCU graduates' hometown and patterns of postgraduate practice is different to that of other Australian medical students and doctors. This early evidence supports the JCU model of distributed non-metropolitan medical education, and suggests more regionally-located internship and specialty training places would further increase the medical workforce in northern and/or rural Australia. The workforce impact of the seven cohorts of graduates in this study is starting to be felt in rural and regional Australia, and, if these trends continue, will result in significant workforce improvements over the next decade. These results support further investment in regional and rural medical education.
Key words: graduate, medical, practice location, regional, workforce.
Introduction
Health workforce shortages and mal-distribution continue to constrain the equitable delivery of healthcare services to much of the Australian population living outside of metropolitan and adjacent conurbations1. In response, there has been substantial investment during the past 15 years in rural clinical school infrastructure and an increase in medical student numbers, particularly those with a rural background2.
Included in this expansion is the James Cook University (JCU) School of Medicine, which was established in 1999 almost 1400 km north of the nearest metropolitan area of Brisbane to address the workforce needs of underserved populations in northern Australia3. This predominantly undergraduate entry Bachelor of Medicine, Bachelor of Surgery (MBBS) program has applied the available Australian and international evidence on rural student selection, curriculum and assessment design, and placement location4-8. Several other new medical schools around the world have followed similar developmental pathways9.
Following this substantial investment it is important to determine the effectiveness of these innovations. It is, however, early days for such long-term strategies. Most studies so far show that student intentions to practise rurally increase after experiencing undergraduate rural placements1,10,11, and that students from a rural clinical school are more likely to choose an internship at a regional hospital12,13. However, the Australian evidence that regionally-located medical schools and/or undergraduate rural placements actually result in significant numbers of graduates practising post-internship in a rural location is inconclusive14,15. Furthermore, there are many influences on a graduate's decision to practise rurally, making it difficult to separate the influence of prior intent from curricular experiences, regional familiarity associated with long-term clinical placements and external life events.
This paper presents early evidence for the effectiveness of the first of Australia's new, regionally-located medical schools. Postgraduate practice locations of the initial seven cohorts are described for postgraduate years (PGY) 1-7, with additional analyses showing the associations between applicants' hometown origin, internship location and practice location.
Methods
Design
This analysis of practice location data is part of an ongoing longitudinal cohort study that will continue to provide information about JCU MBBS graduate outcomes. Annual practice location data was obtained for graduates in the first seven cohorts who entered the workforce as interns (PGY 1 doctors) from 2006 to 2012, PGY 2 from 2007 to 2012, etc. Data are thus available for seven cohorts in PGY 1, six cohorts in PGY 2, and so on. Correspondingly, location of practice in 2006 reflects one cohort, and two cohorts in 2007, etc.
Practice location
Practice location data and information on postgraduate training undertaken were obtained from several sources. Consent to join an alumni contact list and permission for subsequent contact by the medical school via email, telephone and Facebook was obtained from an annual exit survey of graduating medical students, which has been conducted since 2005 as part of the JCU longitudinal tracking project on graduate outcomes. Contact was made by email and telephone communication, and via a JCU School of Medicine Facebook page, which was initiated on student advice in 2005 and has been continued since for all graduating cohorts. These three strategies provided practice location data for 456 of 536 (85%) of all graduates from 2005 to 2011.
Additional data on practice location data was sourced from the Australian Health Practitioner Regulation Authority (AHPRA) website (http://www.ahpra.gov.au), the validity of which was checked by a comparison of 20 practice locations obtained via direct contact, showing agreement for 18/20 (90%) of cases. In combining these strategies, practice locations could be identified for 530 out of a total of 536 graduates, representing 99% of all graduates. The latest available data from 2008 on the practice location of Australian clinicians and proportion of population they serve were sourced from the Department of Health and Ageing2.
Hometown location
'Hometown at application to medical school' data for JCU MBBS graduates were retrieved from administrative databases held by the university and were available for 499 graduates (93% of the total). Data for the town Australian medical students commencing in 2011 'had lived in the longest' was obtained from the Medical Schools Outcomes Database (MSOD) project16.
Defining location rurality
The Australian Standard Geographical Classification Remoteness Area (ASGC-RA) index was used to categorise location data - both for hometown and practice since graduation - into 'metropolitan' (RA 1), 'inner regional' (RA 2), 'outer regional' (RA 3), 'remote' (RA 4) or 'very remote' (RA 5)17. Graduates who did not spend an entire calendar year in one location were classified according to the self-defined location they provided when asked where they had spent the majority of the year. The term 'non-metropolitan' was used for categories RA 2-5, and the term 'rural' for categories RA 3-5.
Specialty choice
Data on specialty training choice was described for only the first four graduating cohorts (2005-2008) to allow at least four years for graduates to choose their desired specialty.
Analysis
Graduates' PGY 2-7 practice locations across RA 1-5 were categorised depending upon their hometown at application and practice location of internship year. Graduates having a 'metropolitan (metro) hometown & metro-based internship' were compared to graduates having a 'non-metro hometown & metro internship', 'metro hometown & non-metro internship' or 'non-metro hometown & non-metro internship'. Analysis involved the estimation of odds ratios (OR) with associated confidence intervals using the Woolf (logit) method18, and the calculation of p values using two-tailed Pearson χ² tests.
Ethics approval
Ethics approval for the study was obtained from the JCU Human Research Ethics Committee; ethics approval number H1804.
Results
The primary location of practice for graduates' internship and later postgraduate years are shown in Table 1. As shown in Table 2, the 536 tracked JCU MBBS graduates spent a total of 1925 'graduate-years' practising in Australia (not including years graduates practised overseas, missing or not in the medical workforce). About 60-70% of graduates in these seven cohorts worked as interns outside of major cities (RA 1), including 20% in RA 2 and 44% in RA 3-5, supporting previously reported data11. Figure 1 shows the geographical spread of the communities within Australia where JCU MBBS graduates are known to have practised all or most of a 'graduate-year' between 2006 and 2012. These demonstrate a non-metropolitan pattern of practice, predominantly in regional Queensland, with the most popular internship locations being Townsville (311 graduate-years) and Cairns (128 graduate-years).
Table 2 shows that the majority of the 499 JCU MBBS graduates with an identified home town at application had non-metropolitan home locations: 82 (16%) were from a major city (RA 1) and 313 (63%) from a rural location (RA 3-5). Tables 3 and 4 show how practice locations across PGY 1-7 relate to graduates having a non-metropolitan (RA 2-5) or metropolitan (RA 1) hometown at application to medical school, and by undertaking their internship in either a non-metropolitan (RA 2-5) or metropolitan town (RA 1), respectively. Non-metropolitan origin graduates predominantly chose inner regional or rural towns to undertake their internship (69%), while metropolitan origin graduates predominantly chose major cities for their internship (57%), and this pattern remained similar across PGY 2-7. Interestingly, 6% of non-metropolitan origin graduates were practising in a remote or very remote town across PGY 4-7, compared to almost none of the metropolitan origin graduates, although numbers are low and statistical significance cannot be calculated.
Differences in the distribution of graduates' practice location across PGY 1-7 are noted in relation to the location of internship. Table 4 demonstrates that by PGY 6 and 7, around 30% of JCU MBBS graduates who undertook a non-metropolitan internship were practising in a major city location (RA 1), while around 60% of graduates who undertook a metropolitan internship were practising in a major city. Table 3 also shows a similar proportion of metropolitan origin graduates were practising in metro areas in PGY 6 and 7 (57%) as non-metro-origin graduates were practising in a non-metro location in PGY 6 and 7 (67%).
Table 2 summarises the data on JCU graduate locations from 2006 to 2012, and provides a comparison with data on the hometown location of these graduates and of all commencing Australian medical students in 201116, as well as demographic data on the distribution of Australian medical practitioners and the Australian population2. Sixty-three per cent of JCU MBBS graduates had a hometown in RA 3-5 at application to medical school, compared with 13% of all Australian medical students. Further, Australian clinicians were predominantly located in RA 1 and 2 locations in 2011, with only 6% practising in rural or remote locations (RA 3-5)2; in contrast, 43% of JCU MBBS graduate-years were spent in rural or remote locations between 2006 and 2012.
Table 1: James Cook University MBBS graduates' primary location of practice in postgraduate years 1-7?
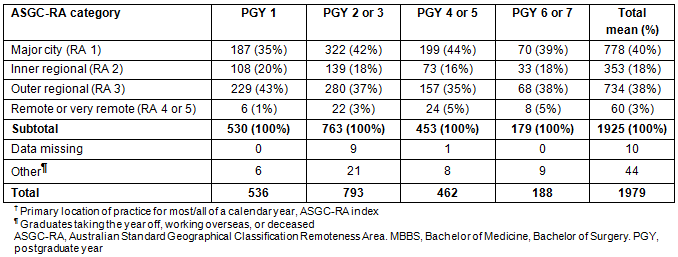
Table 2: Summary of James Cook University MBBS graduates' hometown at application and postgraduate years 1-7 primary location of practice in ASGC-RA locations, compared to the population of Australian clinicians and the general Australian population
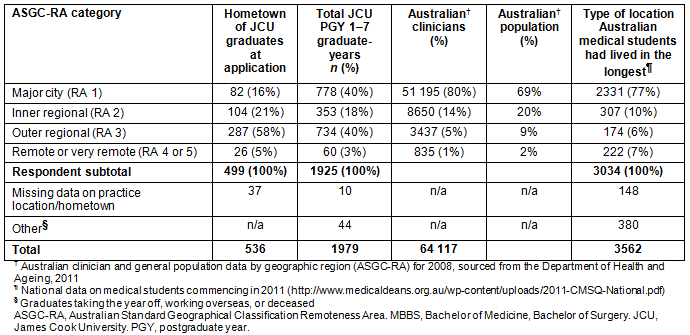
Table 3: Practice locations for James Cook University MBBS graduates across postgraduate years 1-7, classified by ASGC-RA of hometown at application to medical school (non-metropolitan centre ('non-MC') = RA 2-5 location, and metropolitan centre ('MC origin') = RA 1 location)
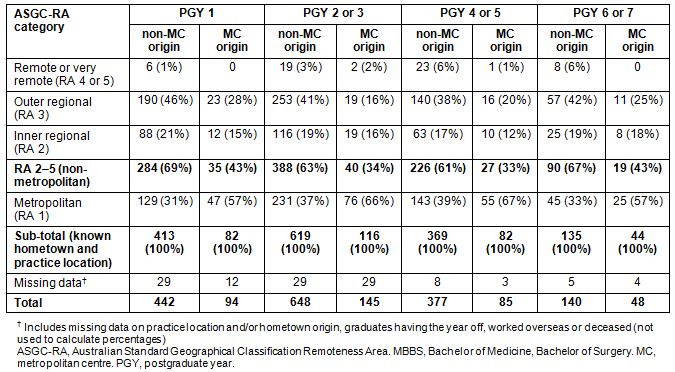
Table 4: Practice locations for James Cook University MBBS graduates across postgraduate locations 1-7, classified by ASGC-RA location of internship
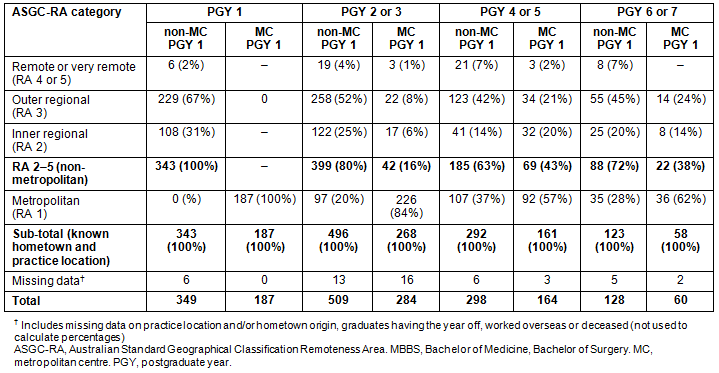
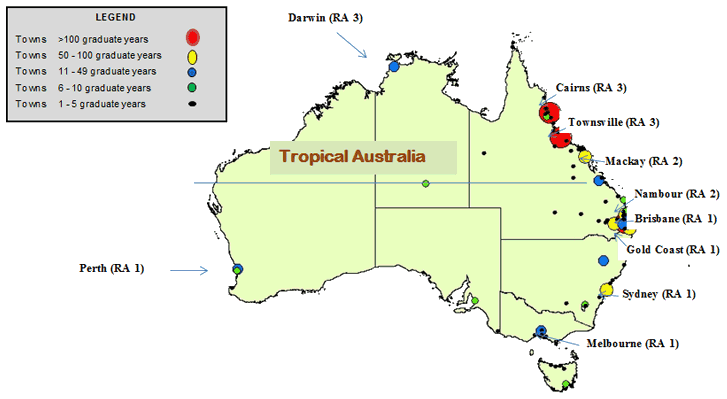
Figure 1: Australian locations of 530 James Cook University medical graduates for most or all of a calendar year, 2006 to 2012. Red dots: Townsville, Cairns and Brisbane; yellow dots: Mackay, Nambour, Gold Coast, Sydney and Toowoomba; blue dots: Rockhampton, Darwin, Perth, Melbourne, Sunshine Coast and Tamworth; green dots: Hobart, Fremantle, Innisfail, Bundaberg, Adelaide, Alice Springs, Hervey Bay and Canberra; Black dots, various smaller towns.
Table 5 summarises the choice of specialty of the first four cohorts (2005-2008 graduates). Only this subset was considered because the other three cohorts were so close to graduation that relatively few had committed to specialty training. Seventy-seven per cent (203/265) of JCU medical graduates who had reached at least PGY 3 were known to have undertaken training in one or more specialties. The most frequent postgraduate specialty training undertaken or completed was general practice (48%; 97/203), including 13% (27/203) who undertook the 'rural medicine' subspecialty. Other popular training choices were Adult Internal Medicine (including subspecialties) at 14% (28/203), surgery (and subspecialties) at 11% (23/203), and both obstetrics and gynaecology (11/203) and paediatrics (10/203) at 5%. Thirty-nine graduates from the first four cohorts had not committed to a specialty, while specialty training data was missing for 23 graduates.
Table 6 and Figure 2 display the number of graduate-years from PGY2-7 that were practised across RA categories. The data shows that graduates having a metropolitan hometown at application and a metropolitan internship practice location are least likely to practise rurally, and that those with a non-metropolitan hometown and a non-metropolitan internship are most likely to practise rurally (RA 3-5). When graduates with a metropolitan hometown and a non-metropolitan internship were compared with graduates from a non-metropolitan hometown and metropolitan internship, the first group were more likely to practise in rural locations (RA 3-5) (OR 6.1 vs 2.6; p<0.001) and in inner regional locations (RA 2) (OR 3.1 vs 1.6, p=0.003).
Table 5: Specialty training undertaken by the first four cohorts of James Cook University MBBS graduates (at least 3 years post-graduation)
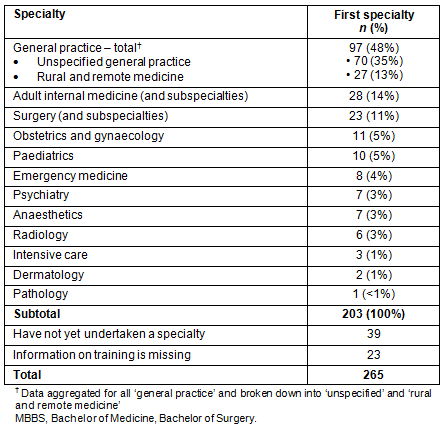
Table 6: James Cook University MBBS graduate practice locations 2006-2012, across ASGC-RA categories (n=442 (6 graduates with missing 'hometown at application' and 2012 interns not included); 1368 graduate-years across postgraduate years 2-7).
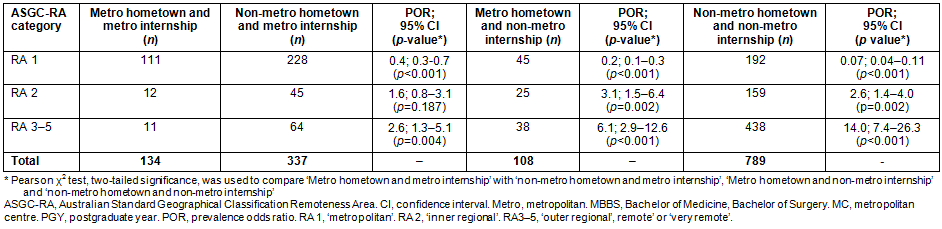
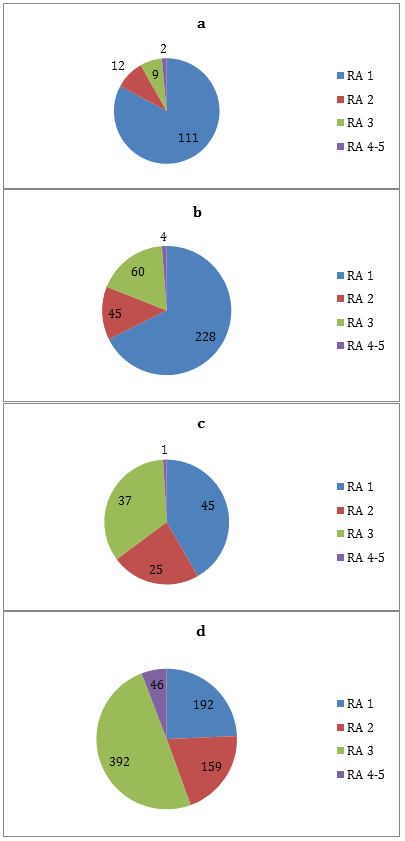
Figure 2: James Cook University medical graduate practice locations 2006-2012, distributed across ASGC-RA categories (n=442; 1368 graduate-years across postgraduate years 2-7) with (a) metropolitan hometown and metropolitan internship; (b) non-metropolitan hometown and metropolitan internship; (c) metropolitan hometown and non-metropolitan internship; (d) non-metropolitan hometown and non-metropolitan internship. RA 1, 'metropolitan'; RA 2, 'inner regional'; RA 3, 'outer regional'; RA 4 or 5, 'remote' or 'very remote'.
Discussion
The data tracking home and practice location up to PGY 7 provide a comprehensive picture of the location of practice of these graduates from 2006 to 2012, and the high response rates enable exploration of the patterns of practice by RA to be conducted with considerable confidence. From 2006 to 2012, two-thirds of JCU MBBS graduates undertook an internship in either inner regional, outer regional or remote locations (RA 2-5) - mostly in northern Australia - with this trend continuing across PGY 2-7. Thus, within 7 years of graduation, JCU graduates are already demonstrating a different pattern of practice to the overall Australian medical workforce. A substantial proportion of JCU graduates are practising in rural and remote (RA 3-5) locations, where there are currently inadequate numbers of clinicians to meet the needs of the population.
With the hometown locations of JCU MBBS graduates demonstrating a different pattern compared to other Australian medical students - fewer JCU graduates from metropolitan areas and more from rural areas - their greater likelihood of practising rurally is consistent with literature that rural background is predictive of future rural practice. Hometown location for JCU graduates demonstrates a different pattern to the general Australian population, reflecting the School's selection policy in favour of rural- and regional-origin applicants. It is not clear from these data why a higher proportion of JCU graduates practise in major cities than come from these areas, although this may be due to postgraduate training opportunities, desire for a lifestyle change (for example, 'different', bigger city experiences), or influence from a partner. However, the 40% of JCU 'graduate-years' in an RA 1 location suggests a different pattern of practice to the 80% of Australian clinicians who practise in major cities.
After PGY 2, around 40% of graduates who have come from a major city choose to practise in a non-metropolitan location, possibly reflecting the influence of the JCU Medical School's regionally-based, decentralized medical program and its rural placement program. By PGY 4-5, JCU graduates were even more likely to work outside a major city if they also undertook their internship outside of a major city. The percentage of JCU graduates practising in remote or very remote locations also increased from PGY 2. However, this dispersion of graduates after several postgraduate years into a range of smaller, more remote communities appears to be largely due to the group of graduates having a non-metropolitan hometown. Relatively few JCU graduates having a metropolitan hometown have ever practised in a remote or very remote location by PGY 7, although a significant proportion (30-40%) practise in RA 2 or 3 in each postgraduate year. This early data supports JCU's emphasis on selecting applicants with a propensity for working rurally, such as those from rural and regional locations, as a strategy to recruit doctors to areas of workforce shortage in northern Australia.
Table 6 and Figure 2 demonstrate an important association between location of internship and subsequent rural practice (RA 3-5). Graduates with a non-metropolitan hometown who also undertook a non-metropolitan internship were, as expected, much more likely to practise rurally than the group having a metropolitan background and metropolitan internship. Interestingly, the group of graduates with a metropolitan hometown/non-metropolitan internship were more likely to practise in non-metropolitan areas (RA 2-5) than the non-metropolitan hometown/metropolitan internship group. The reasons for this finding are unclear, though it is likely some metropolitan students were attracted by the JCU Medical School's rural focus, while others increased their intention to practise rurally over the duration of course, as demonstrated in a previous study11.
Therefore, these early data suggest that JCU is meeting its mission to address local workforce needs by encouraging doctors to practise in northern Australia. While specific reasons for location of practice cannot be determined by this study, they are likely to include prior rural intent of applicants given the mission of the School, the rural focus of the selection process, as well as other factors, such as the School's model of distributed non-metropolitan medical education and the presence of regionally-located internship and specialty training places. Further work is needed to explore the interplay of these issues upon a graduate's decision to practise rurally. However, it does seem clear that the School's evidence-based approach to rural medical education is producing graduates who are demonstrating a different pattern of practice to other Australian graduates, and whose intention to practise rurally has been shown to increase by almost 30% over the duration of the course11. It may be that students who apply to the JCU course, who have a rural background, and/or undertake a non-metropolitan internship, have a prior intent to practise rurally. However, it is important that this potential is realised through programs like JCU, and educational opportunities are provided for students with such 'rural propensity'.
The 48% of the cohort committed to general practice is significantly higher than the 26% of the first cohort of JCU graduates who intended to become a GP at graduation19. This trend, when considered with the rural practice locations of many JCU graduates in PGY 2-5, and the effect of the relatively large group who have not yet committed to a specialty, means it is likely these graduates will have a significant impact on the future medical workforce in northern Australia and other rural areas of Australia.
More work is needed to understand these patterns of practice and reasons for choice of internship location. The School plans to follow these and subsequent cohorts over the next 5-10 years. This early data on actual practice location is encouraging and suggests that the JCU Medical School is meeting its mission to produce graduates able to meet the workforce needs of the region, and of rural and remote Australia. Continuation of these trends will strengthen Australia's rural and regional workforce because the graduating cohort is expected to increase from under 100 to around 200 by 2015, by which time the School expects to have graduated over 1000 doctors. This evidence supports increased investment in rural and regional medical education, including increased rural placements and rural internships, and the targeted selection of students from rural areas, as advocated in the recent Senate Inquiry on factors affecting the supply of health services and medical professionals in rural areas20.
It is imperative that rural, regional and remote Australia benefit from this supply line, and that graduates have access to non-metropolitan training posts, career advice and training pathways. Developing further regionally-located internship and postgraduate specialty training program positions are important strategies in maintaining the workforce 'pipeline' in order to meet the needs of Australia's underserved populations. While understanding reasons for choice of practice location must consider intention, providing regional and rural postgraduate training places is a workforce planning priority. For example, if numbers of non-metropolitan internship places are limited and graduates are unable to undertake internships locally and are forced to move to major cities, then workforce mal-distribution will be exacerbated. This argues the case for an increase in intern places in regional locations, and the implementation of rural initiatives for junior doctors that support their transition into a wide range of vocational careers.
Governments and policy makers have done well to ramp up Australia's rural and remote workforce but more needs to be done both nationally and globally. The 2012 Rendez Vous communiqué21 emphasises this message, recommending that 'the education of health and medical practitioners should be scaled up to provide the needed numbers of practitioners who are likely to work in underserved communities'. The Northern Clinical Training Network (http://www.nctn.net.au) is one example of a horizontally and vertically integrated training pathway that aims to 'join up' the education of senior medical students and junior doctors who share the same workplaces, clinical activities and supervisors. This initiative ensures a seamless transition and a supported pathway into the range of vocational careers that is required to meet the region's needs.
Limitations
While care has been taken to ensure the accuracy of graduate destination data of the JCU Medical School's first seven cohorts, it has been collected from a variety of sources. Data for 85% of students were self-reported, and the additional verification obtained from the AHPRA website was only 90% accurate. The School will continue to follow the first cohorts through to PGY 10 and beyond, when the full workforce impact of the School will be felt as graduate numbers rise.
In addition, the comparison of JCU MBBS graduates and Australian medical students is limited; for JCU graduates, 'hometown' was defined as 'your hometown at application to medical school', while for Australian medical students 'hometown' was defined in the MSOD survey as 'type of location you had lived in the longest'. In addition, while the JCU data relate to graduates from 2005 to 2011, the Australian MSOD data relates only to the entering cohort of 2011, because directly comparable data across these cohorts was not available. Comparison with the Australian clinician data is also limited, as JCU clinician data is only from PGY 1-7, while Australian clinician data is for all years since graduation. For this reason, no statistical tests were applied to these data apart from noting the differing patterns of practice.
The effect of bonded scholarships on practice location was not explored in this study. While over 80% of students (391/473 respondents) did not have any form of scholarship, around 14% (64/473 respondents) had a bonded scholarship. Bonding arrangements only affected a minority of JCU students in this study, but nevertheless may have an important effect that needs to be further investigated.
Conclusions
This paper presents a near-complete data set on the location of practice of the first seven cohorts to graduate from the first of Australia's 'new' medical schools. Graduate outcomes for JCU medical graduates conform to the pattern predicted during the design of the School and previous studies indicating intent to practise7. Higher proportions of JCU MBBS graduates are working in regional, rural and remote locations, in patterns quite distinct from that of the Australian medical workforce overall. While further work is needed to follow the practice locations of these and subsequent cohorts of graduates, this evidence of actual location of practice supports the ongoing development of the JCU model of medical education.
These data suggest the School appears to be meeting its mission to address the health needs of northern Australia by producing graduates who are choosing to practise in non-metropolitan locations. The findings raise the possibility that the impact of the School on the regional, rural and remote workforce could further increase if more internship places and postgraduate training opportunities were available outside of metropolitan centres. In particular, this association between non-metropolitan internship and subsequent non-metropolitan practice is striking. While the explanation may include a range of factors including prior intent, these strategies may have significant implications for workforce planning.
The evidence provided in this study supports the current investment in rural and regional training, and argues for increased levels of funding and support for regional and rural medical education together with increased development of non-metropolitan postgraduate training pathways in a range of generalist specialties.
Acknowledgements
The authors would like to gratefully acknowledge the cooperation of all JCU medical graduates who consented to be contacted for this longitudinal study.
References
1. Australian Medical Workforce Advisory Committee (AMWAC). Influences on participation in the Australian medical workforce. Report 4, Sydney, NSW: AMWAC, 1998.
2. Department of Health and Ageing. Review of the rural medical workforce distribution programs and policies. Canberra, ACT: Deloitte Access Economics, 2011.
3. Hays RB. A new medical school for regional Australia. Medical Journal of Australia 2000; 172(8): 362-363.
4. Hunt DD, Norris T, Ballweg R. The University of Washington WAMI program: 25 years of experience with manpower shortages in rural areas. Australian Journal of Rural Health 1995; 3: 152-158.
5. Rolfe IE, O'Connell DL, Pearson SA, Dickinson JA. Finding solutions to the rural doctor shortage: the roles of selection versus undergraduate medical education at Newcastle. Australian and New Zealand Journal of Medicine 1995; 25: 512-517.
6. Rabinowitz HK, Diamond JJ, Hojat M, Hazelwood CE. Demographic, educational and economic factors related to recruitment and retention of physicians in rural Pennsylvania. The Journal of Rural Health 1999; 15: 212-218.
7. Hays RB. Rural initiatives at the JCU School of Medicine: a vertically integrated regional/rural/remote medical education provider. Australian Journal of Rural Health 2001; 9(Suppl): S2-5.
8. McDonald J, Bibby L, Carroll S. Recruiting and retaining general practitioners in rural areas: improving outcomes through evidence-based research and community capacity building. Evidence-based review: final report. Ballarat, VIC: Centre for Health Research and Practice, University of Ballarat, 2002.
9. Tesson G, Curran V, Pong RW, Strasser R. Advances in rural medical education in three countries: Canada, The United States and Australia. Education for Health 2005 18(3): 405-415.
10. Lee YH, Barnard A, Owen C. Initial evaluation of rural programs at the Australian National University: understanding the effects of rural programs on intentions for rural and remote medical practice. Rural and Remote Health 11: 1602. (Online) 2011. Available: www.rrh.org.au (Accessed 7 November 2011).
11. Sen Gupta T, Murray R, Hays R, Woolley T. Rural medical education promotes rural medical career intentions and internship choices: a comparative outcome survey of a regional Australian medical school. Rural and Remote Health 13: 2313. (Online). 2013. Available: www.rrh.org.au (Accessed 4 February 2014).
12. Azer SA, Simmons D, Elliott S. Rural training and the state of rural health services: effect of rural background on the perception and attitude of first-year medical students at the University of Melbourne. Australian Journal of Rural Health 2001; 9(4): 178-185.
13. Somers GT, Spencer RJ. Nature or nurture: the effect of undergraduate rural clinical rotations on pre-existent rural career choice likelihood as measured by the SOMERS Index. Australian Journal of Rural Health 2012; 20: 80-87.
14. Eley DS, Zhang J, Wilkinson D. Self-sufficiency in intern supply: the impact of expanded medical schools in Queensland. Australian Health Review 2009; 33: 472-477.
15. Dunbabin J, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3(1): 212. (Online) 2003. Available: www.rrh.org.au (Accessed 7 November 2011).
16. Hubraq H. National data on medical students commencing in 2011. Available: http://www.medicaldeans.org.au/wp-content/uploads/2011-CMSQ-National.pdf) (Accessed 24 November 2012).
17. Australian Bureau of Statistics. ASGC Remoteness Classification: purpose and use. Census paper # 03/01. Canberra, ACT: Commonwealth of Australia, 2003.
18. Woolf B. On estimating the relation between blood group and disease. Annals of Human Genetics 1955; 19: 251-253.
19. Veitch C, Underhill A, Hays RB. The career aspirations and relocation intentions of James Cook University's first cohort of medical students: a longitudinal study at course entry and graduation. Rural and Remote Health 6: 537. (Online) 2006. Available: www.rrh.org.au (Accessed 2 December 2011).
20. Senate Standing Committees on Community Affairs. The factors affecting the supply of health services and medical professionals in rural areas. Greater Sudbury, ON: Northern Ontario School of Medicine, 2011.
21. Rendez Vous. Draft recommendations. Communiqué. (Online) 2012. Available: http://www.rendez-vous2012.ca/wp-content/uploads/2012/11/TBCommunique-web2.pdf (Accessed 13 April 2013).













