Prostate and female breast cancer are the leading cancer diagnoses in Queensland, Australia, accounting for 30% and 28% of all cancer diagnoses, respectively1. Despite promising 5-year survival rates of 94% for prostate cancer and 87% for breast cancer, these diagnoses account for the second highest mortality rates from cancer1,2. Of the treatment options available, radiation therapy (RT) is a recommended treatment modality for eligible patients, yielding radical treatment control as well as palliative disease management3. RT involves treatment of the planning target volume with fractionated daily doses of radiation, delivered over weeks. For prostate and breast cancer patients, treatment can take 4-9 weeks to achieve the prescribed dose4,5. Due to the specific quality control and specialised care measures required, the clinics are located largely in major cities or regional areas, restricting geographical access for many, particularly those residing in rural areas6-9.
Recent studies in Australia and Canada have determined that utilisation rates of RT are sub-optimal compared with best practice benchmarks3,10. In 2002, a Radiation Oncology Inquiry was put forth in the Australian Department of Health to improve the provision of these services. However, providing infrastructure is only part of the equation, and it is known that patient factors and referral patterns from doctors and influence the decision to undergo RT3,6,10,11. Several factors have been identified that impact a patient's choice to undergo radiation therapy (box 1). Interestingly, not all factors influence patients in the same manner, and thus findings are contextually sensitive and this area of research is quite unique to the geography and patient base in question12.
An underlying issue remains the physical accessibility of the clinic in terms of distance to the radiation facility7,8,12,13. Access to quality cancer care is fundamental in the management of prostate and breast cancer; but given the dispersed geography of North Queensland (NQ), distance can prove a barrier to receipt of crucial treatment. The northern aspect of Queensland has two major cities, Townsville and Cairns, which lie approximately 1350 km and 1700 km north of the capital city of Brisbane, respectively. NQ extends north from Mackay through Far North Queensland to the Torres Strait on the north-eastern border of Australia and hosts a population of nearly 507 000 people in regional and rural areas14,15. For decades, The Townsville Hospital (TTH) served as the only therapeutic clinic for radiation treatments north of Brisbane, leaving 10.8% of patients to travel more than 6 hours to the treatment facility2. Between 1 July 2010 and 30 June 2011, the clinic served 150 prostate and 246 breast cancer patients14,16.
In July 2011, the Liz Plummer Cancer Centre in Cairns opened its doors to Radiation Oncology Queensland (ROQ) and a second radiotherapy facility commenced treating patients, potentially increasing access to RT. Little is known about the effect of opening this additional centre in terms of patient access and patient volume per clinic. Several studies have been conducted in North America investigating the distance travelled to radiotherapy, unanimously concluding that distance plays a major role in utilisation of RT; however, these studies are not directly applicable to NQ3,6-9.
With its tropical climate, pronounced wet season and vast land area, compounded by scant health facilities and limited public transport, NQ has geographical barriers warranting investigation12. This study aimed to investigate and map the distance travelled in kilometres to the nearest radiation therapy facility in NQ for all prostate and female breast cancer patients who sought RT between 1 July 2010 and 30 June 2013 and the effect of opening another RT facility in Cairns on average travel distance, commute time and attendance numbers in NQ. The authors hypothesised that there would be an increase in overall number of patients attending for RT and a decrease in average distance and time travelled for patients attending RT following inception of the facility in Cairns.

Box 1: Factors identified to influence access to radiation therapy5-8,10,17-23
This retrospective descriptive study used de-identified patient records to address the research questions. All patients diagnosed with prostate or female breast cancer identified between 1 July 2010 and 30 June 2013 in TTH or ROQ radiation oncology databases, residing in NQ or Far North Queensland and having completed radiotherapy treatment within that time parameter at TTH or ROQ Cairns were included. Prostate and female breast cancer were chosen because they are the most common cancer diagnoses for males and females in Queensland, respectively, and both treatment regimens are offered at these radiation oncology services. Exclusion criteria included males with breast cancer and those who travelled by aeroplane.
Data extracted included age, gender, Aboriginal and Torres Strait Islander status, year of treatment, cancer site, treatment received, residential address and the clinic visited. Data were collated into a Microsoft Excel spreadsheet. Address data were geocoded and reconfirmed using Aus-emaps.com and Google Maps by assigning coordinates of latitude and longitude for the patient's residential origin. A total of four individual patient geocodes were excluded, one from 2011-2012 and three from 2012-2013 data because the travel routes required air travel. Ten geocodes over the three time periods had to be approximated to the nearest identifiable geocode because Google Maps could not identify the location of the geocode, most likely due to rurality. The radiotherapy facilities were similarly geocoded and road distance between them calculated. Road travel time was approximated using Google Maps road directions for each year. The shortest travel time was selected for the distance based on the patient's geocode and the hospital visited for treatment by vehicle. Private motor vehicle transport was selected to compare road travel time consistently. The travel time selected accounted for traffic conditions to simulate realistic conditions; however, this time deviated by only 1-3 minutes from those without traffic conditions. This did not take into account additional delays due to construction, nor did it account for those who used alternate methods of transport including public transport, walking or flights from Cairns, Mackay, Mount Isa, Rockhampton or Bundaberg. Geographic data were collated for storage, management, retrieval and analysis using a geographic information system (ArcGIS v10.1; ESRI Corporation; http://www.esri.com). In the maps, buffers of 50 km, 100 km, 200 km and 400 km were placed around each treatment facility to illustrate the catchment zones of the RT clinics. By utilising GIS, the authors were able to calculate and display several layers of information to illustrate the data for each year18,24.
Statistical analysis
Information was analysed in both graphical and tabular format. Patient origin both before and after the opening of the Cairns RT unit was illustrated graphically using ArcGIS maps.
Distance to treatment was calculated for each patient and then bivariate analyses were performed for variations in distance to treatment by centre attended, time period, age, gender, and Aboriginal and Torres Strait Islander status. In addition, median road travel time and distance were calculated for all patients for the three time intervals post-opening to investigate the effect of opening a second clinic.
Data revealed a non-parametric distribution. Median and interquartile ranges are reported for the data. The Mann-Whitney U-test was used to compare age, distance and time between Townsville and Cairns, and the Kruskal-Wallis test was used for analysis involving more than two groups. Chi-squared analysis for trend of proportions was used to determine the association between distance travelled for each corresponding year for Townsville and Cairns. Statistical Software for the Social Sciences v22 (SPSS Inc.; http://www.spss.com) was used for performing the analysis, and p<0.05 was considered statistically significant.
Ethics approval
Ethics approval was granted by the Human Research Ethics Committee (HREC), Darling Downs Hospital and Health Service (HREC/13/QTDD/25) and James Cook University, with site-specific assessment approval for this study conducted at both the Townsville Hospital and ROQ Cairns.
During the 3-year study period a total of 1423 patients underwent radiotherapy; 587 prostate cancer patients and 836 female breast cancer patients were treated, respectively. A total of 1110 patients were treated at TTH and 313 patients treated at ROQ in Cairns (Fig1). In terms of utilisation, 396 prostate and female breast cancer patients were treated with RT in 2010-2011, which increased to 471 in 2011-2012, and finally to 556 in 2012-2013, generating an increase of 16% in 2011-2012 and 29% in 2012-2013 from year 1 data. This indicates increased utilisation of RT as a therapeutic option for these cancers. Table 1 summarises patient demographics.
The median distance to the RT clinic per annum reduced over the time period (Fig2, Table 2). There was a statistically significant reduction in median travel distance annually, from 270.5 km and median road travel time of 201 minutes in 2010-2011 to 68.5 km and 66 minutes in 2011-2012 and finally 48.6 km and 56 minutes in 2012-2013 (p<0.0001; Fig3). This decrease in median road travel time to RT appointments equates to a 72% reduction from 2010 to 2013.
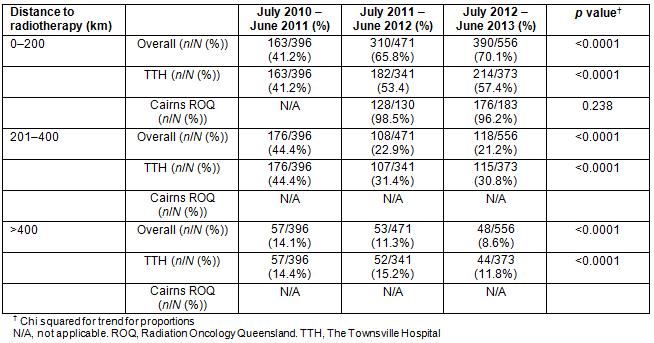
The ArcGIS maps of years 1 and 3 (Figs 4,5) have buffer zones to illustrate the reduction in travel distance to the RT clinic after the Cairns clinic opened. They further demonstrate an area of need south of Townsville to service the Mackay and Rockhampton regions. The overall number of patients travelling from within 200 km of an RT facility increased over the 3-year time interval, from 41.2% in 2010-2011 to 70.1% in 2012-2013, and the number of patients travelling greater than 400 km to a clinic has significantly reduced since a centre opened in Cairns (Table 3).
These results support the two hypotheses that the overall number of prostate and female breast cancer patients has increased since the inception of ROQ Cairns and the median distance and travel time to treatment has reduced.
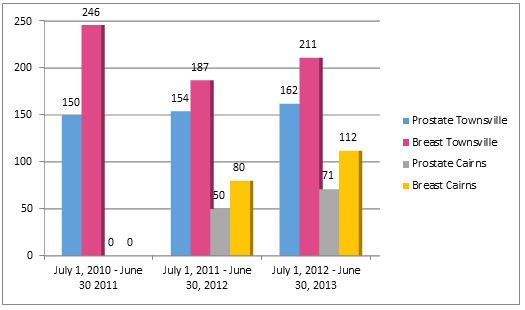
Figure 1: Patients treated in Townsville and Cairns for prostate and breast cancer, by year.
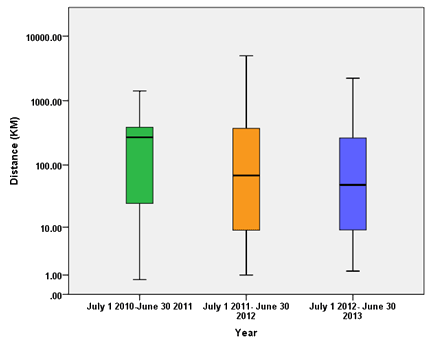
Figure 2: Distance travelled to radiotherapy, by year.
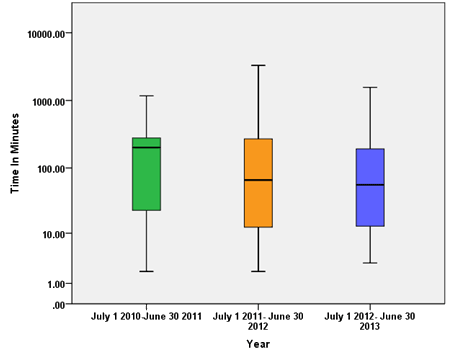
Figure 3: Travel time to radiotherapy, by year.
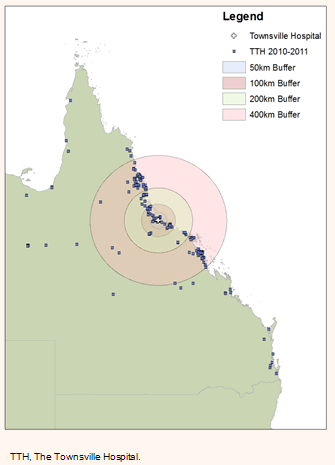
Figure 4: Travel distance to radiotherapy, 1 July 2010 - 30 June 2011.
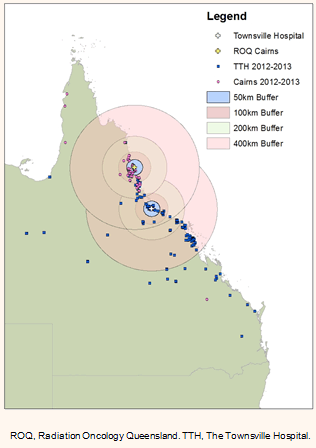
Figure 5: Travel distance to radiotherapy, 1 July 2012 - 30 June 2013.
Table 1: Demographic characteristics of patients receiving radiotherapy
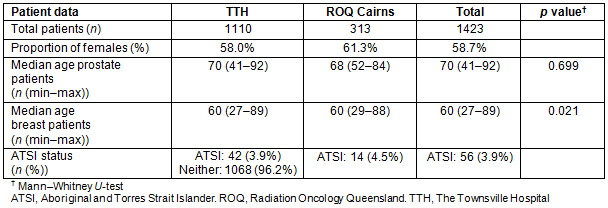
Table 2: Radiotherapy patient data, by year
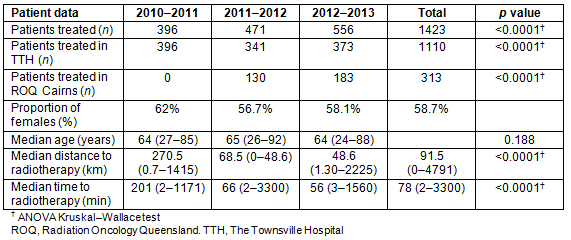
Table 3: Radiotherapy patients travelling 0-200 km, 201-400 km and further than 400 km, by year
Discussion
The study used retrospective audit of two radiotherapy databases and a GIS to illustrate the origins and distance to the RT clinic used over 3 years for prostate and female breast cancer patients in NQ. The opening of a second RT facility in NQ was associated with increased utilisation of RT as a treatment modality and reduced travel distance and time to RT. The maps illustrate the geographic need for the Cairns clinic but also highlight the large distances travelled by those patients south of Townsville, where many commute more than 400 km to TTH for the 9 weeks of their treatment. This strengthens the argument for alternative RT facilities south of the Mackay region, to ease travel pressure on patients, and it illustrates the role of GIS techniques in health service planning.
Global research confirms that distance does play a major role in acceptance of RT and therefore implies that utilisation relies on convenience and proximity to RT facilities; the findings from NQ are likely to be generalisable to other countries with dispersed populations over vast land, such as rural parts of Canada6-8,12,13. However, distance to treatment may have impacts beyond utilisation. A Queensland study identified a correlation between increased distance to a RT facility (more than 50 km) and increased mortality rates in rectal cancer patients18. Although patients with rectal cancer were not considered in this current study, it begs the question 'Does increased distance from radiotherapy lead to sub-optimal outcomes for cancer patients?'
There are several strengths to this research. First, the road travel time calculated using Google Maps demonstrated the most probable route driven by the patient to provide a more accurate and realistic distance than methods available in ArcGIS. Methods cited by previous studies were not indicative of travel distance because distances were often underestimated by Euclidean or straight-line measurements, precluding travel time calculation. Although other factors not accounted for in this study (eg construction delays, inclement weather and parking at the hospital site) would alter these times, they would be expected to increase the travel time and burden on patients. Second, the distance zones calculated were based on actual travel routes taken via Google Maps rather than a straight-line radius of the buffers from ArcGIS, which provides no information on the driven route, which may include detours around mountainous areas. Third, the spatial illustration of patient origin is an evidence-based method for planning the placement of RT clinics, which is valuable when clinics are few and far between. The data presented in this research provide evidence of the impact of an additional facility, and may aid health planners in their service network structure24.
Limitations of this study include that RT facilities in Brisbane were not included; therefore, the proportion of NQ residents travelling to Brisbane for RT treatment during this time is unknown. Also, the study design is set up to assess associations but not causality; thus, the authors were unable to ascertain whether the increase in utilisation of RT was due to improved access, or to increased awareness and local referrals. This research was conducted when ROQ Cairns first opened and the number of patients travelling between 200 km and 40 km could be expected to increase as a greater awareness of ROQ Cairns develops over the years. It may be valuable to repeat analysis after a few years to see if the trend continues as anticipated. Since this research has been completed, privately operated RT clinics have opened along the coastline in Hervey Bay and Bundaberg; their impact on travel distance, time and utilisation remains to be seen.
The Australian Radiation Oncology Inquiry was established by the Department of Health to evaluate utilisation and compare practice guidelines on an international level11. In addition, travel schemes to reduce expenses for rural and regional patients have been enhanced over the last decade11. Any future cost-benefit analysis must take into account the savings under the patient travel scheme resulting from providing treatment closer to home. This study supports the view that improving physical access to RT has improved utilisation of RT and there may be an advantage to creating small and basic RT facilities across Australia - 'satellite centres' for treatments of highly prevalent cancers such as prostate and breast cancer that are capable of providing accurate treatment in less urban environments. These have been trialled in many countries and have been successful in decentralising RT and reducing associated travel burden on patients. Supervision could be provided under a telemedicine model, as has been successfully done for medical oncology19-22.
The distribution of patients between Cairns and Townsville may create less burden on therapists and consultants in this field, in addition to potentially reducing waiting lists for patients. This research had a focus on travel distance and time, just two of the many factors that play a role in selection of treatment. Further research investigating patient experiences with travelling to radiation treatments and the psychosocial influence travel and wait times have on the patient in NQ as well as the financial and social implications for both patients and their families and the health system, remains to be undertaken.
This study concluded that distance and travel time to RT clinics significantly reduced after the opening of an additional RT facility in NQ, and that overall utilisation of RT increased over the 3 years. Although several factors may influence a patient's decision to undertake RT in a specified clinic, physical access to an RT clinic plays an important role.
Acknowledgements
This project was completed as part of the James Cook University Faculty of Medicine Research Scholarship awarded in 2013. The authors thank Mrs Aniko Cooper and Mr Kenton Thompson for allowing access to the oncology database, Mr Alan Goss for his data compilation, Ms Karen Johnston for her ArcGIS assistance, and Mr Shannon Robards for his input and support.
References
1. Westhuyzen J, Zarate D, Colquist S, Harden H. Cancer in Queensland: a statistical overview 2012. Brisbane: Queensland Health, 2012.
2. Cancer Council Queensland. A snapshot of cancer in north Queensland. (Internet). 2011. Available: https://cancerqld.org.au/wp-content/uploads/2015/12/northern_queensland.pdf (Accessed 4 March 2016).
3. Gillan C, Briggs K, Pazos AG, Maurus M, Harnett N, Catton P, Wiljer D. Barriers to accessing radiation therapy in Canada: a systematic review. Radiation Oncology 2012; 7(167): 1-8.
4. Khan F. The physics of radiation therapy 3rd edn. Philadelphia: Lippincott Williams &Wilkins, 2003.
5. Bomford CK, Kunkler IH. Walter and Miller's textbook of radiotherapy: radiation physics, therapy and oncology. 6th edn. Philadelphia: Churchill Livingstone Elsevier Ltd, 2003.
6. Soo J, French J, McGahan CE, Duncan G, Lengoc S. A retrospective study on accessibility of palliative radiation therapy in the management of prostate cancer in British Columbia. Journal of Radiotherapy in Practice 2011; 10(3): 159-172.
7. Schroen AT, Brenin DR, Kelly MD, Knaus WA, Slingluff Jr CL. Impact of patient distance to radiation therapy on mastectomy use in early-stage breast cancer patients. Journal of Clinical Oncology 2005; 23(28): 7074-7080.
8. Boscoe FP, Johnson CJ, Henry KA, Goldberg DW, Shahabi K, Elkin EB, et al. Geographic proximity to treatment for early stage breast cancer and likelihood of mastectomy. Breast 2011; 20(4): 324-328.
9. Voti L, Richardson LC, Reis IM, Fleming LE, MacKinnon J, Coebergh JWW. Treatment of local breast carcinoma in Florida: the role of the distance to radiation therapy facilities. Cancer 2006; 106(1): 201-207.
10. Sundaresan P, King MT, Costa DS, Milross CG. Barriers to radiotherapy utilisation in New South Wales Australia: health professionals' perceptions of impacting factors. Journal of Medical Imaging and Radiation Oncology 2015; 59: 535-541.
11. Department of Health. Radiation Oncology Inquiry (Internet) 2012. Available: http://www.health.gov.au/internet/main/publishing.nsf/content/health-roi-inquiry-report.htm (Accessed 10 November 2015).
12. Sharma DK. Does increased geographical distance to a radiation therapy facility act as a barrier to seeking treament? Australian Medical Student Journal 2015; 6(1): 35-40.
13. Baade P, Youlden DR, Gardiner RA, Ferguson M, Aitken JF, Yaxley J, Chambers SK. Factors associated wth treatment received by men diagnosed with prostate cancer in Queensland, Australia. BJU International 2012; 110: 712-719.
14. Australian Bureau of Statistics. Census of population and housing. (Internet). 2014. Available: http://www.abs.gov.au/census (Accessed 28 July 2014).
15. Ellis CR. Far North and Northern Queensland Population View Point 2010. Sydney: CB Richard Ellis, 2011.
16. The Townsville Hospital. Radiotherapy statistics, The Townsville Hospital. Townsville: The Townsville Hospital, 2013.
17. Tennant M, Kruger E, Shiyha J. Dentist-to-population and practice-to-population ratios: in a shortage environment with gross mal-distribution what should rural and remote communities focus their attention on? Rural and Remote Health (Internet) 2013; 13: 2518. Available: www.rrh.org.au (Accessed 14 January 2014).
18. Baade P, Dasgupta P, Aitken JF, Turrell G. Distance to the closest radiotherapy facility and survival after a diagnosis of rectal cancer in Queensland. Medical Journal of Australia 2011; 195(6): 350-354.
19. Arenas M, Gomez D, Sabater S, Rovirosa A, Biete A, Colomer J. Decentralisation of radiation therapy. Is it possible and beneficial to patients? Experience of the first 5 years of a satellite radiotherapy unit in the province of Tarragona, Spain. Reports of Practical Oncology and Radiotherapy 2015; 20(2): 141-144.
20. Belard A, Dolney D, Zelig T, McDonough J, O'Connell J. Improving proton therapy accessibility through seamless electronic integration of remote treatment planning sites. Telemedicine and e-Health 2011; 17(5): 370-375.
21. Sabesan S, Larkins S, Evans R, Varma S, Andrews A, Beuttner P, et al. Telemedicine for rural cancer care in North Queensland: bringing cancer care home. Australian Journal of Rural Health 2012; 20(5): 259-264.
22. Cameron M, Ray R, Sabesan S. Remote supervision of medical training via videoconference in northern Australia: a qualitative study of the perspectives of supervisors and trainees. BMJ Open 2015; 5: e006444.
23. Underhill C, Bartel R, Goldstein D, Snodgrass H, Begbie S, Yates P, et al. Mapping oncology services in regional and rural Australia. Australian Journal of Rural Health 2009; 17(6): 321-329.
24. McGuire S, Kruger E, Tennant M. Travel patterns for government emergency dental care in Australia: a new approach using GIS tools. Australian Dental Journal 2011; 56: 389-393.



