Rural areas have chronic shortages of health professionals. Strategies known to identify and encourage health professionals to enter rural practice include selecting rural origin students for professional schooling, providing exposure to rural practice during training, selecting students committed to family medicine and providing financial aid linked to a future rural practice obligation1,2.
Colorado has 64 counties of which 24 are rural and 23 are frontier (<6 people/km2)3. All but 12 of Colorado's counties quality as full or partial primary care Health Professional Shortage Areas4. The state's rural areas have shortages of physicians, nurses, pharmacists and dental professionals5.
The University of Colorado operates a variety of health professions training programs with missions to supply a healthcare workforce to meet the needs of the entire state. These programs value interdisciplinary collaboration. These programs all have both on- and off-campus programs to provide students with rural experience and actively seek ways to engage their learners in interdisciplinary learning and practice. While most of these experiences are clinical in nature, students face a wide range of non-clinical issues as they make career location decisions. These include lifestyle, family, recreational, cultural and geographic choices.
The interdisciplinary rural immersion program is designed to provide students with experience in taking an in-depth look at a rural community. Similar programs conducted in Australia, Canada and the USA tend to be either clinically-focused6-8 or include only one or two professions9,10 . This project report describes a 3 year experience of conducting an interdisciplinary, non-clinical rural immersion program in Colorado. The purpose of the experience is to help students learn how to evaluate a wide range of characteristics of a rural location and reflect on their intent to live and work in a rural area.
Each summer a rural area is chosen for the Interdisciplinary Rural Immersion Program. Students who will be completing the first or second year of training in the medical doctor, physician assistant, doctor of pharmacy , master of public health, nursing, psychology and dental medicine programs are informed of the program location, objectives and dates and advised to indicate their interest in participating. Those in a rural track or rural interest program are given priority. Spouse/partners are invited to participate if willing to fully participate in all of the program components. Partner participation is encouraged because the decision to eventually locate in a rural area is a family choice strongly affected by partner lifestyle and career requirements11,12.
Logistical planning for the week-long program is substantial and requires 6 months or more planning and lead time. Local site coordination is provided by a community member identified in each location based on his/her knowledge of the area and personal connections. Funding for each year was secured from a combination of one or more foundations and the Colorado Area Health Education Center program office. Prior to the immersion week, the director and coordinator confirm the orientation speakers and the basic contact list, providing them with a written description of the students who will be attending and the goals of the week. A press release is also sent to local print and broadcast media with a request to inform the community-at-large that the students will be visiting, will be seen around the town and may be encountered personally. This frequently leads to newspaper and radio interviews during the week.
On arrival in the town, a half-day orientation to the community is conducted by inviting local citizens to speak for 20 to 30 min each about general topics. Potential speakers for these topics vary widely from site to site and are identified by the local coordinator based on personal contact (suggestions in parentheses):
- culture and history (Local historian)
- economy (Business leader)
- education (School superintendent, teacher or community college official)
- government and law enforcement (Mayor, elected official, chief of police)
- healthcare (includes acute care, long-term care, mental health and public health) (Hospital administrator, physician, nurse or public health official)
- natural resources (Forest service, public utilities, Department of Natural Resources, Fish and Game).
Following the orientation, students allocate themselves into small groups based approximately on the areas that were presented to them during the community orientation. These are their groups and focus areas for the rest of the week. They are encouraged to place themselves into a focus area that does not necessarily correspond to their area of professional study and to establish groups that contain students from a variety of professional study areas.
Students then check into their hotel or dormitory and, depending on time, can be sent on a 'scavenger hunt' to find local landmarks and find their way around the community prior to a group dinner.
The rest of the week consists of blocks of time during which the small groups arrange contacts, and conduct site visits and interviews within their area of focus. Although they are given some general questions to think about and a basic contact list, they are encouraged to ask their own questions and seek new contacts beyond those provided for them. Each immersion week includes at least one large group tour, arranged in advance, of a site that could not otherwise be visited by small groups because of legal, safety or logistical issues. Examples of large group tours include a state correctional facility, an underground coal mine, a fish hatchery and various farming operations. Other than these pre-arranged tours, the students arrange all visits and interviews themselves.
Each year, at least one evening meal has been hosted by a community organization or funder with local entertainment or program. Community members are invited to attend this event which provides an opportunity for the students to further socialize and for community members to learn about the students' impressions of their area.
The final event of the week is the Friday morning debriefing session during which the groups present their findings in multimedia format using narrative and slide presentations. The community members who spoke at the initial orientation session are invited to this session, as are local media and any other interested community members. Faculty from the students' respective academic programs are also invited.
Data collected to evaluate the program include a written questionnaire, essays, group slide presentations and audio-recordings of their debriefing presentations and personal reflections about the week's effect on their thinking about future rural practice.
Quantitative analysis was performed of the students' assessment of how the program objectives were met. Qualitative analysis consisted of identifying themes that emerged in the essays and presentations.
This program evaluation project report does not identify participants individually and does not require submission to the Colorado Multiple Institutional Review Board.
Fifty-two students and four spouses/partners participated in this program in a 3 year period (Table 1). None participated more than once. Approximately two-thirds of those surveyed about their background had spent significant time in a rural area before professional school, as indicated by having graduated from high school in a rural area or having worked in a rural area.
Each rural town in which the program was conducted (Table 2) is located in a Health Professional Shortage Area.
A model budget includes a US$500 stipend for each participating student (Table 3) and a typical schedule is shown (Table 4).
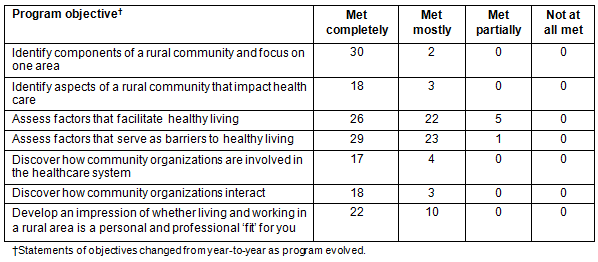
Students overwhelmingly responded that the objectives of the week were met 'completely' or 'mostly' (Table 5). They also uniformly answered that the program was well organized, that the housing and food were adequate and that the experience was worth their time. As the program evolved, minor modifications to the schedule were made in response to student recommendations. Their main recommendation was to allow more unscheduled time, which led to allocation of one afternoon to free time and three unscheduled evenings.
Table 1: Participating students according to discipline and year
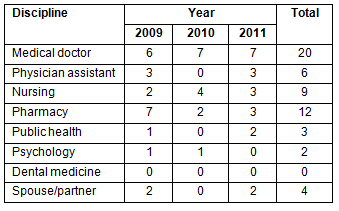
Table 2: Characteristics of rural areas where immersion program was conducted
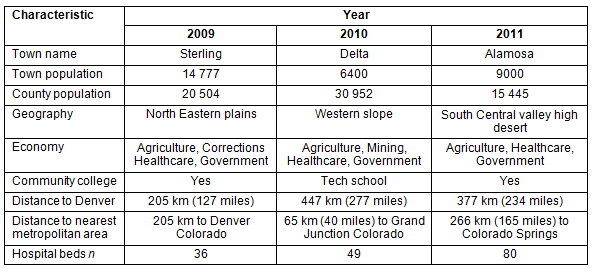
Table 3: Model for a student budget
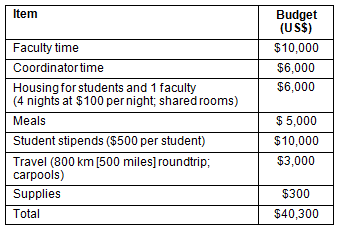
Table 4: Typical student schedule
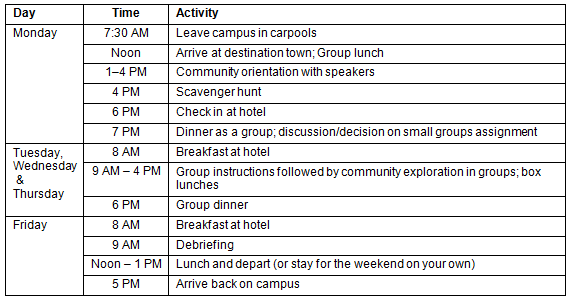
Table 5: Student evaluation of program objectives
The most important results of the program are the students' impressions of rural community life and whether they see themselves as potential future rural healthcare providers. Following the 2011 program, the students were asked how the experience affected their interest in future rural life and work. They answered in 18 of 19 cases that the experience increased (n=15) or reinforced (3) their interest. One student found that the experience resulted in a decreased interest. In 14 of 19 cases they answered that they are surely (2) or very likely (12) to locate in a rural area; the remaining 5 answered that they were unsure.
In all years, their reports and written comments were analyzed for recurring themes. These themes are summarized (Table 6) and represent a wide range of both positive and negative aspects of rural life and work.
Table 6: Themes noted in students' presentations and written comments
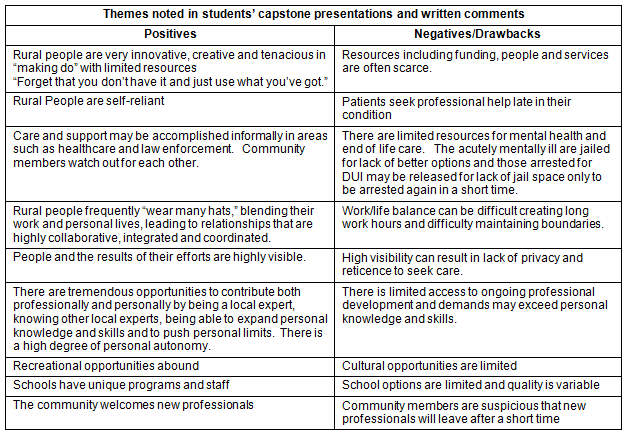
The most commonly cited positive theme was the high degree of collaboration the students observed among community members. Even though each small group was investigating a different area of community life, they encountered overlaps among people who work in fields such as education, government, healthcare and business. They also found that health care is frequently a major component of the local economy. Another frequent theme is the resourcefulness of rural people in banding together to create local solutions with limited resources because they personally 'own' the problems and have a personal stake in solutions. Students also identified that living in a small community would afford them with the chance to have a greater personal impact on local policies, events and systems, as well as to engage in the full scope of their profession.
The students' most commonly cited concern was that they heard repeatedly about the limited funding available for public services such as law enforcement, public health and mental health. The students also noted concerns about the availability and quality of educational and community services for their future children. The outlook for their professional income was also frequently cited as a concern. Several students noted that rural healthcare professionals need to more broadly trained and skilled than their urban counterparts.
Overall, the students frequently were impressed with the friendliness and openness with which they were greeted and the fact that people in the community generously gave of their time and expertise to answer their questions. While community members were eager to tell them about the positive aspects of rural life, they were also open and honest about some negative aspects such as substance abuse, lack of mental health services and the 'revolving door' of healthcare providers who come and go after completing a service obligation for loan repayment.
Finally, the $500 stipend for each participating student is a substantial program expense. However this is believed to be necessary because the program is conducted when students are not registered for classes, and many would otherwise be working to defray their educational expenses. During the 2011 program, the students were asked how important the stipend was in their ability to participate, and only 3 of the 18 who responded indicated that the stipend was essential.
Discussion
The rural immersion program provides students from seven health professions and their spouses/partners with the opportunity to concentrate on learning about rural community life while physically located in that community for 5 days. They reported overwhelmingly positive responses to the experience. Providing students with 5 days dedicated to non-clinical considerations appears to be unique. One other program for only medical and pharmacy students reports similar activities for a single off-campus day preceded by structured on-campus didactics10.
Even though they are a self-selected group with an established interest in future rural life and work, it is clear from their responses that they are open to both the positives and negatives of 'going rural' and are actively involved in seeking answers to their personal questions about that choice. For that reason, offering this experience to health professions students who are already predisposed to rural life and work is a very useful exercise at this point in their career when most have been studying in urban academic centers for many years and are weighing up future options. At this point they have developed questions about their future and the immersion experience provides an opportunity to visualize themselves in the location they are visiting.
The students noted that many of the features of rural professional life can be viewed as either positive or negative depending on an individual's personal preferences, for example life/work overlap, scope of practice and professional autonomy. Those who find personal and professional satisfaction in knowing and being known around town and in feeling part of the community welcome rural life/work overlap; those who want to be anonymous may be more suited to urban practice. Those who want to practice to fullest extent of their professional skills will be more able to do so in a rural area.
Funding for this program is secured from a number of generous funders who are attracted to its value in addressing Colorado's healthcare workforce shortage. The students' responses document that the great majority of them experience increased or reinforced interest in future rural practice as a result of their participation. The apparent willingness of the majority of students to participate without a stipend presents an opportunity to significantly decrease the cost of the program.
Each year, the participants are asked for suggestions to improve the program and these have been incorporated in subsequent years. The main recommendations were for more free time and for more time to prepare their presentations. In future years, it is planned to provide more pre-week opportunities for students from various disciplines to meet because many had not met before the week commenced. It is also hoped to increase the variety of healthcare disciplines represented, to invite participation from other graduate level disciplines such as law, engineering and business and to increase the number of spouse/partners attending.
The results may not reflect the effects that this program would have on students who do not have a pre-established interest in rural life and work. This constitutes an area for further study.
The students already considering future rural practice found that the Interdisciplinary Rural Immersion Program reinforced their interest in rural life and work. Although they have other opportunities for clinical rotations at rural sites, they are preoccupied with clinical duties and may not have the time or opportunity to engage in the larger community or explore interdisciplinary activities. The rural immersion week provides them with the time, structure and permission to move out of their clinical 'comfort zone' and think about the cultural, economic and environmental aspects of rural life and work. Funders committed to addressing the rural healthcare workforce shortage are willing to support this type of program. Other educational institutions wishing to increase rural interest on the part of their students may find that establishing programs similar to the one described in this report may help them meet their goals.
Acknowledgements
Funding and other in-kind support for this program came from the following sources, none of which had any role in designing, conducting, collecting, analyzing or interpreting the data or in the preparation or editing of the manuscript: The Caring for Colorado Foundation, The Colorado Trust, The Kaiser Foundation, Northeast Junior College and Adams State College.
References
1. Rabinowitz HK, Diamond JJ, Markham FW, Paynter NP. Critical Factors for Designing Programs to Increase the Supply and Retention of Rural Primary Care Physicians. JAMA 2001; 286: 1041-1048.
2. Dunbabin JS, Levitt L. Rural origin and rural medical exposure: their impact on the rural and remote medical workforce in Australia. Rural and Remote Health 3(1): 212. (Online) 2003. Available: www.rrh.org.au (Accessed 1 May 2012).
3. Colorado Rural Health Center. Colorado's rural, urban, and frontier counties. (Online) 2010. Available: http://www.coruralhealth.org/resources/documents/countytypemap.pdf (Accessed 17 May 2012).
4. Colorado Department of Public Health and Environment. Primary care health professional shortage. (Online) 2011. Available: http://www.cdphe.state.co.us/pp/primarycare/shortage/pchpsa.pdf (Accessed 17 May 2012).
5. The Colorado Trust. Addressing Colorado's primary care provider shortage; public policy agenda 2011. (Online) 2011. Available: http://www.coloradotrust.org/attachments/0001/3811/Final_WorkforcePolicyAgenda2011-single-page.pdf (Accessed 17 May 2012).
6. Low Country AHEC. South Carolina rural interdisciplinary program of training. (Online) no date. Available: http://www.lcahec.com/script.html (Accessed 17 May 2012).
7. Medves J, Paterson M, Chapman CY, Young JH, Tata E, Bowes D et al. A new inter-professional course preparing learners for life in rural communities. Rural and Remote Health 8: 836. (Online) 2008. Available: www.rrh.org.au (Accessed 25 March 2012).
8. Shannon CK, Baker H, Jackson J, Ory A, Heady H, Gunel E. Evaluation of a Required Statewide Interdisciplinary Rural Health Education Program: Student Attitudes, Career Intents and Perceived Quality. Education for Health 2005; 18(3): 395-404.
9. Toussaint S, Mak DB. 'Even if we get one back here, it's worth it...': evaluation of an Australian Remote Area Health Placement Program. Rural and Remote Health 10: 1546. (Online) 2010. Available: www.rrh.org.au (Accessed 25 March 2012).
10. Sisson DC, Westra RE. Impact of a Rural Interprofessional Experience in Rural Communities on Medical and Pharmacy Students. Family Medicine 2011; 43(9): 653-658
11. Kazanjian A, Pagliccia N. Key factors in Physicians Choice of a Practice Location: Findings from a survey of practitioners and their spouses. Health & Place 1996; 2(1): 21-34.
12. Eley DS, Synnott R, Baker PG, Chater AB. A decade of Australian Rural Clinical School graduates - where are they and why? Rural and Remote Health 12: 1937. (Online) 2012. Available: www.rrh.org.au (Accessed 25 March 2012).




