Introduction
Public health nurses (PHNs) represent the foundation of the US public health system, particularly in predominantly rural and remote areas1. Nurses comprise 25% of the professional public health workforce in the USA2,3. Public health nurses focus on assessing community health, assuring access to care, developing policies that promote population health, advocating for public health policies, communicating with vulnerable populations, and fostering community resiliency4. Since the 1990s, public health systems nationally have moved away from providing direct care to individuals, to a renewed focus on population health. Recently, increasing attention has been paid to strengthening the national public health infrastructure and workforce in response to emergency preparedness concerns and impending workforce shortages5. Concomitantly, issues regarding PHNs' scope of practice and competencies have been raised6-8.
Rural public health challenges
Rural public health has also received increasing attention in the past decade. According to a National Association of County and City Health Officials' 1999 survey, 65% of all local health departments in the USA serve populations of less than 25 000 people9. High priority services provided by these rural public health agencies include environmental health, child health, and communicable disease control, particularly immunizations for adults and children10. In comparison with urban health departments, rural health departments tend to provide more personal health services, such as family planning and maternal/child care, laboratory services, community assessments, and community outreach/education, in spite of operating with lower funding levels, less access to grant funding, and geographic and transportation challenges10. In relation to the core public health functions, Suen and Magruder's research indicated that rural public health agencies had the lowest mean score on core function capacity, due to inadequate funding levels, planning capacity, and public health infrastructure11. Challenges rural public health agencies face include 'attracting a skilled workforce, maintaining strong leadership to advocate for and lead a prevention agenda, and ensuring population health activities' p.18612. In 2004, Bridging the Health Divide: The Rural Public Health Research Agenda identified the need for research in the areas of rural public health infrastructure, workforce development and competency enhancement, rural health disparities, access to care/safety net support, rural public health preparedness, and environmental health issues13.
Internationally, rural and remote public health has been addressed historically and currently in greater depth outside the USA. From a Canadian perspective, Bavington notes that rural and remote public health professionals often function as overworked generalists with long-distance supervision, mentoring, and consultation14. He also notes, however, that professional isolation can result in greater innovation and independence. The other international leader in rural and remote public health is Australia, with a rich history of 'bush nursing', which began in 1910 in Australia's most remote areas and continues today15. John Wakerman, the Director of the Australia's Centre for Remote Health, also speaks to the innovative nature of rural and remote public health and advocates for moving 'away from the deficit model of rural and remote health' (p.54)16.
Rural public health nursing
Several studies have demonstrated that US PHNs provide the majority of public health services, particularly in rural and remote areas. A major concern, however, is that in the USA most rural PHNs' highest level of nursing education is an associate degree, which typically does not include any curricular content in public health. In addition, the public health nursing workforce is aging and retiring at rapid rates, which creates serious workforce concerns, especially in rural and remote areas where recruitment and retention of well prepared nurses has been challenging historically2,5. In general, recruitment and retention of rural public health professionals, particularly nurses, can be problematic due to location, educational opportunities, and financial constraints17. Juhl et al's research supports this concern related to public health funding, particularly as evidenced by chronically low salaries among rural PHNs18. Similarly, Canadian studies with rural PHNs have documented broader scopes of practice, challenges related to inadequate staffing and resources, lower salaries, but moderate levels of job satisfaction among rural compared with urban PHNs19,20. In a study of the public health system in Idaho and Wyoming conducted in the period 1998-1999, Richardson et al. found that Idaho had 39 public health professionals per 100 000 people, over half of whom were nurses21. Consistent with national data, most of these nurses did not have formal preparation in public health. In a study of public health systems in Alaska, Montana, and Wyoming, Rosenblatt and Rosenblatt found that rural PHNs were more likely to work part-time but stayed in their positions longer than their urban counterparts22.
Rural public health nursing challenges
The literature related to public health nursing in the USA's most remote areas (often referred to as 'frontier') is particularly limited. The Frontier Education Center reported that nurses serving frontier areas in general tend to have lower levels of education and earn lower salaries than nurses in non-frontier areas23. They noted:
...because most frontier and rural communities are distant from hospitals, residents may rely on non-hospital based care settings for a greater proportion of their care than their urban counterparts ... thus, nurses serving in home health, public health, primary care, school health or faith-based settings are important resources in communities that may otherwise have no locally-based provider. (p.10-11)23
Public health nurses working in the most isolated areas must provide a variety of services which requires a 'broad knowledge base, versatility, and the ability to improvise' (p.50124. In contrast with less remote settings, service delivery may be primarily home-based due to scarcity of health facilities and travel constraints10,24. Bushy and others note that the more remote the community, the greater the challenge in dealing with health care delivery and workforce issues, including recruitment and retention25,26.
International studies focusing on remote nursing practice in Australia and Canada provide important related insights. Australian studies indicate that issues of high turnover, need for locum relief due to stress and fatigue, communication barriers and inadequate preparation and administrative support were consistent problems voiced by nurses serving remote Australian communities, often in one-nurse outposts27-29. The landmark Canadian study The Nature of Nursing Practice in Rural and Remote Canada examined RN practice in rural and remote areas throughout Canada, in all clinical settings, including 412 nurses employed in community/public health agencies30,31. Results from interviews indicated the importance of local and long-distance collegial networks, accessible resources, and 'distance-proof, responsive management structure and processes' to address the nurses' feelings of being marginalized and 'being out of sight and out of mind' (p.46)32. Andrews et al's33 analysis of the Canadian study data specifically focusing on nurses working alone in rural and remote settings (11.5% of the total sample) represents the most directly applicable comparable study to the present Idaho study. Their analysis included 81 nurses (19.9%) working in community health/public health agencies, which constituted the most common work setting for nurses working in one-nurse settings, followed by outpost nursing stations. They reported that work satisfaction, which was highest among diploma prepared nurses, was positively related to the ability to have face-to-face contact with colleagues, availability of equipment, and decision latitude. Barriers to continuing education and job-related psychological demands were negatively related to work satisfaction. Results specifically from 'outpost nurses' in Canada's remote northern communities, who provide care primarily to Aboriginal populations, indicated the importance of strong preparation, problem solving, critical thinking and adaptability to change skills, self-direction/self-motivation, access to continuing education, and strong administrative support to address the chronic high turnover rates34. These findings support earlier research with Canadian outpost station nurses which documented challenges related to limited resources and travel requirements35. In both Canada and Australia, these isolated 'outpost' nurses 'do it all', providing primary care and crisis/emergency care along with public health services, which differs from US PHNs serving rural/remote communities who have a narrower scope of practice.
Conceptually, isolation has been identified as a distinguishing characteristic of rural and especially remote nursing in the US and internationally23,28,30,35-38. In addressing public health nursing practice in the most remote settings, professional and personal isolation may be particularly relevant challenges. Bushy stated (p.40)36:
Professional isolation is closely related to geographic isolation and can be perceived a positive, negative, or a combination of both. Many rural nurses enjoy the professional independence and creativity not usually found in larger practice settings. Others find that the responsibilities in a rural community health agency can be overwhelming. Often there is no immediately accessible professional network that can provide support and consultation on a matter of concern. Likewise, the lack of immediately available opportunities for establishing relationships with other professionals, or not having the 'central office' nearby, can reinforce feelings of isolation. Professional isolation requires an outstanding ability for a nurse to evaluate and prioritize needs and the types of services that can be provided to the local population. The lack of physical access to other providers, education, and technology can potentially cause considerable role strain.
Telecommunication capability, including phone and internet service, is critical in addressing the isolation challenges of remote nursing practice, however many rural and remote areas lack adequate communication networks, especially cell phone and internet coverage.
Public health nurse competency
In response to the increased attention on public health infrastructure and quality in the USA, in 2004 the Office of Workforce Policy and Planning, Centers for Disease Control and Prevention (CDC) along with the Council on Linkages (COL) between Academia and Public Health Practice, developed a list of core competencies for all public health professions, including the following eight competency domains39:
- analytic assessment skills
- policy development/program planning skills
- communication skills
- cultural competency skills
- community dimensions of practice skills
- basic public health sciences skills
- leadership and systems thinking skills
- financial planning and management skills.
The Quad Council of Public Health Nursing Organizations expanded on these competency domains in relation specifically to public health nursing practice40. The Quad Council competencies are also congruent with the American Nurses Association's (ANA) Public Health Nursing Scope and Standards of Practice8.
Purpose
Thus, the research-based knowledge related to the unique practice area of public health nursing in remote settings is extremely limited. The purposes of this study, therefore, were to: (i) describe the characteristics, competency levels, and practice patterns of PHNs working in remote one-nurse offices; and (ii) compare PHNs working in one-nurse offices with nurses working in multi-nurse offices in Idaho USA, in relation to their demographic characteristics, practice patterns and competency levels.
Methods
This study, conducted March to May 2007 as part of a comprehensive study of public health nursing in Idaho, used a cross-sectional descriptive comparative design.
Setting
Idaho is a predominantly rural state in the Pacific Northwest region of the United States. With a population of 1.5 million, Idaho consists of 44 counties, two-thirds of which are classified as rural or frontier. The Idaho Office of Rural Health defines rural counties as those with no communities having more than 20 000 people, and frontier counties as those with population densities of less than 7 persons per 1.6 km2 (7 persons/mile2), which is consistent with national definitions. The US designation of 'frontier' is similar to the term 'remote' which is used more commonly internationally.
Public health services in Idaho are delivered through a unique, nationally recognized structure of 7 autonomous districts that include 4 to 8 counties each. Each district has a significant rural/frontier proportion of their population. The land areas of the districts range from 12 358 to 27 363 km2 (7679 to 17003 miles2). The population density of the districts based on 2005 population estimates ranges from 7.5 to 43.7 persons per 1.6 km2 (7.5 to 43.7 persons per mile2), with a mean of 19.2 persons per 1.6 km2 (19.2 persons per mile2) and standard deviation of 12.441. All districts have a central headquarters in the largest community in the district, with small outreach offices to serve outlying communities. The required credential to practice as a PHN in Idaho is licensure as a registered nurse (RN). Registered nurses in Idaho can hold either an associate (2 year) or baccalaureate (4 year) degree in nursing. In some districts, licensed practical nurses (LPNs) who are prepared at the technical level and do not hold a degree in nursing are employed as PHNs, due to nursing shortages.
Sample
The total sample consisted of 124 PHNs currently practicing in Idaho's official public health agencies, including 15 serving in one-nurse offices. Inclusion criteria were intentionally broad: nurses currently employed in community settings with the job title 'public health nurse' or who identify themselves as PHNs. Nurses from the state office and each of the 7 public health districts in Idaho were included. The 2006 National Sample Survey of Registered Nurses estimated that there were approximately 70 PHNs in Idaho42. Based on this population estimate, we were confident that the majority of PHNs in Idaho were included in the study.
Procedures
On-site structured interviews with staff nurses and administrators were conducted with all PHNs who met the inclusion criteria. Participation was voluntary, written consent was obtained, and confidentiality strictly protected. Almost all nurses who were approached agreed to be interviewed if available. The study procedures were approved by the university Institutional Review Board prior to data collection. Demographic data including age, ethnicity, sex, experience, and educational background were collected (Table 1). To assess competency levels, participants were asked to rate their level of competency in relation to each of the 8 Council on Linkages Between Academia and Public Health Practice domains on a 1 to 5 scale (1 = beginning competency/awareness and 5 = expert competency/proficiency). Overall competency scores were computed by averaging the domain ratings for each participant (Table 2). The data were statistically analyzed using descriptive statistics, two-tailed Pearson correlations, ANOVAs, and independent t-tests, using a significance level of p <.05.
Results
Characteristics of public health nurses working in one-nurse offices
The 15 PHNs who worked in one-nurse offices were based in 15 different counties (located in 6 of the 7 public health districts), 10 of which were frontier and 5 rural. The counties they served ranged in population (2005 estimates) from 2781 to 28 114 people (mean = 11 013), with land masses of 724.2 to 13 655.3 km2 (mean = 3753; 450 to 8485 miles2, mean = 2332), and population densities ranging from 0.9 to 29.4 persons per 1.6 km2 (0.9 to 29.4 persons/mile2
Demographically, the solo PHNs were all Caucasian females and their ages ranged from 31 to 64 years (mean = 46.9). They reported a mean of 7.7 years in their current position (range = 1-20 years), a mean of 8.6 years experience in public health (range = 1-20), and a mean of 22.5 years experience in nursing in general (range = 7-40 years). Educationally, 7 (47%) held a baccalaureate degree in nursing (BSN), 6 (40%) had associate degrees, 1 (7%) had a diploma in nursing, and 1 (7%) was an LPN. Two-thirds of the sample received their nursing education from in-state nursing programs. These demographic characteristics are fairly representative of the Idaho nurse population, except for the higher rate of baccalaureate prepared nurses among the solo PHN sample43.
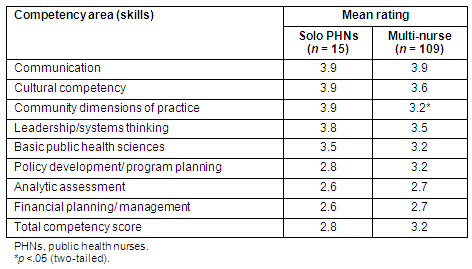
Their self-rated levels of competency were strongest in the areas of communication (mean = 3.9), cultural competency (mean = 3.9), community dimensions of care skills (mean = 3.9), and leadership/systems thinking skills (mean = 3.6) and lowest in the areas of financial management (mean = 2.6), analytical assessment (mean = 2.6), policy development/program planning (mean = 2.8) and basic public health sciences skills (mean = 3.5). Their combined average level of competency ranged from 2.0 to 4.1 with a mean of 3.3.
The solo PHNs reported providing a wide array of services with support from other nurses in the district, including epidemiology, family planning/STD clinics, immunization clinics, communicable disease surveillance, and school nursing. They expressed strong job satisfaction citing the benefits of autonomy, variety and close community ties. One frustration voiced by several solo PHNs related to problems in communication with the main district office and at times feeling 'out of the loop'. Communication with other nurses in the district was conducted mainly by email and phone. Most districts conducted monthly staff meetings at the main office which all nurses attend for training, coordination and networking.
Comparison of solo public health nurses with public health nurses in multi-nurse offices
When compared with the PHNs working in multi-nurse offices, the solo PHNs were found to be quite similar, with no statistically significant differences, except in one competency area (Tables 1, 2). The solo PHNs were slightly younger than the non-solo PHNs. Experientially, the solo PHNs had more total nursing experience but fewer years experience in public health and a slightly higher mean number of years in their current position. In the non-solo sample, 56.4% held a BSN or higher, compared with 50% of the solo PHNs (who were RNs). There were no significant differences between the solo and non-solo PHNs in relation to demographic characteristics or competency ratings, with the exception of the competency area of 'community dimensions of practice skills'. In this area, the mean rating for solo PHNs was 3.9, compared with 3.2 for non-solo PHNs (t = 3.547, p = .002). In the multi-nurse offices, the nurses often reported specialized practices, focusing on a particular program, such as immunizations. In contrast, in the outlying one-nursing offices, the practice was described as more generalized with nurses working across programs in collaboration with other nurses in the district.
Table 1: Comparison of demographic characteristics of public health nurses in solo versus multi-nurse offices
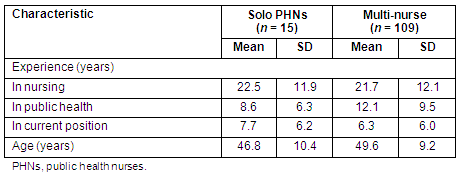
Table 2: Comparison of public health nurses in solo versus multi-nurse offices competency levels
Discussion
This study represents the first description of PHNs serving in single-nurse offices in the USA. The solo PHNs in this study were predominantly middle-aged women with extensive experience in nursing and public health, and less than half of the sample held a bachelor or higher degree. These demographic characteristics are fairly consistent with previous studies in the USA, Australia and Canada. The solo nurses in the Canadian sample were slightly older than the Idaho sample and lived in somewhat smaller communities, with 75% living in communities of 2500 or fewer, and included 29.5% with a bachelor or higher degree (which was slightly higher than the total sample)33. The Idaho sample provided a wide range of public health services with support from other nurses in the district, and expressed strong job satisfaction, citing the benefits of autonomy, variety, and close community ties, however challenges related to isolation and communication with colleagues were noted. These challenges are also consistent with those previously reported by Canadian and Australian nurses in remote practice. Their self-rated levels of competency were highest in the areas of communication, cultural competency, community dimensions of care, and leadership/systems thinking skills, and lowest in the areas of financial management, analytical assessment, policy development/program planning, and basic public health sciences skills. The solo nurses were very similar to their colleagues in multi-nurse offices demographically and in self-rated competency levels, except in the area of community dimension of practice skills, in which the solo PHNs were significantly higher than the non-solo PHNs. These findings suggest that US PHNs practicing in isolated one-nurse offices in rural and remote communities are comparable to PHNs working in less isolated settings; however, solo nurses self-report stronger community dimensions of practice skills. Their practice is more generalized than other PHNs and they express high levels of job satisfaction but some frustration with issues related to isolation and communication. This high level of job satisfaction along with the relatively low turnover rate contrasts with some previous reports from Australia and Canada among nurses in remote practice; however, this may be due to the degree of isolation and the strong connection to the community, along with differing demands and scopes of practice.
The finding that the solo nurses were for the most part quite similar in demographic characteristics, education, experience and competency levels to PHNs working in multi-nurse offices, contradicts some possible biased perceptions that nurses serving the most isolated rural and frontier communities are less prepared than their more urban colleagues. Conversely, the results indicate that the solo nurses are highly autonomous with demanding, generalized practices. Based on these challenges, it could be argued that solo practice requires the highest level of PHN preparation and competency, which was not demonstrated in this study.
A critical finding was the fact that the solo PHNs self-rating of competency in relation to community dimensions of practice was significantly higher than the PHNs in multi-nurse offices. This finding is consistent with previous correlational analysis of competency levels and rurality, as measured by district population density, suggesting that PHNs serving rural and frontier communities feel as competent as nurses serving more urban areas and more competent specifically in the area of community dimensions of practice44. The fact that the solo nurses expressed significantly higher levels of competency in the domain of community dimensions of practice supports rural nursing theory and scholarship that has documented the strong community base of rural/frontier nursing in all areas of practice45. The generalized nature of solo public health nursing practice, in contrast to the more specialized focus of urban practice, may also contribute to the higher levels of self-reported competency among solo nurses in relation to community dimensions of practice skills.
The results also support the conceptual perspective of the influence of isolation on remote public health nursing practice. Maintaining strong communication networks and collegial support for solo PHNs are key strategies in promoting professional satisfaction and program effectiveness.
Limitations
The limitations of this study included the volunteer sample from only one state in the USA. Information regarding practice characteristics, attitudes and concerns among the solo nurses was somewhat limited, due to the brief nature of the structured interviews. Also, the rather simplistic nature in which competency was measured, along with the lack of reliability and validity data to support this measurement approach, represent limitations. This approach was necessitated based on the time demands of the larger study; however, in future research, more detailed assessment using all the Quad Council competency indicators could be used in order to measure competency in greater depth40. The fact that levels of competency were measured only by self-report represents an additional limitation. Validation of self-reported competency levels using supervisor and/or peer ratings would serve to strengthen future studies.
Conclusions and implications
Further research is indicated to compare these findings with other states, nationally, and internationally. In addition, further research is needed to more fully describe this unique subset of PHNs, particularly in terms of factors promoting recruitment and retention. Implications for practice and policy point to the need for ensuring the infrastructure to support PHNs in solo practice through strong support networks and adequate communication systems. Also, given the age and tenure of the solo nurses in this study, efforts to address future education and recruitment of PHNs to remote practice are indicated to ensure an adequate supply of nurses for the future in these vital roles and unique practice settings.
These findings indicate that solo PHNs in Idaho provide essential services to remote communities, much like their colleagues in similar settings internationally. Lessons learned from this study include the need to continue to address resource and communication issues, including technology, to support PHNs in solo practice. The strong collaborative model in which Idaho's solo PHNs are supported by their nursing colleagues through the public health district structure may serve as a model for other states and nations to promote recruitment, retention and quality care. The fact that the PHNs in one-nurse offices were quite comparable to their colleagues in multi-nurse offices speaks to the commonality that an effective district structure with strong collegial and administrative support can produce.
This cross-sectional descriptive study of PHNs in one-nurse versus multi-nurse offices in a predominantly rural state demonstrated the unique aspects of remote public health nursing practice as well as the commonalities with more urban settings. The strong job satisfaction and community orientation of solo PHNs, despite the geographic and professional isolation, affirms the positive nature of this unique practice setting.
Acknowledgement
The authors acknowledge Diane Kenski for her assistance in the preparation of this article.
References
1. Rosenblatt R, Casey S, Richardson M. Rural-urban differences in the public health workforce: findings from local health departments in three rural western states. Working Paper #61. Seattle, WA: WWAMI Center for Health Workforce Studies, 2002.
2. Health Resources and Services Administration. The public health workforce enumeration 2000. New York: Center for Health Policy, Columbia University School of Nursing, 2000.
3. National Association of County and City Health Officials. The local health department workforce: findings from the 2005 national profile of local health departments study. Washington, DC: National Association of County and City Health Officials, 2005.
4. Robert Wood Johnson Foundation. Charting nursing's future. Strengthening public health nursing - part 1. Policies and programs that recognize nursing's role in assuring the public's health. Princeton, NJ: Robert Wood Johnson Foundation, 2008. Available: http://www.rwjf.org/files/research/20081010chartingissue7.pdf (Accessed 12 July 2009).
5. Gebbie K, Raziano A, Elliott S. Public health workforce enumeration. American Journal of Public Health 2009; 99(5): 786-787. Available: http://search.ebscohost.com.libproxy.boisestate.edu/login.aspx?direct=true&db=aph&AN=39654422&site=ehost-live (Accessed 12 July 2009).
6. Quad Council of Public Health Nursing Organizations. The public health nursing shortage: a threat to the public's health. (Online) 2007. Available: http://www.astdn.org/downloadablefiles/Final%20Nursing%20Shortage%20Paper.pdf (Accessed 13 July 2009).
7. Health Resources and Services Administration. Public health work force study. Washington, DC: US Department of Health and Human Services, Bureau of Health Professions, 2005.
8. American Nurses Association. Public health nursing scope and standards of practice. Silver Spring, MD: American Nurses Association, 2007.
9. National Association of County and City Health Officials. Local public health agency infrastructures: a chart book. Washington, DC: National Association of County and City Health Officials, 2001.
10. Berkowitz B. Rural public health service delivery: promising new directions. American Journal of Public Health 2004; 94(10): 1678-1681. Available: Academic Search Premier. http://search.ebscohost.com.libproxy.boisestate.edu/login.aspx?direct=true&db=aph&AN=14653776&site=ehost-live (Accessed 12 July 2009).
11. Suen J, Magruder D. National profile: overview of capabilities and care functions of local public health jurisdictions in 47 states, the District of Columbia and 3 US territories, 2002-2003. Journal of Public Health Management and Practice 2004; 10: 2-12.
12. Berkowitz B, Ivory J, Morris T. Rural public health: policy and research opportunities. The Journal of Rural Health 2002; 18(5): 186-196.
13. Center for Rural Health Practice. Bridging the health divide: the rural public health research agenda. Bradford, PA: Center for Rural Health Practice, University of Pittsburgh, 2004. Available: http://www.upb.pitt.edu/uploadedFiles/About/Sponsored_Programs/Center_for_Rural_Health_Practice/Bridging%20the%20Health%20Divide.pdf (Accessed 12 July 2009).
14. Bavington B. Rural public health. Canadian Journal of Public Health 1994; 85: 295-296. (Editorial)
15. Gartell M. Bush nursing in Australia. RN 1955; 18(10): 54-88. Available: www.cpc.utas.edu.au/documents/ordinary%20women.doc (Accessed 11 December 2009).
16. Wakerman J. Rural and remote public health in Australia: building on our strengths. Australian Journal of Rural Health 2008; 6: 52-55.
17. Quiram B, Meit M, Carpender K, Penne C, Castillo G, Duchicela D. Rural public health infrastructure: a literature review. In: L Gamm, L Hutchison (Eds), Rural healthy people 2010: a companion document to healthy people 2010 Volume 3. College Station, TX: The Texas A&M University System Health Science Center, School of Rural Public Health, Southwest Rural Health Research Center; 2005. Available: http://www.srph.tamhsc.edu/centers/rhp2010/Volume_3/Vol3Ch5LR.htm (Accessed 13 July 2009).
18. Juhl N, Dunkin J, Stratton T, Geller J, Ludtke R. Job satisfaction of rural public and home health nurses. Public Health Nursing 1993; 10(1): 42-47.
19. Leipert B. Women's health and the practice of public health nurses in northern British Columbia. Public Health Nursing 1999; 16(4): 280-289.
20. Henderson-Betkus M, MacLeod M. Retaining public health nurses in rural British Columbia: the influence of job and community satisfaction. Canadian Journal of Public Health 2004; 95(1): 54-58.
21. Richardson M, Casey S, Rosenblatt R. Local health districts and the public health workforce: a case study of Wyoming and Idaho. Working Paper #56. Seattle, WA: WWAMI Center for Health Workforce Studies, 1999; 1-25.
22. Rosenblatt R, Rosenblatt F. The role and function of small, isolated public health departments: case study in three western states. Working Paper #65. Seattle, WA: WWAMI Center for Health Workforce Studies, 2001; 1-20.
23. Frontier Education Center. Addressing the nursing shortage: impacts and innovations in frontier America. (Online) 2004. Available: http://www.frontierus.org/nursing.htm (Accessed 13 July 2009).
24. Stuart-Siddall S, Haberlin JM. Nursing role in rural health nursing. In L Jarvis (Ed.). Community health nursing: keeping the public healthy. Philadelphia, PA: FA Davis, 1985; 495-511.
25. Bushy A. International perspectives on rural nursing: Australia, Canada, USA. Australian Journal of Rural Health 2002; 10: 104-111.
26. Davis D, Droes N. Community health nursing in rural and frontier counties. Nursing Clinics of North America 1993; 28(1): 159-169.
27. Cramer J. Finding solutions to support remote area nurses. Australian Nursing Journal 1994; 2(6): 21-35.
28. Hanna L. Continued neglect of rural and remote nursing in Australia: the link with poor health outcomes. Australian Journal of Advanced Nursing 2001; 19(1): 36-45.
29. Mills J, Birks M, Francis K. Indigenous/remote health: research aims to improve remote area nursing in QLD. Australian Nursing Journal 2009; 16(8): 34-35.
30. MacLeod M, Kulig J, Stewart N, Pitblado J, Knock M. The nature of nursing practice in rural and remote Canada. Canadian Nurse 2004; 100(6): 27-31.
31. Stewart N, D'Arcy C, Pitblado J, Morgan D, Forbes D, Remus G, et al. A profile of registered nurses in rural and remote Canada. Canadian Journal of Nursing Research 2005; 37(1): 122-145.
32. MacLeod ML, Misener MR, Banks K, Morton A, Vogt C, Bentham D. 'I'm a different kind of nurse': advice from nurses in rural and remote Canada. Canadian Journal of Nursing Leadership 2008; 21(3): 40-53.
33. Andrews M, Stewart N, Pitblado J, Morgan D, Forbes D, D'Arcy C. Registered nurses working alone in rural and remote Canada. Canadian Journal of Nursing Research 2005; 37(1): 14-33.
34. Misener MR, MacLeod ML, Banks K, Morton AM, Vogt C, Bentham D. There's rural, and then there's rural: advice from nurses providing primary healthcare in northern remote communities. Canadian Journal of Nursing Leadership 2008; 21(3): 54-63.
35. Macleod ML, Brown AJ, Leipert B. International perspective: Issues for nurses in rural and remote Canada. Australian Journal of Rural Health 2008; 6(2): 72-78.
36. Bushy A. Rural nursing: practice and issues. Silver Springs, MD: American Nurses Association Continuing Education Program, American Nurses Credentialing Center, 2004.
37. Hegney D. Rural nursing in Australia. In: A Bushy (Ed.). Orientation to nursing in the rural community. Thousand Oaks, CA: Sage, 2000; 203-217.
38. Rennie DC, Baird-Crooks K, Remus G, Engel J. Rural nursing in Canada. In: A Bushy (Ed.). Orientation to nursing in the rural community. Thousand Oaks, CA: Sage, 2000; 217-232.
39. Public Health Foundation. Council on Linkages between Academia and Public Health Practice. (Online) 2004. Available: http://www.trainingfinder.org/competencies/background.htm (Accessed 29 July 2009).
40. Quad Council of Public Health Nursing Organizations. Public health nurse competencies. Public Health Nursing 2004; 21(5): 443-452.
41. United States Census Bureau. Idaho quickfacts from the US Census Bureau, state and county quickfacts, population 2005 estimate. Washington, DC: US Census Bureau, 2007. Available: http://quickfacts.census.gov/qfd/states/16000.html (Accessed 12 July 2009).
42. Bigbee JL. The relationships between nurse and physician-to-population ratios and state health rankings. Public Health Nursing 2008; 25(3): 244-225.
43. Idaho Board of Nursing. Idaho Board of Nursing Statistical Report. Boise, ID: Idaho Board of Nursing, 2008. Available: http://ibn.idaho.gov/publications/Annual_Report_2008.pdf (Accessed 28 October 2009).
44. Bigbee JL, Otterness N, Gehrke P. Public health nursing competency in a rural/frontier state. Public Health Nursing 2009; (in press).
45. Bigbee JL. The uniqueness of rural nursing. Nursing Clinics of North America 1993; 28(1): 131-144.


