Many rural and remote regions of Australia struggle to attract and retain medical staff1. Rural clinical schools were established by the Australian Government in 2002 and were funded as part of a long-term strategy to expand the rural medical workforce. There is growing evidence that regional medical schools and Australian rural clinical schools are increasing the numbers of doctors working regionally and rurally2-5.
Tasmania, an island state, has poorer health outcomes and fewer doctors than other states, and the smaller outer regional, remote and very remote towns have patients with the worst health6. These towns have lower socioeconomic status, higher Aboriginality, are under-represented in post-school education statistics, and have reduced access to health services6,7. Attracting and retaining medical staff to these communities remains a major challenge. The north-west coast of Tasmania, the home of the University of Tasmania School of Medicine's Rural Clinical School (UTAS RCS), has fewer general practitioners (GPs) than remote areas of Australia. In 2014 there were 118 GPs working in north-western Tasmania8, which has a population of 110 0009. In 2011 there were 227.8 GPs per 100 000 persons in major cities in Australia, twice that of remote areas (113.0 per 100 000 persons)10. Like many rural Australian areas, health services in north-western Tasmania remain heavily dependent on locum staff and overseas-trained doctors11,12.
All of Tasmania is considered regional or remote under the Australian Standard Geographic Classification - Remoteness Areas (ASGC-RA), including the capital city, Hobart, which is RA213. The Modified Monash Model12,14, a newer classification of regional and remote areas, is able to better differentiate the major cities of Hobart and Launceston, which are category 2 (RA2 or 3, with populations over 50 000), from the remaining regional cities and small towns, which are categories 3-7.
Students enrolled in the UTAS School of Medicine (SoM) undergraduate medical program all spend their first 3 years in Hobart. Thereafter, students can choose to spend their two clinical years in one of three clinical schools: in Hobart, in Launceston or at the rural clinical school based on the north-western coast of Tasmania.
This study sought to assess the proportion of UTAS RCS graduates currently working in rural areas in Australia compared to those UTAS SoM graduates that did not spend a year studying at the UTAS RCS. These early outcomes are compared to published university and rural medical school outcomes. In addition, the study sought to determine the proportions of UTAS SoM and UTAS RCS graduates working in the regional cities and smaller towns in Tasmania, categories 3-7 of the Modified Monash Model.
The cohort study consisted of all graduates of the UTAS SoM between 2002 and 2013. Graduates who had graduated since 2002 were searched for on the Australian Health Practitioner Register (AHPRA) database. The AHPRA database records the graduate's name and postcode where they currently work. Graduates' 2014 primary place of work postcodes were used to identify remoteness classifications from the postcode search function on the DoctorConnect website http://www.doctorconnect.gov.au/internet/otd/Publishing.nsf/Content/locator), where RA1 - major cities; RA2 - inner regional; RA3 - outer regional; RA4 - remote; and RA5 - very remote. Remoteness classifications were investigated in two ways: RA2-5 and RA3-RA5. Tasmanian population data for the Tasmanian postcodes were obtained from the Australian Bureau of Statistics. This allowed remoteness areas to be differentiated according to the Modified Monash Model for graduates working within Tasmania. Only Tasmanian regions are used in this study as the model still requires external validation in each state14.
Data were entered into an Excel spreadsheet then imported into the Statistical Package for the Social Sciences v21 (IBM; http://www.spss.com) for analysis. Frequencies were run to describe the data, with percentages calculated for categorical data, means with standard deviations calculated for normally distributed scale data, and medians and interquartile ranges (IQR) calculated for non-parametric data. Pearson's χ2 and Fisher's exact tests were used to investigate differences in categorical variables between students who had spent at least a year at UTAS RCS and UTAS SoM graduates who only attended the other clinical schools. All tests were two-sided and p<0.05 significance level was used for all tests. Odds ratios (OR) with 95% confidence intervals (CI) were calculated for significant χ2 results.
Ethics approval
Ethics approval was gained from the Social Sciences Research Committee (Tasmania) network, references H12949 and H13913.
There were 974 graduates of UTAS SoM from 2002 to 2013, 202 (21%) of whom spent one or two clinical years at UTAS RCS. Median age at graduation was 24 years (IQR 23-26, range 22-59) for both the UTAS RCS and UTAS SoM graduates, and 508 (51%) graduates were women.
In 2014 a total of 105 (11%) of graduates were unable to be traced through the AHPRA database. AGSC remoteness classifications were available for the remaining 869 graduates. Figure 1 shows the number of UTAS medical graduates working in RA1 and RA3-5 areas by year of graduation. A larger proportion of UTAS RCS students were working in an AGSC RA2-5 area compared to UTAS SoM students (57% vs 49%, χ2(1)=4.3, p=0.038; OR 1.4, 95%CI 1.0-2.0) (Table 1). After restricting the rural category to RA3-5 (outer regional, rural or remote), the difference was considerably greater (28% vs 7%, χ2(1)=59.5, p<0.0001; OR 4.9, 95%CI 3.2-7.6). Female graduates were not more likely than men to be working in an RA3-5 area (53% vs 47%, χ2(1)=0.2, p=0.58).
There were 328 graduates working in Tasmania, with no difference between the schools for the proportion of graduates working in the state (37% vs 38%, χ2(1)=0.1, p=0.76). Twenty five of the 30 graduates working in north-western Tasmania, where the UTAS RCS is hosted, were UTAS RCS graduates. These graduates were predominantly (66%) working in the two postcodes where the two main regional hospitals are situated.
Among the 541 graduates working interstate (mainland Australia), 26 RCS graduates were working in RA3-5 areas, compared to 30 SoM graduates (22% vs 7%, χ2(1)=0.2, p<0.0001; OR 8.9, 95%CI 4.7-17.2). Among the 328 graduates working in Tasmania, 22% were working in RA3-5 areas compared to 7% of SoM graduates (χ2(1)=22.7, p<0.0001; OR 3.8, 95%CI 2.1-6.6).
The Modified Monash Model was applied to the Tasmanian context only. This excluded 531 students who were working interstate in 2014. Among the remaining 328 students, 30 RCS and 21 SoM graduates were working in Modified Monash Model categories 3-5 areas (44% vs 8%, χ2(1)=53.3, p<0.0001; OR 8.9, 95%CI 4.7-17.2) (Table 2). The UTAS RCS supplied 109 graduates per 100 000 people to Modified Monash Model category 2 areas in Tasmania and 16 per 100 000 graduates to category 3 areas in Tasmania (Table 3).
Table 1: Graduates of the University of Tasmania School of Medicine (2002-2013) practice locality
in Australia, 2014, using Australian Standard Geographic Classification - Remoteness Areas
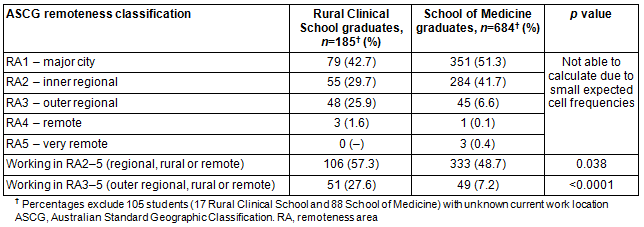
Table 2: Supply of medical graduates to Tasmania using Modified Monash Model
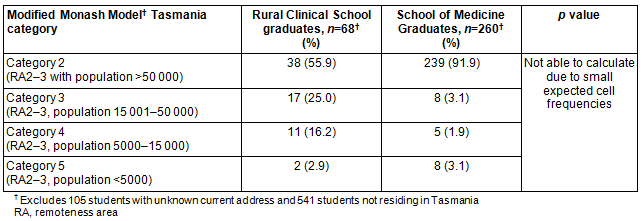
Table 3: Supply of medical graduates to Tasmania, per 100 000 people, using Modified Monash Model
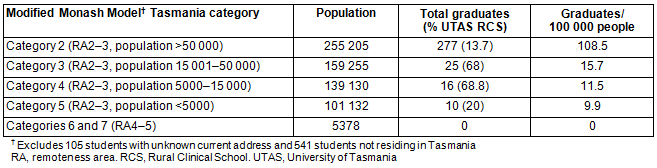
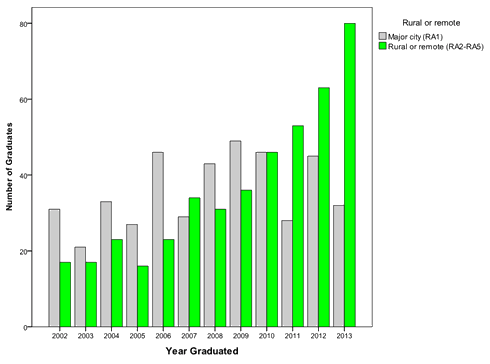
Figure 1: University of Tasmania School of Medicine (including Rural Clinical School)
graduate locality in Australia, 2014, differentiated by remoteness areas 2-5.
Discussion
The UTAS School of Medicine in Tasmania supplies a significant proportion of graduates to the medical workforce in Tasmania. Tasmanian graduates appear more likely to work regionally and rurally than those graduates trained in capital cities on the mainland. Whereas over 49% of graduates in this study were working in RA2-5, 16% of graduates of a rural clinical school cited in a Western Australia study were working in RA2-53; however, this reflects the classification of the Tasmanian capital (Hobart) as RA2 compared with RA1 state capitals on the mainland. The early placement data shows that the 49% working in RA2-5 is most comparable to the regional James Cook University in northern Queensland, where 60% of graduates worked in RA2-54.
When rurality was defined by ASGC RA3-5, graduates that spent at least a year at the UTAS RCS were significantly more likely to work in rural and remote areas (RA3-5) than those UTAS SoM graduates that did not attend the UTAS RCS (27% vs 7%).
The Modified Monash Model helped to illustrate the difference in supply of medical graduates to sparsely populated areas of Tasmania. While it is expected that more graduates would work in Hobart and Launceston, because the bigger hospitals are in these cities, regional hospitals are based in some of the smaller cities (ie Burnie and Devonport). The data does show that both proportionally and absolutely the UTAS RCS is supplying graduates to the smaller cities and towns of Tasmania.
The UTAS RCS started taking students as early as 2002 but had very limited numbers for the first 5 years whilst its infrastructure was being built. The UTAS RCS reached its training quota of 25% of all domestic students in 2009. Most of the UTAS graduates now working in north-western Tasmania are graduates of the UTAS RCS in their early postgraduate years (PGY1-3), reflecting the dates that the UTAS RCS took on larger cohorts of students.
While the data collected is a snapshot of workplaces of UTAS graduates it also demonstrates trend. Doctors in their early years of training are choosing to work in rural locations, but there is a drift back to urban areas, which is particularly evident after PGY3 (Fig1). One possible reason for the urban drift after PGY1-3 is that doctors currently need to move back to the cities to access specialist training. This effect might be reduced with expanded numbers of general practice places in rural and regional areas, allowing more general practitioners to train where they are needed most15. Continued development of regional postgraduate specialty programs is needed to allow graduates to continue their training in regional or rural areas16.
Limitations
The UTAS RCS only started graduating significant numbers in the last 5 years. Doctors take at least another 10 years to finish training and to gain general practice and specialist posts, so these are early figures. Tracking postgraduate choices will continue through the AHPRA database to identify where graduates actually end up in established practice.
This study adds to the growing evidence that training medical students in rural areas delivers graduates that work rurally. The additional year spent in a rural area, even when their medical school is in a regional area, significantly affects their workplace choices over the first 3 years post-graduation. Rural areas that are underserviced need to train medical students locally, even if there is a regional university. The data showed that graduates that train as little as 4 hours away are unlikely to move to work to these areas. The data also confirms the urgent need to align postgraduate training to ensure that more training is undertaken regionally and remotely.
References
1. Australian Insititute of Health and Welfare. Medical workforce 2013. National Health Workforce Series No. 8 (Cat. No. HWL 54). Canberra, ACT: AIHW, 2014.
2. Jamar E, Newbury J, Mills D. Early career location of University of Adelaide rural cohort medical students. Rural Remote Health 14: 2592. (Online) 2014. Available: www.rrh.org.au (Accessed June 2014).
3. Playford DE, Evans SF, Atkinson DN, Auret KA, Riley GJ. Impact of the Rural Clinical School of Western Australia on work location of medical graduates. Medical Journal of Australia 2014; 200(2): 104-107.
4. Sen Gupta T, Woolley T, Murray R, Hays R, McCloskey T. Positive impacts on rural and regional workforce from the first seven cohorts of James Cook University medical graduates. Rural Remote Health 14: 2657. (Online) 2014. Available: www.rrh.org.au (Accessed June 2014).
5. Young L, Kent L, Walters L. The John Flynn Placement Program: evidence for repeated rural exposure for medical students. Australian Journal of Rural Health 2011; 19(3): 147-153.
6. Department of Health and Human Services, Tasmania. State of Public Health 2013. Population health. (Online) 2013. Available: http://www.dhhs.tas.gov.au/__data/assets/pdf_file/0017/132263/State_of_Public_Health_2013_LR.pdf (Accessed July 2014).
7. Mooney G. The health of nations. London: Zed Books, 2012.
8. Tasmanian Health Directory. Tasmania Medicare Local. (Online) 2014. Available: http://www.tasmedicarelocal.com.au/tasmanian-health-directory. (Accessed June 2014).
9. Australian Bureau of Statistics. Census 2011 QuickStats. (Online) 2011. Available: http://www.abs.gov.au/websitedbs/censushome.nsf/home/quickstats (Accessed March 2014).
10. Australian Bureau of Statistics. Australian social trends. Doctors and nurses. Cat. no. 4102.0. (Online 2013). http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/4102.0Main+Features20April+2013#p11 (Accessed June 2014).
11. House of Representatives Senate Committee on Health and Ageing. Australia's medical workforce. (Online) 2012. Available: http://www.aihw.gov.au/WorkArea/DownloadAsset.aspx?id=60129546076 (Accessed June 2014).
12. Mason J. Review of Australian government health workforce programs. (Online) 2013. Available: http://www.health.gov.au/internet/publications/publishing.nsf/Content/work-review-australian-government-health-workforce-programs-toc~chapter-4-addressing-health-workforce-shortages-regional-rural-remote-australia~chapter-4-reform-asgc-ra-rural-classification-system (Accessed May 2014).
13. Australian Bureau of Statistics. Australian Statistical Geography Standard (ASGS). Volume 5 - remoteness structure. (Online) 2011. Available: http://www.abs.gov.au/ausstats/abs@.nsf/Latestproducts/2C28C8B6013FB2D0CA257B03000D6DA8 (Accessed March 2014).
14. McGrail MR, Humphreys JS. A new index of access to primary care services in rural areas. Australian and New Zealand Journal of Public Health 2009; 33(5): 418-423.
15. Dutton P. Rebuilding general practice training. Australian Government Department of Health media release. (Online) 2014. Available: http://www.health.gov.au/internet/budget/publishing.nsf/content/5EF709B6979A1657CA257CD500810CA2/$File/Rebuilding%20General%20Practice%20Training.pdf (Accessed July 2014).
16. Sen Gupta TK, Manahan DL, Lennox DR, Taylor NL. Comment on 'Rural generalism and the Queensland Health pathway - implications for rural clinical supervisors, placements and rural medical education providers'. Rural Remote Health 13(3): 2765. (Online) 2013. Available: www.rrh.org.au (Accessed July 2014).




