As in many countries, consumers in Australia have recently had to accommodate increases in the costs of basic food1. During the financial year 2007-2008, overall food prices rose 3.9%, while some basic food prices rose more sharply: cheese by 14.2%, milk by 12.1%, poultry by 11.0% and bread by 6.8%2. Food cost plays a significant role in mediating food choice among low socio-economic status (SES) groups1,3, who often have to reduce food spending to allow for other essentials such as housing and utilities4-7, leading to decreased food security8. The literature on food access indicates that people from low income backgrounds experience higher rates of food insecurity9 and obesity10,11, and studies have found that affordability is a primary reason given for not choosing healthy foods12,13. Thus, the assessment of food cost and affordability are essential steps in better understanding individual and community food choices.
Food costs entered the political limelight prior to the Australian 2007 federal election, with voters demanding government action to reduce prices. To honour pre-election promises, the newly elected Labor government initiated a national inquiry into grocery pricing soon after taking office. However, following the release of the grocery pricing inquiry report14 and the consequent launch of the government website to monitor prices15, critics considered there would be minimal if any impact on prices16,17. This is partly because of international trends, with Australia not immune to global factors attributed to raising the costs of basic foods18, and partly because the inquiry outcomes did nothing to address food costs.
To be food secure means to have regular access to safe, nutritionally adequate, culturally acceptable food from non-emergency sources. Food insecurity, then, describes a limited or uncertain ability to acquire appropriate foods in socially acceptable ways. This is not merely a lack of food, but occurs when people fear running out of food, or are forced to make significant changes to their usual eating patterns due to economic constraints19. The diets of those who are food insecure are likely to lack variety and be of poor quality with lower levels of micronutrients20-23.
There is some evidence to demonstrate that populations living in rural areas of Australia have to pay more for healthy food than their metropolitan ('metro') counterparts24. The Healthy Food Basket (HFB) survey conducted in Queensland demonstrated higher food costs in rural and remote parts of the state25. In South Australia (SA) a study conducted by Mediniya et al demonstrated that food costs were higher in remote areas of that state26. However, Burns et al in a survey of 42 rural towns in Victoria could find no difference in the cost of a HFB according to rurality, nor did the mean cost of the rural Victorian HFB differ significantly from a basket priced in state capital Melbourne27. However the availability of the complete HFB was variable, especially for fruit and vegetables.
Such research is very important in terms of highlighting areas for policy responses to reduce food costs (especially healthy food) in rural areas. However, it does not take into account the additional impact of SES, whereby healthy food in rural areas may be less affordable for low SES, as compared to high SES, families, thereby requiring policy action to address both the geographical and socio-economic inequities in access to healthy food. The current study does this by presenting data on both the cost and affordability of healthy food in rural compared with metro SA.
A recent publication of the present authors examined the cost and affordability of healthy food across metro Adelaide, showing for the first time that healthy food is much less affordable for lower income families and for those receiving welfare payments when compared with higher income families28. The present publication adds to the existing literature by examining the relative effects of both rurality and SES on the affordability of healthy food.
Assessing the cost of healthy food
In Australia, the HFB is a tool commonly used to measure the cost and availability of healthy food. Although there is no national HFB, there are several HFBs which have been developed in different Australian states and territories25,29-31. The common features of these and other HFB tools are that only one reference family is used in calculating cost and affordability, and the nutrient requirements are based on Recommended Dietary Intakes (RDI)32.
Recently the Victorian Healthy Food Basket (VHFB) was developed by Palermo and Wilson33. The advantages of the VHFB over other HFB methods is that it uses four distinct types of reference families: (i) 'Typical family' (44-year-old male and female, 18-year-old female, 8-year-old male); (ii) 'Single parent family' (44-year-old female, 18-year-old female, eight-year-old male); (iii) 'Elderly pensioner' (71-year-old female); and (iv) 'Single adult' (adult male >31 years). Thus the VHFB provides a useful way of comparing food costs and affordability across different family types.
The VHFB also uses Nutrient Reference Values (NRVs), released in 2006 to replace the 1991 RDIs, to assess nutritional adequacy, and aims to meet greater than 80% of an individual's nutrient requirements, and at least 95% of the energy requirements for all reference families. The basket consists of 44 food items from 5 core food groups (cereals, vegetables and legumes, fruit, meat and alternatives, and dairy) and one non-core food group. The choice of food items is based on the Australian Guide to Healthy Eating34 and has been further modified using data from the 2003-2004 Australian Household expenditure survey. Finally, field trials have confirmed the usefulness of the VHFB24.
This article presents key findings from a study on the cost and affordability of a HFB in selected parts of rural SA.
A detailed account of the present authors' methods for conducting the HFB survey in metro Adelaide has been published previously28, and therefore a more concise version is provided here, alongside the specific components of the former methods used in work undertaken in rural SA. Overall, the study involved a HFB survey in 14 localities across rural SA. A choice was made not to undertake the study in remote areas of SA, due to the sparse populations.
Choice of locations of food stores
This study compared and contrasted cost and affordability of a HFB in rural areas of high and low remoteness (distance from nearest large town) and areas of high and low household income. In so doing use was made of available indices of rurality and of SES. The Accessibility/Remoteness Indexes of Australia (ARIA) and Socio-Economic Indexes for Areas (SEIFA) were used to obtain information on the 'remoteness' and SES of all rural towns in SA. All rural towns were then ranked on the basis of both remoteness and SES, according to high or low SES and high or low remoteness. From this ranking, 4 typologies were identified within which were sampled - 'more remote' and 'low SES'; 'more remote' and 'high SES'; 'less remote' and 'low SES'; and 'less remote' and high SES'. Within each typology, 2 or 3 rural towns were identified; within each town, the main food stores were identified, which were usually supermarkets (including Woolworths, Coles, IGA, Foodland and large general stores). In some towns there was only one supermarket while others had two. The final sample included 10 rural towns and 14 supermarkets (6 towns had 1 supermarket, and 4 towns had 2 supermarkets). In terms of ranges of remoteness scores, the locations deemed 'more remote' had ARIA scores ranging from 6.13 to 10.23 and those deemed 'less remote' had scores ranging from 0.74 to 0.91. In terms of ranges of SES, the locations deemed 'high SES' had SEIFA scores ranging from 925 to 1075 and those deemed 'low SES' had scores ranging from 887 to 912.
Conducting the survey
Data collectors who were dietitians working in rural settings were trained in use of the tools. On the day of the survey, a letter of introduction was presented to the owners of the specialty shops and/or managers of supermarkets prior to conducting each survey. The letter emphasised confidentiality and gave an assurance that no individual store would be identified.
All data for the project were collected between May and June 2010, minimising seasonal variation in the price and quality of foods, especially fresh fruit and vegetables. In addition, the training and pilot test ensured that all data collectors could record the data accurately, according to specified instructions.
Product selection
The selection of products for the HFB was based on the protocol for the VHFB33,35. Products were recorded according to the cheapest brand price in specified sizes of the food items listed in the HFB. When the specified size was not available, the next smallest size was chosen. If this was not available, then the next largest size was selected. In order to provide the cheapest but realistic and comparable HFB, generic brands were not chosen. Where a brand name was specified, only that brand of product was assessed. Finally, the regular price of items was used instead of discounted or 'special' prices to reflect the standard cost of the HFB.
Assessment of cost and affordability
Cost of the VHFB was calculated for each type of reference family, as described in the VHFB survey. Affordability of the HFB was assessed as proportion of household income need to be spent on the HFB. Two kinds of income were used to measure affordability. The first was based on government welfare payments for unemployed families, while the second was based on average Equivalised Disposable Household Income (EDHI) for highest and lowest tertiles for SA 2005-200636, which was adjusted to current values using Labour Price Index37 rises since 2005-2006 (a detailed description of the EDHI calculation was provided in a previous publication of the authors28).
Data analysis
The data were analysed using SPSS v17.0 for Windows (www.spss.com). Cost and affordability of the HFB were calculated for each reference family. Mean (standard error of the mean: mean [SE]) costs were compared between supermarkets in high- and low-income areas using the t-test. Affordability was calculated as a mean (SE) for high- and low-EDHI, assuming that high-EDHI families shopped in high-income household income areas and vice versa. Affordability for families receiving welfare payments was calculated as cost of the HFB as a proportion of income mean (SE) for each family type. The quality of foods was calculated as a mean (SE) quality score, and assessed across high- and low-income areas using the t-test. Food promotions were assessed as the proportion of core and non-core food promotions in selected store areas. Significance was taken as p ≤0.05.
All analyses of affordability were undertaken using data on EDHI and welfare payments. Data on the HFB for metro areas were collected in 2009, and therefore prior to this analysis, a Consumer Price Index (CPI) of 2.8% was applied to the cost of the metro HFBs to align them with 2010 data for the rural HFB (collected in 2010).
The results are presented at two levels. First, the cost and affordability of the HFB are compared between metro and rural areas. Second, the cost and affordability are compared between towns within rural SA.
Cost and affordability of the healthy food basket between metropolitan and rural areas in South Australia
Data on the difference in the costs of the HFB between metro and rural areas is presented for each of the reference families (Table 1). The analyses reveal higher costs of the HFB in rural areas, which are statistically significant for all reference families. For example, a 'typical family' in a rural area would need to spend approximately AU$24 per fortnight more in order to buy a HFB than a similar family in a metro area. In addition, the standard errors are wider in rural areas, indicating a wider variability in costs (in addition to smaller sample sizes).
The affordability of the HFBs in metro and rural areas was compared (Table 2). The HFBs were slightly less affordable in rural areas, although there were no statistically significant difference for any of the reference families.
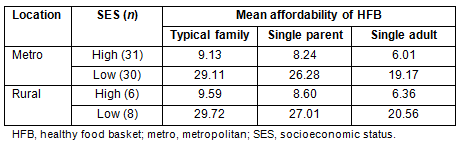
The affordability of the HFB between high and low SES areas in and between both metro and rural areas was compared (Table 3). There was no statistically significant difference between metro and rural areas (Table 2), and this was consistent between high and low SES areas (Table 3). For example, a 'typical family' in a metro high income area would need to spend 9.13% of the EDHI and a similar family in a rural high SES area would need to spend 9.59% of their EDHI. Obviously, the large and important (and statistically significant, p <0.0001) difference in affordability is between high and low SES areas, irrespective of whether they are in metro or rural areas.
Table 1: Mean cost of the healthy food basket (SE) between metro and rural areas for
reference families by Equivalised Disposable Household Income (EDHI) of areas
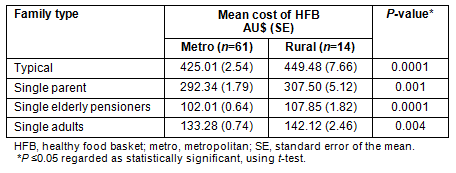
Table 2: Mean percentage (SE) of Equivalised Disposable Household Income (EDHI) spent by family
type on HFB from supermarkets in high and low household income areas
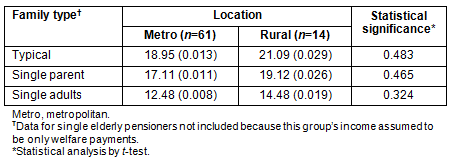
Table 3: Mean percentage of Equivalised Disposable Household Income (EDHI) spent
by family type on the healthy food basket from supermarkets in
high and low household income areas in both metro and rural areas
Cost and affordability of the healthy food basket within rural South Australia
Data are presented for the 14 supermarkets surveyed in rural SA (Table 4). Supermarkets were classified as either 'more remote' or 'less remote' on the basis of their ARIA score, and this was deemed important because this study concerns the affect of geographical proximity to (or remoteness from) service centres within rural SA. Analysis revealed that the HFB was more expensive in 'more remote' locations for every reference family, with a 'typical family' paying $21 per fortnight more for a HFB than a similar family in a less remote (but still rural) area. None of the differences in cost were statistically significant, probably due to the relatively low number of supermarkets in the sample.
Data are presented on a comparison of the affordability of the HFB between 'More Remote' and 'Less Remote' areas (Table 5). There were no statistically significant differences, with families in both More and Less Remote areas needing to pay similar proportions of their EDHI for a HFB..
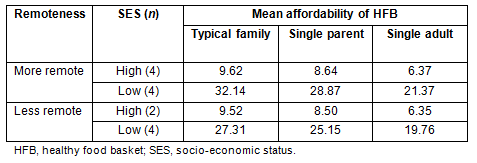
Descriptive data are presented on a comparison of the affordability of the HFB in high and low SES areas in both 'more remote' and 'less remote' areas of Rural SA (Table 6). Due to low numbers, no statistical inferences can be made from this data, although it of note that the least affordable HFB was for a low SES 'typical family' in a 'more remote' area, who would need to spend around 32% of their EDHI in order to buy a HFB. A similar low SES family in a less remote area would need to spend around 27% of their EDHI. While low SES families in 'more remote' areas appear to be at a disadvantage compared with similar low SES families in 'less remote' areas, the obvious disparity is between high and low SES families, irrespective of geographical location.
Table 4: Mean cost of the healthy food basket (SE) between 'More Remote' and
'Less Remote' areas in rural South Australia for reference families by
Equivalised Disposable Household Income (EDHI) of areas
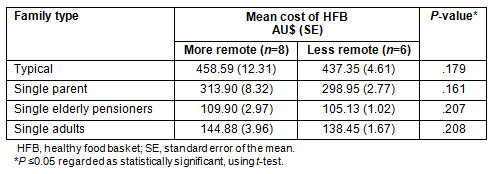
Table 5: Mean percentage (SE) of Equivalised Disposable Household Income (EDHI) spent by
family type on HFB from supermarkets in 'More Remote' and 'Less Remote' areas in rural South Australia
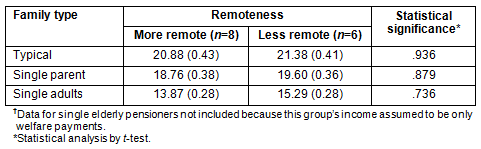
Table 6: Mean percentage of Equivalised Disposable Household Income (EDHI) spent by family type
on HFB from supermarkets in high and low household income areas in both 'More Remote' and
'Less Remote' areas of rural South Australia
Summary of costs and affordability of the healthy food basket across South Australia
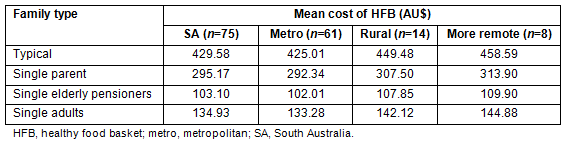
A descriptive summary of the costs of the HFB is provided for different geographical areas across SA (Table 7), revealing the increasing cost of the HFB as one moves from metro to rural, and then within rural SA, to 'more remote' areas. This increase in cost is consistent for all reference families. For example, for a 'typical family', the mean cost of the HFB across SA was approximately $430 per fortnight, although it was only $425 in metro areas, but it was almost $450 in rural areas and almost $460 in the more remote areas. The difference between metro and the 'more remote' areas is approximately $35 per fortnight, or $780 per year. This extra cost does not include the costs incurred in travelling further distances to the supermarkets, in terms of both 'real costs' (petrol, depreciation of car etc) and 'opportunity costs' (ie the things that could have been achieved which had to be foregone in order to travel for food shopping).
Table 7: Summary of costs of the healthy food basket across geographical areas in South Australia for reference families
Discussion
The data reported presents analyses of the price and affordability of the HFB comparing metro (n=61) with rural (n=14) areas of SA. Within the rural areas, the analysis also compared 'more remote' (n=8) with 'less remote' (n=6) areas. Analyses were also undertaken which compare the highest and lowest SES tertiles, which addresses the question: are healthy foods less affordable in lower SES areas?
In terms of cost, there were statistically significant differences between metro and rural areas, with healthy food being more expensive in rural areas, which mirrors earlier findings in SA26. This has obvious implications in terms of both poor nutritional intake and obesity rates in rural areas. People in rural areas have to travel further to obtain their food, and therefore when the increased travel costs (time, fuel, wear of vehicles) are added to the increased food costs, the situation is even worse for people in rural areas. The cost of the HFB was even higher in the 'more remote' areas, although the sample sizes were too small to undertake statistical analyses. Nevertheless, the findings indicate an even worse situation for people living further away from rural service centres.
In terms of affordability, there was no statistically significant difference between metro and rural areas. The main difference in terms of affordability is in relation to SES, with people and families in lower SES areas (both metro and rural) required to spend, on average, an approximately 3 times higher proportion of their income than those in higher SES areas. Therefore the major implication here, much like the authors' previous analyses of the metro HFB data28, relates to addressing the problem of the relative unaffordability of healthy food, or 'food stress', in lower SES areas. This discussion argues that 'food stress' occurs when food costs account for 25% or more of household income, which is an issue for low income rural and metro families. Food pricing shapes dietary choices, especially for low income households and as food is generally regarded as the only essential expense that can be easily modified, rising food prices and choices these necessitate may lead to a negative impact on health and wellbeing.
Steps need to be taken to address the problem of higher food costs in rural areas and lack of affordability for people in lower SES areas (in both metro and rural areas) because these areas also have higher levels of overweight and obesity. While it was not possible to measure a causal pathway, it could well be the case that people in rural and/or lower SES areas cannot afford to eat healthily (as defined by the HFB) and therefore are forced to eat cheaper food (often high fat, high density) which leads to higher levels of obesity in these groups. Any attempts at behavioural interventions and social marketing to increase 'healthy eating' and reduce overweight/obesity in these population groups need to recognise these structural and financial impediments, which must be addressed before a more equitable distribution of healthy eating and a reduction in overweight/obesity is possible. In addition, an opportunity exists for policy makers in SA to monitor food affordability longitudinally by implementing the methodology used within this study as a form of on-going surveillance. In order to reduce obesity, it is imperative to tackle not only the manifestations of obesity, but also the forces that shape it. The environmental determinants of obesity remain poorly understood and under researched, while some policy responses drift towards individual responsibility. The collection and monitoring of food affordability data would provide valuable information to inform the design of broader structural policy responses.
Limitations
It is important to remember that the foods in the HFB used in this South Australian study, and in other studies elsewhere in Australia, do not reflect what people are actually eating or spending on food. This is a hypothetical 'basket' that represents the food required to cook healthy meals for different family types. In addition, the sample of shopping outlets in rural SA was limited to 14 and, therefore, care needs to be taken when attempting to generalise. For example, food outlets in more remote areas of SA or in Aboriginal communities were not sampled. A further limitation of these 'one-off' HFB studies relates to the fluctuation of fresh food prices during the year, according to season and supply. A single time-point measurement may not represent the average price of these food items, even though the specific items included in the HFB are generally available all year round. Therefore, an important implication to arise out of the study is the need to construct a reliable monitoring system for the HFB to assist in assessing the affordability of healthy food. In order to achieve such an aim, longitudinal measurement of the HFB would be required.
Overall, the present study found that the cost of healthy food was statistically significantly higher in rural SA when compared with Metro Adelaide. The cost of healthy food in 'more remote' areas of SA was even higher, although sample sizes were too small to reach statistical significance. Healthy food is slightly less affordable in rural SA compared with Metro Adelaide, although this difference was not statistically significant. However, there was a large and statistically significant difference in the affordability of healthy food on the basis of SES, with healthy food being much less affordable for low SES families. Therefore, these findings suggest the need to consider both rurality and SES when developing policy responses to decrease the cost and increase the affordability of health food in rural and remote areas.
References
1. Harrison M, Coyne T, Lee AJ, Leonard D, Lowson S, Groos A et al. The increasing cost of the basic foods required to promote health in Queensland. Medical Journal of Australia 2007; 186(1): 9-14.
2. Australian Bureau of Statistics. Consumer price index Australia: June quarter 2008. Canberra, ACT: ABS, 2008.
3. Turrell G, Hewitt B, Patterson C, Oldenburg B, Gould T. Socioeconomic differences in food purchasing behaviour and suggested implications for diet-related health promotion. Journal of Human Nutrition and Dietetics 2002; 15: 355-364.
4. Booth S, Smith A. Food security and poverty in Australia - challenges for dietitians. Australian Journal of Nutrition and Dietetics 2001; 58(3): 150-156.
5. Wrigley N, Warm D, Margetts B, Lowe M. The Leeds "food deserts" intervention study: What the focus groups reveal. International Journal of Retail & Distribution Management 2004; 32(2): 123-136.
6. Kirkpatrick S, Tarasuk V. Adequacy of food spending is related to housing expenditures among lower-income Canadian households. Public Health Nutrition 2007; 10: 1464-1473.
7. Douglas J. Food Insecurity in Northern Adelaide. In: SACOSS News. Adelaide, SA: SACOSS, 2006.
8. Law I, Ward P, Coveney J. Food insecurity in South Australian single parents: a livelihoods framework approach. Critical Public Health 2011. Available: http://www.tandfonline.com/toc/ccph20/current (Accessed 8 March 2012).
9. Foley W, Ward P, Carter P, Coveney J, Tsourtos G, Taylor A. An ecological analysis of factors associated with food insecurity in South Australia 2002-7. Public Health Nutrition 2010; 13: 215-221.
10. Wardle J. Sex differences in association with SES and obesity American Journal of Public Health 2002; 92: 1299-1304.
11. Paeratakul S, Lovejoy J, Ryan D, Bray G. The relation of gender, race and socioeconomic status to obesity and obesity comorbidities in a sample of US adults. International Journal of Obesity 2002; 26(9): 1205-1210.
12. Inglis V, Ball K, Crawford J. Socioeconomic variations in women's diets: what is the role of perceptions of the local food environment? Journal of Epidemiology & Community Health 2008; 62: 191-197.
13. Foley R, Pollard C, McGuiness D. Food Cent$: achieving a balanced diet on a limited food budget. Nutrition and Dietetics 1997; 54(4): 167-172.
14. Commonwealth of Australia. Report of the ACCC inquiry into the competitiveness of retail prices for standard groceries. Canberra, ACT: Australian Competition and Consumer Commission, 2008.
15. Commonwealth of Australia. GROCERYchoice. Canberra, ACT: Australian Competition and Consumer Commission, 2008.
16. Dodds K. Government in a spin while Australian retailing comes up trumps - Retail response to ACCC Grocery Prices Inquiry Get Farming. (Online) 2008. Available: http://www.retail.org.au/index.php/articles/Government_in_a_spin_while_Australian_retailing_comes_up_trumps__-_Retail_response_to_ACCC_Grocery_Prices_Inquiry_ (Accessed 2 March 2012).
17. Irvine J. Rudd price check: he's powerless. Sydney Morning Herald, 6 August 2008. Available: http://www.smh.com.au/.
18. Stoeckel A. High food prices: Causes, implications and solutions. In: Rural Industries Research and Development Corporation. Canberra, ACT: Australian Government, 2008.
19. Burns C. A review of the literature describing the link between poverty, food insecurity and obesity with specific reference to Australia. Melbourne, VIC: VicHealth, 2004.
20. NSW Centre for Public Health Nutrition. A planning framework and menu of options for policy and practice interventions. Food Security Options Paper. Sydney, NSW: NSW Department of Health & The University of Sydney, 2003; 1-104.
21. Champagne CM, Casey PH, Connell CL, Stuff JE, Gossett JM, Harsha DW et al. Poverty and Food Intake in Rural America: Diet Quality Is Lower in Food Insecure Adults in the Mississippi Delta. Journal of the American Dietetic Association 2007; 107(11): 1886-1894.
22. Tarasuk V, McIntyre L, Li J. Low-Income Women's Dietary Intakes Are Sensitive to the Depletion of Household Resources in One Month1-3. The Journal of Nutrition 2007; 137(8): 1980-1987.
23. Hamelin AM, Beaudry M, Habicht JP. Characterization of household food insecurity in Quebec: food and feelings. Social Science and Medicine 2002; 54: 119-132.
24. Palermo C, Walker K, Hill P, McDonald J. The cost of healthy food in rural Victoria. Rural and Remote Health 8(4): 1074. (Online) 2008. Available www.rrh.org.au (Accessed 15 February 2012).
25. Queensland Health. The 2000 Healthy Food Access Basket (HFAB) survey: Full Report. Brisbane, QLD: Queensland Government, 2001.
26. Meedeniya J, Smith A, Carter P. Food Supply in Rural South Australia: A Survey on Food Cost, Quality and Variety. Adelaide, SA: South Australian Government, 2000.
27. Burns C, Gibbon P, Boak R, Baudinette S, Dunbar J. Food cost and availability in a rural setting in Australia. Rural and Remote Health 4: 311. (Online) 2004. Available www.rrh.org.au (Accessed 15 February 2012).
28. Wong K, Coveney J, Ward P, Muller R, Carter P, Verity F et al. Availability, affordability and quality of a healthy food basket in Adelaide, South Australia. Nutrition and Dietetics 2011; 68: 8-14.
29. Tsang A, Ndungu M, Coveney J, Dwyer L. The Adelaide Healthy Food Basket: a survey on food cost, affordability and availability in five Local Government Areas in metropolitan Adelaide. Nutrition and Dietetics 2007; 64(4): 241-247.
30. Williams P, James J, Kwan J. The Illawarra Healthy Food Price Index 2: Pricing methods and index trends from 2000-2003. Nutrition and Dietetics 2004; 61(4): 208-214.
31. Williams P, Reid M, Reid M, Shaw K. The Illawarra Healthy Food Price Index 1: development of the food basket. Nutrition and Dietetics 2004; 61(4): 200-207.
32. National Health and Medical Research Council. Recommended Dietary Intakes for Use in Australia. Canberra, ACT: NHMRC, 1991.
33. Palermo C, Wilson A. Development of a healthy food basket for Victoria. Australian & New Zealand Journal of Public Health 2007; 31(4): 360-363.
34. Kellett E, Alison S, Schmerlaib, Y. Australian Guide to Healthy Eating. Canberra, ACT: Deptartment of Health and Family Services,1998.
35. O'Dwyer L, Coveney J. Scoping supermarket availability and accessibility by socioeconomic status in Adelaide. Health Promotion Journal of Australia 2006; 17: 240-246.
36. Australian Bureau of Statistics. Household Income and Income Distribution, Australia, 2005-06. Canberra, ACT: ABS, 2007.
37. Australian Bureau of Statistics. Labour Price Index - March Quarter 2009. Canberra, ACT: ABS, 2009.

